Abstract
The cancer stem cell (CSC) theory states that many types of cancer, including nasopharyngeal cancer (NPC), are initiated from and maintained by CSCs, which may be responsible for tumor relapse and resistance to therapy. It is imperative that nasopharyngeal cancer stem cells (NPCSCs) be specifically targeted to eradicate NPC and prevent recurrence. Epigallocatechin-3-gallate (EGCG) inhibits cancer progression by attenuating NF-κB p65 activity, which is upregulated in CSCs and plays an important role in epithelial–mesenchymal transition (EMT). The purpose of this study is to confirm the self-renewal and migration inhibitory effects of EGCG toward NPCSCs and to clarify its mechanism of activity. We enriched and characterized NPCSCs by collecting spheroid-derived cells grown in serum-free medium (SFM) and examined the effects of EGCG on the characteristics of NPCSCs and studied the underlying mechanisms using soft agar colony assays, transwell migration assays, reverse transcriptase polymerase chain reaction (RT-PCR), Western blot analysis, immunofluorescence staining, and xenograft studies. NPC spheroids enriched from NPC cell lines acquired CSC traits and underwent EMT. EGCG inhibited the NPCSCs’ self-renewal and migration and reversed EMT, and combined treatment with EGCG and cisplatin reduced the growth of CSC tumor xenografts. Moreover, EGCG inhibited NF-κB p65 activity by modulating the cellular localization of p65 and decreasing the transcriptional regulation of NF-κB p65 on Twist1 expression. NF-κB p65 is a novel therapeutic target in NPCSCs, and the inhibition of activated NF-κB p65 in CSCs by EGCG may offer an effective treatment for NPC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Nasopharyngeal cancer (NPC) is a malignant epithelial carcinoma of the head and neck region, and its incidence is high throughout southeast Asia, southern China, and the Mediterranean basin; the 5-year overall survival rate is ∼70 % [1, 2]. NPC has high metastatic potential with frequent initial dissemination to regional lymph nodes. With advances in radiation therapy, excellent local control can be achieved; however, 30–40 % of patients develop distant metastases within 4 years, and these are responsible for the majority of NPC-related deaths [3–5]. Thus, the prognosis remains poor for a large number of NPC patients with metastatic or relapsed disease. Therefore, it is essential to develop a deeper understanding of the mechanisms of NPC progression and to evaluate novel therapies.
To date, evidence has accumulated in support of the cancer stem cell (CSC) theory, which states that many types of cancer initiate from and are maintained by a small population of tumorigenic cells known as CSCs, which exhibit capacities for self-renewal, differentiation, and metastasis [6–8]. In addition, recent studies have indicated that CSCs may be responsible for tumor relapse and resistance to therapy [9, 10]. Accumulating evidence has demonstrated that a variety of human malignancies, including NPC, contains subpopulations of cells that exhibit stem cell-like properties in part as a result of the epithelial–mesenchymal transition (EMT) [11, 12]. EMT increases cancer cell tumorigenicity, establishes a crucial link to metastasis, and eventually results in CSC properties in several human malignancies, including NPC [13, 14]. Therefore, to eradicate NPC and prevent recurrence, specifically targeting CSCs in NPC is imperative.
Green tea is one of the most popular beverages in the world [15]. Significant data amassed from many laboratories around the world have provided convincing evidence that epigallocatechin-3-gallate (EGCG), the most abundant catechin in green tea, is a potent chemopreventative agent against a variety of cancers [16–18]. Moreover, a number of studies have demonstrated in vitro and in vivo that EGCG potently inhibits cancer cell growth, invasion, angiogenesis, and metastasis and induces apoptosis through various molecular targets [19–23]. Notably, recent studies have suggested great potential for EGCG to be used as a chemopreventative agent to target CSCs through several regulatory mechanisms [24–27]. However, the involvement of EGCG in mediating these molecular mechanisms and the therapeutic targets involved in NPCSCs has been largely unexplored.
Nuclear factor kappaB (NF-κB) is a ubiquitous transcription factor, and p65 is the key active subunit of NF-κB signaling that is closely involved in the deregulation of the NF-κB pathway. Aberrant or constitutively active NF-κB p65 is associated with many physiological functions, including inflammation, cellular proliferation, and malignant transformation [28]. Studies have shown that NPC development and progression are closely related to NF-κB p65 activation [29]. New research has suggested that NF-κB p65 activation and its signaling pathway play an important role in the EMT process for NPC [30, 31]. Interestingly, evidence supports the inhibition of NF-κB p65 activation by EGCG in both normal human epidermal cells and cancer cells [32–34]. Therefore, we hypothesized that EGCG could modulate EMT and inhibit the self-renewal and migration capacity of NPCSCs through the inactivation of NF-κB p65.
Non-adherent spheroid assays are increasingly used to enrich and characterize stem cells. These cells may represent a tumor-initiating subpopulation with capacities for self-renewal and unlimited proliferation [35]. We demonstrated that the spheroid-derived NPC cells showed increased invasion, migration, and tumorigenesis compared with their parental cells and that they expressed CSC-related genes and EMT markers; these cells served as model CSCs for further experiments.
The objectives of our study were to enrich and characterize NPCSCs using spheroid-derived cells, to further reveal the anti-tumor effects of EGCG in NPCSCs, and to elucidate the underlying mechanism of the anti-tumor effects of EGCG through the suppression of NF-κB p65 activation.
Materials and methods
Reagents
Dulbecco’s modified Eagle’s medium F12 (1:1 volume, DMEM/F12) and fetal bovine serum (FBS) were purchased from Gibco (USA). Accutase was purchased from Innovative Cell Technologies, Inc., and 1 % penicillin–streptomycin and 2 % B27 supplement were purchased from Invitrogen (Carlsbad, CA, USA). Epidermal growth factor (EGF) and human recombinant basic fibroblast growth factor (bFGF) were purchased from PeproTech (USA). Epigallocatechin-3-gallate (EGCG), crystal violet, and trypsin were purchased from Sigma Aldrich (St. Louis, MO, US). Boyden chambers and polycarbonate membranes (8-mm pore size) for cell invasion assays were obtained from Neuroprobe, Inc. (Gaithersburg, MD). The antibodies against GAPDH, Lamin B1, Bmi-1, Vimentin, E-cadherin, and N-cadherin were purchased from Cell Signaling Technology (Beverly, MA, US). The antibodies against Twist1, NF-κB p65, and P-p65 were obtained from Abcam (Cambridge, MA). Peroxidase-conjugated goat anti-rabbit or anti-mouse secondary antibodies were purchased from Beijing Zhongshan Jinqiao Biotechnology Co., Ltd. (Beijing, China). Nude mice, 4–6 weeks old, were obtained from the Animal Experimental Center of Chongqing Medical University.
Cell culture
To culture the parental monolayer cells, the human NPC cell lines CNE2 and C666-1 were obtained from the cell collection of Chongqing Medical University. The parental cells were cultured in DMEM supplemented with 10 % fetal bovine serum and 1 % penicillin–streptomycin. The cells were cultured in an incubator with 5 % CO2 at 37 °C. For tumor spheroid cell (SC) culture, the tumor spheroids of CNE2 and C666-1 cells were grown in a non-adhesive culture system. Serum-free medium (SFM) consisted of DMEM-F12 supplemented with 2 % B27 supplement, 20 ng/ml bFGF, 20 ng/ml EGF, and 1 % penicillin–streptomycin. Briefly, parental single-cell suspensions were collected and adjusted to a density of 1 × 106/ml; they were then resuspended in T25 or smaller glass culture bottles containing SFM, placed vertically in an incubator, and shaken several times a day. Half of the culture medium was changed every 2–3 days until tumor spheroid formation occurred. The tumor spheroids were dissociated with Accutase to generate single cells, passaged every 6–8 days, and allowed to re-form tumor spheroids.
Tumor spheroid formation assay
To assess self-renewal in vitro, spheroid cells were dissociated into single cells, which were plated in six-well ultra-low attachment plates at a density of 2000 cells/ml in SFM in a humidified incubator (5 % CO2) at 37 °C. On the second day after seeding, tumor spheroids were treated with 0–50 μM EGCG. Spheroids in each well were photographed after 7 days of incubation, collected, and dissociated with Accutase. The cells obtained after dissociation were sieved through a 40-μm filter and counted using a Bio-Rad TC10 Automated Cell Counter (Bio-Rad, USA) and trypan blue dye.
Soft agar colony assay
The NPC parental cells and spheroid-forming cells were dissociated and suspended (103 cells/mL) in 2 mL of 0.3 % agar with SFM overlaid into six-well plates containing a 0.6 % agar base. After the spheroid cells were treated with various doses of EGCG or lentivirus transfection, the plates were incubated for 3 weeks, and the number of spheroids >0.2 mm in diameter were evaluated by light microscopy (Olympus). Three independent experiments were performed.
Transwell migration assay
The cell migration assay was performed with 24-transwell chambers. In brief, the cells were resuspended in SFM at a concentration of 5 × 105 cells/ml. The upper chamber was loaded with 100 μl of cell suspension, and the lower chamber was loaded with 500 μl of serum-containing medium. The cells were fixed after 24 h of incubation with methanol and stained with 0.1 % crystal violet. The number of cells invading through the membrane was counted under a light microscope (Olympus), and six random fields were analyzed; three independent experiments were performed.
Trypan blue assay
Spheroid cells were dissociated with Accutase into single cells, which were plated and seeded into 24-well plates at a density of 1 × 105 cells per well. The cells were then treated as specified. After treatment, the medium was aspirated, and the cells were washed with PBS. Ten microliters of cell suspension was mixed with 10 mL of trypan blue, and the total number of viable cells was determined using a Bio-Rad TC10 Automated Cell Counter (Bio-Rad, USA). The values are expressed as the percent change compared with the total control cells.
Quantitative reverse transcriptase polymerase chain reaction
For the quantification of gene expression, real-time polymerase chain reaction (RT-PCR) was performed with SYBR Green on an ABI PRISMW 7900HT system (Applied Biosystems, Foster City, CA, USA). Briefly, total RNA was isolated from cells using TRIzol reagent (Invitrogen, Carlsbad, CA), and cDNA was synthesized from total RNA using a reverse transcriptase kit (Fermentas) according to the manufacturer’s instructions. PCR was performed in a real-time PCR system, and the expression levels of target genes relative to GAPDH were determined using a SYBR Green-based comparative CT method (relative fold change = 2ΔΔCT). The primers were designed by Sangon Biotech Co. Ltd. (Shanghai, China) and are as follows:
- CD44:
-
Forward: 5′-AAGGAGCAGCACTTCAGGAG-3′
Reverse: 5′-ATCCCAGGTTTCTTGCCTCT-3′
- NF-κB p65:
-
Forward: 5′-GGAGCACAGATACCACCAAGA-3′
Reverse: 5′-CGGCAGTCCTTTCCTACAAG-3′
- Bmi-1:
-
Forward: 5′-CCTGATGTGTGTGCTTTGTG-3′
Reverse: 5′-GGTCTGGTCTTGTGAACTTGG-3′
- Twist1:
-
Forward: 5′-GAGCAAGATTCAGACCCTCAA-3′
Reverse: 5′-CATCCTCCAGACCGAGAAG-3′
- E-cadherin:
-
Forward: 5′-TCGTCACCACAAATCCAGTG-3′
Reverse: 5′-CATTCACATCCAGCACATCC-3′
- N-cadherin:
-
Forward: 5′-CAGATGCGTGAAATGGAAGA-3′
Reverse: 5′-TGGAAGAGGCAGAGAAATCC-3′
- Vimentin:
-
Forward: 5′-TGAATACCAAGACCTGCTCAA-3
Reverse: 5′-ATCAACCAGAGGGAGTGAATC-3
- GAPDH:
-
Forward: 5′-ACGGGAAGCTCACTGGCATGG-3′
Reverse: 5′-GGTCCACCACCCTGTTGCTGTA-3′
Virus-shRNA generation and cell transfection
The NF-κB p65 shRNA constructs (pMAGi c 7.1) were from Shanghai Sunbio (Shanghai, China) with the following sequences:
-
p65 shRNA1-1, sense 5′-CCGGGGAGCACAGATACCACCAATTCAAGAGATTGGTGGTATCTGTGCTCCTTTTTTG3′;
-
p65 shRNA1-2, anti-sense 5′-AATTCAAAAAAGGAGCACAGATACCACCAATCTCTTGAATTGGTGGTATCTGTGCTCC-3′;
-
p65 shRNA 2-1, sense 5′-CCGGGGACATATGAGACCTTCAATTCAAGAGATTGAAGGTCTCATATGTCCTTTTTTG-3′;
-
p65 shRNA 2-2, anti-sense 5′-AATTCAAAAAAGGACATATGAGACCTTCAATCTCTTGAATTGAAGGTCTCATATGTCC-3′;
-
p65 shRNA 3-1, sense 5′-CCGGTCTTCCTACTGTGTGACAATTCAAGAGATTGTCACACAGTAGGAAGATTTTTTG-3′;
-
p65 shRNA 3-2, anti-sense 5′-AATTCAAAAAATCTTCCTACTGTGTGACAATCTCTTGAATTGTCACACAGTAGGAAGA-3′;
-
control-1, sense 5′-CCGGTTCTCCGAACGTGTCACGTTTCAAGAGAACGTGACACGTTCGGAGAATTTTTG-3′; and
-
control-2, anti-sense 5′-AATTCAAAAATTCTCCGAACGTGTCACGTTCTCTTGAAACGTGACACGTTCGGAGAA-3′.
p65 shRNA2 effectively decreased the p65 expression levels and was employed in the following experiments. The pMAGic7.1 lentiviral vector (Shanghai Sunbio), which codes for green fluorescent protein (GFP) and puromycin driven by the RNA polymerase III-specific promoter hU6, was used for shRNA expression. The AgeI and EcoRI sites in pMAGic 7.1 were used to introduce the annealed shRNA oligonucleotides. To anneal the shRNA oligonucleotides, 600 pmol of each of the two oligos was annealed in 50 μl of 0.1 M NaCl and 10 mM Tris HCl (pH 7.6) by heating to 95 °C and cooling to room temperature. Ten nanomoles of annealed shRNA oligonucleotides were ligated to 120 ng of vector cut with AgeI and EcoRI in a 20-μl reaction containing 1 μl of T4 DNA ligase (Fermentas) overnight at 16 °C. These vectors were verified by sequencing and by PCR using the forward primer hU6-F2 (5′-TACGATACAAGGCTGTTAGAGAG-3′) and the reverse primer pM-R(5′-CTATTAATAACTAATGCATGGC-3′). The lentivirus was produced by Shanghai Sunbio (Shanghai, China). Lentiviral infection was performed by adding the virus-shRNA-NF-κBp65 solution to NPCSCs dissociated at the desired multiplicity of infection in the presence of 8 ng/mL polybrene. The expression levels of NF-κB p65 in NPCSCs were evaluated by real-time RT-PCR and Western blot analysis, and the transfected cells were used for future experiments.
Western blot analysis
The proteins of the parental adherent and tumor spheroid cell lysates were prepared in RIPA buffer [50 mM Tris/HCl, pH 7.5, 150 mM NaCl, 1 % (w/v) sodium deoxycholate, 1 % (v/v) Triton X-100, and 0.1 % (v/v) SDS] containing 10 mg/ml each of leupeptin, aprotinin, antipain, pepstatin A, and chymostatin (all from Sigma Aldrich). Then, 40 mg of protein cell lysates was separated on 8 % SDS-PAGE gels, electroblotted onto nitrocellulose membranes, blocked in blocking solution [5 % (w/v) non-fat dried skim milk in Tris-buffered saline with 0.1 % Tween 20 (TBS-T)] for 1 h at room temperature and incubated with primary antibodies overnight at 4 °C. The primary antibodies were as follows: rabbit anti-GAPDH and anti-Lamin B1 (Cell Signaling Technology) diluted 1:1000; rabbit anti-E-cadherin, rabbit anti-bmi-1, rabbit anti-N-cadherin, and rabbit anti-Vimentin (Cell Signaling Technology) diluted 1:1000; and mouse anti-Twist1, rabbit anti-NF-κB p65, and rabbit anti-p-p65(Abcam) diluted 1:1000. Primary antibodies were detected with peroxidase-conjugated goat anti-rabbit or anti-mouse secondary antibodies (Beijing, Zhongshan GoldenBridge Biotechnology Co) diluted 1:3000 in blocking solution for 1 h at room temperature. Antibody-bound proteins were detected with the BeyoECL Plus kit (Beyotime Institute of Biotechnology) and a Western blotting analysis system (Bio-Rad, USA). The proteins were normalized to GAPDH or Lamin B1 and quantified using the ChemiDocTM XRS (Bio-Rad, USA). Three independent experiments were performed.
Immunofluorescence staining
The parental or spheroid cells treated with 50 μmol EGCG for 24 h were plated onto poly-l-lysine-coated glass coverslips and fixed in 4 % paraformaldehyde for 20 min at room temperature. After washing with PBS, the cells were permeabilized with 0.1 % Triton X-100 and blocked with 10 % BSA. The slides were incubated overnight at 4 °C with rabbit anti-NF-κB p65 and rabbit anti-CD44 primary antibodies (Abcam) followed by incubation with secondary fluorescein-conjugated antibodies (AlexaFluor 594, Invitrogen) at room temperature for 1 h. The slides were counterstained with 40-6-diamidino-2-phenylindole (DAPI) and analyzed under a Leica DM 4000B (Leica Microsystems) fluorescent microscope. Three independent experiments were performed.
FACS analysis
The cells were dissociated into single-cell suspensions, washed and resuspended in PBS, counted, and adjusted to 1 × 106 cells per group. The cells were incubated with the appropriate concentration of control or anti-CD44-FITC (Miltenyi Biotec). The proportion of CD44+ cells in each sample was detected by flow cytometry using a FACSCalibur machine (BD Biosciences). The IgG isotype was included as a negative control.
Xenograft tumorigenicity
NPC spheroid cells were treated for 48 h with cisplatin (10 μM) alone, cisplatin (10 μM) plus EGCG (20 μM), or control dimethylsulfoxide (DMSO) in vitro. Then, sorted cells were harvested, centrifuged, washed thoroughly with phosphate-buffered saline (pH 7.4) and adjusted to appropriate concentrations. A total of 5 × 105 cells was subcutaneously injected into the flank regions of 4–6-week-old male BALB/c nude mice. After treatment, tumor size and mouse body weight were monitored weekly. At the end of treatment, the tumors were harvested, and the tissue samples were used for immunohistochemistry analysis. All animal studies were approved by the Institutional Animal Care and Use Committee of Chongqing Medical University.
Luciferase reporter gene assay
Reporter constructs were modified from the psiCHECK-2 plasmid (Promega). The truncated promoter of Twist1NM_000474.3 (1951 bp) containing the predicted p65 binding seed sequence was designed by Shanghai Sunbio and cloned directly upstream of the firefly luciferase gene to create the psiCHECK-2-TWIST1 promoter-Wt plasmid. The site-specific mutation reporter plasmid (psiCHECK-2-TWIST1promoter-Mut) was then generated using the SunBio Cloning kit (SBO). psiCHECK-2-TWIST1promoter-Wt/-Mut (200 ng per well in a 24-well plate) with p65 shRNA lentivirus or NC was transfected into sorted NPCSCs. Twenty-four hours later, the cells were harvested and lysed with passive lysis buffer (Promega). Luciferase activity was measured using a Dual-Luciferase Reporter Assay System (Promega) on a TECAN Infinite M1000 Pro plate reader (TECAN). The luminescence intensity of firefly luciferase was normalized to that of Renilla luciferase.
Statistics
The values are expressed as the means and standard deviations (SD). Differences between groups were analyzed using Student’s t tests. All statistical analyses were performed using SPSS for Windows version 14.0. Values of p < 0.05 were considered significant.
Results
Tumor spheroid cells derived from the human NPC cell lines acquired CSC traits and underwent EMT
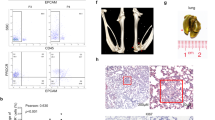
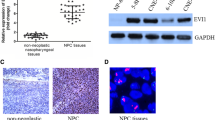
First, we investigated whether spheroid cells could be formed from human NPC CNE2 and C666-1 cell lines in a non-adherent culture system. The spheroid cells were cultured and routinely passaged in SFM (Fig. 1a). By immunofluorescence staining, we found that the expression of the CSC marker CD44 was significantly increased in CNE2 spheroid cells (CNE2-SCs) and C666-1 spheroid cells (C666-1-SCs) compared with the levels in the CNE2 and C666-1 parental cells (Fig. 1b). Moreover, the mRNA levels of the CSC markers CD44 and bmi-1 were increased in CNE2-SCs and C666-1-SCs compared with the parental cells. In addition, decreased mRNA expression of the epithelial marker E-cadherin was detected in spheroid cells; however, the expression of mesenchymal makers, such as N-cadherin and Vimentin, and the transcription factor Twist1, which is involved in EMT, were also increased in spheroid cells compared with the parental cells (Fig. 1c). These results confirmed that CNE2-SCs and C666-1-SCs had a stronger ability to self-renew and migrate than the parental cells (Fig. 1d, e).
Tumor spheroids derived from the human NPC cell lines acquired CSC traits and underwent EMT. a Representative phase-contrast micrographs of parental cells and spheroid cells formed from CNE2 (upper) and C666-1 (lower) cells. The spheroid cells were cultured and routinely passaged in a non-adherent culture system of serum-free medium (SFM) (magnification ×200). b Immunofluorescence showed that the expression of CD44 in CNE2 spheroid cells (CNE2-SCs) and C666-1 spheroid cells (C666-1-SCs) was significantly increased compared with the parental CNE2 and C666-1 cells using an anti-CD44 antibody (red) and DAPI (blue) to stain the nuclei (magnification ×400). c Real-time RT-PCR was used to analyze the mRNA expression of Bmi-1 and Twist1 and the mesenchymal markers N-cadherin and Vimentin; all were significantly increased. However, the epithelial marker E-cadherin was reduced in CNE2-SCs and C666-1-SCs compared with the parental cells. The internal control was the GAPDH gene, and the gene expression of the spheroid cells was normalized to that of the parental cells. d Comparison of the migration of the spheroid cells and parental cells by the transwell migration assay; representative micrographs (left) indicate that the migration of the CNE2-SCs and C666-1-SCs was greater than those of the CNE2 and C666-1 cells. The quantification (right) of migrating cells in the transwell migration assay. e Comparison of colony formation by the spheroid cells and parental cells by the soft agar colony assay; representative micrographs show the colony formation conditions of the CNE2-SCs and C666-1-SCs (left) and the quantification of colonies in the soft agar colony assay (right). The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the respective parental cells
Epigallocatechin-3-gallate inhibits the self-renewal and migration capacity of NPCSCs in vitro
To confirm that EGCG inhibited the growth of CSC spheroids enriched from the NPC cell lines CNE2 and C666-1 by detecting spheroid formation and cell viability in NPCSCs, CNE2-SCs and C666-1-SCs were grown in a non-adherent culture system and treated with various doses of EGCG (0–50 μM) for 7 days. At the end of the incubation period, the spheroids in each well were photographed. EGCG dose-dependently inhibited the growth of the spheroids in suspension (Fig. 2a). The spheroids from each treatment group were collected and resuspended to determine cell viability. EGCG dose-dependently inhibited NPCSC viability (Fig. 2b). To further examine the effects of EGCG on the self-renewal of NPCSCs with a colony formation assay, NPCSCs were grown in agar and treated with various doses of EGCG for 3 weeks. At the end of the incubation period, the colonies were photographed and counted. EGCG dose-dependently inhibited colony growth (Fig. 2c). These data suggested that EGCG effectively inhibits the self-renewal capacity of NPCSCs. To investigate the effects of EGCG on the invasion and migration of NPCSCs in vitro, the transwell migration assay was used. The number of NPCSCs treated with EGCG that migrated to the lower side of the membrane was significantly decreased compared to untreated NPCs; EGCG dose-dependently inhibited NPCSC migration (Fig. 2d).
Epigallocatechin-3-gallate (EGCG) inhibits the self-renewal and migration of nasopharyngeal cancer stem cells (NPCSCs) in vitro. a CNE2-SCs and C666-1-SCs were seeded in suspension and treated with various concentrations of EGCG (0–50 μM) for 7 days. Images of spheroids formed in suspension were captured using light microscopy. b After CNE2-SCs and C666-1-SCs were seeded in suspension and treated with EGCG (0–50 μM) for 7 days, the spheroids were collected and dissociated with Accutase. Cell viability was measured using the trypan blue assay. c EGCG inhibits the colony formation of NPCSCs; representative micrographs (left) show the colony formation by CNE2-SCs and C666-1-SCs treated with various concentrations of EGCG, and the quantification of colonies in the soft agar colony assay is shown at the right. d EGCG inhibits the migration of NPCSCs in a dose-dependent manner as determined by the transwell migration assay. Representative micrographs (left) show the cell migration of CNE2-SCs and C666-1-SCs treated with various concentrations of EGCG, and the quantification of cell migration in the transwell migration assay is shown at the right. The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the respective controls
EGCG reverses epithelial–mesenchymal transition and attenuates CSC-related traits in NPCSCs
We next analyzed whether EGCG has an effect on the expression of EMT markers and stemness genes in NPCSCs. Several markers and genes, including Bmi-1, Twist1, and CD44, are associated with CSC properties. Therefore, we assessed whether the expression of these markers was altered by EGCG treatment. The treatment of NPCSCs with EGCG significantly reduced the mRNA and protein levels of Bmi-1, Twist1, and N-cadherin and increased the expression of E-cadherin (Fig. 3a, b). Flow cytometry analysis was performed to quantify CD44+ cells in the NPCSCs because the CD44+ cell population possesses CSC properties in head and neck squamous carcinoma cells (HNSCs). EGCG treatment significantly decreased the percentage of CD44+ cells from 93.79 to 9.29 % in CNE2-SCs and from 84.17 to 5.78 % in C666-1-SCs (Fig. 3c). These results suggested that EGCG could be a potent suppressor of NPCSC traits.
EGCG reverses epithelial–mesenchymal transition (EMT) and attenuates CSC-related traits in NPCSCs. a CNE2-SCs were treated with EGCG (0–50 μM) for 48 h. Real-time RT-PCR demonstrated that the mRNA expression levels of mesenchymal cell markers N-cadherin and Vimentin and of CSC-related factors CD44, Bmi-1, and Twist1 were effectively reduced in a dose-dependent manner; however, the epithelial marker E-cadherin was increased. b Western blots showed that the protein expression of mesenchymal markers and CSC-related factors in CNE2-SCs and C666-1-SCs treated with EGCG for 48 h was effectively reduced in a dose-dependent manner; however, the epithelial marker E-cadherin was increased. GAPDH expression served as a loading control (left). The changes in protein expression were analyzed by densitometry quantification (right). c Fluorescence-activated cell sorting (FACS) analysis shows that the proportions of CD44+ cells in CNE2-SCs (upper) and C666-SCs (lower) treated with 50 μM EGCG were reduced significantly. The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the respective controls
EGCG combined with cisplatin suppresses NPCSC tumor formation in a xenograft model
To evaluate the effect of EGCG on NPCSC tumor formation in nude mice, a xenograft tumorigenicity assay was performed. CNE2-SCs treated with 20 μM EGCG and 10 μM cisplatin generated very small tumors in nude mice in contrast to the large tumors generated by NPCSCs treated with cisplatin alone or DMSO (Fig. 4a). The weights and volumes of the tumors produced by CNE2-SCs treated with EGCG plus cisplatin were significantly lower than those of the tumors produced by cisplatin- or DMSO-treated cells (Fig. 4b). To investigate the potential mechanisms of tumor growth retardation, xenograft tissue samples were analyzed by immunohistochemical staining for Bmi-1, Twist1, and NF-κB p65. We also investigated the expression of EMT markers, which have been associated with early metastasis following enhanced NF-κB p65 activity (Fig. 4c). Correspondingly, the protein expression levels of Bmi-1, Twist1, and NF-κB p65 were downregulated in CSC tumors co-treated with EGCG and cisplatin, whereas cisplatin or DMSO treatment alone had no effect. Moreover, the expression of E-cadherin, an epithelial cell marker, was upregulated in CSC tumors co-treated with EGCG and cisplatin but was not affected by cisplatin or DMSO alone. In contrast, the expression of N-cadherin, a mesenchymal cell marker, was downregulated in CSC tumors co-treated with EGCG and cisplatin and was not affected by cisplatin or DMSO alone. Taken together, these data suggest that the growth retardation of CSC tumor xenografts by combined EGCG and cisplatin treatment involves anti-tumorigenesis and anti-proliferative mechanisms, which may explain the EGCG inhibition of NF-κB p65 activity and the expression of proteins involved in EMT.
EGCG combined with cisplatin suppresses the tumor formation of NPCSCs in vivo. a CNE2-SCs treated with dimethylsulfoxide (DMSO) or cisplatin (10 μM) alone or with EGCG (20 μM) plus cisplatin (10 μM) were injected subcutaneously into the flanks of nude mice and allowed to grow for 8 weeks. The representative tumors in vivo (left) and the representative dissected tumor nodules after sacrifice of the mouse (right) are shown. (b) The dissected tumors formed by the three treated cell types were weighed and compared (left). The growth differences of the generated tumors were observed in a time-dependent manner in treated cells and control cells, and the size and volume of the tumors produced by CNE2-SCs treated with EGCG plus cisplatin were significantly lower than those of the tumors produced by CNE2-SCs treated with only cisplatin or DMSO (right). The results are the means ± SD (n = 4; **P < 0.01 compared with the respective controls). c A comparative analysis of the corresponding immunohistochemical results for p65, Bmi-1, Twist1, and EMT-associated markers taken from the tumor nodules of the nude mouse after treatment with EGCG combined with cisplatin revealed a marked downregulation of p65, Bmi-1, Twist1, and Vimentin and the upregulation of E-cadherin in CNE2-SCs. Representative images are shown under ×400 magnification
EGCG affects NF-κB p65 expression and modulates its cellular localization in NPCSC spheroids
Our study found that the active subunit of NF-κB signaling, p65, was activated and translocated from the cytoplasm in CNE2 and C666-1 cells into the nucleus in CNE2-SCs and C666-1-SCs (Fig. 5a). The NF-κB pathway has been shown to regulate the expression of EMT transcription factors [36, 37]. Proteins that regulate EMT have been investigated for potential mechanisms to explain the modulation of EMT by EGCG. Therefore, to determine whether EGCG inactivates NF-κB p65 in NPCSCs, the total cellular extracts, cytoplasmic extracts, and nuclear extracts of CNE2–SCs and C666-1-SCs following treatment for 48 h with EGCG (0–50 μM) were prepared for Western blotting analysis. A decrease in nuclear p65 localization and an increase in cytoplasmic expression were observed in both CNE2-SCs and C666-1-SCs after EGCG treatment, although no significant changes in total p65 protein expression were observed (Fig. 5b). Further experiments showed decreased p65 phosphorylation at serine 536 (Fig. 5b). Taken together, these experiments suggest that EGCG treatment inactivates NF-κB p65 transcriptional activation.
EGCG significantly inhibits the expression and nuclear translocation of the p65 subunit of NF-κB in NPCSCs. a Immunofluorescence assays showed that in the CNE2 cells, the p65 subunit of NF-κB was located in the cytoplasm; in the CNE2–SCs, activated NF-κB p65 was located primarily in the nucleus. However, the nuclear accumulation of NF-κB p65 was blocked significantly in a dose-dependent manner when CNE2–SCs were treated with EGCG (0–50 μM) for 24 h (left). This phenomenon also appeared in C666-1 and C666-1-SCs (right). Objective magnification ×400. b Western blotting analysis shows no significant changes in total p65 protein expression. However, decreased phosphorylation of p65 at serine 536 was observed. Next, subcellular fractionation analysis showed that nuclear p65 was reduced and cytoplasmic p65 was increased in a dose-dependent manner by EGCG treatment for 48 h (left). The changes in protein expression were analyzed by densitometry quantification (right). Lamin B1, nuclear loading control; GAPDH, cytoplasmic loading control. The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the respective controls
Knockdown of NF-κB p65 inhibits the migration and colony-forming abilities of NPCSCs and enhances the effects of EGCG on spheroid formation
Lentiviral infection was performed in CNE2-SCs and C666-1-SCs with a virus-shRNA-NF-κB p65 solution, and stable transfected cell lines, CNE2-SC-shp65 and C666-1-SC-shp65, were established (Fig. 6a). To investigate the role of NF-κB p65 in NPCSC self-renewal and migration, the colony formation assay and transwell migration assay were used. The number of CNE2-SC-shp65 and C666-1-SC-shp65 colonies was significantly reduced compared to the respective scrambled shRNA-infected controls (CNE2–SC-Scr and C666-1-SC-Scr; Fig. 6b). Migratory and invasive abilities are important features of CSCs. To investigate the role of NF-κB p65 in maintaining these features, the transwell migration assay was used to evaluate the migration of NF-κB p65-silenced NPCSCs in vitro. The number of CNE2-SC-shp65 and C666-1-SC-shp65 cells that migrated to the lower side of the membrane was significantly decreased compared with the respective scrambled shRNA-infected controls (Fig. 6c). In addition, we examined whether silencing NF-κB p65 affected the anti-proliferative effects of EGCG in human NPCSCs using the trypan blue assay. The data showed that EGCG inhibited stem cell viability in CSC spheroids transduced with scrambled shRNA in a dose-dependent manner; the inhibition of NF-κB p65 by shRNA further enhanced the anti-proliferative effects of EGCG (Fig. 6d). These data suggest that the inhibition of NF-κB p65 may be an attractive method to enhance the anticancer activities of EGCG in CSCs.
Knockdown of NF-κB p65 inhibits the migration and colony formation of NPCSCS and enhances the effects of EGCG on spheroid formation. a The transfected CNE2–SCs (upper) and C666-1-SCs (lower) were collected and observed under white light (left) and with fluorescence (right) microscopy after 72 h (magnification ×200). b Representative micrographs (left) show the migration of p65 shRNA-treated and scrambled shRNA-treated spheroids, and the quantification of the migrated cells is shown at the right. c Representative micrographs (left) show the colony formation of p65 shRNA-treated and scrambled shRNA-treated spheroids, and the quantification of colonies is shown at the right. d The trypan blue assay demonstrated that EGCG inhibited stem cell viability in CSC spheroids transduced with scrambled shRNA in a dose-dependent manner; the inhibition of NF-κB p65 by shRNA further enhanced the anti-proliferative effects of EGCG on NPCSCs. The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the scrambled shRNA-infected controls
Knockdown of NF-κB p65 reverses EMT and suppresses relevant transcription factors in NPCSCs
The protein levels of EMT markers and relevant transcription factors were detected by Western blotting. p65, Twist1, and Bmi-1 levels were reduced in CNE2-SC-shp65 and C666-1-SC-shp65 cells compared with the scrambled shRNA-infected controls. N-cadherin and Vimentin levels were also reduced. However, the E-cadherin levels were increased in CNE2-SC-shp65 and C666-1-SC-shp65 cells compared with the scrambled shRNA-infected controls (Fig. 7). These results suggested that NF-κB p65 plays an important role in NPCSC characteristics.
NF-κB p65 knockdown reverses EMT and suppresses the relevant transcription factors of NPCSCs. (left) Western blot analysis that the protein expression of p65, Twist1, Bmi-1, N-cadherin, and Vimentin was reduced in CNE2-SC-shp65 and C666-1-SC-shp65 cells compared with the scrambled shRNA-treated controls; however, expression of E-cadherin was increased. GAPDH expression served as a loading control. (right) The changes in protein expression were analyzed by densitometry quantification. The data are expressed as the means ± SD of three independent experiments; *P < 0.05, **P < 0.01 compared with the scrambled shRNA controls
EGCG inhibits the transcriptional regulation of NF-κB p65 on Twist1 expression
Because previous evidence in this study demonstrated that EGCG could inactivate NF-κB p65 transcriptional activation, we next sought to examine the effects of EGCG on the transcriptional regulation of NF-κB p65 on the EMT transcription factor Twist1. A luciferase reporter assay was performed to analyze Twist1 promoter activity in spheroids treated with shp65, 50 μM EGCG for 24 h, shp65 combined with 50 μM EGCG for 24 h, or scrambled shRNA. As shown in Fig. 8, Twist1 promoter activity was significantly reduced in the CNE2–SCs and C666-1-SCs treated with shp65 or 50 μM EGCG compared to the spheroids treated with the scrambled shRNA controls. Combined treatment with shp65 and 50 μM EGCG reduced the Twist1 promoter activity in CNE2-SCs and C666-1-SCs more significantly. This result confirmed that NF-κB p65 interacts with and regulates the Twist1 promoter in NPCSCs. Taken together, these experiments suggest that EGCG inhibits the transcriptional regulation of NF-κB p65 on Twist1 expression.
EGCG inhibits the transcriptional regulation of NF-κB p65 on Twist1 expression. Luciferase reporter assays to assess the activity of the Twist1 promoter were conducted on spheroids treated with shp65, 50 μM EGCG for 24 h, shp65 combined with 50 μM EGCG for 24, or scrambled shRNA. Twist1 promoter activity was significantly reduced in the CNE2–SCs and C666-1-SCs treated with shp65 or 50 μM EGCG compared with the spheroids treated with scrambled shRNA control. The combined treatment of shp65 with 50 μM EGCG reduced the Twist1 promoter activity in CNE2-SCs and C666-1-SCs more significantly. The data are expressed as the means ± SD of three independent experiments; **P < 0.01 compared with the respective controls, # P < 0.05 and &P < 0.05 spheroids treated with combination compared with single-agent treatments
Discussion
The CSC theory holds that the biological characteristics of NPC metastasis, relapse, and resistance to therapy are closely related to the presence of CSCs. In this experimental study, tumor spheroid cells were enriched and expanded from human NPC cell lines in a non-adherent culture system, and we characterized the phenotypic and functional properties of NPC spheroids. Our data showed that invasion and self-renewal were enhanced in spheroid cells and further revealed that the mRNA expression of stemness-related genes Bmi-1 and Twist1 and the putative stem cell marker CD44 was distinctly increased in the tumor spheroid cells. Furthermore, the spheroid cells underwent EMT. The data indicated that the tumor spheroid cells contain putative CSCs and were endowed with CSC features [38, 39].
The CSC theory suggests that the targeted eradication of NPCSCs may represent a new treatment strategy for NPC [40]. Considerable attention has recently been focused on the fact that certain edible phytochemicals alter gene expression, directly or indirectly, thereby regulating the carcinogenic processes. (-)-Epigallocatechin-3-gallate (EGCG) has been shown to block each stage of carcinogenesis by modulating signal transduction pathways [41, 42]. However, the concrete effect and molecular mechanisms by which EGCG controls NPCSC traits was lacking. Our study demonstrates that EGCG can dose-dependently inhibit spheroid formation in SFM and inhibit colony formation by NPC spheroid cells grown in agar. This result indicated that EGCG could effectively suppress the self-renewal capacity of NPCSCs. Moreover, EGCG regulates the invasive-like phenotypes characterized by EMT of the tumor spheroid cells grown in SFM. Specifically, EGCG decreased the expression of the EMT marker and relevant transcription factor Twist1 and the stemness-related gene Bmi-1. In addition, we also demonstrated that combined treatment of EGCG with cisplatin significantly inhibited tumor formation and suppressed the expression of NF-κB p65, Bmi-1, Twist1, and EMT markers in nude mouse xenograft tumors, which suggested that EGCG might have an inhibitory effect on tumorigenesis, metastasis, and recurrence of NPC when used in combination with standard treatments in vivo.
Previous studies have reported several therapeutic strategies of targeting CSCs; inhibiting the key signaling pathways active in CSCs is one of the most promising strategies for the treatment of cancer [43]. Studies have shown that EGCG inhibits spheroid formation by neuroblastoma BE(2)-C CSCs [24]. EGCG analogs can inhibit the spheroid formation and cell proliferation of breast CSCs through the activation of the AMP-activated protein kinase pathway [44], and they can inhibit the self-renewal capacity of CSCs by inhibiting the sonic Hedgehog pathway in HNSC CSCs [26]. These studies have revealed certain signaling pathways targeted by EGCG; however, the concrete molecular mechanisms involved in the EGCG-induced control of NPCSC traits have remained unclear.
Recent studies have found that the NF-κB signaling pathway plays an important role in maintaining the biological characteristics of cancer stem cells [45]. Moreover, the suppression of NF-κB activity is one of the mechanisms of EGCG activity [32, 33, 46]. Therefore, the downregulation of NF-κB signaling by EGCG may represent a novel approach for NPC therapy. To determine whether EGCG inhibits the stemness of NPCSCs through the inactivation of NF-κB, our study first found that the active subunit of NF-κB signaling, p65, was activated and translocated from the cytoplasm of adherent parent cells into the nucleus of NPCSCs. To determine the effect of EGCG on p65 cellular localization, subcellular fractionation experiments were performed on NPC spheroid cells treated with EGCG for 48 h. Western blot analysis showed no significant changes in total p65 protein expression, but a decrease in nuclear p65 localization was observed in both CNE2-SCs and C666-1-SCs. However, this increase was observed in the cytoplasm. Decreased phosphorylation of p65 at serine 536 was observed, which is consistent with previous data and suggested that phosphorylation at this site occurs independently of canonical NF-κB signaling [47]. NF-κB was recently identified as a central mediator of EMT and metastasis and has been implicated in the regulation of EMT markers and transcription factors, including Twist1 [48–52]. Therefore, NF-κB p65 was knocked down in NPCSCs with a lentiviral vector. The data showed that knockdown of NF-κB p65 reversed EMT, inhibited the expression of the transcription factor Twist1 and the stemness-related gene Bmi-1, and suppressed the migration and colony formation of NPCSCs. Next, using luciferase reporter assays, we found that the transcriptional regulation of Twist1 expression by NF-κB p65 was decreased following the shp65 treatment, similar to the effect produced with EGCG treatment, and the treatment of shp65 combined with EGCG reduced the Twist1 promoter activity in NPCSCs more significantly. This result confirmed that NF-κB p65 interacts with the Twist1 promoter and regulates Twist1 transcription in NPCSCs, providing a direct link between EGCG treatment and the inhibition of Twist1 expression. In addition, evidence from a previous study strongly supports the interaction of the Twist1 and Bmi-1 oncoproteins to regulate the traits involved in CSC behavior [53, 54]. Therefore, we believe that the transcriptional regulation of NF-κB p65 on Twist1 expression can influence the expression of Bmi-1. We will continue to study the transcriptional regulation of NF-κB p65 on Bmi-1 expression in the future.
Overall, our findings revealed that treatment with EGCG could inhibit the migration and self-renewal capacity of NPCSCs and reverse EMT by inactivating NF-κB p65 and reducing its transcriptional regulation of Twist1. The findings reported here support the use of EGCG as a new treatment for NPCSCs because it may prove beneficial in cancer prevention. Further investigations concerning the molecular mechanism of EGCG activity in NPCSCs, based on the present results, could help in the development of novel drug combinations capable of eliminating NPCSCs.
Abbreviations
- CSC:
-
Cancer stem cell
- NPC:
-
Nasopharyngeal cancer
- NPCSCs:
-
Nasopharyngeal cancer stem cells
- SC:
-
Spheroid cell
- EMT:
-
Epithelial–mesenchymal transition
- EGCG:
-
Epigallocatechin-3-gallate
- SFM:
-
Serum-free medium
- NF-κB:
-
Nuclear factor κB
- RT-PCR:
-
Quantitative reverse transcriptase polymerase chain reaction
- DMSO:
-
Dimethylsulfoxide
- FACS:
-
Fluorescence-activated cell sorting
- FBS:
-
Fetal bovine serum
- EGF:
-
Epidermal growth factor
- bFGF:
-
Human recombinant basic fibroblast growth factor
- DMEM/F12:
-
Dulbecco’s modified Eagle’s medium F12
References
Yu MC, Yuan JM. Epidemiology of nasopharyngeal carcinoma. Semin Cancer Biol. 2002;12:421–9.
Lee AW, Yau TK, Wong DH, Chan EW, Yeung RM, Ng WT, et al. Treatment of stage IV(A-B)nasopharyngeal carcinoma by induction-concurrent chemoradiotherapy and accelerated fractionation. Int J Radiat Oncol Biol Phys. 2005;63:1331–8.
Yeh SA, Tang Y, Lui CC, Huang YJ, Huang EY. Treatment outcomes and late complications of 849 patients with nasopharyngeal carcinoma treated with radiotherapy alone. Int J Radiat Oncol Biol Phys. 2005;62:672–9.
Lo KW, To KF, Huang DP. Focus on nasopharyngeal carcinoma. Cancer Cell. 2004;5:423–8.
Le QT, Tate D, Koong A, Gibbs IC, Chang SD, Adler JR, et al. Improved local control with stereotactic radiosurgical boost in patients with nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2003;56:1046–54.
Visvader JE, Lindeman GJ. Cancer stem cells in solid tumours: accumulating evidence and unresolved questions. Nat Rev Cancer. 2008;8:755–68.
Er O. Cancer stem cells in solid tumors. Onkol. 2009;32:605–9.
Lang SH, Anderson E, Fordham R, Collins AT. Modeling the prostate stem cell niche: an evaluation of stem cell survival and expansion in vitro. Stem Cells Dev. 2010;19:537–46.
Jones RJ, Matsui WH, Smith BD. Cancer stem cells: are we missing the target? J Natl Cancer Inst. 2004;96:583–5.
Sakariassen PO, Immervoll H, Chekenya M. Cancer stem cells as mediators of treatment resistance in brain tumors: status and controversies. Neoplasia. 2007;9:882–92.
Su J, Xu XH, Huang Q, Lu MQ, Li DJ, Xue F, et al. Identification of cancer stem-like CD44+ cells in human nasopharyngeal carcinoma cell line. Arch Med Res. 2011;42:15–21.
Wang J, Guo LP, Chen LZ, Zeng YX, Lu SH. Identification of cancer stem cell-like side population cells in human nasopharyngeal carcinoma cell line. Cancer Res. 2007;67:3716–24.
Kong D, Banerjee S, Ahmad A, Li Y, Wang Z, Sethi S, et al. Epithelial to mesenchymal transition is mechanistically linked with stem cell signatures in prostate cancer cells. PLoS One. 2010;5:e12445.
Polyak K, Weinberg RA. Transitions between epithelial and mesenchymal states: acquisition of malignant and stem cell traits. Nat Rev Cancer. 2009;9:265–73.
Shankar S, Ganapathy S, Srivastava RK. Green tea polyphenols: biology and therapeutic implications in cancer. Front Biosci. 2007;12:4881–99.
Yang CS, Wang X, Lu G, Picinich SC. Cancer prevention by tea: animal studies, molecular mechanisms and human relevance. Nat Rev Cancer. 2009;9:429–39.
Ju J, Lu G, Lambert JD, Yang CS. Inhibition of carcinogenesis by tea constituents. Semin Cancer Biol. 2007;17:395–402.
Landis-Piwowar KR, Huo C, Chen D, Milacic V, Shi G, Chan TH, et al. A novel prodrug of the green tea polyphenol (-)-epigallocatechin-3-gallate as a potential anticancer agent. Cancer Res. 2007;67:4303–10.
Shankar S, Ganapathy S, Hingorani SR, Srivastava RK. EGCG inhibits growth, invasion, angiogenesis and metastasis of pancreatic cancer. Front Biosci. 2008;13:440–52.
Shirakami Y, Shimizu M, Adachi S, Sakai H, Nakagawa T, Yasuda Y, et al. (-)-Epigallocatechin gallate suppresses the growth of human hepatocellular carcinoma cells by inhibiting activation of the vascular endothelial growth factor-vascular endothelial growth factor receptor axis. Cancer Sci. 2009;100:1957–62.
Takahashi H, Nomata K, Mori K, Matsuo M, Miyaguchi T, Noguchi M, et al. The preventive effect of green tea on the gap junction intercellular communication in renal epithelial cells treated with a renal carcinogen. Anticancer Res. 2004;24:3757–62.
Tang GQ, Yan TQ, Guo W, Ren TT, Peng CL, Zhao H, et al. (-)-Epigallocatechin-3-gallate induces apoptosis and suppresses proliferation by inhibiting the human Indian Hedgehog pathway in human chondrosarcoma cells. J Cancer Res Clin Oncol. 2010;136:1179–85.
Zhu BH, Chen HY, Zhan WH, Wang CY, Cai SR, Wang Z, et al. (-)-Epigallocatechin-3-gallate inhibits VEGF expression induced by IL-6 via Stat3 in gastric cancer. World J Gastroenterol. 2011;17:2315–25.
Nishimura N, Hartomo TB, Pham TV, Lee MJ, Yamamoto T, Morikawa S, et al. Epigallocatechin gallate inhibits sphere formation of neuroblastoma BE(2)-C cells. Environ Health Prev Med. 2012;17:246–51.
Chen D, Pamu S, Cui Q, Chan TH, Dou QP. Novel epigallocatechin gallate (EGCG) analogs activate AMP-activated protein kinase pathway and target cancer stem cells. Bioorg Med Chem. 2012;20:3031–7.
Tang SN, Fu J, Nall D, Rodova M, Shankar S, Srivastava RK. Inhibition of sonic Hedgehog pathway and pluripotency maintaining factors regulate human pancreatic cancer stem cell characteristics. Int J Cancer. 2012;131:30–40.
Burnett J, Newman B, Sun D. Targeting cancer stem cells with natural products. Curr Drug Targets. 2012;13:1054–64.
Hayden MS, Ghosh S. Shared principles in NF-kappa B signaling. Cell. 2008;132:344–62.
Yan Z, Yong-Guang T, Fei-Jun L, Fa-Qing T, Min T, Ya C. Interference effect of epigallocatechin-3-gallate on targets of nuclear factor kB signal transduction pathways activated by EB virus encoded latent membrane protein 1. IntJ Biochem Cell Biol. 2004;36:1473–81.
Uchibori R, Tsukahara T, Mizuguchi H, Saga Y, Urabe M, Mizukami H, et al. NF-κB activity regulates mesenchymal stem cell accumulation at tumor sites. Cancer Res. 2013;73:364–72.
Liu M, Sakamaki T, Casimiro MC, Willmarth NE, Quong AA, Ju X, et al. The canonical NF-kappaB pathway governs mammary tumorigenesis in transgenic mice and tumor stem cell expansion. Cancer Res. 2010;70:10464–73.
Afaq F, Adhami VM, Ahmad N, Mukhtar H. Inhibition of ultraviolet B-mediated activation of nuclear factor kappaB in normal human epidermal keratinocytes by green tea constituent (-)-epigallocatechin-3-gallate. Oncogene. 2003;22:1035–44.
Gupta S, Hastak K, Afaq F, Ahmad N, Mukhtar H. Essential role of caspases in epigallocatechin-3-gallate-mediated inhibition of nuclear factor kappa B and induction of apoptosis. Oncogene. 2004;23:2507–22.
Syed DN, Afaq F, Kweon MH, Hadi N, Bhatia N, Spiegelman VS, et al. Green tea polyphenol EGCG suppresses cigarette smoke condensate-induced NF-kappaB activation in normal human bronchial epithelial cells. Oncogene. 2007;26:673–82.
Lee J, Kotliarova S, Kotliarov Y, Li A, Su Q, Donin NM, et al. Tumor stem cells derived from glioblastomas cultured in bFGF and EGF more closely mirror the phenotype and genotype of primary tumors than do serum-cultured cell lines. Cancer Cell. 2006;9:391–403.
Li CW, Xia W, Huo L, Lim SO, Wu Y, Hsu JL, et al. Epithelial-mesenchymal transition induced by TNF-alpha requires NF-kappaB-mediated transcriptional upregulation of Twist1. Cancer Res. 2012;72:1290–300.
Pham CG, Bubici C, Zazzeroni F, Knabb JR, Papa S, Kuntzen C, et al. Upregulation of twist-1 by NF-kappaB blocks cytotoxicity induced by chemotherapeutic drugs. Mol Cell Biol. 2007;27:3920–35.
Frame FM, Maitland NJ. Cancer stem cells, models of study and implications of therapy resistance mechanisms. Adv Exp Med Biol. 2011;720:105–18.
Mani SA, Guo W, Liao MJ, Eaton EN, Ayyanan A, Zhou AY, et al. The epithelial-mesenchymal transition generates cells with properties of stem cells. Cell. 2008;133:704–15.
Hu Y, Fu L. Targeting cancer stem cells: a new therapy to cure cancer patients. Am J Cancer Res. 2012;2:340–56.
Na HK, Surh YJ. Intracellular signaling network as a prime chemopreventive target of (-)-epigallocatechin gallate. Mol Nutr Food Res. 2006;50:152–9.
Jung YD, Ellis LM. Inhibition of tumour invasion and angiogenesis by epigallocatechin gallate (EGCG), a major component of green tea. Int J Exp Pathol. 2001;82:309–16.
Takebe N, Harris PJ, Warren RQ, Ivy SP. Targeting cancer stem cells by inhibiting Wnt, Notch, and Hedgehog pathways. Nat Rev Clin Oncol. 2011;8:97–106.
Chen D, Pamu S, Cui Q, Chan TH, Dou QP. Novel epigallocatechin gallate (EGCG) analogs activate AMP-activated protein kinase pathway and target cancer stem cells. Bioorg Med Chem. 2012;20:3031–7.
Zhou J, Zhang H, Gu P, Bai J, Margolick JB, Zhang Y. NF-kappaB pathway inhibitors preferentially inhibit breast cancer stem-like cells. Breast Cancer Res Treat. 2008;111:419–27.
Shimizu M, Deguchi A, Lim JT, Moriwaki H, Kopelovich L, Weinstein IB. (-)-Epigallocatechin gallate and polyphenon E inhibit growth and activation of the epidermal growth factor receptor and human epidermal growth factor receptor-2 signaling pathways in human colon cancer cells. Clin Cancer Res. 2005;11:2735–46.
Sasaki CY, Barberi TJ, Ghosh P, Longo DL. Phosphorylation of RelA/p65 on serine 536 defines an I{kappa}B{alpha}-independent NF-{kappa}B pathway. J Biol Chem. 2005;280:34538–47.
Huber MA, Beug H, Wirth T. Epithelial-mesenchymal transition: NF-kappaB takes center stage. Cell Cycle. 2004;3:1477–80.
Huber MA, Azoitei N, Baumann B, Grünert S, Sommer A, Pehamberger H, et al. NF-Kb is essential for epithelial-mesenchymal transition and metastasis in a model of breast cancer progression. J Clin Invest. 2004;114:569–81.
Min C, Eddy SF, Sherr DH, Sonenshein GE. NF-kappaB and epithelial to mesenchymal transition of cancer. J Cell Biochem. 2008;104:733–44.
Li S, Kendall SE, Raices R, Finlay J, Covarrubias M, Liu Z, et al. TWIST1 associates with NF-κB subunit RELA via carboxyl-terminal WR domain to promote cell autonomous invasion through IL8 production. BMC Biol. 2012;10:73.
Do SI, Kim JY, Kang SY, Lee JJ, Lee JE, Nam SJ, et al. Expression of TWIST1, Snail, Slug, and NF-κB and methylation of the TWIST1 promoter in mammary phyllodes tumor. Tumor Biol. 2013;34:445–53.
Yang MH, Hsu DS, Wang HW, Wang HJ, Lan HY, Yang WH, et al. Bmi1 is essential in Twist1-induced epithelial–mesenchymal transition. Nat Cell Biol. 2010;12:982–92.
Chiba T, Miyagi S, Saraya A, Aoki R, Seki A, Morita Y, et al. The polycomb gene product BMI1 contributes to the maintenance of tumor-initiating side population cells in hepatocellular carcinoma. Cancer Res. 2008;68:7742–9.
Acknowledgments
This research is supported by the General Program of the National Natural Science Foundation of China (No. 81171365).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, YJ., Wu, SL., Lu, SM. et al. (-)-Epigallocatechin-3-gallate inhibits nasopharyngeal cancer stem cell self-renewal and migration and reverses the epithelial–mesenchymal transition via NF-κB p65 inactivation. Tumor Biol. 36, 2747–2761 (2015). https://doi.org/10.1007/s13277-014-2899-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-014-2899-4