Abstract
To improve early melanoma detection, educational programs have been developed for general practitioners (GPs). This study aimed to determine whether the adjunct of teaching basic knowledge of pigmented skin lesions (PSL) to the training in melanoma diagnosis improves the GPs’ diagnostic accuracy of melanoma. An interventional prospective study was conducted over a 3-month period where GPs attended a 2-h training course. The 1st session taught clinical melanoma recognition and the 2nd session instructed basic knowledge of PSL. Prior to training, after the 1st, and after the 2nd session, GPs were asked to select the malignant or benign nature of 15 clinical images associated to their clinical history. In total, 56 GPs participated in this study. The number of GPs identifying correctly ≥ 50% of the melanomas increased the most after the 1st session from 15 (26.8%; CI = (15.2; 38.4)) to 44 (78.6%; CI = (67.8; 89.3)) GPs (P < 0.001). The number of GPs correctly identifying ≥ 50% of the benign PSL only increased after completing the entire training, going from 10 (17.9%; CI = [(7.8; 27.9)) GPs to 50 (89.3%; CI = (81.2; 97.4)) GPs (P < 0.001). In this study, GPs identified benign PSL most accurately after the 2nd session. This suggested that teaching GPs the basics of PSL would especially improve their diagnostic accuracy for benign PSL, which could reduce unnecessary referrals to dermatologists. Teaching basic knowledge of PSL in addition to melanoma recognition seemed to enable GPs to triage skin lesions more effectively than when they were only trained to recognize melanoma.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The last two decades, general practitioners (GPs) have been recognized to play a key role in early melanoma detection [1, 2]. In order to help GPs dealing with suspicious skin lesions of melanoma, training programs in melanoma diagnosis especially designed for GPs have been developed [3, 4].
All these training programs included training in melanoma recognition using clinical (naked eye) diagnostic tools, such as the ABCD rule [5], pattern recognition [6], and the “ugly duckling” sign [7], sometimes supplemented by training in dermoscopy [4]. Dermoscopy uses a handheld device, which allows observation of skin structures invisible to the naked eye. So far, it has been the most widely non-invasive in vivo technique used in clinical practice to assess skin tumors [8]. Less frequently, some training programs complemented the GPs’ training in melanoma diagnosis by teaching them basic knowledge of the most common types of pigmented skin lesions (PSL) [9,10,11]. Basic knowledge refers to the theoretical notions to be known about melanoma, i.e., risks factors of melanoma, preferred locations of this cancer according to gender, normal/abnormal evolution of PSL, and characteristics of the most common benign PSL.
In these previous studies, the diagnostic accuracy of the participating GPs was assessed on images of PSL in a training setting, which does not always reflect the GPs’ performances in a clinical setting. Still, a major French study conducted in real life has demonstrated a positive long-term impact of their training course in clinical melanoma diagnosis [12]. This training was supplemented by teaching of basic knowledge on the epidemiology of melanoma (risk factors of melanoma and recognition of at-risk melanoma patients) and of its differential diagnoses (typical nevus, seborrheic keratosis, and actinic lentigo). Unlike most other trainings, it has been followed by a screening campaign. The latter showed a decrease of the incidence of very thick melanomas (Breslow thickness ≥ 3 mm) over a 3-year period. However, the respective contributions of basic knowledge and differential diagnoses, on the one hand, and of training in clinical melanoma recognition, on the other hand, in the success of this study has not been reported.
While the efficacy of training GPs in melanoma diagnosis using clinical diagnostic tools and/or dermoscopy is widely acknowledged [3, 13, 14], the added value of teaching basic knowledge of PSL to GPs in order to improve their diagnostic accuracy of melanoma has not yet, to the best of our knowledge, been studied.
In that respect, this prospective study aimed to determine whether the adjunct of teaching basic knowledge of PSL to training in melanoma diagnosis improved the GPs’ diagnostic accuracy of melanoma.
Methods
Study Design
This interventional prospective study was conducted over a 3-month period from January 2020 to March 2020 among French-speaking GPs in Belgium. The study was approved by the Ethical Committee of the Catholic University of Louvain in Brussels, Belgium. The leaders of five groups of Continuing Medical Education in General Practice in the districts of Brussels, Hainaut, Namur, and Brabant-Wallon of Belgium were contacted by email to participate in a training program in melanoma diagnosis. Four groups accepted the invitation.
Training Program
GPs attended a 2-h-live training course, which was divided in two sessions. The 1st session lasted 30 min and trained the GPs in naked-eye diagnosis of melanoma using three main clinical melanoma diagnostic tools: the ABCD rule [5], pattern recognition [6], and the “ugly duckling” sign [7]. To illustrate the diagnostic tools, a large number of clinical images of melanomas were shown. The 2nd session lasted 45 min and taught melanoma basics, i.e., risk factors of melanoma, preferred locations of melanoma according to gender, normal/abnormal evolution of PSL according to age categories, and the characteristics of the most common benign PSL: seborrheic keratosis, typical nevi, blue nevi, congenital nevi, halo nevi, actinic lentigo, and subungual/subcorneal hematomas. Clinical images of the benign PSL were shown to help the GPs memorize their clinical aspects.
Data Collection
All study data was collected using REDCap® (Research Electronic Data Capture, Vanderbilt University, USA) tools hosted at the Cliniques Universitaires Saint-Luc [15, 16].
Prior to training, GPs completed a survey collecting their socio-demographic and medical practice data. They were asked about their age, gender, workplace (urban, suburban, or rural area), work practice (solo or medical group), qualification, and previous attendance to a training program in melanoma diagnosis. Then, they assessed 15 clinical images of PSL associated to their clinical history. They were asked to decide on the malignant or benign nature of each lesion. The GPs re-assessed the same clinical images after the 1st session and, once more, after completing the entire training.
The 15 clinical cases had been peer-reviewed by two dermatologists, who validated the PSL to be easily recognizable on the basis of the clinical image and clinical history. The images consisted of five melanomas (three superficial spreading melanomas, one nodular melanoma, and one lentigo maligna) and 10 benign PSL (two typical nevi, one seborrheic keratosis, one irritated typical nevus, one halo nevus, one congenital nevus, one actinic lentigo, one blue nevus, one subungual and one subcorneal hematomas) (Figs. 1 and 2). The clinical history of the lesions included in each case the patient’s age and gender, localization and evolution (new onset or old lesion, change in shape or size) of the lesion.
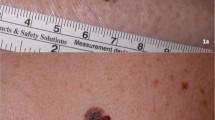
Test set of 15 clinical cases of pigmented skin lesions. (1A-E) Malignant lesions. (2A-J) Benign lesions. (1A) Woman, aged 76 years. New lesion of the lower limb noticed by her daughter this summer. Melanoma. (1B) Woman, aged 46 years. New lesion of the buttock, growing in size. Melanoma. (1C) Man, aged 55 years. Newly appeared lesion of the back. Melanoma. (1D) Man, aged 66 years. Growing lesion on the back, where there used to be a brown spot in the last 2 years. Melanoma. (1E) Woman, aged 75 years. A 10-year-old lesion of the external canthus of the eye, which is slowly spreading. Lentigo maligna. (2A) Woman, aged 26 years. Slowly growing lesion of the trunk that appeared 2 years ago. Benign nevus. (2B) Man, aged 38 years. Lesion on the foot sole stable since puberty. Benign nevus. (2C) Woman, aged 35 years. Lesion on shoulder for 10 years but bleeding and erythema appeared following scratching. Irritated benign nevus. 2D. Women, aged 23 years. Lesion with a recent white halo noticed on her back. Halo nevus. (2E) Woman, aged 25 years. Lesion of the right hand stable since childhood but recurrent rubbing. Congenital nevus. (2F) Man, aged 38 years. Lesion of the wrist, stable since puberty. Blue nevus. (2G) Woman, aged 68 years. Lesion stable in size, that appeared 2 years ago but darkened this summer of the left cheek. Actinic lentigo. (2H) Man, aged 65 years. Lesion of the back that appeared 2 years ago, itching sometimes. Seborrheic keratosis. (2I) Man, aged 40 years, athletic. Lesion of the left heel that appeared two weeks ago. Subcorneal hematoma. (2J) Man, aged 50 years. Fingernail lesion that appeared a month ago on the right hallux. Subungual hematoma
Three major pigmented skin lesions of the test set and their basic characteristics important to know. a Slowly growing 10-year-old lesion of the external canthus of the right eye in a 75-year-old woman. Diagnosis: Lentigo maligna. Lentigo maligna is little known to general practitioners (GPs). They are often unaware that these lesions appear on previously photo-exposed body areas in the elderly and tend to extent slowly (over several years). b Woman, aged 23, noticed a recent white halo on one of her moles on her back. Diagnosis: Halo nevus. Halo nevi have a very characteristic clinical aspect consisting of a white, regular, and round halo that circumscribes a benign nevus. This inflammatory phenomenon is relatively common in teenagers and young adults. GPs, knowing this particular reaction, can easily reassure their young patients. c Fingernail lesion that appeared a month ago on the right hallux of a 50-year-old man. Diagnosis: Subungual hematoma. The notion of recent microtraumas is important to look for in the clinical history of the lesion. Indeed, this hematoma located under the nail occurs after repeated microtraumas of the nail while walking or running with new unsuitable footwear or during very long walks. Unlike pigmented melanocytic lesions of the nail matrix, which form brownish-black longitudinal bands of the nails, the subungual hematoma forms a reddish-brown spot under the nail with convoluted borders. Knowing these basic characteristics allows GPs to reassure their patient and reduces unnecessary referrals to the dermatologist
Statistical Analysis
The statistical analysis was performed using SAS software (SAS© 9.4, SAS Institute Inc., USA). Descriptive statistics were used to summarize the results considering absolute numbers, percentages and 95% confidence intervals. McNemar test for two correlated proportions was used to test for variations between the three questionnaires with regard to the number of GPs that correctly identified the melanomas and the benign PSL. All tests were considered to be significant for p value < 0.05 and the conservative Bonferroni correction method was used to adjust p values for multiple comparisons.
Results
Characteristics of the Study Population
Fifty-six GPs participated in the training program. All completed the three questionnaires and none were excluded. Table 1 summarizes the characteristics of these 56 GPs. Of them, 29 were qualified GPs and 27 were GP trainees. Women (61%) and young GPs (54%) were predominantly represented.
Assessment of the Clinical Cases of PSL
Table 2 shows the evolution of the GPs’ correct responses for each clinical case and Table 3 resumes the global evolution of the GPs’ responses throughout the training sessions.
Prior to training, only 15 (26.8%; CI = (15.2; 38.4)) GPs gave ≥ 50% correct responses for the five melanoma cases and 10 (17.9%; CI = (7.8; 27.9)) GPs gave ≥ 50% correct answers for the 10 benign PSL. Comparing before and after the 1st session of the training, the number of GPs that correctly identified the malignant lesion had at least doubled after the training in clinical melanoma diagnostic tools for each case of melanoma (all P < 0.001, see Table 2). In contrast, no statistically significant improvement of the GPs’ answers to the clinical cases of the benign lesions were found (pNS). Comparing the answers after the 1st and the 2nd session, benign PSL were significantly better identified by the GPs after the session on the characteristics of PSL (P < 0.001). To note that the number of GPs giving the correct answer for the melanoma cases continued to increase slightly.
Overall, the number of GPs identifying correctly ≥ 50% of the melanoma cases increased from 15 (26.8%; CI = (15.2; 38.4)) to 44 (78.6%; CI = (67.8; 89.3)) GPs after the 1st session of the training (P < 0.001) and to 52 (92.9%; CI = (86.1; 99.6)) GPs after the 2nd session (P = 0.02). The number of GPs correctly identifying ≥ 50% of the 10 benign PSL only increased after completing the entire training, going from 8 (14.3%; CI = (5.1; 23.5)) GPs after the 1st session to 50 (89.3%; CI = (81.2; 97.4)) GPs after the 2nd session (P < 0.001).
Discussion
This prospective study aimed to determine whether the adjunct of teaching basic knowledge of PSL to training in melanoma diagnosis improved the GPs’ diagnostic accuracy of melanoma.
In this study, GPs correctly identified, as expected, more malignant and benign lesions after the training. The results showed that the number of GPs correctly identifying the melanomas had at least doubled for each clinical case after the 1st session (Table 1). This confirms, as shown in a recent Cochrane review, that training GPs in clinical melanoma diagnosis improves their diagnostic accuracy for melanoma [17]. However, it also indicates that clinical examination alone was insufficient for some of the GPs to identify malignant lesions. As the sensitivity of the GPs continued to increase after the 2nd session, learning the basics of melanoma seemed to have been an aid for sharper decision-making.
Comparison with Existing Literature
The positive impact of basic knowledge to improve early melanoma detection has already been recognized in 2004, when the notion of “evolving,” characterizing a lesion that had changed over time, was added to the ABCD rule as a supplementary key criteria for malignancy [18]. Then, a triage approach for GPs based on clinical examination in consideration of the patient’s age taken together with the report of evolution of a lesion was proposed in 2012 [19]. In the Netherlands, a recent study revealed that even know skin lesions suspicious of melanoma were mostly triaged on the basis of clinical examination and patient’s medical history. However, the authors showed that the patient’s medical history often lacked important criteria, such as family history of melanoma and evolution of the lesion, for appropriate management of suspicious skin lesions [20]. As a cause, they cited a GPs’ lack of basic knowledge.
In the present study, benign lesions were rather better identified by the GPs after completing the 2nd session. This suggests that teaching GPs the basics of PSL especially improves their diagnostic accuracy for benign PSL. Another efficient tool to improve the diagnosis of benign skin lesions is dermoscopy [21]. When used by properly trained GPs, it already demonstrated to improve the triage of suspicious skin lesions in primary care without increasing the number of unnecessary referrals to dermatologists because not only malignant but also benign lesions were better diagnosed [13]. Furthermore, another recent Cochrane review found dermoscopy to be more accurate when interpreted in a clinical setting, with the patient present in person, rather than in a training setting using dermoscopic images of the skin lesions [22]. This implies that collecting information of the clinical history of the lesion (and patient) further improves the diagnostic accuracy of the physicians. Regarding these findings and the results of our study, teaching the basics of PSL to GPs could be complementary to further reduce the number of unnecessary referrals to dermatologists.
Strengths and Limitations
This is the first study to evaluate the added value of teaching basic knowledge of PSL in addition to clinical melanoma recognition to GPs in order to improve their diagnostic accuracy of melanoma in a training setting. There are some limitations to our study. Firstly, only 56 GPs completed the questionnaire. Secondly, the 15 clinical images of PSL shown to the GPs were subjectively chosen. The proportion of melanomas (one melanoma/two benign PSL) was higher than the actual cases encountered in daily general practice. However, this was necessary in order to determine whether the several clinical types of melanomas were properly diagnosed by the GPs. Thirdly, the diagnostic accuracy of the GPs was assessed in a training setting using clinical images of PSL associated to a brief clinical history. The advantage of these clinical cases was to place the GPs in a realistic situation, but it might not always reflect the GPs’ performances in their daily clinical practice.
Implications for Research and Practice
In this training setting, GPs acquired important theoretical knowledge about melanoma and learned to recognize common typical benign PSL, such as subungueal hematoma and halo nevus, by their clinical and theoretical characteristics. They learned how to use this knowledge when dealing with a patient seeking medical advice for a suspicious skin lesion. Teaching this basic knowledge allowed GPs to better triage the lesions into melanomas and benign lesions. This seems promising for reducing unnecessary dermatologist referrals in clinical practice. In the future, further clinical trials are needed to confirm the complementarity and long-term effectiveness of teaching these basics along with training in melanoma detection using clinical diagnosis or dermoscopy.
References
Buckley D, McMonagle C (2014) Melanoma in primary care. The role of the general practitioner. Ir J Med Sci 183:363–368. https://doi.org/10.1007/s11845-013-1021-z
Grange F, Barbe C, Mas L, Granel-Brocard F, Lipsker D, Aubin F, Velten M, Dalac S, Truchetet F, Michel C, Mitschler A, Arnoult G, Buemi A, Dalle S, Reuter G, Bernard P, Woronoff AS, Arnold F (2012) The role of general practitioners in diagnosis of cutaneous melanoma: a population-based study in France. Br J Dermatol 167:1351–1359. https://doi.org/10.1111/j.1365-2133.2012.11178.x
Goulart JM, Quigley EA, Dusza S, Jewell ST, Alexander G, Asgari MM et al (2011) Skin cancer education for primary care physicians: a systematic review of published evaluated interventions. J Gen Intern Med 26:1027–1035. https://doi.org/10.1007/s11606-011-1692-y
Fee JA, McGrady FP, Rosendahl C, Hart ND (2019) Training primary care physicians in dermoscopy for skin cancer detection: a scoping review. J Cancer Educ 35:643–650. https://doi.org/10.1007/s13187-019-01647-7
Friedman RJ, Rigel DS, Kopf AW (1985) Early detection of malignant melanoma: the role of physician examination and self-examination of the skin. CA Cancer J Clin 35:130–151. https://doi.org/10.3322/canjclin.35.3.130
Girardi S, Gaudy C, Gouvernet J, Teston J, Richard MA, Grob JJ (2006) Superiority of a cognitive education with photographs over ABCD criteria in the education of the general population to the early detection of melanoma: a randomized study. Int J Cancer 118:2276–2280. https://doi.org/10.1002/ijc.21351
Gachon J, Beaulieu P, Sei JF, Gouvernet J, Claudel JP, Lemaitre M, Richard MA, Grob JJ (2005) First prospective study of the recognition process of melanoma in dermatological practice. Arch Dermatol 141:434–438. https://doi.org/10.1001/archderm.141.4.434
Bakos RM, Blumetti TP, Roldán-Marín R, Salerni G (2018) Noninvasive imaging tools in the diagnosis and treatment of skin cancers. Am J Clin Dermatol 19:3–14. https://doi.org/10.1007/s40257-018-0367-4
Peuvrel L, Quereux G, Jumbou O, Sassolas B, Lequeux Y, Dreno B (2009) Impact of a campaign to train general practitioners in screening for melanoma. Eur J Cancer Prev 18:225–229. https://doi.org/10.1097/CEJ.0b013e32831bc3b2
Eide MJ, Asgari MM, Fletcher SW, Geller AC, Halpern AC, Shaikh WR, Li L, Alexander GL, Altschuler A, Dusza SW, Marghoob AA, Quigley EA, Weinstock MA, for the INFORMED (INternet course FOR Melanoma Early Detection) Group (2013) Effects on skills and practice from a web-based skin cancer course for primary care providers. J Am Board Fam Med 26:648–657. https://doi.org/10.3122/jabfm.2013.06.130108
Beecher SM, Keogh C, Healy C (2018) Dedicated general practitioner education sessions can improve diagnostic capabilities and may have a positive effect on referral patterns for common skin lesions. Ir J Med Sci 187:959–963. https://doi.org/10.1007/s11845-018-1788-z
Grange F, Woronoff AS, Bera R, Colomb M, Lavole B, Fournier E, Arnold F, Barbe C (2014) Efficacy of a general practitioner training campaign for early detection of melanoma in France. Br J Dermatol 170:123–129. https://doi.org/10.1111/bjd.12585
Argenziano G, Puig S, Zalaudek I, Sera F, Corona R, Alsina M, Barbato F, Carrera C, Ferrara G, Guilabert A, Massi D, Moreno-Romero JA, Muñoz-Santos C, Petrillo G, Segura S, Soyer HP, Zanchini R, Malvehy J (2006) Dermoscopy improves accuracy of primary care physicians to triage lesions suggestive of skin cancer. J Clin Oncol 24:1877–1882. https://doi.org/10.1200/JCO.2005.05.0864
Koelink CJL, Vermeulen KM, Kollen BJ, de Bock GH, Dekker JH, Jonkman MF, van der Heide WK (2014) Diagnostic accuracy and cost-effectiveness of dermoscopy in primary care: a cluster randomized clinical trial. J Eur Acad Dermatology Venereol 28:1442–1449. https://doi.org/10.1111/jdv.12306
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)-a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381. https://doi.org/10.1016/j.jbi.2008.08.010
Harris PA, Taylor R, Minor BL, Elliott V, Fernandez M, O’Neal L et al (2019) The REDCap consortium: building an international community of software platform partners. J Biomed Inform 95:103208. https://doi.org/10.1016/j.jbi.2019.103208
Dinnes J, Deeks JJ, Grainge MJ, Chuchu N, Ferrante di Ruffano L, Matin RN, et al. (2018) Visual inspection for diagnosing cutaneous melanoma in adults. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD013194
Abbasi NR, Shaw HM, Rigel DS, Friedman RJ, McCarthy WH, Osman I et al (2004) Early Diagnosis of cutaneous melanoma. JAMA 292:2771–2776. https://doi.org/10.1001/jama.292.22.2771
Argenziano G, Giacomel J, Abramavicus A, Pellacani G, Longo C, De Pace B et al (2012) Improving triage and management of patients with skin cancer: challenges and considerations for the future. Expert Rev Anticancer Ther 12:609–621. https://doi.org/10.1586/era.12.38
Ahmadi K, Prickaerts E, Smeets JGE, Joosten VHMJ, Kelleners-Smeets NWJ, Dinant GJ (2018) Current approach of skin lesions suspected of malignancy in general practice in the Netherlands: a quantitative overview. J Eur Acad Dermatology Venereol 32:236–241. https://doi.org/10.1111/jdv.14484
Kittler H, Pehamberger H, Wolff K, Binder M (2002) Diagnostic accuracy of dermoscopy. Lancet Oncol 3:159–165. https://doi.org/10.1016/S1470-2045(02)00679-4
Dinnes J, Deeks JJ, Chuchu N, Ferrante di Ruffano L, Matin RN, Thomson DR, et al. (2018) Dermoscopy, with and without visual inspection, for diagnosing melanoma in adults. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD011902.pub2
Acknowledgements
The authors would like to thank all the GPs that kindly participated in this study. They are also grateful to the organizers of the different GLEM (Groupe Local d’Évaluation MÉdicale) as well as the Centre AcadÉmique de MÉdecine GÉnÉrale (CAMG) of the UniversitÉ Catholique de Louvain for their support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
The study was approved by the Ethical Committee of the Catholic University of Louvain in Brussels, Belgium.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Harkemanne, E., Goublomme, N., Sawadogo, K. et al. Early Melanoma Detection in Primary Care: Clinical Recognition of Melanoma is Not Enough, One Must Also Learn the Basics. J Canc Educ 37, 898–904 (2022). https://doi.org/10.1007/s13187-020-01897-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-020-01897-w