Abstract
We describe the case of 74-year-old-male, previously treated with fronto-parietal craniotomy due to primary glioblastoma multiforme (GBM), followed by concurrent radiation therapy (RT) and temozolomide (TMZ) chemotherapy. Magnetic resonance imaging (MRI) of the brain, at 1 month after completing RT + TMZ, depicted partial response. Three months later, the patient was submitted to a further brain MRI, that resulted doubtful for therapy induced changes (i.e., pseudoprogression). The patient, who had been previously treated with prostatectomy for prostate cancer (PC), underwent a positron emission tomography/computed tomography (PET/CT) scan with 18F-choline for PC biochemical recurrence. 18F-choline whole body PET/CT resulted negative for PC relapse, while segmental brain PET, co-registered with MRI, demonstrated increased tracer uptake corresponding to tumor boundaries. In order to solve differential diagnosis between pseudoprogression and GBM recurrence, brain PET/CT with 18F-L-dihydroxy-phenil-alanine (18F-DOPA) was subsequently performed: fused axial PET/MRI images showed increased 18F-DOPA incorporation in the peri-tumoral edema, but not in tumor boundaries, consistent with the suspicion of GBM pseudoprogression, as then confirmed by clinical and radiological follow-up.
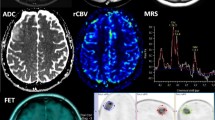
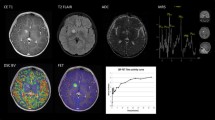
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Over the years, the prognosis of glioblastoma multiforme (GBM), the most frequent and lethal primary brain tumor, has remained dismal, with a median survival from initial diagnosis of less than 15 months [1]. Brain magnetic resonance imaging (MRI) covers a primary role for GBM assessment both at pre-treatment and post-therapy phase [2]. However, recently introduced combined radiotherapy/chemotherapy regimens have determined new challenges for the evaluation of GBM response to treatment, mainly due to the so-called pseudoprogression phenomenon, consisting of treatment-related clinico-radiologic changes mimicking true tumor progression [3]. In this scenario, molecular imaging with positron emission tomography/computed tomography (PET/CT) has been successfully exploited for the discrimination between progression and pseudoprogression, by utilizing different radiopharmaceuticals [4]. Here, we report the different findings of PET-imaging carried out, respectively, with 18F-choline and 18F-L-dihydroxy-phenyl-alanine (18F-DOPA) in a case of a GBM patient, with suspected pseudoprogression.
Case Report
A 74-year-old man, who had been treated with prostatectomy for prostate cancer (PC) (adenocarcinoma, Gleason score 7, pT2) 5 years ago, was diagnosed with isocitrate dehydrogenase (IDH) wild-type grade IV GBM, characterized by O6-methylguanine-DNA-methyltransferase (MGMT) promoter methylated status, submitted to left fronto-parietal craniotomy. Surgical resection was planned to be as maximal as possible avoiding additional neurological morbidity; however, taking into account tumor pattern of infiltration and patient’s overall performance status (pre-operatory Karnofsky Performance Score (KPS) = 70), gross total resection resulted unfeasible. Forty days after surgery, the patient underwent adjuvant concurrent radiotherapy (RT) and chemotherapy. Radiotherapy was carried out through fractionated focal irradiation (i.e., dose = 2 Gy/fraction) administered once daily 5 days per week during a period of 6 weeks, for a total dose of 60 Gy, while concomitant chemotherapy consisted of temozolomide (TMZ) administered at 75 mg/m2 for 42 days concurrently with focal radiotherapy. Brain magnetic resonance imaging (MRI) acquired before RT + TMZ (Fig. 1) demonstrated residual GBM, while MRI at 1-month post RT + TMZ revealed partial regression of the fronto-parietal lesion and the appearance of peri-tumoral edema (Fig. 2). After MRI execution, the patient started the 1st cycle of TMZ as monotherapy that was quickly discontinued due to hematological toxicity (platelets count = 50,000/µL). The patient was monitored through serial clinical and laboratory examinations for the following 3 months. A further MRI, performed at 4-month post RT + TMZ, demonstrated meaningfully enlarged peri-tumoral edema involving the left fronto-parietal and temporal regions with a polycyclic area of enhancement (Fig. 3), doubtful for therapy-induced changes (i.e., pseudoprogression).
Brain magnetic resonance imaging (MRI) acquired before RT + TMZ demonstrated a round-oval, homogeneous, well-demarcated, hyperintense lesion at T2-weighted images in left fronto-parietal region (a, yellow arrow), as a well as a central core of contrast enhancement at T1-weighted image (b, yellow arrow), compatible with residual GBM
MRI, performed at 4-month post RT + TMZ, demonstrated meaningfully enlarged peri-tumoral edema involving the left fronto-parietal and temporal regions as evident at T2-weighted image (a, yellow arrows) with a polycyclic area of enhancement at T1-weighted axial (b, yellow arrow), doubtful for therapy-induced changes (i.e., pseudoprogression)
Since a progressive increase of PSA value (i.e., 1.3 ng/mL) has been registered, the patient was scheduled to perform a PET/CT with 18F-choline by his referring urologist. Two weeks after MRI PET/CT was performed 60 min after the intravenous (i.v.) injection of 3.7 MBq/kg of 18F-choline: standard whole body (from proximal thigh to skull base) PET/CT scan was acquired with a digital Biograph Vision PET/CT system (Siemens Healthcare; Erlangen, Germany) and resulted negative for PC localizations. Immediately after standard whole body execution, brain PET/CT was acquired according to the following procedure: a CT scan of the head was performed with slice thickness of 1.0 mm, pitch factor 1, bone and soft tissue reconstruction kernels and maximum of 120 keV and 90 mAs by applying CARE kV and CARE Dose; after CT scanning, brain PET was acquired with a scanning time of 20 min in 3D (matrix: 440 × 440) with a zoom factor of 1.0. Reconstruction was conducted with a TrueX + TOF algorithm and Gauss-filtered to a transaxial resolution of 2 mm at FWHM (full width at half maximum); attenuation correction was performed using the low dose non-enhanced computed tomography data. Axial PET images were co-registered, through a dedicated software (PET VCAR, Advantage Workstation 4.7; GE Healthcare, Milwaukee, USA), with the corresponding contrast-enhanced T1-weighted MRI: emissive PET and fused PET/MRI images demonstrated mildly increased tracer incorporation within brain tumor boundaries (Fig. 4) with a maximum standardized uptake value (SUVmax) of 2.4 while tumor-to-normal contralateral cortex activity ratio (T/N ratio), indicating the ratio of SUVmax (measured on tumor) and SUVmean (measured on contralateral normal cortex) [5], resulted in 3.1, rising the suspicion of metabolically active GBM viable tissue. The patient was scheduled for the execution of PET/CT with 18F-DOPA to achieve the differential diagnosis between pseudoprogression versus GBM recurrence. Two weeks later, the patient underwent brain PET/CT with 18F-DOPA, which was carried out 20 min after the administration of 200 MBq of the tracer, with a scanning time of 20 min, by employing the same device and reconstruction parameters previously described for 18F-choline brain PET: emissive PET and fused PET/MRI axials showed increased tracer incorporation within the peri-tumoral edema located in the semioval centrum of the left fronto-parietal lobe (Fig. 5): semiquantitative parameters were calculated following international guidelines [6] with a SUVmax of 4.3, a T/N of 2.2, and tumor to striatum (T/S) of 1.4; notably, no meaningful increased tracer uptake was observed within tumor boundaries. The overall 18F-DOPA distribution was considered consistent with non-specific tracer incorporation within RT/TMZ-induced vasogenic edema and, after a multidisciplinary consensus meeting, also taking into account patient’s stable clinical status, he was submitted to steroid therapy with dexamethasone (12 mg daily) and to clinical and imaging monitoring.
18F-choline PET acquired a 4-month and 15 days post treatment. Emissive PET (a), contrast-enhanced T1-weighted MRI (b), and fused PET/MRI axial images (c) demonstrated mildly increased tracer incorporation within brain tumor boundaries (black and white arrows, respectively), suggestive of viable tumor tissue
18F-DOPA PET acquired 2 weeks later.18F-choline PET. Emissive PET (a), contrast-enhanced T1-weighted MRI (b), and fused PET/MRI axial images (c) showed increased tracer incorporation within the peri-tumoral edema located in the semioval centrum of the left fronto-parietal lobe (black and white arrows, respectively), interpreted as vasogenic edema
A follow-up MRI performed after a 3-month interval depicted a meaningful reduction of the peri-tumoral edema, as well as the regression of the pathological polycyclic enhancement previously described (Fig. 6), thus confirming the diagnosis of pseudoprogression.
A follow-up MRI performed after a 3-month interval depicted a meaningful reduction of the peri-tumoral edema (T2-weighted, a, yellow arrow), as well as the regression of the pathological polycyclic enhancement previously described (T1-weighted, b, yellow arrow), thus confirming the diagnosis of pseudoprogression
Discussion
Pseudoprogression represents a well-known phenomenon, occurring more often in the first 3 months after therapy completion in about the 50% of patients treated with concurrent RT + TMZ [7]. This phenomenon has been attributed to increased capillary permeability induced by RT and subsequently enhanced by chemotherapy, leading to interstitial fluid transudation and brain edema. Several efforts have been made to develop innovative MRI techniques, with the aim of discriminating pseudoprogression from GBM recurrence [8]. In this scenario, PET-based approaches, employing several radiopharmaceuticals suitable for investigating pathological processes at a cellular and metabolic level, are warmly welcome. 18F-fluorodeoxyglucose ([18F]FDG), the most widely utilized tracer in clinical practice, has a limited role for the imaging of brain lesions due to the non-favorable tumor-to-background ratio, although it has been demonstrated a correlation between its uptake and tumors’ cellularity and aggressiveness [9]. To overcome the limitations of [18F]FDG PET in neurooncology, other tracers have been introduced. 11C- or 18F-choline, a surrogate biomarker of phospholipids’ synthesis, routinely used for the imaging of non-FDG avid tumors, such as prostate cancer and hepatocellular carcinoma, proved useful for gliomas’ pre-surgical grading and evaluation after therapy [10, 11]. In a previously published meta-analysis [12], choline PET/CT presented high pooled sensitivity (i.e., 0.87) and specificity (i.e., 0.82) for the discrimination between glioma recurrence and radionecrosis. As an alternative to choline PET, radiolabeled amino-acids, such as 11C-methionine (11C-MET), 18F-fluoroethyl-tyrosin (FET), and 18F-DOPA, have been utilized for the imaging of brain tumors through PET/CT [13].
A systematic review and meta-analysis performed by Treglia et al. compared the various tracers ([18F]FDG, radiolabeled choline and amino-acids) for PET/CT imaging of gliomas in different clinical settings (i.e., evaluation of suspicious brain lesions, glioma grading and delineation, diagnosis of recurrence, etc.) and found highest diagnostic performance values for radiolabeled amino-acids with respect to the other radiopharmaceuticals [14]. Furthermore, several reports have underlined the prognostic impact of quantitative PET-derived indices, particularly T/N value, for discriminating recurrence from necrosis [15]. Few studies have compared choline and amino-acid PET for the imaging of gliomas: as far as it concerns the differential diagnosis between radionecrosis (RN) and tumor, Bolcaen and coworkers compared three different tracers (i.e. [18F]FDG, 18F-methylcholine and FET) in a GBM rat model and found that FET outperformed, especially at quantitative analysis, 18F-methylcholine for the discrimination between viable GBM tumor and RN [16]. In our patient, both 18F-choline and 18F-DOPA brain PET showed increased tracer uptake with meaningful T/N value, although with a clearly different pattern of distribution among the 2 radiopharmaceuticals at co-registered PET/MRI. The discrepancy among choline and 18F-DOPA uptake in our patient might be explained by several reasons: firstly, the aforementioned tracers have distinct mechanisms of incorporation, since choline uptake is mediated by choline transporter-like 1 (CTL-1), which has been found up-regulated also in macrophages during inflammatory states [17], while 18F-DOPA enters into tumor cells through system L-amino-acid transporters (LAT) [18]. Secondly, preliminary reports indicate that amino-acid PET tracers’ uptake into brain tumors is less dependent from blood–brain barrier (BBB) breakdown with respect to choline’s uptake [18]. Fused PET/MRI resulted particularly useful to precisely localize tracers’ incorporation in relation to MRI morphological findings: as a matter of fact, in our patient the pattern of 18F-choline’s distribution strictly resembled contrast-enhancement rim, thus being most likely attributable to non-specific uptake due to BBB-rupture and migrating macrophages to lesion’s boundaries. Furthermore, it has to be highlighted that in our patient a time gap of 15 days passed between MRI scan suspected for pseudoprogression and 18F-choline PET execution, and a further fifteen-day interval elapsed before 18F-DOPA scan, therefore we cannot exclude that this time-difference, although not particularly relevant, might have interfered with the results of the 2 distinct PET examinations. Worthy of note, pseudoprogression has been more often reported within the first 12 weeks after RT + CT completion, but some cases with later onset have been described; therefore, the optimal timing for performing PET/CT post therapy has still to be defined yet [13].
The case we describe suggests that a positive finding on 18F-choline PET-imaging, when pseudoprogression is suspected, should be cautiously interpreted. Amino-acid PET, especially when performed through hybrid PET/MRI technology, should be recommended as the first choice radionuclide-imaging modality for the challenging differential diagnosis between tumor and pseudoprogression in GBM.
The introduction of novel combined therapeutic regimens (e.g., RT + TMZ, regorafenib, bevacizumab, etc.) are going to thoroughly change gliomas’ management, also entailing, as a less-welcomed counterpart, novel diagnostic dilemmas. In this perspective, the combined use of a highly performing diagnostic technique, such as hybrid PET/MRI with radiolabeled amino acids, holds the promise to move the field forward [19].
Data Availability
Not applicable.
References
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJB, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005;352:987–96.
Shaffer A, Kwok SS, Naik A, Anderson AT, Lam F, Wszalek T, et al. Ultra-high-field MRI in the diagnosis and management of gliomas: a systematic review. Front Neurol. 2022;13: 857825.
Chawla S, Bukhari S, Afridi OM, Wang S, Yadav SK, Akbari H, et al. Metabolic and physiologic magnetic resonance imaging in distinguishing true progression from pseudoprogression in patients with glioblastoma. NMR Biomed. 2022;35:e4719.
Santo G, Laudicella R, Linguanti F, Nappi AG, Abenavoli E, Vergura V, et al. The utility of conventional amino acid pet radiotracers in the evaluation of glioma recurrence also in comparison with MRI. Diagnostics (Basel). 2022;12:844.
Kong Z, Zhang Y, Liu D, Liu P, Shi Y, Wang Y, et al. Role of traditional CHO PET parameters in distinguishing IDH, TERT and MGMT alterations in primary diffuse gliomas. Ann Nucl Med. 2021;35:493–503.
Law I, Albert NL, Arbizu J, Boellaard R, Drzezga A, Galldiks N, et al. Joint EANM/EANO/RANO practice guidelines/SNMMI procedure standards for imaging of gliomas using PET with radiolabelled amino acids and [18F]FDG: version 1.0. Eur J Nucl Med Mol Imaging. 2019;46:540–57.
Gerstner ER, McNamara MB, Norden AD, LaFrankie D, Wen PY. Effect of adding temozolomide to radiation therapy on the incidence of pseudo-progression. J Neurooncol. 2009;94:97–101.
Thust SC, van den Bent MJ, Smits M. Pseudoprogression of brain tumors: pseudoprogression of Brain Tumors. J Magn Reson Imaging. 2018;48:571–89.
Palumbo B, Angotti F, Marano GD. Relationship between PET-FDG and MRI apparent diffusion coefficients in brain tumors. Q J Nucl Med Mol Imaging. 2009;53:17–22.
Gómez-Río M, Testart Dardel N, Santiago Chinchilla A, Rodríguez-Fernández A, Olivares Granados G, Luque Caro R, et al. 18F-Fluorocholine PET/CT as a complementary tool in the follow-up of low-grade glioma: diagnostic accuracy and clinical utility. Eur J Nucl Med Mol Imaging. 2015;42:886–95.
Filippi L, Schillaci O, Bagni O. Recent advances in PET probes for hepatocellular carcinoma characterization. Expert Rev Med Devices. 2019;16:341–50.
Gao L, Xu W, Li T, Zheng J, Chen G. Accuracy of 11C-choline positron emission tomography in differentiating glioma recurrence from radiation necrosis: a systematic review and meta-analysis. Medicine. 2018;97: e11556.
Galldiks N, Law I, Pope WB, Arbizu J, Langen K-J. The use of amino acid PET and conventional MRI for monitoring of brain tumor therapy. Neuroimage Clin. 2017;13:386–94.
Treglia G, Muoio B, Trevisi G, Mattoli MV, Albano D, Bertagna F, et al. Diagnostic performance and prognostic value of PET/CT with different tracers for brain tumors: a systematic review of published meta-analyses. Int J Mol Sci. 2019;20:E4669.
Chiaravalloti A, Fiorentini A, Villani V, Carapella C, Pace A, Di Pietro B, et al. Factors affecting 18F FDOPA standardized uptake value in patients with primary brain tumors after treatment. Nucl Med Biol. 2015;42:355–9.
Bolcaen J, Descamps B, Deblaere K, Boterberg T, De Vos PF, Kalala J-P, et al. (18)F-fluoromethylcholine (FCho), (18)F-fluoroethyltyrosine (FET), and (18)F-fluorodeoxyglucose (FDG) for the discrimination between high-grade glioma and radiation necrosis in rats: a PET study. Nucl Med Biol. 2015;42:38–45.
Brindle KM, Izquierdo-García JL, Lewis DY, Mair RJ, Wright AJ. Brain tumor imaging. J Clin Oncol. 2017;35:2432–8.
Verburg N, Koopman T, Yaqub M, Hoekstra OS, Lammertsma AA, Schwarte LA, et al. Direct comparison of [11C] choline and [18F] FET PET to detect glioma infiltration: a diagnostic accuracy study in eight patients. EJNMMI Res. 2019;9:57.
Jabeen S, Arbind A, Kumar D, Singh PK, Saini J, Sadashiva N, et al. Combined amino acid PET-MRI for identifying recurrence in post-treatment gliomas: together we grow. Eur J Hybrid Imaging. 2021;5:15.
Author information
Authors and Affiliations
Contributions
LF was responsible for the idea. LF, AS, and BP wrote the manuscript. OB was responsible for PET/CT execution. BP performed PET/MRI co-registration and fusion. OS supervised the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
Luca Filippi, Angela Spanu, Oreste Bagni, Orazio Schillaci, and Barbara Palumbo declare no conflict of interest.
Ethics Approval and Consent to Participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent for Publication
Written consent has been obtained from the participant for the anonymized use of data for research purpose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Filippi, L., Spanu, A., Bagni, O. et al. Imaging Findings of 18F-Choline and 18F-DOPA PET/MRI in a Case of Glioblastoma Multiforme Pseudoprogression: Correlation with Clinical Outcome. Nucl Med Mol Imaging 56, 245–251 (2022). https://doi.org/10.1007/s13139-022-00758-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-022-00758-2