Abstract
Filarial parasites like Brugia pahangi and Brugia malayi can infect dogs. Adults of Brugia genus resides in the lymphatic system and microfilariae, in blood. There are increasing reports of detection of B. malayi microfilariae in dogs. A study was undertaken to compare the efficacy of repeated oral dosing of ivermectin (IVT) and diethylcarbamazine (DEC), individually and in combination against naturally infected B. malayi microfilariae in dogs. The species of the microfilariae was confirmed by acid phosphatase staining and polymerase chain reaction. The three treatment groups were 200 mcg/kg body weight IVT daily for 14 days (I), 6.6 mg/kg body weight DEC daily for 14 days (II) and IVT and DEC together in the same dose for a period of 5 days (III). Microfilarial status of the peripheral blood was assessed on the 0th, 7th, 14th and 21st day. Haematological parameters were measured on day zero and on the 21st day. Though, all the three treatment groups showed a reduction in the microfilarial concentration through the study period, complete absence of detectable microfilaremia was not noticed in any of the three groups by 21st day. Among the haematological parameters, statistically significant difference was observed in the post-treatment means of haemoglobin levels of group III when compared with group II. Since group III regime (IVT + DEC) was shorter and just as effective as the longer ones, it is considered superior to the other two.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A wide range of filarial parasites are being detected in animals. Often these agents have a zoonotic potential. Filariasis due to Brugia malayi accounts to 5% of the human filariasis in India (Suma 2013). Among different states, Kerala is endemic for human brugian filariosis. B. malayi is reported from dogs in Kerala resulting in a wide range of manifestations from amicrofilaremia to lymphedema (Ambily et al. 2011; Chirayath et al. 2017a, b). Albendazole and diethylcarbamazine are the microfilaricidal drugs used worldwide as part of the Global Elimination of Lymphatic Filariosis Program (GELFP) with the objective of reducing microfilariae levels below the transmission rate by Mass Drug Administration (MDA), in areas where the disease is endemic. Successful use of ivermectin and DEC in brugian filariosis has been reported in felines and Indian leaf nose monkey. DEC has been used successfully to treat microfilaremia caused by Dirofilaria immitis in canines but there exists a paucity of literature for the use of these drugs against microfilariae of Brugia spp. Hence the current case study was undertaken to compare the efficacy of these agents in canines.
Materials and methods
Identification of positive cases
A total of 3000 dogs above the age of 4 months presented to the University Veterinary Hospital Kokkalai and Teaching Veterinary Clinical Complex, Mannuthy, Thrissur, Kerala, India, for various complaints, general check-up or vaccination were screened by wet blood film examination for moving microfilariae during 8:00 am to 4:30 pm. Thick blood smears prepared from dogs positive for wet film examination from ear pinna, for moving microfilariae were subjected to Giemsa staining. Blood smears from dogs positive for sheathed microfilariae by Giemsa staining were subjected to acid phosphatase staining according to the procedure described by Chalifoux and Hunt (1971). Eighteen dogs with microfilarial staining pattern by acid phosphatase method as that of B. malayi were selected for the study. Clinical signs were recorded for the positive cases of brugian filariosis.
Species of the microfilariae were confirmed by polymerase chain reaction (PCR). Genomic DNA was extracted from whole blood and PCR was conducted using primers for amplification of Hha 1 repeat sequences (Xie et al. 1994). PCR products obtained were sequenced analyzed using Basic Local Alignment Search Tool (BLAST) and submitted to GenBank.
Treatment protocol
Positive cases with brugian microfilaria were randomly divided into three groups with 6 animals in each group. The drug regimen was started from the subsequent day onwards.
-
Group I—Ivermectin @ 200 µg/kg body weight orally for 2 weeks
-
Group II—Diethylcarbamazine @ 6.6 mg/kg body weight orally for 2 weeks
-
Group III—Ivermectin (IVT) @ 200 µg/kg body weight with diethylcarbamazine (DEC) @ 6.6 mg/kg body weight orally for 5 days
Cases which were heavily positive on wet film examination were given prednisolone @ 1 mg/kg body weight orally for 3 days from the start of the chemotherapy to prevent a possible post-treatment inflammatory reaction activated during the process of killing of microfilariae.
Treatment response
Response to treatment was assessed based on the microflilaremic status of peripheral blood along with improvement in the haematological parameters.
Microfilaremic status
The number of microfilariae in the thick blood smear prepared from 25 µl of peripheral blood was counted on the 0th, 7th, 14th and 21st day.
Haemtological parameters
Haematological parameters were assessed on the 0th and 21st day by collecting whole blood (2 ml) in EDTA vials for evaluation of the total erythrocyte count (TEC), volume of packed red cells (VPRC), haemoglobin (Hb) concentration, total leukocyte count (TLC), differential leukocyte count (DLC) and platelet count using automatic animal blood cell counter.
Statistical analysis
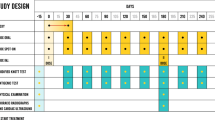
Haematological parameters were analyzed using paired t test. The results in between the groups was assessed using one was analysis of co-variance (ANOVA). The microfilarial counts on weekly basis in the three groups were assessed using repeated measures ANOVA for Day 0, 7, 14 and 21. The analysis was done using the statistical package, Statistical Package for Social Sciences (SPSS) version 24.0 (Fig. 1).
Results
Identification of positive cases
Brugia malayi microfilariae were identified by the demonstration of metabolic activity at four points (amphids, phasmids, anal and excretory pore) by precipitation of red azo dye (Plate 1) after acid phosphatase staining (Chirayath et al. 2015, 2017b).
Polymerase chain reaction with Hha1 primers gave an amplified PCR product of 322 bp. The product obtained was sequenced and analyzed using Basic Local Alignment Search Tool (BLAST). The product revealed 99% homology with B. malayi isolate. Nucleotide sequence data reported in this paper are available in the GenBank™ under the accession number: MG063782.
Out of the 3000 dogs screened, seventy were positive for brugain filariosis. Of the 70 cases, 27 cases were asymptomatic. The clinical symptoms could be divided into generalised signs (anorexia, pyrexia and congested mucous membrane), gastrointestinal signs (vomiting), dermatological signs (alopecia and dermatitis), lymphatic signs (lymphadenopathy, lymphangitis, limb edema, scrotal edema and lameness) and ophthalmological signs (lacrimation and corneal opacity). Pyrexia was the most common clinical finding and was seen in 40% of the cases. Apart from the generalised signs, lymphadenopathy was most commonly observed (31.42%) followed by limb edema (22.85%).
Evaluation of treatment groups bases on microfilaremic count
The microfilaremic counts in individual cases and the mean microfilaremic counts in the three groups are shown in Tables 1, 2, 3 and 4. Though, all the three treatment groups showed a reduction in the microfilarial concentration during the weekly assessment, complete absence of detectable microfilaremia was not noticed in any of the three groups till the 21st day. By the 21st day the average microfilaraemic count had dropped to 1.333 in group I and II, while it was 1.167 in group III.
Evaluation of treatment based on haematological parameters
The mean TEC, VPRC, Hb, TLC, DLC and platelet groups are shown in Tables 5, 6, 7, 8 and 9 respectively. The mean TEC values of the first two groups on day zero and 21st day when compared to the standard values revealed a mild anaemia. Though there was an increase in the TEC values on the 21st day, the difference was not statistically significant. Both the pre and post-treatment mean values of VPRC in all the three groups were below the standard normal range for dogs. A slight increase was noticed in VPRC from the pre-treatment to post-treatment values which were not statistically significant. The pre-treatment haemoglobin values were lower than the standard values in first and second group. The values had improved post-treatment in all the three groups. Statistically significant difference was observed in the post-treatment means of group III when compared with group II.
The average total leukocyte count of Group I and II were higher than the standard values whereas group III was similar to the standard range. The post-treatment total leukocyte values of all the three groups were within the normal range thus indicating an improvement in this parameter. However, the improvement was not statistically different. Both, the pre and post-treatment values were within the standard range for lymphocyte per cent. The pre-treatment granulocyte per cent was slightly higher than the higher range of the standard granulocyte per cent for all the three groups. The post-treatment values were in the standard range for group II and III. The pre-treatment average of platelets in group II was lower than that of the standard value. There was a mild increase in the platelet count in all the three groups post-treatment.
Discussion
In Ivermectin (2 weeks) treated group, gradual decrease in microfilaremia over the weeks was similar to the response noted previously in humans (Reddy et al. 2000) and animals (Murthy et al. 2004; Taweethavonsawat and Chungpivat 2013). Complete microfilaricidal action by the 21st day was detected only in one animal. This treatment was further supported (Phantana et al. 2002) where single oral or subcutaneous administration of ivermectin were used to reduce the microfilarial load in cats with B. malayi microfilariae.
In Diethyl carbamazine (2 weeks) treated group, rapid decrease of microfilarial counts were observed. Similar response is reported with DEC treatment in Indian leaf monkeys with Brugian microfilariae (Murthy et al. 2004). 12 days regimen of DEC followed in human patients also resulted in a rapid short term microfilarial suppression (Fernando et al. 2010). The variance seen in individuals, with some cases showing 100% microfilaricidal action whereas only 72–85% clearance in other cases, similar to previous reports (Stolk et al. 2005), where high variance in the efficacy of the DEC treatment was reported.
When iveremectin was combined with DEC for 5 days, there was drastic reduction in the microfilarial count when compared to the day of presentation. Complete microfilaricidal action was seen in two animals of the group by the 21st day and this finding was comparable to reported results (Chansiri et al. 2005), where single dose of ivermectin and DEC was used in cats infected with B. malayi. They reported that complete clearance of the microfilaria was dependent on the initial microfilaria load and animals with lower burden showed faster clearance. Further studies could investigate long term microfilaricidal action in dogs using single dose administration with a combination. Shorter duration of therapy would increase owner compliance and reduces the cost of the treatment.
Mild anemia, leukocytosis and thrombopaenia were noted in microfilaraemic animals. These finding were similar to that seen in previous studies conducted (Ambily 2009; Chirayath 2013; Thomas 2016). Anaemia, thrombocytosis and leukocytosis in animals infected with Dipetalonema reconditum have been previously reported (Hashem and Badawy 2008) and this was similar to the results of the haematological assessment in the current study. They attributed the anemia to the haemolytic activity of the microfilariae.
There was no statistically significant improvement in the haematological parameters of any of the groups after treatment. Amongst the six haematological parameters assessed between the three groups, statistically significant difference was noted only for the haemoglobin values. Group III (IVT + DEC) showed a statistical increase in the haemoglobin values on the 21st day when compared with group II.
Conclusion
There was no significant difference in the weekly assessment of the microfilaraemic status in between the three treatment groups. A significant difference was noted in the microfilaraemic counts within the groups. The microfilaraemic count was found to be zero in individual cases in all the three groups. None of the treatments resulted in complete absence of detectable microfilaraemia by 21st day. Mild anemia, leukocytosis and thrombopaenia were noted in microfilaremic animals. Amongst the six haematological parameters assessed between the three groups, statistically significant difference was noted only for the haemoglobin values on the 21st day. Group III showed a statistical increase in the haemoglobin values on the 21st day when compared with group II.
Animals of group I (Ivermectin) and group II (DEC) were administered microfilaricidal drug for a period of 2 weeks whereas group III (Ivermectin + DEC) were given microfilaricidal drug for only 5 days. The results of group III showed no statistical difference when compared with the other two groups except for the increase in haemoglobin when compared to group II. However since this treatment regime was shorter and just as effective as the longer ones, it was considered superior to the other two.
References
Ambily VR (2009) Clinico-therapeutic studies on canine microfilariosis. M.V.Sc. thesis, Kerala Agricultural University, Thrissur
Ambily VR, Pillai UN, Arun S, Pramod S, Jayakumar KM (2011) Detection of human filarial parasite B. malayi in dogs by histochemical staining and molecular techniques. Vet Parasitol 181:210–214
Chalifoux L, Hunt RD (1971) Histochemical differentiation of Dirofilaria immitis and Dipetalonema reconditum. J Am Vet Med Assoc 158(5):601–605
Chansiri G, Khawsak P, Phantana S, Sarataphan N, Chansiri K (2005) The efficacy of a single-oral-dose administration of ivermectin and diethylcarbamazine on the treatment of feline Brugia malayi. Mol Cell Probes 16:129–135
Chirayath D (2013) Molecular characterization and therapeutic management of microfilariosis in dogs. Ph.D. thesis, Kerala Veterinary and Animal Sciences University, Pookode
Chirayath D, Alex PC, Usha NP (2015) Microscopic characteristics of canine filariasis in Thrissur District of Kerala. Indian Vet J 92:81–82
Chirayath D, Alex PC, Usha NP, George S, Ajithkumar S, Panicker VP (2017a) Identification of Brugia malayi in dogs in Kerala, India. Trop Biomed 34:804–814
Chirayath D, Alex PC, Usha NP (2017b) Immunoblotting analysis of canine B, malayi microfilarial antigens. Trop Biomed 34:815–821
Fernando SD, Rodrigo C, Rajapakse S (2010) Current evidence on the use of antifilarial agents in the management of bancroftian filariasis. J Trop Med 2011:175941
Hashem M, Badawy A (2008) Hematological and biochemical studies on filariasis of dogs. Internet J Vet Med 4(2):1–7
Murthy PK, Srivastava K, Murthy PSR (2004) Responses of Brugia malayi—Indian leaf monkey (Presbytis entellus), a non-human primate model of filariasis, to diethylcarbamazine, ivermectin and CDRI compound 82–437. Curr Sci 86(3):432–439
Phantana S, Sarataphan N, Chansiri G, Chansiri K (2002) Microfilaricidal efficacy of ivermectin on zoonotic Brugia malayi in naturally infected cats. J Trop Med Parasitol 25(25):11–16
Reddy G, Vengatesvarlou N, Das PK, Vanamail P, Vijayan AP, Kala S, Pani SP (2000) Tolerability and efficacy of single-dose diethyl carbamazine (DEC) or ivermectin in the clearance of Wuchereria bancrofti microfilaraemia in Pondicherry, south India. Trop Med Int Health 5(11):779–785
Stolk WA, Oortmarssen GJV, Pani SP, De Vlas SJ, Subramanian S, Das PK, Habbema JDF (2005) Effects of ivermectin and diethylcarbamazine on microfilariae and overall microfilaria production in bancroftian filariasis. Am J Trop Med Hyg 73(5):881–887
Suma TK (2013) Indian scenario of elimination of lymphatic filariasis. Medicine update. Asso Physicians India, Kolkata, pp 6–9
Taweethavonsawat P, Chungpivat S (2013) Successful Treatment of Brugia pahangi in naturally infected cats with ivermectin. Korean J Parasitol 51(6):759
Thomas J (2016) Clinical investigation on oedema of limbs in dogs. M.V.Sc thesis, Kerala Veterinary and Animal Sciences University, Pookode
Xie H, Bain O, Williams SA (1994) Molecular phylogenetic studies on Brugia filariae using Hha I repeat sequences. Parasite 1(3):255–260
Acknowledgements
The present paper is a part of MVSc thesis submitted to the Kerala Veterinary and Animal Sciences University and the authors are thankful to the University for the Facilities and grant rendered for the research.
Author information
Authors and Affiliations
Contributions
Poojary Vineeta Sadarama—MVSc scholar performed the research. Deepa Chirayath—Major guide for the MVSc Research who formulated the research work and gave instructions in performing the research and helped in preparing the manuscript. Usha Narayana Pillai—Minor guide for the MVSc research and Head of the Department who provided all guidance for the research. Bindu Lakshmanan—Minor Guide for the MVSc Research and guided for ELISA standardization.
Corresponding author
Ethics declarations
Ethical statement
There is no separate funding for this research project. The project is formulated following the guidelines of Institutional Animal Ethics Committee and got approval from faculty Research Committee with code number Ad/9/96/MVM/2015/CM. It is certified that all biomaterials required for the research were collected and the treatments were assigned, with prior written consent from the owners of the animals. There is no conflict of interest for the research findings. The article is a part of thesis submitted to Kerala Veterinary and Animal Sciences and submitted with consent from all authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sadarama, P.V., Chirayath, D., Pillai, U.N. et al. Comparison of efficacy of ivermectin and diethylcarbamazine against naturally infected Brugia malayi microfilaria in dogs. J Parasit Dis 43, 554–559 (2019). https://doi.org/10.1007/s12639-019-01126-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12639-019-01126-2