Abstract
Objectives
To confirm whether multicomponent exercise following vivifrail recommendations was an effective method for improving physical ability, cognitive function, gait, balance, and muscle strength in Chinese older adults.
Methods
This was a multicenter and randomized clinical trial conducted in Jiangsu, China, from April 2021 to April 2022. Intervention lasted for 12 weeks and 104 older adults with functional declines were enrolled. All participants were randomly assigned to a control (usual care plus health education) or exercise group (usual care plus health education plus exercise). Primary outcomes were the change score of Short Physical Performance Battery (SPPB) and activities of daily living (ADL). The secondary outcomes included instrumental activities of daily living, Tinetti scores, Frailty score, short-form Mini Nutritional Assessment, Mini-Mental State Examination, Geriatric Depression Scale-15, the 12-item Short Form Survey, 4-meter gait speed test, 6-min walking distance, grip strength, and body composition analysis.
Results
Among the participants, the average age was 85 (82, 88) years. After 12 weeks of follow-up, the exercise group showed a significant improvement in SPPB, with a change of 2 points (95% confidence interval [0, 3.5], P<0.001) compared to control. In contrast, SPPB remained stable in the control group. Compared to the control group, ADL improved in the exercise group, as did instrumental activities of daily living, Tinetti, Frailty, Short Form Survey, 4-meter gait speed test, and 6-min walking distance. Although there was no significant difference between groups in body composition analysis after post-intervention, the exercise group still improved in soft lean mass (P=0.002), fat-free mass (P=0.002), skeletal muscle mass index (P<0.001), fat-free mass index (P=0.004), appendicular skeletal muscle mass (P<0.001), and leg muscle mass (P<0.001), while the control group had no significant increase. No difference was observed in adverse events during trial period.
Conclusions
The multicomponent exercise intervention following vivifrail recommendations is an effective method for older adults with functional decline and can reverse the functional decline and improve gait, balance, and muscle strength. Additionally, the 12-week multicomponent exercise method provides guidance for Chinese medical professionals working in the field of geriatrics and is a promising method to improve physical function in the general population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Age-related functional decline in physical performance has become a common phenomenon in the aging population (1). Generally, functional assessment means objective evaluation of a person’s status, such as physical health, quality of self-maintenance, intellectual status, social activity, attitude toward the world and themselves, emotional status, and life satisfaction. Hospitals, communities, nursing homes, and homes have a high prevalence of functional decline. However, it was rare to identify functional status in older adults over time. Currently, the common predictor factors for the functional decline are age, dementia, comorbidities, polypharmacy, admission diagnosis, and physical activity, among others (2). As for the specific presentations about functional decline, they have been described variously in previous studies, such as increased health care use, loss of independence ability in society, increased rate of hospitalization, and prolonged hospitalization and increased risk of mortality (3, 4). The functional decline in elderly adults also indicates damage to lower muscle strength, balance performance, grip strength, gait, mobility, and self-care abilities, etc (5, 6). Physical performance measures and intervention in aging-related fields appear to be particularly important (7). Maintaining independence in older adults is a significant goal, particularly for those who have remained at the greatest risk of physical function decline and disability (5). If the process of functional decline is not stopped before it worsens, elderly adults can easily become disabled.
Notably, disability is not the final state from which an individual can recover based on intervention, including exercise (8). A longitudinal study of aging included 7,000 individuals, and after 6 years of follow-up, it showed that the program involved in physical activity exerted a protective role on functional ability (9). Another prospective cohort study found that nondisabled older adults living in the community, had a high risk of subsequent disability (10). Early screening, intervention, and management of functional status among older adults may be a good strategy to prevent disability in the aging process.
Older adults with disabilities usually require enormous costs and medical resources. The number of elderly Chinese people with disabilities was 52.7 million in 2020, which is projected to exceed 77 million by 2030 without intervention (11). Currently, over 1 billion people, or approximately 16% of the global population, are experiencing significant disability.
Older adultsrepresent a significant proportion of people with disabilities.
Some studies have confirmed the strong relationship between exercise and physical health, such as enhancing cardiovascular function, improving cognitive function, increasing muscle strength, reversing frailty, and improving quality of life (12–16). The multicomponent exercise intervention, which includes strength, endurance, and balance training, appears to be an effective method for maintaining a good physical status in elderly adults (17). Currently, several studies have demonstrated that multicomponent intervention is an effective method to reverse aging-related physical status (18–20). The 2021 International Exercise Recommendations in Older Adults put forward that exercise plays important roles and could be regarded as a preventive strategy for many chronic diseases (8). Although multicomponent exercise benefits are well recognized, to the best of our knowledge, there have been no standardized prospective clinical trials on functional decline in the Chinese older population.
China has the world’s largest older population, accounting for 18% of the total population, with 164.5 million individuals aged 65 years in 2019, and the number of older adults is projected to double by 2050 (21). Therefore, it is crucial to conduct the intervention of value among the Chinese population and explore whether the data differ from that of American and European countries. In this study, we aimed to confirm whether multicomponent exercise following vivifrail recommendations was an effective method for improving physical ability, cognitive function, gait, balance, and muscle strength in Chinese older adults. We hypothesized multicomponent exercise among Chinese older adults is a valid method to improve physical function.
Methods
Study Design and Study Participants
This is a prospective multicenter randomized controlled trial (RCT) to identify functional decline and explore the effectiveness of the intervention at an early stage, facilitate unified management, and improve the quality control level. Six nursing homes were selected in the Nanjing area, Jiangsu, China. This clinical trial was planned from 2018 to 2022, and we screened 302 participants from April 2021 to April 2022. All eligible older adults were randomly assigned to a control group (usual care plus health education) or exercise group (usual care plus health education plus exercise). Scientific exercise mainly including exercise style, time, and exercise security. Exercise training were consistent with stretch, aerobic, progressive resistance, and balance exercises. Training intensity starts at low intensity and gradually increases to appropriate intensity gradually. Appropriate intensity and time focus on personal situations where participants feel comfortable and can talk freely. During the research period, at least one experienced medical staff member accompanied the individual to ensure exercise security and effectiveness. In the study, we used stratified randomization, and stratified factors were the research center. The detailed operation methods were as follows: Qualified individuals were screened; subsequently, researchers obtained information from randomized participants through the central Randomization system (IWRS). Randomization sequences were generated using the IWRS system (http://58.213.51.73:9080/newHTEDC/). Before randomization, all individuals underwent face-to-face communication and answered related questions. Finally, 104 older adults were enrolled in this study. There was no financial compensation. This intervention lasted for 12 weeks, and all participants were assessed at three time points (baseline, 6 weeks, and 12 weeks). Further details are showed in Supplementary Document 1. All participants provided written informed consent, and the clinical protocol was reviewed and approved by the ethics committees of NJMU; the ethical number was 2020-SR-72. This clinical trial was registered (https://www.clinicaltrials.gov) with the trial number, ChiCTR2000040328.
Eligibility Criteria
The inclusion criteria were as follows: 1) adults aged 65 years or older, regardless of sex; 2) Barthel index ≥60 points; 3) maintained a stable health condition without severe dementia; 4) the participants could be followed up more than 12 weeks. Participants who presented worsening of some condition, with need for hospitalization or those people whose compliance was poor and could not continue to cooperate with the implementation of intervention measures through communication were excluded from the study.
Intervention Program
Health Education
Health education was conducted twice a month, each session lasting 30–50 min. The contents focused on a healthy diet, scientific exercise, and the related importance and were introduced by professional physical therapists and nutritionists.
Exercise Intervention
The exercise intervention was performed based on the 2020 International Exercise Recommendations in Older Adults and vivifrail multicomponent intervention (22, 23). The exercise group performed multicomponent exercises as follows: low intensity (50%–65% HRmax) exercise time controlled 30–40 min, and medium intensity (65%–75% HRmax) recommended 20–30 min. Experimental group comprised the following four parts: 1) warm-up (5–10 min), slow running or stretching were chosen; 2) aerobic exercise (20–40 min), including walking outdoors, biking, or hydrotherapy; 3) progressive resistance session, starting at 30% of one repetition maximum, with 10–12 per groups and 3–5 groups per day; and 4) balance exercise, involving remaining in the same position and persisting 30 seconds, repeated 3–5 times, such as standing on double, front, and back feet and other Chinese traditional activities, including Taichi, Baduanjin.
Measures
Demographic data, clinical diagnoses, and medication history were collected. The physical performance was assessed using Short Physical Performance Battery (SPPB) scale, 4-meter gait speed test (4MGS), and 6-min walking distance (6MWD). SPPB, 4MGS, and 6MWD have been described in previous studies (23, 24). Hand grip strength (HGS) was measured for both the dominant and non-dominant hand (25). Functional capacity and social activities were evaluated using the instrumental activities of daily living (IADL) and activities of daily living (ADL) (26, 27); quality of life and emotional health were assessed using the 12-item Short Form Survey (SF-12) and Geriatric Depression Scale-15 (GDS-15) (28, 29); Nutritional status was assessed using the short form Mini Nutritional Assessment (MNA-SF) (30). The balanced state was estimated using Tinetti score and cognitive function was calculated using the Mini-Mental State Examination (MMSE) (31, 32). All scales and data were recorded using the designed APP (2021SR0437260) and assessed at baseline, 6 weeks, and 12 weeks. Additionally, body composition was measured using multifrequency bioelectrical impedance analysis (MF-BIA) (InBodyS10, Biospace, Korea).
Outcomes
The primary outcomes were the changes in SPPB and ADL from baseline to 12 weeks (24). The meaningful clinical change was defined as an increase of 1 point for the SPPB or 5 points for the ADL. The secondary outcomes included IADL, Tinetti scores, Frailty score, MNA-SF, MMSE, GDS-15, SF-12, 4MGS, 6MWD, HGS, and body composition.
Sample Size Calculations
Combined with the previous study, SPPB was regarded as the primary evidence (18). Participants in the exercise and control groups were matched at 1:1.5. Assuming an alpha error of α=5%, a correlation between pre-and post-intervention values of SPPB of ρ=0.5, and a standard deviation for SPPB of σ=1.5, the required sample size to achieve a power of 80% to detect a minimum difference of 1 point between groups in the post-pre SPPB score.
The sample size was calculated using PASS15.0.5, and 56 and 37 individuals were estimated in the control and exercise groups, respectively; overall, 93 people needed to be randomized for the efficacy analysis. Eventually, we included 104 individuals (64 and 40 people in control and exercise groups, respectively) in this clinical trial.
Statistics
First, we checked the distribution of quantitative data was normal or abnormal using Shapiro-Wilk test. Continuous univariate of the normal distribution is expressed as mean ± standard deviation (SD) while abnormal distribution is expressed as a median (quartile). Categorical variables are presented as frequency (percentage, %). The comparison between two groups (experiment and control groups) were performed using two-independent sample t-test or the MannWhitney test for continuous variables; the Chi-square (χ2) test or Fisher’s exact test for categorical variables. In addition, this research performed paired sample t test or Wilcoxon signed rank test to examine whether there is a statistically significant difference in a group of participants before and after the experiment. Besides, Analysis of Variance (ANOVA) of repeated measurement data or Generalized Estimating Equations (GEE) analysis has been carried out to test the difference between groups with the influence of clinic intervention and the time.
All statistical analyses were performed using SPSS 23.0, and P< 0.05 was considered statistically signifcant.
Results
Baseline Characteristics
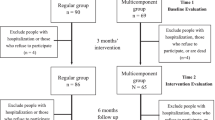
Figure 1 shows the study flow diagram. Overall, 302 eligible older adults were screened. Among them, 104 were enrolled and randomly assigned to control (n = 64) or exercise group (n = 40). Table 1 describes total population characteristics. No statistical difference was found in the baseline regarding physical ability, cognitive function, grip strength, balance, gait, quality of life, and nutritional status; these results are presented in Table 2. The average age in total population was 85 (82, 88) years; among them, control group was 86 (83, 89) years, exercise group was 83 (80, 87) years, and 59 (56.7%) participants were female. During the study, seven people in all groups were eliminated. Therefore, the control and exercise groups included 60 and 37 individuals, respectively. Finally, 69 individuals completed all assessments. Attendance rates were 31 (78%) and 38 (60%) for the exercise and control groups, respectively.
Primary Outcomes
After 12 weeks of intervention, the exercise group showed a significant improvement in SPPB, with a change of 2(0, 3.5) (P< 0.001), when compared to the usual care. In contrast, SPPB remained stable in the control group, the average change was 0(0–6) (P= 0.569) (Table 2). The detailed distribution of SPPB is presented in Figure 2. The subgroup analysis of SPPB was used to assess the efficiency of this clinical trial; we discovered that despite low(0–6 points), intermediate (7–9 points), or high (10–12 points) SPPB, differences between groups at 12 weeks were significant at post-intervention at 12 weeks (P= 0.001) (Supplementary Table 1). Similar tendencies were observed with ADL (Table 2, Supplementary Table 2). Overall, we believed that multicomponent exercise was an effective method of reversing the functional decline in older adults.
Secondary Outcomes
Cognitive Function, Grip Strength, Balance, Gait, and Quality of Life
Regarding the secondary outcomes, exercise intervention was likely to be valid in enhancing the 4MGS after 12 weeks; the exercise group had an average time of 4 seconds (95% CI [3,6], P= 0.001) compared with the control group, and the time remained stable; additionally, the control group average increased 3 seconds (95% CI [3, 6.2], P= 0.005). Tinetti score increased by 1.3 points (95% CI [0, 4.5], P< 0.001) in the exercise group, with a relative increase of 5% after 12 weeks; the non-exercise group declined slightly or remained stable compared with the baseline (6 weeks, −2 (−5,1), P= 0.119; 12 weeks, 0 (−3,1), P< 0.001) (Tables 2 and 3). Similarly, 6MWD was a positive result for support exercise intervention; 12 weeks follow-up showed 299.1±120.2 m and 184.2±101.7 m for the experimental and control groups, respectively. The difference between groups was significant. However, grip strength, MMSE, and GDS-15 did not change between groups (Table 2).
Change in Body Composition
Table 3 presents the difference between groups regarding body composition after 12 weeks. Although no significant differences were found in parameters between groups, some indicators involved muscle strength still improved after exercise when compared to their baseline measurements. Leg muscle mass improved in the post-exercise (13.7–14.8 kg), with a change of 0.7 (−0.1, 2.4) kg (P< 0.001); leg muscle mass remained constant in the control group (14.5–15.3 kg), with a change of 0.2 (−0.6, 1.0) kg (P= 0.337). Similar results were found in Appendicular skeletal muscle mass, soft lean mass and fat-free mass. Fat mass, arm circumference, arm muscle circumference, waist circumference, and visceral fat area decreased in the exercise group. The analysis was objective and further confirmed that exercise could improve muscle mass for older adults. More analysis results were attached in Supplementary Document 2.
Adverse Events
Supplementary Table 3 recorded the intervention-related adverse events. Adverse events were defined as falls, infections, hospitalization, and death during the study period. The total number of adverse events was three in the control group (one person fell, one was hospitalized, and one died). The exercise group had three adverse events (one person fell, and two were hospitalized). No obvious difference existed between the two groups. The result indicated that exercise among older adults might be a safe way according to the 12 weeks follow-up.
Discussion
The MIFDCE trial describes that an older adults consensusbased multicomponent intervention with low-medium intensity could provide a significant benefit during a short time, which could reverse older adults’ functional decline, keep a good balance and enhance muscle strength. Overall, we extend new evidence of multicomponent exercise intervention on functional decline in Chinese older adults.
Few RCTs have assessed the effects of exercise intervention on functional outcomes in older adults. Vivifrail was one of the positive programs that classified elderly individuals into different function statuses using SPPB; it found that 3-month personalized training could decrease the risk of falls and improve cognitive function, muscle function, and depression (18). Jay et al demonstrated that a multicomponent home-based physical therapy intervention did not result in a statistically significant improvement in walk distance after a 16-week intervention by recruiting elderly adults with hip fractures (33). Martínez-Velilla et al showed that a 5-day multicomponent exercise intervention was safe and effective in reversing the functional decline associated with acute hospitalization in very older patients (24). Recently, evidence has demonstrated that a 12-week multicomponent exercise program can improve frailty among community-dwelling Chinese older adults (34). In contrast to previous studies, we discovered a significant improvement between groups in physical status, balance, frailty, gait velocity, and quality of life. Similar falls outcome, MMSE, and body composition were found between groups. The explanation may result from the heterogeneity of response and the difference between the inclusion group.
As for body composition measurements, we choose using MF-BIA, because of its convenience and acceptance. Our research suggested that 12-week multicomponent exercises between older adults could benefit in muscle mass, such as improvement in soft lean mass, fat-free mass, skeletal muscle index, fat-free mass index, leg muscle mass, and lean body mass. In addition, bone mineral content raised and visceral fat area reduced in the exercise program. These result indicated multicomponent exercise in short time is a promising strategy to preserve physical function. However, future studies are warranted to demonstrate its long term effects among Chinese older adults, such as prevention and treatment of disability, sarcopenia, gait instability, and falls.
To identify functional decline and explore the effectiveness of the intervention at an early stage, facilitate unified management, and improve the quality control level, the nursing home was our first consideration. However, additional occasions, such as home, hospital, and community-dwelling, should still emphasize and explore the information related to elderly adults. The intervention benefit was not obvious at 6 weeks and became apparent at 12 weeks, indicating that a longer follow-up period is required.
The strengths of this study are as follows: first, application exercise intervention individually - generally, the training time, style, and frequency were based on older adults’ status. Rehabilitation by biking or walking was common practice; when older adults were trained, one or two nursing staff and a physical therapist would supervise, instruct, and ensure the appropriate exercise intensity. Meanwhile, medical professionals in the geriatrics department regularly instructed participants to recognize potential risks. In addition, the assessment tool was designed specially to collect data during different times, and it is convenient to deal with data and reduce errors. The evaluator was blinded to the group allocation, and it could reduce the bias of evaluation results to some extent.
Our study had some limitations. First, many occasions were strictly prohibited because of the COVID-19 outbreak, and unpredictable individuals were excluded from the research period. To some extent, it was limited to enrolling more individuals. Second, the included individuals lived in the same circumstance; people who were categorized into the control group can exercise based on the circumstance effect. Third, even though we arranged all participants with similar clothes and evaluated timepoint, season changes inevitably influenced the analysis of body composition, such as weight and body mass index.
Conclusions
The multicomponent exercise intervention following vivifrail recommendations is an effective method for older adults with functional decline, as it can reverse the functional decline and improve gait, balance, and muscle strength. Additionally, it widens vivifrail research and provides some guidance for Chinese medical professionals working in the field of geriatrics; 12-week multicomponent exercise between all population might be a promising method to improve physical function.
References
Gore PG, Kingston A, Johnson GR, Kirkwood TBL, Jagger C. New horizons in the compression of functional decline. Age Ageing 2018;47:764–768. doi:https://doi.org/10.1093/ageing/afy145.
Braes T, Flamaing J, Sterckx W et al. Predicting the risk of functional decline in older patients admitted to the hospital: a comparison of three screening instruments. Age Ageing 2009;38:600–603. doi:https://doi.org/10.1093/ageing/afp097.
Peron EP, Gray SL, Hanlon JT. Medication use and functional status decline in older adults: a narrative review. Am J Geriatr Pharmacother 2011;9:378–91. doi:https://doi.org/10.1016/j.amjopharm.2011.10.002.
Beaton K, Grimmer K. Tools that assess functional decline: systematic literature review update. Clin Interv Aging 2013:485. doi:https://doi.org/10.2147/CIA.S42528.
Kahraman T, çekok FK, üğǼt BO, Keskinoğlu P, Genç A. One-Year Change in the Physical Functioning of Older People According to the International Classification of Functioning Domains. J Geriatr Phys Ther 2021;44:E9–E17. doi:https://doi.org/10.1519/JPT.0000000000000234.
Stathi A, Greaves CJ, Thompson JL et al. Effect of a physical activity and behaviour maintenance programme on functional mobility decline in older adults: the REACT (Retirement in Action) randomised controlled trial. Lancet Public Health 2022;7:e316–e326. doi:https://doi.org/10.1016/S2468-2667(22)00004-4.
Guralnik JM, Branch LG, Cummings SR, Curb JD. Physical performance measures in aging research. J Gerontol 1989;44:M141. doi:https://doi.org/10.1093/geronj/44.5.M141.
Izquierdo M, Merchant RA, Morley JE et al. International Exercise Recommendations in Older Adults (ICFSR): Expert Consensus Guidelines. J Nutr Health Aging 2021;25:824–853. doi:https://doi.org/10.1007/s12603-021-1665-8.
Unger JB, Johnson CA, Marks G. Functional decline in the elderly: evidence for direct and stress-buffering protective effects of social interactions and physical activity. Ann Behav Med 1997;19:152–60. doi:https://doi.org/10.1007/BF02883332.
Guralnik JM, Ferrucci L, Simonsick EM, Salive ME, Wallace RB. Lower-extremity function in persons over the age of 70 years as a predictor of subsequent disability. N Engl J Med 1995;332:556–61. doi:https://doi.org/10.1056/NEJM199503023320902.
Luo Y, Su B, Zheng X et al. Trends and Challenges for Population and Health During Population Aging — China, 2015–2050. China CDC Weekly 2021;3:593–598. doi:https://doi.org/10.46234/ccdcw2021.158.
Lavie CJ, Arena R, Swift DL et al. Exercise and the Cardiovascular System. Circ Res 2015;117:207–219. doi:https://doi.org/10.1161/CIRCRESAHA.117.305205.
Villareal DT, Aguirre L, Gurney AB et al. Aerobic or Resistance Exercise, or Both, in Dieting Obese Older Adults. N Engl J Med 2017;376:1943–1955. doi:https://doi.org/10.1056/NEJMoa1616338.
Karssemeijer E, Aaronson JA, Bossers WJ, Smits T, Olde RM, Kessels R. Positive effects of combined cognitive and physical exercise training on cognitive function in older adults with mild cognitive impairment or dementia: A meta-analysis. Ageing Res Rev 2017;40:75–83. doi:https://doi.org/10.1016/j.arr.2017.09.003.
Angulo J, El AM, Alvarez-Bustos A, Rodriguez-Manas L. Physical activity and exercise: Strategies to manage frailty. Redox Biol 2020;35:101513. doi:https://doi.org/10.1016/j.redox.2020.101513.
Ortega FB, Mora-Gonzalez J, Cadenas-Sanchez C et al. Effects of an Exercise Program on Brain Health Outcomes for Children With Overweight or Obesity: The ActiveBrains Randomized Clinical Trial. JAMA Netw Open 2022;5:e2227893. doi:https://doi.org/10.1001/jamanetworkopen.2022.27893.
Cadore EL, Rodríguez-Mañas L, Sinclair A, Izquierdo M. Effects of Different Exercise Interventions on Risk of Falls, Gait Ability, and Balance in Physically Frail Older Adults: A Systematic Review. Rejuvenation Res 2013;16:105–114. doi:https://doi.org/10.1089/rej.2012.1397.
Casas Herrero Á, Sáez De Asteasu ML, Antón Rodrigo I et al. Effects of Vivifrail multicomponent intervention on functional capacity: a multicentre, randomized controlled trial. J Cachexia Sarcopenia Muscle 2022;13:884–893. doi:https://doi.org/10.1002/jcsm.12925.
Tarazona-Santabalbina FJ, Gómez-Cabrera MC, Pérez-Ros P et al. A Multicomponent Exercise Intervention that Reverses Frailty and Improves Cognition, Emotion, and Social Networking in the Community-Dwelling Frail Elderly: A Randomized Clinical Trial. J Am Med Dir Assoc 2016;17:426–433. doi:https://doi.org/10.1016/j.jamda.2016.01.019.
Buto MSS, Fiogbé E, Vassimon Barroso V et al. Pre-Frail Multicomponent Training Intervention project for complexity of biological signals, functional capacity and cognition improvement in pre-frail older adults: A blinded randomized controlled study protocol. Geriatr Gerontol Int 2019;19:684–689. doi:https://doi.org/10.1111/ggi.13672.
Fang EF, Xie C, Schenkel JA et al. A research agenda for ageing in China in the 21st century (2nd edition): Focusing on basic and translational research, long-term care, policy and social networks. Ageing Res Rev 2020;64:101174. doi:https://doi.org/10.1016/j.arr.2020.101174.
Bull FC, Al-Ansari SS, Biddle S et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br J Sports Med 2020;54:1451–1462. doi:https://doi.org/10.1136/bjsports-2020-102955.
Casas-Herrero A, Anton-Rodrigo I, Zambom-Ferraresi F et al. Effect of a multicomponent exercise programme (VIVIFRAIL) on functional capacity in frail community elders with cognitive decline: study protocol for a randomized multicentre control trial. Trials 2019;20:362–374. doi:https://doi.org/10.1186/s13063-019-3426-0.
Martínez-Velilla N, Casas-Herrero A, Zambom-Ferraresi F et al. Effect of Exercise Intervention on Functional Decline in Very Elderly Patients During Acute Hospitalization. Jama Intern Med 2019;179:28–36. doi:https://doi.org/10.1001/jamainternmed.2018.4869.
Reijnierse EM, de Jong N, Trappenburg MC et al. Assessment of maximal handgrip strength: how many attempts are needed? J Cachexia Sarcopenia Muscle 2017;8:466–474. doi:https://doi.org/10.1002/jcsm.12181.
Mahoney FI, Barthel DW. Functional evaluation: the Barthel Index. Md State Med J 1965;14:56–61.
Katz S. Assessing Self-maintenance: Activities of Daily Living, Mobility, and Instrumental Activities of Daily Living. J Am Geriatr Soc 1983;31:721–727. doi:https://doi.org/10.1111/j.1532-5415.1983.tb03391.x.
Jakobsson U. Using the 12-item Short Form health survey (SF-12) to measure quality of life among older people. Aging Clin Exp Res 2007;19:457–464. doi:https://doi.org/10.1007/BF03324731.
D’Ath P, Katona P, Mullan E, Evans S, Katona C. Screening, Detection and Management of Depression in Elderly Primary Care Attenders. I: The Acceptability and Performance of the 15 Item Geriatric Depression Scale (GDS15) and the Development of Short Versions. Fam Pract 1994;11:260–266. doi:https://doi.org/10.1093/fampra/11.3.260.
Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B. Screening for undernutrition in geriatric practice: developing the short-form mini-nutritional assessment (MNASF). J Gerontol A Biol Sci Med Sci 2001;56:M366–72. doi:https://doi.org/10.1093/gerona/56.6.m366.
Raîche M, Hébert R, Prince F, Corriveau H. Screening older adults at risk of falling with the Tinetti balance scale. Lancet 2000;356:1001–1002. doi:https://doi.org/10.1016/S0140-6736(00)02695-7.
Crum RM, Anthony JC, Bassett SS, Folstein MF. Population-based norms for the Mini-Mental State Examination by age and educational level. JAMA 1993;269:2386–91. doi:https://doi.org/10.1001/jama.1993.03500180078038.
Magaziner J, Mangione KK, Orwig D et al. Effect of a Multicomponent Home-Based Physical Therapy Intervention on Ambulation After Hip Fracture in Older Adults. JAMA 2019;322:946–956. doi:https://doi.org/10.1001/jama.2019.12964.
Dun Y, Hu P, Ripley-Gonzalez JW et al. Effectiveness of a multicomponent exercise program to reverse pre-frailty in community-dwelling Chinese older adults: a randomised controlled trial. Age Ageing 2022;51:afac026. doi:https://doi.org/10.1093/ageing/afac026.
Acknowledgments
The authors would like to thank the external reviewers for their work on the literature. We are grateful to the study participants for their consent to participate. We thank all the other physicians and nursing staff at the six nursing homes for their support during the study. We would like to thank Editage (www.editage.cn) for English language editing.
Funding
Funding: This study was supported by the National Key Research and Development Program of China (grant number 2018YFC2002100, and 2018YFC2002102), the Jiangsu Province Capability Improvement Project through Science, Technology and Education (grant number CXZX202228), the National Natural Science Foundation of China (grant number 81871115, and 82171516), the Natural Science Foundation of Jiangsu Province (grant number BK20211377), the Cadre Health Care Research Project of Jiangsu Province (grant number BJ20018), the Natural science research project of colleges and universities in Jiangsu Province (grant number 20KJB320002); and the Outstanding Young and Middle-aged Talents Support Program of the First Affiliated Hospital with Nanjing Medical University, the Six Talent Peaks Project in Jiangsu Province. Sponsors played no role in the undertaking of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest: None declared.
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Chen, B., Li, M., Zhao, H. et al. Effect of Multicomponent Intervention on Functional Decline in Chinese Older Adults: A Multicenter Randomized Clinical Trial. J Nutr Health Aging 27, 1063–1075 (2023). https://doi.org/10.1007/s12603-023-2031-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-023-2031-9