Abstract
Background
Proton-pump inhibitors (PPI) are extensively prescribed in older patients. However, little information is available on factors associated to PPI prescribing patterns among older patients discharged from hospital.
Objective
To evaluate the appropriateness and clinical correlates of PPI prescription at discharge in a population of 1081 older patients discharged from acute care Italian hospitals.
Design
We used data from the CRiteria to Assess Appropriate Medication Use among Elderly Complex Patients (CRIME) study, a multicenter observational study. The appropriateness of PPI prescriptions was defined according to the Italian Medicines Agency (AIFA) rules. Correlates of overprescribing (i.e prescribing without recognized AIFA indications) and underprescribing (i.e. not prescribing despite the presence of recognized AIFA indications) were investigated by logistic regression analysis.
Results
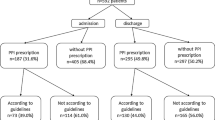
Overprescribing was observed in 30% of patients receiving PPIs at discharge. Underprescribing was observed in 11% of patients not receiving PPIs at discharge. Overprescribing of PPIs at discharge was negatively associated with age (OR=0.88, 95%CI=0.85-0.91), depression (OR=0.58, 95%CI=0.35-0.96), use of aspirin (OR=0.03, 95%CI=0.02-0.06) and systemic corticosteroids (OR=0.02, 95%CI=0.01-0.04). The negative association with number of medications (OR=0.95, 95%CI=0.88-1.03) and overall comorbidities (OR=0.92, 95%CI=0.83-1.02) was nearly significant. Conversely, older age (OR=1.09, 95%CI=1.04-1.14), use of aspirin (OR=24.0, 95%CI=11.5-49.8) and systemic corticosteroids (OR=19.3, 95%CI=11.5-49.8) and overall comorbidities (OR=1.22, 95%CI=1.04-1.42) were independent correlates of underprescribing.
Conclusion
Overprescribing of PPIs is more frequent in younger patients with lower burden of depression, whilst underprescribing is characterized by older age and greater burden of comorbidity and polypharmacy. Hospitalization should be considered as a clue to identify inappropriate use of PPIs and improve appropriateness of prescribing.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Proton pump inhibitors (PPIs) are widely prescribed to suppress gastric acid secretion in gastrointestinal disorders, including gastroesophageal reflux disease (GERD), peptic ulcer disease and upper gastrointestinal bleeding (1-3). In recent years, there has been a significant rise in the prescriptions for PPIs, especially in older populations (1), making these agents one of the most prescribed drugs worldwide (4, 5). Recent studies raised concerns about the potential risks associated with prolonged and potentially non-judicious use of PPIs, including mortality (6-8), functional decline (9), Clostridium difficile infections (10), fractures (11), cardiovascular events (12). Additionally, since PPIs are mainly metabolized by the cytochrome P450 system, interactions with other drugs also represent a relevant concern (13).
PPIs are often prescribed without a clear indication (14), thus contributing to increased expenditure for inappropriately prescribed medications (15). Nevertheless, only few studies have investigated the clinical correlates of inappropriate prescribing of PPIs in older population (16, 17). A better knowledge regarding additional PPI use is of paramount importance to identify effective strategies aimed at improving the quality of prescriptions. Therefore, the aim of the present study is to identify the clinical correlates of PPIs prescription and to evaluate the appropriateness of such prescriptions among older patients discharged from acute care hospitals in a large multicenter observational study.
Methods
Patients
This study uses data from the CRiteria to Assess Appropriate Medication Use among Elderly Complex Patients (CRIME) project, a multicenter prospective observational study aimed at collecting data about the patterns and quality of prescriptions among older patients admitted to seven geriatric and internal medicine acute care wards throughout Italy. The methods of the CRIME study have been extensively described elsewhere (18). Briefly, all patients consecutively admitted to participating wards between June 2010 and May 2011, were asked to participate in the study. Exclusion criteria included age<65 years and unwillingness to participate in the study. After obtaining a written informed consent, all participants were assessed within the first 24 hours from hospital admission and followed until discharge. Information was collected on demographic, socioeconomic, and clinical characteristics, with detailed data collection on pharmacological therapy and comprehensive geriatric assessment. After discharge, patients were reassessed at 3, 6, and 12 months. All Ethics Committees at participating institutions approved the study protocol.
This present study uses data collected during the hospitalization (time from hospital admission to discharge). Overall, 1123 patients were enrolled in the CRIME study. Patients who died during hospital stay (n=42, 3.7%) were excluded from this analysis, thus 1081 patients were included in this report.
Outcome
Drugs were coded using the Anatomical and Therapeutic Classification (ATC) (19). Participants taking PPIs at discharge were identified according to ATC code A02BC.
The appropriateness of the prescription of PPIs at discharge was evaluated according to indications released by the Italian Medicines Agency (AIFA) (20). Treatment with PPI was deemed appropriate in: i) patients on chronic treatment with systemic corticosteroids or low-dose ASA when one or more of the following risk factors is present: a. history of gastrointestinal bleeding or ulceration, b. treatment with anticoagulants or corticosteroids, c. age ≥75 years; ii) patients with peptic ulcer or GERD.
An analytical variable was created to compare patients receiving appropriate prescription of PPIs to those receiving PPIs without fulfilling any AIFA indications (overprescribing group). Similarly, we compared characteristics of patients fulfilling AIFA indications but not receiving PPIs (underprescribing group) with patients appropriately not receiving PPIs at discharge.
Variables
Variables included in the analysis were age, gender, cognitive impairment (age- and education-adjusted Mini Mental State Examination, MMSE score<24) (21), depression (Geriatric Depression Scale, GDS score>5) (22), dependency in basic activities of daily living (BADL) (23) , alcohol consumption(>2 wine glasses/day), nutritional status (Body Mass Index, BMI<20 kg/m2, serum albumin<3.5 g/dl), number of drugs prescribed at discharge with the exclusion of PPIs, and history of adverse drug reaction (ADR) during hospital stay. Use of PPIs before hospital admission was considered as a potential confounder. Drugs potentially affecting the prescription of PPIs (i.e. aspirin and other antiplatelet agents, anticoagulants, NSAIDs, and systemic steroids) were also considered in the analysis. Selected conditions were considered as potential confounders, including: i) indications to the use of antiplatelet drugs (cardio- and cerebro-vascular diseases, peripheral artery disease, heart failure and diabetes mellitus) (24); ii) diseases for which the risk is increased by PPIs (infections and osteoporosis) (10, 25, 26); iii) potential side effects of PPIs (diarrhea and constipation). Anemia was defined as haemoglobin<1 g/dl for males and <12 g/dl for females, and was also considered among potential confounders. Finally, the overall number of comorbidities was calculated by excluding peptic ulcer (with or without haemorrhage) and GERD and included in the analysis.
Analytic approach
Patients were initially grouped on the basis of receiving or not receiving a prescription of PPIs at discharge. Therefore, patients receiving overprescribed PPIs at discharge were compared to patients receiving appropriate prescription of PPIs with regard to study variables. Similarly, patients in the underprescribing group were compared to those in which PPIs were appropriately not prescribed. The chi-square test or one way analysis of variance was used when appropriate.
Variables significantly distinguishing groups in preliminary analysis were entered into separate logistic regression models to investigate independent correlates of overprescription and underprescription at discharge. All analyses were performed using SPSS V10.0 Statistical Software Package for Windows.
Results
Participants included in the analysis had mean age of 81.2±7.4 years and 604 (55.9%) were women.
At discharge, overprescribed PPI patients were younger, had a lower number of comorbidities and were taking a lower number of drugs at discharge, including aspirin and systemic corticosteroids, when compared to patients with an appropriate PPI prescription.
In regards to comorbidities, overprescribed patients had a lower prevalence of depression, coronary artery disease, heart failure, and constipation (Table 1).
At discharge, underprescribed PPI patients, were older, had a significantly greater number of comorbidities, and were more frequently prescribed aspirin and systemic corticosteroids, received a greater number of drugs. In regards to specific comorbidities, these patients had a greater prevalence of peripheral artery disease and constipation compared to appropriately not prescribed patients. In addition, there was a greater prevalence of PPI use at the time of admission in the underprescribed PPI group compared to patients for which PPIs were appropriately not prescribed (Table 1).
After adjusting for potential confounders, the overprescription of PPIs at discharge was negatively associated with age, depression, use of aspirin and systemic corticosteroids. The negative association with number of medications and overall comorbidities was nearly significant (Table 2). After excluding the use of aspirin and systemic steroids from the multivariable model, age (OR=0.94, 95%CI=0.92-0.96), depression (OR=0.66, 95%CI=0.45-0.97), and number of medications (OR=0.89, 95%CI=0.83-0.95) were significantly associated with overprescribing. Conversely, older age, use of aspirin, systemic corticosteroids and overall comorbidities were independent correlates of underprescription of PPI (Table 2). After excluding the use of aspirin and systemic steroids from the model, age (OR=1.09, 95%CI=1.05- 1.14) and number of medications (OR=1.21, 95%CI=1.09-1.33) qualified as significant correlates of undeprescribing, while the association with overall comorbidity (OR=1.16, 95%CI=0.99- 1.30) was nearly significant.
Discussion
This report confirms that overprescribing of PPIs is frequent among patients discharged from hospital. Though less frequent, underprescribing at discharge can be observed in a not negligible proportion of patients. The overprescribing of PPIs has been previously reported and has been shown to range between 27% and 71% (16, 27, 28). More recently, an overprescribing of PPIs was found in 80% of 2686 patients discharged with a PPI prescription over a 4-year period (29). On the other hand, the few studies investigating the underprescribing of PPIs at discharge showed a prevalence ranging between 28% and 60% (30, 31).
Compared to previous studies, we found that overprescribing was inversely associated with age, depression, number of diagnoses, aspirin, systemic steroids and the number of drugs prescribed at discharge. Ahrens et al. (32) demonstrated that the use of PPI before hospital admission was an independent determinant of overprescribing in multivariable analysis, as well as low dose aspirin, older age and hospitalization in a regional care center. Jarchow-MacDonald et al (17) found that institutionalization, polypharmacy and overall comorbidity were significantly associated with overprescribing of PPIs during hospitalization. A possible explanation of this discrepancy may be related to increasing use of ulcer prophylaxis, even for low-risk patients, especially in the presence of selected clinical conditions (i.e. heart diseases, acute renal failure) which are perceived as risk factors despite their lack of evidence (33). However, it is important to recall that long-term use of PPIs has been associated with several negative outcomes. For example, the use of PPIs was found to be associated with functional decline (1, 34) and mortality (8) among older patients discharged from hospital. PPIs are known to increase the risk of cardiovascular events (35) and infections (10, 25). Long-term use of PPIs is also associated with a reduced absorption of calcium, vitamin B12, iron, and magnesium (36). Additionally, use of PPIs was found associated with lower insulin-like growth factor-1 (IGF-1), suggesting a potential mechanism by which PPIs may exert negative effects of nutritional status and adverse outcomes among older people (37). Osteoporotic fractures have been reported as potential negative effects of PPIs (26). Finally, since PPIs are mainly metabolized by the cytochrome P450 system, interactions with other drugs using this system are expected (13). The above evidence, together with our results, raises the need to make further efforts to identify specific appropriateness for PPI prescriptions, especially in older patients vulnerable to negative outcomes. Considering that hospitalization for an acute event may create a potential basis for drug treatment strategies, studies are needed to show specific indications (as from guidelines), for the appropriate use of PPI prescribing at discharge.
Interestingly, we found that an underprescription of PPI was associated with older age, use of aspirin and systemic steroids, and overall comorbidity. Although comorbidity is widely correlated with polypharmacy, our results are in accordance with a previous study report by McDonald et al. (17) showing that the number of drugs was a risk factor for underprescription. Additionally, advanced age may be a risk factor that is considered negligible at the time of discharge in patients receiving no prophylaxis compared to patients receiving antiplatelet therapy (38). Current evidence suggests that polypharmacy and older age should not discourage from prescribing PPIs when there is a clear clinical indication. Indeed, the extensive use of gastroprotective agents can substantially reduce the morbidity and mortality associated with long-term NSAID and aspirin use (39), especially in older patients (40). Recent cohort studies in France (41) and Japan (42) have demonstrated significant reductions in upper gastrointestinal bleeding through appropriate prescribing of PPIs. Our findings suggest that a treatment-risk paradox (i.e. treatment selection bias in which high-risk patients are less likely to receive therapy than low-risk ones) might affect PPI prescribing. Since the absolute benefits of PPI treatment are substantially necessary in patients with a high risk profile, physicians should be aware of such paradox in order to avoid negative clinical outcomes. Additionally, this paradox is an important confounder and needs to be recognized when drawing conclusions about treatment effects on the basis of associations between treatment exposure and outcomes (43).
Our study design includes some limitations. This study was only performed in geriatric and internal medicine units, which might result in an under-representation of selected indications for the use of PPIs (e.g. peptic ulcer). Additionally, the cross-sectional design does not allow to capture information regarding the duration of PPI use. Finally, factors related to the organization of participating wards, as well as internal policies of participating hospitals might influence the use of PPIs.
However, our study protocol holds a multicenter design and the population enrolled did not have stringent inclusion/exclusion criteria to allow for a greater awareness of appropriateness of PPI prescribing in a general population of older patients.
Conclusion
In conclusion, our study indicates that overprescribing and, to a lesser extent, underprescribing of PPIs are frequent among patients discharged from hospital. Accordingly, the hospital setting may improve the quality of PPI prescription only to some extent. Patients receiving PPIs without any recognized indication at discharge are younger with less comorbidities compared to those receiving appropriate PPI prescriptions. Given the potential for associated negative consequences, individuals not meeting prescribing indications would create a basis for future trials investigating withdrawal of PPIs. On the contrary, underprescribed patients are characterized by a high-risk profile. Hospitalization provides an important opportunity to improve the quality of PPI prescriptions.
Ethical standards: The study was supported by the Italian Ministry of Health (grants n. GR-2007-685638 and RF-2009-1530442) and comply with the current laws in Italy.
Acknowledgments: The study group CRIME: (Gemelli Hospital, Center of Aging Medicine, Catholic University of the Sacred Heart, Rome, Italy; University of Perugia, University of Ferrara, Italian National Research Center on Aging - INRCA situated in Ancona, Cosenza, Stationary , and Rome)
Conflict of interest disclosure form: All authors declare to have no conflict of interest with this manuscript.
References
McCarthy DM. Adverse effects of proton pump inhibitor drugs: clues and conclusions. Curr Opin Gastroenterol. 2010 Nov;26:624–31.
Bhatt DL, Scheiman J, Abraham NS, Antman EM, Chan FK, Furberg CD, Johnson DA, Mahaffey KW, Quigley EM. ACCF/ACG/AHA 2008 expert consensus document on reducing the gastrointestinal risks of antiplatelet therapy and NSAID use: a report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents. Circulation. 2008 Oct 28;118:1894–909.
Pilotto A, Franceschi M, Leandro G, Scarcelli C, D’Ambrosio LP, Seripa D, Perri F, Niro V, Paris F, et al. Clinical features of reflux esophagitis in older people: a study of 840 consecutive patients. J Am Geriatr Soc. 2006 Oct;54:1537–42.
IMS Health Report: IMS National Prescription Audit. New Jersey: IMS; 2011. Available at http://www.imshealth.com/ims/Global/Content/Insights/IMS%20 Institute%20for%20Healthcare%20Informatics/IHII_Medicines_in_U.S_ Report_2011.pdf Last accessed June 13, 2013
L’uso dei farmaci in Italia-Rapporto OsMed. December 2012. Available at http://www.agenziafarmaco.gov.it/it/content/luso-dei-farmaci-italia-rapporto-osmedgennaio-settembre-2012. Last accessed June 13, 2013
Bell JS, Strandberg TE, Teramura-Gronblad M, Laurila JV, Tilvis RS, Pitkala KH. Use of proton pump inhibitors and mortality among institutionalized older people. Arch Intern Med. 2010 Sep 27;170:1604–5.
Teramura-Gronblad M, Bell JS, Poysti MM, Strandberg TE, Laurila JV, Tilvis RS, Soini H, Pitkala KH. Risk of death associated with use of PPIs in three cohorts of institutionalized older people in Finland. J Am Med Dir Assoc. 2012 Jun;13:488e9-13.
Maggio M, Corsonello A, Ceda GP, Cattabiani C, Lauretani F, Butto V, Ferrucci L, Bandinelli S, Abbatecola AM, et al. Proton pump inhibitors and risk of 1-year mortality and rehospitalization in older patients discharged from acute care hospitals. JAMA Intern Med. 2013 Apr 8;173:518–23.
Corsonello A, Maggio M, Fusco S, Adamo B, Amantea D, Pedone C, Garasto S, Ceda GP, Corica F, et al. Proton pump inhibitors and functional decline in older adults discharged from acute care hospitals. J Am Geriatr Soc. 2014 Jun;62:1110–5.
Linsky A, Gupta K, Lawler EV, Fonda JR, Hermos JA. Proton pump inhibitors and risk for recurrent Clostridium difficile infection. Arch Intern Med. 2010 May 10;170:772–8.
Yu EW, Bauer SS, Bain PA et al. Proton-pump inhibitor and risk of fractures: a metaanalysis of 11 international studies. Am J Med 2011; 124: 519–526
Charlot M, Grove EL, Hansen PR, Olesen JB, Ahlehoff O, Selmer C, Lindhardsen J, Madsen JK, Kober L, et al. Proton pump inhibitor use and risk of adverse cardiovascular events in aspirin treated patients with first time myocardial infarction: nationwide propensity score matched study. BMJ. 2011;342:d2690.
Shi S, Klotz U. Proton pump inhibitors: an update of their clinical use and pharmacokinetics. Eur J Clin Pharmacol. 2008 Oct;64:935–51.
Patterson Burdsall D, Flores HC, Krueger J, Garretson S, Gorbien MJ, Iacch A, Dobbs V, Homa T. Use of proton pump inhibitors with lack of diagnostic indications in 22 Midwestern US skilled nursing facilities. J Am Med Dir Assoc. 2013 Jun;14:429–32.
Godman B, Wettermark B, van Woerkom M, Fraeyman J, Alvarez-Madrazo S, Berg C, Bishop I, Bucsics A, Campbell S, et al. Multiple policies to enhance prescribing efficiency for established medicines in Europe with a particular focus on demandside measures: findings and future implications. Front Pharmacol. 2014;5:106.
Parente F, Cucino C, Gallus S, Bargiggia S, Greco S, Pastore L, Bianchi Porro G. Hospital use of acid-suppressive medications and its fall-out on prescribing in general practice: a 1-month survey. Aliment Pharmacol Ther. 2003 Jun 15;17:1503–6.
Jarchow-Macdonald AA, Mangoni AA. Prescribing patterns of proton pump inhibitors in older hospitalized patients in a Scottish health board. Geriatr Gerontol Int. 2013 Oct;13:1002–9.
Tosato M, Settanni S, Antocicco M, Battaglia M, Corsonello A, Ruggiero C, Volpato S, Fabbietti P, Lattanzio F, et al. Pattern of medication use among older inpatients in seven hospitals in Italy: results from the CRiteria to assess Appropriate Medication use among Elderly complex patients (CRIME) project. Curr Drug Saf. 2013 Apr;8:98–103.
Pahor M, Chrischilles EA, Guralnik JM, Brown SL, Wallace RB, Carbonin P. Drug data coding and analysis in epidemiologic studies. Eur J Epidemiol. 1994 Aug;10:405–11.
http://www.agenziafarmaco.gov.it/sites/default/files/Note_AIFA_testo_06-07.pdf
Folstein MF, Folstein SE, McHugh PR. «Mini-mental state». A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975 Nov;12:189–98.
Lesher EL, Berryhill JS. Validation of the Geriatric Depression Scale—Short Form among inpatients. J Clin Psychol. 1994 Mar;50:256–60.
Katz TF. A.D.L. Activities of Daily Living. JAMA 1963;185:914
Lai KC, Lam SK, Chu KM, Wong BC, Hui WM, Hu WH, Lau GK, Wong WM, Yuen MF, et al. Lansoprazole for the prevention of recurrences of ulcer complications from long-term low-dose aspirin use. N Engl J Med. 2002 Jun 27;346:2033–8.
Gulmez SE, Holm A, Frederiksen H, Jensen TG, Pedersen C, Hallas J. Use of proton pump inhibitors and the risk of community-acquired pneumonia: a population-based case-control study. Arch Intern Med. 2007 May 14;167:950–5.
Yang YX, Lewis JD, Epstein S, Metz DC. Long-term proton pump inhibitor therapy and risk of hip fracture. JAMA. 2006 Dec 27;296:2947–53.
Nardino RJ, Vender RJ, Herbert PN. Overuse of acid-suppressive therapy in hospitalized patients. Am J Gastroenterol. 2000 Nov;95:3118–22.
Gullotta R, Ferraris L, Cortelezzi C, Minoli G, Prada A, Comin U, Rocca F, Ferrara A, Curzio M. Are we correctly using the inhibitors of gastric acid secretion and cytoprotective drugs? Results of a multicentre study. Ital J Gastroenterol Hepatol. 1997 Aug;29:325–9.
Leri F, Ayzenberg M, Voyce SJ, Klein A, Hartz L, Smego RA, Jr. Four-year trends of inappropriate proton pump inhibitor use after hospital discharge. South Med J. 2013 Apr;106:270–3.
Tett SE, Sketris I, Cooke C, Veldhuyzen van Zanten S, BarozziN. Differences in utilisation of gastroprotective drugs between 2001 and 2005 in Australia and Nova Scotia, Canada. Pharmacoepidemiol Drug Saf 2013; 22: 735–743
Valkhoff VE, van Soest EM, Sturkenboom MC, Kuipers EJ. Time-trends in gastroprotection with nonsteroidal anti-inflammatory drugs (NSAIDs). Aliment Pharmacol Ther. 2010 Jun;31:1218–28.
Ahrens D, Behrens G, Himmel W, Kochen MM, Chenot JF. Appropriateness of proton pump inhibitor recommendations at hospital discharge and continuation in primary care. Int J Clin Pract. 2012 Aug;66:767–73.
Sheikh-Taha M, Alaeddine S, Nassif J. Use of acid suppressive therapy in hospitalized non-critically ill patients. World J Gastrointest Pharmacol Ther. 2012 Dec 6;3:93–6.
Sganga F, Vetrano DL, Volpato S, Cherubini A, Ruggiero C, Corsonello A, Fabbietti P, Lattanzio F, Bernabei R, Onder G. Physical performance measures and polypharmacy among hospitalized older adults: results from the CRIME study. J Nutr Health Aging. 2014;18:616–21.
Charlot M, Ahlehoff O, Norgaard ML, Jorgensen CH, Sorensen R, Abildstrom SZ, Hansen PR, Madsen JK, Kober L, et al. Proton-pump inhibitors are associated with increased cardiovascular risk independent of clopidogrel use: a nationwide cohort study. Ann Intern Med. 2010 Sep 21;153:378–86.
Ito T, Jensen RT. Association of long-term proton pump inhibitor therapy with bone fractures and effects on absorption of calcium, vitamin B12, iron, and magnesium. Curr Gastroenterol Rep. 2010 Dec;12:448–57.
Maggio M, Lauretani F, De Vita F, Butto V, Cattabiani C, Masoni S, Sutti E, Bondi G, Dall’aglio E, et al. Relationship between use of proton pump inhibitors and IGF system in older subjects. J Nutr Health Aging. 2014 Apr;18:420–3.
Morneau KM, Reaves AB, Martin JB, Oliphant CS. Analysis of gastrointestinal prophylaxis in patients receiving dual antiplatelet therapy with aspirin and clopidogrel. J Manag Care Pharm. 2014 Feb;20:187–93.
Rostom A, Dube C, Wells G, Tugwell P, Welch V, Jolicoeur E, McGowan J. Prevention of NSAID-induced gastroduodenal ulcers. Cochrane Database Syst Rev. 2002:CD002296.
Straube S, Tramer MR, Moore RA, Derry S, McQuay HJ. Mortality with upper gastrointestinal bleeding and perforation: effects of time and NSAID use. BMC Gastroenterol. 2009;9:41.
Laharie D, Droz-Perroteau C, Benichou J, Amouretti M, Blin P, Begaud B, Guiard E, Dutoit S, Lamarque S, et al. Hospitalizations for gastrointestinal and cardiovascular events in the CADEUS cohort of traditional or Coxib NSAID users. Br J Clin Pharmacol. 2010 Mar;69:295–302.
Miyamoto M, Haruma K, Okamoto T, Higashi Y, Hidaka T, Manabe N. Continuous proton pump inhibitor treatment decreases upper gastrointestinal bleeding and related death in rural area in Japan. J Gastroenterol Hepatol. 2012 Feb;27:372–7.
McAlister FA. The end of the risk-treatment paradox? A rising tide lifts all boats. J Am Coll Cardiol. 2011 Oct 18;58:1766–7.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schepisi, R., Fusco, S., Sganga, F. et al. Inappropriate use of proton pump inhibitors in elderly patients discharged from acute care hospitals. J Nutr Health Aging 20, 665–670 (2016). https://doi.org/10.1007/s12603-015-0642-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0642-5