Abstract
The effect of Lactobacillus rhamnosus CRL1505 (Lr) on macrophages (Ma) and dendritic cells (DC) in the orchestration of anti-pneumococcal immunity was studied using malnutrition and pneumococcal infection mouse models. Monocytes (Mo), Ma, and DC in two groups of malnourished mice fed with balanced diet (BCD) were studied through flow cytometry; one group was nasally administered with Lr (BCD+Lr group), and the other group was not (BCD group). Well-nourished (WNC) and malnourished (MNC) mice were used as controls.
Malnutrition affected the number of respiratory and splenic mononuclear phagocytes. The BCD+Lr treatment, unlike BCD, was able to increase and normalize lung Mo and Ma. The BCD+Lr mice were also able to upregulate the expression of the activation marker MHC II in lung DC and to improve this population showing a more significant effect on CD11b+ DC subpopulation. At post-infection, lung Mo values were higher in BCD+Lr mice than in BCD mice and similar to those obtained in WNC group. Although both repletion treatments showed similar values of lung Ma post-infection, the Ma activation state in BCD+Lr mice was higher than that in BCD mice. Furthermore, BCD+Lr treatment was able to normalize the number and activation of splenic Ma and DC after the challenge.
Lr administration stimulates respiratory and systemic mononuclear phagocytes. Stimulation of Ma and DC populations would increase the microbicide activity and improve the adaptive immunity through its antigen-presenting capacity. Thus, Lr contributes to improved outcomes of pneumococcal infection in immunocompromised hosts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Macrophages (Ma) and dendritic cells (DC) are key components of the mononuclear phagocyte system and are critically important for mediating protective immune responses in tissues. These cells have several functions such as the identification of pathogens through pattern recognition receptors, the phagocytosis of invading pathogens, and the modulation of inflammatory processes by secreting cytokines. In addition, they play an essential role in adaptive immunity as antigen-presenting cells (APC) [1]. Many APC subsets deliver not only signal 1 (the antigen) but also late signals to instruct the differentiation process of B cells into plasma cells in both a T cell–dependent and T cell–independent manner [2].
Tissue Ma and DC populations are distributed throughout the body but are typically found in higher numbers at strategic sites, such as the mucosal surfaces, which are entry points for pathogens, and secondary lymphoid organs, where adaptive immune responses are initiated. In steady state, monocytes (Mo) and pre-DC produced in the bone marrow are released into circulation and can finally extravasate in distant lymphoid and non-lymphoid tissues to generate tissue-resident Ma and DC populations [1, 3]. Ma are found in great amounts in the alveolar space, so they are crucial for pathogen clearance and the suppression of local inflammatory processes. It has been described that circulating Mo are precursors of alveolar Ma. This process requires an obligatory intermediate step, the differentiation of blood Mo into parenchymal lung Ma which subsequently migrate to the alveolar space [4]. Apart from Ma, there are plasmacytoid DC (pDC) and at least two myeloid DC populations (CD103− CD11bhight and CD103+ CD11blow) in the lung. Both CD11bhight and CD103+ DC have a relatively short lifespan in the lung and migrate to bronchial lymph nodes [5]. It has been shown that Mo can give rise to CD11bhight DC, and pre-DC may produce CD103+ DC [1]. The spleen, a lymphoid organ and part of the mononuclear phagocyte system, contains various populations. The red pulp Ma remove old erythrocytes and recycle iron; the marginal zone Ma protect the host by capturing and destroying blood-borne pathogens; and the white pulp CD11chigh DC initiate adaptive immunity by presenting blood-borne antigens to T cells [6]. Splenic DC, unlike Ma, do not originate from Mo, but instead from pre-DC [7, 8]. The spleen under steady state also contains a large reservoir of Mo which do not differentiate locally. The splenic Mo are important because they can re-enter blood circulation and be deployed to distant sites in response to inflammation [1].
Host immune status associated with age, chronic diseases, and immunosuppression are all significant risk factors for the development of severe pneumococcal infection [9]. While the infection can be serious in immunocompetent individuals, it can be devastating for those who are immunocompromised. In this context, pneumonia and malnutrition are two main causes of morbidity and mortality in childhood. Several interventions that aim to reduce the global burden of deaths from pneumonia have been identified. These include improving nutrition and rates of breast-feeding, reducing housing overcrowding, and improving access to antibiotics [9]. Lactic acid bacteria (LAB) can be used as a strategy as well. Different LAB strains capable of modulating immune responses via the induction of key immune system molecules and cells have been used to improve respiratory immunity [10,11,12,13]. Our research group demonstrated that nasal administration of Lactobacillus rhamnosus CRL1505 during repletion of malnourished mice resulted in diminished susceptibility to the challenge with the respiratory pathogen Streptococcus pneumoniae [14, 15]. Moreover, we showed that the treatment of malnourished mice with balanced conventional diet (BCD) supplemented with L. rhamnosus was able to normalize spleen and lung B cell numbers and to increase the levels of bronchoalveolar and serum anti-pneumococcal antibodies [14]. In addition, this treatment was effective in reducing quantitative and qualitative alterations of CD4 T cells in the bone marrow, thymus, spleen, and lung of malnourished mice [16].
Taking into account the fundamental role of Ma and DC in the generation of adequate and efficient immune response, we studied the effect of nasally administered L. rhamnosus CRL1505 on mononuclear phagocytes, at both respiratory and systemic levels, during (i) the dietary recovery of malnourished mice and (ii) in the setting of pneumococcal infection. This investigation will allow us to know more details of the mechanisms involved in the beneficial effect of L. rhamnosus over the immunity against S. pneumoniae.
Materials and Methods
Microorganisms
Lactobacillus rhamnosus CRL1505 was obtained from the CERELA culture collection. Lactobacilli (stored at − 70 °C) activated and cultured for 12 h at 37 °C (final log phase) in Man-Rogosa-Sharpe (MRS) broth. The bacteria were harvested by centrifugation and washed with sterile 0.01 mol/L PBS, pH 7.2 [17]. Encapsulated S. pneumoniae serotype 14 (ANLIS, Argentina) were isolated from the respiratory tract of a patient from the Children Hospital, Tucuman, Argentina.
Animals and Treatments
Male 3-week-old Swiss-albino mice were obtained from CERELA. Weaned mice were fed with a protein-free diet (PFD) for 21 days, and the mice that weighed 45–50% less than well-nourished mice were selected for the experiments. Malnourished mice were divided into two groups: mice were fed with a balanced conventional diet (BCD) for 7 days (BCD group) or BCD for 7 days, and during the last 2 days, the mice received L. rhamnosus CRL1505 (108 cells/mouse/day) by the nasal route (BCD+Lr group) [14]. A third group of malnourished mice was used as the malnourished control group (MNC). MNC mice received only a PFD during experiments. Normal mice were used as the well-nourished control (WNC) group. WNC mice consumed only the BCD ad libitum during experiments. The compositions of the BCD and PFD diets were described previously [18].
Pneumococcal Infection
Challenge with S. pneumoniae was carried out on the day after the end of each treatment (day 8) by dropping 25 μL of the inoculum containing 105 log-phase cells of S. pneumoniae in PBS into each nostril as described previously [14]. Animals were sacrificed at day 0 (before challenge) and at different days post-infection. Animal studies and protocols were approved by the CERELA Ethical Committee of Animal Care.
Obtaining of Cell Suspensions
Spleen and lung cells from mice were prepared using the method described previously [14, 19]. In brief, spleens were homogenized in RPMI 1640 with 2% FBS and filtered through a mesh. Lungs were minced and incubated 1 h in digestion medium (RPMI-1640 supplemented with 5% FBS and 140 kU/L collagenase type I, Sigma). The samples were homogenized in RPMI 1640 with 5% FBS and filtered through a mesh. Finally, samples were subjected to RBC lysis (Tris-ammonium chloride, BD PharMingen), washed in FACS buffer, counted on a hemacytometer, and kept on ice until immunofluorescent labeling. Viability of the cells was assessed through trypan blue exclusion.
Flow Cytometry and Staining Procedure
Flow cytometry was performed using a BD FACSCalibur TM flow cytometer (BD Biosciences), and data were analyzed using Flow Jo software (Tree Star). Spleen and lung cells were pre-incubated with anti-mouse CD32/CD16 monoclonal antibody (Fc block) and stained with different combinations of the following antibodies from BD PharMingen: FITC-labeled anti-mouse CD11b, FITC-labeled anti-mouse CD11c, PE-labeled anti-mouse MHC II, PE-labeled anti-mouse Gr-1, biotinylated anti-mouse CD11b, biotinylated anti-mouse B220, biotinylated anti-mouse F4/80, APC-labeled anti-mouse CD11c, APC-labeled anti-mouse CD45, and APC-labeled anti-mouse F4/80 antibodies. Streptavidin-PerCP was used as a second-step reagent. In addition, the FL1 channel was used for the assessment of autofluorescence (AF) in pulmonary cells. The number of cells in each population was determined by multiplying the percentages of subsets within a series of marker negative or positive gates by the total cell number determined for each tissue. The results were expressed as absolute number of cells per tissue.
Statistical Analysis
Experiments were performed in duplicate, and results were expressed as mean ± SD. Statistical analysis was conducted using MINITAB software (version 15 for Windows). Two-factor ANOVA was used to test the effects of the experimental groups, time, and their interaction. Tukey’s post hoc test was used to test for differences between the mean values. Significance was set at P < 0.05.
Results
Effect of L. rhamnosus CRL1505 on APC and Their Precursors in the Lungs
First, we identified pulmonary leukocytes through their CD45 expression (Online Resource 1a). We found that the malnutrition significantly impaired the number of lung leukocytes and that the treatment with BCD or BCD+Lr increased this parameter, reaching values similar to WNC group (Fig. 1a).
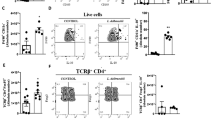
Number of lung leukocytes (a), monocytes (Mo) (b), macrophages (Ma) (c), Gr-1+ Ma (d), and expression of MHC II on Ma (e). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d
It has been proposed that Mo reaching the lung are precursors of Ma and DC [4]. Secondly, we studied pulmonary Mo and Ma as CD11c−CD11b+F4-80+ and CD11c+CD11b−/lowAF+F4-80+ cells, respectively (Online Resource 1b-d) [20]. Results indicated that malnutrition significantly reduced the number of both lung Mo and Ma. Repletion of malnourished mice with BCD increased the number of lung Mo and Ma, but it was not able to normalize these values. Treatment with BCD+Lr also increased the number of those populations. In fact, BCD+Lr mice showed values of both Mo and Ma that were not different from the WNC group (Fig. 1b, c). In addition, we studied the population of Gr-1+ Ma as recently recruited lung Ma. Significantly lower levels of Gr-1+ Ma were detected in MNC mice when compared with WNC mice. Both BCD and BCD+Lr repletion treatments increased the number of Gr-1+ Ma. However, BCD+Lr showed values of Gr-1+ Ma higher than those of the WNC group (Fig. 1d). We studied lung Ma activation by measuring their MHC-II expression (Online Resource 1). Results showed that malnutrition impaired the MHC-II expression on lung Ma, and the mice treated with BCD or BCD+Lr were able to increase MHC-II levels reaching values similar to WNC group (Fig. 1e).
We also evaluated the changes in the respiratory DC. Lung myeloid DC were identified as CD11c+CD11b+AF−F4-80− (subsets CD11blow and CD11b+) and plasmacytoid DC as CD11c+CD11b−/lowAF−F4-80−B220+. In addition, MHC-II expression in DC was studied (Online Resource 1) [21]. MNC mice exhibited a significant decrease of total DC numbers as well as CD11blow, CD11b+, and B220+ DC subpopulations when compared with any other group (Fig. 2). BCD+Lr treatment was more effective than BCD alone in improving the number of DC. The increase of pulmonary DC in BCD+Lr group was mainly at the expense of an increase in CD11b+ DC population (Fig. 2c). In addition, mice treated with BCD and BCD+Lr were able to normalize the number of CD11blow DC and B220+ DC (Fig. 2b, d). Protein deprivation decreased MHC-II expression in lung DC. Both BCD and BCD+Lr treatments increased DC MHC-II expression; however, BCD+Lr showed values of MHC II expression similar or higher than those of the WNC group (Fig. 2e).
Number of lung total dendritic cells (DC) (a) and CD11blow (b), CD11b+ (c) and B220+ (d) DC subpopulations. Expression of MHC II on lung total DC (e). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d
Effect of L. rhamnosus CRL1505 on Mononuclear Phagocytes in Lymphoid Tissue
We studied the effect of malnutrition and repletion treatments in mononuclear phagocyte spleen populations. After identification of total myeloid cells through CD11b+, spleen Mo were subsequently identified as CD11c−CD11bhighF4-80intermediate, Ma as CD11c−CD11b+F4-80highMHCIIlow/intermediate, and DC as CD11chighCD11b+F4-80−MHCIIhigh cells (Online Resource 2) [8].
In the spleen, a decreased number of myeloid cells, Mo, Ma, and DC were detected in MNC mice compared with WNC group (Fig. 3a–c, e). In addition, we observed that malnutrition significantly impaired Ma and DC MHC II expression (Fig. 3d, f). Both BCD and BCD+Lr treatments were able to normalize the number of spleen myeloid cells, Mo, Ma, and DC (Fig. 3a–c, e). Nevertheless, the repletion treatment with BCD+Lr was more effective than the BCD treatment to upregulate the activation surface marker MHC-II on spleen APC. In fact, L. rhamnosus treatment improved expression of MHC-II in both spleen Ma and DC, reaching similar and higher values than WNC group, respectively (Fig. 3d, f).
Number of total myeloid cells (CD11b+) (a), monocytes (Mo) (b), macrophages (Ma) (c), and dendritic cells (DC) (e) in the spleen. Expression of MHC II on spleen Ma (d) and DC (f). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d
Effect of L. rhamnosus CRL1505 on Lung Mononuclear Phagocytes After the Challenge with S. pneumoniae
We evaluated if the changes induced by nasal administration of lactobacilli were able to influence the response of lung presenting cells to the pneumococcal challenge.
An increase in the number of lung leukocytes, Mo, and Ma was produced by the respiratory challenge. The infection induced an increase of lung Ma activation state. In fact, we observed an increase in the number of MHC IIintermediate Ma at the expense of a decrease in the MHC IIlow Ma after infection (Fig. 4). These changes were observed in all experimental groups. In MNC mice, all these parameters were significantly lower than in the WNC group (Fig. 4). In BCD mice, the number of leukocytes after the challenge was not different from the MNC group (Fig. 4a). However, the treatment of malnourished mice with BCD+Lr was able to normalize this parameter at day 5 post-infection. It also increased the number of lung Mo. In fact, BCD+Lr mice showed values of Mo that were higher than BCD mice and similar to the WNC group (Fig. 4b). Although there were no differences in the number of lung Ma, the levels of MHC II on lung Ma in the BCD+Lr group were higher than those in the BCD group (Fig. 4c, e).
Number of lung leukocytes (a), monocytes (Mo) (b), macrophages (Ma) (c), and Gr-1+ Ma (d) after challenge with S. pneumoniae. Expression of MHC II on lung Ma at day 2 post-infection (e). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d. *Significantly higher than the basal values (before the challenge) (P < 0.05)
Furthermore, the infection with S. pneumoniae induced a transient increase in the number of lung DC (Fig. 5). No differences were observed in the number of total DC or their subpopulations between BCD and BCD+Lr groups. They presented similar or higher values than the MNC mice (Fig. 5). The increase of DC after the challenge was accompanied by an increase in the levels of MHC II expression in these cells. Both BCD and BCD+Lr groups showed MHC II expression levels similar to MNC mice (Fig. 5e).
Number of total dendritic cells (DC) (a) and CD11blow (b), CD11b+ (c) and B220+ (d) DC subpopulations in lung after challenge with S. pneumoniae. Expression of MHC II on lung DC at day 2 post-infection (e). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d. *Significantly higher than the basal values (before the challenge) (P < 0.05)
Effect of L. rhamnosus CRL1505 on Spleen Mononuclear Phagocytes After the Challenge with S. pneumoniae
The pneumococcal infection induced an increase in the number of spleen myeloid cells. However, in the BCD+Lr group, this increase was observed on day 2 post-infection reaching similar values to the WNC group. In MNC and BCD groups, the increase of myeloid cells was observed on day 5 post-infection (Fig. 6a). When spleen Mo and Ma were evaluated, we found higher numbers of these cells after the challenge compared with the basal levels (Fig. 6b, c). The MNC mice showed the lowest numbers of spleen Mo and Ma. In the group treated with L. rhamnosus, unlike the BCD group, the number of spleen Mo and Ma was similar to the WNC mice (Fig. 6b, c). In addition, the pneumococcal challenge induced an increase of the expression of MHC II on spleen Ma in all experimental groups. Despite the BCD and BCD+Lr groups showing higher MHC II expression levels than MNC mice on day 2 post-infection, only the BCD+Lr group reached similar values of those to the WNC group (Fig. 6d).
Number of total myeloid cells (CD11b+) (a), monocytes (Mo) (b), and macrophages (Ma) (c) in spleen after the challenge with S. pneumoniae. Expression of MHC II on spleen Ma at day 2 post-infection (d). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d. *Significantly higher than the basal values (before the challenge) (P < 0.05)
The number of spleen DC also increased after the challenge with the respiratory pathogen (Fig. 7a). In the WNC, BCD, and BCD+Lr groups, the increase was at day 2 post-infection while in the MNC group was at day 5 post-infection (Fig.7a). In the BCD and BCD+Lr groups, the number of spleen DC was similar to the WNC group. In addition, the levels of MHC II expression on DC in the BCD+Lr group were higher than the BCD group and similar to WNC (Fig.7b).
Number of spleen dendritic cells (DC) (a) after the challenge with S. pneumoniae and their expression of MHC II at day 2 post-infection (b). Well-nourished mice (WNC), malnourished mice (MNC), and malnourished mice fed BCD for 7 days that were or were not nasally administered L. rhamnosus (BCD and BCD+Lr groups, respectively). Values are means ± SD, n = 6. Means without a common letter differ (P < 0.05), a > b > c > d. *Significantly higher than the basal values (before the challenge) (P < 0.05)
Discussion
We have used the gram-positive bacterium Streptococcus pneumoniae to examine the macrophages and dendritic cells’ role in pulmonary defenses of immunocompromised-malnourished hosts. S. pneumoniae is the most common cause of pneumonia and may spread beyond the lung. The immunocompromised hosts have an increased susceptibility to pneumonia caused by S. pneumoniae as it has been previously demonstrated in our murine model of malnutrition [14, 15, 17, 18]. Moreover, it was shown that the nasal administration of Lactobacillus rhamnosus CRL1505 during malnourished mice repletion was able to increase resistance against the respiratory pathogen [14, 15]. Although the mechanism of this effect is not completely understood, we know that the probiotic, L. rhamnosus CRL1505, improves lung and systemic immune response [14, 15]. In this work, we focus our attention on the effect of L. rhamnosus supplementation on respiratory and systemic macrophages and dendritic cells during the immune response against S. pneumoniae infection in immunocompromised hosts.
L. rhamnosus Effect on Macrophages in the Orchestration of Anti-pneumococcal Immunity
In steady state, alveolar macrophages are the resident phagocytes in the lung, thus constituting 90–95% alveolar cellular content [22]. There are at least two distinct populations of alveolar macrophages. Tissue-resident alveolar macrophages develop outside of the bone marrow, become differentiated into alveolar macrophages shortly after birth, and are capable of self-renewal. Monocyte-derived alveolar macrophages arise from circulating monocytes being mainly recruited to the lung during inflammatory conditions [22]. The lung microenvironment supplies continuous signals to maintain or replace the lung macrophage pool [23]. It is not well known how these signals work; however, granulocyte macrophage colony-stimulating factor (GM-CSF) is known to play an important role [24, 25]. Our findings showed that malnutrition impaired lung macrophage populations and BCD+Lr treatment, unlike BCD, was able to increase the number of lung macrophages reaching similar values to WNC mice. These results are related to previous reports that demonstrated that dietary supplementation with L. rhamnosus CRL1505 improves bone marrow myelopoiesis in malnourished mice through the increase of GM-CSF expression [15]. Humans and mice, genetically deficient in GM-CSF or its receptor, fail to develop alveolar macrophages capable of clearing surfactant protein from the lung resulting in pulmonary alveolar proteinosis [20, 26]. Based on these data, we hypothesize that the recovery of lung macrophages by probiotic lactic acid bacteria could induce changes inside the lung microenvironment favoring the optimal levels of growth factors, especially GM-CSF, and thus promoting the renewal of the resident alveolar macrophages. On the other hand, the increased arrival of monocytes to the lung of BCD+Lr-treated mice could be due to an increased release of monocytes from the bone marrow into circulation. Lung monocytes have the capacity to differentiate on various APC types and contribute to increased Gr-1+ macrophages (recently recruited macrophages) that we observed in the lung of BCD+Lr group.
Alveolar macrophages are key cells in the host defense against pulmonary pathogens, e.g., S. pneumoniae. The bacteria are ingested and killed by alveolar macrophages, but when the bacterial load exceeds the alveolar macrophage’ capacity, leukocyte recruitment begins. These additional phagocytes become critical effectors of bacterial clearance [27]. We observed an increased number of leukocytes, as well as monocytes, macrophages, and dendritic cells in the lungs of mice infected with S. pneumoniae. However, all these populations were impaired by malnutrition, which would explain the difficulties of malnourished mice to eradicate the pathogen from the lungs [14, 15]. Circulating monocytes supply peripheral tissues with macrophages and dendritic cell precursors. Whenever an infection occurs, monocytes also contribute directly to innate immune defense. They are highly sensitive and reactive to pathogen-derived molecules and can enhance microbicide defenses by producing TNF-α and iNOS [28]. Furthermore, monocytes can carry antigens from the infected lungs to lymph nodes and transfer them to dendritic cells which activate the CD4 T cells [29]. On the other hand, the host microbiota play an important role in the modulation of the local immune response during the steady state and lung disease. Investigators have reported that changes in the microbiota can alter the gene expression profile of alveolar macrophages and impair antiviral response against the influenza virus [30]. Here, we showed that the treatment of malnourished mice with BCD plus L. rhamnosus was able to increase and normalize the number of lung monocytes after the challenge with S. pneumoniae. Consequently, the recruited monocytes would either help to eradicate the pneumococcus or give rise to lung macrophages or dendritic cells, or carry antigen to lymph nodes. In fact, we observed that both BCD and BCD+Lr treatments normalized the number of lung macrophages after infection. However, the macrophage activation state of MHC II expression was higher in the BCD+Lr mice than in the BCD group. The ability of L. rhamnosus CRL1505 to stimulate lung macrophages was consistent with the increased microbicidal activity of alveolar macrophages previously observed in the infected BCD+Lr mice [14, 15]. Therefore, the treatment with CRL1505 can improve monocyte recruitment into the lungs and beneficially modulate the microbicide activity and the antigen presentation of pulmonary macrophages.
As previously mentioned, pneumococcal infection can spread beyond the lung, affecting sterile organs. We chose to study anti-pneumococcal immune responses in spleen because it combines an efficient removal of blood-borne microorganisms with a highly organized lymphoid compartment and makes the spleen the most important organ for antibacterial and antifungal immune reactivity [6]. Asplenic individuals have a 50-fold higher risk of developing sepsis and meningitis due to infections with encapsulated bacteria such as S. pneumoniae [31]. Splenic macrophages sense and remove bacteria overcoming the mechanisms of local defense thus reaching the spleen through the bloodstream. At the marginal zone, macrophages cooperate with B cells to develop the early anti-polysaccharide IgM response [32]. Our results showed that, after the pneumococcal infection, only the mice treated with L. rhamnosus were able to increase and normalize the number of splenic macrophages, as well as their activation state. Consequently, normalization and activation of splenic macrophages would reduce the host susceptibility to develop a systemic infection.
L. rhamnosus Effect on Dendritic Cells in the Orchestration of Anti-pneumococcal Immunity
Mucosal dendritic cells are the primary APC responsible for stimulating the production of IgA at the mucosal surface. It was demonstrated that lung dendritic cells induced the T cell–dependent production of IgA more strongly than other pulmonary APC, such as macrophages [33]. Activation and maturation of dendritic cells is vital to initiation and priming of T cell responses. Thus, activated dendritic cells can act on T cells and steer them toward T helper (Th)1, Th2, Th17, and/or T regulatory responses with the subsequent effect of protection against infections [34]. Our results showed that the L. rhamnosus treatment significantly upregulated the expression of activation surface marker MHC II in lung dendritic cells. The BCD+Lr treatment was also able to improve the number of respiratory dendritic cells with a more remarkable effect on CD11b+ dendritic cells subpopulation. As mentioned above, lung monocytes can give rise to CD11bhight dendritic cells [1]; therefore, the increase of monocytes in the lung of BCD+Lr mice could explain the augmentation of lung CD11b+ dendritic cells observed in this group. This subpopulation would be the lung CD11bhightCD103− dendritic cells described by Furuhashi et al. [5]. The authors showed that mouse lung CD11blowCD103+ dendritic cells predominantly elicited Th1 and Th17 responses, whereas lung CD11bhightCD103− dendritic cells primarily provoked a Th2 response. In addition, Suzuki et al. [35] showed that lung CD11bhigh dendritic cells had a more potent capability to induce IgA production than lung CD103+ dendritic cells suggesting that CD11bhigh dendritic cells are the principal APC that introduce IgA to the lung. Our results suggest that the nasal administration of L. rhamnosus can stimulate the activation/maturation of lung dendritic cells and would be able to promote the differentiation of the lung CD11b+ dendritic cells population. This idea is in agreement with our previous results that demonstrated that BCD plus L. rhamnosus treatment enhances bronchoalveolar Th2-cytokines and improves humoral immune response against S. pneumoniae in recovering malnourished mice [16]. Thus, our data could indicate that nasal administration of L. rhamnosus might induce dendritic cell maturation and evoke local humoral immunity upon nasal administration.
It is known that both innate and adaptive immune responses are essential to avoid the invasive pneumococcal disease [36]. Humoral immune activation in the lung also induces the systemic production of antibodies which are responsible for preventing the passage of S. pneumoniae into the blood [37]. In the spleen, after antigen-specific differentiation in the follicles of the white pulp, plasmablasts migrate into the red pulp. It has been found that plasmablasts require myeloid CD11chigh dendritic cells to survive in the red pulp and to make the transition into plasma cells, which generate protective antibodies [6]. In addition, Xu and Banchereau [2] described APC-derived soluble factors and ligand-receptor signals to direct B cell activation, proliferation, survival, and differentiation toward plasma cells. In our experimental model, we found a marked decrease in the number and activation state of the spleen macrophages and dendritic cells in the infected malnourished mice. Those alterations in the spleen of malnourished mice would affect their capacity to mount a systemic humoral response. This is correlated with our prior reports that have shown a significant impairment of the humoral response against S. penumoniae in malnourished mice, which was evidenced by the lower levels of serum anti-pneumococcal antibodies [14]. The mice treated with L. rhamnosus were able to reach values of both spleen macrophages and dendritic cells similar to the WNC mice. This treatment was also more effective than BCD for inducing activation of spleen macrophages and dendritic cells (levels of MCH II expression). Thus, the differences between both replete groups could explain the higher capacity of lactobacilli-treated mice to produce systemic antibodies in response to pneumococcal infection [14].
Conclusion
Novel strategies to reduce S. pneumoniae infection in high-risk populations may have important health benefits. Our results showed that L. rhamnosus CRL1505 nasal administration during a dietary recovery of malnourished mice was able to improve the number and activity of lung and spleen mononuclear phagocytes. Stimulation of respiratory and systemic macrophages and dendritic cell populations would mean an increase in microbicide defenses and a contribution to adaptive immunity through their antigen-presenting capacity and their ability to direct B cell differentiation. Consequently, it would result in a better control of the challenge with S. pneumoniae, thus raising the potential of immunobiotics’ use as a way of preventing respiratory infections in immunocompromised hosts.
In conclusion, L. rhamnosus CRL1505 might improve the number of macrophages and dendritic cells as well as regulate their activation, providing further evidence that this strain has the ability to influence and lead immune response. Although the mechanisms by which L. rhamnosus increases the resistance to S. pneumoniae and improves the immune response against the pathogen have not yet been fully elucidated, this study provides new cellular bases for these effects.
References
Cortez-Retamozo V, Etzrodt M, Pittet MJ (2012) Regulation of macrophage and dendritic cell responses by their lineage precursors. J Innate Immun 4:411–423. https://doi.org/10.1159/000335733
Xu W, Banchereau J (2014) The antigen presenting cells instruct plasma cell differentiation. Front Immunol 4(504). https://doi.org/10.3389/fimmu.2013.00504
Geissmann F, Manz MG, Jung S, Sieweke MH, Merad M, Ley K (2010) Development of monocytes, macrophages, and dendritic cells. Science 327:656–661. https://doi.org/10.1126/science.1178331
Landsman L, Jung S (2007) Lung macrophages serve as obligatory intermediate between blood monocytes and alveolar macrophages. J Immunol 179:3488–3494. https://doi.org/10.4049/jimmunol.179.6.3488
Furuhashi K, Suda T, Hasegawa H, Suzuki Y, Hashimoto D, Enomoto N, Fujisawa T, Nakamura Y, Inui N, Shibata K, Nakamura H, Chida K (2012) Mouse lung CD103+ and CD11bhigh dendritic cells preferentially induce distinct CD4+ T-cell responses. Am J Respir Cell Mol Biol 46:165–172. https://doi.org/10.1165/rcmb.2011-0070OC
Mebius RE, Kraal G (2005) Structure and function of the spleen. Nat Rev Immunol 5:606–616. https://doi.org/10.1038/nri1669
Varol C, Landsman L, Fogg DK, Greenshtein L, Gildor B, Margalit R, Kalchenko V, Geissmann F, Jung S (2007) Monocytes give rise to mucosal, but not splenic, conventional dendritic cells. J Exp Med 204:171–180. https://doi.org/10.1084/jem.20061011
Geissmann F, Gordon S, Hume DA, Mowat AM, Randolph GJ (2010) Unravelling mononuclear phagocyte heterogeneity. Nat Rev Immunol 10:453–460. https://doi.org/10.1038/nri2784
Rodríguez L, Cervantes E, Ortiz R (2011) Malnutrition and gastrointestinal and respiratory infections in children: a public health problem. Int J Environ Res Public Health 8:1174–1205. https://doi.org/10.3390/ijerph8041174
Forsythe P (2014) Probiotics and lung immune responses. Ann Am Thorac Soc 11:S33–S37. https://doi.org/10.1513/AnnalsATS.201306-156MG
Lehtoranta L, Pitkäranta A, Korpela R (2014) Probiotics in respiratory virus infections. Eur J Clin Microbiol Infect Dis 33:1289–1302. https://doi.org/10.1007/s10096-014-2086-y
Licciardi PV, Toh ZQ, Dunne E, Wong S-S, Mulholland EK, Tang M, Robins-Browne RM, Satzke C (2012) Protecting against pneumococcal disease: critical interactions between probiotics and the airway microbiome. PLoS Pathog 8:e1002652. https://doi.org/10.1371/journal.ppat.1002652
Villena J, Oliveira MLS, Ferreira PCD, Salva S, Alvarez S (2011) Lactic acid bacteria in the prevention of pneumococcal respiratory infection: future opportunities and challenges. Int Immunopharmacol 11:1633–1645. https://doi.org/10.1016/j.intimp.2011.06.004
Barbieri N, Villena J, Herrera M, Salva S, Alvarez S (2013) Nasally administered Lactobacillus rhamnosus accelerate the recovery of humoral immunity in B lymphocyte-deficient malnourished mice. J Nutr 143:227–235. https://doi.org/10.3945/jn.112.165811
Herrera M, Salva S, Villena J, Barbieri N, Marranzino G, Alvarez S (2014) Dietary supplementation with lactobacilli improves emergency granulopoiesis in protein-malnourished mice and enhances respiratory innate immune response. PLoS One 9:e90227. https://doi.org/10.1371/journal.pone.0090227
Barbieri N, Herrera M, Salva S, Villena J, Alvarez S (2017) Lactobacillus rhamnosus CRL1505 nasal administration improves recovery of T-cell mediated immunity against pneumococcal infection in malnourished mice. Benefic Microbes 8:393–405. https://doi.org/10.3920/BM2016.0152
Salva S, Nuñez M, Villena J, Ramón A, Font G, Alvarez S (2011) Development of a fermented goats’ milk containing Lactobacillus rhamnosus: in vivo study of health benefits. J Sci Food Agric 91:2355–2362. https://doi.org/10.1002/jsfa.4467
Villena J, Racedo S, Agüero G, Bru E, Medina M, Alvarez S (2005) Lactobacillus casei improves resistance to pneumococcal respiratory infection in malnourished mice. J Nutr 135:1462–1469. https://doi.org/10.1093/jn/135.6.1462
Salva S, Merino MC, Agüero G, Gruppi A, Alvarez S (2012) Dietary supplementation with probiotics improves hematopoiesis in malnourished mice. PLoS One 7:e31171. https://doi.org/10.1371/journal.pone.0031171
Joshi N, Walter JM, Misharin AV (2018) Alveolar macrophages. Cell Immunol 330:86–90. https://doi.org/10.1016/j.cellimm.2018.01.005
Jakubzick C, Helft J, Kaplan TJ, Randolph GJ (2008) Optimization of methods to study pulmonary dendritic cell migration reveals distinct capacities of DC subsets to acquire soluble versus particulate antigen. J Immunol Methods 337:121–131. https://doi.org/10.1016/j.jim.2008.07.005
Morales-Nebreda L, Misharin AV, Perlman H, Budinger GRS (2015) The heterogeneity of lung macrophages in the susceptibility to disease. Eur Respir Rev 24:505–509. https://doi.org/10.1183/16000617.0031-2015
Lavin Y, Winter D, Blecher-Gonen R, David E, Keren-Shaul H, Merad M, Jung S, Amit I (2014) Tissue-resident macrophage enhancer landscapes are shaped by the local microenvironment. Cell 159:1312–1326. https://doi.org/10.1016/j.cell.2014.11.018
Shibata Y, Berclaz P-Y, Chroneos ZC, Yoshida M, Whitsett JA, Trapnell BC (2001) GM-CSF regulates alveolar macrophage differentiation and innate immunity in the lung through PU.1. Immunity 15:557–567. https://doi.org/10.1016/S1074-7613(01)00218-7
Trapnell BC, Whitsett JA (2002) GM-CSF regulates pulmonary surfactant homeostasis and alveolar macrophage-mediated innate host defense. Annu Rev Physiol 64:775–802. https://doi.org/10.1146/annurev.physiol.64.090601.113847
Guilliams M, De Kleer I, Henri S, Post S, Vanhoutte L, De Prijck S, Deswarte K, Malissen B, Hammad H, Lambrecht BN (2013) Alveolar macrophages develop from fetal monocytes that differentiate into long-lived cells in the first week of life via GM-CSF. J Exp Med 210:1977–1992. https://doi.org/10.1084/jem.20131199
Aberdein JD, Cole J, Bewley MA, Marriott HM, Dockrell DH (2013) Alveolar macrophages in pulmonary host defence – the unrecognized role of apoptosis as a mechanism of intracellular bacterial killing. Clin Exp Immunol 174:193–202. https://doi.org/10.1111/cei.12170
Xiong H, Pamer EG (2015) Monocytes and infection: modulator, messenger and effector. Immunobiology 220:210–214. https://doi.org/10.1016/j.imbio.2014.08.007
Samstein M, Schreiber HA, Leiner IM, Susac B, Glickman MS, Pamer EG (2013) Essential yet limited role for CCR2+ inflammatory monocytes during Mycobacterium tuberculosis-specific T cell priming. ELife 2:e01086. https://doi.org/10.7554/eLife.01086
Abt MC, Osborne LC, Monticelli LA, Doering TA, Alenghat T, Sonnenberg GF, Paley MA, Antenus M, Williams KL, Erikson J, Wherry EJ, Artis D (2012) Commensal bacteria calibrate the activation threshold of innate antiviral immunity. Immunity 37:158–170. https://doi.org/10.1016/j.immuni.2012.04.011
Ram S, Lewis LA, Rice PA (2010) Infections of people with complement deficiencies and patients who have undergone splenectomy. Clin Microbiol Rev 23:740–780. https://doi.org/10.1128/CMR.00048-09
den Haan JMM, Kraal G (2012) Innate immune functions of macrophage subpopulations in the spleen. J Innate Immun 4:437–445. https://doi.org/10.1159/000335216
Naito T, Suda T, Suzuki K, Nakamura Y, Inui N, Sato J, Chida K, Nakamura H (2008) Lung dendritic cells have a potent capability to induce production of immunoglobulin a. Am J Respir Cell Mol Biol 38:161–167. https://doi.org/10.1165/rcmb.2007-0237OC
Romagnani S (2006) Regulation of the T cell response. Clin Exp Allergy 36:1357–1366. https://doi.org/10.1111/j.1365-2222.2006.02606.x
Suzuki Y, Suda T, Furuhashi K, Shibata K, Hashimoto D, Enomto N, Fujisawa T, Nakamura Y, Inui N, Nakamura H, Chida K (2012) Mouse CD11bhigh lung dendritic cells have more potent capability to induce IgA than CD103+ lung dendritic cells in vitro. Am J Respir Cell Mol Biol 46:773–780. https://doi.org/10.1165/rcmb.2011-0329OC
Henriques-Normark B, Normark S (2010) Commensal pathogens, with a focus on Streptococcus pneumoniae, and interactions with the human host. Exp Cell Res 316:1408–1414. https://doi.org/10.1016/j.yexcr.2010.03.003
Moore BB, Moore TA, Toews GB (2001) Role of T- and B-lymphocytes in pulmonary host defences. Eur Respir J 18:846–856
Acknowledgments
We thank Prof. Alicia López López (UNdeC) for improving the use of English in the manuscript.
Funding
This work was supported in part by grants from Universidad Nacional de Tucumán: PIUNT 26D/502; Agencia Nacional de Promoción Científica y Tecnológica: PICT 2013-3209; and Consejo Nacional de Investigaciones Científicas y Técnicas (CONICET): PIP 0531.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This study was carried out in strict accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the Guidelines for Animal Experimentation of CERELA (protocol BIOT-CRL-10), and all efforts were made to minimize suffering.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Barbieri, N., Salva, S., Herrera, M. et al. Nasal Priming with Lactobacillus rhamnosus CRL1505 Stimulates Mononuclear Phagocytes of Immunocompromised Malnourished Mice: Improvement of Respiratory Immune Response. Probiotics & Antimicro. Prot. 12, 494–504 (2020). https://doi.org/10.1007/s12602-019-09551-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12602-019-09551-8