Abstract
It has never been investigated whether the assessment tools of Adult Attention Deficit Hyperactivity Disorder Quality-of-Life (AAQoL) scale and the SF-36 measure the same construct. The participants were 101 parents of children with ADHD and 243 parents of school children. The parents completed both the Persian version of the AAQoL and the SF-36 questionnaires. The present study revealed that the Persian version of both AAQoL and SF-36 for the assessment of HRQoL in parents of children with ADHD has convergent and discriminant validity and internal consistency. Multitrait–multimethod correlation matrix showed that the domains of two questionnaires were moderately correlated. Current results support that AAQoL and SF-36 in parents of children with ADHD measure the same HRQoL constructs. Hence, for assessing the HRQoL of parents of children with ADHD, one of the two questionnaires can be used regard to the objective of study. The Persian version of the AAQoL loaded on four domains which were in line with the original version. HRQoL of parents of children with ADHD is markedly less than the community sample of children.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Attention deficit hyperactivity disorder (ADHD) is a very common psychiatric problem in children and adolescents. Its main symptoms are inattentiveness, hyperactivity, and impulsivity. Its prevalence in school-age children is about 3–5 percent (Wolraich et al. 1996; Ghanizadeh 2008; Rowland et al. (2013); Barkley 2014). Longitudinal studies with children having ADHD and retrospective studies with adults having this disorder indicate that ADHD symptoms usually persist into adulthood (Murphy and Barkley 1996; Ramos-Quiroga et al. 2013). The rate of full remission is about 10 %, while 30–70 % of children with ADHD would have some symptoms of this disorder even in adulthood (Faraone et al. 2000; Biederman 2004). Some studies reported unfavorable consequences of ADHD on the future of these children and adolescents (Ghanizadeh et al. 2012). For example, ADHD impacts educational, occupational, psychological, and social functioning. Adults with ADHD are exposed to a higher risk of unemployment, sick leave, substance abuse, and convictions (Ghanizadeh et al. 2011, 2012). On the other hand, comorbidity patterns reveal that ADHD is transmitted independently in families (Biederman et al. 1992). The risk of ADHD in children of parents with ADHD is 75 % (Biederman et al. 1995), and hence, many parents of children with ADHD themselves suffer from ADHD (Ghanizadeh et al. 2008). Moreover, there is a high rate of abuse of parents by children having ADHD. More than half of these parents are victims of physical, financial, verbal, and psychological abuse committed by their children with ADHD (Ghanizadeh and Jafari 2010). We intend to assess the HRQoL of parents of children with ADHD.
Several instruments are available for the assessment of adults with ADHD. These are diagnostic interviews, brief screening instruments, and self-reported scales (Kessler et al. 2005; Magnússon et al. 2006). However, these measures were designed to assess symptoms rather than the effect of ADHD on adults’ health-related quality of life (HRQoL). Brod and colleagues developed the 68-item Adult ADHD Quality-of-Life Measure (AAQoL) to assess the HRQoL of adults (Brod et al. 2005). They also psychometrically validated the AAQoL by developing a formal measurement model. They explored the reliability and validity of the AAQoL as well. After some modifications, the AAQoL changed to a 29-item questionnaire (Brod et al. 2006). Since there is no specific health-related quality-of-life questionnaire available for parents of children with ADHD, we intend to employ the AAQoL to assess the HRQoL of parents of children with ADHD.
As part of the Medical Outcomes Study (MOS), a multi-year and multi-site study to explain variations in patient outcomes, RAND developed the 36-Item Short Form Health Survey (SF-36). The SF-36 is a set of generic, coherent, and easily administered quality-of-life measures. These measures rely upon self-reporting of patients; they are now widely utilized for routine monitoring and assessment of care outcomes in adult patients (Ware and Sherbourne 1992). Montazeri and colleagues translated this questionnaire into Persian. They found its reliability and validity to assess the health-related quality of life among Iran’s general population (Montazeri et al. 2005). The main objective of the present study was to check whether the AAQoL and the SF-36 for assessing the HRQoL of parents of children with ADHD measure the same construct. It was assumed that for assessing the HRQoL of parents of children with ADHD, the AAQoL domains would be moderately correlated with the related SF-36 domains. In this case, the SF-36 can be used instead of the AAQoL. To the best of our knowledge, this topic has not been explored yet. Also, we used control group to show a lower HRQoL among parents of ADHD children than those of general population.
Methods
Participants and instruments
The study was carried out at a child psychiatric clinic affiliated with Shiraz University of Medical Sciences, Fars, Iran. The participants were 101 parents of children with ADHD and 243 parents of healthy school children (control group). They completed both the Persian version of both AAQoL and SF-36 questionnaires. The parents in control group were selected in a two-stage cluster random sampling from the four educational districts of Shiraz in Southern Iran. The study was approved by the ethics committee of the university, and all the participants gave informed written consent. Most parents in the case group (86 %) were mothers. Thus, case and control groups were matched in terms of gender. The mean (±SD) ages of the case and control groups were 34.75 (±6.086) and 37.25 (±7.129), respectively, and they were statistically significant (P = 0.002).
The SF-36 consisted of 36 items with eight subscales including Physical Functioning (PF, ten items), Role limitations due to Physical health problems (RP, four items), Bodily Pain (BP, two items), General Health perceptions (GH, five items), Vitality (VT, four items), Social Functioning (SF, two items), Role limitation due to Emotional problems (RE, three items), and Mental Health (MH, five items) (Ware and Sherbourne 1992).
The AAQoL comprised 29 items, which were divided into four subscales including Life Productivity (eleven items), Psychological Health (six items), Life Outlook (seven items), and Relationships (five items). Individual items were scored on a five-point Likert scale ranging from ‘Not at all/Never’ = 1 to ‘Extremely/Very Often’ = 5. In the two questionnaires, all the subscales were transformed into a 0–100 score, where a higher score indicated a better HRQoL.
Development of Persian version of the AAQoL
First, we contacted the developer of the AAQoL and obtained permission to translate the questionnaire.We conducted a forward–backward translation according to a standardized guideline (Beaton et al. 2000). Two independent bilingual translators, whose native language was Persian, translated the AAQoL into Persian. After reconciliation of the two Persian versions, the questionnaire was translated back into English. Next, the two English versions were sent to the developer. The developer’s comments were then used to make necessary changes. Finally, a focus group was used for more in-depth investigations to finalize the Persian version of the AAQoL.
Statistical analysis
Internal consistency for each domain of the AAQoL and the SF-36 was assessed using Cronbach’s alpha coefficient. An α > 0.70 was considered as an acceptable internal consistency (Chassany et al. 2002). We used the exploratory factor analysis to examine the construct of the Persian version of the AAQoL by using a varimax rotation for all items. The number of factors extracted was determined by eigenvalues >1 (Sharma 1995). The multitrait–multimethod correlation matrix and factor analysis with a varimax rotation were performed to check whether the AAQoL and the SF-36 measure the same constructs. If the two questionnaires measure the same construct, then there should be moderate-to-large correlations between subscales of similar constructs across the two instruments. In contrast, domains intended to measure different constructs in the two instruments should have ignorable-to-small correlations. Spearman correlations of <0.1, 0.1–0.29, 0.3–0.49, and >0.5 were considered as ignorable, small, moderate, and large, respectively (Cohen 1988).
The spearman correlation was used to test convergent and discriminate validity. A correlation coefficient >0.4 between an item and its own subscale is considered an evidence of convergent validity. Discriminate validity confirmed if the correlation between an item and its hypothesized subscale was significantly higher than its correlation with other subscales (Fayers and Machin 2013). Independent sample t tests were performed to compare the case and control groups for both AAQoL and SF-36 domains.
Results
Reliability and validity
As shown in Table 1, Cronbach’s α for the overall and each domain of both AAQoL and SF-36 questionnaires was more than 0.7, except for Relationship (0.57), and Role-Physical (0.69). It ranged from 0.57 (Relationship) to 0.88 (Psychological Health) and from 0.69 (Role-Physical) to 0.86 (Physical Functioning) for AAQoL and SF-36 domains, respectively. The summarized results of convergent and discriminate validity for the Persian version of the AAQoL and the SF-36 are shown in Table 1. This table displays that the success rate of convergent validity in both questionnaires was 100 % for all domains, except for Life Productivity (91 %)—the first domain of the AAQoL. The success rate for discriminate validity ranged from 87 to 100 and 89 to 100 % for the AAQoL and the SF-36, respectively.
Factor analysis
The principal factor analysis with a varimax rotation was used to determine the structure of all questions of the Persian version of the AAQoL. The factors were divided into four domains: Life Productivity (eleven items), Psychological Health (six items), Life Outlook (seven items), and Relationships (five items). Table 2 shows that all of the items were properly loaded on its domains.
Multitrait–multimethod
The factor analysis with a varimax rotation was conducted on the domains of both questionnaires in order to test whether the AAQoL and the SF-36 measure the same construct. Table 3 shows that all domains of the two questionnaires were loaded on Factor 1, except for two domains of the AAQoL questionnaire, namely Life Productivity and Relationships. These two domains are not only loaded on Factor 2 but also had acceptable load (near 0.4) on Factor 1. Moreover, Table 4 shows the correlations of the AAQoL and the SF-36 domains in the multitrait–multimethod correlation matrix. As we expected, similar domains of the two questionnaires were moderately correlated. Mental Health, Role-Emotional, Vitality, and General Health were highly correlated with Psychological Health.
Additional analysis
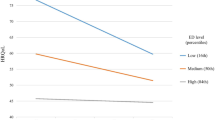
Table 1 shows that parents of children with ADHD have a significantly lower HRQoL than those of school children for total and each domains of the AAQoL. Also, parents of school children have a better HRQoL for total and each domains of the SF-36. However, according to this questionnaire, only General Health, Vitality, and Mental Health were statistically significant across these two groups. Moreover, the greatest mean differences between parents of children with ADHD and parents of school children were found in terms of Psychological Health in the AAQoL and in terms of Mental Health in the SF-36.
Discussion
The Persian version of the AAQoL has high internal consistency, except for the Relationships domain (Cronbach’s α = 0.57), which was in line with the results of two previous studies conducted in the USA (Brod et al. 2006; Matza et al. 2007). The present study reveals that the Persian version of the AAQoL has convergent and discriminant validity as well as internal consistency.
In order to provide more evidence to show that there is a better HRQoL among parents of school children than among parents of children with ADHD, we used the SF-36 questionnaire. It also showed that the SF-36 is internally consistent and proves validity for this questionnaire in parents of children with ADHD. The strength of the present study lies in the fact that it is the first study on the HRQoL of parents of children with ADHD and used two questionnaires simultaneously.
We reported the results of the factor structure of the AAQoL in order to compare our findings with those from a previous study (Brod et al. 2006). The results of the exploratory factor analysis with a varimax rotation reveal that the Persian version of the AAQoL measures the same construct that the original version of the AAQoL intended to measure (Brod et al. 2006).
The multitrait–multimethod correlation matrix showed a significant association between the AAQoL domains and the corresponding domains of the SF-36. Table 4 indicates that the four domains of the AAQoL were more closely associated with the psychosocial SF-36 domains such as Role-Emotional, Mental Health, and Social Functioning. As expected, they assess the overlapping constructs: the Psychological Health domain of the AAQoL, in particular, is strongly correlated with the Mental Health scale of the SF-36. The results of the factor analysis for extraction of the AAQoL and the SF-36 domains reveal that the two domains of the AAQoL, namely Psychological Health and Life Outlook, and all the SF-36 domains have high loading on the first factor. Moreover, two other domains of the AAQoL, namely Life Productivity and Relationships, have acceptable load for that factor. An important finding is that the AAQoL and the SF-36 for the assessment of the HRQoL of parents of children with ADHD measure the same trait and they can be used instead of each other.
It seems that there are some advantages of using each instrument with regard to the objective of study. The AAQoL is more specific as the number of its questions is lower and they are directly related to ADHD symptoms. Other advantage of using the AAQoL is that all of its domains have been able to discriminate between two groups. On the other hand, the international validation of the SF-36 questionnaire previously checked in many diseases. It allows us to assess the HRQoL in a wide variety of diseases. So, it provides comparability of disease groups or of case and control groups.
In comparison with two US studies (Brod et al. 2006; Matza et al. 2007), and ‘diagnosed-ADHD’ and ‘undiagnosed-ADHD’ participants in another US study (Able et al. 2007), our study reports a better HRQoL for participants in all AAQoL domains, except for Psychological Health. Better condition could be attributed to the lack of clinical diagnose for the participants in our study. Participants in three American studies were adults with ADHD, but participants in our study were parents of children with ADHD and some of them were probably without ADHD. Also, in comparison with ‘non-ADHD’ parents in the US studies (Able et al. 2007), parents of children with ADHD in our study showed a lower quality of life according to the AAQoL questionnaire domains.
In the USA (Brod et al. 2006), AAQoL scores in patients with ADHD were significantly lower than that of the control groups, which is similar to our finding. Moreover, the mean scores of all domains of the SF-36 in parents of our study were lower than those of parents of children with epilepsy in China (Lv et al. 2009), parents of children with autism spectrum disorder in Croatia (Benjak et al. 2009), and parents of children with pervasive developmental disorder in Japan (Yamada et al. 2012). In addition, parents of children with heart ailments in Egypt (Arafa et al. 2008) had a better HRQOL in all dimensions of the SF-36 compared to the parents of our study, except for Role-Physical and Vitality subscales.
The following limitations of the present study need to be considered. The major limitation is that we do not know how far cultural, language, and national traits contribute to the observed discrepancies. It could be rephrased as a future direction for a study measuring a range of factors that may contribute to cross-national/cross-cultural differences. Another limitation is that the sample of parents of children with ADHD was a clinical sample. The participants included those parents who visited the clinic and they were maybe more worried about the children. The AAQoL was made for adults with ADHD, but our participants were parents of children with ADHD. Hence, additional studies should assess the clinical diagnosis of these parents and other possible psychiatric diagnoses such as the number of mothers of children with ADHD. Furthermore, it is recommended that an instrument be devised for assessing the HRQoL of parents of children with ADHD. The final limitation is that in the present study, 86 % of these parents were mothers and so our finding could not be generalized to both parents.
Summary
In summary, the AAQoL and the SF-36 have good psychometric properties. For assessing the HRQoL of parents of children with ADHD, one of the two questionnaires can be used regard to the objective of study. Moreover, our findings provide evidence that the HRQoL of parents of Iranian children with ADHD was lower than that of the parents of children with chronic diseases in other countries.
References
Able SL et al (2007) Functional and psychosocial impairment in adults with undiagnosed ADHD. Psychol Med 37(01):97–107
Arafa MA et al (2008) Quality of life among parents of children with heart disease. Health Qual Life Outcomes 6(1):1
Barkley RA (2014) Attention-deficit hyperactivity disorder: a handbook for diagnosis and treatment. Guilford Publications, New York
Beaton DE et al (2000) Guidelines for the process of cross-cultural adaptation of self-report measures. Spine 25(24):3186–3191
Benjak T et al (2009) Comparative study on self perceived health of parents of children with autism spectrum disorders and parents of nondisabled children in Croatia. Croat Med J 50(4):403–409
Biederman J (2004) Impact of comorbidity in adults with attention-deficit/hyperactivity disorder. J Clin Psychiatry 65(3):1477–1478
Biederman J et al (1992) Further evidence for family-genetic risk factors in attention deficit hyperactivity disorder: patterns of comorbidity in probands and relatives in psychiatrically and pediatrically referred samples. Arch Gen Psychiatry 49(9):728–738
Biederman J et al (1995) High risk for attention deficit hyperactivity disorder among children of parents with childhood onset of the disorder: a pilot study. Am J Psychiatry 152(3):431–435
Brod M et al (2005) Conceptualization and assessment of quality of life for adults with attention-deficit/hyperactivity disorder. Prim Psychiatry 12(6):58–64
Brod M et al (2006) Validation of the adult attention-deficit/hyperactivity disorder Quality-of-Life Scale (AAQoL): a disease-specific quality-of-life measure. Qual Life Res 15(1):117–129
Chassany O et al (2002) Patient-reported outcomes: the example of health-related quality of life—a European guidance document for the improved integration of health-related quality of life assessment in the drug regulatory process. Drug Inf J 36(1):209–238
Cohen J (1988) Statistical power analysis for the behavior science. Lawrance Eribaum Association, Mahwah
Faraone SV et al (2000) Attention-deficit/hyperactivity disorder in adults: an overview. Biol Psychiatry 48(1):9–20
Fayers PM, Machin D (2013) Quality of life: the assessment, analysis and interpretation of patient-reported outcomes. Wiley, London
Ghanizadeh A (2008) Distribution of symptoms of attention deficit-hyperactivity disorder in schoolchildren of Shiraz, south of Iran. Arch Iran Med 11(6):618–624
Ghanizadeh A, Jafari P (2010) Risk factors of abuse of parents by their ADHD children. Eur Child Adolesc Psychiatry 19(1):75–81
Ghanizadeh A et al (2008) Comorbidity of psychiatric disorders and parental psychiatric disorders in a sample of Iranian children with ADHD. J Atten Disord 12(2):149–155
Ghanizadeh A et al (2011) Attention deficit hyperactivity disorder in imprisoned individuals—a review. Psychiatr Danub 23(2):139–144
Ghanizadeh A et al (2012) Psychiatric problems and suicidal behaviour in incarcerated adolescents in the Islamic Republic of Iran. East Mediterr Health J 18(4):311
Kessler RC et al (2005) The World Health Organization Adult ADHD Self-report Scale (ASRS): a short screening scale for use in the general population. Psychol Med 35(02):245–256
Lv R et al (2009) Depression, anxiety and quality of life in parents of children with epilepsy. Acta Neurol Scand 120(5):335–341
Magnússon P et al (2006) Validity of self-report and informant rating scales of adult ADHD symptoms in comparison with a semistructured diagnostic interview. J Atten Disord 9(3):494–503
Matza LS et al (2007) Responsiveness of the adult attention-deficit/hyperactivity disorder quality of life scale (AAQoL). Qual Life Res 16(9):1511–1520
Montazeri A et al (2005) The Short Form Health Survey (SF-36): translation and validation study of the Iranian version. Qual Life Res 14(3):875–882
Murphy K, Barkley RA (1996) Attention deficit hyperactivity disorder adults: comorbidities and adaptive impairments. Compr Psychiatry 37(6):393–401
Ramos-Quiroga JA et al (2013) Attention deficit hyperactivity disorder in the European adult population: prevalence, disease awareness, and treatment guidelines. Curr Med Res Opin 29(9):1093–1104
Rowland AS et al (2013) The prevalence of ADHD in a population-based sample. J Atten Disord. doi:10.1177/1087054713513799
Sharma S (1995) Applied multivariate techniques. Wiley, London
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36): I. Conceptual framework and item selection. Med Care 30(6):473–483
Wolraich ML et al (1996) Comparison of diagnostic criteria for attention-deficit hyperactivity disorder in a county-wide sample. J Am Acad Child Adolesc Psychiatry 35(3):319–324
Yamada A et al (2012) Quality of life of parents raising children with pervasive developmental disorders. BMC Psychiatry 12(1):1
Acknowledgments
This work was supported by the Grant Number 90-5844 from Shiraz University of Medical Science Council. This article was extracted from Roghaye Zare’s Master of Science thesis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
Research involved human participants.
Informed consent
All participants signed an informed consent form that was specifically designed for the current study.
Rights and permissions
About this article
Cite this article
Zare, R., Jafari, P. & Ghanizadeh, A. Do Adult Attention Deficit Hyperactivity Disorder Quality-Of-Life (AAQoL) scale and the SF-36 scale measure the same construct of health-related quality of life?. ADHD Atten Def Hyp Disord 9, 39–45 (2017). https://doi.org/10.1007/s12402-016-0206-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12402-016-0206-5