Abstract
This study aimed to demonstrate the effect of transcatheter arterial embolization (TAE) on hepatic segmental arterial mediolysis (SAM). The patient, a 68-year-old female, suddenly developed right upper abdominal pain in October 2021, which was initially relieved. However, she was rushed to a local hospital the next day when her abdominal pain recurred. An abdominal computed tomography scan suggested a ruptured hepatic aneurysm; therefore, she was transferred to our hospital and admitted on the same day. On the first day after admission, she underwent emergency catheterization and N-butyl-2-cyanoacrylate (NBCA)/lipiodol embolization for an aneurysm in the hepatic S6. A multi-detector computed tomography on hospital day 8 to probe for extrahepatic lesions revealed multiple beaded irregularities in the superior mesenteric and bilateral renal arteries. A head magnetic resonance angiography performed on the ninth day showed no aneurysms or irregularities. She did well after TAE, did not have rebleeding, and was discharged on hospital day 16. Rupture of an aneurysm associated with SAM occurs frequently in the colonic and gastroepiploic arteries, and rupture of a hepatic aneurysm is relatively rare. TAE hemostasis was able to save the patient by preventing intraperitoneal bleeding caused by hepatic segmental arterial mediolysis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Segmental arterial mediolysis (SAM) was first proposed by Slavin et al. and it forms a lump [1,2,3]. The clinical characteristics of SAM are as follows: (1) middle-aged and elderly people, (2) onset due to sudden intra-abdominal bleeding, (3) no underlying diseases, such as inflammatory changes or arteriosclerotic changes, and (4) irregular dilation and narrowing of arteries on angiography [4,5,6,7,8]. These features can be clinically diagnosed, even in the absence of pathological findings. In addition, the colonic and gastroepiploic arteries are the most frequent sites of aneurysm rupture associated with SAM, and rupture of hepatic aneurysms is relatively rare [9]. Here, we report a rare case of intraperitoneal bleeding caused by SAM of the liver that was resolved by transcatheter arterial embolization (TAE) hemostasis.
Case report
A 68-year-old female with a history of meningioma presented with right upper quadrant pain. She had no family history and did not smoke or drink.
In October 2021, the patient experienced sudden upper right abdominal pain, which was initially relieved. The following day, the pain recurred, and the patient was transported by ambulance to a nearby doctor. Abdominal computed tomography (CT) revealed rupture of the hepatic aneurysm; therefore, she was transferred to our hospital and hospitalized on the same day.
Symptoms on admission
Her height was 156 cm, weight was 70.0 kg, body temperature was 37.9 ℃, blood pressure was 160/90 mmHg, and pulse was 100 beats/min. The patient had clear consciousness, palpebral conjunctival anemia, and no bulbar conjunctival yellowing. Her abdomen showed swelling, right hypochondral tenderness, and no rebound pain.
Medications taken at the time of referral were as follows: amlodipine besilate 5 mg/day, losartan potassium 50 mg/day, irsogladine maleate 4 mg/day, atorvastatin calcium hydrate 10 mg/day, and ethyl icosapentate 900 mg/day.
Referral admission blood test (Table 1)
White blood cell count and C-reactive protein levels increased and hemoglobin (Hb) levels decreased to 9.2 g/dL. Elevation of transaminase levels was observed. No increase in hepatitis virus or tumor markers was observed. IgG and anti-nuclear antibody (ANA) levels were also negative.
Abdominal contrast-enhanced CT and abdominal angiography (Fig. 1 )
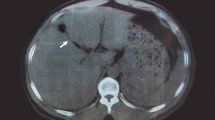
Abdominal computed tomography (CT) with contrast and abdominal angiography. Abdominal contrast-enhanced CT was performed on the first day of hospitalization. A huge aneurysm was found in liver S6, and intraperitoneal bleeding was also observed (a). Abdominal angiography revealed irregular celiac artery (CA). In addition, a giant aneurysm was identified in S6 of the liver and arterial embolization was performed using NBCA and lipiodol (b). Plain CT immediately after TAE showed lipiodol collection in the S6 aneurysm (c); angiography showed similar findings (d)
Abdominal contrast-enhanced CT was performed on the first day of hospitalization. A giant aneurysm was found in the liver S6, and intraperitoneal bleeding was also observed (Fig 1a). Abdominal angiography revealed irregular celiac artery (CA). Arterial embolization was performed using N-butyl-2-cyanoacrylate (NBCA) and lipiodol for the treatment of the giant aneurysm in S6 of the liver (Fig 1b). Since it was difficult to insert into the blood vessel distal to the aneurysm, isolation was performed with NBCA, which reaches the periphery, without using a coil. Plain CT immediately after TAE showed lipiodol collection in the S6 aneurysm (Fig 1c), and angiography showed similar findings (Fig 1d).
Abdominal angiogram at admission and after long-term follow-up (Fig. 2)
Abdominal angiogram at admission and after long-term follow-up. Beaded irregular dilatation and narrowing were also observed in the superior mesenteric artery (yellow arrow) and bilateral renal arteries (red arrow) (a). Approximately 1 year and 6 months later, there was no change in the resulting irregularity at the same site (b)
Beaded irregular dilatation and narrowing were also observed in the superior mesenteric artery and bilateral renal arteries (Fig 2a). Approximately 1 year and 6 months later, there was no change in the resulting irregularity at the same site (Fig 2b).
Clinical course (Fig. 3)
Clinical course. Contrast-enhanced CT performed on the first day of hospitalization revealed a giant aneurysm of liver S6 and intraperitoneal bleeding from the same site. After TAE, an increase in the inflammatory response was observed, and the administration of antibiotics (CTRX1 g/day) was continued to prevent infection. Subsequently, the inflammatory reaction improved, and no rebleeding was observed. The patient was discharged in good condition on the 16th day of hospitalization
Contrast-enhanced CT performed on the first day of hospitalization revealed a giant aneurysm at the S6 liver segment and intraperitoneal bleeding from the same site; therefore, emergency catheterization and transfusion of two unit of red blood cells were performed. After TAE, an increase in the inflammatory response was observed, and administration of antibiotics (CTRX1 g/day) was continued to prevent infection. Subsequently, the inflammatory reaction improved, and no rebleeding was observed. The patient was discharged on the 16th hospital day.
Discussion
In this case, SAM was diagnosed based on abdominal pain due to sudden intra-abdominal bleeding, and angiography and CT images of the vasculature which showed multiple arterial widening and narrowing irregularities in the abdominal cavity. Although the patient was undergoing treatment for hypertension and dyslipidemia, CT showed no clear progression of arteriosclerosis, such as calcification of the arterial wall. In addition, there was no history of connective tissue disease and no increase in ANA or IgG was observed. A clinical diagnosis of SAM was made, although no pathological examination was performed.
In Japan, the middle colic artery is reported to be the most common site of SAM, followed by the pancreaticoduodenal and gastroepiploic artery [10]. In this case, multiple lesions were observed in the hepatic, celiac, superior mesenteric, and bilateral renal arteries. The site of rupture in this case was the hepatic artery; there are few reports of rupture at this site. Rather, it has been reported that most of them are replaced by granulation tissue and heal in several months to 3 years [11,12,13]. Although the exact reason why rupture of the hepatic artery is rare remains unknown, it is believed that the hepatic artery is surrounded by the surrounding liver parenchyma. However, since there are cases of massive bleeding from the hepatic artery, such as in the present case, even when SAM of unruptured hepatic artery origin is diagnosed, prophylactic hemostasis should be considered.
Surgery has been considered the first choice for the treatment of SAM [9, 14], but recently, TAE and conservative treatment have also been selected [15, 16]. Pillai et al. reported that management of SAM should be selected according to clinical findings, lesion vascular site, and the presence or absence of organ ischemia [17]. Surgical therapy is selected instead of TAE in cases in which TAE cannot be performed or when the risk of intestinal ischemia is high due to TAE. However, if vital signs are stable and angiography or CT angiography shows no contrast medium extravasation, conservative treatment is possible. In this case, intraperitoneal bleeding from the liver S6 was confirmed by angiography, and emergency TAE was performed. Unlike the gastrointestinal tract, the hepatic artery is a good indication for TAE because the blood vessels are relatively simple, and intestinal ischemia is not induced. All 7 cases of hepatic SAM (Table 2) reported within the past 10 years received TAE as first-line therapy [18,19,20,21,22,23]. Although there are few reports of rupture of the hepatic artery, there are cases of massive bleeding from the hepatic artery, such as in this case. Adaptation should be considered positively. Of the 7 cases shown in Table 2, 2 cases No. 2 and No. 5 did not develop intra-abdominal bleeding, but prophylactic TAE was performed [19, 22].
A limitation of this study is that no pathological examination was performed to diagnose SAM. However, given the sudden onset of abdominal pain due to intra-abdominal bleeding, and angiography and CT angiograms showing multiple wide and narrow arterial irregularities in the abdominal cavity, it is considered to be a typical SAM. Pathological diagnosis was difficult in this case due to the life-threatening condition.
In conclusion, we encountered a case of SAM in which emergency TAE hemostasis was effective for intraperitoneal rupture of a hepatic aneurysm. Reports of intra-abdominal rupture from the hepatic artery, such as this case, are extremely rare and have been reported.
Abbreviations
- SAM:
-
Segmental arterial mediolysis
- TAE:
-
Transcatheter arterial embolization
- CT:
-
Computed tomography
- MRA:
-
Magnetic resonance angiography
- Hb:
-
Hemoglobin
- CA:
-
Celiac artery
References
Slavin RE, Gonzalez-Vitale JC. Segmental mediolytic arteritis: a clinical pathologic study. Lab Invest. 1976;35:23–9.
Slavin RE, Saeki K, Bhagavan B, et al. Segmental arterial mediolysis: a precursor to fibromuscular dysplasia? Mod Pathol. 1995;8:287–94.
Slavin RE, Cafferty L, Cartwright J Jr. Segmental mediolytic arteritis. A clinicopathologic and ultrastructural study of two cases. Am J Surg Pathol. 1989;13:558–68.
Peng KX, Davila VJ, Stone WM, et al. Natural history and management outcomes of segmental arterial mediolysis. J Vasc Surg. 2019;70:1877–86.
Ko M, Kamimura K, Ogawa K, et al. Diagnosis and management of fibromuscular dysplasia and segmental arterial mediolysis in gastroenterology field: a mini-review. World J Gastroenterol. 2018;24:3637–49.
Michael M, Widmer U, Wildermuth S, et al. Segmental arterial mediolysis: CTA findings at presentation and follow-up. AJR Am J Roentgenol. 2006;187:1463–9.
Kalva SP, Somarouthu B, Jaff MR, et al. Segmental arterial mediolysis: clinical and imaging features at presentation and during follow-up. J Vasc Interv Radiol. 2011;22:1380–7.
Baker-LePain JC, Stone DH, Mattis AN, et al. Clinical diagnosis of segmental arterial mediolysis: differentiation from vasculitis and other mimics. Arthritis Care Res (Hoboken). 2010;62:1655–60.
Shenouda M, Riga C, Naji Y, et al. Segmental arterial mediolysis: a systematic review of 85 cases. Ann Vasc Surg. 2014;28:269–77.
Inada K, Maeda M, Ikeda T. Segmental arterial mediolysis: unrecognized cases culled from cases of ruptured aneurysm of abdominal visceral arteries reported in the Japanese literature [published correction appears in Pathol Res Pract. 2008;204(2):147]. Pathol Res Pract. 2007;203:771–8.
Tabassum A, Sasani S, Majid AJ, et al. Segmental arterial mediolysis of left gastric artery: a case report and review of pathology. BMC Clin Pathol. 2013;13:26.
Shimohira M, Kondo H, Ogawa Y, et al. Natural history of unruptured visceral artery aneurysms due to segmental arterial mediolysis and efficacy of transcatheter arterial embolization: a retrospective multiinstitutional study in Japan. AJR Am J Roentgenol. 2021;216:691–7.
Slavin RE. Segmental arterial mediolysis: course, sequelae, prognosis, and pathologic-radiologic correlation. Cardiovasc Pathol. 2009;18:352–60.
Chao CP. Segmental arterial mediolysis. Semin Intervent Radiol. 2009;26:224–32.
Skeik N, Olson SL, Hari G, et al. Segmental arterial mediolysis (SAM): systematic review and analysis of 143 cases. Vasc Med. 2019;24:549–63.
Srinivasan A, Olowofela A, Rothstein A, et al. A single center 8 year experience of segmental arterial mediolysis management. Ann Vasc Surg. 2022;81:273–82.
Pillai AK, Iqbal SI, Liu RW, et al. Segmental arterial mediolysis. Cardiovasc Intervent Radiol. 2014;37:604–12.
Nagamura N, Higuchi H. Segmental arterial mediolysis with preceding symptoms resembling viral infection hampers the differentiation from Polyarteritis nodosa. Intern Med. 2019;58:2721–6.
Zhakubayev M, Maruya Y, Takatsuki M, et al. Stent treatment for huge aneurysm of the common hepatic artery: a case report. Radiol Case Rep. 2018;14:44–7.
Olivares E, Vingan H, Zhou Q. Spontaneous hemoperitoneum resulting from segmental arterial mediolysis. Radiol Case Rep. 2018;13:732–5.
Beerle C, Soll C, Breitenstein S, et al. Spontaneous rupture of an intrahepatic aneurysm of the right hepatic artery caused by segmental arterial mediolysis. BMJ Case Rep. 2016;2016:bcr2015214109.
Ashfaq A. Money SR biopsy proven hepatic segmental arteriolar mediolysis successfully treated with coil embolization. Circulation. 2015;132:2265–6.
Marshall L, O’Rourke T, McCann A, et al. Spontaneous intrahepatic haemorrhage: two cases of segmental arterial mediolysis. ANZ J Surg. 2015;85:49–52.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Written informed consent was obtained in from the patient.
Human rights
This study was conducted in accordance with the Declaration of Helsinki.
Animal studies
Not applicable.
Approval of the research protocol
Not applicable.
Registry and the registration no. of the study/trial
Not applicable.
Research involving recombinant DNA
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kato, H., Hagiwara, S., Nishida, N. et al. A case of transcatheter arterial embolization for intraperitoneal hemorrhage due to giant hepatic segmental arterial mediolysis. Clin J Gastroenterol 16, 397–401 (2023). https://doi.org/10.1007/s12328-023-01766-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-023-01766-1