Abstract
A 69-year-old woman had received hemodialysis for chronic renal failure and was taking lanthanum carbonate since 63 years of age. She presented with appetite loss and nausea. We performed esophagogastroduodenoscopy, which revealed multiple longitudinal white plaques in the esophagus. Lesion biopsies showed lanthanum deposition, and lanthanum carbonate was found histologically by energy-dispersive X-ray spectroscopy. The plaques of this patient appeared like those of dabigatran-induced esophagitis, and may have occurred due to long-term contact of the esophageal epithelium with lanthanum carbonate because patient spent time in lying state. Although a few studies regarding lanthanum deposition in the stomach have been conducted, there are no reports on lanthanum deposition in the esophagus. This case suggests that the presence of longitudinal white plaques in the esophagus may indicate lanthanum deposition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lanthanum (La) carbonate is a phosphate binder used to treat hyperphosphatemia in patients with chronic renal failure. La is considered safe because absorption into the gastrointestinal tract is reported to be minimal.
La deposition in the gastric or duodenal mucosa of patients taking oral La carbonate has recently been reported. Esophagogastroduodenoscopy (EGD) for patients with gastric La deposition demonstrated a diffuse whitish gastric mucosa [1,2,3,4,5,6].
To our knowledge, esophageal La deposition has not yet been reported. This is the first report describing a case of La deposition in the epithelium of the esophageal mucosa.
Case report
A 69-year-old woman was diagnosed with chronic renal failure and had received hemodialysis for 10 years. She was under treatment with La carbonate (750 mg/day) for prevention of hyperphosphatemia since 63 years of age. She visited our hospital because of appetite loss and nausea. Computed tomography (CT) did not reveal the cause of appetite loss and nausea.
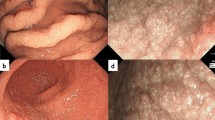
EGD was performed to investigate the cause of her symptoms. EGD demonstrated multiple longitudinal white plaques in the upper to lower esophagus (Fig. 1a, b). White gastric mucosa, suggesting gastric La deposition in the stomach, was not observed (Fig. 1c).
a–f Esophagogastroduodenoscopy (EGD). First EGD showing lanthanum deposition in the epithelium of the esophagus. a–c EGD demonstrated multiple longitudinal white plaques in the upper to lower esophagus (biopsies were taken from white plaques; parts taken for biopsy are indicated using blue arrows). Whitish gastric mucosa suggesting gastric lanthanum deposition was not found in the stomach (a and c are white light images, b is an NBI image). EGD 3 weeks after discontinued lanthanum use. d, e EGD showed no multiple longitudinal white plaques and the appearance of small brownish areas in the esophagus (d is white light image, e is an NBI image). The biopsy was taken from the small brownish area. Yellow arrow indicates the part taken for biopsy. f EGD showed slightly whitish gastric mucosa in the cardia of stomach (white light image). The biopsy was taken from whitish gastric mucosa. Red arrow indicates the part taken for biopsy
A biopsy from the esophageal mucosa showed deposition of an eosinophilic structure (Fig. 2a, b). Scanning electronic microscopy (SEM) showed an amorphous substance of high electron density in the epithelium of the esophageal mucosa (Fig. 3a). La was histologically found in the esophageal mucosa by energy-dispersive X-ray spectroscopy (EDS), and phosphorus (P) was not found at the same site (Fig. 3b, c). The EDS spectrum (detection range of P) was different from the La phosphate deposit published data (Fig. 4a). Thus, La carbonate per se may have been deposited in the esophagus.
a–d Pathological images. Pathological images of lanthanum deposition in the esophagus and the stomach. a, b Hematoxylin and eosin staining showed deposition of an eosinophilic structure in the epithelium of the esophageal mucosa (green arrows). Pathological images 3 weeks after discontinuation of lanthanum use. c Hematoxylin and eosin staining showed numerous macrophages with dark brown granular material in the epithelium of the esophageal mucosa. d Hematoxylin and eosin staining showed numerous macrophages with dark brown granular material in the lamina propria mucosae of the stomach
a–f Scanning electron microscopy (SEM) and energy-dispersive X-ray spectroscopy (EDS). a SEM showed an amorphous substance of high electron density in the epithelium of the esophageal mucosa. b, c EDS showed the distribution of lanthanum (La), but did not show the distribution of phosphate (P) at the same site (white arrow). Lanthanum carbonate per se was deposited in epithelium of the esophageal mucosa. d SEM 3 weeks after discontinued lanthanum use showed an amorphous substance of high electron density in the epithelium of the esophageal mucosa. e, f EDS 3 weeks after discontinued lanthanum use showed the distribution of La and P. Lanthanum phosphate complexes were found in the epithelium of the esophageal mucosa
After the patient discontinued La carbonate use, her symptoms gradually improved. 3 weeks later, EGD showed no longitudinal white plaques, but only a small red area in the esophagus (Fig. 1d, e). A biopsy of these red areas showed numerous macrophages with dark brown granular material in the esophageal mucosa (Fig. 2c). SEM showed an amorphous substance of high electron density in the epithelium of the esophageal mucosa (Fig. 3d). La and P were histologically found in the esophageal mucosa by EDS (Fig. 3e, f). It appeared that La phosphate had been deposited. EDS spectrum showed the presence of La and P (Fig. 4b). We observed the gastric mucosa carefully, because esophageal La deposition had been observed in the previous EGD and detected a slightly whitish gastric mucosa in the cardia of the stomach (Fig. 1f). A biopsy from this lesion showed La phosphate deposition in the lamina propria mucosae of the stomach (Fig. 2d). SEM and EDS findings of the gastric biopsy were similar to that of the esophagus.
An EGD after 1 year showed no longitudinal white plaques and a biopsy from the esophageal mucosa revealed no La deposition.
Although serum P level increased 5 months after discontinuing La carbonate use (P level; 1.3–4.5 mg/dL), the patient had no problems.
Discussion
La carbonate has been used because of its safety. La carbonate binds phosphate and prevents phosphate absorption. Almost all of the La phosphate complexes are excreted via feces because little is absorbed in the gastrointestinal tract [7, 8]. However, La carbonate may combine with dietary phosphate and deposit in the esophageal mucosa.
A diffuse white gastric mucosa has been observed with EGD in patients with La deposition, classified as an annular whitish mucosa, a diffuse whitish mucosa, and whitish spots [1,2,3,4,5,6].
In our patient, the first EGD showed multiple longitudinal white plaques in the upper to lower esophagus and second EGD showed only a small red area. In addition, the histological findings of biopsy sample in the first EGD were different from that of gastric La depositions, because La carbonate per se was deposited. The histological findings of the second biopsy sample was similar to that of gastric La depositions, because these consisted of La phosphate complex deposition phagocytosed by macrophages.
The esophageal multiple longitudinal white plaques of this patient appeared like those of dabigatran-induced esophagitis (DIE). DIE shows longitudinally sloughing epithelial casts in the mid and/or lower esophagus [9]. The longitudinal white plaques in our patient may have occurred due to long-term contact of the esophageal epithelium with La carbonate because the patient spent time in a lying state. Although we thought that this mechanism was similar to other drug-induced esophageal injury including DIE, it was unclear whether the patient had esophageal peristaltic disease because we did not perform barium X-ray examination and high resolution manometry; therefore, we performed biopsies to diagnose La deposition.
In conclusion, we report a case of La deposition in the esophageal mucosa. Multiple longitudinal white plaques were observed with EGD, and La deposition was observed using SEM and scanning and EDS.
References
Tonooka A, Uda S, Tanaka H, et al. Possibility of lanthanum absorption in the stomach. Clin Kidney J. 2015;8:572–5.
Makino M, Kawaguchi K, Shimojo H, et al. Extensive lanthanum deposition in the gastric mucosa: the first histopathological report. Pathol Int. 2015;65:33–7.
Goto K, Ogawa K. Lanthanum deposition is frequently observed in the gastric mucosa of dialysis patients with lanthanum carbonate therapy: a clinicopathologic study of 13 cases, including 1 case of lanthanum granuloma in the colon and 2 nongranulomatous gastric cases. Int J Surg Pathol. 2016;24:89–92.
Iwamuro M, Sakae H, Okada H. White gastric mucosa in the dialysis patient. Gastroenterology. 2016;150:322–3.
Murakami N, Yoshioka M, Iwamuro M, et al. Clinical characteristics of seven patients with lanthanum phosphate deposition in the stomach. Intern Med. 2017;56:2089–95.
Iwamuro M, Urata H, Tanaka T, et al. Lanthanum deposition in the stomach in the absence of Helicobacter pylori infection. Intern Med. 2018;57:801–6.
Pennick M, Dennis K, Damment SJ. Absolute bioavailability and deposition of lanthanum in healthy human subjects administered lanthanum carbonate. J Clin Pharmacol. 2006;46:738–46.
Zhang C, Wen J, Li Z, et al. Efficacy and safety of lanthanum carbonate on chronic kidney disease-mineral and bone disorder in dialysis patients: systematic review. BMC Nephrol. 2013;14:226.
Toya Y, Nakamura S, Tomita K, et al. Dabigatran-induced esophagitis: the prevalence and endoscopic characteristics. J Gastroenterol Hepatol. 2016;31:610–4.
Acknowledgements
We thank Dr. Masaya Iwamuro (Department of Gastroenterology and Hepatology, Okayama University Graduate School of Medicine, Dentistry and Pharmaceutical Science) for his important contributions with SEM and EDS.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Tetsuya Tatsuta, Tatsuya Mikami, Daisuke Chinda, Kazuki Akitaya, Shohei Igarashi, Keisuke Hasui, Hidezumi Kikuchi, Hiroto Hiraga, Manabu Sawaya, Hirotake Sakuraba, Tadashi Shimoyama, Tosihiro Haga, Hiroshi Kijima, and Shinsaku Fukuda declare that they have no conflict of interest.
Human rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from this patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tatsuta, T., Mikami, T., Chinda, D. et al. Case report of lanthanum deposition in the esophagus. Clin J Gastroenterol 13, 683–687 (2020). https://doi.org/10.1007/s12328-019-01085-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-019-01085-4