Abstract
The low phospholipid-associated cholelithiasis (LPAC) syndrome was reported in European adults with cholelithiasis and a mutation of the ATP-binding cassette subfamily B member 4 (ABCB4). The ABCB4 encodes multidrug resistance 3, which is a phospholipid translocator. Reduced phospholipid transport can lead to the formation of biliary cholesterol stones. Here, we describe a 31-year-old Japanese man diagnosed with recurrent biliary colic. Although he recovered quickly after endoscopic treatment for the most recent presentation, he had a family history of similar problems. His mother had required endoscopic treatment for choledocholithiasis and his maternal aunt had died at age 29 years because of liver failure (etiology unknown). We, therefore, performed genetic analysis, which revealed a heterozygous ABCB4C717S. LPAC syndrome was diagnosed and the patient has received ursodeoxycholic acid for 2 years with no recurrence. The same variant was identified in the patient’s mother, who was subsequently found to have a left intrahepatic calculus requiring left-sided lobectomy. She has received ursodeoxycholic acid for 1 year with no recurrence. ABCB4C717S is a novel pathogenic variant, and this is the first patient diagnosed with LPAC syndrome in Japan. We should consider LPAC syndrome in young adults with recurrent cholesterol gallstones to ensure early therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The main risk factors for gallstones are female gender, age, pregnancy, inactivity, and obesity [1]. However, gallstones are rare in young adults without these risk factors. In these cases, multiple and recurrent gallstones can be caused by a mutation in ATP-binding cassette subfamily B member 4 (ABCB4) gene [2,3,4,5]. The ABCB4 gene, which encodes multidrug resistance 3 (MDR3), is located on the long arm of chromosome 7 (7q21.12). MDR3 is phospholipid translocator across the hepatocyte canalicular membrane, and its role in phospholipid translocation is important to their role as a solvent of cholesterol and hydrophobic bile salts in bile by micellization. Reduced or absent phospholipid transport by low- or non-functioning MDR3 can lead to the formation of biliary cholesterol stones and bile salt-induced damage [2,3,4,5]. This low phospholipid-associated cholelithiasis (LPAC) syndrome was first described in 2001 [6] as the association of ABCB4 mutations, low biliary phospholipid concentrations, and recurring symptomatic cholelithiasis. The population prevalence of the disease was estimated to be 1 in 100,000 births in Europe [7]. Thankfully, most patients with LPAC syndrome have favorable outcomes with ursodeoxycholic acid therapy [8]. In this report, we describe the first Japanese case of a patient with LPAC syndrome and report ABCB4C717S as a novel pathogenic variant.
Case report
A 31-year-old man with upper abdominal pain was admitted to our hospital. At ages 18 and 24 years, he had experienced recurrent episodes of upper abdominal pain with liver dysfunction on blood tests and splenomegaly on computed tomography. Clinically, we suspected acute hepatitis at these times, but serological testing showed no abnormalities. When he was 26 years old, based on magnetic resonance cholangiopancreatography showing mild dilatation in some intrahepatic bile ducts, we suspected primary sclerosing cholangitis and performed a liver biopsy. However, the biopsy also showed no abnormality. When he was 30 years old, magnetic resonance cholangiopancreatography was repeated and showed choledocholithiasis, cholecystolithiasis, and intrahepatic stones, so he underwent endoscopic sphincterotomy (Fig. 1a) and laparoscopic cholecystectomy (Fig. 1b). The gallstones were whitish, indicating that they were cholesterol stones. His family history also revealed that his mother had experienced endoscopic treatment for biliary stones at the age of 47 and that his maternal aunt had died of liver failure at the age of 29 years (etiology unknown).
Cholesterol gallstones seen in the common bile duct and gallbladder. Endoscopic sphincterotomy and laparoscopic cholecystectomy were performed at 30 years of age. a Endoscopic retrograde cholangiopancreatography showed choledocholithiasis (closed arrow head), cholecystolithiasis (open arrow head), and intrahepatic stones (closed arrow). b Whitish stones in the gallbladder
At the current presentation, 6 months after cholecystectomy, the patient reported upper abdominal pain and vomiting. On physical examination, his body temperature was 37.2 °C, blood pressure was 88/37 mmHg, and heart rate was 77 beats per min, while abdominal palpitation revealed epigastric tenderness. He was not obese and did not have an unhealthy diet. Biochemical and hematological investigations indicated the presence of mild inflammation and liver dysfunction: white blood cells, 13,290/µL; total bilirubin, 2.7 mg/dL; aspartate aminotransferase, 645 IU/L; alanine aminotransferase, 416 IU/L; lactate dehydrogenase, 475 IU/L; alkaline phosphatase, 484 IU/L; and gamma-glutamyl transpeptidase, 340 IU/L. Contrast-enhanced computed tomography showed that the intrahepatic and common bile ducts were dilated and that both the splenomegaly and the collateral circulation of the portal vein had progressed.
We performed emergency endoscopic retrograde cholangiopancreatography, at which a whitish stone was shown to be impacted at Vater’s ampulla (Fig. 2). We removed the impacted stone with a removal balloon and placed an endoscopic naso-biliary drainage tube in the bile duct. He recovered quickly and was discharged on the eighth day of hospitalization. On discharge, we performed genetic analysis with his informed consent (Yamagata University Faculty of Medicine, Institutional Review Board, approval number: H29-395) because of the recurrent gallstones. This revealed a heterozygous ABCB4 variant, c.T2149A (p.C717S), as shown in Fig. 3. He has since received ursodeoxycholic acid for 2 years and has not suffered recurrence.
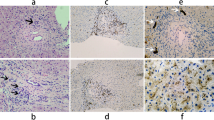
Furthermore, we performed genetic analysis of his immediate family after gaining their informed consent, which revealed the same genetic variant in his mother only (Fig. 3). His mother was a 56-year-old and received a screening test after genetic testing. This uncovered a left intrahepatic calculus and liver abscess for which she underwent a left lobectomy. Pathologically, she had marked fibrosis in the portal region, but no cancer cells were observed. She has since received ursodeoxycholic acid for 1 year without recurrence.
Method used for the mutation analysis
Genomic DNA was extracted from the peripheral blood of each subject using a DNeasy Blood. Whole-exome sequencing (WES) was performed using amplicon-based, next-generation sequencing. Briefly, amplified 317,368 amplicon libraries of 155–245 bp size were constructed using an Ion AmpliSeq Library Kit v2.0 (Thermo Fisher Scientific, Carlsbad, CA, USA), according to the manufacturer’s instructions. After adaptor ligation reaction, quantification of the libraries was performed on a 2200 TapeStation Instrument using D1000 Reagents and D1000 Screen Tape (Agilent Technologies, Santa Clara, CA, USA). Each 100 pmol of the amplified libraries was submitted to emulsion polymerase chain reaction using an Ion OneTouch2 Instrument with an Ion P1 Template Hi-Q OT2 200 Kit. Ion sphere particles were enriched using the Ion OneTouch ES Instrument. Ion sphere particles were then loaded on an Ion P1 Chip. Massive parallel sequencing was performed by an Ion Proton semi-conductor sequencer with an Ion P1 Hi-Q Sequencing 200 Kit.
Read sequence files were assessed through two independent genetic variant calling pipelines, Bowtie2-Platypus and BWA-Platypus, to address the human reference assembly (hg38) and to obtain the variant call format files. Then, concordant genetic variants were annotated using ANNOVAR, with population technical frequency from 1000 Genome and ExAC databases, protein damaging Phred score from SHIFT, GERP, and CADD databases, and genetic pathogenicity from the ClinVar database.
Finally, to confirm the mutation identified by WES, Sanger sequencing was performed using a BigDye V3.1 terminator Kit on ABI 3500 sequencer (Thermo Fisher Scientific). Primer sequences were obtained from Primer3. Polymerase chain reaction was performed to obtain a 680-bp product for the targeting chromosome position of ABCB4 exon 17. Sequence data were analyzed using EMBOSS and BLAST.
Discussion
The clinical phenotypes of ABCB4 mutations are broad but can broadly be divided into two forms. On the one hand, missense and heterozygous forms tend to be associated with biliary stone formation in young adulthood. On the other hand, nonsense and homozygous forms tend to progress to liver cirrhosis in childhood [9]. Furthermore, several studies have reported that mutations in ABCB4 increased the risk of cholangiocarcinoma, hepatocellular carcinoma, and gallbladder carcinoma [10,11,12,13,14,15,16]. ABCB4 mutation-associated cholelithiasis in young adults has been named the LPAC syndrome [6], and these patients typically present younger than 40 years at symptom onset and with recurrent biliary symptoms after cholecystectomy. Splenomegaly was observed in our case, which seems to have been caused by liver damage due to MDR3 dysfunction.
Most cases of LPAC syndrome are of the heterozygous missense form [8], with most disease-causing mutations localized to the central part of the molecule, close to nucleotide-binding domain 1, or in adjacent transmembrane domains [9]. Transmembrane 7, encoded by exon 17, is a part of the phospholipid translocation pathway [17]. To date, the C717S of ABCB4 detected in our patient and his mother has not been described. This variant located in exon 17 leads to a substitution of the amino acid serine with the amino acid cysteine at position 717, causing a neutral residue to be substituted with a polar residue. In turn, this may alter the interaction of the transmembrane segment of the phospholipid-binding pocket with phospholipids. The C717S of ABCB4 is conserved in mammalian ABCB4 and human ABCB1. ExAC, which is the largest reference dataset of human genetic variation [18], indicates that the frequency of C717S in ABCB4 is 0.000008239, making it exceedingly rare. We validated the same variant in the patient’s mother, who had also suffered from gallstones. Furthermore, the C717S in ABCB4 was predicted to be probably damaged by GERP++ [19]. Accordingly, we deemed that the C717S in ABCB4 caused disease.
Treat-to-target in patients with LPAC syndrome aims to prevent gallstone recurrence and progressive liver damage. For this purpose, ursodeoxycholic acid therapy has been shown to be effective in most patients [9]. Ursodeoxycholic acid is hypothesized to increase hydrophilic bile acid and to stimulate biliary secretion [20]. Recently, the cystic fibrosis transmembrane conductance regulator potentiator, ivacaftor, was reported to be a potential therapy in selected patients who harbor mutations in the ATP-binding site of ABCB4 [21].
In conclusion, ABCB4C717S was identified as a novel disease-causing variant in this first case report of a Japanese patient with LPAC syndrome. This diagnosis should be considered in young adults with recurrent cholesterol gallstones, splenomegaly, and a family history of relevant disease. When diagnosed, therapy with ursodeoxycholic acid should be initiated early to prevent recurrent gallstones and progressive liver damage.
References
Lammert F, Gurusamy K, Ko CW, et al. Gallstones. Nat Rev Dis Primers. 2016;2:16024.
Rosmorduc O, Poupon R. Low phospholipid associated cholelithiasis: association with mutation in the MDR3/ABCB4 gene. Orphanet J Rare Dis. 2007;2:29.
Gordo-Gilart R, Andueza S, Hierro L, et al. Functional analysis of ABCB4 mutations relates clinical outcomes of progressive familial intrahepatic cholestasis type 3 to the degree of MDR3 floppase activity. Gut. 2015;64:147–55.
Delaunay JL, Durand-Schneider AM, Dossier C, et al. A functional classification of ABCB4 variations causing progressive familial intrahepatic cholestasis type 3. Hepatology. 2016;63:1620–31.
Park HJ, Kim TH, Kim SW, et al. Functional characterization of ABCB4 mutations found in progressive familial intrahepatic cholestasis type 3. Sci Rep. 2016;6:26872.
Rosmorduc O, Hermelin B, Poupon R. MDR3 gene defect in adults with symptomatic intrahepatic and gallbladder cholesterol cholelithiasis. Gastroenterology. 2001;120:1459–67.
Gonzales E, Spraul A, Jacquemin E. Clinical utility gene card for: progressive familial intrahepatic cholestasis type 3. Eur J Hum Genet. 2014. https://doi.org/10.1038/ejhg.2013.188.
Poupon R, Rosmorduc O, Boëlle PY, et al. Genotype-phenotype relationships in the low phospholipid associated cholelithiasis syndrome: a study of 156 consecutive patients. Hepatology. 2013;58:1105–10.
Rosmorduc O, Hermelin B, Boëlle PY, et al. ABCB4 gene mutation-associated cholelithiasis in adults. Gastroenterology. 2003;125:452–9.
Smit JJ, Schinkel AH, Oude Elferink RP, et al. Homozygous disruption of the murine mdr2 P-glycoprotein gene leads to a complete absence of phospholipid from bile and to liver disease. Cell. 1993;75:451–62.
Wendum D, Barbu V, Rosmorduc O, et al. Aspects of liver pathology in adult patients with MDR3/ABCB4 gene mutations. Virchows Arch. 2012;460:291–8.
Tougeron D, Fotsing G, Barbu V, et al. ABCB4/MDR3 gene mutations and cholangiocarcinomas. J Hepatol. 2012;57:467–8.
Vij M, Safwan M, Shanmugam NP, et al. Liver pathology in severe multidrug resistant 3 protein deficiency: a series of 10 pediatric cases. Ann Diagn Pathol. 2015;19:277–82.
Tebbi A, Levillayer F, Jouvion G, et al. Deficiency of multidrug resistance 2 contributes to cell transformation through oxidative stress. Carcinogenesis. 2016;37:39–48.
Vij M, Shanmugam NP, Reddy MS, et al. Hepatocarcinogenesis in multidrug resistant P-glycoprotein 3 deficiency. Pediatr Transplant. 2017;21.
Mhatre S, Wang Z, Nagrani R, et al. Common genetic variation and risk of gallbladder cancer in India: a case-control genome-wide association study. Lancet Oncol. 2017;18:535–44.
Degiorgio D, Colombo C, Seia M, et al. Molecular characterization and structural implications of 25 new ABCB4 mutations in progressive familial intrahepatic cholestasis type 3 (PFIC3). Eur J Hum Genet. 2007;15:1230–8.
Lek M, Karczewski KJ, Minikel EV, et al. Analysis of protein-coding genetic variation in 60,706 humans. Nature. 2016;18:285–91.
Davydov EV, Goode DL, Sirota M, et al. Identifying a high fraction of the human genome to be under selective constraint using GERP++. PLoS Comput Biol. 2010;6:e1001025.
Poupon R. Ursodeoxycholic acid and bile acid mimetics as therapeutic agents for cholestatic liver diseases: an overview of their mechanisms of action. Clin Res Hepatol Gastroenterol. 2012;36:S3–12.
Delaunay JL, Bruneau A, Hoffmann B, et al. Functional defect of variants in the adenosine triphosphate-binding sites of ABCB4 and their rescue by the cystic fibrosis transmembrane conductance regulator potentiator, ivacaftor (VX-770). Hepatology. 2017;65:560–70.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Human/animal rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ishizawa, T., Makino, N., Kakizaki, Y. et al. A novel pathogenic variant of ATP-binding cassette subfamily B member 4 causing gallstones in a young adult. Clin J Gastroenterol 12, 637–641 (2019). https://doi.org/10.1007/s12328-019-00991-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-019-00991-x