Abstract
Purpose
The purpose of the study was to evaluate if during a common activity as walking, altered quadriceps muscular activity may be present in patellofemoral pain syndrome (PFPS) patients.
Methods
Forty subjects with clinically diagnosed PFPS and forty healthy males matching in age, weight, height and level of sport activity were enrolled in the study. Subjects were asked to walk on an instrumented walking path at their self-selected speed. Force platform and motion tracking system were used for the analysis of the gait. Wireless surface EMG probes were used to evaluate quadriceps muscles activity. Rectus femoris, vastus medialis and lateralis activity percentage, onset and offset time, walking speed, cadence, step length, stride length, knee ROM during gait were measured and reported. Tegner activity questionnaire was reported.
Results
Patient group showed a significant increasing in all quadriceps muscles activity when compared to the control (p < 0.05). In particular, for VM and VL muscle onset time was anticipated and offset time was postponed in PFPS group when compared with healthy group (p < 0.05). Knee range of motion during walking was significantly decreased in the patient group.
Conclusions
Young athletes with PFPS showed increased length of quadriceps muscles activity and reduced functional knee Rom while walking, comparing with healthy subjects, in particular muscular onset was anticipated in respect of the loading response event of the gait. Nonetheless, walking parameters were not affected by these alterations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patellofemoral pain syndrome (PFPS) is one of the most common musculoskeletal disorders, that commonly affects young athletes (18–35 years), especially women [1–4].
It is defined as an anterior knee or rear of patella aspecific pain [5–7], which onset is often related to activities such as stair climbing, squatting, kneeling and prolonged sitting [1, 8].
Although the etiological factors of PFPS are not defined, it has been shown that most important causes of PFPS are abnormalities of patellofemoral biomechanics, in particular increased Q-angle, patellar maltracking and alterations of lower limb axis, such as excessive foot pronation and excessive external torsion [1, 3, 9, 10].
Anatomical studies described the aponeurosis between the tendons of vastus medialis (VM), vastus intermedius (VI) and medial patellofemoral ligament (MPFL) [11]. Their fibers merge at the patellar insertion creating an inseparable aponeurosis that moves the patella during the quadriceps contractions [12, 13]. This has led to think that muscle functional alterations or impairments for the VM and vastus lateralis (VL) muscles maybe related to PFPS.
Reduction in the force-production capabilities of the VM it has been hypothesized as a possible cause of the syndrome, in particular the VM cannot antagonize the VL, resulting in patellar maltracking [14–16].
Difference in contraction intensity, timing and onset activation of the quadriceps muscles, in particular VM and VL muscles, have been proposed as possible cause of patellar maltracking [8, 10, 17–20]. Consequently, researchers investigated different tasks and condition comparing EMG timing and onset of activation, mostly for VM and VL muscles, between PFPS subjects and control. EMG activity was evaluated during functional activities as walking [19, 21], running [22] and stair ascent and descent [19, 21, 23], but contrasting results were found. Moreover, contrasting results were found also when other activities, such as extensor muscles exercises [24–28], open [29] and close kinetic [2, 30, 31] quadriceps exercises, reflex response tests [20, 32] and squatting [24, 25], were evaluated.
These contrasting results seemed to be due to the variability of subjects groups, in particular patients with different symptoms and condition may have been grouped together, as highlighted by other researchers [19]. In addition, small sample size [2, 32, 33] and difference in onset time detection method [15, 20–22, 32–34] may have influenced the results.
The purpose of this study is to evaluate if competitive young male athletes with diagnosed PFPS will show alterations in the quadriceps muscular activity as a response to the pain during a common activity as walking.
We hypothesized that patients will increase length of muscular activity while walking, anticipating onset and postponing offset of muscular contraction for quadriceps muscles comparing to healthy subjects.
Materials and methods
Participants
Forty male subjects with clinically diagnosed PFPS and forty healthy males matching in age, weight, height (Table 1) were enrolled in the study. Furthermore, all subjects have the same level of sport activity, measured with the Tegner score. Participants in both groups were excluded if neurological disorders, MMSE <26, history of knee extensor muscles injuries and knee surgery were present. Exclusion criteria for healthy participants were knee pain or any disorder in the last 12 months that had interfered with regular physical activity.
Inclusion criteria for PFPS subjects were presence of pain (at least score 3 from VAS) in the last month, onset of pain while performing at least 2 functional activities [8], detection of at least 3 sign or symptoms as previously described [9].
All subjects were asked to read and sign an informed consent form prior to their inclusion in the study.
Clinical evaluation
A clinical evaluation was performed to all subjects by the same clinician, and all participants were asked to compile a Tegner activity questionnaire in order to evaluate the level of physical activity. PFPS subjects were asked to indicate their activity level (Tegner score) also before the onset of the symptoms. PFPS subjects were asked to indicate the level of pain using the visual analog scale (VAS) for pain.
Experimental protocol
Opto-electric motion tracking system (Vicon, Oxford Metrics Ltd, UK), consisting of 10 infrared cameras, was used to evaluate lower limbs kinematics and spatiotemporal parameters during gait. Two force platforms (AMTI, MA, USA) embedded on the floor were used to record ground reaction force during walking. Data were acquired at a sampling rate of 250 Hz.
Electrical activity of the muscles was detected using a wireless bipolar surface EMG (BTS FREEEMG 300, Milano, Italy) with 10 GΩ input impedance and acquired with a sampling rate of 1000 Hz. Dedicated software (BTS EMG analyzer 300, Milano, Italy) was used for data collection and visualization.
Firstly, the subjects were equipped with reflective markers which were placed on the subjects legs following the Vicon plug-in gait markerset [35]. Then EMG probes were placed bilaterally on the VM, VL and RF muscles. Skin was shaved and prepared with methylated spirits and sandpaper. The electrode for VM muscle was placed at 80% on the line between the anterior spina iliaca superior and the joint space in front of the anterior border of the medial ligament. The electrode for RF muscle was placed at 50% on the line from the anterior spina iliaca superior to the superior part of the patella. The electrode for VL muscle was placed at 2/3 on the line from the anterior spina iliaca superior to the lateral side of the patella [36].
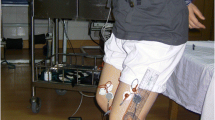
Subjects initially performed a static trial, standing with the arms folded across the chest and staying still for 5 s. After the static trial, subjects were asked to walk on the 15-meter instrumented walking path in the biomechanical laboratory at their self-selected normal walking speed until three successful trials were collected (Fig. 1).
Data analysis
Force platform data were used to define temporal events such as initial contact and toe-off of both sides. Markers trajectories were processed using the biomechanical model Vicon Plug-in-Gait (Oxford Metrics) biomechanical modeling software to get kinematics profiles. Kinematics data were normalized using a complete gait cycle, starting from the ground contact of one foot to the successive ground contact of the same foot.
Knee range of motion (ROM) in the sagittal plane was calculated as the differences between the maximum and minimum peaks during a gait cycle. Spatiotemporal parameters, including walking speed, cadence, step length, stride length, stance and swing percentage of gait cycle, were evaluated for each trial.
EMG data were analyzed; in particular, EMG data were band-pass filtered (fifth-order Butterworth filter 10–500 Hz) and then rectified. The linear envelope was obtained by applying a low-pass filter (fifth-order Butterworth filter with 4 Hz cut-off) and an amplitude normalization was obtained using the mean dynamic activity method [37], whereby the mean of the linear envelope was calculated and considered as 100% of the amplitude.
The onset and the offset of each muscle were calculated as previously described by Freddolini et al. [38]: firstly, a threshold was calculated as the sum of the mean of the EMG data recorded during resting plus 3 standard deviation (SD) of that mean. Onset of EMG activity was detected when the signal exceeded this threshold for at least 150 ms. Offset time was detected using the same threshold but analyzing the EMG signal from the end of a contraction.
Muscle was considered active between the onset and offset times. For VM and VL muscle onset (VMon and VLon) and offset (VMoff and VLoff) times were reported, normalized by the gait cycle duration. As the RF muscles presented an additional activation approximately at toe-off, two onsets (RFon and RFTOon) and two offsets times (RFoff and RFTOoff) were reported for this muscle. VM, VL and RF total onset duration times (VM%, VL% and RF%) were expressed as percentage of the gait cycle.
Statistical analysis
The Shapiro–Wilks test and the Levene’s Test for Equality of Variances were used to confirm that the assumptions of normality and homogeneity of variance of the statistical model were met for all variables analyzed. Independent T test was used to assess between groups comparison. Paired T test was used to evaluate differences for the Tegner score in the PFPS group before and after symptoms offset and to evaluate differences between VMon and VLon percentage in the same group. Level of significance was set at 0.05. Effect size calculation was performed using the Cohen’s d coefficient for all significant comparisons [39].
Results
Tegner score was not significantly different when PFPS group score prior the symptoms (7.2 ± 1.1) was compared to healthy subjects (7.7 ± 1.5), indicating a similar activity level (p > 0.05). The Tegner score was significantly different when the PFPS score regarding activity after symptoms onset group (4.5 ± 1.5) was compared to healthy group (p = 0.008, Cohen’s d = 2.13) and to the PFPS group score before symptoms onset (p = 0.010, Cohen’s d = 2.05), showing that as a result of the injury, patients decreased significantly their level of physical activity. Spatiotemporal gait parameters were not significantly different in the two groups (p > 0.05, Table 2). Knee ROM significantly decreased in the PFPS group when compared with control (p = 0.000, mean difference = 5.1°, Cohen’s d = 1,21; Table 2). EMG results for VM and VL muscles are summarized in Fig. 2. Significant differences were found when comparing EMG parameters in these two groups; in particular, VM% (p = 0.000, mean difference = 17.49%, Cohen’s d = 2.59), VL% (p = 0.000, mean difference = 8.91%, Cohen’s d = 1.11) and RF% (p = 0.000, mean difference = 11.80%, Cohen’s d = 1.54) significantly increased in the PFPS group as it is shown in Table 3. Moreover, as reported in Table 3, VMon (p = 0.000, mean difference = 6.38%, Cohen’s d = 2.26), VLon (p = 0.000, mean difference = 4.35%, Cohen’s d = 1.44) and RFon (p = 0.011, mean difference = 2.93%, Cohen’s d = 0.78) onset times were significant different, indicating an earlier activation of these muscles during gait cycle in the PFPS group when compared to healthy subjects. In addition, VMoff (p = 0.000, mean difference = 10.95%, Cohen’s d = 2.47), VLoff (p = 0.000, mean difference = 7.35%, Cohen’s d = 1.42) and RFoff (p = 0.010, mean difference = 5.02%, Cohen’s d = 0.80) offset times were also significant different, indicating later deactivation of these muscles during gait cycle in the PFPS group when compared to healthy subjects (Table 3). On the other hand, no significant difference was found for RFTOon and RFTOoff times between the two groups (p > 0.05, Table 3). No significant difference was present when comparing VMon and VLon time in both control and PFPS groups (p > 0.05).
Onset and Offset of the EMG activity for the vastus medialis (VM) and vastus lateralis (VL) muscles during gait for control and PFPS group. Onset are indicated by the left edge of the horizontal bar, while offset by the right edge of the horizontal bar. Error bars indicate standard deviation. Zero percent of gait cycle (GC) indicates initial contact. *Indicates significant difference (p < 0.05) between control and PFPS groups
Discussion
Patients with PFPS have to be examined carefully with regard to functional causes [40] and the treatment, that is always non-operative, should address the etiological causes.
Objective biomechanical outcomes, such as surface EMG, can help clinicians in evaluating functional alterations in PFPS.
In our study focusing on competitive athletes with PFPS, we evaluated if the electrical activity of the quadriceps muscle group could be altered as a result of the patellar pain.
Our results showed that RF, VM and VL muscles were activated for longer time in the patients group when compared to healthy group. In particular, the quadriceps muscle group activated earlier and de-activated later in the PFPS group when compared to healthy control. In addition, PFPS group showed reduced knee ROM during this activity.
Previous studies showed contrasting results comparing to the current study; Powers and co-workers [21] showed no significant difference in the VM and VL onset/offset timing between PFPS and control. This may be due to differences in EMG onset detection method, in the population investigated, as Powers et al. [21] evaluated female participants. In addition, there was no indication about the activity level of the subjects, as we evaluate competitive athletes that may be difficult to be compared to general population. Conversely, similar results were found by mohr et al. [19] and VL and VM length of activation was found in PFPS for walking and stair ascending as a response of the pain.
Results can be explained as a compensatory strategy in response to the pain, which it was applied in an everyday life activity such as walking. As it is often seen in other anatomical districts, or in other diseases, muscle contraction is directly related to pain sensation: Stabilizing the joint with muscle contraction may lead to a pain reduction [38, 41–43]. The knee ROM reduction, combined with the increased muscle activity, may be a strategy to increase joint stiffness, which, in turn, limits motion, decreasing risks of further damage and pain [43].
It needs to be highlighted that differences in muscle activation and knee ROM did not alter gait parameters such as walking speed, cadence, step length, stride length, stance and swing percentage of gait cycle, implying that this compensatory strategy did not interfere with gait performance.
It could be also possible that these alterations may be the cause of the pain, adding more compressive load and reducing femoral contact area, which, in turn, increased load in the knee joint. Quadriceps muscles alterations may indicate also a reduction in the neuromuscular efficiency in PFPS group as they required earlier activation to prepare the limb for the loading response and delayed deactivation after push off.
As a limitation, the present research was a cross-sectional study and it was not able to evaluate the cause and effect association between pain and EMG alterations, that it should be investigated in the future. Pain and muscular alteration may operate in circle, reinforcing each other, with persisting of pain and leading to chronic condition such as knee OA. In this case, a combination of pain reliefs and muscle restoring exercise treatment may be useful to interrupt this circle and reduce symptoms. In particular, muscles can be retrained to perform the movements correctly, with the right timing of muscle activation and correcting the sporting gesture. Moreover, PFPS is a complex syndrome, caused by different cofactors, such as abnormalities of patellofemoral biomechanics and alterations of lower limb axis. For this reason, it may be essential to identify these alterations and design a complete rehabilitation program, which may include specific exercises, sport devices and specific training to restore both muscular and biomechanical alteration of the lower limbs, resulting in clinically important reduction of pain, improvement in functional ability and muscle functioning [3, 44].
Limitation of this study was that patients group was limited to male athletes, and it may be difficult to be compared with similar previous studies that involved mainly female participants and different level of activity. Further longitudinal studies are required to evaluate these parameters in other population and for other activities.
Conclusion
Young athletes with PFPS showed increased length of quadriceps muscles activity and reduced functional knee Rom while walking, comparing with healthy subjects, in particular muscular onset was anticipated in respect of the loading response event of the gait. Nonetheless, walking parameters were not affected by these alterations.
References
Bevilaqua-Grossi D, Felicio LR, Leocádio LP (2008) Analysis of the reflex response time of the patellar stabilizer muscles in individuals with patellofemoral pain syndrome. Braz J Phys Ther 12:26–30. doi:10.1590/S1413-35552008000100006
Cerny K (1995) Vastus medialis oblique/vastus lateralis muscle activity ratios for selected exercises in persons with and without patellofemoral pain syndrome. Phys Ther 75:672–683
Rothermich MA, Glaviano NR, Li J, Hart JM (2015) Patellofemoral pain: epidemiology, pathophysiology, and treatment options. Clin Sports Med 34:313–327. doi:10.1016/j.csm.2014.12.011
Roush JR, Curtis Bay R (2012) Prevalence of anterior knee pain in 18–35 year-old females. Int J Sports Phys Ther 7:396–401
Biedert RM, Warnke K (2001) Correlation between the Q angle and the patella position: a clinical and axial computed tomography evaluation. Arch Orthop Trauma Surg 121:346–349
Powers CM, Maffucci R, Hampton S (1995) Rearfoot posture in subjects with patellofemoral pain. J Orthop Sports Phys Ther 22:155–160. doi:10.2519/jospt.1995.22.4.155
Wilk KE, Reinold MM (2001) Principles of patellofemoral rehabilitation. Sports Med Arthrosc Rev 9:325–336. doi:10.1097/00132585-200110000-00010
Cowan SM, Bennell KL, Hodges PW et al (2001) Delayed onset of electromyographic activity of vastus medialis obliquus relative to vastus lateralis in subjects with patellofemoral pain syndrome. Arch Phys Med Rehabil 82:183–189. doi:10.1053/apmr.2001.19022
Coqueiro KRR, Bevilaqua-Grossi D, Bérzin F et al (2005) Analysis on the activation of the VMO and VLL muscles during semisquat exercises with and without hip adduction in individuals with patellofemoral pain syndrome. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol 15:596–603. doi:10.1016/j.jelekin.2005.03.001
Insall J (1982) Current Concepts Review: patellar pain. J Bone Joint Surg Am 64:147–152
Davis IS, Powers CM (2010) Patellofemoral pain syndrome: proximal, distal, and local factors, an international retreat, April 30-May 2, 2009, Fells Point, Baltimore, MD. J Orthop Sports Phys Ther 40:A1–16. doi:10.2519/jospt.2010.0302
Placella G, Tei M, Sebastiani E et al (2015) Anatomy of the Medial Patello-Femoral Ligament: a systematic review of the last 20 years literature. Musculoskelet Surg 99:93–103. doi:10.1007/s12306-014-0335-y
Placella G, Tei MM, Sebastiani E et al (2014) Shape and size of the medial patellofemoral ligament for the best surgical reconstruction: a human cadaveric study. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 22:2327–2333. doi:10.1007/s00167-014-3207-y
Fagan V, Delahunt E (2008) Patellofemoral pain syndrome: a review on the associated neuromuscular deficits and current treatment options. Br J Sports Med 42:789–795. doi:10.1136/bjsm.2008.046623
Witvrouw E, Sneyers C, Lysens R et al (1996) Reflex response times of vastus medialis oblique and vastus lateralis in normal subjects and in subjects with patellofemoral pain syndrome. J Orthop Sports Phys Ther 24:160–165. doi:10.2519/jospt.1996.24.3.160
Ahmed AM, Burke DL, Hyder A (1987) Force analysis of the patellar mechanism. J Orthop Res Off Publ Orthop Res Soc 5:69–85. doi:10.1002/jor.1100050110
Chen H-Y, Chien C-C, Wu S-K et al (2012) Electromechanical delay of the vastus medialis obliquus and vastus lateralis in individuals with patellofemoral pain syndrome. J Orthop Sports Phys Ther 42:791–796. doi:10.2519/jospt.2012.3973
Bennett JG, Stauber WT (1986) Evaluation and treatment of anterior knee pain using eccentric exercise. Med Sci Sports Exerc 18:526–530
Mohr KJ, Kvitne RS, Pink MM et al (2003) Electromyography of the quadriceps in patellofemoral pain with patellar subluxation. Clin Orthop. doi:10.1097/01.blo.0000093918.26658.6a
Voight ML, Wieder DL (1991) Comparative reflex response times of vastus medialis obliquus and vastus lateralis in normal subjects and subjects with extensor mechanism dysfunction. An electromyographic study. Am J Sports Med 19:131–137
Powers CM, Landel R, Perry J (1996) Timing and intensity of vastus muscle activity during functional activities in subjects with and without patellofemoral pain. Phys Ther 76:946-955-967
MacIntyre DL, Robertson DG (1992) Quadriceps muscle activity in women runners with and without patellofemoral pain syndrome. Arch Phys Med Rehabil 73:10–14
Rathleff MS, Samani A, Olesen JL et al (2013) Neuromuscular activity and knee kinematics in adolescents with patellofemoral pain. Med Sci Sports Exerc 45:1730–1739. doi:10.1249/MSS.0b013e318292be30
Hwangbo P-N (2015) The effects of squatting with visual feedback on the muscle activation of the vastus medialis oblique and the vastus lateralis in young adults with an increased quadriceps angle. J Phys Ther Sci 27:1507–1510. doi:10.1589/jpts.27.1507
Souza DR, Gross MT (1991) Comparison of vastus medialis obliquus: vastus lateralis muscle integrated electromyographic ratios between healthy subjects and patients with patellofemoral pain. Phys Ther 71:310–316
Boucher JP, King MA, Lefebvre R, Pépin A (1992) Quadriceps femoris muscle activity in patellofemoral pain syndrome. Am J Sports Med 20:527–532
Doxey G, Eisenman P (1987) The influence of patellofemoral pain on electromyographic activity during submaximal isometric contractions. J Orthop Sports Phys Ther 9:211–216
Møller BN, Krebs B, Tidemand-Dal C, Aaris K (1986) Isometric contractions in the patellofemoral pain syndrome. An electromyographic study. Arch Orthop Trauma Surg Arch Für Orthop Unf-Chir 105:24–27
Felicio LR, Baffa ADP, Liporacci RF et al (2011) Analysis of patellar stabilizers muscles and patellar kinematics in anterior knee pain subjects. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol 21:148–153. doi:10.1016/j.jelekin.2010.09.001
Reynolds L, Levin TA, Medeiros JM et al (1983) EMG activity of the vastus medialis oblique and the vastus lateralis in their role in patellar alignment. Am J Phys Med 62:61–70
Stiene HA, Brosky T, Reinking MF et al (1996) A comparison of closed kinetic chain and isokinetic joint isolation exercise in patients with patellofemoral dysfunction. J Orthop Sports Phys Ther 24:136–141. doi:10.2519/jospt.1996.24.3.136
Karst GM, Willett GM (1995) Onset timing of electromyographic activity in the vastus medialis oblique and vastus lateralis muscles in subjects with and without patellofemoral pain syndrome. Phys Ther 75:813–823
Sheehy P, Burdett RG, Irrgang JJ, VanSwearingen J (1998) An electromyographic study of vastus medialis oblique and vastus lateralis activity while ascending and descending steps. J Orthop Sports Phys Ther 27:423–429. doi:10.2519/jospt.1998.27.6.423
Morrish GM, Woledge RC (1997) A comparison of the activation of muscles moving the patella in normal subjects and in patients with chronic patellofemoral problems. Scand J Rehabil Med 29:43–48
Davis RB III, Õunpuu S, Tyburski D, Gage JR (1991) A gait analysis data collection and reduction technique. Hum Mov Sci 10:575–587. doi:10.1016/0167-9457(91)90046-Z
Hermens HJ, Freriks B, Disselhorst-Klug C, Rau G (2000) Development of recommendations for SEMG sensors and sensor placement procedures. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol 10:361–374
Yang JF, Winter DA (1984) Electromyographic amplitude normalization methods: improving their sensitivity as diagnostic tools in gait analysis. Arch Phys Med Rehabil 65:517–521
Freddolini M, Strike S, Lee RYW (2014) The role of trunk muscles in sitting balance control in people with low back pain. J Electromyogr Kinesiol 24:947–953. doi:10.1016/j.jelekin.2014.09.009
Cohen J (1988) Statistical power analysis for the behavioral sciences. Lawrence Erlbaum Associates Publishers, New York, NY
Petersen W, Ellermann A, Gösele-Koppenburg A et al (2013) Patellofemoral pain syndrome. Knee Surg Sports Traumatol Arthrosc 22:2264–2274. doi:10.1007/s00167-013-2759-6
Graven-Nielsen T, Svensson P, Arendt-Nielsen L (1997) Effects of experimental muscle pain on muscle activity and co-ordination during static and dynamic motor function. Electroencephalogr Clin Neurophysiol Mot Control 105:156–164. doi:10.1016/S0924-980X(96)96554-6
Souza RB, Powers CM (2009) Differences in hip kinematics, muscle strength, and muscle activation between subjects with and without patellofemoral pain. J Orthop Sports Phys Ther 39:12–19. doi:10.2519/jospt.2009.2885
Childs JD, Sparto PJ, Fitzgerald GK et al (2004) Alterations in lower extremity movement and muscle activation patterns in individuals with knee osteoarthritis. Clin Biomech Bristol Avon 19:44–49
van der Heijden RA, Lankhorst NE, van Linschoten R, et al (2015) Exercise for treating patellofemoral pain syndrome. Cochrane Database Syst Rev 1:CD010387. doi: 10.1002/14651858.CD010387.pub2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Freddolini, M., Placella, G., Gervasi, G.L. et al. Quadriceps muscles activity during gait: comparison between PFPS subjects and healthy control. Musculoskelet Surg 101, 181–187 (2017). https://doi.org/10.1007/s12306-017-0469-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-017-0469-9