Abstract
Purpose
The aim of this study is to report the clinical and radiological results of reverse total shoulder arthroplasty (rTSA) in elderly patients who have been treated for complex humeral fractures.
Materials and methods
From January 2005 to December 2014, we have implanted rTSA for proximal humeral fractures in 95 patients (80 womens, 15 mens) about 75 years old on average (range 62–95 years). All rates and results on intraoperative and postoperative complications have been collected in a specific database. In all cases we have used a modular implant prosthesis (Lima Corporate, San Daniele del Friuli, Italy). The prosthesis was implanted cementless in 92 cases. Because of the presence of a high percentage of comorbidities in the elderly patients, we have retrospectively analyzed the necessity of a secondary hospitalization, from a week to a 6-month time after the discharge, due to general health problems and specific postoperative shoulder complications. The mean follow-up was 5 years (range 1–9 years) for 70 of 95 patients, 50 of whom had adequate radiographic controls.
Results
None of 95 patients has required a reoperation or a hospitalization for general health problems from 1 week to 6 months postoperative. No early or late infection of prosthesis has been observed. There were seven cases of perioperative complications, three humeral vertical bone fissuring, two glenoid fractures and two cases of deltoid muscle damage. We have had three cases of postoperative hematoma and one case of ulnar nerve neuropathy. The mean constant score was 85.4, and the mean simple shoulder test was 7.4. We have observed a grade 1 scapular notching in 15 cases (30 %). In the remaining 35 reviewed cases, there was no notching. Peri-articular heterotopic ossifications were found in 11 cases (22 %).
Conclusion
Reverse shoulder prosthesis in complex humeral fractures in the elderly can be considered as a reliable surgical procedure, which leads to very good clinical and radiological results in case of cementless prosthesis, as well.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Proximal humeral fractures represent 6–8 % of all fractures, and most of them are low-energy osteoporotic injuries in the elderly patients; moreover, their incidence is increasing in the light of an ageing population. The diversity of fracture patterns encountered renders objective classification of prognostic value challenging. Absolute indications for surgery are infrequent and include comminuted head-splitting fractures, fracture dislocations and three- to four-part displaced fractures. A constantly expanding range of reconstructive and replacement options, however, is extending the indications for surgical management of complex proximal humerus fractures, also in elderly patients. As such, a wide range of fracture patterns has been described [1, 2], making accurate and reproducible classification of prognostic value complex and difficult.
Neer’s classification [2] remains the most commonly used system [3]. Additional classification systems have been described recently, and they can give very useful indications to the surgeon for the type of surgery to adopt [4].
In the last decade reverse total shoulder arthroplasty (rTSA) has been utilized to treat complex proximal humeral fractures and their sequelae [5]. Few studies, regarding this difficult topic, have been made with a large number of patients [5, 6]. There are controversial opinions about the age of implant, surgical techniques, prosthesis design, tuberosities management, cemented or cementless stem and complications rate.
On one side some studies report a high rate of complications, from 14 to 75 % [5]; on the other side some studies describe few complications and no required reoperation also in the learning phase [6].
The aim of this study is to report our clinical and radiological results and complications of rTSA implanted in the elderly patients.
Materials and methods
From January 2005 to December 2014, 95 rTSA were implanted by the senior author (RR) for complex proximal humeral fractures. The patients’ average age was 75 years (range 62–95 years). Before the implant, X-rays according to trauma series and CT scan were taken in all patients. In 19 of them (20 %), a grade III/IV fatty degeneration [7] of rotator cuff muscles was found. One patient (1.4 %) suffered from chronic supraspinatus calcification (Fig. 1a, b), 12 (12.6 %) from rotator cuff tear arthropathy and two (2.1 %) from concentric osteoarthritis. We have analyzed retrospectively the rate of postoperative general complications from 1 week to 6 months after the prosthetic implant but also perioperative and postoperative shoulder complications and the clinical and radiological results. We have followed 70 of 95 (73.6 %) treated patients with a minimum follow-up of 1 year; 12 of them were excluded because they had been operated less than 12 months before, five were died, and eight were lost at follow-up.
Of these 70 patients, 50 (6 mens and 44 womens) were evaluated by the constant score and shoulder’s X-ray; moreover, 15 among the 50 patients also had a CT scan. The remaining 20 patients were called and evaluated by a simple shoulder test.
A Lima rTSA (Lima Corporate, San Daniele del Friuli, Italy) has been implanted in all patients, and in all cases we used a 36-mm glenosphere. We have practiced a deltopectoral approach in all patients, because we found it very comfortable for the glenoid baseplate implant. A 36-mm glenosphere, which was always flush with the inferior border of glenoid, has been implanted in all cases, and the baseplate inclination was systematically with a 5°–10° inferior tilt. A cemented humeral stem has been used in three cases (3.2 %); in the others it was cementless.
Operative technique
Through the deltopectoral space the long head of biceps was identified and followed until the glenoid tubercle, by opening the rotator interval. The two tuberosities were tagged with two non-absorbable sutures. In most of the cases the supraspinatus tendon was present and it was released till the muscular junction. The separation of the two tuberosities allowed to remove easily the humeral head and identify the several humeral fracture patterns. A complete glenoid circumferential capsulotomy was made, and the triceps tendon was partially released in order to allow the scapular pillar’s exposition. The glenoid surface was gently refined avoiding exposure of glenoid cancellous bone, and the base plate was implanted flush with the inferior glenoid edge. A 36-mm glenosphere has been always implanted on it.
The surgical technique used for tuberosities reconstruction is based on the technique described by Brems in acute fractures treated with hemiarthroplasty, called the “puzzle pieces” [8]. In this technique the intraoperative surgical reconstruction requires a detailed knowledge of the osseous and muscular anatomy and physiology. The proximal humerus must be reconstructed in a way that establishes proper humeral head version and proper myofascial sleeve tension within the rotator cuff and deltoid musculature. Tuberosity placement and fixation techniques are emphasized, recognizing that anatomic restoration of the cuff is crucial if the patient is to achieve a pain-free and functional limb after joint arthroplasty for fracture.
We gave a great emphasis to the “puzzle” reconstruction of small fragments as well, using osteo-sutures and cancellous chips graft below the tuberosity, Fig. 2.
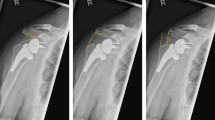
Sixty patients were treated with this reconstruction of the tuberosities (Brems’ technique). In 2008 we modified the Brems’ technique [8], with BCAT (bone collar and tie) technique [9] in order to improve the bone quantity around the humeral prosthesis especially in case of comminuted greater tuberosity fractures and in order to improve bone healing. The BCAT technique consists in the use of the fractured humeral head, appropriately modeled and placed collar like around the prosthesis and under the tuberosities (Fig. 3).
This bone support functions mechanically and biologically to improve cuff tension moving it laterally. By this technique we improve the healing of tuberosities and the shoulder rotations. Thirty-five patients have been treated with this technique of reconstruction of the tuberosities since 2008. All treated patients were immobilized with an adduction sling arm for 3–4 weeks.
Rehabilitation
The mean time of immobilization in sling was 23 days, but the patients were allowed to move passively their arm 2 days after surgery. Hydrokinesitherapy was started 4 weeks after surgery in 70 % of patients, in the same rehabilitation center following a specific protocol: For the first 2 months a passive rehabilitation was done to reach the highest anterior elevation, and then they worked on the improvement of external rotation. In 30 % of cases the passive rehabilitation and then active rehabilitation were started gradually after 4 weeks immobilization without a specific protocol, since the patients could not attend rehabilitation centers.
Results
In our series of 95 elderly patients, there was no case of second hospitalization due to general postoperative (cardiac, pulmonary, abdominal and hematological) complications in the 6 months following discharge.
About the clinical results, among the 50 patients with a minimum follow-up of 1 year the mean absolute constant score [10] was 73.6 (58.7–88.5), while the one adapted to the age was 89.5 (68.2–105.8). The mean SST score was 7.4 (6–12).
Perioperative complications included three humeral shaft fractures treated with cerclages, two glenoid fractures fixed with screws and cancellous bone from humeral head and two cases of deep damage of anterior bundle of the deltoid muscle. In one case we observed an ulnar neuropathy settled down after 1 year and three cases of postoperative hematoma that solved spontaneously.
No early or late infection of prosthesis has been observed.
Among the fifty patients with long clinical and radiographic follow-up, 28 operated from 2005 to 2007 were treated with Brems’ technique of tuberosity reconstruction and 22 with BCAT technique. In the first group of 28 patients (Brems’ technique), the average anterior flexion was 125° (90°–165°), abduction was 109° (65°–140°), external rotation in RE1 was 25° (0°–45°), and internal rotation was from lateral thigh to L5. In the other 22 cases treated using the BCAT technique, we observed an increased shoulder function especially in elevation with a mean forward elevation of 160° (120°–180°), a mean external rotation of 55° in RE1 and internal rotation at L4 (Table 1).
Radiological outcomes
Among the 50 patients with clinical and radiographic follow-up longer than 1 year, scapular notching according to Nerot classification [11] was grade 0 in 35 cases (70 %) (Fig. 4) and grade 1 in 15 cases (30 %). The scapular spur was observed in 11 cases (22 %). Peri-articular heterotopic ossifications were found in 11 (22 %) cases, but without limitation of the shoulder range of motion.
No case of radiolucency was observed on the glenoid base plate. In six patients a radiolucency bigger than 2 mm has been observed around the superior baseplate screw.
In our oldest patient (operated at 96 years), we have observed radiolucency in the superior and inferior baseplate screw at 3 years of follow-up.
In four cases of cementless stem, we observed a radiolucent line in 1–2–7 zone [11–17].
Partial lysis of the greater tuberosity was observed in 18 cases (36 %), 12 (24 %) operated with Brems’ technique and six (12 %) with BCAT technique (Fig. 5a, b).
Discussion
Reverse shoulder arthroplasty (rTSA) was originally described by Grammont [12], to treat eccentric shoulder arthropathy, but in the last decade its use to treat complex three- and four-part humeral head fractures in the elderly is increased. There are few significant studies in the literature (six retrospective and three prospective) with a small number of patients enrolled [13–15]. There are controversial opinions about the use of rTSA based on indications, age, implant design, surgical technique and approach and the high rate of complications reported [16, 17]. Actually the indications for rTSA in the elderly have widely expanded, and several recommendations on the patient selection have been reported, but there are still concerns about the use of this prosthesis among patients below 80 years old due to high rate complications. Deltopectoral or transdeltoid approach is still subjects of debate [18, 19]; we prefer the deltopectoral one for the deltoid muscles integrity and to have a proper exposure and view of the inferior part of the glenoid, leading to a good orientation and inferior implant of the glenosphere.
In the elderly due to a high incidence of osteoporosis, especially in women, it is not clear whether is better to use cemented or uncemented humeral stems. In our series we implanted cementless stems even in oldest patients and we did not observe any secondary problem. Obviously this concept is not widely valid especially in case of hidden diaphyseal fissuring, and to bring out this we recommend a special attention to CT scan images. In our experience we had to carry out preventive cerclage in three cases to avoid a very important intraoperative complication and we used a cemented stem in three cases due to a stability problem. Another important step to keep in mind during the diaphysis preparation is the planning of definitive implant height considering the assembling of prosthesis pieces, especially if the humeral system is modular. In our experience the Brems’ technique, initially used only in hemiarthroplasty [20], allows us to identify more precisely the real fragment position and the native height of metaphyseal bone. We estimated that the metallic component can be flush with the superior part of the greater tuberosity or exceed for a maximum 1 cm above this level. Assembling the trial stem and matching the humeral component with glenosphere, we can easily decide which type of polyethylene liner used (from 0 mm to 6 mm). One of the most feared complications reported is the secondary instability of the reverse prosthesis that can range between 3.5 and 30 % [16–18]. In our series we had no cases of secondary instability even in the first 20 cases deemed as learning curve. We think that the reason of this good result (0 % of secondary dislocation) was the attention for preserving and reconstructing carefully both tuberosities. In the first 20 cases we observed a modest external rotation recovery both in RE1 and in RE2 and a high incidence of greater tuberosity reabsorption (Fig. 5).
In 2008 we modified Brems’ technique in BCAT technique (bone collar and tie) in order to enhance the quantity of bone around the prosthesis posteriorly and laterally especially in case of comminuted fractures of the greater tuberosity; this technique led to preserve external rotation activity of teres minor and residual infraspinatus when tuberosities were healed around the prosthesis implant (Fig. 6a, b). The clinical results showed a statistically significant improvement in external rotation (mean 24°) in those treated with BCAT and at radiographic examination a lateralization of the greater tuberosity and a significant reduction in reabsorption of the great tuberosity.
We had a lower rate of deep infection (0 %) than reported in the literature (until 10 %) [21–23]. We performed all rTSA implants in a standard operative room without ultraviolet light or positive pressure ventilation and using perioperative antibiotic administration. Some studies underline the importance to use an antibiotic-impregnated cement and clorexidine lavage during the procedure [21–23], but in most of our patients we did not use both of them. We did not observe case of instability of rTSA in our series, while in the literature has been reported a high rate (from 3.5 to 31 %) [24].
The deltopectoral approach in our opinion allows to have a good exposition of the glenoid and managing properly its defects and replacement. The frequency and importance of scapular notching rate in our cases are lower than others in the literature [25], and especially in case of fractures we believe that a good balance of anterior and posterior tendons could be the key point to avoid this complication.
The strengths of this study are the fairly good number of patients treated by the same surgeon in a single unit where the patients were followed also during the rehabilitation time. Another important aspect is the clinical and radiological results observed in patients with osteoporosis (66 cases), all treated using cementless prosthesis with a low percentage of pain and high number of bone increase around the stem. The recovery of forward elevation and external rotation placing a bone augmentation under the teres minor was significant compared with the results reported in the literature [15–25]. This bone augmentation, as recently demonstrated biomechanically [26], may cause an increase in teres minor tension with a raise in its function.
The observation reported in the literature about the necessity to increase the glenosphere [27, 28] diameter up to 44 mm or change its morphology to better stabilize the prosthesis, to avoid scapular notching and increase the functional results especially in elevation, was not followed in our series, and we used in all cases a glenosphere with a classical shape and 36 mm diameter with no negative effect both on range of motion and on secondary instability. A limitation of this study is a missed control group treated with other technique and the number of patients lost at long follow-up, but to date the clinical and radiological results reached are very satisfying.
References
Robinson CM, Page RS (2003) Severely impacted valgus proximal humeral fractures. Results of operative treatment. J Bone Joint Surg Am 85-A:1647–1655
Neer CS (1970) Displaced proximal humeral fractures. I. Classification and evaluation. J Bone Joint Surg Am 52:1077–1089
Handoll HH, Ollivere BJ, Rollins KE (2012) Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev 12:CD000434
Russo R, Cautiero F, Della Rotonda G (2012) The classification of complex 4-part humeral fractures revisited: the missing fifth fragment and indications for surgery. Musculoskelet Surg 96(Suppl 1):S13–S19
Hatzidakis AM, Norris TR, Boileau P (2007) Reverse shoulder arthroplasty indications, technique, and results. Tech Shoulder Elbow Surg 16:e55
Sershon RA, Van Thiel GS, Lin EC, McGill KC, Cole BJ, Verma NN, Romeo AA, Nicholson GP (2014) Clinical outcomes of reverse total shoulder arthroplasty in patients aged younger than 60 years. J Shoulder Elbow Surg 23:395–400
Fuchs B, Weishaupt D, Zanetti M, Hodler J, Gerber C (1999) Fatty degeneration of the muscles of the rotator cuff: assessment by computed tomography versus magnetic resonance imaging. J Shoulder Elbow Surg 8:599–605
Brems JJ (2002) Shoulder arthroplasty in the face of acute fracture: puzzle pieces. J Arthroplasty 17(4 Suppl 1):32
Ciccarelli M, Russo R, Della Rotonda G, Cautiero F (2013) The “Bone-Collar-and-Tie” (BCAT). J Bone J Surg Br 93(II):202
Constant CR, Murley AHG (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 214:160–164
Valenti PH, Boutens D, Nerot C (2001) 2000 shoulder prostheses: two to ten year follow-up. In: Walch G, Boileau P, Molé D (eds.), Montpellier, Paris, France: Sauramps Medical. Delta 3 reversed prosthesis for osteoarthritis with massive rotator cuff tear: long term results. pp 253–259
Grammont PM, Baulot E (1993) Delta shoulder prosthesis for rotator cuff rupture. Orthopedics 16:65–68
Ross M, Hope B, Stokes A, Peters SE, McLeod I, Duke PF (2015) Reverse shoulder arthroplasty for the treatment of three-part and four-part proximal humeral fractures in the elderly. J Shoulder Elbow Surg 24(2):215–222
Jobin CM, Galdi B, Anakwenze OA, Ahmad CS, Levine WN (2015) Reverse shoulder arthroplasty for the management of proximal humerus fractures. J Am Acad Orthop Surg 23(3):190–201
Cazeneuve JF, Cristofari DJ (2014) Grammont reversed prosthesis for acute complex fracture of the proximal humerus in an elderly population with 5 to 12 years follow-up. Orthop Traumatol Surg Res 100(1):93–97
Groh GI, Groh GM (2014) Complications rates, reoperation rates and the learning curve in reverse shoulder arthroplasty. J Shoulder Elbow Surg 23:388–394
Walch G, Wall B, Mottier F (2006) Complications and revision of the reverse prosthesis, a multicenter study of 457 cases. In: Walch G, Boileau P, Molè D, Favard L, Lévigne C, Sirveaux F (eds) Reverse shoulder arthroplasty. Sauramp Medical, Montpellier, pp 335–352
Gillespie RJ, Garrigues GE, Chang ES, Namdari S, Williams GR Jr (2015) Surgical exposure for reverse total shoulder arthroplasty: differences in approaches and outcomes. Orthop Clin North Am 46(1):49–56
Molé D, Wein F, Dézaly C, Valenti P, Sirveaux F (2011) Surgical technique: the anterosuperior approach for reverse shoulder arthroplasty. Clin Orthop Relat Res 469(9):2461–2468
Russo R, Lombardi LV, Cautiero F, Giudice G, Ciccarelli M (2008) Medial reconstruction technique in the treatment of complex fractures of humeral proximal epiphysis with SMR prosthetic modular system. Chir Organi Mov 91(2):117–123
Nowinski RJ, Gillespie RJ, Shishani Y, Cohen B, Walch G, Gobezie R (2012) Antibiotic-loaded bone cement reduce deep infection rates for primary reverse total shoulder arthroplasty: a retrospective, cohort study of 501 shoulders. J Shoulder Elbow Surg 21:324–328
Cheung EV, Sperling JW, Cofield RH (2008) Infection associated with hematoma formation after shoulder arthroplasty. Clin Orthop Relat Res 466:1363–1367
Brown NM, Cipriano CA, Moric M, Sporer SM, Della Valle CJ (2012) Diluite betadine lavage before closure for the prevention of acute postoperative deep periprosthetic joint infection. J Arthroplasty 27:27–30
Boileau P, Melis B, Duperron D, Moineau G, Rumian AP, Han Y (2013) Revision surgery of reverse shoulder arthroplasty. J Shoulder Elbow Surg 22(10):1359–1370
Brorson S, Rasmussen JV, Olsen BS, Frich LH, Jensen SL, Hróbjartsson A (2013) Reverse shoulder arthroplasty in acute fractures of the proximal humerus: a systematic review. Int J Shoulder Surg 7:70–78
Budge MD, Moravek JE, Zimel MN, Nolan EM, Wiater JM (2013) Reverse total shoulder arthroplasty for the management of failed shoulder arthroplasty with proximal humeral bone loss: is allograft augmentation necessary? J Shoulder Elbow Surg 22(6):739–744
Langohr GD, Giles JW, Athwal GS, Johnson JA (2014) The effect of glenosphere diameter in reverse shoulder arthroplasty on muscle force, joint load, and range of motion. J Shoulder Elbow Surg (in press)
De Biase CF, Delcogliano M, Borroni M, Castagna A (2012) Reverse total shoulder arthroplasty: radiological and clinical result using an eccentric glenosphere. Musculoskelet Surg 96(Suppl 1):S27–S34
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Russo, R., Della Rotonda, G., Cautiero, F. et al. Reverse shoulder prosthesis to treat complex proximal humeral fractures in the elderly patients: results after 10-year experience. Musculoskelet Surg 99 (Suppl 1), 17–23 (2015). https://doi.org/10.1007/s12306-015-0367-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-015-0367-y