Abstract
Platelets undergo remarkable morphological changes during storage. Platelets change into different sizes and densities and differ in their biochemistry and functions. However, the correlation between structural heterogeneity and platelet autophagy is largely unknown. The aim of this study was to investigate the autophagy process in vitro, such as routine storage of platelets, and explore the role of reactive oxygen species (ROS) involved in the regulation of platelet autophagy. The ROS and autophagy levels of platelet concentrates from apheresis platelets were evaluated through flow cytometry. The expression levels of autophagy-associated proteins (LC3I, LC3II, Beclin1, Parkin, and PINK1) were measured via Western blot. All biomarkers were dynamically monitored for seven days. Moreover, the morphological characteristics of platelet morphology during storage were analyzed through transmission electron microscopy (TEM). Flow cytometry showed that the levels of total cell ROS and mitochondria ROS increased in the stored platelets. Together with the increase in mitochondrial ROS, the autophagy signal LC3 in the platelets was strongly amplified. The number of swollen platelets (large platelets) considerably increased, and that of autophagy signal LC3 was remarkably higher than that of the normal platelets. Western blot revealed that the expression levels of Beclin1 and LC3 II/LC3 I ratio were enhanced, whereas those of Parkin and PINK1 almost did not change during the seven days of storage. The existence of autophagosomes or autophagolysosomes in the platelets at the middle stage of platelet storage was observed via TEM. Our data demonstrated that the subpopulation of large (swollen) platelets exhibited different autophagy patterns. Furthermore, increased platelet autophagy was associated with mitochondrial ROS. These preliminary results suggest that swelling platelets have a higher autophagy pattern than normal platelets during storage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Platelets are characterized as anucleate hemocytes with a short life span in mammal vessels; they play key roles in hemostasis, thrombosis, inflammation, immunity, and host defense [1, 2]. They are derived from megakaryocytes and only live for 7–10 days in the bloodstream. Apheresis platelets placed in a polyolefin container with high oxygen permeability can be stored for up to 5 days in vitro. Stored platelets develop storage lesions that limit their survival in vitro [3], and these lesions are manifested as biochemical, morphological, and functional changes in platelets. These changes lead to decreased efficacy of platelet transfusion and may contribute to the development of adverse reactions in recipients.
Autophagy is recognized as a survival pathway that is closely related to cellular responses to stress, such as reactive oxygen species (ROS) [4]. ROS is essential for autophagy and promotes platelet storage lesion (PSL) by encouraging platelet degranulation and oxidative damage [5].
Under pathological conditions, dysfunctional mitochondria produce numerous ROS, thus destroying cell homeostasis. The process of removing damaged mitochondria by autophagy is called mitophagy, and it is essential for maintaining cell functions [6, 7]. Autophagy and mitophagy are important cellular processes responsible for removing excess ROS and damaged organelles.
Exposure to high levels of ROS is associated with platelet activation and aggregation, and platelet activation is the pivotal cause of PSL [6, 8]. However, a basal autophagy process, which is critical for normal platelet activation and aggregation, has been demonstrated to appear in platelets from healthy people [7, 9, 10]. The autophagy that occurs in platelets can be induced by starvation and rapamycin [7, 9]. Moreover, a substantial mitophagy induction (i.e., above basal autophagy levels) in diabetic platelets has been reported [11]. Mitophagy protects platelets against substantial oxidative stress and platelet apoptosis by removing damaged mitochondria.
LC3 and Beclin1 are considered as the basis and markers of autophagy. LC3 is the homolog of Atg8 in mammals [12], and it is also known as microtubule-associated protein 1 light chain 3 (map1lc3), which includes two mutually convertible forms: LC3-I and LC3-II. They participate in the formation of autophagosome membranes. LC3-I (localized in the cytoplasm) is coupled with the substrate PE on the surface of an autophagosome membrane, forming a membrane-bound form of LC3-II. LC3-II is an important marker molecule of autophagosomes, and the expression levels of LC3-II are significantly upregulated under autophagy with the increase in autophagosome membrane. Beclin1 is a central player in autophagy and constitutes a molecular platform for the regulation of autophagosome synthesis and maturation. Beclin1 acts as an overall scaffold for the PI3K complex, facilitating the localization of autophagic proteins to the phagophore [13]. PINK1/Parkin mitophagy is a key mechanism that contributes to mitochondrial quality control [14]. PINK1 and Parkin are activated to promote the proteasomal degradation of mitochondrial outer membrane proteins and selective elimination of damaged mitochondria by autophagy.
Circulating platelets are heterogeneous in size, age, and responsiveness, similar to platelets in vitro [15]. During storage, platelets of different in sizes, ages, and genetics can lead to discrepancies in biochemistry, morphology, and function. The present study evaluated the ROS production and autophagy processes in platelets and subpopulations of platelets, which are stored as platelet concentrates (PCs), and explored the role of ROS in the regulation of platelet autophagy.
Materials and Methods
Samples
Apheresis platelets were collected from five healthy blood donors in Ningbo Central Blood Station, Zhejiang Province, China. None of the donors took aspirin or other drugs that would affect platelet function for two weeks prior to the donation. The PLT counts of these blood donors were all between 250 and 450*109/L, which met the standards of a double platelet collection. After communication, the donors agreed to collect a single platelet for clinical supply and an additional 50 mL of platelets for this study. Written informed consent was obtained from all donors, and this study was approved by the local ethical committee.
Each sample, including 50 mL of PCs with over 1 × 109 PLT/mL, was collected by a blood component separator (MCS + 9000, Haemonetics, USA). On the day of PC collection (Day 0), each PC in a bag was equally split into five parts (for five test times) by using a connecting device (TSCD-II, Terumo Sterile Tubing Welder, TerumoBCT, Japan) and a digital balance (Sartorius, Germany). The PCs were kept in a platelet incubator maintained at 22 °C ± 2 ℃ with continuous gentle agitation throughout the full storage time. All parameters were tested on storage days 1, 2, 3, 4, and 7.
Measurement of ROS and LC3
Flow cytometry (FC500, Beckman Coulter, Fullerton, CA, USA) was employed for the measurement of ROS (total cell ROS and mitochondria ROS) and the autophagy marker LC3.
Total cell ROS and mitochondria ROS were measured using the molecular probes DCFH2-DA and MitoSOX™, respectively. Each 200 µl of PCs was incubated with 10 µM DCFH2-DA (Solarbio, Beijing, China) and 5 µM MitoSOX™ Red (Invitrogen, Carlsbad, CA, USA) at 37 ℃ in the dark for 20 min. The PCs were washed with PBS three times to remove the probe residues, and their fluorescent signal was measured at 510/580 nm or 588/525 nm by flow cytometry.
The FIX & PERM Kit (Multi Science, Hangzhou, China) was used for cell fixation and membrane perforation to detect LC3 in the PCs, and the platelets were subsequently incubated with rabbit anti-LC3 primary antibody (Abcam, Boston, MA, USA) in the dark for 2 h. They were washed with PBS to remove the antibody residues then incubated with goat anti-rabbit secondary antibody conjugated with FITC (Abclonal, Wuhan, China) in the dark for 30 min. Afterward, the platelets were washed with PBS then analyzed via flow cytometry [16].
Data on 10,000 platelets per sample were collected and analyzed. Each experiment was performed at least three times.
Western Blot
Standard Western blot analysis protocols were followed. First, 25 µg of platelet protein lysates was separated in 12% gels (Genscript, Nanjing, China). Three or more independent replicates were used for quantification. Antibodies for LC3 and Beclin1 were obtained from Abcam and those for PINK1, Parkin, β-actin from Abclonal. Integrated density values were calculated using Image J analysis software (NIH).
Transmission Electron Microscopy
The organelles of the platelets were observed via transmission electron microscopy (TEM). Following the standard protocol for preparing TEM samples [17], 106 cells were fixed with 2.5% PBS-buffered glutaraldehyde at 4 °C overnight and then washed three times with PBS to remove the fixative. Postfixation was performed by immersing the samples in 1% OsO4 for 3 h at room temperature. The samples were rinsed with PBS to remove OsO4 carefully, and then dehydrated through a graded ethanol series and acetone. Subsequently, the samples were washed three times with 100% acetone (for 30 min each time) and embedded in Embed-812 (EMS, USA). Sections of Embed-812-embedded platelets were cut with an ultramicrotome (EM UC7, Leica, Germany). The samples were then placed on 300-mesh copper grids and routinely stained with 5% uranium acetate and 1% lead citrate. Finally, the sections were viewed under a Hitachi-7650 transmission electron microscope (Hitachi, Japan).
Analysis of platelet organelle and autophagic structures was performed by referring to reference images from Neumüller et al. [9, 17, 18].
Statistical Analysis
All data were presented as frequency or mean with SD. GraphPad Prism 8 statistical software (GraphPad Software, La Jolla, CA, USA) was used for the analysis. Nonparametric Kruskal–Wallis ANOVA was applied to compare the data from different time groups, and a P-value less than 0.05 was considered statistically significant.
Results
ROS Products in PCs During Platelet Storage
The results of mean fluorescent intensity after DCFH2-DA staining were analyzed using Beckman Coulter CXP software, which presented the generation of total cell ROS. As shown in Fig. 1, the PCs from the five individuals showed different total cell ROS trends. However, most of the curves exhibited V-shaped changes, with the total cell ROS initially decreasing then increasing over time.
The results of mean fluorescent intensity after MitoSOX™ staining were analyzed by FlowJo software version 10. Given that ROS were partially generated within the platelet’s mitochondria, the levels of mitochondrial ROS were confirmed using MitoSOX-Red. The results showed that the levels of mitochondrial ROS continuously increased over storage time. However, the platelets gradually divided into two clusters. On Day 4, two cell clusters with different mean fluorescent intensities were distinctly observed: a cell cluster with a low fluorescent intensity that had a low mitochondria ROS level and another cell cluster that showed the opposite (Fig. 2).
Morphology of Organelles in PCs During Platelet Storage
TEM revealed the dramatic morphological characteristics of the platelets’ organelles (Fig. 3). Increased autophagosomes (double-membrane structure that wraps something with low electron density) or autolysosomes (monolayer with several vesicles inside that wraps something with low electron density) were observed in the PCs during platelet storage (Fig. 3B) relative to those in the fresh platelets (Fig. 3A). However, we were unable to demonstrate clearly whether mitochondria were present in the autophagosomes or autolysosomes.
Transmission Electron Microscopy (TEM) analysis of platelet morphology during prolonged storage. The image below is a partial enlargement of the black square of the upper image. Scale bar indicates 0.5 μm (above) and 0.2 μm (below). A Representative image of stored platelets on day 0 (fresh platelet). Data of Apheresis platelets collected from 2 blood donors are shown. B Representative image of stored platelets on day 4 (stored platelet). Red dotted circles: double-membrane autophagic structures (autophagosomes); blue dotted circles: autolysosomes. Data of Apheresis platelets collected from 2 blood donors are shown
Expression of Autophagy-Associated Proteins in PCs
To determine whether the autophagy process could be induced during platelet storage, we examined the autophagy marker LC3 via flow cytometry and Western blot.
As shown in Fig. 4, the fluorescence signal of total LC3 was extensively generated in the stored platelets, and the mean fluorescence intensity of platelet LC3 sharply increased on day 4.
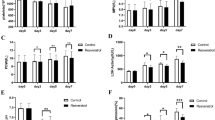
Subsequently, we monitored the autophagy-related proteins (Beclin1, LC3-II, LC3II/LC3I, PINK1, and Parkin) during platelet storage. Western blot revealed that although the LC3II levels did not substantially increase, those of LC3I sharply decreased, with the LC3II/LC3I ratio increasing over time. Moreover, another autophagy-related protein, i.e., Beclin1 [7, 19, 20], and mitophagy markers, i.e., Parkin and PINK1 [21,22,23], were detected. The levels of Beclin1 were enhanced, whereas those of Parkin and PINK1 remained stable throughout storage (Fig. 5).
Expression of autophagy-related proteins during platelet storage. A Western blot analysis of the autophagy-related proteins (Beclin1, LC3II/LC3I, Parkin, PINK1) in stored platelet. B Ratio of LC3II/LC3I, relative expression of Beclin1, PINK1, and Parkin to β-actin were subjected to semi-quantitative analysis by Image J software, n = 5
Expression of Autophagy Marker LC3 and Mitochondria ROS Products in Platelet Subgroups
To assess whether the autophagy process differed in the platelet subgroups during platelet storage, we evaluated the autophagy marker LC3 and mitochondrial ROS products in the platelet subgroups (Fig. 6A). Data showed that the LC3 in the normal-sized platelets continuously increased over storage time, which is consistent with the overall LC3 expression previously observed. However, the pattern of LC3 expression in the large-sized platelets was markedly different, with a wave-like change in W type, and the highest proportion of LC3-positive cells in the large platelets appeared on Day 3 (Fig. 6B).
The LC3-FITC and MitoSox-Red analysis in platelet size sub-populations during platelet storage. A Flow cytogram depicting large and small platelet sort in FC500 based on forward and side scatter characteristics.FITC-LC3-labeled platelet colocalize with the MitoSox-red-labeled platelet. B The proportion of LC3 positive cells in platelet size sub-populations, n = 5
We further analyzed the mean fluorescence intensity of LC3-FITC and MitoSOX-Red in the platelet size subpopulations during platelet storage. The results showed that the mean fluorescence intensity of LC3-FITC and MitoSOX-Red were higher in the large-sized platelets than in the normal-sized platelets at all the observed time points. The mean fluorescence intensity of LC3-FITC was consistent with that of MitoSOX-Red in either the large-sized or normal-sized platelets, suggesting that the platelets with low levels of oxidative stress had lower levels of autophagy and vice versa (Fig. 7).
The FITC-LC3 and MitoSox-Red average fluorescence intensity in platelet size sub-populations during platelet storage. A Mean fluorescent intensity of MitoSOX™-Red, large platelet colocalize with the normal platelet. B Mean fluorescent intensity of FITC-LC3, large platelet colocalize with the normal platelet
Discussion
Autophagy is a “self-digesting” pathway by which protein aggregates and organelles are delivered to lysosomes for degradation and recycling via double-membrane vesicles called autophagosomes [7, 24]. According to the current TEM results, the number of autophagic vesicles in the stored platelets was higher than that in the fresh platelets, indicating the increased activity of the autophagy pathway in vitro. The Western blot results showed that the apheresis platelets in storage underwent autophagy. The expression levels of Beclin1 and LC3-II proteins increased significantly with the prolongation of the storage duration, which coincides with the results of Tang H. et al. [25] who detected the expression levels of Beclin1 and LC3 in apheresis platelets after storage for 2, 3, and 5 days.
First, all the PCs were in the routine storage condition (without any nutrition supplement). Second, the platelets in the PCs were prevented from interacting with each other via continuous shaking in the incubator. These two reasons can induce platelets to have high respiration and ROS generation. Accompanied with the increase in total cell ROS and mitochondrial ROS, the autophagy signal LC3 in the platelets was strongly amplified. Thus, the increased activity of autophagy could have been induced by the accumulation of the ROS level during platelet storage. ROS are major intracellular signaling sensors that maintain autophagy. The main source of ROS in cells is widely believed to be the mitochondrial respiratory chain. ROS are extensively reported as an early inducer of autophagy [18, 26,27,28]. At low levels, ROS can serve as signaling molecules. However, at high levels, ROS lead to oxidative damage [4].
Mitochondria are organelles that open and regulate autophagy as the primary locus of ROS production. However, when the function of mitochondria is chronically impaired, ROS can be produced in large numbers, transforming its role from a massive autophagy inducer to a signal for mitochondrial self-elimination through a selective process called mitophagy. This process provides a good mechanism for negative feedback regulation through which autophagy eliminates the sources of oxidative stress and protects cells from oxidative damage. However, the current Western blot results revealed that platelets could upregulate the expression of autophagy-associated proteins (LC3 and Beclin1) but did not result in remarkable changes in mitophagy-associated proteins (PINK1 and Parkin) during platelet storage. The result may be associated with the active form of the proteins PINK1 and Parkin. Parkin is activated by PINK1-dependent phosphorylation [29], and PINK1 autophosphorylation is essential for Parkin recruitment to damaged mitochondria [30]. However, we were unable to demonstrate clearly whether mitochondria were present in the autophagosomes or autolysosomes by TEM because of the lack of instrument clarity. Thus, future studies need to determine the detailed structure of double-membrane autophagosomes or autolysosomes and should ascertain whether they have damaged mitochondria. Studies on the location of mitochondria insist that damaged mitochondria are degraded in lysosomes, but some researchers have reported that mitochondria can be shed from cells [27, 28, 31,32,33] or even transferred horizontally between cells [20, 28, 31]. Hence, further studies are needed to show the co-localization of ROS and LC3 by immunofluorescence.
In recent years, researchers have gradually realized that platelet heterogeneity may lead to differences in platelet biochemistry and function [34]. Our study suggests that the differences in the autophagy patterns of platelets in numerous studies may have stemmed from the heterogeneity of platelets. In the present study, the platelet subgroups showed differences in ROS generation and autophagic properties. In summary, the large platelets had higher ROS generation and autophagic flux than the small platelets. Previous studies have shown that the high levels of platelet ROS during platelet storage can be directly correlated with PSLs, such as platelet receptor loss, granule release, and viability impairment [5, 35, 36]. Given that the present study on PSLs with focus on the total platelet populations is limited, further investigation of the biochemistry and function properties of platelet subgroups during storage might help enhance our understanding of the physiological changes in stored platelets and optimize the guidelines for platelet storage. Future research may rely on big data obtained by proteomics or single-cell sequencing techniques to analyze the relationship between mitophagy and mitochondrial ROS and clarify the contribution of mitophagy to PSL [37].
Platelets during storage tend to lose their discoid shape and turn into spherical forms, with prominent dilations of the open canalicular system, reduction in the number of dense bodies, release and presence of large alpha granules, and formation of filopodia [17]. These events are collectively known as characteristics of PSL. According to the current TEM results, as the storage time increased, the numbers of platelets that were swollen or had swollen and disintegrated internal structures (globules) increased, and this increase was accompanied with the presence of filopodia. Platelets are not a homogenous group of cells but consist of different subpopulations with different ages and functional states. On the basis of forward-scattering characteristics of platelet populations, researchers have evaluated the expression of various activation markers, namely, CD42b, CD36, CD62p, and phosphatidyl serine, in platelet populations of different sizes during storage. They found higher levels of CD42b and CD62P expression in large platelet populations than in normal platelet populations [38]. In our study, the subpopulation of large (swollen) platelets had higher ROS and LC3 levels than the normal platelets. The platelet subgroups exhibited different autophagy patterns during storage, highlighting the heterogeneity of platelet composition. This information may help deepen our understanding of PSL.
This study explored the relationship between ROS and autophagy during routine platelet storage in vitro. We demonstrated that platelet subgroups have different autophagy patterns. A comprehensive understanding of the characteristics and functions of platelet subsets is of particular interest to transfusion medicine.
References
Jurk K, Kehre BE (2005) Platelets: physiology and biochemistry. Semin Thromb Hemost 31(4):381–392
Andrews RK, Berndt MC (2004) Platelet physiology and thrombosis. Thromb Res 114(5–6):447–453
Devine DV, Serrano K (2010) The platelet storage lesion. Clin Lab Med 30(2):475–487
Scherz-Shouval R, Shvets E, Fass E, Shorer H, Gil L, Elazar Z (2007) Reactive oxygen species are essential for autophagy and specifically regulate the activity of Atg4. EMBO J 26(7):1749–1760
Ghasemzadeh M, Hosseini E (2017) Platelet granule release is associated with reactive oxygen species generation during platelet storage: a direct link between platelet pro-inflammatory and oxidation states. Thromb Res 156:101–104
Vucic M, Stanojkovic Z, Antic A, Vucic J, Pavlovic V (2018) Evaluation of platelet activation in leukocyte-depleted platelet concentrates during storage. Bosn J Basic Med Sci 18(1):29–34
Feng W, Chang C, Luo D, Su H, Yu S, Hua W, Chen Z, Hu H, Liu W (2014) Dissection of autophagy in human platelets. Autophagy 10(4):642–651
Ohto H, Nollet KE (2011) Overview on platelet preservation: better controls over storage lesion. Transfus Apher Sci 44(3):321–325
Ouseph MM, Huang Y, Banerjee M, Joshi S, MacDonald L, Zhong Y, Liu H, Li X, Xiang B, Zhang G, Komatsu M, Yue Z, Li Z, Storrie B, Whiteheart SW, Wang QJ (2015) Autophagy is induced upon platelet activation and is essential for hemostasis and thrombosis. Blood 126(10):1224–1233
Cao Y, Cai J, Zhang S, Yuan N, Li X, Fang Y, Song L, Shang M, Liu S, Zhao W, Hu S, Wang J (2015) Loss of autophagy leads to failure in megakaryopoiesis, megakaryocyte differentiation, and thrombopoiesis in mice. Exp Hematol 43:488–494
Lee SH, Du J, Stitham J, Atteya G, Lee S, Xiang Y, Wang D, Jin Y, Leslie K, Spollett G, Srivastava A, Mannam P, Ostriker A, Martin KA, Tang WH, Hwa J (2016) Inducing mitophagy in diabetic platelets protects against severe oxidative stress. EMBO Mol Med 8(7):779–795
Tanida I, Ueno T, Kominami E (2008) LC3 and autophagy. Methods Mol Biol 445:77–88
Tran S, Fairlie WD, Lee EF (2021) BECLIN1: protein structure, function and regulation. Cells 10(6):1522
Chen X, Wang Q, Li S, Li XJ, Yang W (2022) Mitochondrial-dependent and independent functions of PINK1. Front Cell Dev Biol 10:954536
Mangalpally KK, Siqueiros-Garcia A, Vaduganathan M, Dong JF, Kleiman NS, Guthikonda S (2010) Platelet activation patterns in platelet size sub-populations: differential responses to aspirin in vitro. J Thromb Thrombolysis 30(3):251–262
Eng KE, Panas MD, Karlsson Hedestam GB, McInerney GM (2010) A novel quantitative flow cytometry-based assay for autophagy. Autophagy 6(5):634–641
Neumüller J, Meisslitzer-Ruppitsch C, Ellinger A, Pavelkaa M, Jungbauerb C, Renzb R, Leitnerc G, Wagner T (2013) Monitoring of platelet activation in platelet concentrates using transmission electron microscopy. Transfus Med Hemother 40(2):101–107
Lee J, Giordano S, Zhang J (2012) Autophagy, mitochondria and oxidative stress: cross-talk and redox signalling. Biochem J 441(2):523–540
Luo XL, Jiang JY, Huang Z, Chen LX (2019) Autophagic regulation of platelet biology. J Cell Physiol 234(9):14483–14488
Al Amir Dache Z, Otandault A, Tanos R, Pastor B, Meddeb R, Sanchez C, Arena G, Lasorsa L, Bennett A, Grange T, El Messaoudi S, Mazard T, Prevostel C, Thierry AR (2020) Blood contains circulating cell-free respiratory competent mitochondria. FASEB J 34(3):3616–3630
Zhou H, Li D, Zhu P, Hu S, Hu N, Ma S, Zhang Y, Han T, Ren J, Cao F, Chen Y (2017) Melatonin suppresses platelet activation and function against cardiac ischemia/reperfusion injury via PPARgamma/FUNDC1/mitophagy pathways. J Pineal Res 63(4):e12438
Zhang W, Ren H, Xu C, Zhu C, Wu H, Liu D, Wang J, Liu L, Li W, Ma Q, Du L, Zheng M, Zhang C, Liu J, Chen Q (2016) Hypoxic mitophagy regulates mitochondrial quality and platelet activation and determines severity of I/R heart injury. Elife 5:e21407
Yu L, McPhee CK, Zheng L, Mardones GA, Rong Y, Peng J, Mi N, Zhao Y, Liu Z, Wan F, Hailey DW, Oorschot V, Klumperman J, Baehrecke EH, Lenardo MJ (2010) Termination of autophagy and reformation of lysosomes regulated by mTOR. Nature 465(7300):942–946
Portal-Núñez S, Esbrit P, Alcaraz MJ, Largo R (2016) Oxidative stress, autophagy, epigenetic changes and regulation by miRNAs as potential therapeutic targets in osteoarthritis. Biochem Pharmacol 108:1–10
Tang H, Gao M, Fu Y, Gui R, Ma X (2020) The effect of autophagic activity on the function of apheresis platelets and on the efficacy of clinical platelet transfusion. Transfus Med Hemother 47(4):302–313
Sui X, Kong N, Ye L, Han W, Zhou J, Zhang Q, He C, Pan H (2014) p38 and JNK MAPK pathways control the balance of apoptosis and autophagy in response to chemotherapeutic agents. Cancer Lett 344(2):174–179
Davis CH, Kim KY, Bushong EA, Mills EA, Boassa D, Shih T, Kinebuchi M, Phan S, Zhou Y, Bihlmeyer NA, Nguyen JV, Jin Y, Ellisman MH, Marsh-Armstrong N (2014) Transcellular degradation of axonal mitochondria. Proc Natl Acad Sci U S A 111(26):9633–9638
Torralba D, Baixauli F, Sánchez-Madrid F (2016) Mitochondria know no boundaries: mechanisms and functions of intercellular mitochondrial transfer. Front Cell Dev Biol 4:107
McWilliams TG, Barini E, Pohjolan-Pirhonen R, Brooks SP, Singh F, Burel S, Balk K, Kumar A, Montava-Garriga L, Prescott AR, Hassoun SM, Mouton-Liger F, Ball G, Hills R, Knebel A, Ulusoy A, Di Monte DA, Tamjar J, Antico O, Fears K, Smith L, Brambilla R, Palin E, Valori M, Eerola-Rautio J, Tienari P, Corti O, Dunnett SB, Ganley IG, Suomalainen A, Muqit MMK (2018) Phosphorylation of Parkin at serine 65 is essential for its activation in vivo. Open Biol 8(11):180108
Okatsu K, Oka T, Iguchi M, Imamura K, Kosako H, Tani N, Kimura M, Go E, Koyano F, Funayama M, Shiba-Fukushima K, Sato S, Shimizu H, Fukunaga Y, Taniguchi H, Komatsu M, Hattori N, Mihara K, Tanaka K, Matsuda N (2012) PINK1 autophosphorylation upon membrane potential dissipation is essential for Parkin recruitment to damaged mitochondria. Nat Commun. 3:1016
Hayakawa K, Esposito E, Wang X, Terasaki Y, Liu Y, Xing C, Ji X, Lo EH (2016) Transfer of mitochondria from astrocytes to neurons after stroke. Nature 535(7613):551–555
Jiao H, Jiang D, Hu X, Du W, Ji L, Yang Y, Li X, Sho T, Wang X, Li Y, Wu YT, Wei YH, Hu X, Yu L (2021) Mitocytosis, a migrasome-mediated mitochondrial quality-control process. Cell 184(11):2896–2910
Marcoux G, Duchez AC, Rousseau M, Lévesque T, Boudreau LH, Thibault L, Boilard E (2017) Microparticle and mitochondrial release during extended storage of different types of platelet concentrates. Platelets 28(3):272–280
Lesyk G, Jurasz P (2019) Advances in platelet subpopulation research. Front Cardiovasc Med 6:138
Ghasemzadeh M, Hosseini E, Roudsari O, Zadkhak P (2018) Intraplatelet reactive oxygen species (ROS) correlate with the shedding of adhesive receptors, microvesiculation and platelet adhesion to collagen during storage: does endogenous ROS generation downregulate platelet adhesive function? Thromb Res 163:153–161
Hosseini E, Hojjati S, Afzalniaye Gashti S, Ghasemzadeh M (2020) Collagen-dependent platelet dysfunction and its relevance to either mitochondrial ROS or cytosolic superoxide generation: a question about the quality and functional competence of long-stored platelets. Thromb J 18(1):18
Tyagi T, Jain K, Gu S, Qiu M, Gu V, Melchinger H, Rinder H, Martin K, Gardiner E, Lee A, Tang W, Hwa J (2022) A guide to molecular and functional investigations of platelets to bridge basic and clinical sciences. Nat Cardiovasc Res 1:223–237
Vučetić D, Ilić V, Vojvodić D, Subota V, Todorović M, Balint B (2018) Flow cytometry analysis of platelet populations: usefulness for monitoring the storage lesion in pooled buffy-coat platelet concentrates. Blood Transfus 16(1):83–92
Funding
We thank Yan Wang and Huihui Feng for contribution to serve the blood donors and PCs collection. This work was supported by grants from Natural Science Foundation of Ningbo (No.2019A610273 and No.2019A610268); Ningbo Public welfare science and technology project (No.2019C50083); Natural Science Foundation of Zhejiang Province (No.LY20H290006); Open Foundation of key laboratory of blood safety research of zhejiang province (No.2018KF010).
Author information
Authors and Affiliations
Contributions
GD and QL conceived and designed the experiments; LY, SY and YH performed the experiments and evaluated the results; LY and QL wrote the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest was reported by all authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, L., Yu, S., He, Y. et al. High Autophagy Patterns in Swelling Platelets During Apheresis Platelet Storage. Indian J Hematol Blood Transfus 39, 670–678 (2023). https://doi.org/10.1007/s12288-023-01638-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12288-023-01638-1