Abstract
Purpose of Review
The emergence of a group of previously unknown or unrecognized dimorphic fungal species causing systemic human disease resulted in taxonomic shifts and the creation of a new genus, Emergomyces, within Onygenales. We review the morphology, taxonomy, physiology, and ecology of Emergomyces spp., and the epidemiology, clinicopathology, diagnosis, and management of disease.
Recent Findings
Emergomyces species have been reported as causes of human disease in Europe, Asia, Africa, and North America. Es. pasteurianus is most cosmopolitan, and Es. africanus, in southern Africa, causes the largest reported disease burden; in fact, emergomycosis is the most common endemic mycosis diagnosed in South Africa. The classic clinical picture is of disseminated disease, often with cutaneous involvement, in immunocompromised individuals.
Summary
Members of the genus Emergomyces are uncommon but important agents of systemic disease in immunocompromised hosts worldwide. Knowledge gaps include the biology of the fungus, and the pathophysiology and management of disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Recently, a new genus of thermally-dimorphic fungi within the Ajellomycetaceae was described to accommodate Emmonsia pasteuriana and several newly-named species of “Emmonsia-like” fungal pathogens [1]. Emergomyces was so-named because of the apparent emergence of related but previously unknown fungi causing systemic disease in immunocompromised hosts globally. Evidence of the earliest case of this mycosis (known as emergomycosis, formerly disseminated emmonsiosis) dates back to at least 1992 [2]; however, the recent recognition of these fungi and the disease they cause are attributed more to the contemporary use of molecular identification techniques in clinical and research laboratories than their sudden emergence as human pathogens [3].
Etiological Agents
Emergomycosis is caused by several fungal species within the newly-described genus, Emergomyces [1]. The type species, Es. pasteurianus, was first described as Emmonsia pasteuriana in 1998, based on apparent relatedness to Ea. crescens and Ea. parva [4]. Similarly, Es. africanus was thought to be a novel Emmonsia species when it was first reported [3]. The most-recently described species is Es. orientalis [5], reported from Asia; additional proposed species include Es. europaeus, currently represented by a strain isolated from the lung of a patient with rheumatoid arthritis in Germany [6] and Es. canadensis, from immunocompromised patients in Canada and the USA [2, 7].
Taxonomy
The genus Emergomyces is currently placed within the family Ajellomycetaceae alongside other thermally-dimorphic fungal pathogens such as Histoplasma, Blastomyces, and Paracoccidioides [1, 8]. Although some members of the group were initially described as novel species of Emmonsia, subsequent phylogenetic analyses revealed the genus Emmonsia to be polyphyletic [9, 10]. Consequently, a need was identified to accommodate several emerging thermally-dimorphic Emmonsia-like fungi distinguished in part from Ea. parva and Ea. crescens, the classic Emmonsia species, by small yeast-like cells rather than adiaspores as the parasitic phase [1, 11]. To date, only the anamorph (asexual form) of Emergomyces has been described [1]. Whole genome sequencing data show that both Es. africanus and Es. pasteurianus contain the alpha mating-type locus (MAT1–1) [1].
Epidemiology
Cases of emergomycosis have been reported from four continents: Europe, Asia, Africa, and North America. The true geographic range of Emergomyces spp. is unknown.
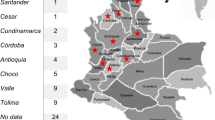
The largest described burden of emergomycosis is among HIV-infected persons in South Africa, where most cases are attributed to Es. africanus. In fact, emergomycosis is now recognized to be the most common endemic mycosis in South Africa [8]. Cases have since been diagnosed in six of nine provinces [8, 12], which include (in decreasing frequency) Western Cape [3, 12,13,14,15], Eastern Cape [12], Gauteng [8, 12, 16], Free State [12], Mpumalanga [12], and KwaZulu-Natal provinces (authors’ unpublished data). In addition, emergomycosis has been reported in a patient from Lesotho [12]. Although country-level surveillance data is lacking, a clinical and laboratory surveillance study diagnosed 17 culture-proven cases of emergomycosis over 15 months at public hospitals in Cape Town (authors’ unpublished data), a city in Western Cape province with an estimated 3.7 million inhabitants [17] and an estimated HIV prevalence of 5.2% [18].
Es. pasteurianus appears to be the most cosmopolitan species, causing disease on three continents. Emergomycosis due to Es. pasteurianus has been diagnosed in patients from Italy [4], Spain [19], France [20], India [21], China [22, 23], and South Africa [8].
Disease caused by Es. orientalis has been diagnosed only once, from a patient in Shanxi, China whose only reported comorbidity was diabetes mellitus [5]. Emergomycosis has been recently described in North America [8]. Four cases have been diagnosed, in immunocompromised patients from Saskatchewan, Canada, and Colorado and New Mexico, USA [2, 8].
Another proposed new species has been reported to cause disease in a single case: a farmer from Germany treated with corticosteroids for rheumatoid arthritis who was diagnosed with a chronic pneumonia [6].
Nearly all cases of emergomycosis have been reported in immunocompromised patients. Most cases have been diagnosed in patients with advanced HIV-infection [3, 4, 7, 12, 14,15,16, 21, 24] or other defects of cell-mediated immunity, like immunosuppression for organ transplantation [2, 13, 24].
Ecology
Knowledge of the environmental reservoir of Emergomyces spp. is important for understanding the organism’s biology, and may be useful in predicting the geographic range; for other described thermally-dimorphic fungi, the environmental reservoir harboring the mold-phase is soil or other organic material [25]. When the mold is disturbed, conidia are aerosolized, and may become inhaled by mammals and, in some cases, cause disease [25].
Environmental sampling studies have only been reported for Es. africanus. Molecular detection of Es. africanus was demonstrated in 30% of soils sampled from South Africa (mostly from Western Cape), including from a wide range of soil habitats [26]. Soil samples were also evaluated for culturable fungus using direct culture methods as well as indirect culture, including via mice inoculation; despite the finding that the latter technique could detect as few as 102 conidia in 10 g of soil (similar to PCR), attempts to culture Es. africanus from soil have thus far been unsuccessful [26].
Schwartz et al. also used molecular techniques to detect Es. africanus propagules trapped in air samples collected in an industrial area of Cape Town [27]. The presence of airborne Es. africanus propagules was observed on 10% of all days, suggesting that exposure to the conidia may be common even in urban areas.
To date, animal infection with Emergomyces has not been demonstrated. Cronjé et al. did not find evidence of Es. africanus in the lungs of 1402 animals (comprising 23 species) from South Africa screened with PCR [28]. To our knowledge, no cases of veterinary disease have been reported.
Although exposure to Es. africanus conidia is likely common in some heavily-populated endemic areas [29], only a small portion of patients with severely impaired cell-mediated immunity develop emergomycosis [15]. The reasons why only some exposed immunocompromised persons develop the disease are not clear, and further investigation is warranted.
Clinical Manifestations
Emergomycosis is typically a disseminated disease of immunocompromised hosts. The most common clinical manifestation—best described for disease caused by Es. africanus [12])—is the appearance of widespread cutaneous lesions, which can include papules, plaques, or ulcerations [3, 4, 7, 12, 22, 23] (Fig. 1).
Cutaneous lesions in two patients caused by Emergomyces africanus. a Widespread papules. b Widespread plaques and ulcers. (Photographs courtesy of Dr. Che Daniels and Dr. Rosie Burton, respectively, Khayelitsha District Hospital, Cape Town, South Africa). Reproduced with permission from [39]
Pulmonary disease is also common, and three-quarters of patients have abnormal chest radiographs [12]. Radiographic changes may include diffuse interstitial infiltrates, focal airspace disease, and/or hilar lymphadenopathy. In a minority of cases, upper airway involvement is reported, with symptoms such as epistaxis, rhinorrhea, or nasal congestion [12]. Although inhalation is presumed to be the route of infection [10], disease limited to the lungs is uncommon [6]. Extrapulmonary disease involving organs other than skin has been reported, including of liver [30], lymph node [7, 12], and cervix [7].
In at least half of HIV-infected patients, the diagnosis of emergomycosis only becomes apparent after the appearance or worsening of widespread cutaneous lesions after initiation of antiretroviral therapy (ART), suggesting an unmasking immune reconstitution inflammatory syndrome (IRIS) [12, 15].
Pathogenesis
Knowledge of the pathogenesis is inferred from clinical observations and extrapolation from related dimorphic fungi. Emergomycosis is presumed to occur following the inhalation of conidia released from environmental, saprobic mycelia [10]. In the lungs, a temperature-dependent transformation of the conidia to yeast-like cells occurs. A molecular switch, analogous to DRK1 (dimorphism-regulating kinase-1) in B. dermatiditis and H. capsulatum [31], has not yet been identified. In the absence of a competent host immune response, the yeast-like cells are capable of causing pulmonary and, upon hematogenous dissemination, extrapulmonary disease [3].
Among HIV-infected individiuals, the host response appears to be a function of CD4+ T-lymphocyte count, mediated by ART status. The histopathological picture in patients with low CD4 counts, who are not yet on ART, is of many yeast-like cells, with little or no inflammatory response; patients on ART demonstrate a more robust immune response, with few yeast-like cells [3]. This finding, combined with the clinical observation that many patients develop new or worsening cutaneous lesions upon ART initiation [12], suggests that the phenomenon of unmasking IRIS is common. In contrast, paradoxical IRIS (apparent clinical worsening of previously controlled disease upon ART initiation) appears to be uncommon [32].
Diagnosis
Diagnosis of emergomycosis is currently made by detection of the yeast phase from affected tissue during histopathology examination or by isolation of the fungus from appropriate specimens such as skin tissue, blood, bone marrow, respiratory tissue, liver tissue, and lymph node tissue [10]. Non-culture-based methods to detect fungal antigens or DNA directly from clinical specimens could potentially improve the speed of diagnosis but are not yet commercially available.
Histopathology
Histopathological examination of affected tissue is, in most cases, the fastest way to establish the diagnosis of deep fungal infections [33]; however, specificity is limited because the yeast-like cells of Emergomyces morphologically resemble those of H. capsulatum and, to a lesser extent, Sporothrix schenckii sensu stricto (Fig. 2)
Histopathology of skin biopsies from South African patients with HIV-associated systemic mycoses. a Sporothrix schenckii sensu stricto. Ovoid yeast-like forms that measure 2–8 μm in size (long arrows), as well as elongated “cigar bodies” that vary in diameter from 2 to 4 and in length from 4 to 10 μm (short arrows). The larger size of the yeast-like forms and the presence of elongated forms are helpful to distinguish S. schenkii from Histoplasma capsulatum and Emergomyces africanus. (Periodic Acid Schiff [PAS], ×1000). b H. capsulatum. Round to ovoid yeasts that vary in size from 2 to 3 to 3–5 μm with single budding nuclei and thin walls. Intra- and extracelluar organisms are present (arrows). (PAS, ×1000). c, d Es. africanus. Morphological features of fungal elements in tissue sections simulate the yeasts of H. capsulatum in particular (arrows). (PAS, ×1000). Reproduced with permission from [15]
[15]. Small (2 to 5 μm), intracellular and extracellular oval to round narrow-budding yeast-like cells may be observed in tissue sections stained with hematoxylin and eosin, Periodic acid-Schiff, Gomori’s methenamine silver, or Wright-Giemsa. The yeast-like cells of Emergomyces (Fig. 2a, b) are similar in size and morphology to those of H. capsulatum (2 to 5 μm) (Fig. 2c) [15] but smaller than those of B. dermatitidis (10 to 15 μm) which may demonstrate budding with broad-bases [33]; while the yeast-like cells of S. schenckii are similar in size, they may also assume a more elongated morphology (Fig. 2 d) [15]. Affected tissue should be submitted in saline for fungal culture to make an etiological diagnosis.
Culture
Appropriate biosafety precautions should be implemented when culturing these agents. There are currently no risk assessments published by national or international bodies, but given that disease has only been reported in immunocompromised individuals, we recommend that mycelial cultures should be handled under biosafety level 2 conditions (i.e., in class II biosafety cabinets with additional personal protective equipment such as N95 respiratory masks).
Emergomyces spp. can be isolated using standard fungal media, such as Sabouraud agar, malt extract agar, or potato dextrose agar [1, 3]. Growth is observed after 7 to 30 days of incubation at 24 to 30 °C. Morphologically, colonies appear beige and are slow-growing and filamentous at room temperature (Fig. 3). Conidiophores are short, unbranched, arising at right angles from thin-walled hyaline hyphae, slightly swollen at the top, sometimes with short, secondary conidiophores bearing ‘florets’ of conidia [1, 3]. Mold to yeast conversion can be helpful for confirming the identification and is achieved by transferring a piece of the mold colony into enriched media such as brain heart infusion (BHI, with or without 5% blood) or malt extract agar and incubating at 35 °C for 7 to 21 days [1, 3]. Yeast-phase colonies appear small, cream to smooth gray-brown, and heaped [1]. Small round to oval yeast-like cells with narrow buds are formed [1, 3].
Mycelial-phase culture of Emergomyces africanus on Sabouraud agar (20-day-old colonies). Note the white to pale brown colonies, which were glabrous at first, and have become powdery and wrinkled or cerebriform with age. Reproduced with permission from [39]
Antibody and Antigen Detection
There are no commercially available serological assays developed specifically for emergomycosis. However, some assays developed for other dimorphic fungi partially cross-react with Emergomyces. For example, three of the ten urine samples from patients with culture-proven emergomycosis are caused by Es. africanus tested positive with the second-generation IMMY H. capsulatum (galactomannan) antigen enzyme immunoassay (EIA) (ImmunoMycologics, Norman, OK), which uses monoclonal Histoplasma antibodies [15]. Moreover, antigen derived from Es. africanus yeast-phase culture filtrates cross-reacts with the same Histoplasma EIA (authors’ unpublished data).
Molecular Detection and Genotyping
Molecular tools have been helpful in the detection of Es. africanus in clinical and environmental samples [27, 29], and for the identification of clinical isolates to species level [1, 3]. Identification is usually achieved by amplification and sequencing of the internal transcribed spacer (ITS) region of the ribosomal gene using ITS 1 and ITS4 primers, ITS1 and ITS2 primers or 28S rDNA (large subunit or D1/D2) primers [1, 3, 5, 12], followed by sequence alignment with those deposited in the GenBank-NCBI (National Center for Biotechnology Information) database.
Multilocus sequence typing has proven to be useful for delineating the taxonomy of Emergomyces [1]. In addition, whole genome sequencing of three Emergomyces strains (Es. africanus (CBS136260), Es. pasteurianus (CBS 101426), and Es. orientalis (CBS 124587 = CGMCC2.4011) has been completed [1, 34].
Prevention and Treatment
Although it is now recognized to be the most common endemic mycosis diagnosed in South Africa [8], emergomycosis remains a relatively rare HIV-associated opportunistic infection. Apart from program-level interventions to diagnose HIV infection earlier and to early initiation of ART, there are no specific strategies currently recommended to prevent emergomycosis. Clinical detection might be improved by educating clinicians caring for HIV-infected patients in areas of higher endemicity (i.e., South Africa) on early recognition of the clinical syndrome of fever, widespread skin lesions, and systemic signs that should prompt the inclusion of systemic mycoses on differential diagnoses. Skin biopsies are imperative for early diagnosis [15].
There are no randomized-controlled trials available to guide the management of HIV-associated emergomycosis. Consequently, we recommend that clinicians caring for patients with emergomycosis follow the Infectious Diseases Society of America guidelines for the management of other endemic mycoses in immunocompromised persons [35, 36]. Generally, this should include amphotericin B (deoxycholate at a dose of 0.7–1 mg/kg daily or a lipid formulation at a dose of 3 mg/kg daily) for 7–14 days followed by a triazole antifungal agent for at least 12 months. Longer courses of treatment may be required in patients who do not achieve immune reconstitution. Although fluconazole is cheaper and easier to obtain than other triazoles, limited in vitro susceptibility data suggest that itraconazole (or voriconazole or posaconazole) may be preferred for the oral step-down phase following amphotericin B therapy [7, 8, 37].
The optimal timing of ART initiation following diagnosis of emergomycosis, among those who are ART-naïve, has not been established. Several potential interactions may occur between antifungals and ART and, where applicable, anti-tuberculosis therapy, and dosages may need to be adjusted [38].
Conclusion
While relatively rare, fungi within the novel genus Emergomyces cause a potentially-fatal disseminated mycosis among immunocompromised persons in endemic areas. Much work remains to be done to understand the geographic range, ecology, epidemiology, and immunopathogenesis of this fungal disease, to understand the full clinical spectrum of disease and to optimize clinical diagnostic and treatment pathways in areas of endemicity.
References
Dukik K, Muñoz JF, Jiang Y, Feng P, Sigler L, Stielow JB, et al. Novel taxa of thermally dimorphic systemic pathogens in the Ajellomycetaceae (Onygenales). Mycoses. 2017;60(5):296–309. https://doi.org/10.1111/myc.12601.
Sanche S, Wong A, Sigler L, Angel S, Peterson S. Invasive infection caused by a novel Emmonsia species in a renal transplant patient. In: focus fungal infect. 2005. Miami, p Abstr 87.
Kenyon C, Bonorchis K, Corcoran C, Meintjes G, Locketz M, Lehloenya R, et al. A dimorphic fungus causing disseminated infection in South Africa. N Engl J Med. 2013;369(15):1416–24. https://doi.org/10.1056/NEJMoa1215460.
Gori S, Drouhet E. Cutaneous disseminated mycosis in a patient with AIDS due to a new dimorphic fungus. J Mycol Med. 1998;8:57–63.
Wang P, Kenyon C, de Hoog S, Guo L, Fan H, Liu H, et al. A novel dimorphic pathogen, Emergomyces orientalis (Onygenales), agent of disseminated infection. Mycoses. 2017;60(5):310–9. https://doi.org/10.1111/myc.12583.
Wellinghausen N, Kern WV, Haase G, Rozdzinski E, Kern P, Marre R, et al. Chronic granulomatous lung infection caused by the dimorphic fungus Emmonsia sp. Int J Med Microbiol. 2003;293(6):441–5. https://doi.org/10.1078/1438-4221-00281.
Schwartz IS, Sanche S, Wiederhold N, Patterson TF, Sigler L. Emergomyces canadensis, a dimorphic fungus causing fatal systemic human disease in North America. Emerg Infect Dis. 2018 (In Press).
Maphanga TG, Britz E, Zulu TG, MR S, Naicker SD, Schwartz IS, et al. In vitro antifungal susceptibility of the yeast- and mould-phases of the dimorphic fungal pathogen, Emergomyces africanus (formerly Emmonsia species), from HIV-infected south African patients. J Clin Microbiol. 2017;55(6):1812–20. https://doi.org/10.1128/JCM.02524-16.
Peterson SW, Sigler L. Molecular genetic variation in Emmonsia crescens and Emmonsia parva, etiologic agents of adiaspiromycosis, and their phylogenetic relationship to Blastomyces dermatitidis (Ajellomyces dermatitidis) and other systemic fungal pat. J Clin Microbiol. 1998;36(10):2918–25.
Schwartz IS, Kenyon C, Feng P, Govender NP, Dukik K, Sigler L, et al. 50 years of Emmonsia disease in humans: the dramatic emergence of a cluster of novel fungal pathogens. PLoS Pathog. 2015;11(11):e1005198. https://doi.org/10.1371/journal.ppat.1005198.
Sigler L. Adiaspiromycosis and other infections caused by Emmonsia species. In: Hay RJ, Merz WG, editors. Topley Wilson’s microbiology and microbial infections. 10th ed. London: Arnold Hodder; 2005. p. 809–24.
Schwartz IS, Govender NP, Corcoran C, Dlamini S, Prozesky H, Burton R, et al. Clinical characteristics, diagnosis, management and outcomes of disseminated emmonsiosis: a retrospective case series. Clin Infect Dis. 2015;61(6):1004–12. https://doi.org/10.1093/cid/civ439.
Heys I, Taljaard J, Orth H. An emmonsia species causing disseminated infection in South Africa. N Engl J Med. 2014;370(3):283–4. https://doi.org/10.1056/NEJMc1314277#SA1.
Lochan H, Naicker P, Maphanga T, Ryan A, Pillay K, Govender NP, et al. A case of emmonsiosis in an HIV-infected child. S Afr J HIV Med. 2015;16:2–5.
Schwartz IS, Kenyon C, Lehloenya R, Claasens S, Spengane Z, Prozesky H, et al. AIDS-related endemic mycoses in western cape, South Africa and clinical mimics: a cross-sectional study of adults with advanced HIV and recent-onset, widespread skin lesions. Open Forum Infect Dis. 2017;4(4) https://doi.org/10.1093/ofid/ofx186.
van Hougenhouck-Tulleken WG, Papavarnavas NS, Nel JS, Blackburn LY, Govender NP, Spencer DC, et al. HIV-associated disseminated Emmonsiosis, Johannesburg, South Africa. Emerg Infect Dis. 2014;20(12):2164–6. https://doi.org/10.3201/eid2012.140902.
City of Cape Town - 2011 Census. Compiled by Information and Knowledge Management Department, City of Cape Town, using 2011 Census data supplied by Statistics South Africa. Available from http://www.capetown.gov.za/Family%20and%20home/education-and-research-materials/data-statistics-andresearch/cape-town-census. Accessed 10 Jan 2018.
Shisana O, Rehle T, Simbayi LC, Zuma K, Jooste S, Zungu N, et al. South African national HIV prevalence, incidence and behaviour survey, 2012. Cape Town: HSRC Press; 2014.
Pelegrín I, Alastruey-Izquierdo A, Ayats J, Cuenca-Estrella M, Cabellos C. A second look at Emmonsia infection can make the difference. Transpl Infect Dis. 2014;0:1–2.
Lavergne R-A, Kandel-Aznar C, Khatchatourian L, Garcia-Hermoso D, Jeddi F, Boutoille D, et al. Emmonsia pasteuriana: une cause rare d’infection fongique chez l’immunodéprimé. J Mycol Med. 2017;27(3):e7–8. https://doi.org/10.1016/j.mycmed.2017.04.025.
Malik R, Capoor MR, Vanidassane I, Gogna A, Singh A, Sen B, et al. Disseminated Emmonsia pasteuriana infection in India: a case report and a review. Mycoses. 2016;59(2):127–32. https://doi.org/10.1111/myc.12437.
Feng P, Yin S, Zhu G, Li M, Wu B, Xie Y, et al. Disseminated infection caused by Emmonsia pasteuriana in a renal transplant recipient. J Dermatol. 2015;42(12):1179–82. https://doi.org/10.1111/1346-8138.12975.
Tang XH, Zhou H, Zhang XQ, De Han J, Gao Q. Cutaneous disseminated emmonsiosis due to Emmonsia pasteuriana in a patient with cytomegalovirus enteritis. JAMA Dermatology. 2015;151(11):1263–4. https://doi.org/10.1001/jamadermatol.2015.1792.
Pelegrín I, Ayats J, Xiol X, Cuenca-Estrella M, Jucglà A, Boluda S, et al. Disseminated adiaspiromycosis: case report of a liver transplant patient with human immunodeficiency infection, and literature review. Transpl Infect Dis. 2011;13(5):507–14. https://doi.org/10.1111/j.1399-3062.2011.00611.x.
Restrepo A, Baumgardner DJ, Bagagli E, Cooper RC, MR MG, Lázera MS, et al. Clues to the presence of pathogenic fungi in certain environments. Med Mycol. 2000;38(Suppl 1):67–77. https://doi.org/10.1080/mmy.38.s1.67.77.
Schwartz IS, Lerm B, Hoving JC, Kenyon C, Basson WJ, Horsnell WG, et al. Emergomyces africanus in soil, South Africa. Emerg Infect Dis. 2018;24(2) https://doi.org/10.3201/eid2402.171351.
Schwartz IS, McLoud JD, Berman D, Botha A, Lerm B, Colebunders R, et al. Molecular detection of airborne Emergomyces africanus, a thermally dimorphic fungal pathogen, in cape town, South Africa. PLoS Negl Trop Dis. 2018; https://doi.org/10.1371/journal.pntd.0006174.
Cronje N, Schwartz IS, Retief L, et al. Attempted molecular detection of the thermally dimorphic human fungal pathogen Emergomyces africanus in terrestrial small mammals in South Africa. Med Mycol. 2017; https://doi.org/10.1093/mmy/myx065.
Schwartz IS, Sampson N, Lerm B, et al (2016) An investigation into the ecological niche of Emmonsia sp. 2nd EMBO work. AIDS-related mycoses.
Mutyaba A, Sonderup MW, Locketz M, Okpechi I, Spearman CW, Tooke A. Disseminated Emmonsia in an HIV-HBV co-infected man. IDCases. 2015;2(2):35–6. https://doi.org/10.1016/j.idcr.2015.01.003.
Sil A, Andrianopoulos A. Thermally dimorphic human fungal pathogens-polyphyletic pathogens with a convergent pathogenicity trait. Cold Spring Harb Perspect Med. 2014;5:a019794.
Crombie K, Spengane Z, Locketz M, Dlamini S, Lehloenya R, Wasserman S, et al. Paradoxical immune reconstitution inflammatory syndrome caused by Emergomyces africanus infection in an HIV-infected male taking itraconazole. PLoS Negl Trop Dis. 2018; https://doi.org/10.1371/journal.pntd.0006173.
Guarner J, Brandt ME. Histopathologic diagnosis of fungal infections in the 21st century. Clin Microbiol Rev. 2011;24(2):247–80. https://doi.org/10.1128/CMR.00053-10.
Yang Y, Ye Q, Li K, et al. Genomics and comparative genomic analyses provide insight into the taxonomy and pathogenic potential of novel Emmonsia pathogens. Front Cell Infect Microbiol. 2017;7:105.
Wheat LJ, Freifeld AG, Kleiman MB, Baddley JW, McKinsey DS, Loyd JE, et al. Clinical practice guidelines for the management of patients with histoplasmosis: 2007 update by the Infectious Diseases Society of America. Clin Infect Dis. 2007;45(7):807–25. https://doi.org/10.1086/521259.
Kauffman CA, Hajjeh R, Chapman SW. Practice guidelines for the management of patients with sporotrichosis. For the mycoses study group. Infectious Diseases Society of America. Clin Infect Dis. 2000;30(4):684–7. https://doi.org/10.1086/313751.
Dukik K, Al-Hatmi AMS, Curfs-Breuker I, Faro D, de Hoog S, Meis JF. Antifungal susceptibility of emerging dimorphic pathogens in the family Ajellomycetaceae. Antimicrob Agents Chemother AAC. 2018;62(1):e01886–17.
Schwartz IS, Wasserman S. Itraconazole and antiretroviral therapy: strategies for empiric dosing. Lancet Infect Dis. 2017;17(11):1122–3. https://doi.org/10.1016/S1473-3099(17)30568-6.
Govender NP, Maphanga TG, Schwartz IS. Emergomycosis (formerly disseminated emmonsiosis). In: González Á, Hernández O, Rúa ÁL, Gomez BL, Tobón Á, Restrepo Moreno Á, editors. Essentials of human mycosis. Colombia: Corporación para Investigaciones Biológicas and the Universidad de Antioquia; 2018. In Press.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Epidemiology of Fungal Infections
Rights and permissions
About this article
Cite this article
Schwartz, I.S., Maphanga, T.G. & Govender, N.P. Emergomyces: a New Genus of Dimorphic Fungal Pathogens Causing Disseminated Disease among Immunocompromised Persons Globally. Curr Fungal Infect Rep 12, 44–50 (2018). https://doi.org/10.1007/s12281-018-0308-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12281-018-0308-y