Abstract
Valvular heart disease and congenital heart defects represent a major cause of death around the globe. Although current therapy strategies have rapidly evolved over the decades and are nowadays safe, effective, and applicable to many affected patients, the currently used artificial prostheses are still suboptimal. They do not promote regeneration, physiological remodeling, or growth (particularly important aspects for children) as their native counterparts. This results in the continuous degeneration and subsequent failure of these prostheses which is often associated with an increased morbidity and mortality as well as the need for multiple re-interventions. To overcome this problem, the concept of tissue engineering (TE) has been repeatedly suggested as a potential technology to enable native-like cardiovascular replacements with regenerative and growth capacities, suitable for young adults and children. However, despite promising data from pre-clinical and first clinical pilot trials, the translation and clinical relevance of such TE technologies is still very limited. The reasons that currently limit broad clinical adoption are multifaceted and comprise of scientific, clinical, logistical, technical, and regulatory challenges which need to be overcome. The aim of this review is to provide an overview about the translational problems and challenges in current TE approaches. It further suggests directions and potential solutions on how these issues may be efficiently addressed in the future to accelerate clinical translation. In addition, a particular focus is put on the current regulatory guidelines and the associated challenges for these promising TE technologies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
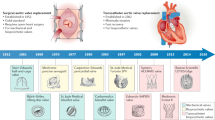
Valvular heart disease and congenital heart defects, often affecting the left and right ventricular outflow tracts and the great arteries, represent a major cause of morbidity and mortality all over the world [1–3]. The conventional surgical treatment for these types of cardiovascular disease (i.e., valve replacement or surgical correction of the congenital malformation) is safe and has been the standard of care for several decades for affected adult and pediatric patients. In addition, minimally invasive, transcatheter technologies have been safely implemented into clinical routine in recent years [4]. In both the adult and pediatric settings, transcatheter approaches have proven to be valid alternatives for selected patient cohorts and their clinical adoption is constantly increasing. However, despite this rapid evolution and the availability of various treatment options for affected patients, it is important to highlight that the currently used prostheses are non-regenerative replacements as they lack remodeling, self-repair, or growth capacity [5]. In general, this leads to an increased risk of cardiac adverse events as well as the need for multiple re-operations, resulting in an elevated morbidity and mortality throughout the lifetime. In the adult setting, major complications include infection, thromboembolic events (i.e., after mechanical heart valve replacement), or progressive degeneration over time (i.e., in case of bioprosthetic heart valve replacements), as reviewed elsewhere [6]. In the pediatric setting, instead, the lack of growth capacity represents a major problem that may require multiple high-risk redo interventions [7, 8].
To address this huge clinical problem, tissue engineering (TE) has been proposed as a promising solution to fulfill the need for cardiovascular replacements with regenerative and growth capacities, suitable for young adults and pediatric patients [9]. The original paradigm of in vitro heart valve TE as described by Langer and Vacanti more than 20 years ago comprises a scaffold seeded with (autologous) cells and in vitro extracellular matrix (ECM) production in a bioreactor [10]. However, from the technical and logistical standpoint, these classical approaches are challenging, and although some simplified (in vitro) cardiovascular TE approaches have already been advanced into clinical pilot trials (e.g., pre-seeded allografts [11–13] and xenograft [14] valve replacements, and vascular prosthesis [15, 16]), there is a significant need for improvement to facilitate broad clinical adoption.
Therefore, in general, researchers are currently focusing on more simplified, clinically relevant strategies such as so-called in situ TE techniques that rely on the recipients’ regenerative potential to integrate and remodel the implanted acellular construct. Indeed, the scaffold material used for such approaches (e.g., decellularized xenogenic, allogenic, or engineered tissues; biodegradable polymeric substrates) has a fundamental role as it has to sustain the native mechanical environment and provide functionality immediately upon implantation. Over time, the balance between de novo ECM production and scaffold degradation should be carefully considered, in order to have sufficient mechanical properties that can ensure the functionality at any time upon implantation. In addition, the cell-free implanted biomaterial should favor cell adhesion, proliferation, and ECM production to enable physiological remodeling towards a native-like functional living tissue [17, 18]. Further information about the different cardiovascular TE approaches can be found elsewhere for both valves [5, 19, 17, 20, 21] and vascular grafts [22–24]. In recent years, the in situ approach has become clinical practice [25–27], with the implantation of non-seeded decellularized allogenic valves that also showed spontaneous re-cellularization [28, 29].
Although cardiovascular TE approaches have demonstrated promising results in both pre-clinical [30–36] and clinical pilot [11–13, 28, 29, 37, 38, 15] trials, as reviewed elsewhere [39], their broad clinical adoption is limited as many key challenges do remain. These include scientific key questions to enable a safe clinical translation and logistical, technical, and infrastructural challenges for the production and commercialization of such TE products (Fig. 1).
Translational challenges in cardiovascular tissue engineering and their relationship to the different aspects (research, development, and manufacturing) of the product life cycle. Scientific challenges are usually addressed by in vitro testing and are mainly correlated to the research part of the product life cycle. Clinical challenges, instead, can influence product design and development and are addressed via in vivo animal studies. Finally, regulatory and infrastructural challenges are responsible for the regulation of product manufacturing while clinical trials can influence the marketing approval
The aim of this review is to provide an overview on the most important aspects and challenges when designing and producing a (cardiovascular) tissue engineered medical product (TEMP). It specifically focuses on the different scientific, clinical, technical, and regulatory challenges that still need to be addressed to enable a safe and broad clinical adoption of tissue engineered cardiovascular replacements.
Challenges in the Development of Tissue Engineered Products
With the release of the European regulation 1394/2007 [40], TEMPs are considered as so-called advanced therapy medicinal products, together with cell and gene therapies, and are classified as medicinal products. By definition, a medicinal product is meant to treat or prevent diseases in humans and to restore, correct, or modify a physiological function by exerting an immunological, pharmacological, or metabolic action upon administration [41, 42]. TEMPs may or may not contain viable cells and extracellular matrix components, being therefore difficult to distinguish from certain cell therapies. In addition, they are used in view to regenerate, repair, and/or replace a tissue or an organ [43]. The Food and Drug Administration (FDA), instead, defines TEMPs as human medical products, together with drugs, tissues, biological products, and medical devices, intended for implantation, transplantation, infusion, or transfer into a human recipient. Since TEMPs contain different product categories, the FDA regulates them under three different pathways: drug, biological product, or medical device [44, 41]. Of note, due to the increased incidence of cardiovascular diseases and resulting surgeries and interventions, there is a growing market for any cardiovascular device, attracting the interest of investors and biomedical corporations. However, and despite the promising experience from pre-clinical and clinical pilot trials, the clinical translation and commercialization of TE constructs as true products is still limited. The reasons for this problem are multifaceted and will be comprehensively discussed in this review.
Classification of the Product
Due to their great heterogeneity, the overall classification of TEMPs is difficult as they may contain polymeric matrices, cells, proteins, and bioactive molecules. Thus, the primary mode of action by which the product achieves its therapeutic effect needs to be determined before it could be assigned to its respective category [45]. In particular, and importantly, devices containing living cells have usually a clear pharmacological, immunological, or metabolic function upon implantation and are therefore usually classified by the FDA as biological or pharmaceutical products. On the other hand, decellularized tissues can be classified either as medical devices, if their main function occurs by physical means (e.g., heart valve allografts by CryoLife, Inc.—Kennesaw, GA, USA—are considered as class II medical devices), or as biological products (e.g., tissue engineered constructs that do not contain viable cells) [44]. Similar discrepancies are present also in the European classification for these novel regenerative products. However, in the past years, some efforts have been undertaken to solve these differences: according to the medical device regulation (MDR) which is currently under development ([46]), all the non-living (i.e., decellularized, devitalized, fixed) products, such as decellularized homografts or even decellularized tissue engineered constructs, will be categorized as medical device while, until now, they are completely differently regulated depending on the respective European country.
Therefore, the different regulatory agencies (such as the FDA; the European Medicines Agency (EMA); the Ministry of Health, Labour and Welfare in Japan; the Swissmedic in Switzerland; the Paul Ehrlich Institute in Germany; or the Therapeutic Goods Administration in Australia) will be required to develop new, universal TEMP regulations which are consistent among the different countries, in order to better support commercialization of these products worldwide.
However, besides thoughtful classification, there are also several other challenges to be addressed before advancing TEMPs into commercialization: scientific and clinical issues will particularly depend on the medical indication, while logistical and infrastructural requirements are necessary to deliver a product suitable for commercialization [40].
Scientific Requirements
By definition, TEMPs should have the capacity to regenerate, repair, and/or replace a tissue or an organ [43] by performing similarly to the corresponding native tissue. Therefore, the choice of a starting material that is capable of integrating and remodeling upon implantation till becoming a native-like tissue is of the utmost importance.
A possible way to mimic the native tissue is to use decellularized homografts for the development of TEMPs. In fact, thanks to the lack of immunoreactivity, these materials showed sufficient functionality, the potential capacity for re-cellularization post implantation, and partial adaptive growth in clinical settings [28, 26]. However, donor shortage limits the availability of these allogenic tissues, inducing researchers to optimize novel materials. Abundant and easily accessible glutaraldehyde-fixed or decellularized xenogenic tissues (e.g., bovine pericardium, porcine valves, and intestinal submucosa) are creating a new market for various (cardiovascular) applications (e.g., CorMatrix, Roswell, GA, USA, and Cook Biotech, West Lafayette, IN, USA). While glutaraldehyde-fixed tissues cannot undergo repair and remodeling upon implantation, the use of decellularized xenogenic materials showed promising results in pre-clinical settings for both valves [47–49] and vascular conduits [50, 51]. Nevertheless, due to their residual immunogenicity, clinical application of decellularized xenogenic valves led to dramatic results: failure, degeneration, and stenosis that determined the need for surgical replacement of the implant in more than 50% of the patients [52–55].
To overcome the lack of allogenic materials, fully tissue engineered products may provide a potential solution. In order to be clinically relevant and to avoid immunogenic response, TEMPs produced via the classic in vitro TE approach should be based on autologous cells. However, to be adaptable to a routine clinical scenario, the cell source of choice plays an important role not only in the manufacturing but also in the clinical adaptation of such a product. While vascular-derived cells, isolated from the recipient veins, are commonly used for both blood vessel [56, 31] and heart valve [14, 32] TE, alternative sources that do not require a surgical intervention (e.g., bone marrow-derived [57, 16], adipose tissue-derived [58], and blood-derived [59] cells) are gaining potential interest to hasten the preparation of the replacement. Independently of the selected cell type, it is important to consider that cells react and depend on the surrounding environment [60] and can undergo differentiation in response to different scaffold characteristics, such as fiber size [61, 62]. An overview of cells used for cardiovascular tissue engineering can be found elsewhere [63].
The use of homografts as scaffold for in situ approaches has proved to be feasible [28, 26, 37, 64, 29] but, due to shortage of donor material, not widely applicable, suggesting the need for new easily available options. To fulfill this need, the use of acellular scaffolds based on decellularized tissue engineered constructs [65, 66, 36] or polymeric biodegradable scaffolds [67–69] has been introduced, with the advantage of being off-the-shelf and non-immunogenic replacements, capable of integrating, remodeling, and even growing into the recipient body [36].
Among the different aspects a cardiovascular TEMP needs to fulfill (e.g., sufficient mechanical properties to constantly adapt to the continuously changing hemodynamic environment, favor cell adhesion and infiltration, resistance to calcification, and immunogenicity), anti-thrombogenicity is among the most important. In fact, cardiovascular TEMPs are meant to be in direct contact with blood, and therefore, they may be associated with thrombotic and thromboembolic complications due to platelet adhesion and activation [70]. Being the endothelium as the only known fully hemocompatible surface, researchers investigated the role of endothelial cell (EC) seeding and culture on different cardiovascular devices. Clinical trials showed that human pulmonary valves seeded with autologous ECs showed good functionality and performance up to 10 years [12]. However, clinical investigation of EC-seeded vascular grafts had led to less promising outcomes, with modest improvement in patency and anti-thrombogenic properties, probably related to heterogeneous EC coverage [71–74]. In addition, EC seeding prior to implantation is a time-consuming approach that requires a piece of native vessel or the differentiation of blood progenitor cells (e.g., endothelial colony-forming cells [18]) or stem cells (e.g., adipose stem cells [75], mesenchymal stem cells [76]) to obtain the autologous ECs needed for the formation of a confluent endothelium on the prosthesis. To avoid expensive and risky procedure of in vitro cell isolation and differentiation, a lot of research focuses on surface modifications of cardiovascular products, to ensure the formation of a functional endothelium in situ [77] by enhancing endothelial (progenitor) cell recruitment, adhesion, and differentiation by using antibodies (e.g., against CD34 [78, 67, 79] or CD133 [80, 81]), peptides (e.g., fibronectin-derived peptides RGD [82, 83] and REDV [84, 85], laminin-derived peptide YIGSR [86, 87], heparin), and growth factors (e.g., VEGF [88, 51, 89, 67]). However, these material modifications usually use a general biomolecule that can induce the recruitment and differentiation of different cell types other than the ECs, leading to undesired effects (e.g., stenosis and intimal hyperplasia by using CD34 antibodies [79], endothelial-to-mesenchymal differentiation by using the transforming growth factor β1 [90], and recruitment of smooth muscle progenitor cells by using SDF1α [91]). This suggests that cell recruitment should be controlled by using a more complicated combination of these bioactive molecules to be able to guide cell differentiation towards the desired phenotype [87]. In addition, the stability of these specific surface treatments should be ensured over time to prevent denaturation of the adsorbed protein and antibodies, with related loss of coating functionality, and they must have a continued and controlled release of the biomolecule of interest [92].
Clinical Requirements
In order to allow for a safe and broad clinical adoption of a TEMP, several clinical aspects need to be considered [93]. First, the safety of such technologies needs to be ensured by defining how the success of implantation and the function of the TEMP is controlled. Therefore, specific clinical protocols and guidelines are mandatory. They should comprise of the exact definition of clinical indication, patient selection, post-implantation follow-up algorithm, and, most importantly, the definition of bail out strategies in case of failure. A particular focus should be put on the development of a comprehensive monitoring and surveillance strategy for all patients who have received a TEMP. This particularly includes a thoughtful and continuous clinical follow-up using state-of-the-art imaging techniques including echocardiography, computed tomography, magnetic resonance imaging, or hybrid techniques to detect early signs of malfunction, developing failure, or other complications such as infections or thromboembolic events. This is particularly relevant for any TEMP, since its success or failure is directly linked to the recipients’ individual intrinsic regeneration and remodeling potential which may vary between patients. Therefore, in particular, the presence of comorbidities or any other condition that may alter the recipients’ regenerative potential that may promote potential failures needs to be evaluated prior to any TEMP implantation. In this regard, novel screening strategies such as tissue-on-a-chip technologies [94] could be a very useful tool to assess the patients’ individual regenerative capacity and, thereby, to detect candidates that may not be suitable for a TEMP implantation. Furthermore, to allow for broad clinical adoption, the utilization of the TEMP should be simple, straightforward, and applicable in an average clinical setting and institution (i.e., non-academic institutions, city hospitals, etc.). In order to prevent any potential error during its use, the product should be easy to handle and, ideally, comparable to the standard clinically used cardiovascular prostheses the operators (i.e., surgeons and interventionists) are used to. In addition, detailed instructions, including a summary of the product characteristics, as well as the in vitro demonstration and/or training of the standard operating procedures (SOPs) on how to use the TEMP are required for the users.
Regulatory and Infrastructural Requirements
The classical development of a TEMP is summarized in Table 1 and extensively reviewed elsewhere [95]. Upon definition of the specific medical indication the product aims to treat, the regulation of the manufacturing process and the assessment of the quality of the product are essential to have a standardized and controlled final output. For this reason, the International Organization for Standardization (ISO) provides requirements, specifications, or guidelines that can be voluntarily used to ensure the quality and efficacy of a product and, therefore, facilitate world commercialization. However, for instance, when considering valve replacements, these norms are usually designed to test mechanical or fixed biological prostheses and cannot be directly translated to assess the behavior of tissue engineered products. In fact, TEMPs are usually composite materials, based on cells, the extracellular matrix, and/or a scaffold for which the development of appropriate testing platforms is challenging because of the complex three-dimensional structure and the heterogeneous composition of the product. In addition, TEMPs are expected to undergo remodeling and changes (i.e., scaffold degradation, de novo ECM formation) in vivo. For this reason, in vitro tests are not sufficient to provide information about the clinical safety and efficacy of the device because of the modifications that will occur upon implantation. While the remodeling potential of a TEMP should be estimated via studies in relevant (large) animal models for proof-of-concept, efficacy, and safety evaluation, in vitro tests can be used to assess the individual components of the product (e.g., scaffold degradation rate and cytotoxicity; cell identity, purity, and potency), independently on the nature of the TEMP (e.g., allogenic or xenogenic tissue, cellular or decellularized tissue engineered matrices, polymeric substrates). For example, scaffold biocompatibility can be determined by following ISO 10993: Biological evaluation of medical devices (part 5: Tests for in vitro cytotoxicity). Subsequently, the performance and efficacy of the final TEMP should be addressed by using tests specific for the application to ensure that the product will be able to function upon implantation (e.g., in vitro valve testing in a pulse duplicator system to assess the prosthesis functionality, burst pressure test to determine whether a vascular graft is sufficiently robust to sustain the systemic pressure). For any cardiovascular device, different norms have been proposed: the ISO 13485 (Medical devices: quality management system—requirements for regulatory purposes), ISO 5840 (Cardiovascular implants: cardiac valve prostheses), ISO 7198 (Cardiovascular implants and extracorporeal systems—Vascular prostheses: Tubular vascular grafts and vascular patches), and ISO 25539 (Cardiovascular implants: endovascular devices).
In addition, to enable rapid and safe clinical application and commercialization, the following criteria need to be implemented in the developing process of the TEMP: (1) the whole production process needs to be carried out in a good manufacturing practice (GMP) facility (which aims at manufacturing consistent batches of a product according to pre-defined quality criteria); (2) the testing should be performed under good laboratory practice (GLP) quality system (which aims at protecting scientific data integrity by having a clear record of planning, performance, and archiving of non-clinical research studies); and (3) the results need to be evaluated by an accredited notified body [45].
Since TEMPs are based on the use and manipulation of cells and tissues, the quality control of the final product requires specific methodologies in order to comprehensively define and characterize it with particular regard to purity, safety, and biological activity [40]. In addition, novel methods to monitor tissue development during culture, while maintaining the sterility and integrity of the TEMP, need to be explored to ensure the quality of the final product [96].
If compared to the classic in vitro TE, the in situ approach offers substantial advantages when it comes to the manufacturing process. While terminal sterilization of cell-free constructs is a standard procedure, this is not applicable for living cellularized TE products which require special aseptic handling throughout the entire production process until final use. Similarly, the stability and integrity of such viable TE products are difficult to preserve over a long period of time, while the off-the-shelf availability of cell-free constructs allows for easy handling, storage, and shipment.
Another important parameter that should be considered when designing a TEMP is the role of the scaffold in the final product. Usually, the scaffold is an integral part of such a construct and, therefore, its chemical and physical properties (e.g., porosity, stiffness, topography, hydrophilicity, and biodegradation) should be defined and characterized according to ISO 10993 (Biological evaluation of medical devices—part 9: framework for identification and quantification of potential degradation products; part 18: chemical characterization of materials; part 19: physico-chemical, morphological and topographical characterization of materials). In addition, any potential effect of the scaffold, or scaffold degradation products, on the cells (e.g., adhesion, proliferation, viability, and differentiation) should be also investigated and defined. Once the development of the TEMP is standardized and its therapeutic role is addressed and tested in vitro, pre-clinical studies can be initiated to define the pharmacological and toxicological effects in vivo. Overall, the results obtained from a pre-clinical testing should confirm feasibility, safety, and efficacy of the product and, therefore, are mandatory for all TEMPs under development. The identification of the correct animal model is of high importance and considered one of the most challenging steps. Thus, the pre-clinical study protocol should be ideally designed in collaboration with competent authorities [95] and the advantages and limitations of the chosen animal model have to be justified and balanced. For instance, the sheep model is usually chosen for testing biological heart valve replacements [97, 98]. In fact, due to its high calcium metabolism, the sheep is considered the “worst case scenario” in terms of degeneration and progressive calcification of the implant, two common causes of failure of bioprostheses. Therefore, this animal model will also allow to obtain excellent predictions about the durability and functionality of tissue engineered heart valves [98]. On the other hand, it however remains controversial as to what extent the obtained results are directly translatable into the human setting. Therefore, the combination with additional animal models being closer to the human patho-(physiology) (i.e., non-human primates) could be helpful to further validate the findings.
Finally, the clinical development of a TEMP should comprise studies to address the safety and efficacy of the product in humans. Usually, the first clinical study is an “early feasibility,” used to evaluate the device design concept and the initial clinical safety and device functionality in less than ten subjects (phase 0). Upon this initial test, the product design can be further optimized and finalized according to the obtained results. Subsequently, for all the other phases of clinical investigation (phases I, II, and III trials), the design cannot be changed, the product should be produced according to GMP regulations, and the clinical trials have to be designed in accordance to the good clinical practice (GCP) guidelines.
For the manufacturing, testing, and commercialization of TEMPs, the developers can refer to different important European legislations other than the mentioned Regulation EC 1394/2007, as summarized in Table 2 and reviewed elsewhere [40]. For the American market, instead, we refer the reader to a comprehensive review with selected standards relevant for tissue engineering and regenerative medicine products [44].
Conclusions
In light of our aging population, there is a growing prevalence of diseases affecting the heart and vascular system requiring the replacement of afflicted valves or blood vessels. In addition, the correction of congenital heart defects, pathologies considered fatal until 30 years ago, has increased over the last decades [36]. Although the current treatment strategies incorporating surgical, transcatheter, or hybrid approaches are safe and applicable to many patients, the currently available prostheses used for replacement or reconstruction of the defect do not have any ability to grow or remodel after implantation, resulting in continuous calcification and degeneration. Affected patients may therefore require multiple re-operations, which is also a common problem in the congenital setting as the child outgrows the prosthesis, leading to a significant size mismatch [99].
Tissue engineering has been proposed as a promising solution to provide products capable of remodeling and growing after implantation. Thanks to these advantages, cardiovascular TEMPs may soon dramatically reduce the healthcare costs related to the required periodic replacement of standard non-regenerative cardiovascular prosthesis (e.g., polytetrafluoroethylene vascular grafts, glutaraldehyde-fixed bioprosthesis) currently used in pediatric and young adult patients.
The broad clinical adoption and commercialization of a TEMP is yet to be achieved due to major remaining scientific, clinical, technical, and logistical challenges (Table 3). The increasing number of publications in the regenerative medicine area suggests that this is a very active sector [100]. However, most of the regenerative therapies that have been tested in first clinical pilot trials did not contribute to the development of commercial products, primarily due to high costs and logistics for subsequent large-scale trials [101].
While researchers and physicians focus on the scientific and clinical aspects of the development of a TEMP, the importance of major regulatory and infrastructural requirements is usually neglected. Companies are seeking new global markets, but the divergences in technical and regulatory requirements from country to country induce industry to duplicate test procedures, in order to market new products internationally. To solve this issue, the initiation of an international organization to discuss scientific and technical aspects of TEMP registration between Europe, the USA, and Japan—as previously done for the pharmaceutical field by the International Council for Harmonization of Technical Requirements for Pharmaceuticals for Human Use (ICH)—will be extremely beneficial. By performing production and pre-clinical and clinical evaluation of the product in accordance to these international guidelines, it will be possible to ensure safety, quality, and efficacy of TEMPs in different countries worldwide. These indications will therefore lead to the commercialization of the product in the different areas included in the organization while still ensuring and protecting public health.
Abbreviations
- EC:
-
Endothelial cell
- ECM:
-
Extracellular matrix
- GCP:
-
Good clinical practice
- GLP:
-
Good laboratory practice
- GMP:
-
Good manufacturing practice
- ISO:
-
International Organization for Standardization
- SOP:
-
Standard operating procedure
- TE:
-
Tissue engineering
- TEMP:
-
Tissue engineered medical product
References
Marelli, A. J., Mackie, A. S., Ionescu-Ittu, R., Rahme, E., & Pilote, L. (2007). Congenital heart disease in the general population: changing prevalence and age distribution. Circulation, 115(2), 163–172. doi:10.1161/CIRCULATIONAHA.106.627224.
Nkomo, V. T., Gardin, J. M., Skelton, T. N., Gottdiener, J. S., Scott, C. G., & Enriquez-Sarano, M. Burden of valvular heart diseases: a population-based study. The Lancet, 368(9540), 1005–1011. doi:10.1016/S0140-6736(06)69208-8.
Supino, P. G., Borer, J. S., Preibisz, J., & Bornstein, A. (2006). The epidemiology of valvular heart disease: a growing public health problem. Heart Failure Clinics, 2(4), 379–393. doi:10.1016/j.hfc.2006.09.010.
Cribier, A., Eltchaninoff, H., Bash, A., Borenstein, N., Tron, C., Bauer, F., et al. (2002). Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description. Circulation, 106(24), 3006–3008.
Fioretta, E. S., Dijkman, P. E., Emmert, M. Y., & Hoerstrup, S. P. (2016). The future of heart valve replacement: recent developments and translational challenges for heart valve tissue engineering. Journal of Tissue Engineering and Regenerative Medicine. doi:10.1002/term.2326.
Schoen, F. J., & Gotlieb, A. I. (2016). Heart valve health, disease, replacement, and repair: a 25-year cardiovascular pathology perspective. Cardiovascular Pathology, 25(4), 341–352. doi:10.1016/j.carpath.2016.05.002.
Alexi-Meskishvilia, V., Ovroutskib, S., Ewertb, P., DaÈhnertb, I., Bergerb, F., Langeb, P. E., et al. (2000). Optimal conduit size for extracardiac Fontan operation. European Journal of Cardio-Thoracic Surgery, 18(690–695).
Yacoub, M. H., & Takkenberg, J. J. (2005). Will heart valve tissue engineering change the world? Nature Clinical Practice. Cardiovascular Medicine, 2(2), 60–61. doi:10.1038/ncpcardio0112.
Mendelson, K., & Schoen, F. J. (2006). Heart valve tissue engineering: concepts, approaches, progress, and challenges. Annals of Biomedical Engineering, 34(12), 1799–1819. doi:10.1007/s10439-006-9163-z.
Langer, R., & Vacanti, J. P. (1993). Tissue engineering. Science, 260(5110), 920–926.
Dohmen, P. M., Lembcke, A., Hotz, H., Kivelitz, D., & Konertz, W. F. (2002). Ross operation with a tissue-engineered heart valve. The Annals of Thoracic Surgery, 74(5), 1438–1442.
Dohmen, P. M., Lembcke, A., Holinski, S., Pruss, A., & Konertz, W. (2011). Ten years of clinical results with a tissue-engineered pulmonary valve. The Annals of Thoracic Surgery, 92(4), 1308–1314. doi:10.1016/j.athoracsur.2011.06.009.
Cebotari, S., Lichtenberg, A., Tudorache, I., Hilfiker, A., Mertsching, H., Leyh, R., et al. (2006). Clinical application of tissue engineered human heart valves using autologous progenitor cells. Circulation, 114(1 Suppl), I132–I137. doi:10.1161/CIRCULATIONAHA.105.001065.
Dohmen, P. M., Lembcke, A., Holinski, S., Kivelitz, D., Braun, J. P., Pruss, A., et al. (2007). Mid-term clinical results using a tissue-engineered pulmonary valve to reconstruct the right ventricular outflow tract during the Ross procedure. The Annals of Thoracic Surgery, 84(3), 729–736. doi:10.1016/j.athoracsur.2007.04.072.
Naito, Y., Imai, Y., Shin’oka, T., Kashiwagi, J., Aoki, M., Watanabe, M., et al. (2003). Successful clinical application of tissue-engineered graft for extracardiac Fontan operation. The Journal of Thoracic and Cardiovascular Surgery, 125(2), 419–420. doi:10.1067/mtc.2003.134.
Shinoka, T., & Breuer, C. (2008). Tissue-engineered blood vessels in pediatric cardiac surgery. Yale Journal of Biology and Medicine, 81, 161–166.
Bouten, C. V., Dankers, P. Y., Driessen-Mol, A., Pedron, S., Brizard, A. M., & Baaijens, F. P. (2011). Substrates for cardiovascular tissue engineering. Advanced Drug Delivery Reviews, 63(4–5), 221–241. doi:10.1016/j.addr.2011.01.007.
Fioretta, E. S., Fledderus, J. O., Burakowska-Meise, E. A., Baaijens, F. P., Verhaar, M. C., & Bouten, C. V. (2012). Polymer-based scaffold designs for in situ vascular tissue engineering: controlling recruitment and differentiation behavior of endothelial colony forming cells. Macromolecular Bioscience, 12(5), 577–590. doi:10.1002/mabi.201100315.
Dijkman, P. E., Fioretta, E. S., Frese, L., Pasqualini, F. S., & Hoerstrup, S. P. (2016). Heart valve replacements with regenerative capacity. Transfusion Medicine and Hemotherapy, 43(4), 282–290. doi:10.1159/000448181.
Cheung, D. Y., Duan, B., & Butcher, J. T. (2015). Current progress in tissue engineering of heart valves: multiscale problems, multiscale solutions. Expert opinion on biological therapy. [early online].
Jana, S., Tefft, B. J., Spoon, D. B., & Simari, R. D. (2014). Scaffolds for tissue engineering of cardiac valves. Acta Biomaterialia, 10(7), 2877–2893. doi:10.1016/j.actbio.2014.03.014.
Kurobe, H., Maxfield, M. W., Breuer, C. K., & Shinoka, T. (2012). Concise review: tissue-engineered vascular grafts for cardiac surgery: past, present, and future. Stem Cells Transl Med, 1(7), 566–571. doi:10.5966/sctm.2012-0044.
Patterson, J. T., Gilliland, T., Maxfield, M. W., Church, S., Naito, Y., Shinoka, T., et al. (2012). Tissue-engineered vascular grafts for use in the treatment of congenital heart disease: from the bench to the clinic and back again. Regenerative Medicine, 7(3), 409–419. doi:10.2217/rme.12.12.
Fioretta, E. S., Fledderus, J. O., Baaijens, F. P., & Bouten, C. V. (2012). Influence of substrate stiffness on circulating progenitor cell fate. Journal of Biomechanics, 45(5), 736–744. doi:10.1016/j.jbiomech.2011.11.013.
Tudorache, I., Horke, A., Cebotari, S., Sarikouch, S., Boethig, D., Breymann, T., et al. (2016). Decellularized aortic homografts for aortic valve and aorta ascendens replacement. European Journal of Cardio-Thoracic Surgery, 50(1), 89–97. doi:10.1093/ejcts/ezw013.
Sarikouch, S., Horke, A., Tudorache, I., Beerbaum, P., Westhoff-Bleck, M., Boethig, D., et al. (2016). Decellularized fresh homografts for pulmonary valve replacement: a decade of clinical experience. European Journal of Cardio-Thoracic Surgery. doi:10.1093/ejcts/ezw050.
Neumann, A., Cebotari, S., Tudorache, I., Haverich, A., & Sarikouch, S. (2013). Heart valve engineering: decellularized allograft matrices in clinical practice. Biomed Tech (Berl), 58(5), 453–456. doi:10.1515/bmt-2012-0115.
Cebotari, S., Tudorache, I., Ciubotaru, A., Boethig, D., Sarikouch, S., Goerler, A., et al. (2011). Use of fresh decellularized allografts for pulmonary valve replacement may reduce the reoperation rate in children and young adults: early report. Circulation, 124(11 Suppl), S115–S123. doi:10.1161/CIRCULATIONAHA.110.012161.
da Costa, F. D. A., Costa, A. C. B. A., Prestes, R., Domanski, A. C., Balbi, E. M., Ferreira, A. D. A., et al. (2010). The early and midterm function of decellularized aortic valve allografts. The Annals of Thoracic Surgery, 90(6), 1854–1860. doi:10.1016/j.athoracsur.2010.08.022.
Hoerstrup, S. P., Sodian, R., Daebritz, S., Wang, J., Bacha, E. A., Martin, D. P., et al. (2000). Functional living trileaflet heart valves grown in vitro. Circulation, 102(19 Suppl 3), III44–III49.
Hoerstrup, S. P., Cummings Mrcs, I., Lachat, M., Schoen, F. J., Jenni, R., Leschka, S., et al. (2006). Functional growth in tissue-engineered living, vascular grafts: follow-up at 100 weeks in a large animal model. Circulation, 114(1 Suppl), I159–I166. doi:10.1161/CIRCULATIONAHA.105.001172.
Shinoka, T., Ma, P. X., Shum-Tim, D., Breuer, C. K., Cusick, R. A., Zund, G., et al. (1996). Tissue-engineered heart valves. Autologous valve leaflet replacement study in a lamb model. Circulation, 94(9), II164–II168.
Weber, B., Scherman, J., Emmert, M. Y., Gruenenfelder, J., Verbeek, R., Bracher, M., et al. (2011). Injectable living marrow stromal cell-based autologous tissue engineered heart valves: first experiences with a one-step intervention in primates. European Heart Journal, 32(22), 2830–2840. doi:10.1093/eurheartj/ehr059.
Driessen-Mol, A., Emmert, M. Y., Dijkman, P. E., Frese, L., Sanders, B., Weber, B., et al. (2014). Transcatheter implantation of homologous “off-the-shelf” tissue-engineered heart valves with self-repair capacity: long-term functionality and rapid in vivo remodeling in sheep. Journal of the American College of Cardiology, 63(13), 1320–1329. doi:10.1016/j.jacc.2013.09.082.
Syedain, Z., Reimer, J., Schmidt, J., Lahti, M., Berry, J., Bianco, R., et al. (2015). 6-month aortic valve implantation of an off-the-shelf tissue-engineered valve in sheep. Biomaterials, 73, 175–184. doi:10.1016/j.biomaterials.2015.09.016.
Syedain, Z., Reimer, J., Lahti, M., Berry, J., Johnson, S., & Tranquillo, R. T. (2016). Tissue engineering of acellular vascular grafts capable of somatic growth in young lambs. Nature Communications, 7, 12951. doi:10.1038/ncomms12951.
Sievers, H.-H., Stierle, U., Schmidtke, C., & Bechtel, M. (2003). Decellularized pulmonary homograft (SynerGraft) for reconstruction of the right ventricular outflow tract: first clinical experience. [journal article]. Zeitschrift für Kardiologie, 92(1), 53–59. doi:10.1007/s00392-003-0883-x.
Hibino, N., McConnell, P., Shinoka, T., Malik, M., & Galantowicz, M. (2015). Preliminary experience in the use of an extracellular matrix (CorMatrix) as a tube graft: word of caution. Seminars in thoracic and cardiovascular surgery, doi:10.1053/j.semtcvs.2015.08.008.
Iop, L., & Gerosa, G. (2015). Guided tissue regeneration in heart valve replacement: from preclinical research to first-in-human trials. BioMed Research International, 2015, 432901. doi:10.1155/2015/432901.
Salmikangas, P., Schuessler-Lenz, M., Ruiz, S., Celis, P., Reischl, I., Menezes-Ferreira, M., et al. (2015). Marketing regulatory oversight of advanced therapy medicinal products (ATMPs) in Europe: the EMA/CAT perspective. Advances in Experimental Medicine and Biology, 871, 103–130. doi:10.1007/978-3-319-18618-4_6.
Yano, K., Watanabe, N., Tsuyuki, K., Ikawa, T., Kasanuki, H., & Yamato, M. (2015). Regulatory approval for autologous human cells and tissue products in the United States, the European Union, and Japan. Regenerative Therapy, 1, 45–56. doi:10.1016/j.reth.2014.10.001.
Sanzenbacher, R., Dwenger, A., Schuessler-Lenz, M., Cichutek, K., & Flory, E. (2007). European regulation tackles tissue engineering. Nat Biotech, 25(10), 1089–1091.
Commission Directive 2009/120/EC of 14 September 2009 amending Directive 2001/83/EC of the European Parliament and of the Council on the Community code relating to medicinal products for human use as regards advanced therapy medicinal products (2009). Official Journal of the European Union, 242, 3).
Lee, M. H., Arcidiacono, J. A., Bilek, A. M., Wille, J. J., Hamill, C. A., Wonnacott, K. M., et al. (2010). Considerations for tissue-engineered and regenerative medicine product development prior to clinical trials in the United States. Tissue Engineering. Part B, Reviews, 16(1), 41–54.
Lu, L., Arbit, H. M., Herrick, J. L., Segovis, S. G., Maran, A., & Yaszemski, M. J. (2015). Tissue engineered constructs: perspectives on clinical translation. Annals of Biomedical Engineering, 43(3), 796–804. doi:10.1007/s10439-015-1280-0.
Law, E. U. (2012). Proposal for a regulation of the European Parliament and of the council on medical devices. EUR-Lex, 52012PC0542, http://eur-lex.europa.eu/legal-content/EN/TXT/?uri=celex:52012PC50542.
Lichtenberg, A., Tudorache, I., Cebotari, S., Suprunov, M., Tudorache, G., Goerler, H., et al. (2006). Preclinical testing of tissue-engineered heart valves re-endothelialized under simulated physiological conditions. Circulation, 114(1 Suppl), I559–I565. doi:10.1161/CIRCULATIONAHA.105.001206.
Baraki, H., Tudorache, I., Braun, M., Hoffler, K., Gorler, A., Lichtenberg, A., et al. (2009). Orthotopic replacement of the aortic valve with decellularized allograft in a sheep model. Biomaterials, 30(31), 6240–6246. doi:10.1016/j.biomaterials.2009.07.068.
Iop, L., Bonetti, A., Naso, F., Rizzo, S., Cagnin, S., Bianco, R., et al. (2014). Decellularized allogeneic heart valves demonstrate self-regeneration potential after a long-term preclinical evaluation. PloS One, 9(6), e99593. doi:10.1371/journal.pone.0099593.
Row, S., Peng, H., Schlaich, E. M., Koenigsknecht, C., Andreadis, S. T., & Swartz, D. D. (2015). Arterial grafts exhibiting unprecedented cellular infiltration and remodeling in vivo: the role of cells in the vascular wall. Biomaterials, 50, 115–126. doi:10.1016/j.biomaterials.2015.01.045.
Koobatian, M. T., Row, S., Smith Jr., R. J., Koenigsknecht, C., Andreadis, S. T., & Swartz, D. D. (2016). Successful endothelialization and remodeling of a cell-free small-diameter arterial graft in a large animal model. Biomaterials, 76, 344–358. doi:10.1016/j.biomaterials.2015.10.020.
Simon, P., Kasimir, M. T., Seebacher, G., Weigel, G., Allrich, R., Salzer-Muhar, U., et al. (2003). Early failure of the tissue engineered porcine heart valve SYNERGRAFT in pediatric patients. European Journal of Cardio-Thoracic Surgery, 23(6), 1002–1006.
Voges, I., Brasen, J. H., Entenmann, A., Scheid, M., Scheewe, J., Fischer, G., et al. (2013). Adverse results of a decellularized tissue-engineered pulmonary valve in humans assessed with magnetic resonance imaging. European Journal of Cardio-Thoracic Surgery, 44(4), e272–e279. doi:10.1093/ejcts/ezt328.
Ruffer, A., Purbojo, A., Cicha, I., Glockler, M., Potapov, S., Dittrich, S., et al. (2010). Early failure of xenogenous de-cellularised pulmonary valve conduits—a word of caution! European Journal of Cardio-Thoracic Surgery, 38(1), 78–85. doi:10.1016/j.ejcts.2010.01.044.
Woo, J. S., Fishbein, M. C., & Reemtsen, B. (2015). Histologic examination of decellularized porcine intestinal submucosa extracellular matrix (CorMatrix) in pediatric congenital heart surgery. Cardiovascular Pathology. doi:10.1016/j.carpath.2015.08.007.
Watanabe, M., Shin’oka, T., Tohyama, S., Hibino, N., Konuma, T., Matsumura, G., et al. (2001). Tissue-engineered vascular autograft: inferior vena cava replacement in a dog model. Tissue Engineering, 7(4), 429–439.
Hoerstrup, S. P., Kadner, A., Melnitchouk, S., Trojan, A., Eid, K., Tracy, J., et al. (2002). Tissue engineering of functional trileaflet heart valves from human marrow stromal cells. Circulation, 106(suppl I), I-143–I-150. doi:10.1161/01.cir.0000032872.55215.05.
Frese, L., Sanders, B., Beer, G. M., Weber, B., Driessen-Mol, A., Baaijens, F. P. T., et al. (2015). Adipose derived tissue engineered heart valve. Journal of Tissue Science & Engineering, 06(03). doi:10.4172/2157-7552.1000156.
Sodian, R., Schaefermeier, P., Begg-Zips, S., Kuebler, W. M., Shakibaei, M., & Daebritz, S. (2010). Use of human umbilical cord blood-derived progenitor cells for tissue-engineered heart valves. Ann.Thorac.Surg., 89(3), 819–828.
Bayon, Y., Vertes, A. A., Ronfard, V., Egloff, M., Snykers, S., Salinas, G. F., et al. (2014). Translating cell-based regenerative medicines from research to successful products: challenges and solutions. Tissue Engineering. Part B, Reviews, 20(4), 246–256. doi:10.1089/ten.TEB.2013.0727.
Fioretta, E. S., Simonet, M., Smits, A. I., Baaijens, F. P., & Bouten, C. V. (2014). Differential response of endothelial and endothelial colony forming cells on electrospun scaffolds with distinct microfiber diameters. Biomacromolecules, 15(3), 821–829. doi:10.1021/bm4016418.
Nisbet, D. R., Forsythe, J. S., Shen, W., Finkelstein, D. I., & Horne, M. K. (2009). Review paper: a review of the cellular response on electrospun nanofibers for tissue engineering. Journal of Biomaterials Applications, 24(1), 7–29.
Jana, S., Tranquillo, R. T., & Lerman, A. (2016). Cells for tissue engineering of cardiac valves. Journal of Tissue Engineering and Regenerative Medicine, 10(10), 804–824. doi:10.1002/term.2010.
da Costa, F. D., Dohmen, P. M., Duarte, D., von Glenn, C., Lopes, S. V., Filho, H. H., et al. (2005). Immunological and echocardiographic evaluation of decellularized versus cryopreserved allografts during the Ross operation. European Journal of Cardio-Thoracic Surgery, 27(4), 572–578. doi:10.1016/j.ejcts.2004.12.057.
Dijkman, P. E., Driessen-Mol, A., Frese, L., Hoerstrup, S. P., & Baaijens, F. P. (2012). Decellularized homologous tissue-engineered heart valves as off-the-shelf alternatives to xeno- and homografts. Biomaterials, 33(18), 4545–4554. doi:10.1016/j.biomaterials.2012.03.015.
Syedain, Z. H., Meier, L. A., Reimer, J. M., & Tranquillo, R. T. (2013). Tubular heart valves from decellularized engineered tissue. Annals of Biomedical Engineering, 41(12), 2645–2654. doi:10.1007/s10439-013-0872-9.
Melchiorri, A. J., Hibino, N., Yi, T., Lee, Y. U., Sugiura, T., Tara, S., et al. (2015). Contrasting biofunctionalization strategies for the enhanced endothelialization of biodegradable vascular grafts. Biomacromolecules, 16(2), 437–446. doi:10.1021/bm501853s.
Tara, S., Kurobe, H., Maxfield, M. W., Rocco, K. A., Yi, T., Naito, Y., et al. (2015). Evaluation of remodeling process in small-diameter cell-free tissue-engineered arterial graft. Journal of Vascular Surgery, 62(3), 734–743. doi:10.1016/j.jvs.2014.03.011.
Talacua, H., Smits, A. I., Muylaert, D. E., van Rijswijk, J. W., Vink, A., Verhaar, M. C., et al. (2015). In situ tissue engineering of functional small-diameter blood vessels by host circulating cells only. Tissue Engineering. Part A, 21(19–20), 2583–2594. doi:10.1089/ten.TEA.2015.0066.
Ekdahl, K. N., Lambris, J. D., Elwing, H., Ricklin, D., Nilsson, P. H., Teramura, Y., et al. (2011). Innate immunity activation on biomaterial surfaces: a mechanistic model and coping strategies. Advanced Drug Delivery Reviews, 63(12), 1042–1050. doi:10.1016/j.addr.2011.06.012.
Smyth, J. V., Welch, M., Carr, H. M., Dodd, P. D., Eisenberg, P. R., & Walker, M. G. (1995). Fibrinolysis profiles and platelet activation after endothelial cell seeding of prosthetic vascular grafts. Annals of Vascular Surgery, 9(6), 542–546. doi:10.1007/BF02018827.
Laube, H. R., Duwe, J., Rutsch, W., & Konertz, W. (2000). Clinical experience with autologous endothelial cell-seeded polytetrafluoroethylene coronary artery bypass grafts. The Journal of Thoracic and Cardiovascular Surgery, 120(1), 134–141. doi:10.1067/mtc.2000.106327.
Zilla, P., Fasol, R., Deutsch, M., Fischlein, T., Minar, E., Hammerle, A., et al. (1987). Endothelial cell seeding of polytetrafluoroethylene vascular grafts in humans: a preliminary report. Journal of Vascular Surgery, 6(6), 535–541. doi:10.1016/0741-5214(87)90266-7.
Herring, M. B. (1991). Endothelial cell seeding. Journal of Vascular Surgery, 13(5), 731–732. doi:10.1016/0741-5214(91)90365-2.
Shi, Z., Neoh, K. G., & Kang, E. T. (2013). In vitro endothelialization of cobalt chromium alloys with micro/nanostructures using adipose-derived stem cells. Journal of Materials Science: Materials in Medicine, 24(4), 1067–1077. doi:10.1007/s10856-013-4868-7.
Kim, Y., & Liu, J. C. (2016). Protein-engineered microenvironments can promote endothelial differentiation of human mesenchymal stem cells in the absence of exogenous growth factors. Biomaterials Science, 4(12), 1761–1772. doi:10.1039/C6BM00472E.
Melchiorri, A. J., Hibino, N., & Fisher, J. P. (2013). Strategies and techniques to enhance the in situ endothelialization of small-diameter biodegradable polymeric vascular grafts. Tissue Engineering. Part B, Reviews, 19(4), 292–307. doi:10.1089/ten.TEB.2012.0577.
Lin, Q., Ding, X., Qiu, F., Song, X., Fu, G., & Ji, J. (2010). In situ endothelialization of intravascular stents coated with an anti-CD34 antibody functionalized heparin-collagen multilayer. Biomaterials, 31(14), 4017–4025. doi:10.1016/j.biomaterials.2010.01.092.
Rotmans, J. I., Heyligers, J. M., Verhagen, H. J., Velema, E., Nagtegaal, M. M., de Kleijn, D. P., et al. (2005). In vivo cell seeding with anti-CD34 antibodies successfully accelerates endothelialization but stimulates intimal hyperplasia in porcine arteriovenous expanded polytetrafluoroethylene grafts. Circulation, 112(1), 12–18. doi:10.1161/CIRCULATIONAHA.104.504407.
Lu, S., Zhang, P., Sun, X., Gong, F., Yang, S., Shen, L., et al. (2013). Synthetic ePTFE grafts coated with an anti-CD133 antibody-functionalized heparin/collagen multilayer with rapid in vivo endothelialization properties. ACS Applied Materials & Interfaces, 5(15), 7360–7369. doi:10.1021/am401706w.
Jordan, J. E., Williams, J. K., Lee, S. J., Raghavan, D., Atala, A., & Yoo, J. J. (2012). Bioengineered self-seeding heart valves. The Journal of Thoracic and Cardiovascular Surgery, 143(1), 201–208. doi:10.1016/j.jtcvs.2011.10.005.
Ravi, S., Qu, Z., & Chaikof, E. L. (2009). Polymeric materials for tissue engineering of arterial substitutes. Vascular, 17(Supplement 1), S45-S54, doi:10.2310/6670.2008.00084.
Zheng, W., Wang, Z., Song, L., Zhao, Q., Zhang, J., Li, D., et al. (2012). Endothelialization and patency of RGD-functionalized vascular grafts in a rabbit carotid artery model. Biomaterials, 33(10), 2880–2891. doi:10.1016/j.biomaterials.2011.12.047.
Caiado, F., Carvalho, T., Silva, F., Castro, C., Clode, N., Dye, J. F., et al. (2011). The role of fibrin E on the modulation of endothelial progenitors adhesion, differentiation and angiogenic growth factor production and the promotion of wound healing. Biomaterials, 32(29), 7096–7105. doi:10.1016/j.biomaterials.2011.06.022.
Rodenberg, E. J., & Pavalko, F. M. (2007). Peptides derived from fibronectin type III connecting segments promote endothelial cell adhesion but not platelet adhesion: implications in tissue-engineered vascular grafts. Tissue Engineering, 13(11), 2653–2666. doi:10.1089/ten.2007.0037.
Jun, H.-W., & West, J. L. (2005). Modification of polyurethaneurea with PEG and YIGSR peptide to enhance endothelialization without platelet adhesion. Journal of Biomedical Materials Research Part B: Applied Biomaterials, 72B(1), 131–139. doi:10.1002/jbm.b.30135.
Aubin, H., Mas-Moruno, C., Iijima, M., Schutterle, N., Steinbrink, M., Assmann, A., et al. (2016). Customized interface biofunctionalization of decellularized extracellular matrix: toward enhanced endothelialization. Tissue Engineering. Part C, Methods, 22(5), 496–508. doi:10.1089/ten.TEC.2015.0556.
Liu, P., Zhao, Y., Yan, Y., Hu, Y., Yang, W., & Cai, K. (2015). Construction of extracellular microenvironment to improve surface endothelialization of NiTi alloy substrate. Mater Sci Eng C Mater Biol Appl, 55, 1–7. doi:10.1016/j.msec.2015.05.047.
Smith Jr., R. J., Koobatian, M. T., Shahini, A., Swartz, D. D., & Andreadis, S. T. (2015). Capture of endothelial cells under flow using immobilized vascular endothelial growth factor. Biomaterials, 51, 303–312. doi:10.1016/j.biomaterials.2015.02.025.
Wang, H., Leinwand, L. A., & Anseth, K. S. (2014). Cardiac valve cells and their microenvironment—insights from in vitro studies. Nature Reviews. Cardiology, 11(12), 715–727. doi:10.1038/nrcardio.2014.162.
Yin, Y., Zhao, X., Fang, Y., Yu, S., Zhao, J., Song, M., et al. (2010). SDF-1α involved in mobilization and recruitment of endothelial progenitor cells after arterial injury in mice. Cardiovascular Pathology, 19(4), 218–227. doi:10.1016/j.carpath.2009.04.002.
Liu, T., Liu, S., Zhang, K., Chen, J., & Huang, N. (2014). Endothelialization of implanted cardiovascular biomaterial surfaces: the development from in vitro to in vivo. Journal of Biomedical Materials Research. Part A, 102(10), 3754–3772. doi:10.1002/jbm.a.35025.
Emmert, M. Y., & Hoerstrup, S. P. (2016). Tissue engineered heart valves: moving towards clinical translation. Expert Review of Medical Devices, 13(5), 417–419. doi:10.1586/17434440.2016.1171709.
Beebe, D. J., Ingber, D. E., & den Toonder, J. (2013). Organs on chips 2013. Lab on a Chip, 13(18), 3447–3448. doi:10.1039/c3lc90080k.
Ram-Liebig, G., Bednarz, J., Stuerzebecher, B., Fahlenkamp, D., Barbagli, G., Romano, G., et al. (2015). Regulatory challenges for autologous tissue engineered products on their way from bench to bedside in Europe. Advanced Drug Delivery Reviews, 82-83, 181–191. doi:10.1016/j.addr.2014.11.009.
Hurtado-Aguilar, L. G., Mulderrig, S., Moreira, R., Hatam, N., Spillner, J., Schmitz-Rode, T., et al. (2016). Ultrasound for in vitro noninvasive, real time monitoring and evaluation of tissue-engineered heart valves. Tissue Engineering. Part C, Methods. doi:10.1089/ten.TEC.2016.0300.
Ozaki, S., Herijgers, P., & Flameng, W. (2004). A new model to test the calcification characteristics of bioprosthetic heart valves. Annals of Thoracic and Cardiovascular Surgery, 10, 23–28.
Taramasso, M., Emmert, M. Y., Reser, D., Guidotti, A., Cesarovic, N., Campagnol, M., et al. (2015). Pre-clinical in vitro and in vivo models for heart valve therapies. Journal of Cardiovascular Translational Research, 8(5), 319–327. doi:10.1007/s12265-015-9631-7.
Yuan, S. M., Mishaly, D., Shinfeld, A., & Raanani, E. (2008). Right ventricular outflow tract reconstruction: valved conduit of choice and clinical outcomes. Journal of Cardiovascular Medicine, 9, 327–337.
Bayon, Y., Vertes, A. A., Ronfard, V., Culme-Seymour, E., Mason, C., Stroemer, P., et al. (2015). Turning regenerative medicine breakthrough ideas and innovations into commercial products. Tissue Engineering. Part B, Reviews, 21(6), 560–571. doi:10.1089/ten.TEB.2015.0068.
de Wilde, S., Guchelaar, H. J., Herberts, C., Lowdell, M., Hildebrandt, M., Zandvliet, M., et al. (2016). Development of cell therapy medicinal products by academic institutes. Drug Discovery Today, 21(8), 1206–1212. doi:10.1016/j.drudis.2016.04.016.
Acknowledgments
The authors have received funding support from the European FP 7 Framework Programme under grant agreement no. 604514 (ImaValve).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
Associate Editor Adrian Chester oversaw the review of this article
Maximilian Y. Emmert and Emanuela S. Fioretta contributed equally.
Rights and permissions
About this article
Cite this article
Emmert, M.Y., Fioretta, E.S. & Hoerstrup, S.P. Translational Challenges in Cardiovascular Tissue Engineering. J. of Cardiovasc. Trans. Res. 10, 139–149 (2017). https://doi.org/10.1007/s12265-017-9728-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-017-9728-2