Abstract
Sialolithiasis is the most common pathology of the salivary gland characterized by the development of salivary stones, known as calculi or sialoliths. Sialoliths commonly measure between 5 and 10 mm in size, and all stones over 10 mm can be reported as sialoliths of unusual size. Sialolith of more than 15 mm is defined as giant sialolith and is extremely rare. Most salivary sialolith occurs in the submandibular gland duct, especially located in the distal third of the duct. The main signs and symptoms are local pain and swelling. The treatment option to remove the sialolith is according to its size and location. For giant sialolith, surgical removal with or without the gland excision needs to be considered. Here, we report a case of giant submandibular gland sialolith of 35 mm in greatest dimension. And this is the first reported case of giant salivary gland duct sialolith discharged spontaneously.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The term sialolithiasis is derived from the Greek words sialon (saliva) and lithos (stone), and the Latin-iasis meaning “process” or “morbid condition” [1]. Most salivary calculi (80–95%) occur in the submandibular gland, whereas 5 to 20% are found in the parotid gland [2, 3]. The sublingual gland and minor salivary glands are rarely (1–2%) affected [2]. In the literature, sialolith size ranges from less than 1 to 72 mm [4]. Sialoliths commonly measure between 5 and 10 mm in size, and giant sialoliths are classified as those exceeding 1 g in weight or 15 mm [2] or 35 mm [4] in any one dimension. Giant salivary sialoliths are rarely reported. Furthermore, there has been no report of an unusual or giant sialolith discharged spontaneously.
Report of Case
A 29-year-old man presented to the emergency room of the dental department complaining of a rapid growth yellow-solid mass in the right sublingual region for 3 days. He reported no obvious pain or edema or any other clinical symptom presence apart from uncomfortable when swelling 3 days ago, so he did not receive any examination before. Intraoral examination showed a cylinder-shaped yellow mass in the orifice of the right submandibular gland duct. Bimanual palpation revealed a hard mass measuring approximately 40 mm in length; the diameter of the mass in the duct seems to be larger than the exposed half. The diagnosis was made only based on clinical examination and direct visualization of the mass exposed in oral (Fig. 1). The patient had not undergone ultrasonic or radiographic examinations like computed tomography (CT) or magnetic resonance imaging (MRI). Removal of the sialolith was performed directly by the use of mosquito forceps in the emergency room under local anesthesia but without incision. The lacerated tissue around the duct orifice was partially sutured (Fig. 2a). The sialolith measured approximately 35 mm in length and its dehydrated weight was 14.9 g (Fig. 2b). The patient was recalled 1 month after operation; secretion of saliva from the orifice of the submandibular duct was observed.
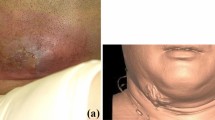
Intraoral view showing the yellowish, cylindrical sialolith partially excluded from the orifice of right submandibular gland duct. The exposed part of the sialolith in the mouth was about 10 mm in length. Surrounding mucosa was normal in color. Poor oral hygiene could be seen and moderate gingivitis with a wider band of inflammation accompanied by yellowish dental calculus was visible. a Anterior view of the sialolith. b Lateral view of the sialolith
a An enlarged submandibular duct orifice could be seen after removal of the sialolith. Conversely, the orifice of the left submandibular gland duct is not as obviously as the right one. The arrow showing the lacerated mucosa on the inner side of the orifice. The lacerated mucosa was rotated outward with an everted suture in order to keep the ductal orifice open. b Giant sialolith removed from the right submandibular duct. The yellowish sialolith measured 35 mm in length and 5 mm in width. The exposed part in the mouth is cylinder-shaped; the surface of this part is not very smooth, whereas the other part which is in the duct is spindle-shaped with a much smooth surface
Discussion
Sialoliths are mainly composed of inorganic material. Carbonate apatite was identified in 99% of the stones, phosphate in 88%, calcium in 87%, magnesium in 68%, struvite in 44%, oxalate in 38%, and carbonate in 35% [5]. The exact mechanism of lithogenesis of salivary stones is not completely understood. Kraaij et al. [6] revealed that systemic diseases, medication, smoking, and alcohol consumption play no or only a limited role in the onset of salivary stones. Kati et al. [7] found that for patients who have kidney stones, the percentage of dental calculus formation was significantly higher than the patients without stones. They wondered the formation of a visible stone, such as dental calculus, may be an indicator of other types of stones, such as kidney stones. In our case, according to the results of the clinical oral examination, we could see the young male patient of poor oral hygiene; moderate gingivitis with a wider band of inflammation accompanied by yellowish dental calculus was visible. However, no evidence is available to support whether there is a correlation between dental calculus and the formation of sialolith.
The ability of a sialolith to grow and become a giant sialolith depends mainly on the reaction of the affected duct. It might be asymptomatic for a long period if the duct adjacent to the sialolith is able to dilate, allowing nearly normal secretion of the saliva around the stone, and eventually, a giant calculus will be created [2]. As the stone increases in size beyond the ability of the duct to dilate, a sialo-oral fistula will develop and the sialolith will partially protrude into the oral cavity [2]. In this particular case, nearly half of the sialolith excluded from the opening of the right submandibular gland duct within 3 days. Fortunately, no symptom such as pain or abscess related to obstructive sialolithiasis was presented before. Based on 120 submandibular gland sialendoscopy studies, Marchal et al. [8] observed the presence of a sphincter system in the first 3 cm of Wharton’s duct in 90% of their studied cases and suggested that variation of such sphincter-like mechanism within the salivary ducts could be responsible for easier retrograde migration of oral materials. In the present case, the sialolith was located in the distal third of Wharton’s duct, 35 mm in length, and fusiform-formed end. We concluded that the presence of the sphincter-like system together with the sialolith’s location and its three-dimensional appearance attributed most for the reasons why the sialolith could be excluded spontaneously.
Conclusion
The etiology of sialoliths remains unclear; hence, it is of great importance to provide information to clarify the etiopathogenesis of salivary stones, to facilitate diagnosis, to prevent formation, and to improve treatment. Salivary gland fibrosis and dysfunction could be avoided if diagnosis and treatment performed early.
References
Sengupta S, Bose S (2018) Sialolithiasis of right submandibular duct of unusual size. Indian J Surg 80(2):190–191. https://doi.org/10.1007/s12262-018-1723-6
Bodner L (2002) Giant salivary gland calculi: diagnostic imaging and surgical management. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology 94(3):320–323. https://doi.org/10.1067/moe.2002.123863
Sigismund PE, Zenk J, Koch M, Schapher M, Rudes M, Iro H (2015) Nearly 3,000 salivary stones: some clinical and epidemiologic aspects. Laryngoscope 125(8):1879–1882. https://doi.org/10.1002/lary.25377
Rai M, Burman R (2009) Giant submandibular sialolith of remarkable size in the comma area of Wharton’s duct: a case report. J Oral Maxil Surg 67(6):1329–1332. https://doi.org/10.1016/j.joms.2008.11.014
Kraaij S, Brand HS, van der Meij EH, de Visscher JG (2018) Biochemical composition of salivary stones in relation to stone- and patient-related factors. Med Oral Patol Oral Cir Bucal 23(5):e540–e544. https://doi.org/10.4317/medoral.22533
Kraaij S, Karagozoglu KH, Kenter YAG, Pijpe J, Gilijamse M, Brand HS (2015) Systemic diseases and the risk of developing salivary stones: a case control study. Oral Surg Oral Med Oral Pathol Oral Radiol 119(5):539–543. https://doi.org/10.1016/j.oooo.2015.01.010
Kati B, Kalkan E, Pelit ES, Yagmur I, Ciftci H (2018) Do dental calculi predict the presence of renal stones? Arch Ital Urol Androl 90(3):159–162. https://doi.org/10.4081/aiua.2018.3.159
Marchal F, Kurt AM, Dulguerov P, Lehmann W (2001) Retrograde theory in sialolithiasis formation. Arch Otolaryngol Head Neck Surg 127(1):66–68. https://doi.org/10.1001/archotol.127.1.66
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, W., Wang, K. & Yang, F. Spontaneous Discharged Submandibular Gland Duct Sialolith: Α Rare Case Report. Indian J Surg 82, 205–207 (2020). https://doi.org/10.1007/s12262-019-01927-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-019-01927-y