Abstract
The purpose of this prospectively collected database is to evaluate the safety of placement of a feeding jejunostomy (FJ) in patients undergoing upper gastrointestinal surgery and evaluating the gastrointestinal (GI) and mechanical complications. A total of 46 consecutive patients who underwent upper gastrointestinal surgery for various benign and malignant diseases were included. All of these patients underwent Witzel feeding jejunostomy at the time of laparotomy. The patients were followed postoperatively to record the gastrointestinal and/or mechanical complications that occurred during the hospital stay of the patients. Feeding jejunostomy could be performed in 100% of the patients and postoperatively, jejunostomy feeds could be started in 97.8% of the patients. 34.8% of the patients underwent an emergency laparotomy; 81.25% of the patients in the emergency group developed a significant postoperative FJ related complications with significant mechanical complications in the emergency group. GI complications were 82.14%; diarrhea was the most frequently encountered (69.5%). GI complications were more frequent and significant in patients with a low preoperative serum albumin (< 3.5 g/dl). No mortalities were recorded as a direct consequence of a FJ. Jejunostomy feeding is an excellent method of providing enteral nutritional support in patients undergoing major abdominal surgery and in patients with upper aero digestive tract pathologies who cannot be fed by mouth. Tube feeding is associated with complications which are minor and self-limiting or can be managed by simple bedside maneuvers. Feeding jejunostomy should be considered in all patients who may require short- or long-term enteral nutrition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients undergoing upper gastrointestinal surgery are at a high risk of developing malnutrition because oral intake is often interrupted. The nutritionally depleted patients are at a high risk of postoperative complications. Nutritional support is a treatment modality that may directly impact outcomes [1, 2]. Providing support for patient’s postoperative nutritional requirements has become an important part of perioperative period until they can be fed by mouth [3, 4]. The benefits of early postoperative nutritional support include early recovery and decreased complications. The current guidelines of the European Society for Parenteral and Enteral nutrition (ESPEN) recommend routine use of early enteral nutrition in patients undergoing major gastrointestinal surgery for cancer [5]. The preferred feeding strategies include nasojejunal tube feeding, jejunostomy tube feeding, and parenteral nutrition [6]. However, none of the analyzed feeding strategies in this study were found superior with respect to time to resumption of normal oral intake, morbidity, and mortality.
Feeding jejunal tubes provide an excellent method for postoperative enteral nutritional support [4, 7, 8]. The indications for this type of feeding are increasing and include a variety of clinical conditions. Placement of a feeding jejunostomy (FJ) is often preferred during esophagectomy [3, 9], pancreaticoduodenectomy [10, 11], gastrectomy [12], pancreatic necrosectomy [13], acute corrosive injury [14], and for upper respiratory tract malignancies [15]. A potential benefit of placing a surgical jejunostomy tube is to provide a “safety valve” in case of delay in resumption of oral intake. Another reason is to provide early enteral nutrition to reduce postoperative complications [9].
The presence of a jejunostomy tube allows enteral therapy for longer periods especially in patients with complications, thus avoiding the need for parenteral nutrition [4]. Jejunostomy tube placement is reported to result in shorter hospital stay and reduces postoperative complications [4, 16, 17].
Methodology
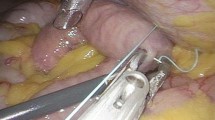
This was a prospective, observational audit conducted in a tertiary care hospital of northern India. The study included 46 consecutive patients of either sex and of age more than 18 years, who underwent placement of a FJ. Those patients who were less than 18 years of age or had a FJ tube placed in another facility were not included in the study. All of these patients underwent a Witzel’s feeding jejunostomy at the time of laparotomy using a 12F or 14F nasogastric tube (Figs. 1, 2, 3, 4). Enteral tube feeds were started on the second or third postoperative day depending on the clinical condition of the patient. Over the next 24–28 h, the volume and concentration of the feeds were gradually increased to achieve the target calorie requirement of the patient. The tube was flushed clean with 20–40 cm3 normal saline after each feed.
The patients were assessed for development gastrointestinal or mechanical complications, and these were recorded.
All data was entered on a personal computer in Microsoft Excel/SPSS software. The data was analyzed using SPSS software. During analysis of data, continuous variables were compared using the student t test. Dichotomous variables (e.g., sex) were compared using the chi-square test. Descriptive statistics were used wherever required. Where appropriate, differences in distribution were tested with the ×2 or Fischer’s exact test. Other statistical methods were utilized wherever appropriate. The p value less than 0.05 was considered statistically significant.
Results
Demographics
Forty-six patients were included in the study. The age of the patients in the study ranged from 18 to 87 years, majority of the patients were in the age group of 55 to 75 years with a mean of 57.15 (± 15.39). Males were predominant in the study (33 males and 13 females). Male to female ratio was 2.5:1. Twenty-two males (66.7%) and six females (46.1%) suffered from postoperative complications related to the placement of a feeding jejunostomy.
Twenty-four patients (52.17%) had co-morbidities such as diabetes mellitus, hypertension, heart disease, or an immunodeficient condition (chemotherapy/corticosteroid intake) and were part of the study group. Fourteen patients (58.34%) had diabetes mellitus, 19 patients (79.17%) had hypertension, ten patients (41.67%) were suffering from coronary artery disease, and seven patients (29.17%) had an immunodeficient condition such as corticosteroid intake or chemo/radiotherapy.
Discontinuation of Feeding
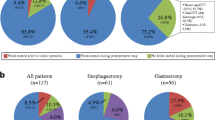
Forty-five patients (97.8%) were started on enteral feeds via the feeding jejunostomy as per the study guidelines. Only one patient was not started on enteral feeds in view of critical condition and worsening clinical parameters. Enteral feeds were discontinued in 12 patients (26.1%). Out of the 12 patients, in eight patients (66.67%), the enteral feeding via a jejunostomy was discontinued temporarily and restarted and in four patients (33.34%), the enteral feeds via feeding jejunostomy had to be stopped permanently.
The most common reason for temporary discontinuation of enteral feeds was abdominal bloating, observed in five patients (62.5%) for which no intervention was required and the feeds were restarted after 1 day of discontinuation. Two patients (25%) were re-operated, one for a mesenteric bleed and the other for band intestinal obstruction and the feeds were restarted within 1 and 4 days, respectively. One patient (12.5%) had a complete tubal blockage for which a feeding tube-related intervention was done, and the tube was withdrawn by 1 cm and feeds were continued thereon after a discontinuation of 1 day.
In four patients (33.34%), the feeding had to be stopped permanently. The reasons for permanent discontinuation of feeds were intestinal perforation along the feeding tube (one patient), enterocutaneous fistula (one patient), persistent high-nasogastric output (one patient), and worsening general condition and clinical parameters (one patient).
Complications in Emergency Surgery
Sixteen patients (34.8%) underwent an emergency surgical procedure along with placement of a feeding jejunostomy. Thirteen patients (81.25%) out of the 16 patients who underwent an emergency surgical procedure experienced a feeding jejunostomy-related complication. On evaluation, the incidence of complications in an emergency surgery was calculated to be statistically significant with a p value = 0.039.
Nine patients (56.3%) had a gastrointestinal complication out of the emergency surgery group but the results were not statistically significant; p value = 0.536.
Five patients (38.46%) who underwent an emergency surgery had a postoperative mechanical complications which was calculated to be statistically significant; p value = 0.04.
Gastrointestinal Complications
Twenty-three patients (82.14%) developed gastrointestinal-related complications after the placement of a feeding jejunostomy. The most frequently encountered gastrointestinal complication was diarrhea, occurring in 16 patients (69.5%), followed by abdominal bloating in eight patients (34.7%). Five patients (21.7%) complained of nausea/vomiting, two patients (8.6%) developed constipation, and one patient (4.3%) each developed abdominal cramps and aspiration pneumonitis, respectively.
A statistically significant correlation was retrieved between the incidence of gastrointestinal complications and low-preoperative serum albumin levels (< 3.5 g/dl) suggesting that low-preoperative serum albumin levels are directly linked with postoperative gastrointestinal complications associated with the placement of a feeding jejunostomy with a p value of 0.04.
Mechanical Complications
Seven patients (15.2%) developed mechanical complications due to a feeding jejunostomy. Five patients (71.4%) developed localized skin ulceration, erosion, or necrosis around the feeding jejunostomy site. One of these patients also had an intestinal perforation along the feeding tube, the exact cause of which could not be assessed (14.2%). Two patients (28.5%) developed feeding tube obstruction out of which one patient had a partial obstruction, and feeds were continued at a slower rate, and the other patient had a complete feeding tube obstruction postoperatively for which a bedside intervention of withdrawal of the feeding tube by 1 cm was done which facilitated feeding through the tube thereon at the recommended rate. These findings were not statistically significant.
Discussion
Enteral feeding via a feeding tube is considered a standard practice for patients undergoing major gastrointestinal surgery for malignant and non-malignant conditions. Enteral feeding aims to maintain nutrition postoperatively and prevents complications associated with lack of nutrition. Many studies have emphasized the beneficial effects of a feeding jejunostomy to maintain postoperative nutrition in patients who are unable to withstand oral nutritional support. Enteral feeding via a tube jejunostomy is not without complications as reported in literature by various authors, and there is considerable debate over the severity and frequency of complications arising from a tube jejunostomy. The common gastrointestinal complications include diarrhea and abdominal distension [8], and the major mechanical problems reported include enteral migration of the tube [7], jejunojejunal intussusception [18], intraperitoneal leakage, and catheter occlusion [19].
Gastrointestinal Complications
Out of the 23 patients who suffered a gastrointestinal complication, 17 patients (73.9%) had a low-preoperative serum albumin level and six patients (26.08%) had a normal preoperative albumin level. This difference was statistically significant, p = 0.04, suggesting that a low-preoperative serum albumin level is a risk factor for developing postoperative feeding jejunostomy-related complication.
In a study of 204 patients undergoing the placement of a feeding jejunostomy at the time of an esophagectomy, 30 patients developed feed-related complications out of which 16 patients (53.34%) developed diarrhea and 14 patients (46.67%) developed abdominal distension. Most of these patients could tolerate the feeds. Only a few developed minor complications, which could be managed by simple bedside maneuvers. Further, in this study, there were no significant results correlating preoperative serum albumin levels and the incidence of postoperative complications [8].
Many authors report the deleterious effects of a feeding jejunostomy and discourage their routine use. In a study conducted on patients undergoing feeding jejunostomy tube placement at the time of pancreaticoduodenectomy, 126 patients were included and 18 patients (14%) had complications related to the feeding jejunostomy, with primary catheter malfunction (seven patients) as the most common feeding tube-related complication, followed by peritubal infection (six patients), pneumatosis intestinalis (four patients), and severe feed intolerance in three patients. The study also concluded that preoperative hypoalbuminemia was an independent factor for the frequency of complications noted during the study. The author concluded that feeding jejunostomy-related morbidity is common and associated with inferior outcomes following pancreaticoduodenectomy [11].
Mechanical Complications
In our study, no major surgical intervention was required for any of the mechanical complication encountered in the study and the complications could be managed by bedside maneuvers.
In a study, conducted by Srinathan et al., 111 patients underwent an esophagectomy for carcinoma and 103 patients had a jejunostomy tube placed. Six patients (5.4%) experienced complications attributable solely to a jejunostomy tube. Three patients (2.9%) required a surgical intervention for jejunal ischemia, bowel obstruction and jejunal perforation, and a small bowel leak and with a localized abscess. The other three patients had a jejunal site-related skin infection for which two patients were managed by tube removal, and one patient was managed by antibiotics. The study concluded that, for certain group of patients as those with substantial weight loss before surgery, a jejunostomy tube may be reasonable. Jejunostomy tubes can lead to serious complications and frequent but less serious adverse events in a group of patients already at high risk for complications. They concluded that placement of a jejunostomy tube was unreasonable in the absence of convincing evidence in the literature [9].
There are contrasting studies that suggest that jejunostomy tube feeding is a safe adjunct to major abdominal surgeries despite of its minor complications.
A retrospective study was conducted by Masry et al., in which 36 patients who underwent pancreatic surgeries and a feeding tube placement for nutritional support were analyzed for tube-related complications. Eight patients had complications directly attributable to the tube including, blockage, dislodgement, pericatheter leakage, and peritonitis in a patient with downstream adhesive obstruction. Twenty patients suffered complications that included transient diarrhea, abdominal distension, nausea/vomiting, and pain. They concluded that although providing nutrition by the enteral route can be a challenging exercise in pancreatic patients who typically have two or more vulnerable upper intestinal anastomosis, bilio-pancreatic insufficiency, and gastric stasis. Despite many minor shortcomings, jejunostomy tube feeding appeared to be a safe adjunct to pancreatic surgery [20].
In another recent study, a retrospective analysis was done to evaluate the placement of a feeding jejunostomy in resection of gastric cancers in 2980 subjects. Seven hundred fifteen subjects had a feeding jejunostomy tube placed as part of their primary procedure. The two groups, feeding tube placed and non-feeding tube groups, were compared, and there were no statistically significant differences in the 30-day overall complications (p = 0.320) or mortality (p = 0.08). There were also no differences in the major complications, surgical site infections, or early reoperation. They concluded that although, concomitant placement of a feeding jejunostomy tube at the time of gastrectomy may result in slightly increased operative times but does not appear to lead to increased perioperative morbidity or mortality [1].
Conclusion
During the course of our study, we found that gastrointestinal complications were more frequently encountered as compared to the mechanical complications. The most common gastrointestinal complications were diarrhea (69.5%) and abdominal bloating (34.7%). The most common mechanical complications were skin erosion/ulceration (71.4%) and tube obstruction (28.5%). The complications encountered were minor and could be managed conservatively or by bedside maneuvers.
We concluded that, in an emergency surgical setting, the complications associated with a feeding jejunostomy tube placement were frequent. The patients undergoing a feeding tube placement as part of an emergency procedure had a statistically significant incidence of developing postoperative tube-related complications. The mechanical complications were predominant in an emergency setting than the gastrointestinal complications.
We could also demonstrate through our study, the higher incidence of gastrointestinal complications in the patients with a low-preoperative serum albumin levels (< 3.5 g%). Our results were statistically significant, p = 0.04, suggesting that poor nutritional status corresponds as an independent risk factor for the development of postoperative gastrointestinal complications in these patients.
We recommend that a feeding jejunostomy is a safe and effective route to provide enteral nutrition to patients undergoing major abdominal surgery. Tube feeding is not free from complications, but the complications encountered are minor and self-resolving or can be managed by simple bedside maneuvers. In an emergency setting, precision and proper technique should be followed to avoid complications. Also improving serum albumin levels preoperatively may also reduce the incidence of complications associated with feeding jejunostomy.
References
Sun Z, Shenoi MM, Nussbaum DP, Keenan JE, Gulack BC, Tyler DS, Speicher PJ, Blazer DG III (2016) Feeding jejunostomy tube placement during resection of gastric cancer. J Surg Res 200(1):189–194. https://doi.org/10.1016/j.jss.2015.07.014
Boukerrouche A (2015) Complications associated with enteral nutrition using tube jejunostomy after esophageal reconstruction. J Gastrointest Dig Syst 5:252. https://doi.org/10.4172/2161-069x.10000252
Huang K, Wu B, Ding X et al Post esophagectomy tube feeding: a retrospective comparison of jejunostomy and a novel gastrostomy feeding approach. PLoS One 9(3):e89190. https://doi.org/10.1371/journal.pone.0089190
Torres LG, de Vasvasconcellor Santos FA, Correia MLTD (2014) Randomized clinical trial: nasoenteral tube or jejunostomy as a route for nutrition after major upper gastrointestinal operations. World J Surg 38(9):2241–2246. https://doi.org/10.1007/s00268-014-2589-9
Weimann A, Braga M, Harsanyi L, Laviano A, Ljungqvist O, Soeters P, DGEM (German Society for Nutritional Medicine), Jauch KW, Kemen M, Hiesmayr JM, Horbach T, Kuse ER, Vestweber KH, ESPEN (European Society for Parenteral and Enteral Nutrition) (Apr 2006) ESPEN guidelines on enteral nutrition: surgery including organ transplantation. Clin Nutr 25(2):224–244. https://doi.org/10.1016/j.clnu.2006.01.015
Gerritsen A, Besselink MC, Cieslak KP et al (2012) Efficacy and complications of nasojejunal, jejunostomy and parenteral feeding after pancreaticoduodenectomy. J Gastrointest Surg 16(6):1144–1151. https://doi.org/10.1007/s11605-012-1887-5
Ozben V, Karatas A, Atasoy D et al (2011) A rare complication of jejunostomy tube: enteral migration. Turk J Gastroentral 22(1):83–85. https://doi.org/10.4318/tjg.2011.0162
Gupta V (2009) Benefit versus risks: a prospective audit. Feeding jejunostomy tube during esophagectomy. World J Surg 33(7):1432–1438. https://doi.org/10.1007/s00268-009-0019-1
Srinathan SK, Hamin T, Walter S, Tan AL, Unruh HW, Guyatt G (2013) Jejunostomy tube feeding in patients undergoing esophagectomy. Can J Surg 56(6):409–413. https://doi.org/10.1503/cjs.008612
Padussis JC, Zani S, Blazer DG, Tyler DS, Pappas TN, Scarborough JE (2014) Feeding jejunostomy during Whipple’s is associated with increased morbidity. J Surg Res 187(2):361–366. https://doi.org/10.1016/j.jss.2012.10.010
Nussbaun DP, Zani S, Penne K, et al (2014) Feeding jejunostomy tube placement in patients undergoing pancreaticoduodenectomy: an ongoing dilemma. J Gastrointest Surg 18(10):1752–1759
Patel SH, Kooby DA, Staley CA, Maithal SK (2013) An assessment of feeding jejunostomy tube placement at the time of resection for gastric adenocarcinoma. J Surg Oncol 107(7):728–734. https://doi.org/10.1002/jso.23324
Mangiante G, Rodella L, Cerofolini A, Giacopuzzi S, Passeri V, Sterzi E, Catalano F, Schenal G, de Manzoni G (2013) Severe necrotic and septic pancreatitis: indications to endoscopic, surgical and nutritional therapy. G Chir 34(9-10):284–287
Kochhar R, Poornachandra KS, Puri P, Dutta U, Sinha SK, Sethy PK, Wig JD, Nagi B, Singh K (2009) Comparative evaluation of nasoenteral feeding and jejunostomy feeding in acute corrosive injury: a retrospective analysis. Gastrointest Endose 70(5):874–880. https://doi.org/10.1016/j.gie.2009.03.009
Rezaii J, Hajimohamadi F, Esfandian K et al (2008) Time of jejunostomy after upper gastrointestinal and respiratory tract cancers would be affecting on complications of jejunostomy. J Med Sci 8:583–586
Ghafouri A, Salehi OA, Keshavarz SA, Hosseini S, Shojaifard A, Khorgami Z (2012) Evaluation of supporting role of early enteral feeding via tube jejunostomy following resection of upper gastrointestinal tract. Med J Islam Repub Iran 26(1):7–11
Wani ML, Ahangar AG, Lone GN, Singh S, Dar AM, Bhat MA, Lone RA, Irshad I (2010) Feeding jejunostomy: does the benefit outweigh the risk (a retrospective study from a single centre). Int J Surg 8(5):387–390. https://doi.org/10.1016/j.ijsu.2010.05.009
Maheshwari G, Maheshwari N (2014) Jejunojejunal intussuception after feeding jejunostomy: a rare complication of a common surgery. JMED Res 2014:483746. https://doi.org/10.5171/2014.483746
Sonowane RN, Thombare MM, Kumar A et al (1997) Technical complications of feeding jejunostomy: a critical analysis. Trop Gastroenterel 18:127–128
El-Masry NS (2002) The role of T-tube feeding jejunostomy in patients with pancreatic surgery. Egypt J Surg 21:978–982
Funding
This was an independent study as part of a 3-year residency program and did not receive any funding from any organization nor did it have any bias.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Justification
According to guidelines setup by ICMR (1994) and Helsinki declaration (modified 1989), the following will be adhered to all patients and volunteers involved in the study. All the possible treatment options will be given, and none will be withheld. Patients will be enrolled in the study with their knowledge, and study will be done by utilizing known investigation modalities, regarding which proper information will be provided to the patients. Patient will be given the option of quitting from the study during the protocol if he or she desires; no element of compulsion will be extorted. Confidentiality of data due to contribution source or individual will be given. Written informed consent will be obtained from all the patients included in the study. In the cases where the patients are not eligible for giving consent due to poor neurological status, consent of the close relative available will be taken. There will be no difference in the management of the patients, and all the patients will be treated by standard protocol of the department of General Surgery, Fortis Hospital, Mohali, in the best interest of the patient.
Rights and permissions
About this article
Cite this article
Bansal, S., Singh, I., Maheshwari, G. et al. A Clinical Study of the Morbidity Associated with the Placement of a Feeding Jejunostomy. Indian J Surg 81, 37–42 (2019). https://doi.org/10.1007/s12262-017-1709-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-017-1709-9