Abstract
The advent of information and communication technology in healthcare sector has taken the world to a new pervasive horizon. Cloud computing is a ubiquitous way of information and data transfer. Implementation of cloud computing in daily healthcare operations can bring numerous benefits. However, there is a resistance towards the usage of this modern technology by healthcare organizations and staff due to lack of IT exposure, resources, infrastructure, patient data privacy, and security issues. Therefore, there is a need to provide an empirical evidence on how healthcare industry is responding to this new technology and to point out the factors that hinder its implementation in healthcare sector. In this paper, we aim to conduct an empirical study to investigate the behavioural intention of healthcare organizations’ staff, towards the usage of cloud-based healthcare services to carry out their daily jobs. We used unified theory of acceptance and use of technology (UTAUT) as a theoretical basis to test the predictors i.e. performance expectancy, effort expectancy, facilitating conditions, and social influence in order to find the behavioural intention of the healthcare organizations’ staff. Age, experience, and gender were also studied as moderators to investigate their effect on the behavioural intention of the user. An online questionnaire-based survey was conducted with 147 healthcare professionals in Malaysia, Pakistan, and Saudi Arabia. The results showed that social influence was the least influencing predictor in determining the dependent variable and the years of experience positively influenced user’s behavioural intentions towards using cloud-based healthcare services.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Cloud computing has emerged as a novel way of delivering information services to individual users and organizations over the years, in diverse domains i.e. information security, software development, healthcare etc. [1–3]. Cloud computing provides the user with on demand applications known as software as a service (Saas), hardware known as Infrastructure as a Service (IaaS), and Platform as a Service (PaaS) through the Internet and dedicated data centres [4]. In healthcare research and development, cloud computing has been adopted as a progressive domain in recent past due to its on-time resource availability feature and high return on investment [1, 2, 5]. Healthcare industry is making use of technological advancement in almost all the domains to bring state-of-the-art solutions in health and medicine; cloud computing brings a new dimension to this.
In past half a decade, a surge has been noticed in the number of studies focused on the incorporation of cloud computing in healthcare services (e.g. [6–9]). This merger of cloud computing with healthcare services can be seen as a next step to mobile health (m-health) technology. For instance, literature evidences that the proposed cloud computing solutions enhance the mobile health services by effectively collecting and analysing patient’s data while being at distributed locations [8], utilizing cloud services for large data collection and processing [9], and using cloud computing to provide emergency healthcare services [7].
The successful implementation and usage of technological advancement in healthcare industry majorly depends on its acceptance by the physicians, healthcare staff, and even patients in some cases. Also, it depends on the willingness of the healthcare-based IT organizations to make use of cloud computing in e-health services. Literature analysis shows resistance from healthcare staff in adopting e-health services. For instance, the healthcare staff resisted the usage of electronic healthcare record (EHCR) due to several reasons including lack of familiarity with this technology, lack of time to learn new technology, patient data privacy issues, high investment, and interoperability issues [10–12]. Another hindrance factor is that electronic advancements in healthcare industry using the internet are characterized risky in terms of putting your privacy at stake due to global accessibility of information [13]. However, cloud service providers ensure data security, authenticity, availability, and updating [14].
The critical factors that influence the decision of adopting cloud-based healthcare services are studied in the literature such as human factors (perceived technical competence and innovation), technological factors (data security, compatibility, scalability, time, and cost), environmental factors (government policy, perceived industrial pressure), and organizational factors (internal and external collaboration, adequate resource, benefits) [15, 16]. Furthermore, several recent studies focused on data security and privacy issues involved in cloud-based healthcare services (e.g. [17–19]). Thus, the need of security, privacy, and data confidentiality to mitigate the risk factor involved herein puts trust and acceptance of the technology by the individual ahead for its successful application in a certain domain [17, 18]. This motivated us to conduct a comprehensive study on how cloud computing-based healthcare services are taken up in the field. Although technology has stepped into an era of advancement, yet healthcare industry stakeholders (including physicians and paramedical staff) still have resistance towards its acceptance and usage. Considering the fact that the usage of modern healthcare technology in under developed or developed countries is nascent, hence, moving to cloud-based services needs large investment, infrastructure, and wide acceptance. However, in the long run, this advanced healthcare technology can help to improve communication among institutions, to detect and monitor patients at remote locations, and to assist in managing medication in developing countries [20].
In this study, we aim to investigate acceptance of cloud computing as an emerging technology in healthcare industry from the perspective of healthcare professionals (physicians and paramedical staff). For the successful surge of any emergent technology, its infiltration into the functional units of the application domain is of prime importance. Therefore, we aim to study the behavioural intention of the healthcare staff to use cloud-based services through a unified theory of acceptance and use of technology (UTAUT). We explore on how the performance expectancy, effort expectancy, social influence, and facilitating conditions help the stakeholders to adopt cloud-based services in healthcare industry.
The rest of the paper is structured as follows: Section 2 explains the background of the study. Section 3 describes the proposed research model for this study. Section 4 presents the research method adopted for this study. Section 5 states the results and discussion. Section 6 concludes the paper.
2 Background
In past few decades, a burgeoning trend has been witnessed in the usage of electronic services in health sector. The applications are not only limited to electronic medical record (EMR), EHCR, clinical decision support (CDS), and machine-to-machine (M2M) communication systems for e-healthcare society ([21–23]). Technology has taken a step forward and provided healthcare industry with mobile services such as mobile-EMR on tablets [24], mobile electronic medical record administration [25], mobile physical order entry [26], wireless health outcome monitoring system (WHOMS) [27], and among many. The recent research shows that users gave positive feedback regarding the future of personal health devices [28]. Literature shows that mobile healthcare services are moving healthcare industry towards the ubiquitous availability of services to patients [29]. Literature shows that mobile healthcare services are used by healthcare staff (i.e. community health workers) for various purposes including field-based data collection, conducting person-to-person communication, issuing alerts and reminders, providing job aids and decision support, accessing health education material, and supervising other healthcare workers [30, 31]. The main focus of research articles published in last one decade was to introduce new methods, models, techniques, and applications of mobile and cloud health services. However, little attention was paid on studying the acceptance level and perception of this emerging technological advancement in healthcare industry. Only a handful of studies discussed the intentions of healthcare workers and physicians to use web-based and mobile health services (e.g. [21, 32, 33]).
For instance, a study was conducted to find the intention of nurses towards using web-based healthcare services [32]; acceptance level of physicians was tested towards the usage of EHCR [21]; acceptance of cloud computing framework was studied among the healthcare professionals in Ghana [33]. Examples from the literature showed that the perception and acceptance of healthcare staff and physicians were focused in several studies. Conversely, a successful implementation of mobile cloud healthcare technology deems acceptance from all the stakeholders. This establishes the fact that patients and healthcare providing organizations should not be left behind. Examples can be seen in the literature in terms of studying the acceptance level and perception of patients towards using e-health services such as EMR [34–36] and health information system (HIS) [37].
Literature evidences the fact that mobile health services related studies are still in their premature phase as compared to health information system studies [38]. Since, cloud health services are the future of mobile healthcare services industry. Albeit a handful of studies explore its acceptance among healthcare staff and patients. Hence, there is a need to conduct more empirical and longitudinal studies to strengthen the findings and to generalize the results. Therefore, in this paper, it is aimed to close this research gap by empirically exploring the acceptance and perception of healthcare workers (hospital staff, nurses, doctors, and technicians) towards the cloud-based health services.
3 Research model
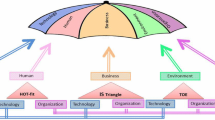
Technology acceptance model (TAM) is widely used to assess human (users) behaviour towards acceptance of a new technology with the help of several factors that influence user’s decision [39]. These factors are perceived ease of use and perceived usefulness. The variants of TAM are TAM2 and TAM3 that are used to find the factors determining perceived usefulness and factors that affect the acceptance of technology, respectively [40, 41]. Over the course of time, TAM has proved to be an adequate predictor especially in healthcare studies [42]. However, Venkatesh et al. believed that TAM has several limitations in terms of having a unified perspective when explaining acceptance of a certain technology [43]. The UTAUT integrates the previously developed TAM(s) [43] and explains the user intentions [44]. UTAUT has four constructs or independent variable (IV) as shown in Fig. 1, that is driven from the previous models explained as performance expectancy defined as how technology helps with their job performance, effort expectancy as user’s perception of the effort required to use the technology, social influence defined as the degree of an individual’s perception of how others believe the individual should use the new technology, and facilitating conditions defined as user’s perception of technology support provided by the IT infrastructure and the organization, as the predictors of behavioural intentions and usage behaviour [43].
UTAUT research model [43]
The proposed research model is designed to investigate the acceptance of cloud computing-based healthcare services among healthcare staff and patients. In particular, we aim to identify the factors that are conducive in influencing the usage of cloud computing services in healthcare industry. Our research model is inspired on UTAUT designed by Venkatesh et al. in [43]. The UTAUT comprises of dependent variables, independent variables, and moderators (as shown in Fig. 2). The research model has four main constructs explaining its independent variables including performance expectancy (PE), effort expectancy (EE), social influence (SI), and facilitating conditions (FC). PE is defined as the degree to which the respondent finds the proposed system helpful in attaining better performance [43]. EE is defined as the amount of effort the respondent deems to be required in using the system [43]. SI is defined as the degree to which others believe that the respondent should use the system [43]. FC is defined as the degree to which logistic support is available from organization and individuals to support the usage of the system [43]. The behavioural intention to use (BI) is the dependent variable. It defines the respondent’s intention to use the system depending on the independent factors. The moderators selected for the proposed research model are inspired by Venkatest et al. in [43] including age, gender, and years of experience.
This work is aimed to find out the behavioural intention of the healthcare industry stakeholders in adopting and using cloud-based healthcare services in future. For this, the independent factors chosen are PE, EE, SI, and FC. In addition, the effect of moderators is also of interest such as how age, gender, and experience influence the respondent’s decision to use cloud-based healthcare services in future. Therefore, we proposed four hypotheses using the UTAUT model to find if statistically significant relationship exists between the variables. The proposed hypotheses are stated as follows:
-
H1A: Performance expectancy has a statistically significant relationship with behavioural intention to use cloud computing.
-
H1B: The effect of performance expectancy on behaviour intention to use cloud computing-based file storage should be moderated by gender, age, and experience.
-
H2A: Effort expectancy has a statistically significant relationship with behavioural intention to use cloud computing.
-
H2B: The effect of effort expectancy on behaviour intention to use cloud computing-based file storage should be moderated by gender, age, and experience.
-
H3A: Social influence has a statistically significant relationship with behavioural intention to use cloud computing.
-
H3B: The effect of social influence on behaviour intention to use cloud computing-based file storage should be moderated by gender, age, and experience.
-
H4A: Facilitating conditions have a statistically significant relationship with behavioural intention to use cloud computing.
-
H4B: The effect of facilitating conditions on behaviour intention to use cloud computing-based file storage should be moderated by gender, age, and experience.
4 Research methodology
The research design followed in this study is quantitative. We have followed a non-experimental methodology and have used inferential statistical model to answer research questions and to test hypotheses. The selected research approach is found suitable for such cases in which opinions are collected from selected population and are analysed to infer results [45, 46]. There are examples that have successfully employed quantitative approach to examine subjective data regarding technology acceptance by healthcare industry (e.g. [47–51]).
Data were gathered through a single data collection method i.e. questionnaire-based survey because survey is considered as the most appropriate method to gather subjective data [45, 46]. Electronic deployment of survey enabled efficient data collection from large population as found in several examples [52–54]. However, in several cases, questionnaires were printed and distributed for data collection. On the other hand, the usage of single data collection method is also considered as a limitation of our work because it may cause lapse of information. Use of data triangulation may solve this problem where data is gathered through multiple methods to cover any missing information.
The questionnaire was deployed using a third party online platform due to time and budget constraints. Although, the usage of online survey deployment platforms makes it hard to select a justified population sample for instance having more male members than female respondents. The questionnaires were sent to hospitals and healthcare staff of three countries i.e. Malaysia, Pakistan, and Saudi Arabia due to researchers’ location and budget constraints. However, for wide application and generalization of the results, sample needs to be collected from diverse sources. The sample size was kept small to keep the confidence level and estimated error limited. If the estimated error is narrowed down, larger sample would be required. This compromise might have some effect on the quality of our results.
4.1 Population
The population of interest for this research was hospital healthcare staff including doctors, nurses, and technical staff. The sample size of the study is calculated using the sample size calculation formula shown in Eq. 1.
where
- n :
-
number to sample,
- Z 2 :
-
confidence value
- P :
-
“best guess” for number of responses received (e.g. ±0.50),
- E :
-
maximum tolerable error or degree of precision for the prevalence estimate (e.g. ±0.05)
The acceptable confidence value Z 2 is 95% which is 1.96 [55]. With the estimated value of response return rate as 50% (0.50) and value of maximum tolerable error as 4% (0.04), the minimum sample size was calculated as 114 and we collected 120 responses in total.
4.2 Research instrument
Questionnaire was used for data collection. The self-administered questionnaire was constructed using Google Docs service (attached as Appendix A). However, the questionnaire was printed and distributed in several cases as well. The questionnaire comprised of three sections. Section 1 describes the demographics of the respondents and collects data related to moderators. The respondents were asked about their age, gender, role, location, and years of experience. In section 2, we collected information regarding organization’s size and usage of computerized or online services. Section 3 consisted of questions designed to gather the respondents’ opinion on independent variables. A five-point likert scale is used that ranges from strongly agree (5) to strongly disagree (1). The independent variables and their respective questionnaire items (questions) are listed below in Table 1.
4.3 Data analysis
First, the responses collected from online self-administered questionnaire were recorded in an excel spreadsheet screenshots are shown in Fig. 3.
Second, the data reliability was tested for all the variables using Cronbach’s alpha [56, 57], composite reliability test [58], and average variance extracted (AVE). To check the reliability of the data, mean, average, and standard deviation of the responses collected against all of the variables were calculated. SPSS version 20 was used to calculate the values of Cronbach alpha, composite reliability test, and AVE. We also made sure if removal of any item could improve internal consistency. Third, the moderators were tested using Spearman’s correlation coefficient (ϱ pronounced Rho) to find out how the moderators influence the behavioural intention of the respondents to use cloud-based healthcare services. Fourth, regression analysis [59] was performed to test the model and to determine the effect of independent variables (PE, EE, FC, and SI) on the dependent variable (BI).
5 Results and discussion
In this section, we present the summary of the demographic characteristics of the respondents, the results of the statistical tests performed on data for reliability analysis, hypotheses testing, and moderators’ testing. It also includes discussion on the results to prove the significance of our proposed hypothesis.
5.1 Demographic characteristics of the sample
Data were collected from the hospitals located in several cities of Malaysia, Pakistan and in Riyadh, Saudi Arabia based on the physical reachability of the authors and budget of this research project. The demographics and frequency distribution of the respondents are shown in Table 2.
It can be seen that the respondents fall in the range of all age groups mentioned in the questionnaire from 20 to 60 years. However, we did not manage to find any participant above 61 years of age. The reason behind is the normal retirement age limit for healthcare staff is 60 years in Malaysia, Pakistan, and Saudi Arabia. The questionnaires were distributed in both public and private sector hospitals, research centres, and nursing homes. The percentage of male participants was larger than female participants. However, the data sample collected from Malaysian hospitals had more female participants as compared to the sample collected from Pakistan and Saudi Arabia, which reflects the general employment trend of the healthcare organizations of these countries.
Large percentage of the respondents had considerable experience i.e. 2 to 5 years (38%) and 6 to 9 (25%) years and above 9 years (11%) of experience. This shows that around 72% of the respondents fall in the category of mid-level and high level experienced professionals. The large percentage of experienced population also establishes the reliability of our data. The demographic data showed that 45% of our respondents were physicians and 20% were nurses (male and female both), and 15% were technicians including X-ray technicians, dialysis technicians, sonographers, and MRI technicians. Special attention was given to the equivalent distribution of questionnaires to gather a wide perspective of responses.
During data collection, we found that postgraduate interns also serve as medical officers in the medical institutes and research centres, along with their postgraduate studies. Therefore, the sample also had 5% postgrad interns. The sample showed that major part of the population (70%) was working in small to middle-sized hospitals (21–100 beds). The participants were also inquired about their acquaintance with the cloud-based healthcare services. This question was posed to get an idea of the respondents’ acquaintance with cloud computing services and if it affects their decision. But the result percentage showed that only a small segment of population (36%) had prior experience with cloud computing services. In depth analysis of the data showed that these 36% of the respondents with prior experience of using cloud computing-based healthcare services worked in large-sized hospitals (above 200 beds). This shows that some of the large medical institutes, medical complexes, research facilities, and hospitals have started using cloud computing services in their daily operation. However, it is noticeable that the fragment of population that is using these cloud-based services was only physicians. This brings our attention to twofold issues: first, it shows that there is a need to implement cloud computing healthcare services in the hospitals, Second the healthcare staff should be trained and motivated to use cloud-based healthcare services in their daily practice.
5.2 Data reliability
To test the data reliability average, mean, and standard deviation, values of the responses against each variable are calculated, shown in Table 3. Cronbach’s alpha, composite reliability, and AVE values are shown in Table 4.
It can be seen that the Cronbach alpha values of the variables fall in the acceptance range (above 0.80%), approximately [60]. The Cronbach’s alpha value for social influence is 0.79 which is also considered acceptable (e.g. in [61]). To confirm the results obtained from Cronbach alpha, composite reliability and average variance extracted were calculated. The AVE results showed substantial amount of variance in the values, with AVE values greater than 0.50 [61]. Overall, it can be seen that composite reliability and average variance extracted values calculated for the variables also support the Cronbach alpha’s results and uphold the reliability of the variable values (as shown in Table 4).
5.3 Finding acceptance of cloud-based healthcare services
To explore the relationship between the dependent variable (BI) and independent variables (PE, EE, SI, FC), Spearman correlation is performed. This inter-variable correlation is performed using Spearman correlation to determine the effect of variables on each other. For instance, the correlation results helped us to understand the fact that how performance expectancy of the respondent influenced his/her effort expectancy. This inter-variable correlation helped in determining the complete picture of our research model. The Spearman correlation coefficient calculated for each variable is shown in Table 5.
The inter-correlation coefficient value is 1 for all of the variables that shows maximum correlation. The correlation value is always 1 when two variables are similar or when the variable is checked against itself; therefore, we will ignore them. The correlation results showed that most of the correlation values fall in the moderate correlation range r from 0.39–0.49 according to fields [62]. However, several inter-correlations show low correlation, less than minimum value e.g. PE-SI (0.161). The results also showed that there was no correlation value exceeding 0.90 which means that no perfect inter-correlation relationship existed in this sample. Overall, the correlation values showed promising results in terms of inter-relationship among the variables.
The cross correlation results between dependent and independent variables showed highest correlation value for BI-PE (0.711), BI-EE (0.543), and BI-FC (0.367). The correlation coefficient value was lowest for BI-SI (0.235) which shows weak correlation among social influence and behavioural intention to use cloud services. The correlation results showed that performance expectancy, effort expectancy, and the facilitating conditions help to find the behavioural intention of the respondents to use cloud-based services in performing their daily duty.
Regression analysis is performed to find out the significance of the independent variables in predicting the dependent variable, hence to prove our hypotheses. The regression analysis results (showed in Table 6) revealed that the significance values for all the independent variables are within range (*ρ < .05. **ρ < .01). Hence, it proves that there is a significant relationship between the dependent variable and independent variables, and this rejects the null hypotheses. Furthermore, the results revealed that PE (β = 0.345, ρ < 0.01), EE (β = 0.143, ρ < 0.05), FC (β = 0.282, ρ < 0.05), and SI (β = 0.252, ρ < 0.05) have a significant positive effect on B1 that approves the proposed hypotheses; H1A performance expectancy has a statistically significant relationship with behavioural intention to use cloud computing; H2A effort expectancy has a statistically significant relationship with behavioural intention to use cloud computing; H3A social influence has a statistically significant relationship with behavioural intention to use cloud computing; H4A facilitating conditions have a statistically significant relationship with behavioural intention to use cloud computing. The regression analysis also shows that the independent variables account 62.3% variance in predicting behavioural intention of the respondents to use cloud-based healthcare services.
5.4 Checking moderators’ effect on behavioural intention
To investigate the effect of moderators (age, experience, and gender) on dependent and independent variables, Spearman’s correlation was performed. The Spearman’s correlation coefficient (rho) calculated for each moderator is shown in Table 7. The correlation coefficient clearly showed that age and gender had no influence on PE, EE, SI, FC, and BI. The correlation coefficient (rho) values calculated for age and gender against all variables were close to 0 that showed less or no correlation. Therefore, it can be determined that age and gender were not the stimulating factors that influence respondent’s behaviour to use cloud-based healthcare services. However, years of experience showed positive correlation with PE (0.661), EE (0.591), FC (0.498), and BI (0.641) that signifies relationship between them. Here, we took 0.50 as the minimum correlation value [62]. Hence, it can be concluded that years of experience can possibly influence the respondents’ behavioural intention to use cloud-based healthcare services in future. Summary of hypotheses acceptance and rejection is shown in Table 8.
6 Conclusion
The study was aimed to find out the behavioural intention of physicians and paramedical staff to use secure cloud-based healthcare services in performing their daily jobs. Hypotheses were proposed, and research model was designed to guide this study. We used UTAUT model to find out on how the independent variables i.e. performance expectancy, effort expectancy, facilitating conditions, and social influence affect the behavioural intention of the users to use cloud services. Moderators like age, experience, and gender were also studied in terms of their effect on user’s decision towards using cloud-based healthcare services. An online questionnaire-based survey was conducted with 147 members of different healthcare organizations located in several cities of Malaysia, Pakistan, and Saudi Arabia. Mean, average, and standard deviation of the responses collected against the variables were calculated to check the data reliability by using Cronbach’s alpha, composite reliability test, and average variance extracted. Statistical analysis was performed (i) to find out if the model was fit to determine the dependent variable using the predictors by using regression analysis and (ii) to determine the correlation among variables using Spearman’s correlation. The results showed promising confidence in the model. The findings revealed that the social influence was found to be the least influencing predictor among the rest. The results also showed that years of experience influenced the respondents in determining their behavioural intention to use cloud-based healthcare services in performing their daily duties. This means that with increasing experience, individuals observe improved trust on the cloud services in providing privacy of their data and security of overall system. It can be inferred that there is a direct relationship between the experience of respondents and their trust level on the security of mobile cloud-based healthcare systems.
The study can be replicated using a large and diverse sample to produce more generalized results. We also propose to include patients along with healthcare organization’s staff in the survey to provide a wider perspective of the acceptance of this new technology in the health care sector. We also propose to include variables like IT knowledge of the healthcare organization’s respondents, their previous experience with online services, and their knowledge of healthcare rules and regulations in determining the future of this technology.
References
Griebel L, Prokosch H, Köpcke F, Toddenroth D, Christoph J, Leb I, Engel I, Sedlmayr M (2015) A scoping review of cloud computing in healthcare. BMC Med Inform Decis Mak 15(17):1–16
Mellado D, Fernández-medina E (2012) A systematic review of information security governance frameworks in the cloud computing environment. J Univers Comput Sci 18(6):798–815
Inayat I, Salim SS, Kasirun ZM (2013) Agile-based software product development using cloud computing services: findings from a case study. Sci Int 25(4):1065–1069
Armbrust M, Fox A, Griffith R, Joseph AD, Katz R, Konwinski A, Lee G, Patterson D, Rabkin A, Stoica I (2010) A view of cloud computing. Commun ACM 53:4
Majhi SK, Bera P (2014) OHMF: a query based optimal healthcare medication framework. Int J Inf Process 8(3):1–12
Youssef AE (2014) A framework for secure healthcare systems based on big data analytics in mobile cloud computing environments. Int J Ambient Syst Appl 2(2):1–11
V. Koufi, F. Malamateniou, G. Vassilacopoulos, and A. Prentza, “An android-enabled mobile framework for ubiquitous access to cloud emergency medical services,” in Second Symposium on Network Cloud Computing and Applications, 2012, pp. 95–101.
Rolim CO, Koch FL, Westphall CB, Werner J, Fracalossi A, Salvador GS (2010) A cloud computing solution for patient’s data collection in health care institutions. In: 2nd International Conference on eHealth, Telemedicine and Social Medicine, pp 95–99
Nkosi MT and Mekuria SM (2010) Cloud computing for enhanced mobile health applications. In: 2nd IEEE International Conference on Cloud Computing Technology and Science, pp 629–633
Yarbrough AK, Smith TB (2007) Technology acceptance among physicians. Med Care Res Rev 64(6):650–672
Curry SJ (2007) eHealth research and healthcare delivery. Am J Prev Med 32:127–130
Atienza AA, Hesse BW, Baker TB, Abrams DB, Rimer BK, Croyle RT, Volckmann LN (2007) Critical issues in eHealth research. Am J Prev Med 32:71–74
Featherman MS, Pavlou PA (2003) Predicting e-services adoption: a perceived risk facets perspective. Int J Hum Comput Stud 59:451–474
Ramgovind S, Eloff MM, Smith E (2010) The management of security in cloud computing. In: Information Security for South Africa, pp 1–7
Lian J, Yen DC, Wang Y (2014) An exploratory study to understand the critical factors affecting the decision to adopt cloud computing in Taiwan hospital. Int J Inf Manag 34(1):28–36
Lero ML, Kieran C (2013) Factors affecting the adoption of cloud computing: an exploratory study. In: 21st European Conference on Information Systems foundation, pp 1–12
Latif R, Abbas H, Latif S, Masood A (2016) Distributed denial of service attack source detection using efficient traceback technique (ETT) in cloud-assisted healthcare environment. J Med Syst 40(7):161–173
Sajid A, Abbas H (2016) Data privacy in cloud-assisted healthcare systems: state of the art and future challenges. J Med Syst 40(6):155
Latif R, Abbas H, Assar S Distributed denial of service (DDoS) attack in cloud-assisted wireless body area networks: a systematic literature review. J Med Syst 38:128–2014
Blaya BJA, Fraser HSF, Holt B (2010) E-health technologies show promise in developing countries. Health Aff 29(2):244–251
Manuel J, Egea O, Victoria M, González R (2011) Explaining physicians’ acceptance of EHCR systems: an extension of TAM with trust and risk factors. Comput Human Behav 27:319–332
Demirkan H, Tacoma W (2013) A smart healthcare systems framework. IT Professional 5:38–45
Saleem K, Derhab A, Al-Muhtadi J, Shahzad B (2015) Human-oriented design of secure machine-to-machine communication system for e-Healthcare society. Comput. Human Behav. 51(NOVEMBER):977–985
Fleischmann R, Duhm J, Hupperts H, Brandt SA (2015) Tablet computers with mobile electronic medical records enhance clinical routine and promote bedside time: a controlled prospective crossover study. J Neurol 262:532–540
Hsieh S, Hou I, Cheng P, Tan C, Shen P, Hsu K, Hsieh S, Lai F (2010) Design and implementation of web-based mobile electronic medication administration record. J Med Syst 39:947–958
Ying A (2003) Mobile physician order entry. J Heal Informatics Manag 17:58–63
Bielli E, Carminati F, La Capra S, Lina M, Brunelli C, Tamburini M (2004) A wireless health outcomes monitoring system (WHOMS): development and field testing with cancer patients using mobile phones. BMC Med. Inform. Decis. Mak. 4(7):1–13
Sun N, Rau PP (2015) The acceptance of personal health devices among patients with chronic conditions. Int J Med Inform 84(4):288–297
Vilaplana J, Solsona F, Abella F, Filgueira R, Rius J (2013) The cloud paradigm applied to e-Health. BMC Med. Inform. Decis. Mak. 13(35):1–10
Derenzi B, Borriello G, Jackson J, Kumar VS, Parikh TS, Virk P, Lesh N (2011) Mobile phone tools for field-based health care workers in low-income countries. Mt Sinai J Med 78:406–418
Braun R, Catalani C, Wimbush J, Israelski D (2013) Community health workers and mobile technology: a systematic review of the literature. PLoS One 8(6):4–9
Chen I-J, Yang K-F, Tang F-I, Yu S (2008) Applying the technology acceptance model to explore public health nurses’ intentions towards web-based learning: a cross-sectional questionnaire survey. Int J Nurs Stud 45(6):869–878
Sedem AA, Panford JK (2015) Cloud computing framework for e-Health in Ghana: adoption issues and strategies: case study of Ghana health service. 118(17):13–17
Inkelman WAJW, Eonard KEJL, Ossos PEGR (2005) Patient-perceived usefulness of online electronic medical records: employing grounded theory in the development of information and communication technologies for use by patients living with chronic illness. J Am Med Informatics Assoc 12(3):306–314
Ierdon STP, Eitz DED, Uck SAK, Rtiz EDO (2004) Patient experiences and attitudes about access to a patient electronic health care record and linked web messaging. J. Am. Med. Informatics Assoc. 11(6):505–513
Wilson EV, Lankton NK (2004) Modeling patients’ acceptance of provider-delivered e-health. J. Am. Med. Informatics Assoc. 11(4):241–248
Ahlan AR, Isma’eel BA (2014) User acceptance of health information technology (HIT) in developing countries: a conceptual model. Procedia Technol 16:1287–1296
Sezgin E, Özkan S (2014) A literature review on attitudes of health professionals towards health information systems: from e-Health to m-Health. Procedia Technol. 16:1317–1326
Davis FD (1989) Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q 13(3):319–340
Venkatesh V, Davis FD (2000) A theoretical extension of the technology acceptance model: four longitudinal field studies. Manag Sci 46(2):186–2014
Venkatesh V, Bala H (2008) Technology acceptance model 3 and a research agenda on interventions. Decis Sci 39(2):273–315
Chau PYK, Hu PJ (2002) Investigating healthcare professionals’ decisions to accept telemedicine technology: an empirical test of competing theories. Inf Manag 39:297–311
Venkatesh V, Morris MG, Davis GB, Davis FD (2003) User acceptance of information technology: toward a unified view. MIS Q 27(3):425–478
Im I, Hong S, Soo M (2011) Information & Management an international comparison of technology adoption testing the UTAUT model §. Inf Manag 48:1–8
Creswell JW (2009) Research design: Qualitative, quantitative, and mixed methods approaches, 3rd ed. Sage Publications Inc, Thousand Oaks, California
Vogt WP (2009) Quantitative research methods for professionals. Pearson Education, Boston, MA, US
Chow M, Herold DK, Cho T-M, Chan K (2012) Extending the technology acceptance model to explore the intention to use second life for enhancing healthcare education. Comput Educ 59(4):1136–1144
Egea JMO, González MVR (2011) Explaining physicians’ acceptance of EHCR systems: an extension of TAM with trust and risk factors. Comput. Human Behav. 27:319–332
Moores TT (2012) Towards an integrated model of IT acceptance in healthcare. Decis Support Syst 53:507–516
Pai F-Y, Huang K-I (2011) Applying the technology acceptance model to the introduction of healthcare information systems. Technol Forecast Soc Chang 78:650–660
Wu I-L, Li J-Y, Fu C-F (2011) The adoption of mobile healthcare by hospital’s professionals: an investigative perspective. Decis Support Syst 51:587–596
Zhang H, Cocosila M, Archer N (2010) Factors of adoption of mobile information technology by homecare nurses. Comput Informatics, Nurs 28(1):49–56
Kowitlawakul Y (2011) The technology acceptance model: predicting nurses’ intention to use telemedicine technology (eICU). 29(7), 411-418. Comput. Informatics, Nurs. 29(7):411–418
Carayon P, Cartmill R, Blosky MA, Brown R, Hackenberg M, Hoonakker P, Walker JM (2013) ICU nurses’ acceptance of electronic health records. J. Am. Med. Informatics Assoc. 18:812–819
Groves RM, Fowler FJ, Couper MP, Lepkowski JM, Singer E, and Tourangeau R (2009) Survey Methodology, 2nd ed. Wiley, p 488
Cronbach L (1949) Essentials of psychological testing. Harper & Row, New York, p 726
Cronbach L (1951) Coefficient alpha and the internal structure of tests. Psychometrika 16:297–334
Raykov T (1997) Estimation of composite reliability for congeneric measures. Appl Psychol Meas 21(2):173–184
Sykes AO (2007) An introduction to regression analysis. Am Stat 61:1–33
Straub DW (1989) Validating instruments in MIS research. MIS Q 13(2):147–169
Hair JF, Tatham RE, Anderson RL, Black W (1998) Multivariate data analysis Englewood Cliffs: Prentice Hall, 5th edn. Prentice Hall, Englewood Cliffs
Field A (2009) Discovering statistics using SPSS, 3rd edn. SAGE Publications Inc., Thousand Oaks, California
Acknowledgements
This Project was funded by the National plan of Science, Technology and Innovation (MAARIFAH), King Abdulaziz City for Science and Technology, Kingdom of Saudi Arabia, Award Number (12-INF2817-02).
Author information
Authors and Affiliations
Corresponding author
Appendix A
Appendix A
Questionnaire.

Rights and permissions
About this article
Cite this article
Amin, R.u., Inayat, I., Shahzad, B. et al. An empirical study on acceptance of secure healthcare service in Malaysia, Pakistan, and Saudi Arabia: a mobile cloud computing perspective. Ann. Telecommun. 72, 253–264 (2017). https://doi.org/10.1007/s12243-016-0553-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12243-016-0553-4