Abstract
Vascular fibrosis, the formation of excess fibrous tissue on the blood vessel wall, is characterized by unmitigated proliferation of fibroblasts or myofibroblast-like cells exhibiting α-smooth-muscle-actin in vessel lumen and other vascular layers. It likely contributes to vascular unresponsiveness to conventional therapies. This paper demonstrates a new flow-induced vascular fibrosis mechanism. Using our developed flow system which simulates the effect of vessel stiffening and generates unidirectional high pulsatility flow (HPF) with the mean shear flow at a physiological level, we have shown that HPF caused vascular endothelial dysfunction. Herein, we further explored the role of HPF in vascular fibrosis through endothelial-to-mesenchymal transdifferentiation (EndMT). Pulmonary arterial endothelial cells (ECs) were exposed to steady flow and HPF, which have the same physiological mean fluid shear but different in flow pulsatility. Cells were analyzed after being conditioned with flows for 24 or 48 h. HPF was found to induce EndMT of cells after 48 h stimulation; cells demonstrated drastically decreased expression in EC marker CD31, as well as increased transforming growth factor β, α-SMA, and collagen type-I, in both gene and protein expression profiles. Using the flow media from HPF-conditioned endothelial culture to cultivate arterial adventitial fibroblasts (AdvFBs) and ECs respectively, we found that the conditioned media respectively enhanced migration, proliferation and α-SMA expression of AdvFBs, and induced EndMT of ECs. It was further revealed that cells exposed to HPF exhibited much higher percentage of caspase-positive cells compared to those exposed to steady flow. Apoptotic cells together with remaining, caspase-negative cells suggested the presence of apoptosis-resistant dysfunctional ECs which likely underwent EndMT process and perpetuated fibrosis throughout vascular tissues. Therefore, our results indicate that prolonged HPF stimuli induce vascular fibrosis through triggering EndMT and EC-mediated AdvFB activation and migration, which follows initial endothelial inflammation, dysfunction and apoptosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tissue fibrosis is the formation of excess fibrous connective tissue, due to increased activities of fibroblast-like cells in a reparative or reactive process. It is often preceded by tissue inflammation and resulting in increased content of collagen type I to improve structural integrity of injured or weak tissues. As a consequence of fibrosis, collagen-rich scar tissues accumulated with fibroblast- or myofibroblast- like cells replace normal functional tissues. Therefore, fibrosis is common in a number of diseases showing gradual tissue deterioration, as in the case of vascular tissue fibrosis, which is an important aspect of extracellular matrix remodeling in hypertension and other cardiovascular diseases. The exact cell type contributing to vascular fibrosis during blood vessel remodeling after injury is unclear. Evidence shows fibrosis may occur in all vascular tissue layers, namely intima, media and adventitial layers, as occurring in atherosclerosis, pulmonary artery hypertension, vascular grafting anastomose or stenting. Vascular fibrosis likely involves all resident vascular cell types, endothelial cell (EC), smooth muscle cell (SMC) and adventitial fibroblast (AdvFB).3,5,11,22,29,33,35 Understanding of vascular fibrosis pathologies are further complicated by all cells within vessel walls presenting α-smooth muscle actin (α-SMA),11,43 most commonly associated with SMC previously. Studies also suggested that these α-SMA+ cells might be associated with the presence of transforming growth factor β (TGF-β).40,42 Though the majority of previous studies have focused on illustrating the role of SMCs in vascular neointimal hyperplasia and fibrosis, evidence from recent studies supports the potential trans-differentiation of other vascular cells (ECs and AdvFBs) into the myofibroblast phenotype during pathological vascular remodeling,37 but the underlying mechanism, particularly in relation to hemodynamics present in vascular diseases, has been seldom explored.
Increasing attention is now given to endothelial-to-mesenchymal transition (EndMT) and to its occurrence and roles in artery maturation during embryonic development as well as in intimal fibrosis during vascular remodeling.2,8,10,28 EndMT is believed to contribute, at least partially, to pulmonary, renal, and cardiac fibrosis in adult mammals.15,44–46 Activation of EndMT can result from biomechanical and/or biochemical signaling. It was shown increasing the mean magnitude of shear stresses from 0.5 to 5.0 Pa promoted murine and chicken embryonic ECs to the EndMT process, showing reduced endothelial marker and increased α-SMA expression.8,9 While flow-induced EndMT was thought to be a necessary step during vascular development, it may be harmful to healthy blood vessels. Recent findings have highlighted the contribution of EndMT to vascular pathogenesis in a number of fibrotic diseases.15,24,44,46 The EndMT process is particularly correlated to the presence of TGF-β.3,15,17,19,25,44,45 In addition to EndMT, activation of AdvFB migration, proliferation or matrix production may also contribute to vascular fibrosis, hardening and reduced response to vasodilation therapy. Activation of AdvFB can be triggered by flow and/or cytokine stimuli. High interstitial flow was shown to activate AdvFB migration.1,4,13 TGF-β was also found to be involved in activating AdvFB proliferation and matrix production.18 Though the respective contributions of EC and AdvFB to vascular fibrosis the fibrotic process. Understanding the cellular mechanisms during vascular fibrosis and hardening could greatly assist the during remodeling are increasingly recognized, few studies have examined their collaborative efforts in drivingdevelopment of new therapeutic approaches towards cardiovascular disease and hypertension.
Our previous studies have established unidirectional high pulsatility flow (HPF), a proximal stiffening-induced flow condition indicated in disease and aging,26,31 as a determinant to distal pulmonary artery endothelial health.21 We have shown that HPF altered pulmonary artery SMC physiology via vasoactive substances and cytokines produced by the endothelium.38 In response to HPF with physiologic, mean shear stresses (1.2 Pa), distal ECs also demonstrated acute inflammatory response, simulating that occurring in pulmonary hypertension. Growing evidence supports that vascular intimal thickening of distal pulmonary arteries in diseased condition, due to inflammation or fibrosis, might contribute to the unresponsiveness of arteries to vasodilation therapies.12,32 Palevsky et al. showed that an intimal area of more than 18% of the vascular cross-section had an 85% predictive value for identifying poor outcome from vasodilation treatment.30 It is well known that during wound healing, fibrosis follows inflammatory events. This might occur during flow-induced vascular inflammation and remodeling. To further establish the role of HPF (with the mean flow shear at a physiological level) in fibrosis of vascular intima and other vascular layers, we therefore sought to test the hypothesis that prolonged HPF stimuli induce vascular fibrosis through triggering EndMT and EC-mediated AdvFB activation and migration, following initial endothelial inflammation. To address this hypothesis, we applied our developed flow system, simulating the effects of vessel stiffening, and HPF generation on the downstream cells.
Materials and Methods
Cell Culture
Human pulmonary arterial ECs (HPAEC) were obtained from Lonza Inc, and kept in a CO2 incubator at 37 °C and 5% CO2. Cells were thawed as needed and grown to approximately 70–80% confluency using EGM-2 with additional growth factor and fetal bovine serum bullet kit (Lonza, Basel, Switzerland). Once confluent, cells at passages of 3–8 were seeded on two glass slides for the flow experiment. Human pulmonary artery adventitial fibroblasts were maintained in DMEM media containing 10% FBS and cultured in similar conditions.
Flow Setup and Experiments
To examine the response of HPAECs to various flow conditions, plain microscope glass slides were chemically functionalized with 20% of aqueous sulfuric acid and then coated with 6% of 3-aminopropyltriethoxysilane in acetone. After silanization, the glass slides were treated with 1.5% of glutaraldehyde solution. This formed an aldehyde which could initiate amine linkage to protein coating. The slides were then coated with 25 µg/ml fibronectin aqueous solution for 30–60 min to provide a functional attachment layer for the HPAECs. HPAECs at a concentration of 6.0 × 105 per ml were seeded on the fibronectin-coated slides and given 1 h to attach to the slides, and then the cells were covered in growth media and allowed to reach confluency, before they were transferred to the flow chamber apparatus.
To ensure the sterility and cleanness of the flow experiments, the exterior of a pulsatile blood pump (Harvard Apparatus Inc; Holliston, MA) or a peristaltic pump (Cole Parmer), which was used to circulate the medium, was sterilized by wiping it with 70% ethanol. Sterilization of the flow circuit was completed through perfusing all the tubings, pump chamber and connectors with 10% hydrogen peroxide (H2O2) under ultraviolet light within a biosafety cabinet Type II for a minimum of 30 min. To clean the circuit of any cytotoxicity, sterile Dulbecco’s phosphate buffered solution (DPBS) was circulated through and removed. Perfusion with DPBS was repeated twice before flow experiments started. For generating HPF condition, the blood pump simulated the heart function generating cardiac output, while the compliance-adjustment chamber simulated the flow buffering or cushion function of proximal arteries. The fluid levels of the compliance-adjustment chamber allowed for pulsatility control of dynamic flows, with lower fluid levels allowing greater dampening of dynamic pressures. Downstream to the compliance-adjustment chamber was the cell-plate flow chamber which holds the endothelium representing the distal pulmonary artery endothelium. Each component was connected by stiff polystyrene tubing. The circulating media used in the experiments consisted of a basal media (EBM-2, Lonza, Basel, Switzerland), medical grade dextran (MP-products Inc, Solon, OH) (7% w/w), and penicillin/streptomycin (2% v/v), as its viscosity was close to blood viscosity so that it reduces volumetric flow rate while maintaining a high shear stress. For flow measurements, a digital flow meter (Alicat Scientific Inc, Tucson, AZ) was placed before the flow chamber. A manifold section was used to run parallel studies.
Two flow conditions were applied within a closed fluid circuit: high pulsatility flow (HPF) using the blood pump and steady flow using peristaltic pump. Both pulsatile flows had the same mean flow rate with a mean surface flow shear stress of 1.2 Pa, at the frequency of 1 Hz. The steady flow showed no great variation in flow velocity with the flow pulsatility index (PI) less than 0.2, while the PI value of HPF was determined to be 1.7,26,31 using the following equation:
For all the experiments, cells were preconditioned at low or no pulsatility (PI < 0.5) with low shear stress for between 4 and 6 h before experimental flow conditions began. Experiments consisted of 24 and 48 h of flow conditions. For the pharmacological treatment of cells using taxol (Paclitaxel, Sigma-Aldrich Inc), the experiments were performed with the addition of 10 ng/ml of taxol in the flow culture media. HPAECs grown in the absence of flow (the static condition) were used as a control. After HPAECs were exposed to different flows, they were collected and analyzed for gene expression using real-time PCR and for protein expression using western blotting. The circulating media during flow culture period were collected as flow conditioned media (FCM) for studies that evaluate EC and AdvFB activation, in which confluent HPAECs and AdvFBs were cultured for 24 h in FCM. Western blot analysis was performed on resulting cells, comparing α-SMA protein expression with β-actin. FCM was also used to evaluate its potential to induce AdvFB migration and proliferation.
Western Blot
Western blot analyzes were performed as per the manufacturer’s suggestions (Invitrogen, Carlsbad, CA). Briefly, to retrieve proteins, ECs were gently scraped off glass slides, lysed with RIPA lysis buffer, and then centrifuged at 14,000 rpm for 20 min at 4 °C. Supernatant was then transferred to a clean tube. Protein concentrations were determined using a standard curve of BSA. Twenty micrograms of protein from each sample were separately loaded and subjected to gel electrophoresis. Following electrophoresis, resulting protein was transferred to a nitrocellulose membrane. The membrane was blot with COL1A1 rabbit polyclonal antibody, PECAM-1 mouse monoclonal, TGFβ1 mouse monoclonal, and 1A4 (α-SMA) antibodies (all antibodies from Santa Cruz Biotech, Santa Cruz, CA).
Real-Time PCR
To study the effects of HPF on the pulmonary artery endothelium, HPAECs were conditioned with HPF and steady flow for 24 and 48 h, respectively. Real-time PCR was used to analyze the gene expression of the biomarkers important for EndMT. Cell samples were gently scraped from slides after applying RLT buffer tissue lyser using the RNeasy mini-kit from Qiagen (QIAGEN, Hilden, Germany), according to the manufacturer’s instructions. Samples were then prepared as per manufacturer’s instructions for real time- PCR using RT2 SYBR Green FAST Mastermix and corresponding gene primers, also from QIAGEN. Gene expression in 24 and 48-h flow cycles were examined for PECAM-1 (CD31), α-SMA (ACTA2), TGF-β (TGF-beta1), and Collagen-I (COL1A1) with β-actin expression (ACTB) as the housekeeping gene. Primers (PPH01362E, PPH00508A, PPH01299F and PPH01300B) were directly obtained from Qiagen Inc. Data was analyzed using the ΔΔCT method, and plotted. Statistical significance between groups was found using Welch’s t test using degrees of freedom derived from the Welch-Satterthwaite equation for unequal sample sizes and unequal variances.
Fibroblast Migration and Proliferation Assay
The flow conditioned media (FCM) from HPAECs were taken from those exposed to steady or HPF culture conditions for 24 or 48 h, and were used to determine migration and proliferation of AdvFB. For cell migration study, the FCM was placed in the bottom well covered with a 3-mm transwell insert (BD Biosciences, San Jose, CA), while AdvFBs were placed on top of the insert and cultured for 24 h. Subsequently, the cells on the top of the insert were gently scraped off with a cotton tip, and the cells on the other side of the insert were stained with 2% crystal violet or DAPI, and then imaged under a light microscope. The number of migrated cells was determined using ImageJ (National Institute of Health, Bethesda, MD).
For measurement of fibroblast proliferation, FCM was used to culture adventitial fibroblasts for 24 h. Then, CyQuant proliferation assay kit (Invitrogen, Grand Island, NY) was used according to the manufacturer’s instruction. Proliferation of AFB was measured using a CyQuant proliferation assay kit (Invitrogen, Grand Island, NY). Cells were cultured in FCM for 24 h, and the assay was completed as per manufacturer’s instructions.
Apoptosis Assay
Apoptosis assay was applied to cells after exposure to flow for 24 h. FLICA poly caspase reagent (Immunochemistry Technology LLC, Bloomington, MN) including fluorescent-labeled inhibitor of caspases, is a simple yet accurate method to measure apoptosis via caspase activity in whole cells. The assay was performed by following the manufacturer’s instruction.
Data Analysis
All data are expressed as mean ± SEM, and the number of sample studied (n) is ≥3. One-way ANOVA was used to determine effects of flow pulsatility on gene expression. If significantly difference exists, Student’s t test for one-to-one comparison and Tukey for post hoc analysis were used to compare means of each individual group. A p value <0.05 was considered significantly different.
Results
HPF induced EndMT after 48 h stimulation
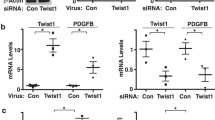
Our previous studies have shown that HPF changes vasoactive and proinflammatory activities of bovine PAECs.38 Similar to the responses of bovine cells to HPF, HPAECs produced pro-vasoconstriction and pro-inflammation factors after exposure to HPF (S-Fig. 1 in the Supplemental information). We further asked whether HPAECs would resolve acute inflammation and vasoconstrictive response by making the phenotypic transition to a mesenchymal phenotype. As shown in Fig. 1a, results demonstrated that HPF significantly increased HPAEC mRNA expression of α-SMA, TGF-β1, and COL1A1 molecules by 4-20 folds, when compared to steady flow after 48 h of flow condition, while no significant difference in all these mRNAs were found between cells under HPF and steady flow after 24 h of flow condition. Also, HPF enhanced cell mRNA expression of these EndMT markers after cells were exposed to the flow for a longer period of time (48 vs. 24 h), whereas steady flow reduced cell expression of these mRNAs over the time, which, except COL1A1, showed no significant difference from the static condition after 48 h. On the other side, HPAEC exposure to HPF for 48 h significantly reduced mRNA expression of EC marker, PECAM-1, exhibiting up to 148-fold decrease when compared to the steady flow or static conditions (Fig. 1b). Comparison to the static control provided baseline EC response to fluid shear within the study, and reinforced the steady flow as a relevant model for comparison to HPF. These results indicate that EndMT occurs in the endothelial cells exposed to the HPF condition after 48 h, a relatively longer period of time than that needed to induce pro-inflammatory responses (6–24 h).
Gene expression results showing that ECs after 48 h HPF stimulation undergo the EndMT process. (a) The EC expression of αSMA, COL1A1 (for collagen type I) and TGF-β1 mRNAs after 24 or 48 h under steady flow or HPF, using the static condition for comparison. Compared to those exposed to the steady flow, cells after 48 h of HPF stimulation showed significantly higher levels in all of these mesenchymal phenotypic genes while cells after 24 h of HPF stimulation only showed significantly higher expression in α-SMA mRNA. The ∆∆CT method was used to determine the gene expression. (b) The mRNA expression of endothelial marker, platelet endothelial cell adhesion molecule (PECAM-1), in ECs after flow stimulation. Compared to those under steady flow, the cells under HPF for 48 h showed significantly reduced PECAM-1 mRNA expression, indicating a reduction in EC phenotype; the cells under HPF for 24 h did not show different PECAM-1 expression when compared to those under steady flow. These results suggest that HPF promoted the mesenchymal transition of ECs after stimulation for a longer time period (48 h). Statistical analysis using ANOVA and Welch’s two-tailed t-test: *indicates p < 0.05 vs. the steady flow after flow stimulation for the same period of time.
To confirm the findings from gene expression, protein analyzes were performed on selected molecular markers. Results from western blots support the PCR results. As shown in Fig. 2, when compared to the cells under steady flow for 48 h, ECs under the HPF condition for the same duration increased the protein expression of α-SMA, TGF-β1, and COL1A1, by 191, 33, and 25%, respectively, while these HPF-stimulated ECs exhibited 42.8% reduction in PECAM-1 protein expression.
Results from western Wetting assays show the EndMT-related markers expressed by ECs after 48 h of flow stimulation. Compared to the steady flow condition, HPF significantly downregulated EC marker PECAM while it upregulated all the mesenchymal phenotype markers, which demonstrates the change of ECs under HPF from the endothelial phenotype to the mesenchymal, myofibroblast-like phenotype. Quantitative measures of protein expression increase and representative western blotting bands are shown. Statistical significance (p < 0.05) was found in all the protein expression comparisons between the steady and the HPF.
Flow-Conditioned Media from ECs Under HPF Induced EndMT of HPAEC and Activated Migration and Proliferation of AdvEC
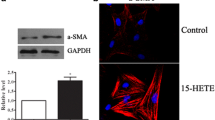
As we found that HPF promoted EC production of TGF-β1, we further asked whether TGF-β1 and other cytokines produced by the cells remain active in the flow conditioned media (FCM) and sufficient to affect neighboring ECs or AdvFBs. To address this question, FCM were collected after 24 or 48 h flow experiments and were used to culture normal HPAEC and AdvFB, respectively. As shown in Fig. 3, results demonstrated that FCM taken from the EC culture stimulated by the HPF condition for 48 h significantly increased α-SMA protein expression in both AdvFB and EC, when compared to all the other FCM conditions. This suggests the cytokines secreted by HPAECs under HPF could sustain continuous trans-differentiation of ECs and activation of AdvFBs.
Flow-conditioned media (FCM) from ECs after 48 h stimulation with HPF induced quiescent ECs and AdvFBs to express α-SMA protein expression. AdvFBs and ECs both cultured in FCM pre-conditioned with steady flow and HPF for both 24 and 48 h time points. Quantitative measures of protein expression increase and representative western blotting bands are shown. (a) Fold change of α-SMA/β-actin in AdvFBs cultured in different FCM conditions relative to that from the steady FCM. (b) Fold change of α-SMA/β-actin in ECs cultured in different FCM conditions relative to that from the steady FCM. Results showed that fractional differences in 5MA dramatically increase for the 48 h time points, with 127 and 52% for AdvFBs and ECs respectively *shows p < 0.05 vs. FCM from the steady flow condition after the same stimulation period.
In addition, migration and proliferation assays were performed on the AdvFB cultured with various FCM. As shown in Fig. 4, migration assay results showed that significantly more AdvFB cells migrated towards FCM taken from ECs under HPF, when compared to the cells migrated towards steady flow, for both 24 and 48 h time points. Proliferation assay results showed that AdvFB cell proliferation in FCM from HPF conditions was also significantly higher, when compared to that in FCM from steady flow, for both 24 and 48 h time points.
Flow-conditioned culture media from ECs exposed to HPF significantly enhanced AdvFB migration and proliferation. (a) Representative images showing AdvFB migration towards flow conditioned media (FCM) from ECs under different flow conditions. AdvFBs are stained on the opposite side of the filter with crystal violet. (b) Quantitative results from AdvFB migration assays, showing fold changes of migrated cells in comparison with the control using unconditioned culture media. (c) Cell proliferation results of AdvFB cultured with FCM. Statistically significant results (p < 0.05) in AdvFB migration or proliferation are shown between FCM from high pulsatility flow and FCM from steady flow by (*) for similar time points, †shows statistically significant results (p < 0.01) between experimental conditions and the unconditioned media (control).
Taxol Reduced EndMT Response of HPAEC
Herein, we asked whether inhibiting microtubule dynamics using Paclitaxel (taxol) could inhibit microtubulin dynamics, and reverse the EndMT process of HPAECs under HPF stimuli. As shown in Fig. 5, the addition of taxol reduced EndMT markers in HPAECs under HPF, including α-SMA, TGF-β1 and COLIA1, and retained the expression level of endothelial marker (PECAM-1). Microtubulin thus played an essential role in HPF-induced EndMT and stabilized the EC structure to protect cells from transitioning to a mesenchymal myofibroblast-like phenotype.
Results fiom western blowing assays show that taxol induced changes after 48 h of HPF stimulation. Fractional increase in EC expression of EMT-related proteins after taxol treatment (HPF + Taxol) is shown in comparison with the untreated group, HPF(−). Quantitative measures of protein expression increase and representative western blotting bands are shown Statistical significance (p < 0.05) was found in all the protein expression comparisons between the treated and untreated groups. Increased PECAM expression as well as decreased TGF-β1 collagen I. and α- SMA all indicate a reduction in phenotype changes in ECs caused by HPF.
Cell Apoptosis Preceded the EndMT
Previous studies have shown that EC released TGF-β1 during EC apoptosis.6,39 These in conjunction with our findings that show ECs exposed to HPF continuously produce TGF-β1 which further induce EC transition to mesenchymal fibroblastic phenotype and enhance AdvFB activities, suggest that ECs might show enhanced apoptotic activity prior to the EndMT process, releasing TGF-β1 for autocrine and paracrine signaling towards fibrosis. We therefore studied whether the occurrence of endothelial transition into a pathological fibroblastic phenotype were preceded by endothelial apoptosis. To address this question, caspase assay was used to assess cell apoptosis after 24 h flow conditioning. Results showed that HPF induced much higher percentage of apoptotic cells (~55%) when compared to steady flow (~2%), as shown in Fig. 6. The co-existence of apoptotic cells and non-apoptotic cells are interesting facts of the HPF-induced changes.
Discussion
Results from the present study demonstrate that HPF induces EndMT in HPAECs, likely stemming from HPF-induced endothelial dysfunction characterized by inflammation, adverse production of vasoactive substances and apoptotic responses. Evidence is presented in gene and protein assays of cells after 48 h exposure to HPF, showing dramatic downregulation of PECAM-1 (EC marker), and significant upregulation of mesenchymal cell markers including α-SMA, COL1A1, and TGF-β1. This demonstrates EC changes into a myofibroblast-like mesenchymal phenotype. In addition, flow-conditioned media further sustained the stimulating effects of HPF on EndMT and on activation, migration and proliferation of AdvFBs, all of which are related to progressive fibrosis of vascular tissues in diseased conditions. We also found that paclitaxel application in the flow media effectively reduced EndMT response.
TGF-β1 could play a critical role in perpetuating flow-induced vascular fibrosis. TGF- β1 is such a highly potent cytokine that it alone may not only induce the inflammatory response, but also induce EndMT of ECs.11,42,43 The presence of TGF-β1 produced by HPAECs under HPF is likely instrumental in sustaining EndMT and increasing fibroblast proliferation, migration and activation to α-SMA+ myofibroblasts through myogenic process. Our finding is consistent with previous studies showing that TGF-β1 release was found after EC apoptosis,34,35,39 or during EC exposure to high shear.6,41 TGF-β1 has also been repeatedly shown to increase fibrosis and the encapsulation phase of the inflammatory response. More relevant to the current study is that TGF-β1 was shown to directly initiate EndMT in a number of previous studies.15,17,19,25,44
Though little is known about cellular mechanisms underlying the EndMT and few successful chemical signals have been shown to prevent EndMT, evidence emerges that lack of primary cilia, acetylated microtubule, primes the EndMT process in the endothelium, while EndMT diminished with increasing primary cilia expression in ECs.9 Our previous study showed that the microtubulin played an important role in transducing HPF to proinflammatory signals.21 Paclitaxel (taxol), inhibits microtubule dynamics and thus cell proliferation in cancer chemotherapy, has also been previously used to reinforce primary cilia.14,16 Paclitaxel is commonly used in cancer chemotherapy to prevent tumor growth, and as prevention in restenosis through preventing SMC migration and proliferation.20 This study suggests that paclitaxel may attenuate vascular dysfunction by additionally helping to stabilize EC cytoskeleton and reduce EndMT via altered endothelial mechano-transduction of HPF.9,16
Different from previous studies on flow-induced endothelial dysfunction using disturbed flow,27 or oscillatory flow shear conditions47 with the mean flow shear stress below a physiological value, as occurring in the case of arterial stenosis, HPF is characterized by unidirectional flow condition with the mean flow shear within the physiological range, and is correlated to increased upstream vascular stiffness.23 The results shown here as well as our previous studies have provided evidence that HPF would create a positive feedback loop through applying high flow pulsatility to ECs on a stiff structure, exacerbating endothelial dysfunction and vascular fibrosis. Besides enhanced inflammatory response and EndMT in EC, HPF also led to increased apoptosis prior to EndMT. Previous studies have shown that a direct result of apoptosis-resistant EC, due to unfavorable flow conditions, chemically-induced EC apoptosis, or growth factor inhibition, is post-apoptosis proliferation of these cells; apoptosis-resistant ECs, likely showing a mesenchymal phenotype, may be hyperproliferative and more capable of withstanding harsh biochemical and biophysical stimuli.6,34–38,41 HPF fosters the emergence of mesenchymal fibroblasts, which likely are apoptosis-resistant cells either proliferating to thicken vascular intima by fibrosis or producing cytokines to activate fibroblast migration and proliferation. This may further explain in vivo findings of vascular fibrosis, which often is characterized by α-SMA + cells in all vascular layers and/or increased intimal area.7 The possible mechanism of HPF on vascular fibrotic remodeling is illustrated in Fig. 7.
Change history
08 September 2021
This article has been retracted. Please see the Retraction Notice for more detail: https://doi.org/10.1007/s12195-021-00701-z
Abbreviations
- EndMT:
-
Endothelial-to-mesenchymal transdifferentiation
- HPF:
-
High pulsatility flow
- EC:
-
Endothelial cell
- SMC:
-
Smooth muscle cell
- AdvFB:
-
Adventitial fibroblast
- HPAEC:
-
Human pulmonary arterial ECs
- PI:
-
Pulsatility index
- TGF-β:
-
Transforming growth factor β
References
Acharya, P. S., et al. Fibroblast migration is mediated by CD44-dependent TGF activation. J. Cell Sci. 121:1393–1402, 2008.
Arciniegas, E., L. Ponce, Y. Hartt, A. Graterol, and R. G. Carlini. Intimal thickening involves transdifferentiation of embryonic endothelial cells. Anat. Rec. 258:47–57, 2000.
Arciniegas, E., A. B. Sutton, T. D. Allen, and A. M. Schor. Transforming growth factor beta 1 promotes the differentiation of endothelial cells into smooth muscle-like cells in vitro. J. Cell Sci. 103:521–529, 1992.
Battegay, E. J., E. W. Raines, R. A. Seifert, D. F. Bowen-Pope, and R. Ross. TGF-beta induces bimodal proliferation of connective tissue cells via complex control of an autocrine PDGF loop. Cell 63:515–524, 1990.
Berard, X., et al. Role of hemodynamic forces in the ex vivo arterialization of human saphenous veins. J. Vasc. Surg. 57:1371–1382, 2013.
Cucina, A., A. V. Sterpetti, V. Borrelli, S. Pagliei, A. Cavallaro, and L. S. D’Angelo. Shear stress induces transforming growth factor–beta1 release by arterial endothelial cells. Surgery 123:212–217, 1998.
Dilley, R. J., J. K. McGeachie, and F. J. Prendergast. A review of the histologic changes in vein-to-artery grafts, with particular reference to intimal hyperplasia. Arch. Surg. 123:691–696, 1988.
Egorova, A. D., et al. Tgfβ/Alk5 signaling is required for shear stress induced klf2 expression in embryonic endothelial cells. Dev. Dyn. 240:1670–1680, 2011.
Egorova, A. D., et al. Lack of primary cilia primes shear-induced endothelial-to-mesenchymal transition. Circ. Res. 108:1093–1101, 2011.
Egorova, A. D., et al. Endothelial colony-forming cells show a mature transcriptional response to shear stress. Vitro Cell. Dev. Biol. Anim. 48:21–29, 2012.
Frid, M. G. Mature vascular endothelium can give rise to smooth muscle cells via endothelial-mesenchymal transdifferentiation. Vitro Anal. Circ. Res. 90:1189–1196, 2002.
Gan, C. T.-J., et al. Noninvasively assessed pulmonary artery stiffness predicts mortality in pulmonary arterial hypertension. CHEST J. 132:1906–1912, 2007.
Garanich, J. S., R. A. Mathura, Z.-D. Shi, and J. M. Tarbell. Effects of fluid shear stress on adventitial fibroblast migration: implications for flow-mediated mechanisms of arterialization and intimal hyperplasia. AJP Heart Circ. Physiol. 292:H3128–H3135, 2007.
Hamel, E., A. A. Del Campo, M. C. Lowe, and C. M. Lin. Interactions of taxol, microtubule-associated proteins, and guanine nucleotides in tubulin polymerization. J. Biol. Chem. 256:11887–11894, 1981.
Hashimoto, N., et al. Endothelial–mesenchymal transition in bleomycin-induced pulmonary fibrosis. Am. J. Respir. Cell Mol. Biol. 43:161–172, 2010.
Hierck, B. P., et al. Primary cilia sensitize endothelial cells for fluid shear stress. Dev. Dyn. Off. Publ. Am. Assoc. Anat. 237:725–735, 2008.
Imamura, H., et al. Transdifferentiation of bone marrow-derived endothelial progenitor cells into the smooth muscle cell lineage mediated by tansforming growth factor-β1. Atherosclerosis 211:114–121, 2010.
Khalil, N., Y. D. Xu, R. O’Connor, and V. Duronio. Proliferation of pulmonary interstitial fibroblasts is mediated by transforming growth factor-beta1-induced release of extracellular fibroblast growth factor-2 and phosphorylation of p38 MAPK and JNK. J. Biol. Chem. 280:43000–43009, 2005.
Kokudo, T., Y. Suzuki, Y. Yoshimatsu, T. Yamazaki, T. Watabe, and K. Miyazono. Snail is required for TGF -induced endothelial-mesenchymal transition of embryonic stem cell-derived endothelial cells. J. Cell Sci. 121:3317–3324, 2008.
Lao, L. L., and S. S. Venkatraman. Adjustable paclitaxel release kinetics and its efficacy to inhibit smooth muscle cells proliferation. J. Control. Release Off. J. Control. Release Soc. 130:9–14, 2008.
Li, M., K. R. Stenmark, R. Shandas, and W. Tan. Effects of pathologic flow on pulmonary artery endothelial production of vasoactive mediators and growth factors. J. Vasc. Res. 46:561–571, 2009.
Li, L., et al. Cellular and morphological changes during neointimal hyperplasia development in a porcine arteriovenous graft model. Nephrol. Dial. Transplant. 22:3139–3146, 2007.
London, G., et al. Arterial aging and arterial disease: interplay between central hemodynamics, cardiac work, and organ flow—implications for CKD and cardiovascular disease. Kidney Int. Suppl. 1:10–12, 2011.
Maddaluno, L., et al. EndMT contributes to the onset and progression of cerebral cavernous malformations. Nature 498:492–496, 2013.
Medici, D., S. Potenta, and R. Kalluri. Transforming growth factor-β2 promotes Snail-mediated endothelial–mesenchymal transition through convergence of Smad-dependent and Smad-independent signalling. Biochem. J. 437:515–520, 2011.
Mitchell, G. F., et al. Arterial stiffness, pressure and flow pulsatility and brain structure and function: the age, gene/environment susceptibility—reykjavik study. Brain 134:3398–3407, 2011.
Nagel, T., N. Resnick, C. F. Dewey, and M. A. Gimbrone. Vascular endothelial cells respond to spatial gradients in fluid shear stress by enhanced activation of transcription factors. Arterioscler. Thromb. Vasc. Biol. 19:1825–1834, 1999.
Nakajima, Y., T. Yamagishi, S. Hokari, and H. Nakamura. Mechanisms involved in valvuloseptal endocardial cushion formation in early cardiogenesis: roles of transforming growth factor (TGF)-β and bone morphogenetic protein (BMP). Anat. Rec. 258:119–127, 2000.
Owens, C. D. Adaptive changes in autogenous vein grafts for arterial reconstruction: clinical implications. J. Vasc. Surg. 51:736–746, 2010.
Palevsky, H. I., et al. Primary pulmonary hypertension. Vascular structure, morphometry, and responsiveness to vasodilator agents. Circulation 80:1207–1221, 1989.
Panaritis, V., et al. Pulsatility index of temporal and renal arteries as an early finding of arteriopathy in diabetic patients. Ann. Vasc. Surg. 19:80–83, 2005.
Pries, A. R., B. Reglin, and T. W. Secomb. Remodeling of blood vessels: responses of diameter and wall thickness to hemodynamic and metabolic stimuli. Hypertension 46:725–731, 2005.
Rekhter, M., S. Nicholls, M. Ferguson, and D. Gordon. Cell proliferation in human arteriovenous fistulas used for hemodialysis. Arterioscler. Thromb. Vasc. Biol. 13:609–617, 1993.
Sakao, S. Apoptosis of pulmonary microvascular endothelial cells stimulates vascular smooth muscle cell growth. AJP Lung Cell. Mol. Physiol. 291:L362–L368, 2006.
Sakao, S., L. Taraseviciene-Stewart, J. D. Lee, K. Wood, C. D. Cool, and N. F. Voelkel. Initial apoptosis is followed by increased proliferation of apoptosis-resistant endothelial cells. FASEB J. 19:1178–1180, 2005.
Sakao, S., K. Tatsumi, and N. F. Voelkel. Endothelial cells and pulmonary arterial hypertension: apoptosis, proliferation, interaction and transdifferentiation. Respir. Res. 10:95, 2009.
Sakao, S., et al. VEGF-R blockade causes endothelial cell apoptosis, expansion of surviving CD34 + precursor cells and transdifferentiation to smooth muscle-like and neuronal-like cells. FASEB J. 21:3640–3652, 2007.
Scott, D., Y. Tan, R. Shandas, K. R. Stenmark, and W. Tan. High pulsatility flow stimulates smooth muscle cell hypertrophy and contractile protein expression. AJP Lung Cell. Mol. Physiol. 304:L70–L81, 2013.
Solovyan, V. T., and J. Keski-Oja. Apoptosis of human endothelial cells is accompanied by proteolytic processing of latent TGF-β binding proteins and activation of TGF-β. Cell Death Differ. 12:815–826, 2005.
Suwanabol, P. A., et al. Transforming growth factor-β increases vascular smooth muscle cell proliferation through the Smad3 and extracellular signal-regulated kinase mitogen-activated protein kinases pathways. J. Vasc. Surg. 56:446.e1–454.e1, 2012.
Ten Dijke, P., A. D. Egorova, M.-J. T. H. Goumans, R. E. Poelmann, and B. P. Hierck. TGF-β signaling in endothelial-to-mesenchymal transition: the role of shear stress and primary cilia. Sci. Signal. 5:pt2, 2012.
Tsai, S., et al. TGF-β through Smad3 signaling stimulates vascular smooth muscle cell proliferation and neointimal formation. Am. J. Physiol. Heart Circ. Physiol. 297:H540–H549, 2009.
Varcoe, R. L., et al. The role of the fibrocyte in intimal hyperplasia. J. Thromb. Haemost. 4:1125–1133, 2006.
Zeisberg, E. M., S. E. Potenta, H. Sugimoto, M. Zeisberg, and R. Kalluri. Fibroblasts in kidney fibrosis emerge via endothelial-to-mesenchymal transition. J. Am. Soc. Nephrol. 19:2282–2287, 2008.
Zeisberg, E. M., S. Potenta, L. Xie, M. Zeisberg, and R. Kalluri. Discovery of endothelial to mesenchymal transition as a source for carcinoma-associated fibroblasts. Cancer Res. 67:10123–10128, 2007.
Zeisberg, E. M., et al. Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nat. Med. 13:952–961, 2007.
Ziegler, T., K. Bouzourène, V. J. Harrison, H. R. Brunner, and D. Hayoz. Influence of oscillatory and unidirectional flow environments on the expression of endothelin and nitric oxide synthase in cultured endothelial cells. Arterioscler. Thromb. Vasc. Biol. 18:686–692, 1998.
Acknowledgment
The authors wish to thank Dr Kurt Stenmark’s lab for providing help and acknowledge funding sources, including AHA (13GRNT16990019 to W.T) and NHLBI (HL 097246 and HL119371 to W.T.).
Conflict of interest
The authors, Winston Elliott, Yan Tan, Min Li and Wei Tan, declare that they have no conflicts of interest.
Ethical Standards
No human studies were carried out by the authors for this article. No animal studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Michael R. King oversaw the review of this article.
About this article
Cite this article
Elliott, W.H., Tan, Y., Li, M. et al. RETRACTED ARTICLE: High Pulsatility Flow Promotes Vascular Fibrosis by Triggering Endothelial EndMT and Fibroblast Activation. Cel. Mol. Bioeng. 8, 285–295 (2015). https://doi.org/10.1007/s12195-015-0386-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12195-015-0386-7