Abstract
The prevalence of heart failure grows yearly, and incidence rates are expected to potentiate given the growing aging population. There have been numerous advancements over the past several decades in the management of heart failure, yet the burden of disease in the form of quality of life, frequency of hospitalization, and healthcare cost remains high. Several comorbid conditions, lifestyle factors, pharmacologic agents, and biochemical markers have been associated with increased risk of heart failure resulting in the formulation of risk models for prediction. Although further investigation is still needed in order to more clearly elucidate individuals most at risk for the development of heart failure, this remains a critical objective in order to allow for the implementation of preventive strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Heart failure (HF) is a growing public health concern, with a prevalence of 5.1 million in the USA and an incidence that increases with age [1]. Over the next 50 years, the aging population is expected to rise with a projected 92 million people aged greater than 65 and 18 million people aged greater than 85 [2]. In spite of the predominance of elderly HF patients, they remain an underrepresented population in clinical trials due to comorbid conditions and concern for polypharmacy [3]. The cost of HF further adds to the burden of this disease in the USA with a projected indirect cost of $17.4 billion and direct cost of $77.7 billion in 2030 [4]. The American Heart Association and the American College of Cardiology encourage a proactive approach in the staging of heart failure to include “stage A” for patients with risk factors for heart failure but without structural heart disease [5]. Similarly, patients in “stage B” who have structural heart disease but no overt symptoms are ideal targets for prevention of progression. The anticipated rise in the elderly population and presumed worsening of the heart failure epidemic compounded by its economic strain highlights the paramount need for risk factor identification and implementation of prevention strategies.
Risk Factors for Heart Failure
There are a variety of risk factors that have been described for heart failure, including certain comorbidities, lifestyle factors, biochemical markers, and pharmacologic exposures (Table 1).
Comorbidities
Comorbid conditions such as obesity, hypertension, diabetes, valvular heart disease, and coronary heart disease are independent risk factors for HF [6••]. Among Medicare beneficiaries, more than twice as many patients with HF were greater than 85 compared to 65–69 years of age. The very elderly HF patients were less likely to have underlying coronary artery disease or hypertension and more likely to have worse renal function [7]. Another study of elderly patients found male gender, older age, diabetes, lack of emotional support, hypertension, and increase body mass index to be risk factors for the development of heart failure [8]. Pulse pressure has also been shown to be an independent predictor of HF in the elderly [9]. Hyperlipidemia is a risk for HF; however, it is unclear if this is related to atherosclerosis [10]. Depression in elderly women, but not men, is an independent risk factor for HF [11]. Elderly patients with renal insufficiency have an increased risk of HF, and the risk increases with increasing creatinine level [12]. Sleep-disordered breathing is another important risk factor of HF, independent of other known risk factors [13].
Lifestyle Factors
Physical inactivity, cigarette smoking, as well as less education are all risk factors for HF [6••]. Moderate alcohol consumption, independent of reduction in myocardial infarction risk, is associated with lower risk of heart failure in the elderly [14]. While there has been discrepancy in the role of caffeine in heart failure, a meta-analysis found an inverse relationship between four cups of coffee per day and incidence of heart failure [15]. In overweight individuals, increased dietary sodium intake is a strong independent risk factor for HF [16].
Pharmacologic Exposures
Among elderly HF patients taking diuretics, the use of non-steroidal anti-inflammatory drugs resulted in a twofold increased risk of first hospitalization for heart failure [17]. Risk of heart failure was also increased in patients taking doxazosin [18]. Among diabetics, use of thiazolidinediones was associated with fluid retention and heart failure [19]. Various chemotherapeutic agents such as anthracyclines, alkylating agents, taxanes, and monoclonal antibodies have all been associated with increased risk of heart failure [20].
Echocardiographic Parameters
In an elderly cohort, ventricular dysfunction and abnormalities in left ventricular diastolic filling was predictive of HF [21]. In addition, left ventricular mass was shown to predict heart failure independent of myocardial infarction [22]. Left atrial volume independently predicted HF in patients with preserved systolic function [23].
Biochemical Markers
Cystatin C, an alternate measure of renal function, was shown to be an independent risk factor for HF in the elderly [24]. Elevations in inflammatory markers such as interleukin-6, tumor necrosis factor-α, and C-reactive protein are also associated with increased risk of HF in elderly patients [25, 26]. In adults without prior myocardial infarction, elevated plasma homocysteine levels independently predicted HF development [27]. Albuminuria, regardless of the presence or absence of diabetes, is a risk factor for cardiovascular events and heart failure hospitalization [28]. Higher rates of insulin-like growth factor-1 are associated with lower incidences of heart failure [29].
Genetic Factors
Polymorphisms of the β1-adrenergic receptor (β1Arg389) and α2C-adrenergic receptor (α2CDel322-325) are synergistically associated with increased risk of heart failure among black subjects [30].
Risk Factor Models
Although there are numerous known risk factors for HF, individual risk factors are not enough to predict incident HF in the general population. As such, several risk models have been developed.
Framingham Heart Study
The Framingham Heart Failure Risk Score (FHFRS) assessed the probability of developing heart failure in subjects’ aged 45 through 94 years over the course of a 38-year study period [31••]. A 4-year event score was created based on the variables of age, forced vital capacity, systolic blood pressure, heart rate, left ventricular hypertrophy on electrocardiogram, coronary artery disease, valve disease, diabetes, and cardiomegaly. However, there are several limitations to this model. The population studied was primarily white, and thus, the applicability of this model to individuals in other racial groups is unknown. In addition, subjects were required to have a known history of coronary artery disease, hypertension, or valvular disease. Furthermore, the requirement of chest radiography and pulmonary function testing for certain variables limits the large-scale use of this score in the general population where that data may be unavailable. This model has also not been externally validated in independent cohorts (Table 2).
Health, Aging, and Body Composition Study
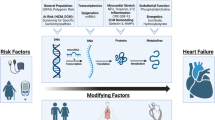
The Health, Aging, and Body Composition (Health ABC) study followed patients aged 70–79 years to determine the incidence of HF, the population-attributable risk of independent risk factors for HF, and outcomes of incident HF [27]. Investigators subsequently developed the Health ABC HF Score which included the variables age, heart rate, fasting glucose, coronary artery disease, smoking, creatinine, left ventricular hypertrophy, albumin, and systolic blood pressure in order to predict 5-year HF risk (Fig. 1) [32••]. In comparison to the FHFRS, the Health ABC HF Score had better discrimination for incident HF. In addition, the score predicted risk equally in both white and male subjects. The variables in the score are readily obtainable in the clinical setting, and eight of the nine variables are modifiable, providing opportunities for prevention. The Health ABC HF model was externally validated in the Cardiovascular Health Study (CHS), a large community-based cohort of individuals aged 65–100 years [33]. Limitations to this model include the lack of data collection on valvular heart disease as well as inclusion of only elderly patients who were relatively healthy, and thus, the applicability of this score to patients of variable ages or with higher burden of comorbid disease remains unknown.
Atherosclerosis Risk in Communities Study
The Atherosclerosis Risk in Communities (ARIC) study analyzed a biracial cohort of middle-aged participants to examine the external validity of the FHFRS and Health ABC scores in addition to the derivation of an ARIC HF risk score [34]. The optimal model for the prediction of 10-year HF risk was determined to include age, race, sex, prevalent coronary heart disease, systolic blood pressure, use of blood pressure lowering medication, diabetes, smoking status, heart rate, and body mass index. Furthermore, the inclusion of N-terminal pro-B-type natriuretic peptide (NT-proBNP) significantly improved HF risk prediction. Overall, the ARIC risk score was found to be superior to the FHFRS and comparable to the Health ABC HF score.
Prevention of Events with Angiotensin-converting Enzyme Inhibition
The Prevention of Events with Angiotensin-converting Enzyme Inhibition (PEACE) study examined 82,890 patients with stable coronary artery disease in order to develop a risk model for the prediction of HF [35]. Characteristics included in the risk score are age, body mass index, history of myocardial infarction, coronary artery bypass graft, diabetes, hypertension, angina, stroke, smoking status, left ventricular ejection fraction, estimated glomerular filtration rate in addition to use of any diuretic, digitalis, calcium channel blocker, anti-arrhythmic, and absence of lipid lowering medication.
Multi-Ethnic Study of Atherosclerosis
The Multi-Ethnic Study of Atherosclerosis (MESA) followed 6814 patients without clinical cardiac disease at baseline with the intent to develop a 5-year risk score for incident HF [36]. In this cohort of patients, a model was developed based on age, gender, body mass index, smoking status, systolic blood pressure, heart rate, diabetes, and NT-proBNP. These parameters are all readily available in the clinic setting. Similar to the ARIC study, the addition of NT-proBNP provided the largest contribution to risk assessment.
Intermountain Heart Collaborative Study
The Intermountain Risk Score (IMRS) incorporates information from the complete blood count and basic metabolic panel in addition to age and sex, initially intended to predict mortality at 30 days, 1 year, and 5 years [37]. The IMRS was shown to also be predictive of HF, left ventricular ejection fraction, readmission for HF, incident HF, myocardial infarction diagnosis, incident myocardial infarction, atrial fibrillation, and chronic obstructive pulmonary disease. The red cell distribution width was shown to be particularly predictive of HF.
Beyond Clinical Risk Factors
Echocardiographic parameters and biomarkers such as natriuretic peptides and troponin have been studied to determine whether they provide an added role in the prediction of HF. In the CHS cohort, ejection fraction, enlarged left atrium, and E/A ration were independent predictors of HF risk when added to the Health ABC HF Score [38•]. In addition, NT-proBNP levels were independently associated with HF risk when added to the ABC HF Risk Score and the combination of NT-proBNP and echocardiography had incremental value over each modality alone. In the same cohort, baseline levels of cardiac troponin T (cTnT) were strongly associated with incident HF and cardiovascular death independent of other risk factors [39]. Furthermore, changes in cTnT over 2–3 years were also associated with increased risk of HF.
The emerging field of genomics adds further potential for risk stratification. Microarrays can allow for the quantification and monitoring of gene expression; however, use is currently limited to the investigational arena [40]. The incorporation of genetic polymorphisms in risk prediction is appealing; however, genetic markers would need to show incremental improvement over validated risk scores and must be uncorrelated with known risk factors to ensure independent risk [41].
Conclusion
Heart failure poses a unique challenge due to the high incidence among the elderly and the burgeoning aging population. The identification of risk factors is critical in order to curb the anticipated rise in disease and healthcare costs. While there are a variety of known risk factors for incident heart failure, individual risk factors are alone not enough to predict who will develop this disease and as a result, several risk models have been proposed. Overall, further investigation is needed prior to the large scale implementation of these screening models in clinical practice.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance, •• Of major importance
Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Drazner MH, et al. 2013 ACCF/AHA guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013;128:1810–52.
Bureau USC. National population projections: summary tables. Table 2. Projections of population by selected age groups and sex for the United States: 2015 to 2060. 2012.
Heiat A, Gross CP, Krumholz HM. Representation of the elderly, women, and minorities in heart failure clinical trials. Arch Intern Med. 2002;162:1682–8.
Heidenreich PA, Trogdon JG, Khavjou OA, Butler J, Dracup K, Ezekowitz MD, et al. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation. 2011;123:933–44.
Hunt SA, Abraham WT, Chin MH, Feldman AM, Francis GS, Ganiats TG, et al. 2009 Focused update incorporated into the ACC/AHA 2005 Guidelines for the Diagnosis and Management of Heart Failure in Adults: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines developed in collaboration with the International Society for Heart and Lung Transplantation. J Am Coll Cardiol. 2009;53:e1–90.
He J, Ogden LG, Bazzano LA, Vupputuri S, Loria C, Whelton PK. Risk factors for congestive heart failure in US men and women: NHANES I epidemiologic follow-up study. Arch Intern Med. 2001;161:996–1002. This epidemiologic follow-up study examined a large population of patients to determine risk factors for heart failure and their corresponding attributable risk.
Havranek EP, Masoudi FA, Westfall KA, Wolfe P, Ordin DL, Krumholz HM. Spectrum of heart failure in older patients: results from the National Heart Failure project. Am Heart J. 2002;143:412–7.
Chen YT, Vaccarino V, Williams CS, Butler J, Berkman LF, Krumholz HM. Risk factors for heart failure in the elderly: a prospective community-based study. Am J Med. 1999;106:605–12.
Chae CU, Pfeffer MA, Glynn RJ, Mitchell GF, Taylor JO, Hennekens CH. Increased pulse pressure and risk of heart failure in the elderly. JAMA. 1999;281:634–43.
Kenchaiah S, Narula J, Vasan RS. Risk factors for heart failure. Med Clin North Am. 2004;88:1145–72.
Williams SA, Kasl SV, Heiat A, Abramson JL, Krumholz HM, Vaccarino V. Depression and risk of heart failure among the elderly: a prospective community-based study. Psychosom Med. 2002;64:6–12.
Fried LF, Shlipak MG, Crump C, Bleyer AJ, Gottdiener JS, Kronmal RA, et al. Renal insufficiency as a predictor of cardiovascular outcomes and mortality in elderly individuals. J Am Coll Cardiol. 2003;41:1364–72.
Shahar E, Whitney CW, Redline S, Lee ET, Newman AB, Nieto FJ, et al. Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the Sleep Heart Health Study. Am J Respir Crit Care Med. 2001;163:19–25.
Abramson JL, Williams SA, Krumholz HM, Vaccarino V. Moderate alcohol consumption and risk of heart failure among older persons. JAMA. 2001;285:1971–7.
Mostofsky E, Rice MS, Levitan EB, Mittleman MA. Habitual coffee consumption and risk of heart failure: a dose-response meta-analysis. Circ Heart Fail. 2012;5:401–5.
He J, Ogden LG, Bazzano LA, Vupputuri S, Loria C, Whelton PK. Dietary sodium intake and incidence of congestive heart failure in overweight US men and women: first National Health and Nutrition Examination Survey Epidemiologic Follow-up Study. Arch Intern Med. 2002;162:1619–24.
Heerdink ER, Leufkens HG, Herings RM, Ottervanger JP, Stricker BH, Bakker A. NSAIDs associated with increased risk of congestive heart failure in elderly patients taking diuretics. Arch Intern Med. 1998;158:1108–12.
Messerli FH. Doxazosin and congestive heart failure. J Am Coll Cardiol. 2001;38:1295–6.
Delea TE, Edelsberg JS, Hagiwara M, Oster G, Phillips LS. Use of thiazolidinediones and risk of heart failure in people with type 2 diabetes: a retrospective cohort study. Diabetes Care. 2003;26:2983–9.
Curigliano G, Mayer EL, Burstein HJ, Winer EP, Goldhirsch A. Cardiac toxicity from systemic cancer therapy: a comprehensive review. Prog Cardiovasc Dis. 2010;53:94–104.
Aurigemma GP, Gottdiener JS, Shemanski L, Gardin J, Kitzman D. Predictive value of systolic and diastolic function for incident congestive heart failure in the elderly: the Cardiovascular Health Study. J Am Coll Cardiol. 2001;37:1042–8.
de Simone G, Gottdiener JS, Chinali M, Maurer MS. Left ventricular mass predicts heart failure not related to previous myocardial infarction: the Cardiovascular Health Study. Eur Heart J. 2008;29:741–7.
Takemoto Y, Barnes ME, Seward JB, Lester SJ, Appleton CA, Gersh BJ, et al. Usefulness of left atrial volume in predicting first congestive heart failure in patients > or = 65 years of age with well-preserved left ventricular systolic function. Am J Cardiol. 2005;96:832–6.
Sarnak MJ, Katz R, Stehman-Breen CO, Fried LF, Jenny NS, Psaty BM, et al. Cystatin C concentration as a risk factor for heart failure in older adults. Ann Intern Med. 2005;142:497–505.
Vasan RS, Sullivan LM, Roubenoff R, Dinarello CA, Harris T, Benjamin EJ, et al. Inflammatory markers and risk of heart failure in elderly subjects without prior myocardial infarction: the Framingham Heart Study. Circulation. 2003;107:1486–91.
Kalogeropoulos A, Georgiopoulou V, Psaty BM, Rodondi N, Smith AL, Harrison DG, et al. Inflammatory markers and incident heart failure risk in older adults: the Health ABC (Health, Aging, and Body Composition) study. J Am Coll Cardiol. 2010;55:2129–37.
Kalogeropoulos A, Georgiopoulou V, Kritchevsky SB, Psaty BM, Smith NL, Newman AB, et al. Epidemiology of incident heart failure in a contemporary elderly cohort: the health, aging, and body composition study. Arch Intern Med. 2009;169:708–15.
Gerstein HC, Mann JF, Yi Q, Zinman B, Dinneen SF, Hoogwerf B, et al. Albuminuria and risk of cardiovascular events, death, and heart failure in diabetic and nondiabetic individuals. JAMA. 2001;286:421–6.
Vasan RS, Sullivan LM, D’Agostino RB, Roubenoff R, Harris T, Sawyer DB, et al. Serum insulin-like growth factor I and risk for heart failure in elderly individuals without a previous myocardial infarction: the Framingham Heart Study. Ann Intern Med. 2003;139:642–8.
Small KM, Wagoner LE, Levin AM, Kardia SLR, Liggett SB. Synergistic polymorphisms of β1- and α2C-adrenergic receptors and the risk of congestive heart failure. N Engl J Med. 2002;347:1135–42.
Kannel WB, D’Agostino RB, Silbershatz H, Belanger AJ, Wilson PW, Levy D. Profile for estimating risk of heart failure. Arch Intern Med. 1999;159:1197–204. Using patients enrolled in the Framingham Study, this study developed a model to identify high-risk candidates for heart failure.
Butler J, Kalogeropoulos A, Georgiopoulou V, Belue R, Rodondi N, Garcia M, et al. Incident heart failure prediction in the elderly: the Health ABC Heart Failure Score. Circ Heart Fail. 2008;1:125–33. This study developed a prediction model for 5-year risk of incident heart failure in the elderly.
Kalogeropoulos A, Psaty BM, Vasan RS, Georgiopoulou V, Smith AL, Smith NL, et al. Validation of the Health ABC Heart Failure model for incident heart failure risk prediction: the Cardiovascular Health Study. Circ Heart Fail. 2010;3:495–502.
Agarwal SK, Chambless LE, Ballantyne CM, Astor B, Bertoni AG, Chang PP, et al. Prediction of incident heart failure in general practice: the Atherosclerosis Risk in Communities (ARIC) Study. Circ Heart Fail. 2012;5:422–9.
Lewis EF, Solomon SD, Jablonski KA, Rice MM, Clemenza F, Hsia J, et al. Predictors of heart failure in patients with stable coronary artery disease: a PEACE study. Circ Heart Fail. 2009;2:209–16.
Chahal H, Bluemke DA, Wu CO, McClelland R, Liu K, Shea SJ, et al. Heart failure risk prediction in the Multi-Ethnic Study of Atherosclerosis. Heart. 2015;101:58–64.
Horne BD, May HT, Kfoury AG, Renlund DG, Muhlestein JB, Lappe DL, et al. The Intermountain Risk Score (including the red cell distribution width) predicts heart failure and other morbidity endpoints. Eur J Heart Fail. 2010;12:1203–13.
Kalogeropoulos AP, Georgiopoulou VV, deFilippi CR, Gottdiener JS, Butler J. Echocardiography, natriuretic peptides, and risk for incident heart failure in older adults: the Cardiovascular Health Study. JACC Cardiovasc Imaging. 2012;5:131–40. This study found that echocardiography and natriuretic peptide measurment offers heart failure risk reclassification over a clinical prediction model.
deFilippi CR, de Lemos JA, Christenson RH, Gottdiener JS, Kop WJ, Zhan M, et al. Association of serial measures of cardiac troponin T using a sensitive assay with incident heart failure and cardiovascular mortality in older adults. JAMA. 2010;304:2494–502.
Donahue MP, Marchuk DA, Rockman HA. Redefining heart failure: the utility of genomics. J Am Coll Cardiol. 2006;48:1289–98.
Thanassoulis G, Vasan RS. Genetic cardiovascular risk prediction: will we get there? Circulation. 2010;122:2323–34.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Drs. Hamo and Butler report no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the author.
Additional information
This article is part of the Topical Collection on Heart Failure Prevention
Rights and permissions
About this article
Cite this article
Hamo, C.E., Butler, J. How to Best Identify Elderly Individuals Who May Develop Heart Failure. Curr Cardiovasc Risk Rep 10, 19 (2016). https://doi.org/10.1007/s12170-016-0500-y
Published:
DOI: https://doi.org/10.1007/s12170-016-0500-y