Abstract
Cystic Hygroma (CH) also referred to as lymphangioma, is a cystic malformation of the lymphatic vessels that can occur anywhere in the body. Its incidence in adulthood is considered rare and its occurrence in the neck is even rarer and only a few case reports are available till date. We present a case of adult CH of the neck and the literature review of the same. A 30-year-old male presented with painless swelling in the left side of the neck of 2 years duration. Investigations showed a cystic mass on the left lower anterior part of the neck which was surgically removed in-toto with the intact capsule. The biopsy report confirmed the diagnosis. A differential diagnosis of CH should be considered when a cystic lesion is encountered in the neck of an adult, cytological and radiological evaluation is necessary for defining its location and diagnosis. Although various conservative modalities of management are available, they are employed only in certain situations, and surgical excision of CH is considered the gold standard. The chances of recurrence range from 15 to 20%.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Cystic hygroma (CH), or lymphangioma, is due to benign aberrant proliferation of lymphatic vessels and is a known disease of childhood, its occurrence is rarely seen among adults.CH can occur anywhere in the body, common in the cervicofacial region, axilla, and groin. [1,2,3]. The etiology of CH is disputed, trauma and respiratory tract infections are proposed as its cause among adults. [4, 5]. Diagnosis is often aided by the use of fine needle aspiration for cytology, and radiological investigations for defining its exact location and its relations to the adjacent vital structures. A complete surgical excision with an intact capsule is considered the gold standard treatment [6], however, various conservative modalities of management are available and are preferred in certain specific conditions.
Here we present a case report of an adult cervical cystic hygroma and the literature review of the same.
Case Presentation
A 30-year-old male presented to ENT OPD with complaints of painless swelling in the left lower anterior part of the neck, insidious in onset and slowly progressed to attain the present size in 2 years’ duration.
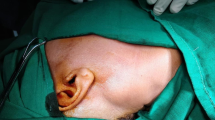
On clinical examination, there was a single smooth cystic swelling of 8 cm x 6 cm size in the left supraclavicular fossa, which was, non-tender, fluctuant, mobile, trans-illuminant and non-pulsatile. (Fig. 1).
Ultrasonography of the neck showed a cystic lesion in the left supraclavicular fossa of size 7.39 cm × 3 cm with multiple septations, Contrast-enhanced Computed tomography showed an iso-intense, well-circumscribed cystic lesion deep to the left sternocleidomastoid muscle medially and subcutaneous plane laterally, suggestive of cystic hygroma. (Fig. 2A, B).
A & B Contrast-enhanced Computed tomography—axial view showed an iso-intense, well-circumscribed cystic lesion of the lower part of the left supraclavicular fossa of about 7.2 × 6.2 × 5.2 cm in size deep to the left sternocleidomastoid muscle medially and subcutaneous plane laterally suggestive of cystic hygroma
Fine needle cytology showed a straw-colored fluid with few inflammatory infiltrates composed of lymphocytes in a thin proteinaceous background with no epithelial cells.
After obtaining consent, the patient underwent surgical excision of the cyst under general anaesthesia. A transverse cervical skin crease incision was placed, and a subplatysmal flap was raised, the greater auricular nerve was preserved, and the EJV was ligated. A single cyst of size 8.5 × 6 × 4.5 cm, translucent and multiloculated was identified and delineated from the SCM anteriorly, the trapezius, the scalenus medius, and the levator scapulae posteriorly. The transverse cervical artery was identified and preserved. The cyst was resected completely, with an intact capsule and the wound was closed in layers. (Fig. 3A & B).
Histopathological examination revealed a multilocular cyst with a wall thickness of 0.2 mm, filled with thin serous pale-yellow fluid and lined with flat endothelial-like cells, with no solid areas, necrosis, and haemorrhage, consistent with a diagnosis of cystic hygroma. (Fig. 4A & B).
Post-operatively, the patient recovered well, with no signs of any neurological dysfunction.
Discussion
CH was first described by Reden Backer in 1828 as a tumor of the lymphatic system and the term “cystic hygroma” was coined by Wernker in 1834. [7]. The word hygroma is derived from Greek which means “water tumor” or “moist tumor” because of its contents [8]. The etiology of CH among adults is not very conclusive, a delayed proliferation of lymphoid remnants secondary to neck trauma or respiratory tract infections is said to be the reason for its occurrence [9, 10].
Mulliken et al. has described CH based on their histologic appearance as either capillary lymphangiomas consisting of small lymphatic vessels, cavernous lymphangiomas consisting of larger lymphatic vessels (the most common type), or cystic lymphangiomas consisting of large macroscopic lymphatic spaces containing collagen and smooth muscle. [11] Based on histopathological findings, our case belonged to the cystic lymphangioma type.
CHs may remain asymptomatic in a patient for a long time, but if left untreated, there may be recurrent episodes of infection or haemorrhage within the cyst that can cause sudden increase in size leading to respiratory distress, oesophageal compression, and cosmetic disfigurement. In our patient, there were no compressive symptoms and the cyst was excised because the patient was concerned about cosmetic disfigurement and malignant transformation.
Surgical excision is considered the gold standard treatment for CH, complications due to surgical resection can be hematoma, postoperative seroma, chyle leak, chylous fistula owing to the location of the cyst and injuries to surrounding vital structures depending on its location. In our case we have surgically excised the lesion in-toto with an intact capsule and our patient had uneventful post op period. This patient is on a regular follow up with us and there is no recurrence for the last 1 year.
The likelihood of recurrence is approximately 15–20% with surgery, mainly due to incomplete resection or residual lesion. However, an in-toto excision is known to reduce the incidence of recurrence [12]. The risk of malignant transformation in CH or any lymphangiomas is very rare although clinical follow up is recommended for these patients. [13].
Conservative or combined management is opted in cases of inoperability where the mass involves critical structures such as airways, great vessels, and nerves of the neck that includes simple drainage or aspiration, electrocautery, cryotherapy, embolization, radiation therapy, laser surgery (using solid lasers like Nd: YAG laser or gases like CO2 laser, and semiconductor diode laser), intralesional steroid administration, intralesional sclerotherapy with OK 432 (picibanil), bleomycin, doxycycline, cyclophosphamide, alcohol, and sirolimus. However, there are concerns about the side effects of sclerosing agents [14].
Conclusion
Cystic lesions of the neck are rare among adults and there are many differential diagnosis, CH/ lymphangioma should be considered as one of them. We recommend fine needle aspiration cytology and appropriate radiological investigations to know its cytology and exact location. Although the risk of malignant transformation is unknown, they can have mass effects on vital neck structures. We recommend complete surgical excision whenever possible, and to have a regular follow up to identify recurrence.
Data and Code Availability
Not Applicable.
References
Bloom DC, Perkins JA, Manning SC (2004) Management of lymphatic malformations. Curr Opin Otolaryngol Head Neck Surg 12(6):500–504. https://doi.org/10.1097/01.moo.0000143971.19992.2d
Fliegelman LJ, Friedland D, Brandwein M, Rothschild M (2000) Lymphatic malformation: predictive factors for recurrence. Otolaryngol Head Neck Surg 123(6):706–710. https://doi.org/10.1067/mhn.2000.110963
Potdar DP, Deshpande S, Chaugule S (2013) Development and molecular characterization of cystic hygroma cell line to be used as an in Vitro model system to study the progression of hygroma in young children. Pediatr Res Int J. https://doi.org/10.5171/2013.879081
Mukakala AK, Banza MI, Musapudi EM, Lubosha NA, Kasanga TK, Nafatalewa DK, Yumba SN, Ngabunda PM, Mwenibamba RM (2020) Lymphangiome kystique du cou chez un adulte jeune: à propos d’un cas et revue de la littérature [Cystic hygroma of the neck in a young adult: about a case and literature review]. Pan Afr Med J 2(36):54. https://doi.org/10.11604/pamj.2020.36.54.21758
Damaskos C, Garmpis N, Manousi M, Garmpi A, Margonis GA, Spartalis E, Doula C, Michail-Strantzia C, Patelis N, Schizas D, Arkoumanis PT, Andreatos N, Tsourouflis G, Zavras N, Markatos K, Kontzoglou K, Antoniou EA (2017) Cystic hygroma of the neck: single center experience and literature review. Eur Rev Med Pharmacol Sci 21(21):4918–4923
McCaffrey F, Taddeo J (2015) Surgical management of adult-onset cystic hygroma in the axilla. Int J Surg Case Rep 7C:29–31. https://doi.org/10.1016/j.ijscr.2014.11.017
Bahl S, Shah V, Anchlia S, Vyas S (2016) Adult-onset cystic hygroma: a case report of rare entity. Indian J Dent 7(1):51–54. https://doi.org/10.4103/0975-962X.179374
Dogruyol T, Tozum H, Eren TS (2017) Rapidly growing cystic hygroma in an adult patient. Asian Cardiovasc Thorac Ann 25(5):395–397. https://doi.org/10.1177/0218492317713426
Morley SE, Ramesar KC, Macleod DA (1999) Cystic hygroma in an adult: a case report. J R Coll Surg Edinb 44(1):57–58
Smith RJ, Burke DK, Sato Y, Poust RI, Kimura K, Bauman NM (1996) OK-432 therapy for lymphangiomas. Arch Otolaryngol Head Neck Surg 122(11):1195–1199. https://doi.org/10.1001/archotol.1996.01890230041009
Mulliken JB, Glowacki J (1982) Hemangiomas and vascular malformations in infants and children: a classification based on endothelial characteristics. Plast Reconstr Surg 69(3):412–422. https://doi.org/10.1097/00006534-198203000-00002
Derin S, Şahan M, Dere Y, Çullu N, Şahan L (2014) Cervical cystic hygroma in an adult. Case Rep Pathol. 2014:209427. https://doi.org/10.1155/2014/209427
Laranne J, Keski-Nisula L, Rautio R, Rautiainen M, Airaksinen M (2002) OK-432 (Picibanil) therapy for lymphangiomas in children. Eur Arch Otorhinolaryngol 259(5):274–278. https://doi.org/10.1007/s00405-001-0438-6
Kim DW (2014) OK-432 sclerotherapy of lymphatic malformation in the head and neck: factors related to outcome. Pediatr Radiol 44(7):857–862. https://doi.org/10.1007/s00247-014-2889-0
Acknowledgements
Not Applicable
Funding
No funding was received for this case presentation.
Author information
Authors and Affiliations
Contributions
SC conceptualized, prepared and edited the manuscript. SA contributed to the preparation, edited and reviewed the manuscript. AN participated in preparation of the manuscript and reviewed. KRC contributed to the preparation and reviewed the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Ethical Approval
Ours is a medical record based case report for which institute ethical committee acceptance is not applicable and hence was not applied for. In our institute, case reports are not presented for ethical committee clearance. Informed consent was obtained from participant included in the case report.
Consent to Participate
Informed consent was obtained from participant included in the case report.
Consent for Publication
Written consent obtained from the participant.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chilakamarri, S., Amalanathan, S., Natarajan, A. et al. An Unusual Neck Tumor in Adult: A Case Report. Indian J Otolaryngol Head Neck Surg 76, 2813–2816 (2024). https://doi.org/10.1007/s12070-024-04508-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-024-04508-y