Abstract
Background
Objective of this study is to review our experience in the management of traumatic diaphragmatic hernias over 17 years.
Methods
Following Ethical Committee clearance, records of all patients who underwent traumatic diaphragmatic hernia surgery at Shanthabai Devarao Shivaram (SDS) Tuberculosis Research Centre and Rajiv Gandhi Institute of Chest Diseases, Bengaluru, India from January 1998 to December 2015 were reviewed. Data collected and analyzed were clinical presentation, mode of diagnosis, intraoperative findings and the postoperative clinical outcomes.
Results
Sixty patients underwent traumatic diaphragmatic hernia repair during this period. Age ranged between 10 and 80 years. The most common presentation was dyspnea. Blunt trauma was the cause in 52 (86.67%) cases and penetrating trauma in 8 (13.33%) cases. The diagnosis was within 24 h in 45 (75%) cases and in 15 (25%) cases the diagnosis was made after 24 h. Thoracotomy was the preferred approach for the repair in the absence of associated abdominal injuries. The most common site of rupture was the central tendon. The perioperative mortality was 8.33%. The hospital stay ranged between 5 and 84 days (mean 22 days).
Conclusion
Right-sided diaphragmatic hernias are notorious to be missed on initial evaluation. Despite advances in diagnostic modalities, chest X-ray still continues to be useful in the diagnosis of traumatic ruptures. A high index of suspicion, together with the knowledge of mechanism of trauma is the key factor for the correct diagnosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diaphragmatic injuries occur in 1.1–3.9% of patients suffering from thoracoabdominal trauma [1]. Traumatic diaphragmatic hernias occur in less than 50% of patients with diaphragmatic injuries [2]. The incidence of traumatic diaphragmatic rupture (leading to hernia) is rising because of the increasing number of road traffic accidents, together with better prehospital and hospital resuscitation of severely injured patients and improved diagnostic facilities.
A high index of suspicion is needed to diagnose traumatic diaphragmatic hernias, failing which results in delayed presentation with life-threatening complications.
Here, we report a review of our experience with traumatic diaphragmatic hernias.
Methods
This study is a review of 60 patients with traumatic diaphragmatic hernia, who underwent surgery at Shanthabai Devarao Shivaram (SDS) Tuberculosis Research Centre and Rajiv Gandhi Institute of Chest Diseases, Bengaluru, India from January 1998 to December 2015. Out of 3478 patients treated for thoracic trauma at our center during this period, 60 (1.72%) patients underwent surgery for diaphragmatic hernias.
After obtaining ethical clearance from the Hospital Committee, the following data were collected and analyzed: age, sex, presenting symptoms, clinical evaluation, diagnostic evaluation [chest X-ray, computerized tomogram (CT) thorax, ultrasound (USG) abdomen, and CT abdomen when indicated], operative approach, intraoperative findings, postoperative course and outcomes, and the hospital stay.
All patients underwent surgical repair of diaphragmatic rupture (hernia) following the diagnosis. Thoracotomy was the preferred method in the absence of associated abdominal injuries. Associated abdominal injuries as diagnosed the clinical examination, USG abdomen, and CT abdomen warranted laparotomy/thoracoabdominal approach. The diaphragmatic defect was amenable to direct closure after reduction of herniated contents using interrupted polypropylene sutures in all patients.
Results
Out of 3478 patients treated for thoracic trauma at our center during this period, 60 (1.72%) patients underwent surgery for traumatic diaphragmatic hernias. There were 48 (80%) males and 12 (20%) females. Age ranged between 10 and 80 years.
Mode of presentation was as follows: blunt trauma was the cause in 52 (86.67%) patients and penetrating trauma in 8 (13.33%) patients. Blunt injuries included 42 cases of road traffic accidents, 8 cases with history of fall and 2 cases of pedestrian hit by motor vehicles. Penetrating injuries included five stab injuries, two bullgore injuries and one gunshot injury. The left-sided rupture was seen in 50 (83.33%) cases and the right-sided rupture in 10 (16.67%) cases.
The presenting symptoms are summarized in Table 1.On clinical evaluation, reduced breath sounds were present in 48 (80%) cases and in 8 (13.33%) cases auscultation revealed bowel sounds in the thoracic cavity.
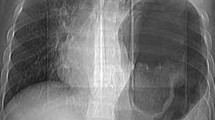
Forty-five (75%) patients were diagnosed to have traumatic diaphragmatic hernia within 24 h of injury. Out of 15 (25%) patients diagnosed after 24 h (25 h to 2 years), 8 patients were asymptomatic at the time of trauma, 5 patients had right-sided diaphragmatic hernia and were missed on initial evaluation, and 2 patients presented late. Among those two patients, one presented after 2 years of initial injury with herniation, gangrene and perforation of the transverse colon with tension fecopneumothorax (Fig. 1).
Chest X-ray was diagnostic in 40 (66.67%) cases, 14 (23.33%) cases needed CT chest for the diagnosis and 6 (10%) cases were diagnosed intraoperatively.
The comparison between the left and the right diaphragmatic hernias with respect to their mode of presentation and the diagnostic modalities are summarized in Table 2.
The associated injuries were present in 41 (68.33%) cases and are summarized in Table 3.
Operative
Thoracotomy was the preferred approach in the absence of abdominal injuries. The laparotomy was done in 10 patients with associated abdominal injuries. The thoracoabdominal approach was used in one patient.
The most common site of rupture was the central tendon seen in 42 (70%) patients, muscular part in 10 (16.67%) patients and the combined muscular and tendinous portion in 8 (13.33%) patients. The length of the diaphragmatic tear ranged from 6 to 10 cm.
Ten (16.67%) patients required additional procedures. Splenorrhaphy was done in three (5%) patients and the splenectomy in one (1.67%) patient. Suprapubic cystostomy was done in one (1.67%) patient, colostomy in two (3.33%) patients, repair of gastric laceration in two (3.33%) patients and one (1.67%) patient who had presented late required a decortication procedure.
Postoperative
On table extubation was possible in 25 (41.67%) patients. Twelve (20%) patients required elective ventilation ranging from 10 h to 5 days. Reasons for prolonged ventilation were head injury in five (8.33%) cases, hypotension in five (8.33%) cases and extensive lung contusions in two (3.33%) cases.
The postoperative morbidity was seen in 11 (18.33%) patients. The reasons were renal failure in three (5%) cases, wound infection in three (5%) cases, peritoneal abscess in one (1.67%) case, liver failure in one (1.67%) case, respiratory failure in one (1.67%) case and minor sepsis in two (3.33%) cases.
The perioperative mortality was 8.33% (five cases). Three (5%) patients died due to sepsis with multiorgan failure, one (1.67%) patient due to renal failure, and one (1.67%) case due to bacterial peritonitis.
The mean duration of hospital stay was 22 days (range 5–84 days). Recurrent herniation requiring the operation was seen in three (5%) patients.
Discussion
Diaphragmatic injuries were first described in 1541 by Sennertus. Diaphragmatic injuries are quite uncommon and often result from either blunt or penetrating trauma. They can occur in isolation or can be associated with abdominal injuries.
The incidence of diaphragmatic ruptures after thoracoabdominal trauma is 0.8–5% [3], and up to 30% diaphragmatic hernias present late [4]. Incorrect interpretation of the X-ray or only intermittent hernial symptoms is the frequent reason for the incorrect diagnosis [5].
Blunt trauma causes sudden rise in the intraabdominal pressure, which in turn increases the transdiaphragmatic pressure gradient between the abdominal compartment and the thorax causing avulsion of the diaphragm from its points of attachments, resulting in diaphragmatic rupture, hence diaphragmatic hernia [6, 7].
The presentation may be early or delayed. The presenting complaints include nonspecific symptoms such as a new or vague abdominal pain, nausea, vomiting, dyspnea and the shoulder or the chest pain. Some patients may remain symptom-free even at the time of diagnosis [8]. Patients with delayed diaphragmatic herniation frequently present months to years after the initial injury with manifestations of visceral herniation, incarceration, obstruction, ischemia from the strangulation or the perforation. A high index of suspicion, together with the knowledge of the mechanism of trauma is the key factor for the correct diagnosis [9].
Traumatic diaphragmatic hernia is a frequently missed diagnosis and there is commonly a delay between the trauma and the diagnosis [10]. The delay in presentation could be explained by various different hypotheses, which are: delayed rupture of a devitalized diaphragmatic muscle several days after the initial injury [11] or the presence of omentum and the viscera plugging the diaphragmatic defect temporarily, allowing for symptomatic visceral herniation to occur months to years later. Literature search reveal cases of diaphragmatic hernias presenting days to years following the injury [12,13,14]. Symbas et al. observed a delay in diagnosis in 8% of cases of diaphragmatic injury from 18 h to 15 years after the injury [15].
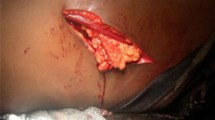
In our study, one patient presented 2 years later following a blunt chest trauma with tension fecopneumothorax secondary to strangulation, gangrene and perforation of the herniated transverse colon (Fig. 2).
Turhan Kutsal et al. [16] and Kalliopi Athanassiadia et al. [17] in their series showed that, about 5–12% patients with diaphragmatic hernias diagnosed after 24 h. In our series, 25% cases were diagnosed after 24 h.
The most common cause of delayed diagnosis was the missed diagnosis at the initial evaluation in our study, which is similar to the reported series [17].
The commonest etiology of diaphragmatic injury was blunt trauma seen in 52 (86.67%) patients in our study; this is compared well with other series [18, 19]. Dyspnea was the most common presenting complaint in our study. The most common presenting symptom described is dyspnea [16].
According to reports, only 17% of the cases with right-sided rupture are diagnosed by the chest X-ray [20]. The diagnosis of right-sided ruptures is difficult; serial chest X-rays and the CT scan are recommended in the diagnosis of right-sided ruptures [21]. One (1.67%) of our patients of right-sided rupture was diagnosed by chest X-ray at the initial evaluation.
Studies have reported approximately 69% of hernias are left sided, 24% are right sided and 15% are bilateral [22, 23].In our study, 50 (83.33%) cases were left-sided and 10 (16.67%) cases were right-sided hernias.
Despite its limitations, chest X-ray still plays a major role in the diagnosis of diaphragmatic injuries [16, 17].
USG chest has been used to diagnose diaphragmatic injuries, especially during the initial evaluation in the emergency department. It is also useful in evaluating associated intraabdominal injuries. USG markers of diaphragmatic injuries include, abnormal diaphragm movement and visualization of a diaphragmatic tear or flap.
But, the appropriate diagnosis depends on the skills of the sonographer and not all hospitals are equipped with in-house sonographers who are comfortable in evaluating the diaphragm. Also, there are no consensuses on criteria for the diagnosis of diaphragmatic rupture by the ultrasound.
With the developments in CT imaging technology, the sensitivity of the CT scan in picking up the diaphragmatic rupture has significantly increased [24]. CT is reported to have a sensitivity of 71% (78% left and 50% right) and a specificity of 100%, and an accuracy of 88% for the left and 70% for the right-sided injuries [25]. The chest and the abdominal CT scans are routinely performed in trauma victims, because chest and abdominal CT scanning is routinely performed in trauma victims, it may provide a more convenient way to detect diaphragmatic injuries. Nchimi et al. [24] has evaluated CT findings of the chest and the upper abdomen, which could be strong predictors of blunt diaphragmatic rupture. These are diaphragmatic discontinuity, diaphragmatic thickening, segmental nonrecognition of the diaphragm, intrathoracic herniation of the abdominal viscera, elevation of the diaphragm and both hemothorax and hemoperitoneum. On the other hand, Iwasaki et al. [26] states that, the inherent anatomical and physiological characteristics of the diaphragm make it difficult to detect abnormalities by means of CT. In summary, CT does not appear to provide significant additional benefit over chest radiographs for the diagnosis of acute diaphragmatic rupture. Tiberio et al. [27] in his series quoted the sensitivity of preoperative chest skiagram and computed tomography to be 86 and 100% respectively in presence of visceral herniation and 14 and 0% respectively in absence of visceral hernia.
Magnetic resonance imaging (MRI) is being used to diagnose diaphragmatic ruptures. Shanmuganathan and colleagues in their study showed that MRI is accurate in the diagnosis of traumatic hernia [28]. In the diagnosis of right-sided ruptures, the use of MRI has also been reported [20]. Although this modality may be highly accurate, it is not currently safe or feasible to bring critically ill trauma patients to the MRI scanner.
Recently, thoracoscopy and laparoscopy have been used to identify traumatic diaphragmatic injuries. Spann and colleagues suggested thoracoscopy and laparotomy to identify diaphragmatic injuries following blunt trauma. Authors concluded that thoracoscopy is as accurate as laparotomy for the identification of these injuries [29]. Other studies have made similar claims about the laparoscopy, but this procedure is not suitable for an unstable trauma patient [30]. Thoracoscopy and laparoscopy probably do not have any benefit in a trauma patient requiring laparotomy, but these procedures may improve our ability to diagnose occult diaphragmatic injuries in clinically stable trauma patients.
Video-assisted thoracoscopic surgery (VATS) and visual inspection of the diaphragm have been described for the diagnosis of diaphragmatic injuries in hemodynamically stable patients [31].
During the initial period, traumatic diaphragmatic injuries were diagnosed based on the clinical examination and the chest X-ray at our center (Government hospital setup) because of the nonavailability of USG and CT abdomen, CT chest, MRI scan, and the economic status of consulting patients. Later on, USG abdomen (CT abdomen if indicated) and the CT chest were included in the diagnostic armentarium. In our study, chest X-ray was diagnostic in 66.67% of patients. CT scan was required for the diagnosis in 23.33% of patients. In 10% cases, the diagnosis was made on table.
Associated injuries were present in 41 (68.33%) patients. The most common associated injury was rib fracture (including scapular fracture), which was present in 18 (43.90%) cases. Rubikas et al. [1] has reported the associated injuries to be present in 86–88% of the cases. Fracture of the chest wall bones was reported to be the most common injury followed by intraabdominal injuries [1].
It is difficult to a draw conclusion concerning the best approach. Given that the majority of patients with blunt or penetrating traumatic diaphragmatic injuries have other intraabdominal injuries, it follows that laparotomy would be the exposure of choice to diagnose and treat all of these injuries. Shah et al. recommend laparotomy as the preferable approach [32]. Niville et al. derived their preference for a laparotomy approach from their patient series [33], thinking that it can easily be extended into the chest if necessary in cases with recent diaphragmatic ruptures.
Despite the overwhelming support for laparotomy, some authors still recommend thoracotomy for repairing traumatic diaphragmatic injuries. McCune et al. and Johnson et al. preferred thoracotomy to repair right-sided diaphragmatic defects [34, 35]. Galan et al. reviewed 1696 patients who suffered blunt thoracic trauma and found 40 patients with diaphragmatic injuries requiring immediate repair; the preferred approach was thoracotomy in the absence of intraabdominal injuries [36]. Tsuda et al. also has considered the abdominal approach at the surgery, only in presence of associated injuries to intraabdominal organs [37].
In cases of delayed presentation, thoracotomy is an accepted approach [31] as it is difficult to release the intrathoracic adhesions through a laparotomy. In acute presentations, the recommended approach is a laparotomy [38] to explore intraabdominal organs for associated injuries.
In our study, thoracotomy was the preferred approach in the absence of intraabdominal injuries. We have found it is easier to reduce the herniated contents and repair the diaphragm through a thoracotomy when there are no intraabdominal injuries. We were able to explore the large bowel through the diaphragmatic defect and carry out the repair of colonic perforation. We were even able to achieve hemostasis by packing small liver lacerations. This has an advantage of reducing the morbidity associated with laparotomy.
In our study, laparotomy was done in 10 (16.67%) cases and thoracoabdominal incision was used in 1 (1.67%) patient.
The mortality was 8.33% in our study, which is comparable with the reported mortality of 1–28% [39, 40].
Conclusion
Diaphragmatic injuries are more common after blunt trauma chest. Dyspnea is the most common mode of presentation. Some patients may be asymptomatic during the initial period after the trauma and present late with life-threatening complications; hence, a high index of suspicion is needed to reduce the mortality and the morbidity. Inspite of all different imaging modalities available today, X-ray chest is still very useful in the diagnosis of diaphragmatic ruptures. Right-sided ruptures are easily missed on the chest X-ray; hence, CT scan and even MRI can be considered in patients with suspected right-sided ruptures.
References
Rubikas R. Diaphragmatic injuries. Eur J Cardio-thorac Surg. 2001;20:53–7.
Hanna Wael C, Ferri Lorenzo E, Fata P, Razek T, Mulder DS. The current status of traumatic diaphragmatic injury: Lessons learned from 105 patients over 13 years. Ann Thorac Surg. 2008;85:1044–8.
Rossetti G, Brusciano L, Maffetone V, et al. Giant right post-traumatic diaphragmatic hernia: laparoscopic repair without a mesh. Chir Ital. 2005;57:243–6.
Pappas-Gogos G, Karfis E, Kakadellis J, Tsimoyiannis EC. Intrathoracic cancer of the splenic flexure. Hernia. 2007;11:257–9.
DeBlasio R, Maione P, Avallone U, Rossi M, Pigna F, Napolitano C. Late posttraumatic diaphragmatic hernia. A clinical case report. Minerva Chir. 1994;49:481–7.
Sangster G, Ventura VP, Carbo A, Gates T, Garayburu J, D'Agostino H. Diaphragmatic rupture: a frequently missed injury in blunt thoracoabdominal trauma patients. Emerg Radiol. 2007;13:225–30.
Walchalk LR, Stanfield SC. Delayed Presentation of Traumatic Diaphragmatic Rupture. J Emerg Med. 2010;39:21–4.
Kulstad EB, Pisano MV, Shirakbari AA. Delayed presentation of traumatic diaphragmatic hernia. J Emerg Med. 2003;24:455–7.
Mintz Y, Easter DW, Izhar U, Edden Y, Talamini MA, Rivkind AI. Minimally invasive procedures for diagnosis of traumatic right diaphragmatic tears: a method for correct diagnosis in selected patients. Am Surg. 2007;73:388–92.
Faul JL. Diaphragmatic rupture presenting forty years after injury. Injury. 1998;29:479–80.
Goh BK, Wong AS, Tay KH, Hoe MN. Delayed presentation of a patient with a ruptured diaphragm complicated by gastric incarceration and perforation after apparently minor blunt trauma. Canadian J Emer Med. 2004;6:277–80.
Sirbu H, Busch T, Spillner J, Schachtrupp A, Autschbach R. Late bilateral diaphragmatic rupture: challenging diagnostic and surgical repair. Hernia. 2005;9:90–2.
Al-Mashat F, Sibiany A, Kensarah A, Eibany K. Delayed presentation of traumatic diaphragmatic rupture. Indian J Chest Dis Allied Sci. 2002;44:121–4.
Singh S, Kalan MM, Moreyra CE, Buckman RF Jr. Diaphragmatic rupture presenting 50 years after the traumatic event. J Trauma. 2000;49:156–9.
Symbas PN, Vlasis SE, Hatcher C Jr. Blunt and penetrating diaphragmatic injuries with or without herniation of organs into the chest. Ann Thorac Surg. 1986;42:158–62.
Turhan K, Makay O, Cakan A, et al. Traumatic diaphragmatic rupture: look to see. Eur J Cardiothorac Surg. 2008;33:1082–5.
Athanassiadi K, Kalavrouziotis G, Athanassiou M, Vernikosc P, Skrekasd G, Poultsidie A. Blunt diaphragmatic rupture. Eur J Cardiothorac Surg. 1999;15:469–74.
Kucuk HF, Demirhan R, Kurt N, Ozyurt Y, Topaloğlu I, Gülmen M. Traumatic diaphragmatic rupture: analysis of 48 cases. Ulus Travma Derg. 2002;8:94–7.
Gelman R, Mirvis SE, Gens D. Diaphragmatic rupture due to blunt trauma: sensitivity of plain chest radiographs. AJR Am J Roentgenol. 1991;156:51–7.
Shanmuganathan K, Mirvis SE. Imaging diagnosis of nonaortic thoracic injury. Radiol Clin North Am. 1999;37:533–51.
Ala-Kulju K, Verkkala K, Ketonen P, Harjola P-T. Traumatic rupture of the right hemidiaphragm. Stand J Thorac Cardiovasc Surg. 1986;20:109–14.
Kuhlman JE, Pozniak MA, Collins J, Knisely BL. Radiographic and CT findings of blunt chest trauma: Aortic injuries and looking beyond them. Radiographics. 1998;18:1085–106.
Feliciano DV, Cruse PA, Mattox KL, et al. Delayed diagnosis of injuries to the diaphragm after penetrating wounds. J Trauma. 1988;28:1135–44.
Nchimi A, Szapiro D, Ghaye B, et al. Helical CT of blunt diaphragmatic rupture. AJR Am J Roentgenol. 2005;184:24–30.
Dosios T, Papachristos IC, Chrysicopoulos H. Magnetic resonance imaging of blunt traumatic rupture of the right hemidiaphragm. Eur J Cardio-thorac Surg. 1993;7:553–4.
Iwasaki M, Inoue H. Traumatic injuries of the diaphragm. Kyobu Geka. 2004;57:795–9.
Tiberio GA, Portolani N, Coniglio A, Baiocchi GL, Vettoretto N, Giulini SM. Traumatic lesions of the diaphragm. Our experience in 33 cases and review of the literature. Acta Chir Belg. 2005;105:82–8.
Shanmuganathan K, Mirvis SE, White CS, Pomerantz SM. MR imaging evaluation of hemidiaphragms in acute blunt trauma: experience with 16 patients. AJR Am J Roentgenol. 1996;167:397–402.
Spann JC, Nwariaku FE, Wait M. Evaluation of video-assisted thoracoscopic surgery in the diagnosis of diaphragmatic injuries. Am J Surg. 1995;170:628–30.
Matz A, Alis M, Charuzi I, Kyzer S. The role of laparoscopy in the diagnosis and treatment of missed diaphragmatic rupture. Surg Endosc. 2000;14:537–9.
Ben-Nun A, Orlovsky M, Best LA. Video-assisted thoracoscopic surgery in the treatment of chest trauma: Long-term benefit. Ann Thorac Surg. 2007;83:383–7.
Shah R, Sabanathan S, Mearns AJ, Choudhury AK. Traumatic rupture of diaphragm. Ann Thorac Surg. 1995;60:1444–9.
Niville EC, Himpens JM, Bruos PL, Gruwez JA. The use of laparotomy in the treatment of recent diaphragmatic rupture due to blunt trauma. Injury. 1983;15:153–5.
McCune RP, Roda CP, Eckert C. Rupture of the diaphragm caused by blunt trauma. J Trauma. 1976;16:531–7.
Johnson CD. Blunt injuries of the diaphragm. Br J Surg. 1988;75:226–30.
Galan G, Penalver JC, Paris F, et al. Blunt chest injuries in 1696 patients. Eur J Cardiothorac Surg. 1992;6:284–7.
Tsuda M, Ichiki K, Doki Y, Yamashita S, Misaki T, Sugiyama S. Thoracic surgical approach for traumatic diaphragmatic hernia. Kyobu Geka. 2004;57:949–52.
Naumheim KS. Adult presentation of unusual diaphragmatic hernias. Chest Surg Clin North Am. 1998;8:359–69.
Haciibrahimoglu G, Solak O, Olcmen A, Berinhan MA, Solmazer N, Gurses A. Management of traumatic diaphragmatic rupture. Surg Today. 2004;34:111–4.
Esme H, Solak O, Sahin DA, Sezer M. Blunt and penetrating traumatic ruptures of the diaphragm. Thorac Cardiovasc Surg. 2006;54:324–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
None.
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Haranal, M.Y., Buggi, S., Sanjeevaiah, S. et al. Traumatic diaphragmatic hernia—17 years experience. Indian J Thorac Cardiovasc Surg 34, 38–43 (2018). https://doi.org/10.1007/s12055-017-0534-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12055-017-0534-x