Abstract
IL-3, a haematopoiesis regulatory factor, has previously been shown to inhibit both mouse and human osteoclast differentiation and bone resorption. Here, the role of rat IL-3 on rat osteoclast differentiation was evaluated to address whether the inhibitory action of IL-3 on osteoclastogenesis is conserved in various species. It was observed that IL-3 inhibited rat osteoclast differentiation induced by both TNF-α and receptor activator of NF-κB ligand (RANKL). TNF-α is known to induce bone loss in postmenopausal osteoporotic women and it also synergise with many pro-osteoclastogenic cytokines to cause huge pathological bone loss. Importantly, it was found that rat IL-3 inhibits the synergistic action of TNF-α with RANKL and IL-1β, TGF-β1 and TGF-β3. IL-3 downregulates the TNF-α-induced nuclear translocation of NF-κB-p65 and c-fos without affecting c-jun. Interestingly, we observed that IL-3 also inhibits osteoclast differentiation in vivo in rats induced by TNF-α. All these results suggest that inhibitory action of IL-3 on osteoclastogenesis is conserved in various species including mice, rats and humans. Thus, our results clearly indicate that IL-3 has therapeutic potential to treat pathological bone loss in important skeletal diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Osteoclasts are multinuclear cells which differentiate from haematopoietic precursors of monocyte/macrophage lineage (Akagawa et al. 1996). Bone loss by increased osteoclast activity is a key pathological feature in important skeletal diseases including osteoporosis and rheumatoid arthritis (Abu-Amer 2009). Osteoclastogenesis is induced by receptor activator of NF-κB ligand (RANKL) secreted by osteoblasts (Weitzmann and Pacifici 2006). Osteoclastogenesis and bone homeostasis is also regulated by immune cell-derived cytokines including IL-1, IL-6, TNF-α and TGF-β (Roggia et al. 2001; Ritchlin et al. 2003; Braun and Zuerina 2011; Walsh et al. 2018). TNF-α plays an important role in inducing osteoclastogenesis in osteoporosis and rheumatoid arthritis (Pfeilschifter et al. 2002). Both RANKL and TNF-α independently or synergistically show a profound effect on pathological bone resorption (Lam et al. 2000).
IL-3 is a pleiotropic cytokine secreted by the cells of haematopoietic origin and it is also required for their survival, proliferation and differentiation (Saeland et al. 1988; Sonada et al. 1988; Lantz et al. 1998). The role of IL-3 in bone homeostasis has recently been investigated. We have earlier documented that IL-3 inhibits RANKL-induced osteoclast differentiation by downregulating NF-κB (Khapli et al. 2003) and inhibits TNF-α-induced osteoclast differentiation by downregulating TNF-receptors 1 and 2 (Yogesha et al. 2005). IL-3 also inhibits RANKL-induced human osteoclast differentiation in human peripheral blood monocytes (Gupta et al. 2010). Recently, other groups have also documented the anti-osteoclastic action of IL-3 (Hong et al. 2013; Hirose et al. 2014; Lee et al. 2016).
Cytokines function differently on bone cells depending on the species used for the study. IL-7 have anti-osteoclastic activity in mouse cells (Lee et al. 2003), however, it is pro-osteoclastogenic in human cells (Weitzmann et al. 2000). Similarly, TNF-α inhibits osteoblast differentiation of mouse mesenchymal stem cells (MSCs), while it enhances osteoblast differentiation of human MSCs (Osta et al. 2014). Different species metabolise a given drug differently and exhibit variation in their responses (Martignoni et al. 2006). The extrapolation of animal data to the human application is possible if a drug is tested for its activity in different species. Consequently, a conserved action of a drug in different species makes it more suitable for human clinical trials. Since IL-3 showed anti-osteoclastic role in mouse and human cells, it is necessary to test the anti-osteoclastic potential of IL-3 in different species. Ovariectomy-induced pathological bone loss in rats is closer to human postmenopausal osteoporosis (Turner 2001). Therefore, in the present study we evaluated whether the anti-osteoclastic action of rat IL-3 is conserved in rats.
The effect of rat IL-3 on rat osteoclast differentiation and function was evaluated with emphasis mainly on TNF-α-induced osteoclast differentiation, which is the key factor in inducing pathological bone loss in vivo. We observed that IL-3 inhibits both TNF-α and RANKL-induced osteoclast differentiation and also their synergistic action with other pro-osteoclastogenic cytokines. IL-3 inhibits rat osteoclast differentiation by inhibiting NF-κB and AP-1 pathways. Moreover, IL-3 inhibits TNF-α-induced osteoclastogenesis in vivo. Thus, we show for the first time that the anti-osteoclastic action of IL-3 is conserved in mice, rats and humans.
2 Materials and methods
2.1 Animals
Wistar rats of 3 months old obtained from National Centre for Cell Science, Pune, India were used for isolation of osteoclast precursors and in vivo studies. All animal experiments were approved by Institutional Animal Ethics Committee (IAEC/2016/B-277).
2.2 Reagents
Recombinant rat TNF-α, IL-1β, TGF-β1, TGF-β3 and anti-IL-3 neutralizing antibody were purchased from R & D Systems. Recombinant murine macrophage colony-stimulating factor (M-CSF), RANKL, and rat IL-3 were purchased from Peprotech Asia. Anti-p-NF-κB-p65 antibody was obtained from Santa Cruz Biotechnology. Polyclonal antibodies for c-fos and c-jun were obtained from Cell Signalling Technology. Secondary FITC labelled antibody was obtained from Bangalore Genei. TRIzol reagent, cDNA synthesis kit and SYBR Green were purchased from Invitrogen. Minimal essential medium-alpha modification (α-MEM) and para-nitrophenyl phosphate were obtained from Sigma-Aldrich.
2.3 Osteoclast differentiation
Osteoclast precursors were isolated from rats by method as described earlier for mice (Yogesha et al. 2005). Briefly, femora and tibiae were harvested and bone ends were cut to flush the marrow cavity using α-MEM. A single-cell suspension was made by vigorously agitating bone marrow suspension. Cells were washed, resuspended at 3×105 cells/ml in α-MEM containing 10% FBS and M-CSF (10 ng/ml). After 24 h, non-adherent cells were collected, washed and resuspended in α-MEM and layered on Ficoll-Hypaque. The cells were centrifuged and buffy coat formed at the interface of the gradient was collected and 5×104 cells/well were plated in 96-well culture plate. Cells were incubated with M-CSF (30 ng/ml) and RANKL (30 ng/ml) or TNF-α (40 ng/ml) with various concentrations of rat IL-3. Anti-IL-3 neutralising antibody was also used according to the experimental strategy. To study the synergistic action of TNF-α with other pro-osteoclastogenic cytokines, cells were incubated with M-CSF and TNF-α in presence of either IL-1β or TGF-β1 or TGF-β3 (5 ng/ml each) and rat IL-3. On day 3 cultures were half fed by replacing 100 µl of culture medium with fresh medium. After 4 days cells were fixed with formalin and stained for tartrate-resistant acid phosphatase (TRAP). TRAP+ multinuclear cells (MNCs) were counted.
2.4 Quantitative TRAP assay
Cells were fixed with 10% formalin, washed and dried. The cells were then treated with 100 µl of 5 mM para-nitrophenyl phosphate in 50 mM citrate buffer for 1 h at 37°C. The reaction was terminated by adding 100 µl of 1N NaOH and absorbance was read at 415 nm.
2.5 Bone resorption assay
Bone slices were bleached in 4% sodium hypochlorite for 15 minutes, washed, dried and mounted onto glass slides, and then sputter coated with gold (K550X Sputter Coater). Bone slices were observed under reflected light microscopy and percent bone resorption was quantitated.
2.6 RNA Isolation, RT-PCR and qPCR
RNA was isolated using TRIzol method and cDNA was synthesized using Thermoscript RT. RT-PCR was performed for 30 cycles and each cycle consists of 30 s of denaturation at 94°C, 30 s of annealing at 58°C, and 30 s of extension at 72°C followed by final extension for 2 min. qPCR was set up with reaction mixture containing SYBR green and 10 pmol of each primer (IDT) and analysed using StepOnePlus system (Applied Biosystems). Reaction was performed for 40 cycles with each cycle of 30 s of denaturation at 94°C, 30 s of annealing at 58°C and 30 s of extension at 72°C, followed by melt curve at the end. GAPDH was used as endogenous control.
Primer sequences used were: TRAP, 5′- ACCTTGGCAATGTCTCGGCACAAA-3′ (sense), 5′-AATTGCCACACAGCATCACGGT-3′(antisense); cathepsin K, 5′-TGACGAAAACTGCGACCGTGAT-3′(sense), 5′-TTTGTTTCCCCAGCTTTCTCCCCA-3′(antisense); integrin β3, 5′-ACTTGGCAAAAACGCGGTGAACT-3′ (sense), 5′-AGAGTAGCAAGGCCAATGAGCAGA-3′(antisense); CTR, 5′-TGCTCTGATTGCTTCCATGGGGAT-3′(sense), 5′-TGCAACTTATAGGATCCCGTCGCA-3′ (antisense); GAPDH, 5′-TGATGGGTGTGAACCACGAG-3′(sense), 5′-CCCTTCCACGATGCCAAAGT-3′(antisense). Real-time analysis was done by comparative CT method and fold change was calculated by 2-ΔΔCT method.
2.7 Immunofluorescence microscopy
Cells were fixed with 3.7% paraformaldehyde for 10 min and permeabilised using Triton X-100 (0.1%) for 5 min. Cells were incubated with primary antibody against p-NF-κB-p65 or c-fos or c-jun for 2 h, washed and treated with FITC-conjugated secondary antibody and 4’,6-diamidino-2-phenylindole (1 μg/ml) for 1 h. Cells were washed, mounted on slides using FragEL mounting medium (Oncogene) and images were acquired at 63×magnification using Zeiss LSM 510 Confocal microscope.
2.8 In vivo studies
To evaluate the anti-osteoclastic potential of rat IL-3 in vivo, Wistar rats were randomly divided into four groups and injected subcutaneously over the calvaria with PBS or TNF-α (1 μg/day) or TNF-α + IL-3 (1 μg/day) or IL-3 alone for 5 consecutive days. All the rats were sacrificed 4 days after the last injection and calvariae were dissected free of soft tissues. Total RNA was isolated from each calvarium and mature osteoclasts markers were analysed by real-time PCR.
2.9 Statistical analysis
The results are presented as mean ± SEM. Statistical significance was calculated using one way ANOVA followed by Bonferroni’s correction for multiple comparisons. p < 0.05 was taken as statistically significant value.
3 Results
3.1 IL-3 inhibits TNF-α-induced rat osteoclastogenesis
TNF-α is known to induce osteoclast differentiation independent of RANKL (Zhao et al. 2012). Its level also increases in postmenopausal osteoporosis and inflammatory arthritis (Osta et al. 2014). Therefore, to evaluate the effect of rat IL-3 on TNF-α-induced rat osteoclastogenesis we incubated bone marrow-derived osteoclast precursors in 96-well plate (5×104 cells/well) with M-CSF (30 ng/ml) and TNF-α (40 ng/ml) with various concentrations of IL-3. After 4 days TRAP+ MNCs were counted. We observed that IL-3 significantly inhibited rat osteoclast differentiation in a dose-dependent manner (figure 1A). Photomicrographs in figure 1B show the inhibitory action of IL-3 on osteoclasts. To confirm the anti-osteoclastic effect of IL-3, cells were incubated with M-CSF, TNF-α, IL-3 (1 ng/ml) and anti-IL-3 neutralizing antibody (1 μg/ml). Addition of anti-IL-3 antibody restored the number of osteoclasts (figure 1C) and TRAP activity (figure 1D) inhibited by IL-3. IL-3 also downregulated the mRNA expression of osteoclast genes such as TRAP, integrin β3, cathepsin K, and calcitonin receptor (CTR) (figure 1E to H) which were restored by anti-IL-3 antibody. Since RANKL is a physiological differentiation factor for osteoclasts we further evaluated the effect of IL-3 on RANKL-induced osteoclastogenesis by incubating osteoclast precursors with M-CSF and RANKL and different concentrations of rat IL-3. TRAP staining revealed that IL-3 dose-dependently inhibited osteoclast formation (figure 2A and B) and TRAP activity (figure 2C). The expression of osteoclast genes was also downregulated by IL-3 (figure 2D). These results indicate that IL-3 inhibits rat osteoclastogenesis induced by both TNF-α and RANKL.
IL-3 inhibits TNF-α-induced rat osteoclast differentiation. (A) M-CSF-dependent osteoclast precursors were plated in 96-well plate (5×104 cells/well) and incubated with M-CSF (30 ng/ml), TNF-α (40 ng/ml) and different concentrations of IL-3. After 4 days, cells were stained for TRAP and the number of TRAP+ MNCs was counted. (B) Representative images of osteoclasts in the presence of IL-3 (1 ng/ml) (Magnification, 10X). (C) Osteoclast precursors were incubated for 4 days with M-CSF, TNF-α and IL-3 (1 ng/ml) with or without anti-IL-3 neutralizing antibody (1 μg/ml). The number of TRAP+ MNCs was counted. (D) TRAP activity was measured colorimetrically at 415 nm. Osteoclast markers like TRAP (E), integrin β3 (F), cathepsin K (G) and CTR (H) were analysed by real-time PCR. Data in A, C and D is presented as the mean ± SEM of six replicates per group and is a representative of three independent experiments. Data in E, F and H is representative of two independent experiments and (G) representative of three independent experiments. M, M-CSF; MT, M-CSF and TNF-α. #p < 0.05; ##p < 0.01; ####p < 0.0001 vs. M; *p < 0.05; **p < 0.01; ****p < 0.0001 vs. MT; $p < 0.05; $$$$p < 0.0001 vs. MT+IL-3.
Effect of IL-3 on RANKL-induced rat osteoclast differentiation in vitro. (A) Bone marrow derived M-CSF-dependent osteoclast precursors were plated at a density of 5×104 cells/well in 96-well plate and incubated with M-CSF (30 ng/ml) and RANKL (30 ng/ml) in the absence or presence of different concentrations of IL-3 for 4 days . Cells were fixed and stained for TRAP and the number of TRAP+ MNCs was counted. (B) Representative microscopic images of TRAP+ cells in the presence of IL-3 (1 ng/ml) (Magnification, 10 X). (C) TRAP activity was measured colorimetrically at 415 nm. (D) RT-PCR shows the expression of osteoclast specific markers such as TRAP, cathepsin K and integrin β3. IL-3 used was 1 ng/ml. NTC, No Template Control. Data (A and C) are represented as the mean ± SEM of six replicates per group. M, M-CSF; R, RANKL. Similar results were observed in two independent experiments. ####p < 0.0001 vs. M-CSF; **p < 0.01; ***p < 0.001; ****p < 0.0001 vs. M-CSF and RANKL.
3.2 IL-3 inhibits the synergistic effect of TNF-α and RANKL on osteoclastogenesis
TNF-α synergise with RANKL and enhances osteoclastogenesis in vivo in disorders associated with bone loss (Lam et al. 2000). To evaluate the role of rat IL-3 on the synergistic action of TNF-α and RANKL on rat osteoclast differentiation, cells were incubated with M-CSF and sub-optimal concentrations of TNF-α (10 ng/ml) and RANKL (5 ng/ml) in presence of IL-3 (1 ng/ml). It was observed that the sub-optimal concentrations of TNF-α and RANKL alone were inefficient in inducing osteoclast formation, however, both cytokines together showed strong synergism and augmented mature osteoclast formation. Interestingly, IL-3 inhibited the synergistic effect of TNF-α and RANKL on osteoclastogenesis (figure 3A). The expression level of osteoclast genes were also downregulated by IL-3 (figure 3B to 3E). These results indicate that IL-3 has potent inhibitory action on rat osteoclastogenesis.
IL-3 inhibits the synergistic action of TNF-α and RANKL on rat osteoclast differentiation and bone resorption. (A) Osteoclast precursors were plated in 96-well plate (5×104 cells/well) and incubated with M-CSF and TNF-α (10 ng/ml) or RANKL (5 ng/ml) or both with or without IL-3 (1 ng/ml). Cells were stained for TRAP and the number of TRAP+ MNCs was counted. Osteoclast markers such as TRAP, (B) integrin β3 (C), cathepsin K (D), and CTR (E) were analysed by real-time PCR. (F) Osteoclast precursors (5×104 cells/well) were cultured on bone slices for 12 days with M-CSF and TNF-α or RANKL or both with IL-3 (10 ng/ml). The bone slices were washed, bleached and sputter coated with gold and percent bone resorption was calculated. (G) Microscopic images of bone resorption (Magnification, 10X). Data are presented as mean ± SEM of three (A and F), four (B) and two (C, D and E) experiments. M, M-CSF; MT, M-CSF and TNF-α; MR, M-CSF and RANKL; MTR, M-CSF, TNF-α and RANKL. #p < 0.05; ##p < 0.01; ###p < 0.001; ####p < 0.0001 vs. MT or MR; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001 vs. MTR.
In many bone disorders, not only osteoclast differentiation but activity of mature osteoclast is increased. Therefore, the role of rat IL-3 was assessed on bone resorption by osteoclasts. Cells were cultured on bone slices with M-CSF and sub-optimal concentrations of TNF-α and RANKL as described above in presence of IL-3 for 12 days. The bone slices were processed for evaluation of resorption pits. TNF-α and RANKL independently do not resorb bone at sub-optimal concentrations, however, together synergise to induce bone resorption. Interestingly, IL-3 inhibited bone resorption induced by synergistic action of TNF-α and RANKL (figure 3F). Photomicrographs in figure 3G show significant inhibition of bone resorption by IL-3. These results indicate that IL-3 inhibits synergistic action of TNF-α and RANKL on both osteoclastogenesis and bone resorption.
3.3 IL-3 inhibits osteoclastogenesis induced by synergistic action of TNF-α with different cytokines
Under normal physiological conditions RANKL is needed for osteoclastogenesis but in pathological conditions other cytokines play an important role in enhancing osteoclastogenesis and bone resorption. These cytokines include IL-1, IL-6 and TGFs which synergise with RANKL or TNF-α and augment osteoclastogenesis (Pfeilschifter et al. 2002). Therefore, we further evaluated the effect of IL-3 on rat osteoclastogenesis induced by synergistic action of TNF-α and IL-1β or TGF-β1 or TGF-β3. Cells were incubated with M-CSF and TNF-α (10 ng/ml) with or without IL-1β or TGF-β1 or TGF-β3 (5 ng/ml each) in presence of IL-3 (10 ng/ml) with or without anti-IL-3 antibody (1 μg/ml). We observed that these cytokines synergise with TNF-α to induce osteoclast differentiation. The synergistic action of these cytokines was inhibited by IL-3 and anti-IL-3 antibody restored both osteoclasts and TRAP activity (figure 4A and 4B). All these results indicate that rat IL-3 is a potent anti-osteoclastic molecule and inhibit osteoclastogenesis even in the presence of several pro-osteoclastogenic cytokines.
Effect of IL-3 on TNF-α-induced osteoclast differentiation in presence of pro-osteoclastogenic cytokines. (A) Osteoclast precursors were plated at a density of 5×104 cells/well in 96-well plate and incubated with M-CSF (30 ng/ml) and TNF-α (10 ng/ml) in the absence or presence IL-1β (5 ng/ml) or TGF-β1 (5 ng/ml) or TGF-β3 (5 ng/ml) without or with IL-3 (1 ng/ml) for 4 days. Anti-IL-3 Ab (1 μg/ml) was also added. Cells were fixed, stained for TRAP and the number of TRAP+ MNCs was counted. (B) TRAP activity was measured colorimetrically at 415 nm. Data is represented as the mean ± SEM of three to six cultures per group. Data (A) and (B) are representative of three and two independent experiments respectively. ###p < 0.001; ####p < 0.0001 vs. M-CSF and TNF-α; ***p < 0.001; ****p < 0.0001 vs. M-CSF, TNF-α and IL-1β/TGF-β1/TGF-β3; $p < 0.05; $$p < 0.001; $$$$p < 0.0001 vs. IL-3.
3.4 IL-3 inhibits TNF-α-induced phosphorylation and nuclear translocation of p-NF-κB p65
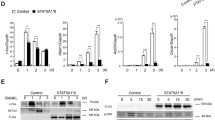
TNF-α induce osteoclast formation by activation of NF-κB and AP-1 transcription factors (Wang et al. 1992; Wagner and Eferl 2005; Boyce et al. 2015). To understand the molecular mechanism(s) for inhibitory action of rat IL-3 on TNF-α-induced osteoclastogenesis, cells were cultured with M-CSF and IL-3 (1 ng/ml), and TNF-α (10 ng/ml) was added on day 3 and cells were further incubated for 30 min. We found that IL-3 inhibited TNF-α-induced phosphorylation and nuclear translocation of p-NF-κB p65 (figure 5A). The nuclear translocation of c-fos but not c-jun was also inhibited by IL-3 (figure 5B). These observations indicated that IL-3 downregulates TNF-α-induced activation of p-65 and c-fos to inhibit osteoclast differentiation.
Effect of IL-3 on nuclear translocation of NF-κB p65 and c-fos. Osteoclast precursors were plated on glass coverslips in 24-well plate (4 × 104 cells/well) and incubated with M-CSF and IL-3 (10 ng/ml). On day 3, TNF-α (40 ng/ml) was added to the cultures and cells were further incubated for 30 min. Cells were fixed, permeabilized, and nuclear translocation of p-NF-κB p65 (A), c-fos and c-jun (B) were examined by immunofluorescence (Magnification, 63X). Data are representative of two independent experiments.
3.5 IL-3 inhibits TNF-α-induced osteoclastogenesis in vivo
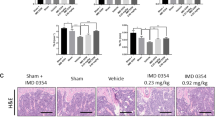
TNF-α is known to induce osteoclast differentiation in vivo (Yoshimatsu et al. 2009; Morita et al. 2010). To validate our in vitro observations, investigational animal model was exploited for studying the role of rat IL-3 on osteoclastogenesis in vivo. Wistar rats were injected subcutaneously over calvaria with TNF-α (1 μg/day) or IL-3 (1 μg/day) alone or in combination for 5 consecutive days. Rats were sacrificed 4 days after the last injection and calvariae were excised for RNA isolation and analysis of mature osteoclasts genes. It was observed that TNF-α increases the expression of TRAP, integrin β3, cathepsin K and CTR (figure 6A-6D). Interestingly, the expression levels of these genes were significantly decreased by IL-3. IL-3 alone had no effect on the osteoclastogenesis in vivo. Thus, our results indicate that rat IL-3 inhibits TNF-α-induced osteoclastogenesis under both in vitro and in vivo conditions in rats.
Effect of IL-3 on osteoclast differentiation in vivo in rats. Wistar rats were divided into four groups and injected subcutaneously over the calvariae with the PBS or TNF-α (1.0 μg/day) or IL-3 (1 μg/day) alone or TNF-α and IL-3 together for five days. The rats were sacrificed four days after the last injection (day 9) and calvariae were harvested and analysed for the expression of TRAP (A), integrin β3 (B), cathepsin K (C), and CTR (D) by real-time PCR. Results are represented as mean ± SEM with n = 5-9 rats in each group. #p < 0.05; ##p < 0.01 vs. PBS; *p < 0.05; **p < 0.01 vs. TNF-α.
4 Discussion
Osteoclasts are bone resorbing cells which helps in maintaining bone homeostasis. Increased differentiation and activity of osteoclasts are main causes of pathological bone loss in skeletal diseases including osteoporosis, arthritis and bone metastases (Eriksen et al. 1990; Hirayama 2002; Raisz 2005; Guise 2009; Nakajima et al. 2016). Therefore, the inhibition of osteoclastogenesis and bone resorption is necessary to control pathological bone loss. IL-3 has long been known to play an important role in haematopoiesis. We have documented that IL-3 has an important role in regulation of pathophysiology of bone and cartilage remodeling. IL-3 inhibits RANKL and TNF-α-induced osteoclastogenesis and diverts the cells toward macrophages and dendritic cells in mice and humans respectively (Khapli et al. 2003; Yogesha et al. 2005; Gupta et al. 2010). IL-3 also prevents bone loss in mouse inflammatory arthritis (Yogesha et al. 2009) and protects degeneration of both cartilage and subchondral bone in mouse osteoarthritis (Kour et al. 2016). These studies indicate that IL-3 has a crucial role in prevention of pathological bone and cartilage loss in important skeletal disorders.
The differentiation of osteoclasts and osteoblasts is regulated by various cytokines and their inhibitory or stimulatory effects depend on the species. IL-7 is reported as anti-osteoclastic in mice and pro-osteoclastic in humans (Weitzmann et al. 2000; Lee et al. 2003). TNF-α inhibits osteoblast differentiation of mouse MSCs and enhances osteoblast differentiation of human MSCs. The action of TNF-α on osteogenesis is dependent not only on species, but also on its concentration. Since IL-3 showed potent inhibitory action on both mouse and human osteoclastogenesis, we further investigated whether the anti-osteoclastic action of rat IL-3 is conserved in rat. We chose rat model because ovariectomy-induced pathological bone loss in rats is closer to bone loss in human postmenopausal osteoporosis (Turner 2001). Moreover, both rat and human bones not only show similar responses to estrogen deficiency but they are also resistant to anabolic actions of estrogen on bone formation (Abe et al. 1993).
We observed that rat IL-3 inhibits both RANKL- and TNF-α-induced rat osteoclast differentiations and 0.001 ng/ml of IL-3 was sufficient for significant inhibition of osteoclast differentiation. The inhibitory effect of IL-3 was neutralized by anti-IL-3 antibody which clearly indicate the IL-3 specific action. The expression of osteoclast genes such as TRAP, cathpesin K and integrin β3 was downregulated by IL-3. These results are consistent with our and others previous findings of inhibitory role of IL-3 on mouse and human osteoclast differentiation (Khapli et al. 2003; Yogesha et al. 2005; Hirose et al. 2014; Lee et al. 2016).
IL-3 inhibits RANKL-induced osteoclastogenesis by inhibiting NF-κB pathway and inhibits TNF-α-induced osteoclastogenesis by downregulation of both the TNF receptors (TNFR1 and TNFR2) and inhibition of nuclear translocation of c-fos (Yogesha et al. 2009; Lee et al. 2016). Notably, TNF-α-induced NF-κB pathway in mouse osteoclasts was not affected by IL-3 (Yogesha et al. 2009). In the present study rat IL-3 inhibited TNF-α-induced nuclear translocation of both NF-κB p65 and c-fos. In skeletal diseases bone loss is a result of synergistic action of TNF-α and RANKL on osteoclast differentiation and bone resorption (Azuma et al. 2000). IL-3 inhibited rat osteoclast differentiation induced by the synergism of TNF-α with RANKL. In addition to RANKL, other cytokines like IL-1β, TGF-β1, and TGF-β3 have also been reported to synergise with TNF-α and enhance osteoclastogenesis (Pfeilschifter et al. 2002). IL-3 was able to abrogate the synergistic action of all these cytokines with TNF-α on osteoclastogenesis.
TNF-α also induces osteoclast differentiation in vivo (Yoshimatsu et al. 2009; Morita et al. 2010). To further evaluate the in vivo role of IL-3 on TNF-α-induced osteoclast differentiation, rat IL-3 was injected subcutaneously over calvariae of rats. TNF-α up-regulated the expression of osteoclast specific genes which were significantly downregulated by IL-3. This indicated that IL-3 also inhibits TNF-α-induced osteoclast differentiation in vivo.
Thus, our study is the first of its kind where we have shown that IL-3 is a potent inhibitor of osteoclast differentiation and that the inhibitory action is conserved across the three species mouse, rat and human. Rat IL-3 inhibits both RANKL- and TNF-α-induced rat osteoclast differentiation and bone resorption in presence of several pro-osteoclastogenic cytokines. Interestingly, IL-3 also inhibits osteoclast differentiation in vivo in rats. Thus, our study suggests the potential of IL-3 for prevention of pathological bone loss in important skeletal diseases. We are further investing the role of IL-3 on bone loss in ovariectomized mice and our preliminary results are encouraging, which also suggest the potential of IL-3 in prevention of pathological bone loss (unpublished data).
Abbreviations
- RANKL:
-
Receptor activator of NF-κB ligand
- MSCs:
-
Mesenchymal stem cells
- M-CSF:
-
Macrophage colony-stimulating factor
- α-MEM:
-
Minimal essential medium-alpha modification
- TRAP:
-
Tartrate-resistant acid phosphatase
- MNCs:
-
Multinuclear cells
- CTR:
-
Calcitonin receptor
References
Abe T, Chow JW, Lean JM and Chambers TJ 1993 Estrogen does not restore bone lost after ovariectomy in the rat. J. Bone Mineral Res. 8 831–838
Abu-Amer Y 2009 Inflammation, cancer, and bone loss. Curr. Opin. Pharmacol. 9 427–433
Akagawa KS, Takasuka N, Nozaki Y, et al. 1996 Generation of CD1+RelB+ dendritic cells and tartrate-resistant acid phosphatase-positive osteoclast-like multinucleated giant cells from human monocytes. Blood 88 4029–4039
Azuma Y, Kaji K, Katogi R, Takeshita S and Kudo A 2000 Tumor necrosis factor-α induces differentiation of and bone resorption by osteoclasts. J. Biol. Chem. 275 4858–4864
Boyce BF, Xiu Y, Li J, Xing L and Yao Z 2015 NF-κB-mediated regulation of osteoclastogenesis. Endocrinol. Metab. 30 35–44
Braun T and Zwerina J 2011 Positive regulators of osteoclastogenesis and bone resorption in rheumatoid arthritis. Arthritis Res. R. 13 235
Eriksen EF, Hodgson SF, Eastell R, Cedel SL, O’Fallon WM and Riggs BL 1990 Cancellous bone remodeling in type I (postmenopausal) osteoporosis: quantitative assessment of rates of formation, resorption, and bone loss at tissue and cellular levels. J. Bone Mineral Res. 5 311–319
Guise TA 2009 Breaking down bone: New insight into site-specific mechanisms of breast cancer osteolysis mediated by metalloproteinases. Genes Dev. 23 2117–2123
Gupta N, Barhanpurkar AP, Tomar GB, Srivastava RK, Kour S, Pote ST and Wani MR 2010 IL-3 inhibits human osteoclastogenesis and bone resorption through downregulation of c-Fms and diverts the cells to dendritic cell lineage. J. Immunol. 185 2261–2272
Hirayama T 2002 Osteoclast formation and activity in the pathogenesis of osteoporosis in rheumatoid arthritis. Rheumatology 41 1232–1239
Hirose J, Masuda H, Tokuyama N, et al. 2014 Bone resorption is regulated by cell-autonomous negative feedback loop of Stat5-Dusp axis in the osteoclast. J. Exp. Med. 211 153–163
Hong H, Shi Z, Qiao P, et al. 2013 Interleukin-3 plays dual roles in osteoclastogenesis by promoting the development of osteoclast progenitors but inhibiting the osteoclastogenic process. Biochem. Biophy. Res. Commun. 440 545–550
Khapli SM, Mangashetti LS, Yogesha SD and Wani MR 2003 IL-3 Acts Directly on osteoclast precursors and irreversibly inhibits receptor activator of NF-κB ligand-induced osteoclast differentiation by diverting the cells to macrophage lineage. J. Immunol. 171 142–151
Kour S, Garimella MG, Shiroor DA, Mhaske ST, Joshi SR, Singh K and Wani MR 2016 IL-3 decreases cartilage degeneration by downregulating matrix metalloproteinases and reduces joint destruction in osteoarthritic mice. J. Immunol. 196 5024–5035
Lam J, Takeshita S, Barker JE, Kanagawa O, Ross FP and Teitelbaum SL 2000 TNF-α induces osteoclastogenesis by direct stimulation of macrophages exposed to permissive levels of RANK ligand. J. Clin. Invest. 106 1481–1488
Lantz CS, Boesiger J, Song CH, Mach N, Kobayashi T, Mulligan RC and Galli SJ 1998 Role for interleukin-3 in mast-cell and basophil development and in immunity to parasites. Nature 392 90–93
Lee J, Seong S, Kim JH, et al. 2016 STAT5 is a key transcription factor for IL-3-mediated inhibition of RANKL-induced osteoclastogenesis. Sci. Rep. 6 30977
Lee S-K, Kalinowski JF, Jastrzebski SL, Puddington L and Lorenzo JA 2003 Interleukin-7 is a direct inhibitor of in vitro osteoclastogenesis. Endocrinology 144 3524–3531
Martignoni M, Groothuis GMM and De Kanter R 2006 Species differences between mouse, rat, dog, monkey and human cytochrome P450-mediated drug metabolism. Expert Opin. Drug Metab. Toxicol. 2 875–894
Morita Y, Kitaura H, Yoshimatsu M, Fujimura Y, Kohara H, Eguchi T and Yoshida N 2010 IL-18 inhibits TNF-α-induced osteoclastogenesis possibly via a T cell-independent mechanism in synergy with IL-12 in vivo. Calcified Tissue Int. 86 242–248
Nakajima K, Kho DH, Yanagawa T, et al. 2016 Galectin-3 cleavage alters bone remodeling: different outcomes in breast and prostate cancer skeletal metastasis. Cancer Res. 76 1391–1402
Osta B, Benedetti G and Miossec P 2014 Classical and paradoxical effects of TNF-α on bone homeostasis. Front. Immunol. 5 00048
Pfeilschifter J, Köditz R, Pfohl M and Schatz H 2002 Changes in proinflammatory cytokine activity after menopause. Endocrine Rev. 23 90–119
Raisz LG 2005 Pathogenesis of osteoporosis: Concepts, conflicts, and prospects. J. Clin. Invest. 115 3318–3325
Ritchlin CT, Haas-Smith SA, Li P, Hicks DG and Schwarz EM 2003 Mechanisms of TNF-α- and RANKL-mediated osteoclastogenesis and bone resorption in psoriatic arthritis. J. Clin. Invest. 111 821–831
Roggia C, Gao Y, Cenci S, Weitzmann MN, Toraldo G, Isaia G and Pacifici R 2001 Up-regulation of TNF-producing T cells in the bone marrow: A key mechanism by which estrogen deficiency induces bone loss in vivo. Proc. Nat. Acad. Sci. USA 98 13960–13965
Saeland S, Caux C, Favre C, et al. 1988 Effects of recombinant human interleukin-3 on CD34-enriched normal haematopoietic progenitors and on myeloblastic leukemia cells. Blood 72 1580–1588
Sonoda Y, Yang YC, Wong GG, Clark SC and Ogawa M 1988 Erythroid burst-promoting activity of purified recombinant human GM-CSF and Interleukin-3: Studies with anti-GM-CSF and anti-IL-3 sera and studies in serum free cultures. Blood 72 1381–1386
Turner AS 2001 Animal models of osteoporosis – Necessity and limitations. Eur. Cells Mater. 1 66–81
Wagner EF and Eferl R 2005 Fos/AP-1 proteins in bone and the immune system. Immunol. Rev. 208 126–140
Walsh MC, Takegahara N, Kim H and Choi Y 2018 Updating osteoimmunology: regulation of bone cells by innate and adaptive immunity. Nat. Rev. Rheumatol. 14 146–156
Wang ZQ, Ovitt C, Grigoriadis AE, Möhle-Steinlein U, Rüther U and Wagner EF 1992 Bone and haematopoietic defects in mice lacking c-fos. Nature 360 741–745
Weitzmann MN, Cenci S, Rifas L, Brown C and Pacifici R 2000 Interleukin-7 stimulates osteoclast formation by up-regulating the T-cell production of soluble osteoclastogenic cytokines. Blood 96 1873–1878
Weitzmann MN and Pacifici R 2006 Estrogen deficiency and bone loss: An inflammatory tale. J. Clin. Invest. 116 1186–1194
Yogesha SD, Khapli SM and Wani MR 2005 Interleukin-3 and granulocyte-macrophage colony-stimulating factor inhibits tumor necrosis factor (TNF)- α-induced osteoclast differentiation by down-regulation of expression of TNF receptors 1 and 2. J. Biol. Chem. 280 11759–11769
Yogesha SD, Khapli SM, Srivastava RK, Mangashetti LS, Pote ST, Mishra GC and Wani MR 2009 IL-3 Inhibits TNF-α-induced bone resorption and prevents inflammatory arthritis. J. Immunol. 182 361–370
Yoshimatsu M, Kitaura H, Fujimura Y, Eguchi T, Kohara H, Morita Y and Yoshida N 2009 IL-12 inhibits TNF-α induced osteoclastogenesis via a T cell-independent mechanism in vivo. Bone 45 1010–1016
Zhao B, Grimes SN, Li S, Hu X and Ivashkiv LB 2012 TNF-induced osteoclastogenesis and inflammatory bone resorption are inhibited by transcription factor RBP-J. J. Exp. Med. 209 319–334
Acknowledgements
VP is the recipient of a Senior Research Fellowship from the University Grant Commission, New Delhi, India.
Funding
This work was supported by the intramural grant from National Centre for Cell Science, Pune.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Animal Rights
The Institutional Animal Ethics Committee approved all animal protocols.
Additional information
Corresponding editor: Dipankar Nandi
Corresponding editor: Dipankar Nandi
Rights and permissions
About this article
Cite this article
Piprode, V., Singh, K., Kumar, A. et al. IL-3 inhibits rat osteoclast differentiation induced by TNF-α and other pro-osteoclastogenic cytokines. J Biosci 46, 63 (2021). https://doi.org/10.1007/s12038-021-00181-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12038-021-00181-3