Abstract
Our previous study has proposed that increased presynaptic NMDARs activities play pivotal roles in the development of opioid tolerance and hyperalgesia, and blocking spinal NMDARs attenuates chronic morphine-induced synaptic plasticity and behavior. However, the cellular signaling mechanisms remain to be investigated. The aim of this research was to address the role of β-ARK1 in opioid analgesia. Opioid tolerance and hyperalgesia was induced by daily systemic morphine injections in rats for eight consecutive days. Whole-cell voltage-clamp was employed to record spontaneous EPSCs and evoked-AMPA-EPSCs in dorsal lamina II neurons. Strikingly, brief application of 1 μM morphine decreased the percentage of inhibition and was followed by a large LTP in the amplitude of monosynaptic evoked-AMPA-EPSCs in opioid-tolerant rats. There was no effect on these responses by postsynaptic dialysis of the G-protein inhibitor. Incubation with the NMDAR blocker AP5 potentiated morphine-induced inhibition and attenuated washout potentiation after cessation of morphine in the amplitude of AMPA-EPSCs. Incubation with β-ARK1 inhibitor had the same effect on these responses. Incubation with β-ARK1 inhibitor diminished NMDAR hyperfunction-increased glutamatergic synaptic transmission and enhanced the analgesic effect of morphine. Intrathecal injections of β-ARK1 inhibitor significantly attenuated opioid-induced hyperalgesia and tolerance. β-ARK1 plays a pivotal role in the development and maintenance of opioid tolerance and hyperalgesia. Blockade of β-ARK1 activation ameliorates morphine tolerance and hyperalgesia via regulating the activity of spinal NMDARs. These findings provide electrophysiological evidence and useful insights regarding the mechanistic action of β-ARK1 inhibitor as a potential anti-hyperalgesic agent to improve the efficacy of opioid therapies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
NMDARs have been proved to negatively regulate the capacity of opioids to alleviate pain [1,2,3,4]. Increased activities of NMDARs complicate the clinical use of opioids for the treatment of neuropathic pain [5, 6]. Blockade of NMDARs could ameliorate the development of tolerance and hyperalgesia to different opioid effects and be the erasure of hyperalgesia and tolerance to morphine, stressing that NMDARs play pivotal roles in both the development and management of opioid hyperalgesia and tolerance [1, 4, 7]. The interaction between the opioid system and NMDARs is underlined by the opioid-dependent regulation of neurotransmission mediated by NMDARs. Our previous study has proposed that increased activities of spinal presynaptic NMDARs contribute to an increase in glutamate release from primary afferents and opioid tolerance and hyperalgesia [8]. These responses could be attenuated by intrathecal injection of NMDARs antagonists, suggesting that blockade of spinal NMDARs hyperfunction effectively ameliorates the development and maintenance of morphine-induced tolerance and hyperalgesia. The relationship between NMDARs and μ-opioid receptors is bidirectional, and μ-opioid receptors-induced potentiation of NMDARs activity results in tolerance to morphine [1, 4, 9, 10]. For example, morphine decreases presynaptic NMDARs-mediated glutamatergic input from primary afferent terminals to relieve pain, but causes long-lastingly increased glutamatergic input through activation of presynaptic NMDARs after repeated opioid injections [11]. However, little is known about the signaling pathways that mediate the NMDARs activity involved in the management of spinal opioid antinociception.
β-ARK1, a type of G-protein-coupled receptor kinases (GRK), induces desensitization of opioid-mediated transmission semaphore, which plays a functional role in the opioid-induced synaptic plasticity and causes central sensitization of neurons in the spinal cord [12,13,14,15]. The activation of β-ARK is simultaneously regulated by the interaction of the kinase with the heterotrimeric G protein βγ subunits and the agonist-occupied form of receptor substrate [16]. It was found that there was a 35% increase in levels of β-ARK1 expression by repeated morphine treatment [17]. An increase in β-ARK1 immunoreactivity by chronic morphine may contribute to opioid-induced tolerance and hyperalgesia. It is well established that the selected G-protein-coupled receptors (GPCRs) regulate NMDARs function and result in NMDAR-dependent plasticity [18, 19]. However, the signaling mechanisms and specific cellular origin involved in morphine-increased activity of β-ARK1 and NMDARs remain unclear.
The current research used a multi-disciplinary approach to investigate the effect of selective kinase β-ARK1 inhibitors at the cellular and system levels on the erasure of opioid-induced hyperalgesia and tolerance. We focused on β-ARK1 because it can modulate the NMDARs activity and play a critical role in central sensitization in the spinal cord, which is a critical mechanism of spinal opioid tolerance and hyperalgesia. In this study, we determined how hyperactivity of β-ARK1 affects morphine-induced analgesia and regulates morphine tolerance-related spinal synaptic plasticity and behavior by chronic morphine injections.
Methods
Animals and Morphine Administration
Male Sprague Dawley (SD) rats (280–320 g) were used in this research. All of the experimental preparation and surgical protocols conformed to the National Natural Science Foundation of China guidelines on the ethical use of animals and were approved by the Animal Care and Use Committee of Huazhong University of Science and Technology. Animals were randomly assigned to one of two groups: morphine group and control (saline) group. With respect to group assignment, all testing was conducted blindly. Opioid tolerance and hyperalgesia were induced with consecutive intraperitoneal administrations of 10 mg/kg morphine (Sigma, USA) for 8 days [8, 20]. In the control group, rats received daily intraperitoneal administrations of the saline. Under isoflurane-induced anesthesia, intrathecal catheters implanted were prepared for behavioral experiments with live rats as described in our previous studies [8, 20]. Before intrathecal injections, the rats were recovered for 5 days [8].
Spinal Cord Slices Preparation and Electrophysiological Recordings
Under 2% isoflurane in O2 anesthesia, the spinal cord in the lumbar segment was immediately removed through laminectomy and rapidly put in ice-cold artificial cerebrospinal fluid (aCSF) as we described previously [8, 21]. The aCSF included (in mM) sucrose 234, MgCl2 1.2, CaCl2 2.5, KCl 3.6, NaHCO3 25.0, NaH2PO4 1.2, and glucose 12.0 and were preconditioned with 5% CO2 and 95% O2. The 400 μm in thickness was cut from transverse spinal cord slices in ice-cold sucrose aCSF and then transferred to Krebs solution preconditioned with 5% CO2 and 95% O2 at 34 °C for at least 1 h.
Whole-cell voltage-clamp techniques were employed to record spontaneous EPSCs and evoked-AMPA-EPSCs in visualized lamina II neurons. The internal solution included (in mM) KCl 5, K-gluconate 135, MgCl2 2.0, CaCl2 0.5, Hepes 5.0, ATP-Mg 5.0, Na-GTP 5.0, EGTA 0.5, and QX314 10 and was used to adjusted to pH 7.25 with 1.0 m CsOH (280–300 mOsm). The impedance was 4–7 MΏ. Through a bipolar tungsten electrode, synaptic currents were evoked from the dorsal root when the evoked AMPA-EPSCs were recorded. At a holding potential of − 60 mV, the AMPA-EPSCs were recorded in the presence of 10 μM land 2 μM strychnine. If the input resistance changed by more than 15%, the recording was abandoned. An amplifier MultiClamp 700A (Axon Instruments, Foster City, CA, USA) with a stimulator (Grass instruments, quincy, MA, USA) was employed to record EPSC and digitized at 10 kHz and filtered at 1–2 kHz. β-ARK1 was purchased from Abcam, and most of the salts used to prepare the external and internal media were purchased from Sigma.
Behavioral Assessment
Rats (morphine group n = 9 rats and control group n = 6 rats) achieved more than three 60-min acclimation to the experiment environment over successive days prior to mechanical and thermal monitoring [8, 20]. After habituations for 30 min, baseline withdrawal thresholds were recorded in response to the mechanical and thermal nociception applied to the hindpaw. The mean value of both of hindpaws tested in each animal was used as the mechanical and thermal nociceptive withdrawal threshold [8, 20]. After the baseline of the mechanical and thermal nociceptive withdrawal threshold was recorded, an intrathecal injection of morphine was then given to the animals and the mechanical and thermal threshold was tested after morphine injection for 30 min in response to the pressure and thermal stimulus.
To quantitatively assess the mechanical nociception, rats were tested with the Ugo Basil Analgesimeter (Varese, Italy). The animal’s nociceptive threshold was recorded on the scale when they displayed pain by withdrawing the paw. A cut-off of 400 g was used to prevent potential tissue injury. The thermal nociception of rats were tested with a thermal testing apparatus (IITC Inc., Woodland Hills, CA, USA). To avoid potential tissue damage, a maximum of 30s was used as a cut-off.
Data Analysis
Averaged data are presented as means ± SEM. For electrophysiological experiment, in the control group minimum numbers were determined based on pertinent literature [8, 21] and in the treatment group minimum numbers were determined based on our pilot experiment for comparable studies in which desired effect sizes were shown to be statistically significant. To determine the amplitude of the evoked AMPA-EPSCs, at least 10 consecutive AMPA-EPSCs were averaged and analyzed offline with Clampfit 10.0 software. SEPSCs were analyzed off-line using a peak detection program (MiniAnalysis; Synaptosoft, Leonia, NJ, USA). The cumulative probability of the amplitude and the interevent interval of the sEPSCs were compared using the Kolmogorov-Smirnov test, which estimates the probability that two distributions are similar. We used Student’s t test to compare two groups and one-way analysis of variance followed by Dunnett’s post hoc test to compare more than two groups. Two-way analysis of variance followed by Bonferroni’s post hoc test was used to determine the difference in the development of opioid tolerance and hyperalgesia between the vehicle-treated and β-ARK1 inhibitor-treated groups. P < 0.05 was considered to be statistically significant.
Results
Morphine application on spinal cord slices from morphine-treated rats produces less inhibition of glutamatergic input and cessation of morphine results in increased glutamatergic input.
Bath application of 1 μM morphine for 3 min significantly inhibited the amplitude of spinal monosynaptic AMPA-EPSCs evoked from the dorsal root in vehicle-treated (n = 12 neurons) and morphine-treated (n = 25 neurons) rats (Fig. 1a, b). However, in comparison with vehicle group (46.25 ± 4.68%, n = 12 neurons, Fig. 1c), there was significantly reduced the percentage of inhibition of the amplitude of AMPA-EPSCs by chronic morphine (18.12 ± 2.63%, Fig. 1c). After washout of morphine, there was a significant decrease in the percentage of inhibition of the amplitude of monosynaptic AMPA-EPSCs in opioid tolerant rats (− 24.07 ± 5.09%, n = 25 neurons, Fig. 1c), but a significant increase in vehicle-treated rats (17.45 ± 4.39%, n = 12 neurons, Fig. 1c).
Presynaptic μ-receptors contribute to opioid-decreased inhibition followed by a large LTP in the morphine-tolerant spinal cord. a Original tracings show the effect of bath application of 1 μM morphine on monosynaptic AMPA-EPSCs of laminal II neurons evoked from the dorsal root in a vehicle- and opioid-tolerant rat (recorded with and without 1 μM GDP-β-S in the pipette solution). b Group data show the effect of bath application of 1 μM morphine on the mean amplitude of evoked AMPA-EPSCs of lamina II neurons in vehicle-treated (n = 12 neurons) as well as morphine-treated rats recorded without GDP-β-S (n = 25 neurons) or with GDP-β-S (n = 33 neurons). c Group data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean amplitude of evoked AMPA-EPSCs in vehicle-treated (n = 12 neurons) as well as morphine-treated rats recorded without GDP-β-S (n = 25 neurons) or with GDP-β-S (n = 33 neurons). d Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean amplitude of AMPA-EPSCs in vehicle-treated (n = 12 neurons) as well as morphine-treated rats recorded without GDP-β-S (n = 25 neurons) or with GDP-β-S (n = 33 neurons). *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Presynaptic mu-opioid receptors contribute to application of morphine-reduced the percentage of inhibition of glutamatergic input and cessation of morphine-increased long-term potentiation (LTP) at the spinal level in the opioid tolerant rats.
To investigate whether postsynaptic μ-opioid receptors contributes to these responses, general G-protein inhibitor GDP-β-S (1 μM) was employed to block postsynaptic MORs in the pipette internal solution [21]. Postsynaptic intracellular application of the MORs blocker GDP-β-S had no effect on these responses in the chronic opioid-tolerant rats (n = 33 neurons, Fig. 1a–c).
To further investigate the role of additional application of morphine in LTP in the opioid tolerant rats, AMPA-EPSCs were recorded for 21 min after cessation of morphine. Surprisingly, after 15 min cessation of morphine, there was a significant and persistent increase in the amplitude of AMPA-EPSCs of chronic morphine-treated spinal lamina II neurons (n = 25 neurons, Fig. 1d). However, in the vehicle group, there was the prolonged inhibition after 15 min cessation of morphine, which was a specific effect of morphine compare to previous studies [21, 22]. Meanwhile, there was no effect on these responses by blocking postsynaptic MORs with GDP-β-S in the pipette internal solution in the opioid-tolerant rats (n = 33 neurons, Fig. 1d).
Additional application of morphine decreases the percentage of inhibition of spinal basal glutamatergic synaptic input to lamina II neurons in the opioid tolerant rats.
Additional treatment with 1 μM morphine for 3 min significantly inhibited the frequency of sEPSCs of spinal lamina II neurons from vehicle-treated (n = 12 neurons, Fig. 2a–c) and morphine-treated rats (n = 14 neurons, Fig. 2a–c). However, in comparison with vehicle group (37.69 ± 3.03%, n = 12 neurons, Fig. 2e), there was significantly reduced percentage of inhibition of the frequency of sEPSCs in chronic morphine rats (20.91 ± 4.20%, n = 14 neurons, Fig. 2e). After morphine washout, in comparison with morphine tolerant group (− 0.14 ± 3.99%, n = 14 neurons, Fig. 2e), there was a significant increase in the percentage of inhibition of the frequency of sEPSCs in vehicle rats (19.78 ± 3.37%, n = 12 neurons, Fig. 2e).
Chronic morphine decreases morphine-inhibited basal glutamatergic input in the spinal cord. a Original recording traces and cumulative plots show the effect of bath application of 1 μM morphine for 3 min on the frequency and amplitude of sEPSCs of a lamina II neuron from a vehicle-treated rat. b Original recordings and cumulative plots show the effect of 1 μM morphine on sEPSCs of a lamina II neuron from an opioid-tolerant rat. c Summary data of the effect of bath application of 1 μM morphine on the mean frequency and amplitude of sEPSCs in vehicle-treated (n = 12 neurons) and morphine-tolerant (n = 14 neurons) rats. d Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean frequency of sEPSCs in vehicle-treated (n = 12 neurons) as well as morphine-treated (n = 14 neurons) rats. e Group data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean frequency of sEPSCs in vehicle-treated (n = 12 neurons) as well as morphine-treated (n = 14 neurons) rats. *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Compared with vehicle group (n = 12 neurons, Fig. 2c, d), after 15 min cessation of morphine, there was significantly increased the frequency of sEPSCs in opioid tolerant rats (n = 14 neurons, Fig. 2c, d). There was no significant effect on the amplitude of sEPSCs in the vehicle-treated (n = 12 neurons, Fig. 2c) and morphine-treated (n = 14 neurons, Fig. 2c) rats.
The role of spinal NMDA receptor activity in morphine application-produced less inhibition and cessation of morphine-induced LTP at the spinal level in the opioid tolerant rats.
After Incubation with the NMDARs blocker 50 μM AP5 for 2 h, bath application of morphine (1 μM) for 3 min induced a significant decrease in the amplitude of monosynaptic AMPA-EPSCs by (n = 27 neurons, Fig. 3a–b).
Contribution of NMDA receptor activity in chronic morphine-induced tolerance and hyperalgesia in the spinal cord. a Original recordings show the effect of 1 μM morphine on evoked AMPA-EPSCs of lamina II neurons from spinal cord slices pretreated with AP5 in a morphine-treated rat. b Summary data show the effect of 1 μM morphine on the mean amplitude of AMPA-EPSCs of lamina II neurons from spinal cord slices pretreated with AP5 in morphine-treated rats. c Group data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean amplitude of evoked AMPA-EPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without AP5 n = 25 neurons and with AP5 n = 27 neurons). d Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean amplitude of AMPA-EPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without AP5 n = 25 neurons and with AP5 n = 27 neurons). *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Compared with morphine group (18.12 ± 2.66%, n = 25 neurons, Fig. 3c), there was a significant increase in the percentage of inhibition of the amplitude of evoked-AMPA-EPSCs after AP5 treatment (32.54 ± 3.79%, n = 27 neurons, Fig. 3c). After 15 min cessation of morphine, there was significantly increased inhibition of percentage of the amplitude of AMPA-EPSCs after AP5 incubation (− 7.41 ± 3.19%, n = 27 neurons, Fig. 3c) compared with morphine group (− 24.07 ± 5.09%, n = 25 neurons, Fig. 3c). There was a significant long-term depression in the amplitude of AMPA-EPSCs in AP5 group after 15 min cessation of morphine (n = 27 neurons, Fig. 3d).
After AP5 incubation for 2 h, bath application of 1 μM morphine for 3 min significantly decreased the frequency of sEPSCs of spinal lamina II neurons (n = 27 neurons, Fig. 4a–c).
Contribution of NMDA receptor activity in chronic morphine-induced basal glutamatergic release in the spinal cord. a Original recording traces show the effect of bath application of 1 μM morphine on the sEPSCs of lamina II neurons from spinal cord slices pretreated with AP5 in a chronic morphine-treated rats. b Cumulative plots show the effect of bath application of 1 μM morphine on the frequency and amplitude of sEPSCs of lamina II neurons from spinal cord slices pretreated with AP5 in a morphine tolerant rat. c Group data show the effect of bath application of 1 μM morphine on the mean frequency of sEPSCs of lamina II neurons from spinal cord slices pretreated with AP5 in morphine-treated rats. d Summary data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean frequency of sEPSCs in vehicle- (n = 11 neurons) and morphine-treated rats (without AP5 n = 14 neurons and with AP5 n = 27 neurons). e Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean frequency of sEPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without AP5 n = 14 neurons and with AP5 n = 27 neurons). *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Compared with morphine group (20.91 ± 4.20%, n = 14 neurons, Fig. 4d), there was a significant increase in the percentage of inhibition of the frequency of sEPSCs after AP5 treatment (42.96 ± 3.37%, n = 27 neurons, Fig. 4d). After 15 min cessation of morphine, compared with morphine group (− 0.14 ± 3.99%, n = 14 neurons, Fig. 4d), there was significantly increased the percentage of inhibition of the frequency of sEPSCs after AP5 incubation (2.01 ± 5.547%, n = 27 neurons, Fig. 4d). Compared with morphine group (n = 14 neurons, Fig. 4e), there was a significant long-term depression in the frequency of sEPSCs in AP5 group after 15 min cessation of morphine (n = 27 neurons, Fig. 4e).
β-ARK1 regulates the increase in spinal NMDARs activities produced by chronic morphine.
β-ARK1, a type of GRK, induces desensitization of opioid-mediated transmission semaphore, which plays a functional role in the opioid-induced synaptic plasticity and causes central sensitization of neurons in the spinal cord [14, 16, 17, 23]. It was proved that there was a significant increase in β-ARK1 activity in the central nervous system by chronic morphine [14, 17]. To determine whether β-ARK1 mediates the increased NMDARs activities by repeated opioid treatment, β-ARK1 inhibitor (a GRK2 selective antagonist) was used. After incubation for 2 h with β-ARK1 inhibitor (100 μM), additional treatment with 50 μM AP5 failed to affect the amplitude of AMPA-EPSCs of morphine-tolerant spinal lamina II neurons from the dorsal root (Fig. 5a–d). AP5 significantly reduced the amplitude of AMPA-EPSCs in morphine-tolerant rats without β-ARK1 inhibitor incubation (n = 11 neurons, Fig. 5a–d). Thus, our data suggest that β-ARK1 play an important role in an increase in spinal NMDARs hyperactivities caused by chronic morphine (n = 27 neurons, Fig. 5d).
β-ARK1 contributes to augmented glutamatergic input to spinal dorsal horn neurons induced by chronic morphine. a Representative recordings show the lack of effect of 50 μM AP5 on the amplitude of AMPA-EPSCs of a lamina II neuron from a spinal cord slice in one morphine-treated rat. b Representative traces plots show the effect of 50 μM AP5 on the amplitude of AMPA-EPSCs of a lamina II neuron from a spinal cord slice in one morphine-treated rat. c Original traces show the lack of effect of 50 μM AP5 on the amplitude of monosynaptic AMPA-EPSCs of the lamina II neuron from a spinal cord slice pretreated with β-ARK1inhibitor in a morphine-treated rat. d Summary data of the effect of 50 μM AP5 on the mean amplitude of evoked AMPA-EPSCs in spinal cord slices in vehicle- (n = 9 neurons) and morphine-treated rats (without n = 11 neurons and with β-ARK1 inhibitor n = 27neurons). *p < 0.05 when compared with respective baseline controls
To analyze the hyperactivity of β-ARK1 in NMDAR-mediated basal glutamate input from primary afferents, β-ARK1 inhibitor was employed in repeated opioid-injected rats. Incubation for 2 h with the β-ARK1 inhibitor (100 μM) abolished the 50 μM AP5-mediated inhibition of the frequency of sEPSCs of morphine-tolerant spinal lamina II neurons (n = 19 neurons, Fig. 6a–c).
β-ARK1 contributes to augmented basal glutamatergic release to spinal dorsal horn neurons induced by chronic morphine. a Representative recordings show the lack of effect of 50 μM AP5 on the frequency and amplitude of sEPSCs of a lamina II neuron from a spinal cord slice pretreated with 100 μM β-ARK1inhibitor in one morphine-treated rat. b Cumulative plots show the lack of effect of 50 μM AP5 on the frequency and amplitude of sEPSCs of a lamina II neuron from a spinal cord slice pretreated with 100 μM β-ARK1inhibitor in one morphine-treated rat. c Summary data of the effect of 50 μM AP5 on the mean frequency and amplitude of sEPSCs (n = 19 neurons) in spinal cord slices pretreated with β-ARK1inhibitor in morphine-treated rats
Contribution of β-ARK1 activity in morphine application produced less inhibition and cessation of morphine-induced LTP at the spinal level in the opioid tolerant rats.
To analyze the role of β-ARK1 activity in chronic morphine-inhibited glutamatergic transmission from primary afferents by morphine treatment, β-ARK1 inhibitor (a GRK2 selective antagonist) was employed to block β-ARK1 activity in morphine-tolerant rats. After incubation with β-ARK1 inhibitor (100 μM) for 2 h, additional treatment with 1 μM morphine for 3 min significantly inhibited the amplitude of monosynaptic AMPA-EPSCs in the spinal cord (n = 22 neurons Fig. 7a, b).
β-ARK1 contributes to augmented morphine-decreased inhibition of glutamatergic input and LTP at the spinal level by chronic morphine. a Original recording traces show the effect of bath application of 1 μM morphine on the amplitude of evoked AMPA-EPSCs of lamina II neurons from spinal cord slices in a vehicle- (without and with β-ARK1 inhibitor) and opioid-tolerant(with β-ARK1 inhibitor) rat. b Summary data show the effect of 1 μM morphine on the amplitude of lamina II neurons from spinal cord slices in vehicle-(without n = 12 neurons and with n = 8 neurons β-ARK1 inhibitor) and morphine-treated (with β-ARK1 inhibitor, n = 22 neurons) rats. c Group data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean amplitude of evoked AMPA-EPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without β-ARK1 inhibitor n = 25 neurons and with β-ARK1 inhibitor n = 22 neurons). d Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean amplitude of evoked AMPA-EPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without β-ARK1 inhibitor n = 25 neurons and with β-ARK1 inhibitor n = 22 neurons). *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Compared with morphine group (18.12 ± 2.66%, n = 25 neurons, Fig. 7c), there was a significant increase in the inhibition of percentage of the amplitude of evoked-AMPA-EPSCs after β-ARK1 inhibitor treatment (30.07 ± 2.96%, n = 18 neurons, Fig. 7c). After 15 min cessation of morphine, compared with morphine group (− 24.07 ± 5.09%, n = 25 neurons, Fig. 7c) there was significantly increased inhibition of percentage of the amplitude of AMPA-EPSCs after β-ARK1 inhibitor incubation (4.69 ± 4.50%, n = 18 neurons, Fig. 7c). Compared with morphine group (n = 25 neurons, Fig. 7d), there was a significant long-term depression in the amplitude of AMPA-EPSCs in β-ARK1 inhibitor group after 15 min cessation of morphine (n = 18 neurons, Fig. 7d).
To analyze whether β-ARK1 activity plays the same role in morphine-inhibited glutamatergic transmission from primary afferents in vehicle-treated rats, β-ARK1 inhibitor was employed to block β-ARK1 activity. After incubation with β-ARK1 inhibitor (100 μM) for 2 h, bath application with 1 μM morphine for 3 min significantly inhibited the amplitude of monosynaptic AMPA-EPSCs in the spinal cord (n = 8 neurons, Fig. 7a, b) in vehicle-treated group. But compared with control, there was no significant effect on morphine-inhibited the amplitude of spinal monosynaptic AMPA-EPSCs after β-ARK1 inhibitor incubation (Fig. 7a, b).
To analyze the role of β-ARK1 activity in chronic morphine-elevated basal glutamatergic synaptic input to spinal lamina II neurons, β-ARK1 inhibitor was employed to block β-ARK1 activity in morphine-tolerant rats. After incubation with the β-ARK1 inhibitor for 2 h, bath application of 1 μM morphine for 3 min significantly inhibited the frequency of sEPSCs of spinal lamina II neurons in chronic opioid-treated spinal cord slices (n = 18 neurons, Fig. 8a–c). There was no significant effect on the amplitude of sEPSCs after β-ARK1 inhibitor treatment (n = 18 neurons, Fig. 8b, c).
Contribution of β-ARK1 activity in chronic morphine-induced basal glutamatergic release in the spinal cord. a Original recording traces show the effect of bath application of 1 μM morphine on the sEPSCs of lamina II neurons from spinal cord slices pretreated with β-ARK1 inhibitor in an opioid tolerant rat. b Cumulative plots show the effect of bath application of 1 μM morphine on the frequency and amplitude of sEPSCs of lamina II neurons from spinal cord slices pretreated with β-ARK1 inhibitor in a morphine-treated rat. c Group data show the effect of bath application of 1 μM morphine on the frequency of sEPSCs of lamina II neurons from spinal cord slices pretreated with β-ARK1 inhibitor in morphine-treated rats. d Summary data show the percentage of inhibition after bath application of 1 μM morphine and cessation of morphine on the mean frequency of sEPSCs in vehicle- (n = 12 neurons) and morphine-treated rats (without n = 14 neurons and with β-ARK1 inhibitor n = 18 neurons). e Mean time courses of lamina II neurons with bath application of 1 μM morphine for 3 min on the mean frequency of sEPSCs in vehicle-treated (n = 12 neurons) and morphine-treated rats (without n = 14 neurons and with β-ARK1 inhibitor n = 18 neurons). *p < 0.05 when compared with respective baseline controls. # p < 0.05 when compared with respective treated group
Compared with morphine group (20.91 ± 4.20%, n = 14 neurons, Fig. 8d), there was a significant increase in the inhibition of percentage of the frequency of sEPSCs after β-ARK1 inhibitor treatment (49.32 ± 3.97%, n = 18 neurons, Fig. 8d). After 15 min cessation of morphine, there was significantly increased inhibition of percentage of the frequency of sEPSCs after β-ARK1 inhibitor incubation (15.87 ± 3.65%, n = 18 neurons, Fig. 8d) compared with morphine group (− 0.14 ± 3.99%, n = 14 neurons, Fig. 8d). Compared with morphine group (n = 14 neurons, Fig. 8e), there was a significant long-term depression in the frequency of sEPSCs in β-ARK1 inhibitor group after 15 min cessation of morphine (n = 18 neurons, Fig. 8e).
Blocking β-ARK1 activity ameliorates morphine-induced tolerance and hyperalgesia in the spinal cord.
To induce morphine tolerance in rats, morphine (10 mg/kg) was used by daily intraperitoneal injection for 8 days. β-ARK1 inhibitor (40 μg) (n = 9 rats) or saline (n = 6 rats) was administered daily through the intrathecal catheter in morphine-tolerant rats. To avoid potential tissue injury when the analgesic effect of morphine was assessed, morphine (5 mg/kg) was intraperitoneally injected. And after behavioral test each day, the remaining morphine (5 mg/kg) was administered. To examine the role of spinal β-ARK1 activation in the reinstatement of opioid antinociception tolerance, 20 μg of β-ARK1 inhibitor or vehicle was injected 5 min before morphine injection. Mechanical and thermal nociception was tested before and 30 min after morphine administration. After the behavioral test each day, the remaining β-ARK1 inhibitor (20 μg) was administered intrathecally along with morphine (5 mg/kg) injected intraperitoneally.
In the vehicle group, the antinociceptive role of morphine in response to application of the mechanical and thermal nociception was gradually attenuated by daily intraperitoneal injection of morphine (10 mg/kg). Within 1 week, in vehicle-treated rats morphine injection (5 mg/kg) failed to produce a significant effect on the paw withdrawal threshold (n = 6 rats, Fig. 9a–b). By comparison, in β-ARK1 inhibitor-injected rats the analgesic role of morphine in the paw withdrawal threshold was gradually reduced but largely sustained during the eight consecutive days of morphine administration (n = 9 rats, Fig. 9a–b). Even on the last day of morphine administration, intraperitoneal injection of 10 mg/kg of morphine significantly enhanced the paw withdrawal threshold in the β-ARK1 inhibitor-treated rats.
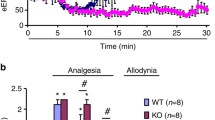
Blocking β-ARK1 at the spinal level attenuates the development of hyperalgesia and analgesic tolerance caused by chronic morphine. a Time course of changes in the baseline nociceptive withdrawal thresholds, tested by applying a noxious pressure stimulus to the hindpaw, and the analgesic effect of morphine in rats treated with intrathecal injections of vehicle (saline n = 6 rats).) or β-ARK1inhibitor (n = 9 rats). b Time course of changes in the baseline nociceptive withdrawal thresholds tested by applying a noxious heat stimulus to the hindpaw, and the analgesic effect of morphine in rats treated with intrathecal injections of saline or β-ARK1inhibitor. The baseline withdrawal threshold was measured before morphine injection each day, and the analgesic effect of morphine was tested 30 min after each morphine injection (5 mg/kg, i.p.). *p < 0.05 compared with the corresponding morphine effect in the vehicle control group. # p < 0.05 compared with the corresponding baseline value in the vehicle control group
In the vehicle group, the baseline paw withdrawal threshold was gradually reduced by daily intraperitoneal morphine (10 mg/kg) treatment. In contrast, the baseline paw withdrawal threshold was largely sustained in β-ARK1 inhibitor-injected rats during the eight consecutive days of morphine administration (n = 9 rats, Fig. 9a–b). In the β-ARK1 inhibitor group, the baseline was similar to that tested before morphine administration even on day 8 of morphine injection. Therefore, our data imply that increased spinal β-ARK1 activities play pivotal roles in the reinstatement of opioid hyperalgesia and tolerance by systemic morphine treatment.
Discussion
In this study, we provide electrophysiological evidence that morphine application on spinal cord slices from morphine-treated animals produces less inhibition of AMPA-EPSCs and the cessation of morphine application results in increased AMPA-EPSCs. These data prove that the development of analgesic tolerance during chronic use requires an increase in the dose of the drug to produce the same pain relief, which occurs in parallel with the progressive reduction of the nociceptive threshold. This is a major obstacle to improving the clinical treatment of moderate to severe pain [3, 24,25,26]. Our data suggest that brief application of morphine induces a decrease short-term inhibition and cessation of morphine result in LTP in spinal glutamatergic input from primary afferents to lamina II neurons in morphine-tolerant rats contribute to morphine tolerance and hyperalgesia.
μ-opioid receptor agonist likely produces spinal antinociception by attenuating presynaptic primary afferent input and by inhibiting postsynaptic dorsal neurons [21, 22, 27]. Our previous study observes, during the μ-opioid receptor agonists’ enkephalin washout, a rebound increase in glutamatergic input to some spinal lamina II neurons in normal rats [28]. However, whether pre- or postsynaptic μ-opioid receptors regulate morphine antinociception mechanism in opioid-tolerant rats is still fragmentary. Postsynaptic intracellular additional treatment with GDP-β-S had no effect on these responses to the spinal lamina II neurons, suggesting that presynaptic μ-opioid receptors play pivotal roles in morphine tolerance and hyperalgesia.
Our data suggest that NMDARs hyperactivities play vital roles in morphine tolerance and hyperalgesia. In the current opinions, there are many proposed mechanisms for opioid-induced hyperalgesia and tolerance involving the central glutaminergic system, spinal dynorphins, and so on [29]. Of these, the central glutaminergic system is considered the most common possibility. Our previous studies and others have confirmed that NMDARs in opioid-induced hyperalgesia and tolerance include activation of the glutamate transporter system, facilitation of calcium regulated intracellular PKC [8, 30, 31]. Our previous data have proposed that the spinal presynaptic hyperactivity of NMDARs contributes to an increase in glutamatergic input from primary afferents and also contributes to tolerance and hyperalgesia produced by repeated morphine administration [7,8,9]. Blocking spinal NMDARs by ketamine and dextromethorphan attenuates chronic morphine tolerance, as well as the related synaptic plasticity and behavior. However, little is known about the unifying intracellular and molecular mechanisms of blockade of NMDAR activation in morphine analgesia at the spinal cord level after long-term morphine administration [1, 4, 21, 22]. AP5, a NMDAR antagonist, produced a significant increase in the percentage of inhibition of the amplitude of spinal monosynaptic evoked AMPA-EPSCs by additional application of morphine and a significant inhibition in long-term potentiation after cessation of morphine. Our findings stress that NMDAR activity contributes to morphine analgesic tolerance.
Our findings suggest that the spinal NMDAR is the target of β-ARK1 in morphine tolerance and hyperalgesia. β-ARK1, as a member of growing family of GRKs, has been identified within the cell bodies of neurons, and within structures including presynaptic axon terminals, dendritic spines, and dendritic shifts [32]. β-ARK1 plays a pivotal role in the mechanism of agonist-specific desensitization and agonist-dependent GPCR phosphorylation [16]. The increased β-ARK1 activity has been proven in the central nervous system by chronic morphine treatment [14, 15, 17]. Our previous studies have proved that chronic stimulation of the μ-opioid receptors increase NMDAR activity at primary afferents, but the precise signaling mechanisms are not fully known. In this study, we found that bath application of NMDAR blocker AP5 failed to significantly affect the amplitude of evoked AMPA-EPSCs and the frequency of sEPSCs in the β-ARK1 inhibitor-incubated spinal cord slices from opioid-tolerant rats. Furthermore, incubation with β-ARK1 inhibitor potentiated the morphine-induced inhibition of the amplitude of evoked AMPA-EPSCs and the frequency of sEPSCs in morphine-treated rats. Our data collectively suggest that β-ARK1 activity contributes to NMDAR hyperfunction-induced glutamatergic synaptic transmission in opioid-tolerant rats, and blockade of β-ARK1 activation reinstates morphine-related synaptic plasticity.
In parallel with these findings, intrathecal injections of β-ARK1 inhibitor significantly attenuated opioid analgesic tolerance. After intrathecal application of β-ARK1 inhibitor, the time course of morphine analgesic effects on the paw withdrawal threshold was gradually reduced but largely sustained during the eight consecutive days of morphine administration. Furthermore, the baseline paw withdrawal threshold failed to be significantly altered by chronic morphine in intrathecal injection of β-ARK1 inhibitor group. Our results suggest that β-ARK1 hyperactivity contributes to both NMDAR hyperfunction-enhanced glutamatergic input and opioid-induced hyperalgesia and tolerance in the spinal cord.
In summary, β-ARK1 hyperactivity plays a pivotal role in development and management of opioid tolerance and hyperalgesia at the spinal cord level. Blockade of β-ARK1 activation ameliorates morphine tolerance and hyperalgesia via regulating the function of spinal NMDAR. These findings provide electrophysiological evidence and useful insights regarding the mechanistic action of β-ARK1 inhibitor as a potential anti-hyperalgesic agent and an effective way to improve the efficacy of opioid therapies.
Abbreviations
- AMPAR:
-
α-Amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor
- AP5:
-
2-Amino-5-phosphonopentanoic acid
- β-ARK1:
-
Beta-adrenergic receptor kinase1
- CNQX:
-
6-cyano-7-nitroquinoxaline-2,3-dione
- EPSCs:
-
Excitatory postsynaptic currents
- GRK:
-
G-protein coupled receptor kinase
- LTP:
-
Long-term potentiation;
- NMDAR:
-
N-Methyl-D-aspartic acid receptor;
- sEPSCs:
-
Spontaneous excitatory postsynaptic currents
References
Trujillo KA, Akil H (1991) Inhibition of morphine tolerance and dependence by the NMDA receptor antagonist MK-801. Science 251:85–87
Rodriguez-Munoz M, Sanchez-Blazquez P, Vicente-Sanchez A, Berrocoso E, Garzon J (2012) The mu-opioid receptor and the NMDA receptor associate in PAG neurons: implications in pain control. Neuropsychopharmacology 37:338–349
Trang T, Al-Hasani R, Salvemini D, Salter MW, Gutstein H, Cahill CM (2015) Pain and poppies: the good, the bad, and the ugly of opioid analgesics. J Neurosci 35:13879–13888
Bashir ZI, Alford S, Davies SN, Randall AD, Collingridge GL (1991) Long-term potentiation of NMDA receptor-mediated synaptic transmission in the hippocampus. Nature 349:156–158
Zhou HY, Chen SR, Byun HS, Chen H, Li L, Han HD, Lopez-Berestein G, Sood AK et al (2012) N-methyl-D-aspartate receptor- and calpain-mediated proteolytic cleavage of K+−Cl- cotransporter-2 impairs spinal chloride homeostasis in neuropathic pain. J Biol Chem 287:33853–33864
Swartjes M, Morariu A, Niesters M, Aarts L, Dahan A (2011) Nonselective and NR2B-selective N-methyl-D-aspartic acid receptor antagonists produce antinociception and long-term relief of allodynia in acute and neuropathic pain. Anesthesiology 115:165–174
Gong K, Bhargava A, Jasmin L (2016) GluN2B N-methyl-D-aspartate receptor and excitatory amino acid transporter 3 are upregulated in primary sensory neurons after 7 days of morphine administration in rats: implication for opiate-induced hyperalgesia. Pain 157:147–158
Zhao YL, Chen SR, Chen H, Pan HL (2012) Chronic opioid potentiates presynaptic but impairs postsynaptic N-methyl-D-aspartic acid receptor activity in spinal cords: implications for opioid hyperalgesia and tolerance. J Biol Chem 287:25073–25085
Baimel C, Borgland SL (2015) Orexin signaling in the VTA gates morphine-induced synaptic plasticity. J Neurosci 35:7295–7303
Ghazvini H, Rezayof A, Ghasemzadeh Z (2015) Zarrindast MR: mu-opioid and N-methyl-D-aspartate receptors in the amygdala contribute to minocycline-induced potentiation of morphine analgesia in rats. Behav Pharmacol 26:383–392
Zhou HY, Chen SR, Pan HL (2011) Targeting N-methyl-D-aspartate receptors for treatment of neuropathic pain. Expert Rev Clin Pharmacol 4:379–388
Ozaki S, Narita M, Iino M, Miyoshi K, Suzuki T (2003) Suppression of the morphine-induced rewarding effect and G-protein activation in the lower midbrain following nerve injury in the mouse: involvement of G-protein-coupled receptor kinase 2. Neuroscience 116:89–97
Dang VC, Chieng B, Azriel Y, Christie MJ (2011) Cellular morphine tolerance produced by betaarrestin-2-dependent impairment of mu-opioid receptor resensitization. J Neurosci 31:7122–7130
Nickolls SA, Humphreys S, Clark M, McMurray G (2013) Co-expression of GRK2 reveals a novel conformational state of the micro-opioid receptor. PLoS One 8:e83691
Lowe JD, Sanderson HS, Cooke AE, Ostovar M, Tsisanova E, Withey SL, Chavkin C, Husbands SM et al (2015) Role of G protein-coupled receptor kinases 2 and 3 in mu-opioid receptor desensitization and internalization. Mol Pharmacol 88:347–356
Onorato JJ, Gillis ME, Liu Y, Benovic JL, Ruoho AE (1995) The beta-adrenergic receptor kinase (GRK2) is regulated by phospholipids. J Biol Chem 270:21346–21353
Terwilliger RZ, Ortiz J, Guitart X, Nestler EJ (1994) Chronic morphine administration increases beta-adrenergic receptor kinase (beta ARK) levels in the rat locus coeruleus. J Neurochem 63:1983–1986
Bailey CP, Oldfield S, Llorente J, Caunt CJ, Teschemacher AG, Roberts L, McArdle CA, Smith FL et al (2009) Involvement of PKC alpha and G-protein-coupled receptor kinase 2 in agonist-selective desensitization of mu-opioid receptors in mature brain neurons. Br J Pharmacol 158:157–164
Yang K, Jackson MF, MacDonald JF (2014) Recent progress in understanding subtype specific regulation of NMDA receptors by G Protein Coupled Receptors (GPCRs). Int J Mol Sci 15:3003–3024
Chen SR, Prunean A, Pan HM, Welker KL, Pan HL (2007) Resistance to morphine analgesic tolerance in rats with deleted transient receptor potential vanilloid type 1-expressing sensory neurons. Neuroscience 145:676–685
Zhou HY, Chen SR, Chen H, Pan HL (2010) Opioid-induced long-term potentiation in the spinal cord is a presynaptic event. J Neurosci 30:4460–4466
Drdla R, Gassner M, Gingl E, Sandkuhler J (2009) Induction of synaptic long-term potentiation after opioid withdrawal. Science 325:207–210
Quillinan N, Lau EK, Virk M, von Zastrow M, Williams JT (2011) Recovery from mu-opioid receptor desensitization after chronic treatment with morphine and methadone. J Neurosci 31:4434–4443
Ferrini F, Trang T, Mattioli TA, Laffray S, Del'Guidice T, Lorenzo LE, Castonguay A, Doyon N et al (2013) Morphine hyperalgesia gated through microglia-mediated disruption of neuronal Cl(−) homeostasis. Nat Neurosci 16:183–192
Pitchers KK, Coppens CM, Beloate LN, Fuller J, Van S, Frohmader KS, Laviolette SR, Lehman MN et al (2014) Endogenous opioid-induced neuroplasticity of dopaminergic neurons in the ventral tegmental area influences natural and opiate reward. J Neurosci 34:8825–8836
Sanna MD, Ghelardini C, Galeotti N (2015) Activation of JNK pathway in spinal astrocytes contributes to acute ultra-low-dose morphine thermal hyperalgesia. Pain 156:1265–1275
Araldi D, Ferrari LF, Levine JD (2015) Repeated mu-opioid exposure induces a novel form of the hyperalgesic priming model for transition to chronic pain. J Neurosci 35:12502–12517
Zhou HY, Chen SR, Chen H, Pan HL (2008) Sustained inhibition of neurotransmitter release from nontransient receptor potential vanilloid type 1-expressing primary afferents by mu-opioid receptor activation-enkephalin in the spinal cord. J Pharmacol Exp Ther 327:375–382
Lee M, Silverman SM, Hansen H, Patel VB, Manchikanti L (2011) A comprehensive review of opioid-induced hyperalgesia. Pain Physician 14:145–161
Granados-Soto V, Kalcheva I, Hua X, Newton A, Yaksh TL (2000) Spinal PKC activity and expression: role in tolerance produced by continuous spinal morphine infusion. Pain 85:395–404
Mao J, Price DD, Mayer DJ (1994) Thermal hyperalgesia in association with the development of morphine tolerance in rats: roles of excitatory amino acid receptors and protein kinase C. J Neurosci 14:2301–2312
Arriza JL, Dawson TM, Simerly RB, Martin LJ, Caron MG, Snyder SH, Lefkowitz RJ (1992) The G-protein-coupled receptor kinases beta ARK1 and beta ARK2 are widely distributed at synapses in rat brain. J Neurosci 12:4045–4055
Funding
This work was supported by a grant from the National Natural Science Foundation of China (No. 81500982).
Author information
Authors and Affiliations
Contributions
XZ contributed to the data collection and the study records. SC and HC contributed to the data collection and data analysis. HP contributed to the data analysis and manuscript preparation. YZ contributed to the study design and conduct of the study.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Zhang, X., Chen, S., Chen, H. et al. Inhibition of β-ARK1 Ameliorates Morphine-induced Tolerance and Hyperalgesia Via Modulating the Activity of Spinal NMDA Receptors. Mol Neurobiol 55, 5393–5407 (2018). https://doi.org/10.1007/s12035-017-0780-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-017-0780-3