Abstract
Ischemic preconditioning (IPC) provides neuroprotection against subsequent severe ischemic insults by specific mechanisms. We tested the hypothesis that IPC attenuates post-ischemic neuronal death in the gerbil hippocampal CA1 region (CA1) throughout hypoxia inducible factor-1α (HIF-1α) and its associated factors such as vascular endothelial growth factor (VEGF) and nuclear factor-kappa B (NF-κB). Lethal ischemia (LI) without IPC increased expressions of HIF-1α, VEGF, and p-IκB-α (/and translocation of NF-κB p65 into nucleus) in CA1 pyramidal neurons at 12 h and/or 1-day post-LI; thereafter, their expressions were decreased in the CA1 pyramidal neurons with time and newly expressed in non-pyramidal cells (pericytes), and the CA1 pyramidal neurons were dead at 5-day post-LI, and, at this point in time, their immunoreactivities were newly expressed in pericytes. In animals with IPC subjected to LI (IPC/LI)-group), CA1 pyramidal neurons were well protected, and expressions of HIF-1α, VEGF, and p-IκB-α (/and translocation of NF-κB p65 into nucleus) were significantly increased compared to the sham-group and maintained after LI. Whereas, treatment with 2ME2 (a HIF-1α inhibitor) into the IPC/LI-group did not preserve the IPC-mediated increases of HIF-1α, VEGF, and p-IκB-α (/and translocation of NF-κB p65 into nucleus) expressions and did not show IPC-mediated neuroprotection. In brief, IPC protected CA1 pyramidal neurons from LI by upregulation of HIF-1α, VEGF, and p-IκB-α expressions. This study suggests that IPC increases HIF-1α expression in CA1 pyramidal neurons, which enhances VEGF expression and NF-κB activation and that IPC may be a strategy for a therapeutic intervention of cerebral ischemic injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hypoxia inducible factor-1 (HIF-1), which is composed of HIF-1α and HIF-1β subunits, has emerged as a central oxygen-sensitive transcription factor triggered by low oxygen conditions [1, 2]. While HIF-1β is constitutively expressed, HIF-1α is upregulated in response to hypoxia. In particular, HIF-1α is upregulated by cerebral ischemia and modulates expressions of multiple genes to initiate various physiological responses against ischemic conditions [3, 4]. Previous papers have demonstrated that hypoxic or chemical preconditioning in brains upregulates HIF-1α, which is related with hypoxic or chemical preconditioning-induced neuroprotection after subsequent cerebral ischemic insults [5, 6]. Some researchers have reported that treatments of neuroprotective agents display neuroprotection against brain ischemic insults with a concurrent decrease in HIF-1α and suggested that the inhibition of HIF-1α is beneficial for neuroprotection against brain injuries including ischemic insults [7, 8]. Until now, however, roles of HIF-1α are still controversial in cerebral ischemia. Indisputably, HIF1α has an important role in complex transcriptional responses to ischemic damage in the brain [9]. In this regard, although HIF-1α is involved in cell’s responses to ischemic insults with a double-edged sword effect, it is unclear whether and how IPC-mediated neuroprotection is related with HIF-1α.
There are more than 100 downstream genes of HIF-1 identified with varying functions [10]. Vascular endothelial growth factor (VEGF), which is well known as an angiogenic and vascular permeability factor, is a representative of one of the downstream genes regulated by HIF-1 [11]. VEGF plays important roles beyond blood vessels in the nervous system [12]. For example, VEGF improves cognitive deficits after focal cerebral ischemia in the rat [13] and shows neuroprotection against ischemic injury [14–16]. These effects are suggested by some researchers who have reported that transient cerebral ischemia results in rapid neuronal and glial induction of VEGF, which may participate in the brain’s endogenous response to ischemic injury [17–19].
On the other hand, nuclear factor-kappa B (NF-κB), a well-known redox-sensitive transcription factor, is activated under various preconditionings [20, 21] as well as brain ischemia [7]; in these conditions, NF-κB can promote neuronal survival and protect neurons from toxic insults or play a role in bringing about neuronal death. These functions are implicated in adaptive responses to inflammatory conditions and neurodegenerative disorders in damaged brains [22, 23]. In addition, Gorlach and Bonello [24] have demonstrated that NF-κB and HIF-1 display important roles together under ischemic condition. In unstimulated cells, NF-κB is bound in the cytoplasm by association with small inhibitory subunit called IκB that sterically blocks the function of NF-κB’s nuclear localization sequences. Following stimulation, IκB proteins are phosphorylated by IκB kinase (IKK) complex, ubiquitinated and degraded, and NF-κB is then released and translocated to the nucleus to activate its target genes [7]. However, the question of whether IPC-mediated NF-κB activation contributes to neuroprotection against ischemia is not precisely known.
Ischemic preconditioning (IPC) is defined as a brief sublethal ischemic insult, and it could mobilize protective mechanisms to ameliorate neuronal damage following a subsequent lethal ischemia [25]. Kitagawa et al. [26] firstly demonstrated that transient ischemia elicited by a brief carotid occlusion afforded neuroprotection in adult gerbils. Further studies have demonstrated that IPC may protect neurons from cerebral ischemic insults [27, 28]. The brain possesses endogenous mechanisms capable of defending itself against ischemic damage. These innate survival pathways can be activated by IPC, whereby exposures to sublethal stressors trigger changes in gene and protein expressions that lead to an “ischemic tolerance” phenotype [29]. However, mechanisms underlying ischemic tolerance are still unclear but are believed to trigger endogenous cellular adaptation.
Variously possible explanations for IPC-mediated protective effects against ischemic insults have been proposed. Above all, it is possible that IPC-mediated neuroprotection may involve the regulation of HIF-1α and its downstream protein VEGF. However, the question of whether IPC-mediated HIF-1α expression contributes to neuroprotection against transient cerebral ischemia still needs to be fully addressed. Thus, purposes of the current study were (1) to investigate IPC-mediated neuroprotective effect against a subsequent ischemia-reperfusion insult, (2) to examine changes in IPC-induced expressions of HIF-1α and VEGF as well as the activation of NF-κB, and (3) to establish the crosstalk between them in IPC-mediated neuroprotection after a subsequent transient cerebral ischemia.
Materials and Methods
Animal Groups
Male Mongolian gerbils (Meriones unguiculatus) obtained from the Experimental Animal Center, Kangwon National University, Chuncheon, South Korea, were used at 6 months (B.W., 65–75 g) of age. The procedures for animal handling and care adhered to guidelines that are in compliance with the current international laws and policies (Guide for the Care and Use of Laboratory Animals, The National Academies Press, 8th Ed., 2011), and they were approved by the Institutional Animal Care and Use Committee (IACUC) at Kangwon National University.
Animals were divided into six groups (n = 14 at each point in time in each group): (1) sham-group, which was exposed to the common carotid arteries bilaterally and given no ischemia (sham-operation); (2) lethal ischemia (LI)-group, which was given a 5-min-transient cerebral ischemia (LI); (3) (IPC+sham)-group, which was subjected to a 2-min-sublethal ischemia (IPC) followed by sham-operation; (4) (IPC+LI)-group, which was subjected to IPC and followed by LI at 1-day post-IPC; (5) (IPC+2ME2+sham)-group, which was treated with 2-methoxyestradiol (2ME2; a HIF-1α inhibitor) at 18-h post-IPC and followed by sham-operation; and (6) (IPC+2ME2+LI)-group, which was treated with 2ME2 at 18-h post-IPC (6 h before LR) and followed by LI. The IPC paradigm has been proven to be very effective at protecting neurons against ischemic damage in this ischemic model. The animals in the groups were given recovery times of 1, 2, and 5 days after LI, because pyramidal neurons in the hippocampal CA1 region do not die until 3 days and begin to die 4 days after LI [30].
Treatment of 2ME2
2ME2 (Sigma-Aldrich, St. Louis, MO, USA), a HIF-1α inhibitor, was administered intravenously dosage of 25 mg/kg at 6 h before LI (5-min-transient cerebral ischemia). 2ME2 is a naturally occurring metabolite of estradiol known to post-transcriptionally downregulate the expression of HIF-1α [31]. It is a lipophilic compound that is constituted in dimethyl sulfoxide (DMSO) as a stock solution and further diluted in phosphate buffer saline to a final volume of 100 μl just before administration (final concentration of DMSO <1 %).
Induction of Transient Cerebral Ischemia for IPC and LI
As previously described [32], in brief, the animals were anesthetized with a mixture of 2.5 % isoflurane in 33 % oxygen and 67 % nitrous oxide. Bilateral common carotid arteries were isolated and occluded using non-traumatic aneurysm clips (Yasargil FE 723K, Aesculap, Tuttlingen, Germany). The complete interruption of blood flow was confirmed by observing the central artery in retinae using an ophthalmoscope (HEINE K180®, Heine Optotechnik, Herrsching, Germany). After 2 min for IPC and 5 min of occlusion for LI, the aneurysm clips were removed from the common carotid arteries. Body (rectal) temperature was maintained under free-regulating or normothermic (37 ± 0.5 °C) conditions with a rectal temperature probe (TR-100; Fine Science Tools, Foster City, CA) and a thermometric blanket before, during and after the surgery until the animals completely recovered from anesthesia. Thereafter, the animals were kept in a thermal incubator (temperature, 23 °C; humidity, 60 %) (Mirae Medical Industry, Seoul, South Korea) to maintain the body temperature until the animals were euthanized.
Tissue Processing for Histology
As previously described [32], the animals (n = 7 at each point in time in each group) were anesthetized with pentobarbital sodium at the designated times and perfused transcardially with 0.1 M phosphate-buffered saline (PBS, pH 7.4) followed by 4 % paraformaldehyde in 0.1 M phosphate-buffer (PB, pH 7.4). The brain tissues were serially sectioned into 30-μm coronal sections and then collected into six-well plates containing PBS.
Staining for Cellular Change
Cresyl Violet Staining
As previously described [33], this staining was performed for cellular distribution. In brief, the sections were stained with 1.0 % (w/v) cresyl violet acetate (Sigma-Aldrich) and dehydrated. They were then mounted with Canada balsam (Kanto chemical, Tokyo, Japan).
Neuronal Nuclei Immunohistochemistry
This was performed to examine neuronal change according to our published procedure [33]. In brief, the sections were incubated with primary mouse anti-neuronal nuclei (NeuN, a neuron-specific soluble nuclear antigen) (diluted 1:1000, Chemicon International, Temecula, CA, USA) by incubating the secondary antibodies (Vector Laboratories Inc., Burlingame, CA, USA) and were developed using Vectastain ABC (Vector Laboratories Inc.). And they were visualized with 3,3′-diaminobenzidine.
Fluoro-Jade B Histofluorescence Staining
For neuronal damage/death, F-J B histofluorescence staining was performed according to a published procedure [34]. Briefly, the sections were immersed in a 0.0004 % F-J B (Histochem, Jefferson, AR, USA) staining solution. After washing, the sections were examined using an epifluorescent microscope (Carl Zeiss, Göttingen, Germany) with blue (450–490 nm) excitation light and a barrier filter.
Cell Counting
The sections were selected according to anatomical landmarks corresponding to AP from −1.4 to −1.8 mm of the gerbil brain atlas. NeuN- and F-J B-positive cells were taken through an AxioM1 light microscope (Carl Zeiss) equipped with a digital camera (Axiocam, Carl Zeiss) connected to a PC monitor. NeuN-immunoreactive and F-J B-positive cells were counted in a 200 × 200 μm square including the stratum pyramidale applied approximately at the center of the CA1 region, and the cell counts were obtained by averaging the total cell numbers from 20 sections taken from each animal per group.
Immunohistochemistry for HIF-1α, VEGF, and NF-κB p65
Immunohistochemical staining was carried out according to our published procedure [33]. The sections were incubated with primary mouse anti-HIF-1α (diluted 1:500, Abcam Incorporated, Cambridge, MA, USA), mouse anti-VEGF (diluted 1:500, Abcam Incorporated), and rabbit anti-NF-κB p65 (diluted 1:100, Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA) followed by incubating the secondary antibodies (Vector Laboratories Inc., Burlingame, CA, USA) and were developed using Vectastain ABC (Vector Laboratories Inc.). And they were visualized with 3,3′-diaminobenzidine. To analyze their immunoreactivity, digital images of the hippocampal CA1 area were captured with an AxioM1 light microscope (Carl Zeiss) equipped with a digital camera (Carl Zeiss) connected to a PC monitor. The images were calibrated into an array of 512 × 512 pixels corresponding to a tissue area of 140 × 140 μm (×40 primary magnification). Their immunoreactivity was measured by a 0–255 Gy scale system. Relative immunoreactivity in cells was calibrated as percent using Adobe Photoshop version 8.0 and then analyzed using NIH Image 1.59 software. A ratio of the relative immunoreactivity was calibrated as percent.
Double Immunofluorescence Staining
To confirm the cell type containing HIF-1α, VEGF, and NF-κB p65 immunoreactivity, the sections were processed by double immunofluorescence staining according to our published procedure [32]. In brief, double immunofluorescence staining was performed using mouse anti-HIF-1α (diluted 1:50, Abcam Incorporated) or mouse anti-VEGF (diluted 1:50, Abcam Incorporated) or rabbit anti-NF-κB p65 (diluted 1:500, Santa Cruz Biotechnology Inc.) /rabbit (or mouse) anti-ionized calcium-binding adapter molecule 1 (Iba-1) (diluted 1:200, Wako, Osaka, Japan) for microglia or rabbit (or mouse) anti-glial fibrillary acidic protein (GFAP) (diluted 1:200, Chemicon International) for astrocytes or rat anti-mouse CD31 (diluted 1:50) for endothelial cells or goat anti-platelet-derived growth factor receptor β (PDGFR-β) (diluted 1:50, Santa Cruz Biotechnology Inc.) for pericytes. The sections were incubated in the mixture of antisera followed by incubating in a mixture of both FITC-conjugated donkey anti-mouse (or rabbit) IgG (diluted 1:200; Jackson ImmunoResearch, West Grove, PA, USA), Cy3-conjugated donkey anti-rabbit (or mouse) IgG (diluted 1:200; Jackson ImmunoResearch), Cy3-conjugated donkey anti-rat IgG (diluted 1:200; Jackson ImmunoResearch), and Cy3-conjugated donkey anti-goat IgG (diluted 1:200; Jackson ImmunoResearch). The immunoreactions were observed under the confocal MS (LSM510 META NLO, Carl Zeiss).
Western Blot Analysis for HIF-1α, VEGF, and p-IκB-α
Animals (n = 7 at each point in time in each group) were sacrificed at designated times (1, 2, and 5 days) after ischemia-reperfusion and used for western blot analysis of HIF-1α, VEGF, and p-IκB-α in the ischemic CA1 region. As previously described [33], briefly, the hippocampal CA1 region was homogenized in 50 mM PBS (pH 7.4) containing 0.1 mM ethylene glycol-bis(2-aminoethylether)-N,N,N′,N′ tetraacetic acid (EGTA) (pH 8.0), 0.2 % Nonidet P-40, 10 mM ethylendiamine tetraacetic acid (EDTA) (pH 8.0), 15 mM sodium pyrophosphate, 100 mM β-glycerophosphate, 50 mM NaF, 150 mM NaCl, 2 mM sodium orthovanadate, 1 mM phenylmethylsulfonyl fluoride (PMSF) and 1 mM dithiothreitol (DTT). The protein level was determined in the supernatants using a Micro BCA protein assay kit with bovine serum albumin as the standard (Pierce Chemical, Rockford, IL, USA). Aliquots containing 20 μg of total protein were boiled in loading buffer containing 150 mM Tris (pH 6.8), 3 mM DTT, 6 % SDS, 0.3 % bromophenol blue, and 30 % glycerol. Then, each aliquot was loaded onto a 12.5 % polyacryamide gel. After electrophoresis, the gels were transferred to nitrocellulose transfer membranes (Pall Crop, East Hills, NY). The membranes were incubated with mouse anti-HIF-1α (diluted 1:1000), mouse anti-VEGF (diluted 1:1000, Chemicon International), and mouse anti-p-IκB-α (diluted 1:1000, Santa Cruz Biotechnology Inc.), respectively, and subsequently exposed to peroxidase-conjugated horse anti-mouse IgG (Santa Cruz Biotechnology Inc.) and an ECL kit (Pierce Chemical). Loading controls were performed using antibodies against beta actin (Abcam Incorporated).
According to our previous method [32], the results of western blot analysis were scanned, and the quantification of the analysis was done using Scion Image software (Scion Corp., Frederick, MD, USA) which was used to count relative optical density (ROD): A ratio of the ROD was calibrated as percent, with sham- or comparative group designated as 100 %.
Statistical Analysis
The estimation of sample size was dependent on the standard deviation as in a published study by Ozkan et al. [35]. Sample size was at least seven gerbils per group with an alpha error of 0.05 and a power of >80 %, and the sample size was calculated with power calculator (UCLA Department of Statistics, http://www.stat.ubc.ca/~rollin/stats/ssize). All data are presented as mean ± SEM. A multiple-sample comparison was applied to test the differences between groups (ANOVA and the Tukey multiple range test as post hoc test using the criterion of the least significant differences). Statistical significance was considered at p < 0.05.
Results
Effects of IPC and IPC+2ME2 on Neurons after LI
CV+ and NeuN+ cells were well detected in all subregions of the hippocampus of the sham-group, and, in this group, no F-J B+ cells were found in any regions of the hippocampus. In particular, neurons in the stratum pyramidale were relatively large, pyramid-like or round in shape (Fig. 1a–d). In the LI-group, the distribution pattern of CV+ and NeuN+ cells were not changed until 2 days after LI, and, in this group, no F-J B+ cells were detected in any regions (Fig. 1e–g). Five days after LI, however, the number of CV+ and NeuN+ neurons was significantly decreased in the stratum pyramidale of the CA1 region, not CA2/3 region (Fig. 1i–k). At this point in time, many F-J B+ cells were found in the stratum pyramidale of the CA1 region (Fig. 1l).
CV staining (left two columns), NeuN immunohistochemistry (third column), and F-J B histofluorescence staining (fourth column) in the hippocampus of the sham-group (first row), at 2 (second row) and 5 days (third row) after LI. Neuronal morphology and number is not changed until 2 days after LI (a–h). Five days after LI, CV+ (asterisk) and NeuN+ (arrows) cells are dramatically decreased in the stratum pyramidale (SP) of the CA1 region, and many F-J B+ cells (asterisk) are shown in the SP of the CA1 region. SO stratum oriens, SR stratum radiatum. Scale bar, a–c = 200 μm, d–l = 50 μm
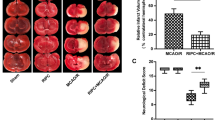
In the (IPC+sham)-group, cellular distribution in the CA1 region was similar to the sham-group (Fig. 2a(a)). In the (IPC + LI)-group, many NeuN+ neurons were detected in the stratum pyramidale of the CA1 region compared to the LI-group, and only a few neurons were positive to F-J B in the CA1 region 5 days after LI (Fig. 2a(f), b, c).
a NeuN immunohistochemistry (first and third columns) and F-J B histofluorescence staining (second and fourth columns) in the stratum pyramidale (SP) of the CA1 region of the sham-group (a–d) and at 5 days (e–h) after LI. In the (IPC+LI)-group, many NeuN+ neurons are shown in the SP and they are maintained until 5 days after LI. In the (IPC+2ME2+LI)-group, a few NeuN+ neurons (arrows) are shown in the SP at 5 days LI, and, at this point in time, many F-J B+ cells are detected in the SP. SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b, c Quantitative analyses of NeuN+ (b) and F-J B+ (c) cells in the CA1 region. Results expressed as mean ± SEM. *p < 0.05 vs sham-group; # p < 0.05 vs pre-time point-group; $ p < 0.05 vs (IPC+LI)-group
In the (IPC+2ME2+sham)-group, distribution patterns of NeuN+ and F-J B+ cells were similar to those in the sham-group (Fig. 2a(c), a(d), b, c). In the (IPC + 2ME2 + LI)-group, however, IPC did not show a significant neuroprotection; numbers of NeuN+ cells were significantly decreased and numbers of F-J B+ cells were significantly increased in the stratum pyramidale of the CA1 region (Fig. 2a(g), a(h), b, c).
Effects of IPC and IPC+2ME2 on HIF-1α Expression After LI
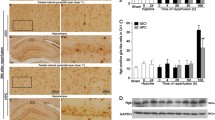
HIF-1α immunoreactivity was hardly detected in the CA1 region of the sham-group (Fig. 3a(a)). In the LI-group, weak HIF-1α immunoreactivity appeared in the stratum pyramidale of the CA1 region 12 h after LI (Fig. 3a(b)). At 1-day post-LI, HIF-1α immunoreactivity was significantly increased in the stratum pyramidale of the CA1 region (Fig. 3a(c)); however, HIF-1α immunoreactivity was not observed in the stratum pyramidale 2 days after LI and newly expressed in cells in the strata oriens and radiatum (Fig. 3a(d)). At 5-day post-LI, HIF-1α immunoreactivity in the cells of the strata oriens and radiatum became much stronger in the immunoreactivity (Fig. 3a(e)). On the other hand, the double-labeling study for HIF-1α+ cells in the strata oriens and radiatum at 5-day post-LI showed that HIF-1α immunoreactivity was co-localized with PDGFR-β, which is a marker for pericytes, immunoreactivity (Fig. 3b); however, HIF-1α immunoreactivity was not found in GFAP+ astrocytes, Iba-1+ microglia, and CD31+ endothelial cells in the CA1 region at any time after LI (data not shown).
a HIF-1α immunohistochemistry in the CA1 region of in the sham-group (a) and LI-group at 12 h (b), 1 day (c), 2 days (d), and 5 days (e) post-LI. HIF-1α immunoreactivity is significantly increased in the stratum pyramidale (SP, asterisks) 1 day after LI and hardly detected at 2-day post-LI. At 5-day post-LI, HIF-1α immunoreactivity is newly expressed in many non-pyramidal cells (arrows). SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b Double immunofluorescence staining for HIF-1α (green, a) and PDGFR-β (red, b), and merged image (c) in the CA1 region at 5-day post-LI. HIF-1α and PDGFR-β co-localizes in non-pyramidal cells. Scale bar=20 μm. c Western blot analysis of HIF-1α in the CA1 region induced by LI. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. sham-group; # p < 0.05 vs pre-time point-group). The bars indicate the means ± SEM
Furthermore, the change pattern of HIF-1α protein level in the CA1 region after LI was generally similar to the change of the immunohistochemical data (Fig. 3c). As shown in Fig. 3c, HIF-1α protein was a little detected in the sham-group; however, HIF-1α protein levels were upregulated in a time-dependent manner following LI and highest 5 days after LI.
HIF-1α immunoreactivity was significantly increased in the stratum pyramidale of the CA1 region of the (IPC+sham)-group compared with the sham-group (Figs. 3a(a), 4a(a)), and the immunoreactivity was maintained in the (IPC+LI)-groups (Fig. 4a(b), (c)). In addition, the levels of HIF-1α protein in the (IPC+LI)-group were similar to the (IPC+sham)-group (Fig. 4b).
a HIF-1α immunohistochemistry in the CA1 region of the (IPC+LI)-group (upper column) and (IPC+2ME2+LI)-group (low column) at sham (a, d), 2 days (b, e) and 5 days (c, f) after LI. In the (IPC+sham)-group, strong HIF-1α immunoreactivity is shown in the stratum pyramidale (SP) and it is maintained until 5-day post-LI. In the (IPC+2ME2+sham)- and (IPC+2ME2+LI)-group, HIF-1α immunoreactivity is distinctively decreased in the SP (asterisks) compared to the (IPC+sham)- and (IPC+LI)-groups, and, HIF-1α immunoreactivity is shown in many non-pyramidal cells (arrows) cells in the (IPC+2ME2+LI)-group at 5-day post-LI. SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b Western blot analysis. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. (IPC+sham)-group; $ p < 0.05 vs (IPC+LI)-group). The bars indicate the means ± SEM
HIF-1α expression in the CA1 region of the (IPC+2ME2+sham)-group was signifcanlty lower than the (IPC+sham)-group (Fig. 4a(d), b). In the (IPC+2ME2+LI)-group, HIF-1α immunoreactivity in the stratum pyramidale was also significantly lower than that in the (IPC+LI)-group; in particular, many non-pyramidal cells in the strata oriens and radiatum showed HIF-1α immunoreactivity at 5-day post-LI (Figs. 4a(e), (f)). In addition, HIF-1α protein levels in the CA1 region of the (IPC+2ME2+LI)-groups were significantly lower than those in the (IPC + LI)-groups (Fig. 4b).
Effects of IPC and IPC+2ME2 on VEGF Expression After LI
Weak VEGF immunoreactivity was detected in the strata pyramidale and radiatum of the CA1 region of the sham-group (Fig. 5a(a)). In the LI-group, VEGF immunoreactivity was increased in the stratum pyramidale at 12-h and 1-day post-LT, although the immunoreactivity in the stratum radiatum was decreased (Fig. 5a(b), (c)). Two days after LI, VEGF immunoreactivity in the stratum pyramidale was decreased compared with that at 1-day post-LI (Fig. 5a(d)). At 5-day post-LI, VEGF immunoreactivity in the stratum pyramidale was more decreased; however, at this point in time, strong VEGF immunoreactivity was newly expressed in non-pyramidal cells in the strata oriens and radiatum (Fig. 5a(e)), and the VEGF+ non-pyramidal cells were identified as PDGFR-β+ pericytes (Fig. 5b), not GFAP+ astrocytes, Iba-1+ microglia, and CD31+ endothelial cells (data not shown). In addition, the level of VEGF in the CA1 region in the LI-group was significantly increased 5 days after LI (Fig. 5c), and, at this point in time, abundant VEGF+ non-pyramidal cells, which were identified as PDGFR-β+ pericytes, were detected and strong in the immunoreactivity (Fig. 5a(e), 5b).
a Immunohistochemistry for VEGF in the CA1 region of the sham-group (a) and LI-group at 12-h (b), 1-day (c), 2-day (d), and 5-day (e) post-LI. One day after LI, VEGF immunoreactivity is increased in the stratum pyramidale (SP, asterisk) and decreased at 5-day post-LI. At 5-day post-LI, VEGF immunoreactivity is expressed in non-pyramidal cells (arrows). SO stratum oriens SR stratum radiatum. Scale bar=50 μm. b Double immunofluorescence staining for VEGF (green, a) and PDGFR-β (red, b) and merged image (c) in the CA1 region at 5-day post-LI. VEGF+ non-pyramidal cells are identified as PDGFR-β+ pericytes. Scale bar=20 μm. c Western blot analysis of VEGF in the CA1 region induced by LI. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. sham-group; # p < 0.05 vs pre-time point-group). The bars indicate the means ± SEM
In the (IPC+sham)-group, VEGF immunoreactivity was significantly increased in the stratum pyramidale compared with that in the sham-group (Figs. 5a(a), 6a(a)). In the (IPC+LI)-group, VEGF immunoreactivity in the stratum pyramidale was similar to that in the (IPC+sham)-group (Fig. 6a(b), (c)). In addition, VEGF protein levels in the (IPC+LI)-group were similar to those in the (IPC+sham)-group (Fig. 6b).
a Immunohistochemistry for VEGF in the CA1 region of the (IPC+LI)-group (upper column) and (IPC+2ME2+LI)-group (low column) at sham (a, d), 2 days (b, e), and 5 days (c, f) after LI. In the (IPC+sham)-group, VEGF immunoreactivity is strong in the stratum pyramidale (SP) and the immunoreactivity is maintained until 5-day post-LI. In the (IPC+2ME2+LI)-group, VEGF immunoreactivity is hardly detected in the SP (asterisk) at 2-day post-LI and VEGF immunoreactivity is newly expressed in many non-pyramidal cells (arrows). SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b Western blot analysis. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. (IPC+sham)-group; # p < 0.05 vs pre-time point-group; $ p < 0.05 vs (IPC+LI)-group). The bars indicate the means ± SEM
In the (IPC+2ME2+sham)-group, VEGF immunoreactivity in the stratum pyramidale was significantly lower than that in the (IPC+sham)-group (Fig. 6a(d)). In the LI-group, VEGF immunoreactivity was hardly detected in the stratum pyramidale at 2-day post-LI (Fig. 6a(e)), and, at 5-day post-LI, many non-pyramidal cells in the strata oriens and radiatum showed VEGF immunoreactivity (Fig. 6a(f)). In addition, VEFG protein levels in the CA1 region of the (IPC+2ME2+LI)-group were significantly low at 2-day post-LI and high at 5-day post-LI compared with the corresponding (IPC+LI)-group (Fig. 6b).
Effects of IPC and IPC+2ME2 on NF-kB p65 or p-IkB-α Expression After LI
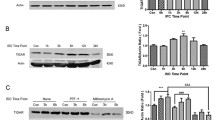
NF-kB p65 immunoreactivity was detected in all layers in the CA1 region of the sham-group (Fig. 7a(a)). In the LI-group, NF-κB p65 immunoreactivity was shown only in the stratum pyramidale at 12-h and 1-day post-LI; at these points in time, NF-κB p65 was found to be translocated into the nuclei (Figs. 7a(b), (c)). However, at 2-day post-LI, NF-κB p65 immunoreactivity was not observed in the stratum pyramidale, and strong NF-κB p65 immunoreactivity was newly expressed in non-pyramidal cells in the strata oriens and radiatum (Fig. 7a(d)). At 5-day post-LI, numbers of NF-κB p65+ non-pyramidal cells were increased in all of the layers (Fig. 7a(e)). In addition, NF-κB p65+ non-pyramidal cells were identified as PDGFR-β+ pericytes at 2- and 5-day post-LI (Fig. 7b), not GFAP+ astrocytes, Iba-1+ microglia, and CD31+ endothelial cells (data not shown), by double immunofluorescence staining. On the other hand, p-IκB-α protein levels in the CA1 region after LI were changed like the NF-κB p65 immunohistochemical data (Fig. 7c). As shown in Fig. 7c, p-IκB-α protein levels were significantly increased at 2- and 5-day post-LI compared with those in the sham-group.
a NF-κB p65 immunohistochemistry in the CA1 region of the sham-group (a) and LI-group at 12-h (b), 1-day (c), 2-day (d), and 5-day (e) post-LI. At 12 h and 1 day after LI, NF-κB p65 immunoreactivity is shown in the nuclei (arrowheads) of the stratum pyramidale (SP). At 2-day post-LI, NF-κB p65 immunoreactivity disappears in the SP (asterisk) and strong NF-κB p65 immunoreactivity is expressed in non-pyramidal cells (arrows). At 5-day post-LI, many NF-κB p65+ non-pyramidal cells (arrows) are distributed throughout all layers. SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b Double immunofluorescence staining for NF-κB p65 (green, a) and PDGFR-β (red, b) and merged image (c) in the CA1 region at 5-day post-LI. NF-κB p65+ non-pyramidal cells are identified as PDGFR-β+ pericytes. Scale bar=20 μm. c Western blot analysis of p-IκB-α in the CA1 region induced by LI. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. sham-group; # p < 0.05 vs pre-time point-group). The bars indicate the means ± SEM
In the (IPC+sham)-group, NF-κB p65 immunoreactivity was shown in the nuclei of pyramidal neurons and significantly higher than that in the sham-group (Figs. 7a(a), 8a(a)). NF-κB p65 immunoreactivity in the (IPC+LI)-group was similar to that in the (IPC+sham)-group (Figs. 8a(b), 8a(c)). On the other hand, levels of p-IκB-α protein in the (IPC+LI)-group were similar to the (IPC+sham)-group and maintained until 5-day post-LI (Fig. 8b).
a NF-κB p65 immunohistochemistry in the CA1 region of the (IPC+LI)-group (upper column) and (IPC+2ME2+LI)-group (low column) at sham (a, d), 2 days (b, e) and 5 days (c, f) after LI. NF-κB p65 immunoreactivity is strong in the stratum pyramidale (SP) of the (IPC+sham)-group and it is maintained until 5-day post-LI. In the (IPC+2ME2+LI)-group, NF-κB p65 immunoreactivity is significantly decreased in the SP (asterisk) compared to the (IPC+LI)-group; however, NF-κB p65 immunoreactivity is newly expressed in many non-pyramidal cells (arrows) at 5-day post-LI. SO stratum oriens, SR stratum radiatum. Scale bar=50 μm. b Western blot analysis for p-IκB-α protein. ROD as percent values of immunoblot band is represented (*p < 0.05 vs. (IPC+sham)-group; # p < 0.05 vs pre-time point-group; $ p < 0.05 vs (IPC+LI)-group). The bars indicate the means ± SEM
In the (IPC+2ME2+sham)-group, NF-κB p65 immunoreactivity in the stratum pyramidale was lower than that in the (IPC+sham)-group (Fig. 8a(d)). In the (IPC+2ME2+LI)-group, NF-κB p65 immunoreactivity was hardly detected in the stratum pyramidale (Figs. 8a(e), (f)), and many non-pyramidal cells showed NF-κB p65 immunoreactivity at 5-day post-LI (Fig. 8a(f)). On the other hand, p-IκB-α protein levels in the (IPC+2ME2+LI)-groups were significantly lower than those in the (IPC+LI)-group (Fig. 8b).
Discussion
Transient cerebral ischemia results in oxygen and glucose deprivation of brain tissues and leads to irreversible brain damage [36]. Gerbils have been used as a suitable animal model to investigate molecular mechanisms of selective neuronal damage/death after transient cerebral ischemia because about 90 % of the gerbils anatomically lack the communicating arteries between the carotid and vertebral circulations [37, 38]. Thus, the transient occlusion of both common carotid arteries evokes transient ischemic insult in the forebrain while the vegetative centers of the brainstem completely are intact.
It is well known that pyramidal neurons in the gerbil hippocampal CA1 region die 4–5 days after 5 min of transient cerebral ischemia [30, 39]. In the present study, we found the same result using CV staining, NeuN immunohistochemistry, and F-J B histofluorescence staining in the LI-group; in this group, HIF-1α immunoreactivity was significantly increased in the CA1 pyramidal neurons at 1-day post-LI, disappeared from 2-day post-LI, and newly expressed in pericytes from 2-day post-LI. On the other hand, we found the IPC-mediated neuroprotection of the CA1 pyramidal neurons in the (IPC+LI)-group like previous studies using gerbils [28, 33] and, in this group, HIF-1α immunoreactivity was significantly increased in the CA1 pyramidal neurons; however, IPC-mediated neuroprotection was gone in the (IPC+2ME2+LI)-group as well as HIF-1α immunoreactivity in the CA1 pyramidal neurons was significantly increased. On the basis of our present finding, the disappearance of HIF-1α immunoreactivity from 2-day post-LI is related with the death of CA1 pyramidal neurons and IPC-mediated neuroprotection in the (IPC+LI)-group is strongly related with the upregulation of HIF-1α following IPC.
It has been demonstrated that the upregulation or stabilization of HIF-1 reduces brain damage and improves functional impairments induced by ischemic insults in vivo and in vitro [40, 41]. To the contrary, Chen et al. [8] demonstrated that HIF-1α inhibition after cerebral ischemia ameliorated neonatal brain injury in a rat pup hypoxic-ischemic model. In addition, the neuron-specific knockdown of HIF-1α aggravates brain injury in a mouse model of transient focal cerebral ischemia [42]. On the other hand, it was reported that HIF-1α upregulation after hypoxic preconditioning provided neuroprotection to subsequent ischemic insults in vivo [6, 43] and that, however, HIF-1α increase after ischemic insult without any preconditioning actually promoted cell death [7]. Furthermore, Vangeison et al. [44] demonstrated that the selective loss of HIF-1α function in astrocytes markedly protected neurons from hypoxia-induced neuronal death, whereas a loss of HIF-1α function in neurons increased neuronal susceptibility to hypoxia-induced damage. In our present study, HIF-1α immunoreactivity in the CA1 pyramidal neurons was hardly detected from 2-day post-LI in the LI-group; thereafter, HIF-1α immunoreactivity was newly expressed in pericytes and significantly increased until 5-day post-LI. Therefore, we suggest that HIF-1α expression could be cell-type specific according to pathological conditions and needs to prudently examine roles of HIF-1α in different cell types for divergent results from various pathological conditions. Anyway, on the basis of our own and other findings, the activation of the genes by HIF-1 can lead to either pro-survival or pro-death effect, which is important for the development of novel therapeutic interventions; targets of HIF-1 include genes that code for molecules participating in cell survival through HIF-1-mediated functions, such as oxygen transport, vasomotor control, pH regulation, and energy metabolism [6, 45].
It has been reported that VEGF stimulates axonal outgrowth and increases the survival of mouse superior cervical and dorsal root ganglion cells [46] and that VEGF promotes the survival of rat mesencephalic neurons in culture [47]. In addition, VEGF possesses neurotrophic and neuroprotective activity, and the direct neurotrophic effect of VEGF could confer the neuroprotection independent of angiogenesis [48, 49]. Furthermore, it has been demonstrated that the induction of endogenous VEGF directly plays a neuroprotective role against cerebral ischemia [50, 51] and that the neuroprotective mechanism of VEGF may be related with angiogenesis [52] or vessel protection [51]. Recently, VEGF is considered one of the possible endogenous molecules of tolerance to hypoxic ischemia induced by various preconditionings [19, 53–55]. Our present results show that VEGF protein levels were changed like changes in HIF-1α in the LI- and the (IPC+LI)-group and that the effects by IPC were abolished by pre-treatment with HIF-1α inhibitor. Therefore, our findings suggest that the upregulation of HIF-1α by IPC is associated with the increase of VEGF level and the protection of neuronal death in hippocampal CA1 region after ischemia-reperfusion.
It has been reported that, in animal models of focal and global cerebral ischemia, VEGF is expressed in neurons, glial, and endothelial cells [18, 56]. We, in this study, show that VEGF immunoreactivity was increased in the CA1 stratum pyramidale after ischemia and disappeared at 5-day post-ischemia; at this point in time, however, VEGF was newly expressed in pericytes stained with PDGFR-β in the strata oriens and radiatum. Pericytes are a major component of BBB ([57]. Although we cannot exactly explain what increases BBB permeability in the damaged brain, it needs to be studied whether VEGF-mediated neuroprotection in the brain with ischemic insults is associated with BBB permeability. It was demonstrated that VEGF promoted vascular permeability in the brain by altering tight junction proteins under ischemic condition [58]. In addition, Yeh et al. [59] reported that the inhibition of HIF-1 reduced VEGF expression in brain microvessels, which was upregulated by ischemia and subsequently reduced BBB permeability.
In our present study, we found that VEGF immunoreactivity was increased in the stratum pyramidale of the (IPC+sham)-group and intensely maintained in the (IPC+LI)-group until 5 days after ischemic insult. In addition, our important finding is that all VEGF+ cells are co-localized with HIF-1α+ cells; in particular, most of IPC-mediated survived CA1 pyramidal neurons expressed strong HIF-1α and VEGF immunoreactivity, which were not observed in damaged CA1 pyramidal neurons. These results are robust in supporting the concept that HIF-1α activation is significantly correlated with VEGF expression in the CA1 pyramidal neurons followed by IPC. Some researchers have shown that HIF-1α and VEGF was upregulated in neuronal cells after neonatal brain injury [60, 61]. Recently, Ara et al. [62] reported that hypoxic preconditioning resulted in an increased expression of VEGF in neurons, astrocytes, and endothelial cells after hypoxia–ischemia in neonatal piglet brain. Furthermore, some previous studies showed that neuroprotection by hypoxic preconditioning required a sequential activation of VEGFR and Akt [63] and that exogenous as well as endogenous VEGF reduced excitotoxic lesions in the brain of the developing mouse, and the VEGF/VEGFR2/Flk1 pathway was involved in neuroprotective response to hypoxic preconditioning [53]. Taken together, those and our results suggest that increased VEGF expression following IPC could reflect a mechanism of neuronal survival from ischemia-induced death.
NF-κB is activated under IPC in the brain [20, 64] and/or ischemia in the brains [7]. The activation of NF-κB in damaged neurons promotes their survival and plasticity, whereas NF-κB activation in glial cells enhances neuronal death [7]. In addition, it has been suggested that the activation of NF-κB is strongly involved in the induction of gene expression associated with IPC [65, 66]. Thus, NF-κB expressed cell type is important for neuronal survival or death in brain ischemia. In present study, NF-κB p65 immunoreactivity was increased in CA1 pyramidal neurons 1 day after LI and disappeared from 2 days after LI, and strong NF-κB p65 immunoreactivity was newly expressed in pericytes in strata oriens and radiatum from 2 days LI. On the other hand, we found that IPC induced a clear upregulation of p-IκB-α in the CA1 pyramidal neurons of the (IPC+sham)-group and maintained until 5 days after LI. In addition, the elevated expressions of p-IκB-α and translocation of NF-κB p65 into nuclei were reversed by the HIF-1α inhibitor 2ME2. Therefore, we, in this study, suggest that the neuronal activation of NF-κB is an important axis of IPC-mediated neuroprotective mechanism.
Walmsley et al. [67] previously reported that hypoxia-induced neutrophil survival in an in vitro system was mediated by HIF-1α-dependent NF-κB activity, and it was demonstrated that HIF-1α and NF-κB were important in various pathological conditions including ischemia [24]. However, defining the relationship between HIF-1α and NF-κB in cerebral ischemia with IPC has proved elusive. A global understanding of HIF-1α and NF-κB crosstalk is challengeable because the engagement of different signaling pathways to NF-κB from HIF-1 and vice versa is very complicated according to cell-type specificity [24]. To the best of knowledge, studies regarding NF-κB and HIF-1α relationship in IPC or ischemia with IPC are rare and still remain unclear in those conditions. In our present study, the inhibition of HIF-1α with 2ME2 removed the neuroprotective effect of IPC and significantly decreased the expressions of VEGF and p-IκB-α, which were significantly increased in the CA1 pyramidal neurons following IPC. Therefore, we strongly suggest that HIF-1α might mediate the expression of VEGF via NF-κB and contribute to neuronal survival of the ischemic hippocampal CA1 region followed by IPC.
In brief, our results provide some novel evidences that IPC-induced neuroprotective effect after a lethal ischemia-reperfusion is mediated, in part, by the upregulation of HIF-1α, which enhances VEGF expression and NF-κB activity in pyramidal neurons of the hippocampal CA1 region induced by a subsequent lethal transient cerebral ischemia.
References
Semenza GL (1998) Hypoxia-inducible factor 1: master regulator of O2 homeostasis. Current opinion in genetics & development 8(5):588–594
Xiong L, Zhu Z, Dong H, Hu W, Hou L, Chen S (2000) Hyperbaric oxygen preconditioning induces neuroprotection against ischemia in transient not permanent middle cerebral artery occlusion rat model. Chin Med J 113(9):836–839
Prabhakar NR, Semenza GL (2012) Adaptive and maladaptive cardiorespiratory responses to continuous and intermittent hypoxia mediated by hypoxia-inducible factors 1 and 2. Physiol Rev 92(3):967–1003. doi:10.1152/physrev.00030.2011
Wang GL, Jiang BH, Rue EA, Semenza GL (1995) Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci U S A 92(12):5510–5514
Jones NM, Lee EM, Brown TG, Jarrott B, Beart PM (2006) Hypoxic preconditioning produces differential expression of hypoxia-inducible factor-1alpha (HIF-1alpha) and its regulatory enzyme HIF prolyl hydroxylase 2 in neonatal rat brain. Neurosci Lett 404(1–2):72–77. doi:10.1016/j.neulet.2006.05.049
Sharp FR, Bernaudin M (2004) HIF1 and oxygen sensing in the brain. Nat Rev Neurosci 5(6):437–448. doi:10.1038/nrn1408
Chang YC, Huang CC (2006) Perinatal brain injury and regulation of transcription. Curr Opin Neurol 19(2):141–147. doi:10.1097/01.wco.0000218229.73678.a8
Chen C, Hu Q, Yan J, Lei J, Qin L, Shi X, Luan L, Yang L et al (2007) Multiple effects of 2ME2 and D609 on the cortical expression of HIF-1alpha and apoptotic genes in a middle cerebral artery occlusion-induced focal ischemia rat model. J Neurochem 102(6):1831–1841. doi:10.1111/j.1471-4159.2007.04652.x
Aminova LR, Siddiq A, Ratan RR (2008) Antioxidants, HIF prolyl hydroxylase inhibitors or short interfering RNAs to BNIP3 or PUMA, can prevent prodeath effects of the transcriptional activator, HIF-1alpha, in a mouse hippocampal neuronal line. Antioxid Redox Signal 10(12):1989–1998. doi:10.1089/ars.2008.2039
Salhanick SD, Belikoff B, Orlow D, Holt D, Reenstra W, Buras JA (2006) Hyperbaric oxygen reduces acetaminophen toxicity and increases HIF-1alpha expression. Acad Emerg Med Off J Soc Acad Emerg Med 13(7):707–714. doi:10.1197/j.aem.2006.01.029
Ferrara N, Davis-Smyth T (1997) The biology of vascular endothelial growth factor. Endocr Rev 18(1):4–25. doi:10.1210/edrv.18.1.0287
Rosenstein JM, Krum JM (2004) New roles for VEGF in nervous tissue—beyond blood vessels. Exp Neurol 187(2):246–253. doi:10.1016/j.expneurol.2004.01.022
Wang Y, Galvan V, Gorostiza O, Ataie M, Jin K, Greenberg DA (2006) Vascular endothelial growth factor improves recovery of sensorimotor and cognitive deficits after focal cerebral ischemia in the rat. Brain Res 1115(1):186–193. doi:10.1016/j.brainres.2006.07.060
Carmeliet P (2003) Angiogenesis in health and disease. Nat Med 9(6):653–660. doi:10.1038/nm0603-653
Zan L, Wu H, Jiang J, Zhao S, Song Y, Teng G, Li H, Jia Y et al (2011) Temporal profile of Src, SSeCKS, and angiogenic factors after focal cerebral ischemia: correlations with angiogenesis and cerebral edema. Neurochem Int 58(8):872–879. doi:10.1016/j.neuint.2011.02.014
Stowe AM, Plautz EJ, Eisner-Janowicz I, Frost SB, Barbay S, Zoubina EV, Dancause N, Taylor MD et al (2007) VEGF protein associates to neurons in remote regions following cortical infarct. Journal of cerebral blood flow and metabolism: official journal of the International Society of Cerebral Blood Flow and Metabolism 27(1):76–85. doi:10.1038/sj.jcbfm.9600320
Marti HH, Risau W (1998) Systemic hypoxia changes the organ-specific distribution of vascular endothelial growth factor and its receptors. Proc Natl Acad Sci U S A 95(26):15809–15814
Lee MY, Ju WK, Cha JH, Son BC, Chun MH, Kang JK, Park CK (1999) Expression of vascular endothelial growth factor mRNA following transient forebrain ischemia in rats. Neurosci Lett 265(2):107–110
Bernaudin M, Nedelec AS, Divoux D, MacKenzie ET, Petit E, Schumann-Bard P (2002) Normobaric hypoxia induces tolerance to focal permanent cerebral ischemia in association with an increased expression of hypoxia-inducible factor-1 and its target genes, erythropoietin and VEGF, in the adult mouse brain. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism 22(4):393–403. doi:10.1097/00004647-200204000-00003
Blondeau N, Widmann C, Lazdunski M, Heurteaux C (2001) Activation of the nuclear factor-kappaB is a key event in brain tolerance. The Journal of neuroscience : the official journal of the Society for Neuroscience 21(13):4668–4677
Simakajornboon N, Gozal E, Gozal D (2001) Developmental patterns of NF-kappaB activation during acute hypoxia in the caudal brainstem of the rat. Brain Res Dev Brain Res 127(2):175–183
Bhakar AL, Tannis LL, Zeindler C, Russo MP, Jobin C, Park DS, MacPherson S, Barker PA (2002) Constitutive nuclear factor-kappa B activity is required for central neuron survival. The Journal of neuroscience : the official journal of the Society for Neuroscience 22(19):8466–8475
Fridmacher V, Kaltschmidt B, Goudeau B, Ndiaye D, Rossi FM, Pfeiffer J, Kaltschmidt C, Israel A et al (2003) Forebrain-specific neuronal inhibition of nuclear factor-kappaB activity leads to loss of neuroprotection. The Journal of neuroscience : the official journal of the Society for Neuroscience 23(28):9403–9408
Gorlach A, Bonello S (2008) The cross-talk between NF-kappaB and HIF-1: further evidence for a significant liaison. The Biochemical journal 412(3):e17–e19. doi:10.1042/BJ20080920
Murry CE, Jennings RB, Reimer KA (1986) Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74(5):1124–1136
Kitagawa K, Matsumoto M, Kuwabara K, Tagaya M, Ohtsuki T, Hata R, Ueda H, Handa N et al (1991) ‘Ischemic tolerance’ phenomenon detected in various brain regions. Brain Res 561(2):203–211
Kirino T, Nakagomi T, Kanemitsu H, Tamura A (1996) Ischemic tolerance. Adv Neurol 71:505–511
Nakamura H, Katsumata T, Nishiyama Y, Otori T, Katsura K, Katayama Y (2006) Effect of ischemic preconditioning on cerebral blood flow after subsequent lethal ischemia in gerbils. Life Sci 78(15):1713–1719. doi:10.1016/j.lfs.2005.08.008
Della-Morte D, Guadagni F, Palmirotta R, Ferroni P, Testa G, Cacciatore F, Abete P, Rengo F et al (2012) Genetics and genomics of ischemic tolerance: focus on cardiac and cerebral ischemic preconditioning. Pharmacogenomics 13(15):1741–1757. doi:10.2217/pgs.12.157
Kirino T (1982) Delayed neuronal death in the gerbil hippocampus following ischemia. Brain Res 239(1):57–69
Shenaq M, Kassem H, Peng C, Schafer S, Ding JY, Fredrickson V, Guthikonda M, Kreipke CW et al (2012) Neuronal damage and functional deficits are ameliorated by inhibition of aquaporin and HIF1alpha after traumatic brain injury (TBI). J Neurol Sci 323(1–2):134–140. doi:10.1016/j.jns.2012.08.036
Lee JC, Kim IH, Park JH, Ahn JH, Cho JH, Cho GS, Tae HJ, Chen BH et al (2015) Ischemic preconditioning protects hippocampal pyramidal neurons from transient ischemic injury via the attenuation of oxidative damage through upregulating heme oxygenase-1. Free Radic Biol Med 79:78–90. doi:10.1016/j.freeradbiomed.2014.11.022
Lee JC, Kim IH, Cho GS, Park JH, Ahn JH, Yan BC, Kwon HM, Kim YM et al (2014) Ischemic preconditioning-induced neuroprotection against transient cerebral ischemic damage via attenuating ubiquitin aggregation. J Neurol Sci 336(1–2):74–82. doi:10.1016/j.jns.2013.10.010
Schmued LC, Hopkins KJ (2000) Fluoro-Jade B: a high affinity fluorescent marker for the localization of neuronal degeneration. Brain Res 874(2):123–130
Ozkan A, Sen HM, Sehitoglu I, Alacam H, Guven M, Aras AB, Akman T, Silan C et al (2015) Neuroprotective effect of humic acid on focal cerebral ischemia injury: an experimental study in rats. Inflammation 38(1):32–39. doi:10.1007/s10753-014-0005-0
Kirino T, Sano K (1984) Selective vulnerability in the gerbil hippocampus following transient ischemia. Acta Neuropathol 62(3):201–208
Janac B, Radenovic L, Selakovic V, Prolic Z (2006) Time course of motor behavior changes in Mongolian gerbils submitted to different durations of cerebral ischemia. Behav Brain Res 175(2):362–373. doi:10.1016/j.bbr.2006.09.008
Selakovic V, Korenic A, Radenovic L (2011) Spatial and temporal patterns of oxidative stress in the brain of gerbils submitted to different duration of global cerebral ischemia. International journal of developmental neuroscience: the official journal of the International Society for Developmental Neuroscience 29(6):645–654. doi:10.1016/j.ijdevneu.2011.02.009
Lee JC, Ahn JH, Kim IH, Park JH, Yan BC, Cho GS, Ohk TG, Park CW et al (2014) Transient ischemia-induced change of CCR7 immunoreactivity in neurons and its new expression in astrocytes in the gerbil hippocampus. J Neurol Sci 336(1–2):203–210. doi:10.1016/j.jns.2013.10.041
Freret T, Valable S, Chazalviel L, Saulnier R, Mackenzie ET, Petit E, Bernaudin M, Boulouard M et al (2006) Delayed administration of deferoxamine reduces brain damage and promotes functional recovery after transient focal cerebral ischemia in the rat. Eur J Neurosci 23(7):1757–1765. doi:10.1111/j.1460-9568.2006.04699.x
Prass K, Ruscher K, Karsch M, Isaev N, Megow D, Priller J, Scharff A, Dirnagl U et al (2002) Desferrioxamine induces delayed tolerance against cerebral ischemia in vivo and in vitro. Journal of cerebral blood flow and metabolism: official journal of the International Society of Cerebral Blood Flow and Metabolism 22(5):520–525. doi:10.1097/00004647-200205000-00003
Baranova O, Miranda LF, Pichiule P, Dragatsis I, Johnson RS, Chavez JC (2007) Neuron-specific inactivation of the hypoxia inducible factor 1 alpha increases brain injury in a mouse model of transient focal cerebral ischemia. The Journal of neuroscience : the official journal of the Society for Neuroscience 27(23):6320–6332. doi:10.1523/JNEUROSCI.0449-07.2007
Bergeron M, Gidday JM, Yu AY, Semenza GL, Ferriero DM, Sharp FR (2000) Role of hypoxia-inducible factor-1 in hypoxia-induced ischemic tolerance in neonatal rat brain. Ann Neurol 48(3):285–296
Vangeison G, Carr D, Federoff HJ, Rempe DA (2008) The good, the bad, and the cell type-specific roles of hypoxia inducible factor-1 alpha in neurons and astrocytes. The Journal of neuroscience: the official journal of the Society for Neuroscience 28(8):1988–1993. doi:10.1523/JNEUROSCI.5323-07.2008
Semenza GL (2003) Targeting HIF-1 for cancer therapy. Nat Rev Cancer 3(10):721–732. doi:10.1038/nrc1187
Sondell M, Lundborg G, Kanje M (1999) Vascular endothelial growth factor has neurotrophic activity and stimulates axonal outgrowth, enhancing cell survival and Schwann cell proliferation in the peripheral nervous system. The Journal of neuroscience : the official journal of the Society for Neuroscience 19(14):5731–5740
Silverman WF, Krum JM, Mani N, Rosenstein JM (1999) Vascular, glial and neuronal effects of vascular endothelial growth factor in mesencephalic explant cultures. Neuroscience 90(4):1529–1541
Sun Y, Jin K, Xie L, Childs J, Mao XO, Logvinova A, Greenberg DA (2003) VEGF-induced neuroprotection, neurogenesis, and angiogenesis after focal cerebral ischemia. J Clin Invest 111(12):1843–1851. doi:10.1172/JCI17977
Han MK, Kim M, Bae SY, Kang L, Han SY, Lee YS, Rha JH, Kim SU et al (2004) VEGF protects human cerebral hybrid neurons from in vitro ischemia. Neuroreport 15(5):847–850
Jin KL, Mao XO, Greenberg DA (2000) Vascular endothelial growth factor: direct neuroprotective effect in in vitro ischemia. Proc Natl Acad Sci U S A 97(18):10242–10247
Hayashi T, Abe K, Itoyama Y (1998) Reduction of ischemic damage by application of vascular endothelial growth factor in rat brain after transient ischemia. Journal of cerebral blood flow and metabolism: official journal of the International Society of Cerebral Blood Flow and Metabolism 18(8):887–895. doi:10.1097/00004647-199808000-00009
Cobbs CS, Chen J, Greenberg DA, Graham SH (1998) Vascular endothelial growth factor expression in transient focal cerebral ischemia in the rat. Neurosci Lett 249(2–3):79–82
Laudenbach V, Fontaine RH, Medja F, Carmeliet P, Hicklin DJ, Gallego J, Leroux P, Marret S et al (2007) Neonatal hypoxic preconditioning involves vascular endothelial growth factor. Neurobiol Dis 26(1):243–252. doi:10.1016/j.nbd.2006.12.020
Lee HT, Chang YC, Tu YF, Huang CC (2009) VEGF-A/VEGFR-2 signaling leading to cAMP response element-binding protein phosphorylation is a shared pathway underlying the protective effect of preconditioning on neurons and endothelial cells. The Journal of neuroscience: the official journal of the Society for Neuroscience 29(14):4356–4368. doi:10.1523/JNEUROSCI.5497-08.2009
Feng Y, Rhodes PG, Bhatt AJ (2010) Hypoxic preconditioning provides neuroprotection and increases vascular endothelial growth factor A, preserves the phosphorylation of Akt-Ser-473 and diminishes the increase in caspase-3 activity in neonatal rat hypoxic-ischemic model. Brain Res 1325:1–9. doi:10.1016/j.brainres.2010.02.029
Lennmyr F, Ata KA, Funa K, Olsson Y, Terent A (1998) Expression of vascular endothelial growth factor (VEGF) and its receptors (Flt-1 and Flk-1) following permanent and transient occlusion of the middle cerebral artery in the rat. J Neuropathol Exp Neurol 57(9):874–882
Liu S, Agalliu D, Yu C, Fisher M (2012) The role of pericytes in blood-brain barrier function and stroke. Curr Pharm Des 18(25):3653–3662
Zhang ZG, Zhang L, Jiang Q, Zhang R, Davies K, Powers C, Bruggen N, Chopp M (2000) VEGF enhances angiogenesis and promotes blood-brain barrier leakage in the ischemic brain. J Clin Invest 106(7):829–838. doi:10.1172/JCI9369
Yeh WL, Lu DY, Lin CJ, Liou HC, Fu WM (2007) Inhibition of hypoxia-induced increase of blood-brain barrier permeability by YC-1 through the antagonism of HIF-1alpha accumulation and VEGF expression. Mol Pharmacol 72(2):440–449. doi:10.1124/mol.107.036418
Mu D, Jiang X, Sheldon RA, Fox CK, Hamrick SE, Vexler ZS, Ferriero DM (2003) Regulation of hypoxia-inducible factor 1alpha and induction of vascular endothelial growth factor in a rat neonatal stroke model. Neurobiol Dis 14(3):524–534
Kaur C, Sivakumar V, Zhang Y, Ling EA (2006) Hypoxia-induced astrocytic reaction and increased vascular permeability in the rat cerebellum. Glia 54(8):826–839. doi:10.1002/glia.20420
Ara J, Fekete S, Frank M, Golden JA, Pleasure D, Valencia I (2011) Hypoxic-preconditioning induces neuroprotection against hypoxia-ischemia in newborn piglet brain. Neurobiol Dis 43(2):473–485. doi:10.1016/j.nbd.2011.04.021
Wick A, Wick W, Waltenberger J, Weller M, Dichgans J, Schulz JB (2002) Neuroprotection by hypoxic preconditioning requires sequential activation of vascular endothelial growth factor receptor and Akt. The Journal of neuroscience : the official journal of the Society for Neuroscience 22(15):6401–6407
Hagberg H, Mallard C (2005) Effect of inflammation on central nervous system development and vulnerability. Curr Opin Neurol 18(2):117–123
Wilhide ME, Tranter M, Ren X, Chen J, Sartor MA, Medvedovic M, Jones WK (2011) Identification of a NF-kappaB cardioprotective gene program: NF-kappaB regulation of Hsp70.1 contributes to cardioprotection after permanent coronary occlusion. J Mol Cell Cardiol 51(1):82–89. doi:10.1016/j.yjmcc.2011.03.011
Kim EJ, Raval AP, Hirsch N, Perez-Pinzon MA (2010) Ischemic preconditioning mediates cyclooxygenase-2 expression via nuclear factor-kappa B activation in mixed cortical neuronal cultures. Transl Stroke Res 1(1):40–47
Walmsley SR, Print C, Farahi N, Peyssonnaux C, Johnson RS, Cramer T, Sobolewski A, Condliffe AM et al (2005) Hypoxia-induced neutrophil survival is mediated by HIF-1alpha-dependent NF-kappaB activity. J Exp Med 201(1):105–115
Acknowledgments
The authors would like to thank Mr. Seung Uk Lee for his technical help in this study. This work was supported by the Bio & Medical Technology Development Program of the NRF funded by the Korean government, MSIP (NRF-2015M3A9B6066835), by the National Research Foundation of Korea (NRF-2013M3A9B6046563), which was funded by the Ministry of Science, ICT, and Future Planning, and by Bio-Synergy Research Project (NRF-2015M3A9C4076322) of the Ministry of Science, ICT and Future Planning through the National Research Foundation.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
Jae-Chul Lee and Hyun-Jin Tae contributed equally to this article.
Rights and permissions
About this article
Cite this article
Lee, JC., Tae, HJ., Kim, I.H. et al. Roles of HIF-1α, VEGF, and NF-κB in Ischemic Preconditioning-Mediated Neuroprotection of Hippocampal CA1 Pyramidal Neurons Against a Subsequent Transient Cerebral Ischemia. Mol Neurobiol 54, 6984–6998 (2017). https://doi.org/10.1007/s12035-016-0219-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-0219-2