Abstract
Intracerebral hemorrhage (ICH) is a serious emergency with high mortality and morbidity. Up to date, a limited understanding of ICH pathogenesis is difficult to implement effective therapeutic strategy. Much evidence demonstrates that the complement cascade is activated after experimental ICH. However, the exact mechanism has not been well studied in ICH. In the current study, C57BL/6J mice were injected with autologous whole blood. C5a/C5aR levels, microglia infiltration, inflammatory cytokine, and fibrinogen-like protein 2 (Fgl-2) expression in the perihematomal region were analyzed following ICH. In addition, brain water content and neurological dysfunction were detected following ICH. Our data demonstrated that ICH induced complement activation, along with an increase of C5a/C5aR levels, microglia infiltration, and inflammatory cytokine levels. However, C5aR−/− mice exhibited significant attenuation of inflammatory reaction, accompanied by a remarkable reduction of Fgl-2, brain water content, and neurological dysfunction. Furthermore, inhibiting extracellular signal-regulated kinase 1/2 (ERK1/2) and p38 efficiently inhibited C5a-mediated Fgl-2 production following ICH. Taken together, these data suggest that C5a/C5aR plays a vital role in the ICH-induced inflammatory damage via Fgl-2, and ERK1/2 and p38 pathways also are involved in the pathogenesis of ICH. Therefore, inhibition of C5a/C5aR activation might enlarge our insights in ICH therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intracerebral hemorrhage (ICH) accounts for 15 % of all stroke subtypes and is associated with high mortality rates about 50 %, and survivors are often living with serious disability [1–3]. After ICH, the brain responds to ICH in complicated pathophysiological ways, such as excitotoxicity, free radical damage, and inflammatory response [4–6].
The complement system is a vital self-defense immune system [7–9]. Complement activation contributes to macrophage activation, opsonization, and phagocytosis of heterogenous cells and exogenous bacteria [10–12]. Complement activation and subsequent brain damage have been found in various central nervous system diseases, including ischemia stroke, brain trauma, and subarachnoid hemorrhage [13–15].
The C5a fragment is the robust proinflammatory factor produced during complement activation, exerting its biological functions through interaction with its specific receptor C5aR [16–18]. A large number of evidence suggest that excessive activation of the complement system leads to production of proinflammatory C5a, which can exaggerate the inflammatory response [19, 20]. In sepsis and experimental cerebral malaria animal models, blocking of C5a/C5aR interactions prevents damages to host organs and improves survival rates, implicating that complement activation can promote the disease severity [21–23].
The purpose of the present study is to investigate whether C5a/C5aR pathway contributes to inflammatory injury after ICH. Our data provide the evidence that C5a/C5aR mediated brain inflammatory after ICH, which involved the mitogen-activated protein kinase (MAPK) signaling pathway in regulating the production and accumulation of fibrinogen-like protein 2 (Fgl-2) in the brain tissue. Our results also represent the therapeutic strategy for stroke and other types of brain damage, particularly traumatic brain injury which is associated with ICH and the underlying inflammatory secondary injury.
Materials and Methods
Mice
Female C5aR KO mice (C5aR−/−) and female C5aR wild-type (WT) mice (WT) were purchased from the Jackson Laboratory (Bar Harbor, ME, USA). Mice were maintained in microisolator cages, fed with standard laboratory chow diet and water, and housed in the animal colony at the animal center of Fuzhou Medical University. Mice of 12 weeks of age were used for experiments. Mice were divided into four groups: (1) C5aR KO mice (sham), (2) C5aR KO mice (ICH), (3) C5aR WT mice (sham), and (4) C5aR WT mice (ICH) (n = 10 per group). All of the in vivo experiments comply with the animal study protocol approved by the ethics committee of Fuzhou Medical University.
ICH Model
Mice were anesthetized with 10 % chloral hydrate (350 mg/kg) and were placed in a stereotaxic frame (Alcott Biotech, Shanghai, China). Through a hole drilled in the skull, a 32-gauge needle was implanted into the striatum, 2.0 mm lateral to the midline, 1.0 mm anterior to the coronal suture, and at a depth of 4.0 mm from the surface of the brain. Each mouse was microinjected with 25 μl of autologous whole blood (right striatum) taken from the tail vein over 10 min using a microinfusion pump (ALC-IP600, Alcott Biotech). Then, the needle was pulled out without blood reflux after 5 min of dwelling, and the wound was sutured. Only the mouse observed to have a neurological deficit was regarded as a successful model. The mice in the sham operation group had the same operation, but no blood was injected.
Immunochemistry Staining
Mice were anesthetized at each of the following time points: 1, 3, and 5 days after injection. Mice were directly decapitated, and their brains were obtained to store at −80 °C for use for further analysis. These mice underwent transcardial perfusion with 200 ml of phosphate-buffered saline (PBS), followed by 100 ml of 4 % paraformaldehyde (PFA) in 0.1 M PBS. The brains were removed and postfixed for 24 h in 4 % PFA and then were placed in 30 % sucrose until sinking. Coronal brain sections of 10 μm thickness were obtained with a freezing microtome (Leica, Nussloch, Germany) and were kept at −20 °C for immunofluorescence. After being washed in PBS for 10 min, the sections were incubated with 5 % bovine serum albumin for 60 min in order to block the nonspecific binding and then were incubated with goat anti-mouse ionized calcium-binding adapter molecule 1 (Iba-1) primary antibody (1:100; R&D Systems, Minneapolis, MN, USA) at 4 °C all the night. After being washed three times with PBS, the sections were incubated with secondary antibody IgG (1:100; KPL, MD, USA) for 60 min at the room temperature. The sections were rinsed three times for 5 min and were cover slipped with a ProLong antifade medium (Molecular Probes, Eugene, OR, USA). The Iba-1-positive cells were visualized using a microscope (Olympus BX51, Japan). For each animal, six representative sections of each brain were selected. IPP6.0 image processing software (Media Cybernetics, MD, USA) was utilized to count the number of positive cells.
Real-Time PCR
Total RNA was isolated tissue using TRIzol Reagent according to the manufacturer’s protocol (Invitrogen). RNA was reversely transcribed using SuperScript First-Strand cDNA System (Invitrogen) according to the manufacturer’s instructions. Quantitative real-time PCR was performed with Taq polymerase (SYBR Premix Ex Taq II; Takara Biotechnology) in a final volume of 20 μl containing 0.5 μg of total RNA with SYBR Green PCR supermix (Takara Biotechnology), in accordance with the manufacturer’s instructions. Quantitative real-time PCR conditions were as follows: initial denaturation at 94 °C for 5 min, 40 cycles with denaturation at 94 °C for 5 s, and annealing at 60 °C for 20 s, followed by melting curve analysis. The transcript amount of the β-actin housekeeping gene was quantified as an internal RNA control. Primers were purchased from BioAsia Corp. (Shanghai, China). The primers for C5a were sense 5′-CGCCAGCTGCTAAGGCAGAAAATAGAAG-3′ and anti-sense 5′-CGCGTCGACTTACCTTCCCAGTTGGACAGG-3′. The primers for C5aR were 5′-GAC CCC ATAGAT AAC AGC A-3′ and anti-sense 5′-CAG AGG CAACAC AAAACC CA-3′. The primers for Fgl-2 were sense 5′-T GGACAA CA AAGT GGCA A A TCT-3′ and anti-sense 5′-TG GAA CA CT TG CC AT C CAA A-3′. The primers for TNF-α were sense 5′-CA CGC TCT TC TG TCT ACTGA A C-3′ and anti-sense 5′-AT CT GAG TG TGA GG G T C T GG-3′. The primers for IL-6 were 5′-AGCATACA GTTT GT GG ACATT-3′ and anti-sense 5′-CAACATTCATATTGCCAGTTCT-3′. The primers for IL-1β were 5′-CAG GCAA CCACTTACCTATTTA-3′ and anti-sense 5′-CCATA CACACGGACAACAACTAGAT-3′ as well as β-actin forward 5′-GGCATCGTG ATGGACTCCG-3′ and anti-sense 5′-GC TGGA AGG TGG ACAGCGA-3′. The PCR amplification was performed for 40 cycles of 94 °C for 30 s, 60 °C for 30 s, and 72 °C for 30 s, on an Applied Biosystems 7900HT Real-Time PCR System with 1.0 μl of cDNA and SYBR Green Real-Time PCR Master Mix (Takara). Data was collected and analyzed by SDS2.3 software (Applied Biosystems). The expression level of each candidate gene was internally normalized against that of β-actin. The relative quantitative value was expressed by the 2−ΔΔCt method. Each experiment was performed in triplicates.
Western Blot
Briefly, the mice were perfused with 0.01 mol/l phosphate-buffered saline 1, 3, or 5 days after ICH, and the cerebral tissues from the perihematomal region were isolated (n = 5). The perihematomal tissues were lysed in 1 ml of radioimmunoprecipitation assay lysis buffer, and then the protein was extracted, electrophoresed, and transferred onto polyvinylidene fluoride membranes (Amersham Pharmacia). The polyvinylidene fluoride membranes were incubated with primary antibodies overnight, followed by incubation with peroxidase-conjugated secondary antibodies for 6 h. The same membranes were probed with an antibody for glyceraldehyde 3-phosphate dehydrogenase (GAPDH). Protein signals were detected with an enhanced chemiluminescence system. The signals were quantified by scanning densitometry and computer-assisted image analysis. Protein levels were expressed as the ratio of the values of the detected protein band to the GAPDH band.
Enzyme-Linked Immunosorbent Assay
The brain tissue was homogenized with a glass homogenizer in 1 ml of buffer containing 1 mM phenylmethylsulfonyl fluoride, 1 mg/l pepstatin A, 1 mg/l aprotinin, and 1 mg/l leupeptin in PBS solution (pH 7.2) and then centrifuged at 12,000g for 20 min at 4 °C. The supernatant was then collected, and total protein was determined using a bicinchoninic acid assay kit (Pierce Biochemicals). The TNF-α, IL-1β, and IL-6 levels in the brain tissue were quantified using enzyme-linked immunosorbent assay (ELISA) kits specific for mouse according to the manufacturer’s instructions.
Evaluation of Neurological Scores
The neurological scores were performed by two researchers who were blinded towards the status of the animals according to the previous reports [24]. Neurological function was assessed on a scale of 1–18; a score of 1 point is regarded as the inability to perform the test or for the lack of a tested reflex. The system comprised of six tests, namely spontaneous activity, symmetry in the movement of four limbs, forepaw outstretching, climbing, body proprioception, and response to vibrissae touch, and each score ranged from 0 to 3. The maximum is 18. The higher the score, the more severe the injury (normal score 2–3; maximal deficit score 18).
Determination of Brain Water Content
Brain water content (BWC) represented the brain edema, which formed as a result of blood-brain barrier (BBB) disruption. Brain water content was monitored according to the previous reports [25]. Mice were selected randomly from each group and euthanized immediately 3 days post hemorrhage for assay of BWC. Brains were quickly removed. A coronal brain slice (approximately 3 mm thick) 2 mm from the frontal pole was cut with a blade. The brain slice was divided into two hemispheres along the midline; each hemisphere was dissected into the cortex and the basal ganglia. The cerebellum was detached to serve as a control. Brain samples were immediately weighed on an electronic analytical balance to obtain the wet weight. Brain samples were then dried at 100 °C for 24 h to obtain the dry weight. The brain water content (%) was calculated as (wet weight − dry weight) / wet weight × 100.
Statistical Analysis
Analyses were performed using SPSS version 17.0 software (SPSS, Inc., Chicago, IL, USA), and all values are presented as the mean ± standard error of the mean (SEM). Student’s t test (two-tailed) and one-way analysis of variance (ANOVA) followed by Scheffé’s post hoc test were used to compare differences between two and three or more groups, respectively. A P value <0 to <0.05 was considered statistically significant.
Results
ICH Induced C5a/C5aR Expression in the Perihematomal Region
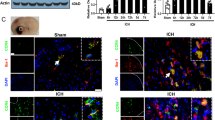
To detect the role of complement activation in the ICH, we utilized the autologous blood model and analyzed the C5a and C5aR levels in the perihematomal region after different time periods in ICH mice. The data demonstrated that C5a and C5aR levels increased at 1 day and peaked at 3 days in WT mice after ICH compared with those in the sham group. However, the changes of C5aR levels in C5aR KO mice after ICH were not significant compared with those in the sham group (P = 0.069) (Fig. 1). These results suggested that ICH induced C5a and C5aR expression in the perihematomal region.
ICH induced C5a/C5aR expression in the perihematomal region. a C5a/C5aR mRNA levels in the perihematomal brain tissues at 1, 3, and 5 days after ICH (n = 10 per group). b C5a/C5aR protein levels in the perihematomal brain tissues at 1, 3, and 5 days after ICH (n = 10 per group). Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
C5aR Enhanced Microglia Infiltration of the Perihematomal Region
Microglia infiltration contributed to the brain inflammatory injury. To detect the role of C5aR in the microglia infiltration, we also analyzed the Iba-1-positive microglia in the perihematomal brain tissues at 3 days after ICH. The data demonstrated that the number of microglia in the perihematomal brain tissues increased at 3 days in WT mice after ICH compared with that in the sham group. However, the number of microglia in C5aR KO mice decreased compared with that in WT mice after ICH (P = 0.062) (Fig. 2). These results suggested that C5aR enhanced microglia infiltration of the perihematomal region in ICH.
C5aR enhanced microglia infiltration of the perihematomal region. After 3 days post ICH modeling, mice (n = 10 per group) were deeply anesthetized in a transcardial manner. The brains were removed and postfixed. The perihematomal region of cerebral tissue was collected, and microglia were analyzed with anti-Iba-1 antibody (×400 magnification, A–D). Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
C5aR Promoted Inflammation of the Perihematomal Region
To detect the effects of C5aR on inflammation, we compared the messenger RNA (mRNA) and protein expression of inflammatory cytokines, such as TNF-α, IL-1β, and IL-6. The results demonstrated that the mRNA and protein expression of inflammatory cytokines in the perihematomal brain tissues significantly increased in the WT ICH mice compared with that in the sham group (P = 0.024). However, the mRNA and protein expression of inflammatory cytokines in the perihematomal brain tissues significantly decreased in the C5aR−/− ICH group compared with that in the WT ICH group (P = 0.037). On the contrary, the difference of the mRNA and protein expression between the C5aR−/− sham group and the WT sham group was not significant (P = 0.071) (Fig. 3). These results suggested that C5aR attenuated inflammation of the perihematomal brain tissues in ICH.
C5aR promoted inflammation of the perihematomal region. After 3 days post ICH modeling, mice (n = 10 per group) were deeply anesthetized in a transcardial manner. The brains were removed and postfixed. The perihematomal region of cerebral tissue was collected, and the tissue lysates were further analyzed for cytokine production with qRT-PCR and western blot assays. Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
C5aR Promoted Fgl-2 Expression in the Perihematomal Region
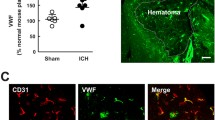
Fgl-2 has the capacity to induce fibrinogen deposition, which then activates the coagulation cascades and finally induces procoagulant activity and brain injury. To explore the role of C5aR on Fgl-2, we analyzed the Fgl-2 expression in the perihematomal region. Our data demonstrated that the mRNA and protein expression of Fgl-2 in the perihematomal brain tissues increased in the WT ICH mice compared with that in the sham group (P = 0.031). However, the mRNA and protein expression of Fgl-2 in the perihematomal brain tissues significantly decreased in the C5aR−/− ICH mice compared with that in the WT ICH mice (P = 0.038) (Fig. 4a, b). In addition, we utilized immunohistochemistry assay to analyze the Fgl-2 expression in the perihematomal brain tissues. We also found that the Fgl-2 expression level in the perihematomal brain tissues significantly increased in the WT ICH mice compared with that in the sham group (P = 0.026). However, the Fgl-2 expression level in the perihematomal brain tissues significantly decreased in the C5aR−/− ICH group compared with that in the WT ICH group (P = 0.027) (Fig. 4c). These results suggested that C5aR promoted Fgl-2 expression in the perihematomal region.
C5aR promoted Fgl-2 expression in the perihematomal region. After 3 days post ICH modeling, mice (n = 10 per group) were deeply anesthetized in a transcardial manner. The brains were removed and postfixed. a, b The perihematomal brain was dissected and homogenated to analyze the Fgl-2 mRNA and protein expression. c The perihematomal brain of 10 μm thickness was obtained with a freezing microtome, and immunohistochemistry assay was utilized to analyze the Fgl-2 expression (×400 magnification, a–d). Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
C5aR Promoted Fgl-2 Expression via Extracellular Signal-Regulated Kinase 1/2 and p38 MAPK Activation
It has been reported that both the extracellular signal-regulated kinase (ERK) and p38 MAPK proteins are important for signaling Fgl-2 expression in murine hepatitis virus strain 3 (MHV-3) infection. To explore the role of C5a/C5aR in ICH-induced MAPK phosphorylation, we detected the tyrosine phosphorylation status of ERK1/2 and p38 proteins in ICH. The data demonstrated that ERK1/2 and p38 phosphorylation levels in the perihematomal brain tissues significantly decreased in the C5aR−/− ICH mice compared with those in the WT ICH mice (P = 0.026). However, the difference of ERK1/2 and p38 phosphorylation levels between the C5aR−/− sham group and the WT sham group was not significant (P = 0.073) (Fig. 5a). To investigate if ERK1/2 and p38 MAPK activation mediates C5aR-dependent Fgl-2 induction, we used the chemical compound PD98059 to selectively inhibit the tyrosine kinase acting upstream of ERK1/2 and SB203580 to directly inhibit the p38 kinase activity. Mice received an intracerebral ventricular injection of PD98059 (2 μl of 30 mg/ml in 0.9 % NaCl), SB203580 (2 μl of 30 mg/ml in 0.9 % NaCl) or vehicle (0.9 % NaCl, 2 μl) 10 min after ICH and were sacrificed 3 days after ICH. These results demonstrated that treatment of PD98059 or SB203580 significantly reduced Fgl-2 production in ICH mice (P = 0.029) (Fig. 5b). These results suggested that C5aR promoted Fgl-2 expression via ERK1/2 and p38 MAPK phosphorylation in the perihematomal region.
C5aR promoted Fgl-2 expression via ERK1/2 and p38 activation. a After 3 days post ICH modeling, mice (n = 10 per group) were deeply anesthetized in a transcardial manner. The brains were removed and postfixed. The perihematomal brain was dissected and homogenated to analyze the ERK1/2 and p38 phosphorylation expression. b Mice (n = 10 per group) received an intracerebral ventricular injection of PD98059 (2 μl of 30 mg/ml in 0.9 % NaCl), SB203580 (2 μl of 30 mg/ml in 0.9 % NaCl), or vehicle (0.9 % NaCl, 2 μl) 10 min after ICH and were sacrificed 3 days after ICH. The perihematomal brain was dissected and homogenated to analyze the ERK1/2 and p38 phosphorylation expression. Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
C5aR Enhanced Neurological Impairment in ICH
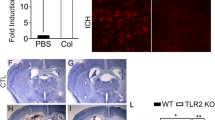
To further evaluate the role of C5aR on the ICH-induced neurological impairment, we compared brain water content and neurological deficit scores of C5aR−/− mice. The results demonstrated that brain water content and neurological deficit scores of WT ICH mice were much higher compared with those of the sham group (P = 0.019). However, brain water content and neurological deficit scores of C5aR−/− ICH mice were much lower compared with those of the WT ICH group (P = 0.017). On the contrary, the difference of brain water content and neurological deficit scores between the C5aR−/− sham group and the WT sham group was not significant (P = 0.064) (Fig. 6). These results suggested that C5aR enhanced ICH-induced neurological impairment.
C5aR enhanced neurological impairment in ICH. a After 3 days post ICH modeling, the cerebral water content of mice (n = 10 per group) was also analyzed. b After 3 days post ICH modeling, mice (n = 10 per group) were in a stable condition, and the neurological deficit tests were performed by behavioral measurement, including composite of motor, sensory, reflex, and balance tests. The results demonstrated that brain water content and neurological deficit scores of WT ICH mice were much higher compared with those of the sham group. However, brain water content and neurological deficit scores of C5aR−/− ICH mice were much lower compared with those of the WT ICH group. Experiments performed in triplicate showed consistent results. Data are presented as the mean ± standard error of mean (SEM) of three independent experiments. *P < 0.05
Discussion
ICH is a public health problem because of high mortality and disability. Treatment of ICH is largely focused on mechanical elimination of the hematoma, prevention of brain edema, and alleviation of intracranial pressure [26–28]. These mentioned methods only prevent further brain damage and related complications. However, effective therapeutic strategy is very limited, and no available treatment has shown promising benefits after ICH [29–31].
The complement cascade plays an important role in the regulation of inflammation through inflammatory cell infiltration, blood-brain barrier damage, and subsequent brain edema [32–34]. Evidence suggests that blockage of complement activation attenuates demyelination and inflammatory response in experimental allergic encephalomyelitis, reduces neutrophil accumulation following traumatic brain damage, and decreases cerebral infarction size in a model of MCAO mice [13, 35–37]. Therefore, identification of the specific complement subcomponents which contributed to post-hemorrhagic damage might provide a promising therapeutic target after ICH.
It was reported that thrombin acts as a C5 convertase to activate complement and C5a generation without C3, providing the relationship between the complement and the clotting system [38]. C5a is known as an anaphylatoxin, which acts its biological function through a combination with each of its G protein-coupled receptors and the C5a receptor (C5aR) that belongs to the rhodopsin family of seven-transmembrane G protein-coupled receptor [39, 40].
Firstly, we analyzed the C5a and C5aR levels in the perihematomal region after different time periods in ICH mice. We found that ICH induced complement activation and C5aR expression in the perihematomal region. Secondly, to detect the role of C5aR in the microglia infiltration and neuroinflammation in ICH, we analyzed the Iba-1-positive microglia and inflammatory cytokines in the perihematomal brain tissues after ICH. These results suggested that C5aR enhanced microglia infiltration and inflammatory cytokines in the perihematomal region in ICH. In addition, to explore the relationship between C5aR and Fgl-2, which could induce procoagulant activity and brain injury, we analyzed the Fgl-2 expression in the perihematomal brain tissues. We found that C5aR promoted Fgl-2 expression in the perihematomal region.
It has been demonstrated that the MAPK activation is vital for the Fgl-2 induction in response to MHV-3 stimulation. MAPK activation is an important downstream molecular event for the C5a-induced inflammatory cytokine production. In accordance with these observations, we have also found that C5a-induced Fgl-2 production in ICH is largely dependent on the activation of the ERK1/2 and p38 pathways. It has been reported that blood-derived lymphocytes infiltrate the brain tissue, worsening brain edema and initiating a neuroinflammatory injury. Therefore, to detect the specific effect of C5aR on the ICH-induced brain injury, we assessed brain water content and neurological deficit scores of C5aR−/− mice. The results demonstrated that brain water content and neurological deficit scores of C5aR−/− ICH mice were much lower compared with those of the WT ICH group. We proved that C5aR enhanced ICH-induced lymphocyte accumulation, leading to brain edema and neurological impairment.
In summary, the results suggest that C5a/C5aR contributed to complement-mediated cerebral injury following ICH induction. In addition, the inhibition of C5aR delivers a theoretical basis for underlying inflammatory secondary injury mechanisms.
References
Sprigg N, Robson K, Bath P, Dineen R, Roberts I, Robinson T, Roffe C, Werring D et al (2016) Intravenous tranexamic acid for hyperacute primary intracerebral hemorrhage: protocol for a randomized, placebo-controlled trial. Int J Stroke 11:683–694
Nishimura K, Koga M, Minematsu K, Takahashi JC, Nagatsuka K, Kobayashi J, Toyoda K (2016) Intracerebral hemorrhage in patients after heart valve replacement. J Neurol Sci 363:195–199
Krishnan K, Scutt P, Woodhouse L, Adami A, Becker JL, Cala LA, Casado AM, Chen C et al (2016) Continuing versus stopping prestroke antihypertensive therapy in acute intracerebral hemorrhage: a subgroup analysis of the efficacy of nitric oxide in stroke trial. J Stroke Cerebrovasc Dis 25:1017–1026
Loftspring MC, McDole J, Lu A, Clark JF, Johnson AJ (2009) Intracerebral hemorrhage leads to infiltration of several leukocyte populations with concomitant pathophysiological changes. J Cereb Blood Flow Metab 29:137–143
Mohan S, Ahmad AS, Glushakov AV, Chambers C, Dore S (2012) Putative role of prostaglandin receptor in intracerebral hemorrhage. Front Neurol 3:145
Wu CH, Chen CC, Lai CY, Hung TH, Lin CC, Chao M, Chen SF (2016) Treatment with TO901317, a synthetic liver X receptor agonist, reduces brain damage and attenuates neuroinflammation in experimental intracerebral hemorrhage. J Neuroinflammation 13:62
Wu X, Spitzer D, Mao D, Peng SL, Molina H, Atkinson JP (2008) Membrane protein Crry maintains homeostasis of the complement system. J Immunol 181:2732–2740
Elward K, Gasque P (2003) “Eat me” and “don’t eat me” signals govern the innate immune response and tissue repair in the CNS: emphasis on the critical role of the complement system. Mol Immunol 40:85–94
Low JM, Moore TLA (2005) Role for the complement system in rheumatoid arthritis. Curr Pharm Des 11:655–670
Price PJ, Banki Z, Scheideler A, Stoiber H, Verschoor A, Sutter G, Lehmann MH (2015) Complement component C5 recruits neutrophils in the absence of C3 during respiratory infection with modified vaccinia virus Ankara. J Immunol 194:1164–1168
Cole DS, Hughes TR, Gasque P, Morgan BP (2006) Complement regulator loss on apoptotic neuronal cells causes increased complement activation and promotes both phagocytosis and cell lysis. Mol Immunol 43:1953–1964
Gu C, Jenkins SA, Xue Q, Xu Y (2012) Activation of the classical complement pathway by Bacillus anthracis is the primary mechanism for spore phagocytosis and involves the spore surface protein BclA. J Immunol 188:4421–4431
Brennan FH, Anderson AJ, Taylor SM, Woodruff TM, Ruitenberg MJ (2012) Complement activation in the injured central nervous system: another dual-edged sword? J Neuroinflammation 9:137
Hamad I, Hunter AC, Szebeni J, Moghimi SM (2008) Poly(ethylene glycol)s generate complement activation products in human serum through increased alternative pathway turnover and a MASP-2-dependent process. Mol Immunol 46:225–232
Woodruff TM, Ager RR, Tenner AJ, Noakes PG, Taylor SM (2010) The role of the complement system and the activation fragment C5a in the central nervous system. Neruomol Med 12:179–192
Khan MA, Hsu JL, Assiri AM, Broering DC (2016) Targeted complement inhibition and microvasculature in transplants: a therapeutic perspective. Clin Exp Immunol 183:175–186
Karsten CM, Laumonnier Y, Kohl J (2014) Functional analysis of C5a effector responses in vitro and in vivo. Methods Mol Biol 1100:291–304
Helske S, Oksjoki R, Lindstedt KA, Lommi J, Turto H, Werkkala K, Kupari M, Kovanen PT (2008) Complement system is activated in stenotic aortic valves. Atherosclerosis 196:190–200
Girke G, Kohl B, Busch C, John T, Godkin O, Ertel W, Schulze-Tanzil G (2014) Tenocyte activation and regulation of complement factors in response to in vitro cell injury. Mol Immunol 60:14–22
Hollmann TJ, Mueller-Ortiz SL, Braun MC, Wetsel RA (2008) Disruption of the C5a receptor gene increases resistance to acute gram-negative bacteremia and endotoxic shock: opposing roles of C3a and C5a. Mol Immunol 45:1907–1915
Jacob A, Hack B, Chiang E, Garcia JG, Quigg RJ, Alexander JJ (2010) C5a alters blood-brain barrier integrity in experimental lupus. FASEB J 24:1682–1688
Sun L, Gao H, Sarma VJ, Guo RF, Ward PA (2006) Adenovirus-mediated in vivo silencing of anaphylatoxin receptor C5aR. J Biomed Biotechnol 2006:28945
Riedemann NC, Guo RF, Hollmann TJ, Gao H, Neff TA, Reuben JS, Speyer CL, Sarma JV et al (2004) Regulatory role of C5a in LPS-induced IL-6 production by neutrophils during sepsis. FASEB J 18:370–372
Yao Y, Tsirka SE (2012) The CCL2-CCR2 system affects the progression and clearance of intracerebral hemorrhage. Glia 60:908–918
Jeon D, Chu K, Lee ST, Jung KH, Ban JJ, Park DK, Yoon HJ, Jung S et al (2013) Neuroprotective effect of a cell-free extract derived from human adipose stem cells in experimental stroke models. Neurobiol Dis 54:414–420
Mould WA, Carhuapoma JR, Muschelli J, Lane K, Morgan TC, McBee NA, Bistran-Hall AJ, Ullman NL et al (2013) Minimally invasive surgery plus recombinant tissue-type plasminogen activator for intracerebral hemorrhage evacuation decreases perihematomal edema. Stroke 44:627–634
Yang Z, Zhong S, Liu Y, Shen H, Yuan B (2015) Scavenger receptor sra attenuates microglia activation and protects neuroinflammatory injury in intracerebral hemorrhage. J Neuroimmunol 278:232–238
Powers WJ (2010) Intracerebral hemorrhage and head trauma: common effects and common mechanisms of injury. Stroke 41:S107–S110
Whiteley WN, Thompson D, Murray G, Cohen G, Lindley RI, Wardlaw J, Sandercock P (2014) Targeting recombinant tissue-type plasminogen activator in acute ischemic stroke based on risk of intracranial hemorrhage or poor functional outcome: an analysis of the third international stroke trial. Stroke 45:1000–1006
Xi G, Strahle J, Hua Y, Keep RF (2014) Progress in translational research on intracerebral hemorrhage: is there an end in sight? Prog Neurobiol 115:45–63
Steiner T, Petersson J, Al-Shahi Salman R, Christensen H, Cordonnier C, Csiba L, Harnof S, Krieger D et al (2011) European research priorities for intracerebral haemorrhage. Cerebrovasc Dis 32:409–419
Croker DE, Monk PN, Halai R, Kaeslin G, Schofield Z, Wu MC, Clark RJ, Blaskovich MA et al (2016) Discovery of functionally selective C5aR2 ligands: novel modulators of C5a signaling. Immunol Cell Biol 94:787–795
Asgari N, Khorooshi R, Lillevang ST, Owens T (2013) Complement-dependent pathogenicity of brain-specific antibodies in cerebrospinal fluid. J Neuroimmunol 254:76–82
Ducruet AF, Zacharia BE, Hickman ZL, Grobelny BT, Yeh ML, Sosunov SA, Connolly ES Jr (2009) The complement cascade as a therapeutic target in intracerebral hemorrhage. Exp Neurol 219:398–403
Neher MD, Rich MC, Keene CN, Weckbach S, Bolden AL, Losacco JT, Patane J, Flierl MA et al (2014) Deficiency of complement receptors CR2/CR1 in CR2(−)/(−) mice reduces the extent of secondary brain damage after closed head injury. J Neuroinflammation 11:95
Stahel PF, Flierl MA, Morgan BP, Persigehl I, Stoll C, Conrad C, Touban BM, Smith WR et al (2009) Absence of the complement regulatory molecule CD59a leads to exacerbated neuropathology after traumatic brain injury in mice. J Neuroinflammation 6:2
Yang S, Wang X, Zhang X, Lu Y, Wang Z (2013) Neuroprotective effects of the SCR1-3 functional domain of CR1 on acute cerebral ischemia and reperfusion injury in rats. Neurol Res 35:976–983
Khan MA, Maasch C, Vater A, Klussmann S, Morser J, Leung LL, Atkinson C, Tomlinson S et al (2013) Targeting complement component 5a promotes vascular integrity and limits airway remodeling. Proc Natl Acad Sci U S A 110:6061–6066
Huber-Lang M, Sarma JV, Zetoune FS, Rittirsch D, Neff TA, McGuire SR, Lambris JD, Warner RL et al (2006) Generation of C5a in the absence of C3: a new complement activation pathway. Nat Med 12:682–687
Palmer E, Gray LC, Stott M, Bowen DJ, van den Berg CW (2012) Roles of promoter and 3′ untranslated motifs in expression of the human C5a receptor. Mol Immunol 52:88–95
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
Bangqing Yuan and Fenlan Fu contributed equally to this study.
Rights and permissions
About this article
Cite this article
Yuan, B., Fu, F., Huang, S. et al. C5a/C5aR Pathway Plays a Vital Role in Brain Inflammatory Injury via Initiating Fgl-2 in Intracerebral Hemorrhage. Mol Neurobiol 54, 6187–6197 (2017). https://doi.org/10.1007/s12035-016-0141-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-0141-7