Abstract
The expression of matrix metalloproteinase-13 (MMP-13) has been shown to be elevated in some pathophysiological conditions and is involved in the degradation of extracellular matrix in astrocytes. In current study, the function of MMP-13 was further investigated. The conditioned medium (CM) collected from activated microglia increased interleukin (IL)-18 production and enhanced MMP-13 expression in astrocytes. Furthermore, treatment with recombinant IL-18 increased MMP-13 protein and mRNA levels in astrocytes. Recombinant IL-18 stimulation also increased the enzymatic activity of MMP-13 and the migratory activity of astrocytes, while administration of MMP-13 or pan-MMP inhibitors antagonized IL-18-induced migratory activity of astrocytes. In addition, administration of recombinant IL-18 to astrocytes led to the phosphorylation of JNK, Akt, or PKCδ, and treatment of astrocytes with JNK, PI3 kinase/Akt, or PKCδ inhibitors significantly decreased the IL-18-induced migratory activity. Taken together, the results suggest that IL-18-induced MMP-13 expression in astrocytes is regulated by JNK, PI3 kinase/Akt, and PKCδ signaling pathways. These findings also indicate that IL-18 is an important regulator leading to MMP-13 expression and cell migration in astrocytes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Astrocytes are the most abundant macroglia cells within the CNS and participate in a wide variety of functions, including releasing growth factors, uptake and clearance of neurotransmitters, and homeostatic maintenance of the extracellular ionic environment [1]. In addition to the physiological functions, astrocytes have also been reported to be an important player in several types of CNS insults like traumatic brain injury [2], neurodegenerative disorders [3], and multiple forms of inflammatory stimuli [4]. In response to the pathological insults, astrocytes become “reactive” and respond in astrogliosis or even undergo migration for glial scar formation when severe neural damages occur [1]. The activation of astrocytes is normally accompanied by the production of cytokines, chemokines, and inflammatory mediators that subsequently trigger downstream multi-cellular events and lead to regulation of the patho-physiological effects of the injured nervous system to prevent secondary damages [1]. The degrees of astrocytic activation, including migration, vary and are tuned by different microenvironments consisting of a vast array of signaling molecules like cytokines and inflammatory mediators [4].
Interleukin (IL)-18, a member of the IL-1 pro-inflammatory cytokines family, exerts diverse actions on the regulation of immunity and inflammation responses of inflammatory-associated disorders. Administration of inflammagens like lipopolysaccharide (LPS) stimulated the secretion of IL-18 from astrocytes and microglial cells [5]. Besides, the expression of IL-18 was significantly elevated in neurons, astrocytes, and microglia under the conditions of infection, hypoxia-ischemic, and traumatic brain injuries [6, 7]. Therefore, IL-18 is implicated to be a key cytokine in modulating immunological responses under neuropathological conditions [8]. One particular function of IL-18 is probably involved in guiding and activating circulating immune cells to the damaged tissues. For example, in a rat brain focal ischemia model, the time point of IL-18 upregulation is closely associated with infiltration of peripheral immune cells, indicating a role of IL-18 in the regulation of glia migration [9]. Many reports have shown that IL-18 is associated with triggering migration of a various kind of cells [10] and that matrix metalloproteinases (MMPs) are involved in IL-18-induced cell migration [11, 12].
MMP is a family of zinc-binding proteolytic enzymes that are capable of decomposing components of extracellular matrix (ECM) and facilitating migration of precursor cells, tumor cells, and others [13]. In the CNS, MMPs are involved in regulating the progression of brain injuries and malignant glioma [14]. Moreover, triggering the expression of MMPs by cytokines and LPS to pathologically degraded substrate has been part of the neuroinflammation responses [14]. Among the MMPs, the collagenolytic MMP-13 is characterized by a wide substrate specificity and is expressed by many types of invasive tumors like breast cancer [15], glioma [16–19], and oral cancer [20]. These reports have demonstrated that upregulation of MMP-13 highly correlated with the malignance of glioma and oral cancer. In addition, MMP-13 participates in the function of astrocytes during pathological conditions. For example, hypoxia insults caused elevated expression of MPP-13 in astrocytes and thus enhanced the permeability of blood–brain barrier [21]. These aforementioned suggest that the collagenolytic MMP-13 is an important regulating molecular for various functions under pathological conditions. Thus, studies to better understand the role of MMP-13 in astrocyte migration under inflammatory conditions and underlying mechanisms may provide clinically relevant insights.
Protein kinase C (PKC) is a family of serine/threonine proteins kinases that play key roles in cellular processes including cell survival and apoptosis, migration, and malignant transformation [22]. Several reports have shown that altered PKC expression is observed in many tumor tissues, and this alteration has linked PKC to tumor invasion involving MMPs [23, 24]. It has been implicated that PKC altered the degrees of cell migration through regulating MMP expression [23–25]. The PKC family consists of a variety of isoforms with different domain structures. One of the isoforms, PKCδ, has been shown in our recent finding to modulate inflammatory homeostasis in microglia [26]. A recent study has also demonstrated that the induced expression of MMP-13 by IL-13 is through the activation of PKC-δ isoform in fibroblasts [27]. Moreover, the induction of angiogenic factors by IL-18 through the activation of PKCδ has been previously addressed [28]. This study investigates whether the pro-inflammatory cytokines IL-18 regulates the expression MMP-13 and astrocytic migration and whether the PKC-δ activation is involved.
Materials and Methods
Materials
Reagents and Antibodies
Dulbecco’s modified Eagle medium (DMEM), fetal bovine serum (FBS), and OPTI-MEM were purchased from Gibco-BRL (Invitrogen Life Technologies, Carlsbad, CA). Goat anti-mouse and anti-rabbit horseradish peroxidase-conjugated IgG, primary antibodies against p85, phosphor-p85, Akt, pAkt, JNK, pJNK, c-Jun, and PCNA were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Primary antibodies against phosphorylated c-Jun and PKCδ (phosphorylated at Thr) were purchased from Cell Signaling and Neuroscience (Danvers, MA). LY294002 and rottlerin were obtained from Sigma-Aldrich (St. Louis, MO). SP600125 were obtained from Tocris Bioscience (Ellisville, MO).
Cell Culture
Primary rat astroctye cultures were obtained according to previous reports [29, 30] with mild modification. Briefly, mixed-glia cultures were prepared from dissected brains of 1-day-old pups of Sprague–Dawley rat. The mechanically dissociated brain cells were seeded onto 75-cm2 culture flasks (5 × 107 cells/per flask) in Dulbecco’s modified Eagle’s medium (DMEM)/F12 fortified with 10 % heat-inactivated fetal bovine serum (FBS), 2 mM l-glutamine, 1 mM sodium pyruvate, 100 mM non-essential amino acids, 100 U/ml penicillin, and 100 mg/ml streptomycin. The cultured cells were incubated at 37 °C in a humidified atmosphere with 5 % CO2 and 95 % air, and medium was replenished twice a week. When the culture reached confluence (usually 12–14 days later), microglia were detached from astrocytes by shaking the flasks at a speed of 180 rpm for 5 h. The cultures were then treated with l-leucine methyl ester to remove microglia from the astrocyte culture. All experiments were performed by using confluent astrocytes grown in the second passage. Afterward, the astrocytes were harvested with trypsin and then seeded in a new flask and grown in DMEM supplemented with 10 % FBS, 100 U/ml penicillin, and 100 mg/ml streptomycin. The cultured astrocyte was confirmed by immunocytochemical staining against CD-11b, GFAP, or MAP-2. The staining showed over 98 % purity of astrocytes and less than 2 % of microglia contamination.
The BV-2 microglial cell was cultured in DMEM with 10 % FBS at 37 °C in a humidified incubator under 5 % CO2 and 95 % air. Confluent cultures were passaged by trypsinization.
Microglial-Conditioned Medium
The murine microglial BV-2 cells were cultured in DMEM containing 10 % FBS (Invitrogen, Carlsbad, CA) and penicillin-streptomycin (100 units/ml, 100 μg/ml) (Invitrogen, Carlsbad, CA) at 37 °C in a humidified incubator with an atmosphere of 5 % CO and 95 % air. Once the culture reached confluence, microglia were replenished with fresh medium and treated with either LPS (100 ng/ml) or PGN (3 μg/ml). After 24 h, the conditioned medium was collected and immediately applied to cultured astrocytes for an additional 6 h.
Wound-Healing Assay
Astrocyte cells were treated with 30 ng/ml of IL-18 or vehicle for the indicated time points. A cell-free gap of 500 mm was generated after removing the Culture-Insert (Ibidi, München, DE). Astrocyte cells that migrated into the wound area were detected under the light microscope, and pictures were acquired at 0 and 24 h with digital camera.
Western Blot Analysis
Cells were treated with IL-18 (30 ng/ml) for indicated time periods followed by being washed with cold PBS and lysed for 30 min on ice with lysis buffer (50 mM HEPES (PH 7.4), 150 mM NaCl, 4 mM EDTA, 10 mM Na4P2O7, 100 mM NaF, 2 mM Na3VO4, 1 % Triton X-100, 0.25 % sodium deoxycholate, 50 mM 4-(2-aminoethyl) benzene sulfonylfluoride, 50 μg/ml leupeptin, and 20 μg/ml aprotinin). Protein samples were then separated by sodium dodecyl sulfate polyacrylamide gels and transferred to polyvinylidene fluoride membranes. The membranes were blocked with 5 % nonfat milk before being probed with primary antibodies of interest at 4 °C overnight. After several PBS washes, the membranes were incubated with secondary antibodies for 1 h at the room temperature. The blots were then visualized by enhanced chemiluminescence kit (ECL kit; GE Healthcare, Piscataway, NJ).
Zymographic Analysis
The secretion of MMPs into the culture medium of astrocyte cells were evaluated after IL-18 treatment. The collected culture medium was mixed with non-reducing sample buffer and then electrophoresed in a 10 % SDS-polyacrylamide gel containing 1 % bovine type B gelatin (Sigma-Aldrich). Later, the gel was washed with 2.5 % Triton X-100 to remove the SDS, rinsed with 50 mM Tris–HCl, pH 7.5, followed by incubation overnight at room temperature in the developing buffer [31]. Enzyme activities of MMPs were determined by staining with 1 % Coomassie Blue. The sample was also loaded onto an SDS-polyacrylamide gel and stained with 1 % Coomassie Blue as a loading control.
Reverse Transcriptase PCR and Quantitative Real-Time PCR
Total RNA was extracted from treated BV-2 cells by using a TRIzol kit (MDBio Inc., Taipei, Taiwan). Later, the reverse transcription reaction was carried out using 2 μg total RNA that was first reverse transcribed into cDNA using oligo(dT) primer. Quantitative real-time PCR was performed as previously reported [18]. Briefly, PCR reaction using SYBR Green Master Mix was carried out using the StepOne Plus System (Applied Biosystems, Singapore), and the PCR was performed under the following conditions: 40 cycles at 95 °C for 10 s and 60 °C for 1 min. The threshold was set within the linear phase of the target gene amplification to calculate the cycle number at which point the transcript was detected (denoted as CT). The oligonucleotide primers were as follows:
-
IL-18: 5′-ACTGTACAACCGCAGTAA-3′ and 5′- AGTGAACATTACAGATTTATCCC-3′;
-
GAPDH: 5′-CTCAACTACATGGTCTACATGTTCCA-3′ and 5′-CTTCCCATTCTCAGCCTTGACT-3′
Electrophoretic Mobility Shift Assay
The protocol of electrophoretic mobility shift assay gel shift kit (Panomics, Redwood City, CA) was used according to our previous report [32]. Nuclear extract (4 μg) of astrocytes was incubated with poly d(I-C) at room temperature for 5 min. The nuclear extract was then incubated with biotin-labeled probes at room temperature for 30 min. After electrophoresis on an 8 % polyacrylamide gel, the samples on gel were transferred onto a presoaked Immobilon-Nyt membrane (Millipore, Billerica, MA). The membrane was cross-linked in an oven for 1 min and then developed with blocking buffer and streptavidin-horseradish peroxidase conjugate before being subjected to western blot analysis.
Statistics
The experimental data was analyzed using the software Graphpad Prism 4.01 (GraphPad Software Inc., San Diego, CA). The values given are means ± SEM. Statistical analysis between two samples was performed using Student’s t test. Statistical comparisons of more than two groups were performed using one-way ANOVA with Bonferroni’s post hoc test. The difference is considered significant if the p value is <0.05.
Results
IL-18 Enhances MMP-13 Expression in Astrocytes
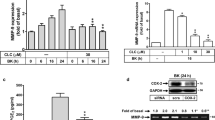
Primary astrocytes were subjected to the microglial-conditioned medium (mgCM) for 6 h, the mRNA level of MMP-13 was then determined by real-time PCR (Fig. 1a). The administration of mgCM, collected from microglia cultures stimulated with either LPS or PGN, effectively increased MMP-13 mRNA expression to approximately twofold in astrocytes. In addition, when microglia were treated with various concentrations of either LPS or PGN, there was a significant elevation of IL-18 mRNA levels (Fig. 1b, c). The induction of IL-18 mRNA expression by LPS or PGN was concentration dependent. Further investigation using the RT-PCR analysis found that MMP-13 mRNA levels in cultured astrocytes was markedly upregulated upon incubation with IL-18 at various time points (Fig. 1d) and various concentrations (Fig. 1e). To determine protein expression of MMP-13 stimulated by IL-18, the gelatin zymography and western blot analysis were applied. The data showed that the production of MMP-13 protein from both the supernatant and the cell lysate extract were upregulated as the concentration of IL-18 increased (Fig. 1f). This upregulation of MMP-13 proteins was dose dependent and was observed as low concentration as 3 to 30 ng/ml of IL-18 treatment. Real-time PCR further confirmed that administration of IL-18 augmented MMP-13 expression to around twofold (Fig. 1g).
Upregulation of MMP-13 induced by IL-18 in astrocytes. a Microglial-conditioned medium (mgCM) collected from microglia treated with LPS (100 ng/ml) or PGN (3 μg/ml) for 24 h. The collected microglial-CM immediately applied to astrocytes for an additional 6 h. Microglia were treated with various concentrations of LPS (b) or PGN (c). mRNA levels of IL-18 were analyzed by real-time PCR and normalized with β-actin. Astrocytes were treated with a concentration of 30 ng/ml IL-18 for indicated time periods (2, 4, 8, and 24 h; d) or with various concentrations of IL-18 (3, 10, or 30 ng/ml for 24 h; e). The relative mRNA levels of MMP-13 were analyzed by RT-PCR. f Astrocytes were incubated with various concentrations of IL-18 (3, 10, or 30 ng/ml) for 24 h, after which the supernatant and cell lysate extracts were collected, and MMP-13 protein levels were determined using gelatin zymography and western blot analysis, respectively. g Astrocytes were treated with 30 ng/ml IL-18 for 8 h, mRNA levels of MMP-13 were analyzed by real time-PCR. The data represent the mean ± SEM of n = 3–4. *p < 0.05, compared with the vehicle control group
MMP-13 Is Involved in IL-18-Directed Astrocyte Migration
The wound-healing assay was performed next to examine whether IL-18 facilitated astrocyte migration. Astrocyte cells with higher migratory activity demonstrated narrower cell-free gap in the culture. The microscopic images showed that as the IL-18 incubation time lengthened, the width differences of the cell-free gap between the vehicle group and the IL-18 treatment group became bigger (Fig. 2a). Our data showed that IL-18 enhanced astrocytes migration. Since IL-18 enhanced MMP-13 production in astrocytes, we then investigated whether MMP-13 was involved in IL-18-directed cell migration. As shown in Fig. 2b, applications of either a broad-spectrum MMP inhibitor (GM 6001) or the specific MMP-13 inhibitor prior to a 24-h-IL-18-treatment markedly attenuated the IL-18-directed cell migration. And, this inhibition of MMP-13 significantly reduced the IL-18-induced migratory index to around the level of the control group (Fig. 2c).
IL-18-directed astrocytic migration involves MMP-13 expression. a Cells were treated with 30 ng/ml IL-18 or vehicle for indicated time periods; the migrated cells were determined by wound-healing assay and visualized by phase-contrast imaging. b Cells were incubated with GM6001 or MMP-13 inhibitor for 30 min, followed by stimulation with IL-18 for 24 h. The migrated cells were determined by wound-healing assay and visualized by phase-contrast imaging. The quantitative results were measured by Image J software (c). Results are the representative of three independent experiments. *p < 0.05 compared with the control group; #p < 0.05 compared with IL-18 treatment group
IL-18 Increases PI3 Kinase/Akt and JNK Signaling Pathways and Induces AP-1 Activation in Astrocytes
It has been reported that IL-18 exerted its neuroprotection via the activation of PI3 kinase/Akt pathways [33]. Another study showed that IL-18 induced angiogenesis via the JNK kinases [34]. We then investigated whether the PI3 kinase/Akt and JNK signaling pathways underlies the function of IL-18 on astrocytes. As shown in Fig. 3a–c, IL-18 treatment increased phosphorylation of p85 (a subunit of PI3 kinase), Akt (the downstream substrate of PI3 kinase), and JNK. The activation of both the PI3 kinase/Akt and JNK/c-Jun pathways were observed as fast as within 5 min after IL-18 administration. Furthermore, phosphorylation of c-Jun, downstream of Akt and JNK, has been shown to participate in IL-18-induced cellular responses such as activation of c-Jun at Ser 63. As shown in Fig. 3d, IL-18 stimulated a time-dependent phosphorylation of c-Jun. The phosphorylation of c-Jun at Ser 63 achieved a maximum at 10–30 min and was sustained to 60 min after IL-18 treatment (Fig. 3d). The involvement of the above pathways were also examined by that the phosphorylation level of c-Jun declined when cells were preincubated with either JNK inhibitor (SP600125) or PI3 kinase inhibitor (LY294002) prior to IL-18 treatment (Fig. 3e). Moreover, c-Jun activation was further confirmed by the binding activity assay. The data showed that IL-18 enhanced the binding activity of pc-Jun to AP-1 DNA binding element, which was markedly negated by the application of SP600125 and LY294002 (Fig. 3f). Taken together, these results suggest that IL-18 stimulates PI3 kinase/Akt and JNK activation in a time-dependent manner and induces c-Jun/AP-1 in astrocytes.
IL-18 increases PI3K/Akt and JNK signaling pathways and induces AP-1 activation. Astrocytes were incubated with IL-18 (30 ng/ml) for indicated time periods, and cell lysates were separated by SDS-PAGE and immunoblotted with anti-phosphoPI3 kinase (p85; a), phosphoAkt (b), phosphoJNK, (c) or phosphoc-Jun (d). e Cells were preincubated with SP600125 (10 μM) or LY294002 (10 μM) for 30 min followed by stimulation with IL-18 (30 ng/ml) for another 30 or 60 min, and the levels of nuclear phosphorylated c-Jun were determined using western blot analysis. Nuclear extracts were collected from cells, the binding of c-Jun to AP-1-DNA binding element were examined by EMSA analysis. Lane 1 was loaded without nuclear extracts (probe). The AP-1-specific complex and free probe are indicated by an arrowhead (f)
IL-18-Directed Cell Migration Requires the Activation of PKCδ Signal Pathways
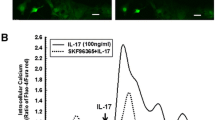
Since PKCδ has been reported to be involved in the regulation of PI3 kinase activity [35] and JNK activation [36]. We next examined whether PKCδ played a role in the function of IL-18-directed astrocytic migration. As demonstrated in Fig. 4a, IL-18 effectively increased the phosphorylation of PKCδ time dependently. The activation of PKCδ was noted in 5–10 min after IL-18 treatment and sustained to 120 min. Application of rottlerin, a specific pharmacological PKCδ inhibitor, attenuated the phosphorylation of Akt and JNK induced by IL-18 (Fig. 4b).
IL-18-increased PKCδ activation regulates Akt and JNK signaling pathways. a Cells were incubated with IL-18 (30 ng/ml) for indicated time periods, and cell lysates were separated by SDS-PAGE and immunoblotted with anti-phosphoPKCδ. b Cells were preincubated with rottlerin (1 μM) for 30 min followed by stimulated with IL-18 (30 ng/ml) for another 60 min. The levels of phosphorylated Akt and phosphorylated JNK were determined using western blot analysis. Note that application of a specific PKCδ inhibitor rottlerin attenuated the phosphorylation of Akt and JNK induced by IL-18
The wound-healing assay was performed to determine whether IL-18-induced cell migration through the activation of the PKCδ, Akt, and JNK signal pathways. The data showed that IL-18-directed migratory effect was significantly suppressed by the treatment with SP600125, LY294002 and rottlerin, as was manifested by the increased width of the cell-free gaps of the microscopic images (Fig. 5a) and the measured migratory index (Fig. 5b). Our results indicated that the activation of PKCδ, Akt, and JNK signal pathways is required for the IL-18-directed astrocytic migration.
PKCδ, Akt and JNK signaling pathways are involved in IL-18-directed astrocytic migration. Cells were pretreated with SP600125 (10 μM), LY294002 (10 μM), or rottlerin (1 μM) for 30 min then stimulated with IL-18 (30 nM) for 24 h. The migrated cells were determined by wound-healing assay and visualized by phase-contrast imaging. The quantitative results were measured by Image J software (b). Results are expressed as the means ± SEM of three independent experiments. *p < 0.05 compared with the control group; #p < 0.05 compared with the IL-18-treated group
Discussion
The present study demonstrated that MMP-13 upregulation in astrocytes in response to IL-18 stimulation fulfills the following criteria as a candidate to be involved in enhancing brain astrocytic migration. First, IL-18 enhanced the protein and mRNA levels of MMP-13 and increased the zymographic activity in primary cultured astrocytes. Second, using wound healing migratory model, stimulation with IL-18 increased astrocytic migration. Third, treatment with MMP pan-inhibitor or MMP-13 inhibitor significantly antagonized the potentiating effect of astrocytic migration. Finally, treatment of conditioned medium of microglia subjected to LPS or PGN increased MMP-13 expression in astrocytes. Additionally, stimulation of LPS of PGN increased IL-18 upregulation in microglia. Das et al. [37] and our previous report [38] showed that stimulated microglia increases IL-18 expression and subsequently induces pathology. Dai et al. has also reported that stimulation of IL-18 induces increases in MMP-13 expression in chondrocytes [39]. Our previous studies also demonstrated MMP-13 plays a pivot role in facilitating cell migratory activity in various cells [17–20, 38]. Importantly, our result also supports previous study that exogenous endothelin-1 increases MMP-13 expression via MAP kinase and PI3 kinase/Akt activation, thereby contributing to cell migration in human glioblastoma [16]. The present study suggests that IL-18-mediated MMP-13 expression in astrocytes may contribute to the astrocytic migration.
Neuroinflammation is an important factor in the pathogenesis of neurodegenerative diseases [40] and psychiatric illnesses such as depression [41]. Importantly, it has recently also been implicated in cognitive decline [42], memory deficits [43], and sickness behavior [44], as well as in aging-sensitization of the immune system [45]. IL-18 is one of the IL-1 family of cytokines comprises 11 secreted factors, which are known for playing a role in host defense and immune system regulation in inflammatory diseases [46]. This cytokine has also been demonstrated to be involved in initiation, regulation, and maintenance of inflammation in immune responses [47]. Importantly, IL-18 overexpression has been observed to initiate inflammatory process in the brain of Alzheimer’s disease patients [48]. Indeed, IL-18-mediated processes resulting in long-term neurodegenerative diseases have been well established [49]. Glial cells, specifically microglia and astrocytes, are the primary immune cells in central nervous system. Activation of these cells then leads to release pro-inflammatory cytokines like IL-18 [46], which promote a number of innate immune processes, thereby responsible for neuroinflammation and associated brain diseases [50].
Overexpression of MMP-13 has been reported in a variety of pathophysiology, such as cardiovascular disease, cerebral ischemia, tumor progression, and bone development [51–55]. Moreover, MMP-13 is involved in brain injury and neuronal death and counteracts the benefits of thrombolytic therapy [56]. MMP-13 expression is also related to an increase in diffusion-weighted image (DWI) lesion in the hyper acute phase of stroke [56]. Astrocytes exert a pivotal function in CNS, such as participation and maintenance of the integrity of the blood–brain barrier (BBB) [57]. Recently, Finsterwald et al. have proposed the potential of astrocytes as targets for the development of drugs treating neurodegenerative diseases [3]. Importantly, Ueno et al. [58] and our previous study [21] demonstrated that the expression of MMP-13 increases the BBB impairment in stroke model. The present study showed that IL-18 enhanced the protein and mRNA expression of MMP-13 and increased the zymographic activity in primary cultured astrocytes. Our results also demonstrated that MMP pan-inhibitor or MMP-13 inhibitor significantly antagonized the potentiating effect of astrocytic migration induced by IL-18 administration.
The effect of IL-18 on the activation of PKCδ was previously addressed [28]. Also, previous studies found that PKCδ activation is a necessary component in signaling MMP-13 expression [59, 60]. Importantly, PKCδ, but not PKCα/β, activation is a principal rate-limiting event in the basic fibroblast growth factor (bFGF)-dependent stimulation of MMP-13 in chondrocytes [61]. In this study, we found that production of MMP-13 and cell migration increased in response to IL-18 due to PKCδ activation in astrocytes. We demonstrated that IL-18-induced astrocytic migration is inhibited by the PKCδ inhibitor indicating that activation of PKCδ may be a mediator of migratory activity in response to IL-18 stimulation. Furthermore, Im et al. also demonstrated that c-Jun/AP-1 activation is associated with MMP-13 expression [61]. Our previous studies also indicate that c-Jun phosphorylation [21] and AP-1 activation [16, 18, 20] is a key modulator in transcription of MMP-13 expression. We also found that exposure of astrocytes to IL-18 increased c-Jun phosphorylation. Using an electrophoretic mobility shift assay (EMSA), we observed that IL-18 induced an increase in AP-1-DNA binding activity. Thus, our results suggest that in primary astrocytes, activation of PKCδ-dependent JNK and PI3 kinase/Akt and the c-Jun/AP-1 as downstream target regulatory molecules are essential for IL-18-induced MMP-13 gene expression and astrocytic migration.
In conclusion, MMP-13 expression increases in primary astrocytes under IL-18-stimulation. IL-18 has been detected in the microglia [62, 63] in the injured brains [7]. Therefore, IL-18 is implicated to be a key cytokine in modulating immunological pathways stimulated by cytotoxic and inflammatory responses under neuropathological condition [8]. Our results showed that astrocytes exposed to microglial-conditioned medium (mgCM) enhanced MMP-13 production. Furthermore, upregulation of IL-18 from microglial cells was initiated by lipopolysaccharide or peptidoglycan administration. Here, we provide evidence to demonstrate the novel regulatory action of MMP-13 in astrocytes in response to IL-18 treatment. Astrocytes appear to play a key role in the etiology of neurodegenerative diseases and psychiatry disorders, a growing interest has arisen for astrocyte-regulated pathways as therapeutic target for new drug development that contributes in the pathophysiology of treatment.
References
Sofroniew MV, Vinters HV (2010) Astrocytes: biology and pathology. Acta Neuropathol 119(1):7–35. doi:10.1007/s00401-009-0619-8
Burda JE, Bernstein AM, Sofroniew MV (2015) Astrocyte roles in traumatic brain injury. Exp Neurol. doi:10.1016/j.expneurol.2015.03.020
Finsterwald C, Magistretti PJ, Lengacher S (2015) Astrocytes: new targets for the treatment of neurodegenerative diseases. Curr Pham Des 21(25):3570–3581
Sofroniew MV (2014) Multiple roles for astrocytes as effectors of cytokines and inflammatory mediators. Neuroscientist 20(2):160–172. doi:10.1177/1073858413504466
Loihl AK, Murphy S (1998) Expression of nitric oxide synthase-2 in glia associated with CNS pathology. Prog Brain Res 118:253–267
Alboni S, Cervia D, Sugama S, Conti B (2010) Interleukin 18 in the CNS. J Neuroinflammation 7:9. doi:10.1186/1742-2094-7-9
Ryu HJ, Kim JE, Kim MJ, Kwon HJ, Suh SW, Song HK, Kang TC (2010) The protective effects of interleukin-18 and interferon-gamma on neuronal damages in the rat hippocampus following status epilepticus. Neuroscience 170(3):711–721. doi:10.1016/j.neuroscience.2010.07.048
Yatsiv I, Morganti-Kossmann MC, Perez D, Dinarello CA, Novick D, Rubinstein M, Otto VI, Rancan M et al (2002) Elevated intracranial IL-18 in humans and mice after traumatic brain injury and evidence of neuroprotective effects of IL-18-binding protein after experimental closed head injury. J Cereb Blood Flow Metab 22(8):971–978. doi:10.1097/00004647-200208000-00008
Jander S, Schroeter M, Stoll G (2002) Interleukin-18 expression after focal ischemia of the rat brain: association with the late-stage inflammatory response. J Cereb Blood Flow Metab 22(1):62–70. doi:10.1097/00004647-200201000-00008
Kast RE (2015) The role of interleukin-18 in glioblastoma pathology implies therapeutic potential of two old drugs-disulfiram and ritonavir. Chin J Cancer 34(4):161–165. doi:10.1186/s40880-015-0010-1
Ishida Y, Migita K, Izumi Y, Nakao K, Ida H, Kawakami A, Abiru S, Ishibashi H et al (2004) The role of IL-18 in the modulation of matrix metalloproteinases and migration of human natural killer (NK) cells. FEBS Lett 569(1–3):156–160. doi:10.1016/j.febslet.2004.05.039
Chandrasekar B, Mummidi S, Mahimainathan L, Patel DN, Bailey SR, Imam SZ, Greene WC, Valente AJ (2006) Interleukin-18-induced human coronary artery smooth muscle cell migration is dependent on NF-kappaB- and AP-1-mediated matrix metalloproteinase-9 expression and is inhibited by atorvastatin. J Biol Chem 281(22):15099–15109. doi:10.1074/jbc.M600200200
Ala-aho R, Kahari VM (2005) Collagenases in cancer. Biochimie 87(3–4):273–286. doi:10.1016/j.biochi.2004.12.009
Yong VW, Power C, Forsyth P, Edwards DR (2001) Metalloproteinases in biology and pathology of the nervous system. Nat Rev Neurosci 2(7):502–511. doi:10.1038/35081571
Sendon-Lago J, Seoane S, Eiro N, Bermudez MA, Macia M, Garcia-Caballero T, Vizoso FJ, Perez-Fernandez R (2014) Cancer progression by breast tumors with Pit-1-overexpression is blocked by inhibition of metalloproteinase (MMP)-13. Breast Cancer Res 16(6):505. doi:10.1186/s13058-014-0505-8
Hsieh WT, Yeh WL, Cheng RY, Lin C, Tsai CF, Huang BR, Wu CY, Lin HY et al (2014) Exogenous endothelin-1 induces cell migration and matrix metalloproteinase expression in U251 human glioblastoma multiforme. J Neuro-Oncol 118(2):257–269. doi:10.1007/s11060-014-1442-1
Tsai CF, Yeh WL, Chen JH, Lin C, Huang SS, Lu DY (2014) Osthole suppresses the migratory ability of human glioblastoma multiforme cells via inhibition of focal adhesion kinase-mediated matrix metalloproteinase-13 expression. Int J Mol Sci 15(3):3889–3903. doi:10.3390/ijms15033889
Lu DY, Leung YM, Cheung CW, Chen YR, Wong KL (2010) Glial cell line-derived neurotrophic factor induces cell migration and matrix metalloproteinase-13 expression in glioma cells. Biochem Pharmacol 80(8):1201–1209. doi:10.1016/j.bcp.2010.06.046
Yeh WL, Lu DY, Lee MJ, Fu WM (2009) Leptin induces migration and invasion of glioma cells through MMP-13 production. Glia 57(4):454–464. doi:10.1002/glia.20773
Chuang JY, Tsai CF, Chang SW, Chiang IP, Huang SM, Lin HY, Yeh WL, Lu DY (2013) Glial cell line-derived neurotrophic factor induces cell migration in human oral squamous cell carcinoma. Oral Oncol 49(12):1103–1112. doi:10.1016/j.oraloncology.2013.08.009
Lu DY, Yu WH, Yeh WL, Tang CH, Leung YM, Wong KL, Chen YF, Lai CH et al (2009) Hypoxia-induced matrix metalloproteinase-13 expression in astrocytes enhances permeability of brain endothelial cells. J Cell Physiol 220(1):163–173. doi:10.1002/jcp.21746
Griner EM, Kazanietz MG (2007) Protein kinase C and other diacylglycerol effectors in cancer. Nat Rev Cancer 7(4):281–294. doi:10.1038/nrc2110
Liu JF, Crepin M, Liu JM, Barritault D, Ledoux D (2002) FGF-2 and TPA induce matrix metalloproteinase-9 secretion in MCF-7 cells through PKC activation of the Ras/ERK pathway. Biochem Biophys Res Commun 293(4):1174–1182. doi:10.1016/s0006-291x(02)00350-9
Urtreger AJ, Grossoni VC, Falbo KB, Kazanietz MG, de Kier Joffe ED B (2005) Atypical protein kinase C-zeta modulates clonogenicity, motility, and secretion of proteolytic enzymes in murine mammary cells. Mol Carcinog 42(1):29–39. doi:10.1002/mc.20066
Sokolova O, Vieth M, Naumann M (2013) Protein kinase C isozymes regulate matrix metalloproteinase-1 expression and cell invasion in Helicobacter pylori infection. Gut 62(3):358–367. doi:10.1136/gutjnl-2012-302103
Wu LH, Lin C, Lin HY, Liu YS, Wu CY, Tsai CF, Chang PC, Yeh WL et al (2015) Naringenin suppresses neuroinflammatory responses through inducing suppressor of cytokine signaling 3 expression. Mol Neurobiol. doi:10.1007/s12035-014-9042-9
Moriya C, Jinnin M, Yamane K, Maruo K, Muchemwa FC, Igata T, Makino T, Fukushima S et al (2011) Expression of matrix metalloproteinase-13 is controlled by IL-13 via PI3K/Akt3 and PKC-delta in normal human dermal fibroblasts. J Invest Dermatol 131(3):655–661. doi:10.1038/jid.2010.361
Amin MA, Mansfield PJ, Pakozdi A, Campbell PL, Ahmed S, Martinez RJ, Koch AE (2007) Interleukin-18 induces angiogenic factors in rheumatoid arthritis synovial tissue fibroblasts via distinct signaling pathways. Arthritis Rheum 56(6):1787–1797. doi:10.1002/art.22705
Hamby ME, Uliasz TF, Hewett SJ, Hewett JA (2006) Characterization of an improved procedure for the removal of microglia from confluent monolayers of primary astrocytes. J Neurosci Methods 150(1):128–137
Chen PS, Peng GS, Li G, Yang S, Wu X, Wang CC, Wilson B, Lu RB et al (2006) Valproate protects dopaminergic neurons in midbrain neuron/glia cultures by stimulating the release of neurotrophic factors from astrocytes. Mol Psychiatry 11(12):1116–1125
Hsu HH, Liu CJ, Shen CY, Chen YJ, Chen LM, Kuo WH, Lin YM, Chen RJ et al (2012) p38alpha MAPK mediates 17beta-estradiol inhibition of MMP-2 and -9 expression and cell migration in human lovo colon cancer cells. J Cell Physiol 227(11):3648–3660. doi:10.1002/jcp.24072
Lin HY, Tang CH, Chen JH, Chuang JY, Huang SM, Tan TW, Lai CH, Lu DY (2011) Peptidoglycan induces interleukin-6 expression through the TLR2 receptor, JNK, c-Jun, and AP-1 pathways in microglia. J Cell Physiol 226(6):1573–1582. doi:10.1002/jcp.22489
Zhou J, Ping FF, Lv WT, Feng JY, Shang J (2014) Interleukin-18 directly protects cortical neurons by activating PI3K/AKT/NF-kappaB/CREB pathways. Cytokine 69(1):29–38. doi:10.1016/j.cyto.2014.05.003
Amin MA, Rabquer BJ, Mansfield PJ, Ruth JH, Marotte H, Haas CS, Reamer EN, Koch AE (2010) Interleukin 18 induces angiogenesis in vitro and in vivo via Src and Jnk kinases. Ann Rheum Dis 69(12):2204–2212. doi:10.1136/ard.2009.127241
Xia S, Forman LW, Faller DV (2007) Protein kinase C delta is required for survival of cells expressing activated p21RAS. J Biol Chem 282(18):13199–13210. doi:10.1074/jbc.M610225200
Mitsutake N, Namba H, Shklyaev SS, Tsukazaki T, Ohtsuru A, Ohba M, Kuroki T, Ayabe H et al (2001) PKC delta mediates ionizing radiation-induced activation of c-Jun NH(2)-terminal kinase through MKK7 in human thyroid cells. Oncogene 20(8):989–996. doi:10.1038/sj.onc.1204179
Das S, Mishra MK, Ghosh J, Basu A (2008) Japanese encephalitis virus infection induces IL-18 and IL-1beta in microglia and astrocytes: correlation with in vitro cytokine responsiveness of glial cells and subsequent neuronal death. J Neuroimmunol 195(1–2):60–72. doi:10.1016/j.jneuroim.2008.01.009
Yeh WL, Lu DY, Liou HC, Fu WM (2012) A forward loop between glioma and microglia: glioma-derived extracellular matrix-activated microglia secrete IL-18 to enhance the migration of glioma cells. J Cell Physiol 227(2):558–568. doi:10.1002/jcp.22746
Dai SM, Shan ZZ, Nishioka K, Yudoh K (2005) Implication of interleukin 18 in production of matrix metalloproteinases in articular chondrocytes in arthritis: direct effect on chondrocytes may not be pivotal. Ann Rheum Dis 64(5):735–742. doi:10.1136/ard.2004.026088
Frank-Cannon TC, Alto LT, McAlpine FE, Tansey MG (2009) Does neuroinflammation fan the flame in neurodegenerative diseases? Mol Neurodegener 4:47. doi:10.1186/1750-1326-4-47
Walker AK, Kavelaars A, Heijnen CJ, Dantzer R (2014) Neuroinflammation and comorbidity of pain and depression. Pharmacol Rev 66(1):80–101. doi:10.1124/pr.113.008144
Ownby RL (2010) Neuroinflammation and cognitive aging. Curr Psychiatry Rep 12(1):39–45. doi:10.1007/s11920-009-0082-1
Hein AM, O’Banion MK (2009) Neuroinflammation and memory: the role of prostaglandins. Mol Neurobiol 40(1):15–32. doi:10.1007/s12035-009-8066-z
Biesmans S, Meert TF, Bouwknecht JA, Acton PD, Davoodi N, De Haes P, Kuijlaars J, Langlois X et al (2013) Systemic immune activation leads to neuroinflammation and sickness behavior in mice. Mediat Inflamm 2013:271359. doi:10.1155/2013/271359
Sparkman NL, Johnson RW (2008) Neuroinflammation associated with aging sensitizes the brain to the effects of infection or stress. Neuroimmunomodulation 15(4–6):323–330. doi:10.1159/000156474
Arend WP, Palmer G, Gabay C (2008) IL-1, IL-18, and IL-33 families of cytokines. Immunol Rev 223:20–38. doi:10.1111/j.1600-065X.2008.00624.x
Dinarello CA (2000) Interleukin-18, a proinflammatory cytokine. Eur Cytokine Netw 11(3):483–486
Meraz-Rios MA, Toral-Rios D, Franco-Bocanegra D, Villeda-Hernandez J, Campos-Pena V (2013) Inflammatory process in Alzheimer’s disease. Front Integr Neurosci 7:59. doi:10.3389/fnint.2013.00059
Felderhoff-Mueser U, Schmidt OI, Oberholzer A, Buhrer C, Stahel PF (2005) IL-18: a key player in neuroinflammation and neurodegeneration? Trends Neurosci 28(9):487–493. doi:10.1016/j.tins.2005.06.008
Zhang Y, Liu L, Peng YL, Liu YZ, Wu TY, Shen XL, Zhou JR, Sun DY et al (2014) Involvement of inflammasome activation in lipopolysaccharide-induced mice depressive-like behaviors. CNS Neurosci Ther 20(2):119–124. doi:10.1111/cns.12170
Spinale FG (2002) Matrix metalloproteinases: regulation and dysregulation in the failing heart. Circ Res 90(5):520–530
Brinckerhoff CE, Rutter JL, Benbow U (2000) Interstitial collagenases as markers of tumor progression. Clin Cancer Res 6(12):4823–4830
Stickens D, Behonick DJ, Ortega N, Heyer B, Hartenstein B, Yu Y, Fosang AJ, Schorpp-Kistner M et al (2004) Altered endochondral bone development in matrix metalloproteinase 13-deficient mice. Development 131(23):5883–5895
Tromp G, Gatalica Z, Skunca M, Berguer R, Siegel T, Kline RA, Kuivaniemi H (2004) Elevated expression of matrix metalloproteinase-13 in abdominal aortic aneurysms. Ann Vasc Surg 18(4):414–420
Hamann GF, Okada Y, Fitridge R, del Zoppo GJ (1995) Microvascular basal lamina antigens disappear during cerebral ischemia and reperfusion. Stroke 26(11):2120–2126
Rosell A, Alvarez-Sabin J, Arenillas JF, Rovira A, Delgado P, Fernandez-Cadenas I, Penalba A, Molina CA et al (2005) A matrix metalloproteinase protein array reveals a strong relation between MMP-9 and MMP-13 with diffusion-weighted image lesion increase in human stroke. Stroke 36(7):1415–1420
Cserr HF, Bunggaard M (1986) The neuronal microenvironment: a comparative view. Ann N Y Acad Sci 481:1–6
Ueno M, Wu B, Nishiyama A, Huang CL, Hosomi N, Kusaka T, Nakagawa T, Onodera M et al (2009) The expression of matrix metalloproteinase-13 is increased in vessels with blood–brain barrier impairment in a stroke-prone hypertensive model. Hypertens Res 32(5):332–338. doi:10.1038/hr.2009.26
Yang CM, Hsieh HL, Yao CC, Hsiao LD, Tseng CP, Wu CB (2009) Protein kinase C-delta transactivates platelet-derived growth factor receptor-alpha in mechanical strain-induced collagenase 3 (matrix metalloproteinase-13) expression by osteoblast-like cells. J Biol Chem 284(38):26040–26050. doi:10.1074/jbc.M109.040154
Huang CY, Lin HJ, Chen HS, Cheng SY, Hsu HC, Tang CH (2013) Thrombin promotes matrix metalloproteinase-13 expression through the PKCdelta c-Src/EGFR/PI3K/Akt/AP-1 signaling pathway in human chondrocytes. Mediat Inflamm 2013:326041. doi:10.1155/2013/326041
Im HJ, Muddasani P, Natarajan V, Schmid TM, Block JA, Davis F, van Wijnen AJ, Loeser RF (2007) Basic fibroblast growth factor stimulates matrix metalloproteinase-13 via the molecular cross-talk between the mitogen-activated protein kinases and protein kinase Cdelta pathways in human adult articular chondrocytes. J Biol Chem 282(15):11110–11121. doi:10.1074/jbc.M609040200
Wheeler RD, Culhane AC, Hall MD, Pickering-Brown S, Rothwell NJ, Luheshi GN (2000) Detection of the interleukin 18 family in rat brain by RT-PCR. Brain Res Mol Brain Res 77(2):290–293
Conti B, Park LC, Calingasan NY, Kim Y, Kim H, Bae Y, Gibson GE, Joh TH (1999) Cultures of astrocytes and microglia express interleukin 18. Brain Res Mol Brain Res 67(1):46–52
Acknowledgments
This work is supported in part by grants from the National Science Council (NSC 102-2320-B-039-051-MY3, NSC 102-2320-B-039-026-MY3, NSC 103-2811-B-039-021, and NSC 104-2320-B-468 -002), China Medical University (CMU103-ASIA-02), and Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW104-TDU-B-212-113002). The authors thank Ms Y.-R Chen and Ms S.-H. Ko for the technical support.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors report that they have no competing interests.
Additional information
Jia-Hong Chen and Chon-Haw Tsai contributed equally to this work.
Rights and permissions
About this article
Cite this article
Chen, JH., Tsai, CH., Lin, HY. et al. Interlukin-18 Is a Pivot Regulatory Factor on Matrix Metalloproteinase-13 Expression and Brain Astrocytic Migration. Mol Neurobiol 53, 6218–6227 (2016). https://doi.org/10.1007/s12035-015-9529-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9529-z