Abstract
The recruitment of neutrophils by endothelial cells during infection has been extensively studied, but little is known about the regulation of neutrophils activity by endothelial cells. To examine the role of microvascular endothelial cells in neutrophil killing, we established a transmigration model using rat intestinal microvascular endothelial cells (RIMVECs) and measured the extracellular and intracellular killing of Escherichia coli, Lactobacillus acidophilus, and Staphylococcus aureus by transendothelial neutrophils. We observed that blood neutrophils engulfed bacteria but did not kill them, and lipopolysaccharide- or hemolysin-injured RIMVECs inhibited the extracellular and intracellular bactericidal activity of transendothelial neutrophils. In comparison, interleukin-1α-induced RIMVECs promoted the extracellular and intracellular killing activity of transendothelial neutrophils and significantly increased MMP-9 concentration and lysozyme activity in transendothelial neutrophils (p < 0.01 and p < 0.001, respectively). Our results demonstrated that activation of endothelial cells enhanced bactericidal activity of transendothelial neutrophils and bacterial toxin damage of endothelial cells led to reduction in bactericidal activity of transendothelial neutrophils. These findings offered new insight into the role of endothelial cells in the bactericidal activity of neutrophils.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neutrophils, or polymorphonuclear leukocytes, are essential effector cells in innate immune system and serve as the initial defense against infectious pathogens. Upon infection, these highly motile cells are rapidly recruited to infection sites and destroy invading pathogens through intracellular or extracellular mechanism [1]. Both intracellular and extracellular neutrophil killing require participation of neutrophil granules. Intracellular killing occurs when antimicrobial proteins are released from granules into the phagocytic vesicles containing engulfed microorganisms, while extracellular killing involves release of granule proteins through exocytosis [2].
Microvascular endothelial cells (MVECs) are often the targets of the toxins and other virulence factors that were produced by pathogenic bacteria [3–5]. In the case of pathogenic bacterial infection, neutrophils are recruited to the infection site and migrate across the vascular endothelium [6]. Endothelium is the main barrier that neutrophils must enter to reach the area where their antimicrobial activity is needed for the elimination of infection [7]. Many researchers have studied the role of the endothelial cells in neutrophil recruitment and revealed that neutrophils interact with activated endothelial cells mainly through adhesion, rolling, and transmigration [7–10]. However, little is known with regard to the regulation of neutrophil activity by endothelial cells [11–15].
In this study, we utilized a transmigration model to examine the bactericidal activities of blood and transendothelial neutrophils. Matrix metalloprotein-9 (MMP-9) concentration and lysozyme activity of the transendothelial neutrophils were also determined. Our findings offered new insight into the role of endothelial cells in the bactericidal activity of neutrophils.
Materials and methods
Animals
Healthy Swiss albino rats (t) of age between 1 and 2 months and weighing between 30 and 40 g were employed in this study. All rats were purchased from the Academy of Military Medical Sciences, Beijing, China (certificate number: SCXK-PLA 2012-0004). The experiment was approved by the Committee for the Care and Use of Experimental Animals at Beijing University of Agriculture.
Biological reagents
Media used for endothelial cell culture and neutrophil isolation were obtained from Amersham Pharmacia Biotech (Little Chalfont, UK) and Gibco (Basel, Switzerland). Media used for bacteria culture were obtained from Sigma-Aldrich (Sigma, St. Louis, USA). Lipopolysaccharide (LPS, E. coli serotype O55:B5), α-hemolysin (HLα, Staphylococcus aureus), and interleukin-1α (IL-1α, rat recombinant, expressed in E. coli) were purchased from Sigma-Aldrich.
Isolation of rat neutrophils
Rat neutrophils were freshly isolated from heparinized whole blood of healthy rats by gradient centrifugation using Percoll (GE Healthcare, Little Chalfont, UK) as described [16, 17]. In brief, red blood cells were removed by addition of 4 % Dextran T-500 and incubation at 4 °C for 4 min. The white blood cells in suspension were collected and subjected to two rounds of Percoll gradient centrifugation at densities of 1.11 g/mL (89 %) and 1.09 g/mL (69 %) and centrifugation at 700×g for 40 min. Neutrophils were collected from the precipitate and washed with 5 mL of PBS. The purity of neutrophil was determined by the Switzerland staining as described [18], and the activity of neutrophil was determined by trypan blue exclusion staining as described [19].
Cells culture
Rat intestinal microvascular endothelial cells (RIMVECs) were obtained from our laboratory as described [20, 21]. Primary cells were identified by phase contrast photomicrograph using an Olympus IX71 inverted microscope (Olympus, Shinjuku, Japan) and the presence of factors VIII and CD34 probed by anti-CD31 antibody (HEC7) and goat anti-mouse IgG H&L (FITC) (Abcam, Cambridge, UK) using immunofluorescence [22]. RIMVECs were cultured from passages 13–15 and maintained in DMEM medium supplemented with 20 % heat-inactivated fetal bovine serum (FBS), 2 mM l-glutamine, and 1 % antibiotics (Life Technologies, USA).
Neutrophil phagocytosis assay
E. coli, L. acidophilus, and S. aureus were cultivated at 37 °C with shaking at 200 rpm in de Man, Rogosa, Sharpe (MRS) or Luria–Bertani (LB) media and reached an intensity of 1 × 103 CFU/mL. Four hundred microliters of blood neutrophils (1 × 106 cells/mL) was treated with 10 μL of bacterial culture in 24-well plates for 3, 6, 9, or 16 h at 37 °C in a 5 % CO2 atmosphere [23].
Measurement of lactate dehydrogenase (LDH) levels
RIMVECs were seeded at an intensity of 1 × 104 cells/well in 96-well plates. Cells were incubated for 6 h to reach confluence and form a monolayer. Subsequently, cells were stimulated by the addition of LPS (0.01 μg/mL–1.0 mg/mL), HLα (0.1 ng/mL–10.0 μg/mL), or IL-1α (0.01 ng/mL–1.0 μg/mL). After incubation at 37 °C for 4 h, cell culture supernatants were collected to measure the LDH level using a microplate reader at 490 nm wavelength. Cytotoxicity was calculated using the formula: cytotoxicity (%) = (absorbance of treated sample − absorbance of the control well)/(absorbance maximum cell activity − absorbance of the control well).
Measurement of transendothelial electrical resistance (TEER) levels
TEER was measured using the Millicell Electrical Resistance System (ERS)-2 (EMD Millipore, Billerica, USA). RIMVECs were seeded at an intensity of 1 × 104 cells/well in 96-well plates. The culture medium was replaced with a reduced serum content (2 %) medium, and plates were incubated overnight. RIMVECs were stimulated with LPS, HLα, or IL-1α at the concentrations stated above at 37 °C for 4 h, and the TEER of RIMVECs was measured according to the manufacturer’s instructions.
Neutrophil transmigration assay
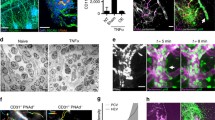
RIMVECs (1 × 104 cells/well) were grown in 24-well plates at 37 °C for 48 h to reach confluence and form a monolayer on 5.0-μm-pore-size polycarbonate resin transwell membranes (Corning, Corning, USA). RIMVECs were treated with LPS (1 μg/mL), HLα (100 ng/mL), or IL-1α (10 ng/mL) for 4 h and then washed with Hanks’ balanced salt solution (HBSS) without Ca2+ and Mg2+. Neutrophils (1 × 106 cells/well) were added to the upper chamber and incubated for additional 4 h [24]. Neutrophils that crossed the polycarbonate filter through the RIMVEC monolayer into the lower compartment were collected and counted using a hemocytometer (Fig. 1).
a Illustration of in vitro neutrophil transmigration model. RIMVECs were grown on a transwell filter until formation of a monolayer. After different simulations were added in upper chamber to treat RIMVECs for 4 h, neutrophils were added to upper chamber and allowed to migrate for another 4 h. Bacteria were then added to the lower chamber and incubated with transendothelial neutrophils at 37 °C for 3 h. b Phase contrast photomicrograph of unstained RIMVECs. c Indirect immunofluorescence staining of CD34 antigen. d Indirect immunofluorescence staining of factor VIII antigen
Bacterial killing assay
Neutrophils collected from the lower chamber of the transwell in the transmigration assay were defined as transendothelial neutrophils and were examined for bactericidal activity. Ten microliters of E. coli, L. acidophilus, or S. aureus (1 × 103 CFU/mL) was incubated with 400 μL of transendothelial neutrophils (1 × 106 cells/mL) for 3 h, respectively. Each of the bacteria/neutrophil mixture was divided into two equal volumes. Half was used to test extracellular bacterial survival by plating the mixture onto agar plate that is appropriate for the bacterium being examined (LB or MRS). The other half was used to detect intracellular bacterial survival. To measure intracellular bacterial survival, penicillin–streptomycin (final concentration of 50–100 μg/mL) was added to the bacteria/neutrophil mixture, following incubation at 37 °C in a CO2 incubator for 2 h. After washing with HBSS to remove the antibiotics, RIPA lysis buffer was added to the mixture to lyse the neutrophils and release intracellular bacteria. Cell lysates were spread onto agar plate and incubated overnight at 37 °C, and bacterial colonies were counted.
ELISA
A Rat Total MMP-9 ELISA Kit (RMP900) (R&D Systems, Abingdon, UK) was used for ELISA. In the transmigration assay, a total of 50 μL of the supernatant collected from the lower chamber after neutrophils crossed the RIMVEC layer was used to measure MMP-9 concentration according to the manufacturer’s instructions.
Fluorometric lysozyme assay
An EnzChek Lysozyme Assay Kit (Molecular Probes, Eugene, USA) was used to assess the lysozyme activity of transendothelial neutrophils. Lysozyme substrate (1 mg of Micrococcus lysodeikticus) and reaction buffer (0.1 M sodium phosphate, 0.1 M NaCl (pH 7.5), and 2 mM sodium azide) were prepared according to the manufacturer’s instructions. Digestion products from the lysozyme substrate were detected by a fluorescence microplate reader (Life Science & Technology, Swindon, UK) at excitation wavelength of 494 nm and emission wavelength of 518 nm [25].
Statistical analysis
Significant differences between groups were calculated using unpaired t test (two groups) or one-way ANOVA (multiple groups) using GraphPad Prism 6.0 software (GraphPad Software, La Jolla, USA). Values are expressed as column diagram (*p < 0.05; **p < 0.01; ***p < 0.001).
Results
Bacteria were engulfed but not degraded by blood neutrophils
To test whether the fresh blood neutrophils that have no interaction with the endothelial cells kill the bacteria, we conducted a neutrophil phagocytosis assay using E. coli, L. Acidophilus, and S. Aureus strains. As shown in Fig. 2b–d, the rat blood neutrophils engulfed three strains of bacteria compared with the negative control (Fig. 2a). To further examine whether these bacteria survive inside the blood neutrophils, neutrophils were cultured with respective bacteria for 3, 6, 9, or 12 h and lysed, and bacteria growth was measured by spectrophotometry (Fig. 2e). We observed that all tested bacteria continued to proliferate inside neutrophils.
Blood neutrophils engulfed bacteria, and bacteria survived inside blood neutrophils. Rat blood neutrophils (>95 % purity) were incubated with E. coli, L. acidophilus, or S. aureus for 3 h. Neutrophils were stained by Switzerland staining and observed by optical microscope (× 1000). a Negative control (no bacteria). b Blood neutrophils incubated with E. coli. c Blood neutrophils incubated with L. acidophilus. d Blood neutrophils incubated with S. aureus. e Blood neutrophils were incubated with bacteria for 3, 6, 9, or 12 h and lysed, and absorbance was measured by UV spectrophotometer (λ = 600 nm) (n = 3)
RIMVECs were injured by LPS and HLα but not IL-1α
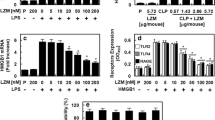
Primary RIMVECs were identified using phase contrast photomicrograph (Fig. 1b) and the CD34 (Fig. 1c) and VIII (Fig. 1d) immunofluorescence staining. Two different methods were used to measure the RIMVEC injury following stimulation with LPS, HLα, or IL-1α at different concentrations. First, release of LDH from injured RIMVECs, an important indicator of membrane integrity, was measured. As shown in Fig. 3a, treatments with LPS (1 μg/mL–1 mg/mL) and HLα (100 ng/mL–10 μg/mL) showed greater than 50 % cytotoxicity against RIMVECs, whereas treatment with IL-1α only showed less than 20 % at the concentrations that were tested (10 ng/mL–1 μg/mL). Generally, LPS and HLα showed greater cytotoxicity than IL-1α; for example, at 1 μg/mL concentration, LPS, HLα, and IL-1α caused 65.3, 65.0, and 12.5 % LDH release in RIMVECs, respectively. Second, the transendothelial electrical resistance (TEER) of RIMVECs was measured to determine the confluence and health status of RIMVECs (Fig. 3b). Similarly, TEER of RIMVECs was significantly decreased compared with the control after treatment with LPS (1 μg/mL–1 mg/mL) or HLα (100 ng/mL–10 μg/mL) (p < 0.001 and p < 0.01, respectively), but there was no significant change in TEER of RIMVECs treated with IL-1α (10 ng/mL–1 μg/mL). These results indicated that LPS and HLα caused injury to RIMVECs, whereas IL-1α did not.
Cytotoxic effectors of LPS, HLα, and IL-1α. a Effect of LPS, HLα, and IL-1α on lactate dehydrogenase (LDH) release by RIMVECs. RIMVECs were incubated with LPS, HLα, or IL-1α at different concentrations for 4 h. Supernatant was collected to detect LDH release. Absorbance was measured by ultraviolet spectrophotometer (λ = 490 nm). All absorbance values are given relative to the maximum LDH release of the cell. b Transendothelial electrical resistance (TEER) of RIMVECs stimulated by LPS, HLα, or IL-1α. Confluent monolayers of RIMVECs on transwell inserts were maintained for 48 h and then treated with different concentrations of LPS, HLα, or IL-1α for 4 h. Error bars represent SEM (n = 3 or 6). **p < 0.01 (compared with non-stimulated cells)
Injury to RIMVECs inhibited bacterial degradation by transendothelial neutrophils
To investigate whether there is a correlation between the injury of endothelial cells and the reduction in bactericidal activity of neutrophils, we established a transmigration model using LPS- and HLα-injured RIMVECs. Bacteria were incubated with neutrophils that had traversed the damaged RIMVEC monolayer, and both intracellular and extracellular survival of bacteria was monitored by bacteria colony counts. Our results showed that there was no significant difference in extracellular bacterial survival compared with controls (Fig. 4a), while intracellular survival was significantly increased (p < 0.01, p < 0.01, or p < 0.001) (Fig. 4b).
Evaluation of bacteria killing activity of neutrophils interacted with LPS or HLα. RIMVECs on transwell chambers were stimulated by LPS (1 μg/mL) or HLα (100 ng/mL) for 4 h. Neutrophils were added to the upper chamber and allowed to migrate across the endothelial cells for 4 h. Transendothelial neutrophils were collected and incubated with E. coli, L. acidophilus, or S. aureus for 3 h, and bacterial survival was determined by colony counts (CFU/mL). a Colony counts of extracellular bacteria incubated with transendothelial neutrophils. b Colony counts of intracellular bacteria incubated with transendothelial neutrophils. Error bars represent SEM from more than three independent experiments. **p < 0.01, values represent ≥ three independent determinations in duplicate ±SEM
IL-1α-induced RIMVECs promoted transendothelial neutrophil killing of S. aureus and L. acidophilus
To investigate the effect of activated RIMVECs on the bactericidal activity of transendothelial neutrophils, we repeated the above experiment using IL-1α-induced RIMVECs instead of HLα- or LPS-injured RIMVECs. After co-culture of bacteria with transendothelial neutrophils that had traversed IL-1α-induced RIMVECs, we observed that both extracellular (Fig. 5a) and intracellular (Fig. 5b) survival of S. aureus and L. acidophilus was significantly reduced compared with controls (p < 0.001). However, no such effect was observed in E. coli. To further confirm that neutrophil killing is promoted by the IL-1α-activated endothelial cells, we examined the bactericidal activity of the blood neutrophils incubated with IL-1α alone. Our results showed that there was no significant difference in both extracellular (Fig. 5c) and intracellular (Fig. 5d) bacteria killing in neutrophils treated with IL-1α alone compared with the control.
Evaluation of bacteria killing activity of neutrophils interacted with IL-1α. Transwell chambers were pretreated with IL-1α (10 ng/mL) for 4 h. Neutrophils were added to the upper chamber and allowed to migrate across RIMVEC monolayer for 4 h. Transendothelial neutrophils were collected and incubated with E. coli, L. acidophilus, or S. aureus for 3 h, and bacterial survival was assessed by colony counts (CFU/mL). a Colony counts of extracellular bacteria incubated with transendothelial neutrophils. b Colony counts of intracellular bacteria incubated with transendothelial neutrophils. As control, blood neutrophils were pretreated with IL-1α for 4 h and then incubated with bacteria for 3 h. Bacterial survival was assessed by colony counts (CFU/mL). c Colony counts of extracellular bacteria incubated with blood neutrophils. d Colony counts of intracellular bacteria incubated with blood neutrophils. Error bars represent SEM from more than three independent experiments. ***p < 0.001, values represent ≥ three independent determinations in duplicate ±SEM
IL-1α-induced RIMVECs increased MMP-9 concentration and lysozyme activity in neutrophils
Next, we investigated the effect of IL-1α-induced RIMVECs on granule enzyme release in transendothelial neutrophils. Specifically, we examined the levels of MMP-9 and lysozyme in the supernatants of transendothelial neutrophils using the ELISA and fluorometric lysozyme assay, respectively. We observed that both MMP-9 concentration (Fig. 6a) and lysozyme activity (Fig. 6b) were significantly increased in the presence of IL-1α-induced RIMVECs compared with the control (p < 0.01 or p < 0.001), whereas no significant difference was observed in the presence of LPS- and HLα-injured RIMVECs.
a Concentrations of MMP-9 in transendothelial neutrophil. b Lysozyme activity of transendothelial neutrophils. After RIMVECs were incubated with LPS, HLα, and IL-1α, blood neutrophils were added to the transwell upper chamber to migrate the cells. The neutrophil collection from down chamber was used to determine the concentrations of MMP-9 and lysozyme. Error bars represent SEM from more than three independent experiments. Error bars represent SEM from more than three independent experiments. **p < 0.01; ***p < 0.001
Discussion
Neutrophils are essential innate immune cells that are required in defending the body against intruding microorganisms [26]. Neutrophils are generated in the bone marrow and circulate in the blood. In response to inflammatory signals, they migrate from blood vessels and cross the endothelium barrier to reach the infection sites [27]. Neutrophil transendothelial migration is an important physiological process that triggers the recruitment of neutrophils. Endothelial cells can promote neutrophil morphological changes and release signaling molecules that are necessary for inducing neutrophil attachment and migration, thereby playing a critical role in neutrophil transendothelial migration [28]. After migrating to the infection sites, neutrophils engulf bacteria and produce granules containing antibiotic and cytotoxic enzymes to degrade bacteria [29, 30]. However, phagocytosis may not immediately result in bacterial killing [31]. In the present study, we observed that blood neutrophils engulfed bacteria but did not digest them, as evidenced by the continuous growth of intracellular bacteria, suggesting that the bactericidal function of blood neutrophils is not fully activated. Therefore, some specific activation process must be needed for neutrophils to fulfill their bacterial killing function.
Endothelial cells are the target of toxins secreted from pathogenic bacteria [32–34]. The phenotype characteristics of injured endothelial cells are cell membrane damage and permeability change. Therefore, we measured the LDH release and TEER of RIMVECs to evaluate the cell injury. The results show that LPS from E. coli and HLα from S. aureus significantly injured the endothelial cells with LDH release increased, and TEER was declined (Fig. 3). The main strategies that bacteria escape neutrophil killing include surviving inside the phagosome [35] or preventing recruitment of neutrophils to the site of infection [36]. In the present study, we showed that there was a correlation between endothelial cell damage and deactivation of neutrophil killing. Neutrophils that crossed an LPS- or HLα-injured endothelial cell monolayer neither killed extracellular bacteria nor degraded the intracellular bacteria that were phagocytosed. On the contrary, the intracellular bacteria survival even increased. It can be hypothesized that the toxins or other cytotoxic products secreted by pathogenic bacteria may aim at damaging the endothelial cells, leading to a reduction in the activation of neutrophil killing, thereby allowing the pathogens to survive.
Previous studies on the relationship between endothelial cells and neutrophils mainly focused on the recruitment of neutrophils by endothelial cells, including adhesion, arrest, scrolling, and migration [37–45]. Here, we showed that migration across the activated endothelial cell monolayer was needed to activate the bactericidal activity of neutrophils. Compared with blood neutrophils or neutrophils that crossed LPS- or HLα-injured endothelial cells, only neutrophils that crossed IL-1α-induced endothelial cells showed increased extracellular and intracellular bactericidal activity. Interestingly, the bactericidal activity was selective to Gram-positive bacteria (L. acidophilus and S. aureus), and Gram-negative bacteria (E. coli) were not eliminated by the activated neutrophils. Whether a different cytokine can stimulate endothelial cells and subsequently activate neutrophil killing of Gram-negative bacteria remains unknown. Following stimulation, neutrophils release three types of granules, and the main granule type is called tertiary granule. MMPs, including MMP-9 and proMMP-9, are the main proteins in tertiary granules and are necessary for migration of neutrophils [46–49]. Another marker of neutrophil killing function activation is lysozyme, which is a key bactericidal enzyme present in all three types of neutrophil granule, and has greater activity against Gram-positive bacteria than Gram-negative bacteria [29, 30].
IL-1α is involved in many physiological or pathology process, such as inflammation, and immunoregulation. In addition, a number of researchers also reported that IL-1-activated endothelial cells produced IL-8 and MIP-2, which subsequently activated neutrophils and promoted neutrophil migration across endothelial cell barriers [43, 49–52]. Our data revealed that IL-1α-activated vascular endothelial cells were required to kill bacteria. Therefore, the potential benefit that IL-1α with this conclusion is valuable. The commercialization of antagonist of IL-1 is more useable with the anti-inflammatory drugs or bactericidal drugs. On another side, some upstream or downstream factors in IL-1 signaling pathway are also the target of clinical application.
In conclusion, we demonstrated that IL-1α-activated vascular endothelial cells were required in the regulation of neutrophil killing of Gram-positive bacteria. To date, most bacterial infections have been treated with antibiotics, and overuse of these drugs has led to the evolution of resistant bacteria, which in turn produce toxins that are even more harmful to human health. Our findings may help to elucidate the mechanism of bactericidal effects of neutrophils and the development of alternative antimicrobial drugs that target promoting neutrophil activation.
Abbreviations
- MVECs:
-
Microvascular endothelial cells
- RIMVECs:
-
Rat intestinal microvascular endothelial cells
- LPS:
-
Lipopolysaccharide
- HLα:
-
α-Hemolysin
- IL-1α:
-
Interleukin-1 alpha
- LDH:
-
Lactate dehydrogenase
- TEER:
-
Transendothelial electrical resistance
- MMP-9:
-
Matrix metalloproteinases-9
- E. coli :
-
Escherichia coli
- L. acidophilus :
-
Lactobacillus acidophilus
- S. aureus :
-
Staphylococcus aureus
References
Hostetter SJ. Neutrophil function in small animals. Vet Clin N Am Small Animal Prac. 2012;42:157.
Segal AW. How neutrophils kill microbes. Annu Rev Immunol. 2005;23:197.
Peacock SJ, Foster TJ, Cameron BJ, Berendt AR. Bacterial fibronectin-binding proteins and endothelial cell surface fibronectin mediate adherence of Staphylococcus aureus to resting human endothelial cells. Microbiology. 1999;145(Pt 12):3477.
Cromer WE, Mathis JM, Granger DN, Chaitanya GV, Alexander JS. Role of the endothelium in inflammatory bowel diseases. World J Gastroenterol. 2011;17:578.
Reddy AT, Lakshmi SP, Kleinhenz JM, Sutliff RL, Hart CM, Reddy RC. Endothelial cell peroxisome proliferator-activated receptor gamma reduces endotoxemic pulmonary inflammation and injury. J Immunol. 2012;189:5411.
Borregaard N. Neutrophils, from marrow to microbes. Immunity. 2010;33:657.
Amulic B, Cazalet C, Hayes GL, Metzler KD, Zychlinsky A. Neutrophil function: from mechanisms to disease. Annu Rev Immunol. 2012;30:459–89.
Mcever RP. Selectins: initiators of leucocyte adhesion and signalling at the vascular wall. Cardiovasc Res. 2015;107:331–9.
Marki A, Esko JD, Pries AR, Ley K. Role of the endothelial surface layer in neutrophil recruitment. J Leukoc Biol. 2015;98:503–15.
Nourshargh S, Alon R. Leukocyte migration into inflamed tissues. Immunity. 2014;41:694.
Cheng Q, McKeown SJ, Santos L, Santiago FS, Khachigian LM, Morand EF, Hickey MJ. Macrophage migration inhibitory factor increases leukocyte-endothelial interactions in human endothelial cells via promotion of expression of adhesion molecules. J Immunol. 2010;185:1238.
Yang L, Kowalski JR, Yacono P, Bajmoczi M, Shaw SK, Froio RM, Golan DE, Thomas SM, Luscinskas FW. Endothelial cell cortactin coordinates intercellular adhesion molecule-1 clustering and actin cytoskeleton remodeling during polymorphonuclear leukocyte adhesion and transmigration. J Immunol. 2006;177:6440.
Roussel L, Houle F, Chan C, Yao Y, Berube J, Olivenstein R, Martin JG, Huot J, Hamid Q, Ferri L, Rousseau S. IL-17 promotes p38 MAPK-dependent endothelial activation enhancing neutrophil recruitment to sites of inflammation. J Immunol. 2010;184:4531.
Williams MR, Azcutia V, Newton G, Alcaide P, Luscinskas FW. Emerging mechanisms of neutrophil recruitment across endothelium. Trends Immunol. 2011;32:461.
Jerke U, Rolle S, Purfurst B, Luft FC, Nauseef WM, Kettritz R. Beta2 integrin-mediated cell-cell contact transfers active myeloperoxidase from neutrophils to endothelial cells. J Biol Chem. 2013;288:12910.
Nauseef WM. Isolation of human neutrophils from venous blood. Methods Mol Biol. 2014;1124:13.
Cotter MJ, Norman KE, Hellewell PG, Ridger VC. A novel method for isolation of neutrophils from murine blood using negative immunomagnetic separation. Am J Pathol. 2001;159:473.
Kimura I, Moritani Y, Tanizaki Y. Basophils in bronchial asthma with reference to reagin-type allergy. Clin Allergy. 1973;3(2):195–202.
Metcalf JA. Laboratory manual of neutrophil function. Raven Press; 1986.
Suo ZW, et al. Effect of berberine on nitric oxide release of rat intestinal mucous microvascular endothelial cells. Acta Anat Sin. 2007;27:832–4.
Duan H, et al. Effect of anemonin on NO, ET-1 and ICAM-1 production in rat intestinal microvascular endothelial cells. J Ethnopharmacol. 2006;104(3):362–6.
Muller AM, et al. Expression of the endothelial markers PECAM-1, vWf, and CD34 in vivo and in vitro. Exp Mol Pathol. 2002;72(3):221–9.
Tsoraeva A, Zhurbenko R. Development and characterization of a mixed nutrient base for the culture of a wide range of microorganisms. Rev Latinoam Microbiol. 2000;42:155.
Bayat B, Werth S, Sachs UJ, Newman DK, Newman PJ, Santoso S. Neutrophil transmigration mediated by the neutrophil-specific antigen CD177 is influenced by the endothelial S536 N dimorphism of platelet endothelial cell adhesion molecule-1. J Immunol. 2010;184:3889.
Hannig C, Spitzmuller B, Hannig M. Characterisation of lysozyme activity in the in situ pellicle using a fluorimetric assay. Clin Oral Investig. 2009;13:15.
O’Brien X, Elisseou N, Flores E, Patel D, Morrissette C, Loosley A, Reichner J. Mechanoregulation of human neutrophil host defense and survival. FASEB J. 2015;29:505–15.
Sarma JV, Ward PA. Neutrophils in endothelial damage. New York: Springer; 2014. pp. 777–84.
Wu X, Newbold MA, Haynes CL. Recapitulation of in vivo-like neutrophil transendothelial migration using a microfluidic platform. Analyst. 2015;140:5055.
Hostetter SJ. Neutrophil function in small animals. Vet Clin North Am Small Anim Pract. 2012;42:157.
Jerke U, Hernandez DP, Beaudette P, Korkmaz B, Dittmar G, Kettritz R. Neutrophil serine proteases exert proteolytic activity on endothelial cells. Kidney Int. 2015;88:764–75.
Hossain M, Qadri SM, Xu N, Su Y, Cayabyab FS, Heit B, Liu L. Endothelial LSP1 Modulates Extravascular Neutrophil Chemotaxis by Regulating Nonhematopoietic Vascular PECAM-1 Expression. J Immunol. 2015;195:2408–16.
Kang YH, Williams R. Endotoxin-induced endothelial injury and subendothelial accumulation of fibronectin in rat aorta. Anat Rec. 1991;229:86.
Pober JS, Min W. Endothelial cell dysfunction, injury and death. Handbook of Experimental Pharmacology. Berlin, Heidelberg: Springer-Verlag; 2006. pp. 135–56.
Fisher M. Injuries to the vascular endothelium: vascular wall and endothelial dysfunction. Rev Neurol Dis. 2008;5(Suppl 1):S4.
Medina E, Rohde M, Chhatwal GS. Intracellular survival of Streptococcus pyogenes in polymorphonuclear cells results in increased bacterial virulence. Infect Immun. 2003;71:5376.
Urban CF, Lourido S, Zychlinsky A. How do microbes evade neutrophil killing? Cell Microbiol. 2006;8:1687.
Butcher EC. Leukocyte-endothelial cell recognition: three (or more) steps to specificity and diversity. Cell. 1991;67:1033.
Jonas E, Dwenger A, Hager A. In vitro effect of ascorbic acid on neutrophil-endothelial cell interaction. J Biolumin Chemilumin. 1993;8:15.
Muller WA. Leukocyte-endothelial-cell interactions in leukocyte transmigration and the inflammatory response. Trends Immunol. 2003;24:327.
Schleimer RP, Rutledge BK. Cultured human vascular endothelial cells acquire adhesiveness for neutrophils after stimulation with interleukin 1, endotoxin, and tumor-promoting phorbol diesters. J Immunol. 1986;136:649.
Bunting M, Harris ES, McIntyre TM, Prescott SM, Zimmerman GA. Leukocyte adhesion deficiency syndromes: adhesion and tethering defects involving beta 2 integrins and selectin ligands. Curr Opin Hematol. 2002;9:30.
Skubitz KM, Skubitz AP. Two new synthetic peptides from the N-domain of CEACAM1 (CD66a) stimulate neutrophil adhesion to endothelial cells. Biopolymers. 2011;96:25.
Gunawan RC, Almeda D, Auguste DT. Complementary targeting of liposomes to IL-1alpha and TNF-alpha activated endothelial cells via the transient expression of VCAM1 and E-selectin. Biomaterials. 2011;32:9848.
Bruehl RE, Moore KL, Lorant DE, Borregaard N, Zimmerman GA, McEver RP, Bainton DF. Leukocyte activation induces surface redistribution of P-selectin glycoprotein ligand-1. J Leukoc Biol. 1997;61:489.
Buscher K, Riese SB, Shakibaei M, Reich C, Dernedde J, Tauber R, Ley K. The transmembrane domains of L-selectin and CD44 regulate receptor cell surface positioning and leukocyte adhesion under flow. J Biol Chem. 2010;285:13490.
Sopata I, Dancewicz AM. Presence of a gelatin-specific proteinase and its latent form in human leucocytes. Biochim Biophys Acta. 1974;370:510.
Borregaard N, Sorensen OE, Theilgaard-Monch K. Neutrophil granules: a library of innate immunity proteins. Trends Immunol. 2007;28:340.
Hager M, Cowland JB, Borregaard N. Neutrophil granules in health and disease. J Intern Med. 2010;268:25.
Faurschou M, Sorensen OE, Johnsen AH, Askaa J, Borregaard N. Defensin-rich granules of human neutrophils: characterization of secretory properties. Biochim Biophys Acta. 2002;1591:29.
Tumpey TM, Fenton R, Molesworth-Kenyon S, Oakes JE, Lausch RN. Role for macrophage inflammatory protein 2 (MIP-2), MIP-1alpha, and interleukin-1alpha in the delayed-type hypersensitivity response to viral antigen. J Virol. 2002;76:8050.
Borregaard N, Kjeldsen L, Rygaard K, Bastholm L, Nielsen MH, Sengelov H, Bjerrum OW, Johnsen AH. Stimulus-dependent secretion of plasma proteins from human neutrophils. J Clin Invest. 1992;90:86.
Borregaard N, Kjeldsen L, Lollike K, Sengelov H. Granules and vesicles of human neutrophils. The role of endomembranes as source of plasma membrane proteins. Eur J Haematol. 1993;51:318.
Acknowledgments
This work was supported by Chinese National Science Foundation Project (31272144 and 31572558), 2011 National “Twelfth Five-Year” Plan for Science & Technology Support (2011BAD34B03), the Beijing Nova Program (Z141105001814041), Beijing Municipal Science and Technology Project (Z121100007412004), the Beijing Nova Program (Z141105001814041), Beijing Municipal Natural Science Foundation (6132007).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Rights and permissions
About this article
Cite this article
Liu, X., Dong, H., Wang, M. et al. IL-1α-induced microvascular endothelial cells promote neutrophil killing by increasing MMP-9 concentration and lysozyme activity. Immunol Res 64, 133–142 (2016). https://doi.org/10.1007/s12026-015-8731-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-015-8731-4