Abstract
Serotonin-specific reuptake inhibitors (SSRIs) are generally considered safe drugs but fatal adverse effects do sometimes occur, often as a consequence of interactions with other serotonin active drugs. Polypharmacy is usually a problem that the elderly encounter, but it can also have dire consequences for young people, especially when an underlying heart condition is present. Thus, failure to diagnose heart disease and the use of contraindicated medications can be a lethal combination, irrespective of age. Here we present a case of a young adult suffering from bipolar disorder who used a combination of two SSRIs (citalopram and fluoxetine) and a monoamine oxidase inhibitor (MAO; moclobemide) with tragic consequences. The deceased also suffered from undiagnosed hypertrophic cardiomyopathy and was carrier of a genotype that may have predisposed him to increased sensitivity to SSRIs. The apparent difficulty in establishing the manner of death in this case is also discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Citalopram has long been considered one of the safest serotonin specific reuptake inhibitors (SSRIs) due to its selectivity and mild CYP450 inhibitory activity [1]. However, in 2011 the Food and Drug Administration (FDΑ) issued a warning concerning the risk of QT prolongation with citalopram use [2]. Both QT prolongation and its association with torsades de pointes (TdP) – a potentially fatal arrhythmia – appear to be dose-related [3], raising concerns regarding the exposure of patients to supratherapeutic levels of citalopram in cases of intentional or unintentional overdose. The latter is often the result of the use of contraindicated combinations of citalopram with other drugs, or of an underlying poor metabolizer status, or both [4, 5]. The ensuing overabundance of serotonin can also lead to excessive activation of serotoninergic pathways and precipitate a serious toxic syndrome known as serotonin syndrome [6]. Unfortunately, in spite of repeated warnings by health authorities and individual physicians [7, 8], patients faced with an apparently refractory condition may resort, by their own initiative, to polypharmacy, often with tragic consequences. The combination of SSRIs with monoamine oxidase inhibitors (MAOIs) is especially dangerous [9, 10]. Here we describe a case of deadly intoxication attributed to the use of contraindicated combinations of antidepressive drugs, of which citalopram reached potentially fatal levels. The possible contribution of an underlying heart condition and of the genetic background of the deceased to his death are also discussed.
Case history
A 25-year-old man was found dead at his home. The man was found in his bed, in the embryonic position, by a relative who lived in the same apartment complex as the deceased. According to his health card and information provided by his relatives, the man suffered from probable bipolar disorder, and had shown signs of depression since the age of 13. He was taking medication for his condition, including citalopram, fluoxetine, moclobemide, quetiapine, alprazolam, and valproic acid. Prescriptions of propranolol, perindopril, flurbiprofen, and desloratadine were also recorded on his health card. He was a smoker and was described as drinking alcohol and using hashish occasionally. His relatives also mentioned that he purchased non-prescribed medication through the internet. No suicide note was found, nor was there any knowledge of past attempts. A number of empty beer bottles were found at the scene, together with a mini-market receipt indicating that two bottles of beer had been purchased three and a half hours before the body was first discovered, providing an upper estimate of the time elapsed since his death.
External examination revealed the beginnings of both hypostasis and rigor mortis. No abrasions or ecchymoses were present. The face and neck were mildly congested and there was froth present around the buccal cavity. There was some dried blood on the lips. Old surgical scars on his left arm and right chest were attributed to past operations for a fractured arm, and a pneumothorax, respectively.
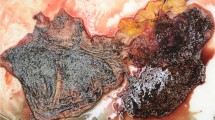
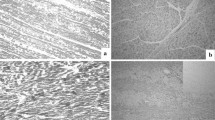
Internal examination showed froth and mucus in the trachea and major bronchi, edema and bronchiectasis in the lungs, medium to heavy arteriosclerotic lesions in the aorta and heavy arteriosclerotic lesions in the coronary arteries. Examination of the heart revealed signs of a recent infarct (ischemic areas with hemorrhagic infiltration) and hypertrophic cardiomyopathy (left ventricle wall thickness = 1.8 cm). His heart weighed 330 g. The stomach was full of barely digested food and produced an odor of ethanol upon dissection. Blood (femoral), and urine were collected for toxicological analysis, approximately 30 h after the estimated time of death.
The urine sample was positive for citalopram, quetiapine, and thetrahydrocannabinol (THC). A urine screen was performed using an enzyme multiplied immunoassay technique (EMIT) for controlled substances, and a GC/MS method for other drugs [11]. The blood sample was positive for citalopram, fluoxetine, moclobemide, quetiapine, THC, diclofenac and ethanol. Citalopram, fluoxetine, moclobemide, and ethanol were quantified (Table I); the rest were present in trace levels - higher than the limit of detection (LOD) but lower from the limit of quantitation (LOQ). Separation and quantification was achieved with an LC-MS/MS method [12]. Of the three quantified drugs none were in the reported fatal range, although their post-mortem concentrations were above usual therapeutic levels even considering an apparent increase due to post-mortem redistribution [13]; ethanol was below reported lethal levels (Table 1).
DNA isolated from the blood of the deceased was genotyped for the CYP2C19*2, and the CYP2D6*3,*4,*5,*10 loss-of-function/reduced function alleles and was found to be negative for all of them. The deceased was not a carrier of the CYP2D6xN polymorphism either. Genotyping for the SLC6A4 rs4795541 (HTTLPR) polymorphism [17] revealed that the deceased was of the SS genotype.
Discussion
According to Pilgrim et al. [4], fatalities involving the use of serotonin active drugs occur most frequently as a result of consuming contraindicated or inadvisable drug combinations, with heart disease the most common co-morbidity. The present case fits this pattern as the combinations of citalopram with moclobemid and of fluoxetine with moclobemid are contraindicated and have been implicated in fatal serotonin toxicity in the past [9, 10]. Indeed, whereas the aforementioned drugs have relatively low (moclobemide) or even very low (citalopram, fluoxetine) fatal toxicity indices [18], the combination of moclobemide, a reversible MAOI, with serotonin reuptake inhibitors (SRIs) is considered to increase significantly the probability of serotonin syndrome even at doses considered as therapeutic in the absence of DDIs [8]. The combination of the three drugs detected in this case is even more dangerous as it can cause extensive pharmacokinetic interactions: moclobemide is an inhibitor of CYP2C19 and of CYP2D6, whereas fluoxetine is an inhibitor mainly of CYP2D6; those two CYP enzymes are responsible for 85% of citalopram’s biotransformation [5], and their inhibition could increase this drug’s blood concentration to toxic levels. Citalopram and fluoxetine are both weak CYP2C19 inhibitors, but their combined action could conceivably increase moclobemide levels, as the latter is primarily biotransformed by that enzyme [5]. The alleged previous use of propranolol and perindopril by the deceased could also cause DDIs with citalopram, fluoxetine and moclobemide, as propranolol can act as a CYP2D6 and a CYP2C19 inhibitor, and perindopril as an ABCB1 inhibitor; although neither drug was detected in the toxicological analyses. On the other hand, as mentioned above, none of the three drugs had a post-mortem concentration clearly in the fatal range, even though citalopram has been found at a concentration as low as 0.6 μg/mL, and fluoxetine at 0.2 μg/ mL, in fatal poisonings together with other drugs or alcohol [19, 20]. Indeed, alcohol consumption may have increased the risk of a fatal outcome even though the post-mortem ethanol concentration was lower than the ones reported in fatal drug–alcohol poisonings [21]. Finally, the deceased being a homozygote for the SS genotype of the rs4795541 polymorphism, which is known to confer low expression of the serotonin reuptake protein (SERT) [22], may have contributed to the drug toxicity in this case as the limited presence of SERT on the presynaptic membrane can increase individual sensitivity to increased serotonin levels compared to carriers of the rs4795541 L allele. Indeed, the SS genotype has been consistently associated with greater adverse drug reaction burden during serotonin specific reuptake inhibitor (SSRI) therapy [23].
Even though drug toxicity on a background of heart disease is evident from the post mortem analysis in this case, it is practically impossible to diagnose serotonin syndrome based exclusively on post-mortem findings, as this condition has very precise diagnostic criteria (neurological, autonomic and mental symptoms) that need to be observed in the living [24]. Moreover, as the body was not found in a position indicating muscle hyperactivity prior to death, nor was any evidence of diaphoresis present, serotonin syndrome appears less likely. In our opinion, it is more likely that the combined use of alcohol together with citalopram, fluoxetine and moclobemide resulted in QT prolongation which, in combination with the poor condition of the victim’s heart (a recent infarct and heavy arteriosclerotic lesions, both uncharacteristic for the age of the deceased) precipitated a fatal arrhythmia. The manner of death cannot be unequivocally established either, as an intentional overdose cannot be excluded; a similar blood concentration of citalopram and a significant QTc prolongation were found in a (living) woman who had ingested 1400 mg of that drug with suicidal intention [25] and the HTTLPR SS genotype has been associated in the past with high scores of suicidality [26, 27], substance abuse [28], and antidepressant-induced mania (AIM) [23]. On the other hand, one cannot exclude a desperate attempt of the deceased to treat an apparently refractive condition; according to some studies carriers of the rs4795541 SS genotype do not respond as well to SSRIs as L allele carriers [29, 30]. Nevertheless, to the best of our knowledge, the influence of the rs4795541 polymorphism on serotonergic drug poisonings has not been tested or even alluded to. Whereas the effect of gene polymorphisms related to the pharmacokinetics of serotonergic drugs have been widely studied with respect to drug-drug interactions and adverse effects [5], polymorphisms in genes associated with the pharmacodynamics of these same drugs (e.g. SLC6A4 or SLC6A3) have received much less attention. We believe that they should be included in future studies.
Key points
-
1.
We report a case of fatal intoxication of a young adult following the simultaneous consumption of three different antidepressants, two SSRIs and an MOI.
-
2.
Other possible contributing factors include the consumption of alcohol, an apparently undiagnosed heart condition, and a possibly predisposing genotype (HTTLPR SS).
-
3.
The difficulties establishing a precise cause and manner of death are discussed.
-
4.
It is hoped that this case will raise awareness against using antidepressant medication in a manner which deviates from well-established therapeutic protocols based on accurate diagnoses.
References
Bezchlibnyk-Butler K, Aleksic I, Kennedy SH. Citalopram--a review of pharmacological and clinical effects. J Psychiatry Neurosci. 2000;25:241–54.
http://www.fda.gov/Drugs/DrugSafety/ucm297391.htm. Accessed 5 Jan 2018.
Friberg LE, Isbister GK, Hackett LP, Duffull SB. The population pharmacokinetics of citalopram after deliberate self-poisoning: a Bayesian approach. J Pharmacokinet Pharmacodyn. 2005;32:571–605.
Pilgrim JL, Gerostamoulos D, Drummer OH. Deaths involving contraindicated and inappropriate combinations of serotonergic drugs. Int J Legal Med. 2011;125:803–15.
Pilgrim JL, Gerostamoulos D, Drummer OH. Review: pharmacogenetic aspects of the effect of cytochrome P450 polymorphisms on serotonergic drug metabolism, response, interactions, and adverse effects. Forensic Sci Med Pathol. 2011;7:162–84.
Boyer EW, Shannon M. The serotonin syndrome. N Engl J Med. 2005;352:1112–20.
Bachmann CJ, Aagaard L, Burcu M, Glaeske G, Kalverdijk LJ, Petersen I, et al. Trends and patterns of antidepressant use in children and adolescents from five western countries, 2005-2012. Eur Neuropsychopharmacol. 2016;26:411–9.
Gillman K. Moclobemide and the risk of serotonin toxicity (or serotonin syndrome). CNS Drug Rev. 2004;10:83–5.
Dams R, Benijts TH, Lambert WE, Van Bocxlaer JF, Van Varenbergh D, Van Peteghem C, et al. A fatal case of serotonin syndrome after combined moclobemide-citalopram intoxication. J Anal Toxicol. 2001;25:147–51.
Wu ML, Deng JF. Fatal serotonin toxicity caused by moclobemide and fluoxetine overdose. Chang Gung Med J. 2011;34:644–9.
Mastrogianni O, Gbandi E, Orphanidis A, Raikos N, Goutziomitrou E, Kolibianakis EM, et al. Association of the CYP2B6 c.516G>T polymorphism with high blood propofol concentrations in women from northern Greece. Drug Metab Pharmacokinet. 2014;29:215–8.
Papazisis G, Goulas A, Sarrigiannidis A, Bargiota S, Antoniadis D, Raikos N, et al. ABCB1 and CYP2D6 polymorphisms and treatment response of psychotic patients in a naturalistic setting. Hum Psychopharmacol. 2018; https://doi.org/10.1002/hup.2644.
Launiainen T, Ojanperä I. Drug concentrations in post-mortem femoral blood compared with therapeutic concentrations in plasma. Drug Test Anal. 2014;6:308–16.
Winek CL, Wahba WW, Winek CL Jr, Balzer TW. Drug and chemical blood-level data 2001. Forensic Sci Int 2001;122:107–123.
Musshoff F, Padosch S, Steinborn S, Madea B. Fatal blood and tissue concentrations of more than 200 drugs. Forensic Sci Int. 2004;142:161–210.
Schulz M, Iwersen-Bergmann S, Andresen H, Schmoldt A. Therapeutic and toxic blood concentrations of nearly 1,000 drugs and other xenobiotics. Crit Care. 2012;16:R136.
Hooten WM, Hartman WR, Black JL 3rd, Laures HJ, Walker DL. Associations between serotonin transporter gene polymorphisms and heat pain perception in adults with chronic pain. BMC Med Genet 2013;14:78.
Ojanperä I, Kriikku P, Vuori E. Fatal toxicity index of medicinal drugs based on a comprehensive toxicology database. Int J Legal Med. 2016;130:1209–16.
Fu K, Konrad RJ, Hardy RW, Brissie RM, Robinson CA. An unusual multiple drug intoxication case involving citalopram. J Anal Toxicol. 2000;24:648–50.
Rohrig TP, Prouty RW. Fluoxetine overdose: a case report. J Anal Toxicol. 1989;13:305–7.
Koski A, Ojanperä I, Vuori E. Interaction of alcohol and drugs in fatal poisonings. Hum Exp Toxicol. 2003;22:281–7.
Collier DA, Stöber G, Li T, Heils A, Catalano M, Di Bella D, et al. A novel functional polymorphism within the promoter of the serotonin transporter gene: possible role in susceptibility to affective disorders. Mol Psychiatry. 1996;1:453–60.
Zhu J, Klein-Fedyshin M, Stevenson JM. Serotonin transporter gene polymorphisms and selective serotonin reuptake inhibitor tolerability: review of pharmacogenetic evidence. Pharmacotherapy. 2017;37:1089–104.
Talarico G, Tosto G, Pietracupa S, Piacentini E, Canevelli M, Lenzi GL, et al. Serotonin toxicity: a short review of the literature and two case reports involving citalopram. Neurol Sci. 2011;32:507–9.
Unterecker S, Warrings B, Deckert J, Pfuhlmann B. Correlation of QTc interval prolongation and serum level of citalopram after intoxication--a case report. Pharmacopsychiatry. 2012;45:30–4.
Kronenberg S, Apter A, Brent D, Schirman S, Melhem N, Pick N, et al. Serotonin transporter polymorphism (5-HTTLPR) and citalopram effectiveness and side effects in children with depression and/or anxiety disorders. J Child Adolesc Psychopharmacol. 2007;17:741–50.
Caspi A, Sugden K, Moffitt TE, Taylor A, Craig IW, Harrington H, et al. Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science. 2003;301:386–9.
Cao J, Hudziak JJ, Li D. Multi-cultural association of the serotonin transporter gene (SLC6A4) with substance use disorder. Neuropsychopharmacology. 2013;38:1737–47.
Andre K, Kampman O, Illi A, Viikki M, Setälä-Soikkeli E, Mononen N, et al. SERT and NET polymorphisms, temperament and antidepressant response. Nord J Psychiatry. 2015;69:531–8.
Landrø NI. Towards personalized treatment of depression: a candidate gene approach. Scand J Psychol. 2014;55:219–24.
Funding
Aristotle University Research Committee Grant no 88228 to Professor N. Raikos.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
Not applicable; only data collected in the process of a routine medico-legal investigation ordered by the legal authorities are presented in this case report.
Informed consent
As above.
Rights and permissions
About this article
Cite this article
Goulas, A., Raikos, N., Krokos, D. et al. Fatal intoxication with antidepressants: a case with many culprits. Forensic Sci Med Pathol 14, 225–228 (2018). https://doi.org/10.1007/s12024-018-9960-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-018-9960-3