Abstract
Metabolic dysfunction-associated steatotic liver disease (MASLD), previously known as nonalcoholic fatty liver disease (NAFLD), is the main cause of chronic liver disease in children and adolescents. Indeed, epidemiological studies have shown that MASLD affects up to 40% of children with obesity. Despite the recent approval of medications that target weight loss in adolescents that could have benefits on pediatric MASLD, lifestyle interventions, such as diet and exercise, remain the mainstay of our therapeutic approach. More specifically, studies on diet alone have focused on the possible role of carbohydrate or fat restriction, albeit without a definite answer on the best approach. Weight loss after dietary intervention in children with obesity and MASLD has a beneficial effect, regardless of the diet used. In relation to the role of exercise in MASLD reversal, indirect evidence comes from studies showing that a sedentary lifestyle leading to poor fitness, and low muscle mass is associated with MASLD. However, research on the direct effect of exercise on MASLD in children is scarce. A combination of diet and exercise seems to be beneficial with several studies showing improvement in surrogate markers of MASLD, such as serum alanine aminotransferase and hepatic fat fraction, the latter evaluated with imaging studies. Several dietary supplements, such as vitamin E, probiotics, and omega-3 fatty acid supplements have also been studied in children and adolescents with MASLD, but with equivocal results. This review aims to critically present available data on the effects of lifestyle interventions, including diet, exercise, and dietary supplements, on pediatric MASLD, thus suggesting a frame for future research that could enhance our knowledge on pediatric MASLD management and optimize clinicians’ approach to this vexing medical condition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Metabolic dysfunction-associated steatotic liver disease (MASLD), formerly known as nonalcoholic fatty liver disease (NAFLD) [1], is the most common cause of chronic liver disease in pediatric populations, more frequently diagnosed in male children with obesity [2]. MASLD encompasses conditions with varying severity, ranging from simple steatosis, which is increased hepatic fat accumulation without inflammation, to the so-called metabolic dysfunction-associated steatohepatitis (MASH), known as nonalcoholic steatohepatitis (NASH). MASH is characterized by increased liver fat accompanied by inflammation and hepatocellular injury, with or without liver fibrosis. MASH progression is not well characterized in children, but it may lead to extensive bridging fibrosis, cirrhosis, and finally, liver failure in early adulthood in a minority of cases [3].
MASLD usually coexists with metabolic syndrome components, such as central adiposity, dyslipidemia, hyperglycemia, and insulin resistance. In addition, several studies have shown that increased liver fat content is associated with an adverse cardiometabolic risk profile already in childhood, adolescence, and early adulthood [4,5,6]. During the last two decades, the exponential increase in the prevalence of pediatric obesity led to an increase in MASLD prevalence as well. Recent studies have shown that MASLD prevalence is between 5% and 10% in the general pediatric population [2], and almost 40% among children with obesity [7]. Even more alarming is the pace at which both the incidence and the prevalence of the disease have been increasing during the last decades [8, 9], rendering the management of children with MASLD a challenging issue. However, no approved pharmacological therapies exist. The most recent guidelines by both the European Society for Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) [10], and the North American Society of Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) [11], advocate the use of lifestyle interventions, including diet and exercise, as therapeutic measures for pediatric MASLD. Nevertheless, no detailed recommendations exist regarding either the ideal diet, or the type, intensity, and duration of exercise that should be followed by the patients, probably because relevant data are scarce. In addition, studies in adults with MASLD have shown that, among dietary supplements, vitamin E may lead to the improvement of liver function tests (LFTs), hepatic steatosis and inflammation [12,13,14,15]. Data on dietary supplements in children with MASLD are even more controversial [16,17,18,19].
The current review focused on clinical studies that have examined the efficacy of lifestyle interventions, namely diet and exercise, alone or in combination, in the management of MASLD in children and adolescents. Studies on dietary supplements in children with the disease were also included. It should be noted that although the terms MASLD and NAFLD are used interchangeably, the criteria for the two diagnoses are not entirely the same [1]. Some very recent studies showed a high concordance between the two diagnoses in adults (98%) [20], but lower in children (≥75%) [21]. Until more data are available regarding the concordance of the two terms, we maintained NAFLD nomenclature for earlier studies that used the prior NAFLD definition, throughout our manuscript.
Materials and methods
Although this is a narrative review, literature was searched according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [22]. A literature search was conducted on PubMed/Medline database for studies from peer-reviewed journals, published between January 1, 1980, and July 31, 2023, using the following key words: “NAFLD”, “non-alcoholic fatty liver disease”, “MASLD”, “metabolic dysfunction-associated steatotic liver disease”, “fatty liver”, “hepatic steatosis”, “nutrition”, “diet”, “exercise”, “physical activity”, “lifestyle interventions”, “dietary supplements”. Studies in English and in pediatric populations were included. Case reports, reviews, editorials, letters to the editor, case-control and cross-sectional studies were excluded from the review. Relevance was initially screened according to title and abstract. At the stage of eligibility, full-text articles of all relevant studies were reviewed. Papers that were identified from the reference lists of the retrieved articles, were also considered.
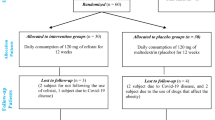
Initial literature search yielded 1304 records of which, 692 were excluded by title and 348 by abstract. In addition, 64 records were excluded because they were not written in English. From the reference list of the retrieved reports, 42 additional records were considered relevant. Among the 242 reports that were retrieved and reviewed in full-text, 199 were excluded for various reasons (Fig. 1). In the end, 43 articles were considered pertinent and were included in the current review.
Results
Dietary interventions
Five studies were found that evaluated the efficacy of diet intervention on NAFLD parameters in children and adolescents (Table 1). The earliest of these studies in 2009 by Vos et al. [23] was a randomized controlled trial (RCT) comprising 10 children with NAFLD. Seven of these children had a liver biopsy demonstrating NASH, while the other three were diagnosed by LFTs and ultrasonography. Six children were assigned to a low-fructose diet, while the other four to a low-fat diet, according to the American Heart Association recommendations [24]. A significant change in alanine aminotransferase (ALT) was not demonstrated in either group. No follow-up biopsy was performed in any of the participants. Low fructose diet was evaluated in another study by Jin et al. comprising 24 overweight Hispanic American adolescents with increased hepatic fat measured by magnetic resonance spectroscopy (MRS) at baseline [25]. These adolescents were randomized to calorie matched fructose-only or glucose-only beverages provided by the study. No other diet or physical activity modification was implemented. After four weeks, no measurable improvement in hepatic steatosis was identified, estimated by a follow-up MRS. However, several factors related to cardiovascular disease were improved, such as insulin sensitivity of adipose tissue, high sensitivity C-reactive protein (hs-CRP) and oxidized low-density lipoprotein cholesterol (LDL-C).
A more restrictive low glycemic diet compared to a low-fat diet was evaluated by Ramon-Krauel et al. [26] in 17 obese children with fatty liver, 8–17 years of age. After six months of follow-up, liver fat along with ALT levels decreased substantially in all participants, without any difference between the two groups. More recently, a study by Schwimmer et al. [27] comprised 40 adolescent boys aged 11 to 16 years with NAFLD, diagnosed by hepatic steatosis >10% and ALT level ≥45 µ/L. The authors used magnetic resonance imaging (MRI) proton density fat fraction (MRI-PDFF) to measure the effect of a diet low in free sugars versus a usual diet on hepatic fat content. The study showed that, after eight weeks, the participants in the low-free sugar diet had a greater reduction in hepatic steatosis compared to the control group. In 2020, the effects of a carbohydrate-restricted vs a fat-restricted diet were evaluated in a study by Goss et al. [28]. More specifically, thirty-two children or adolescents (aged 9–17) with obesity and NAFLD were randomized to a moderately carbohydrate-restricted or fat-restricted diet for 8 weeks. It was shown that hepatic lipid content, measured via MRI, decreased significantly only within the carbohydrate-restricted diet group. In addition, significantly greater decreases in abdominal and total fat mass, and insulin resistance, which are all closely associated with NAFLD, were found in response to the carbohydrate-restricted vs the fat-restricted diet group.
Physical activity interventions
Exercise is recommended as an important lifestyle modification measure in the management of obesity and NAFLD in children and adolescents. Some studies in adults have shown that exercise alone, even in the absence of dietary changes or weight loss, can decrease hepatic fat content and improve its function [29, 30]. Nevertheless, data on pediatric populations are limited and no studies have investigated the effect of exercise alone on children with biopsy-proven NAFLD (Table 1).
Lee et al. conducted two separate studies, one in boys [31] and another in girls [32], investigating the aerobic and resistance exercise effect on children with obesity and, possibly, NAFLD. In the first study [31], forty-five adolescent boys with obesity were randomly assigned to aerobic exercise, resistance exercise, or no exercise group and were followed for three months, without any caloric intake restriction. Intrahepatic lipid was assessed by MRS. A significant reduction in intrahepatic lipid was observed in both exercise groups, compared to controls. Furthermore, the authors observed that the resistance exercise but not the aerobic exercise group, had a significant improvement in insulin sensitivity. Similarly, in the second study [32], forty four adolescent girls with obesity were randomized into an aerobic or a resistance exercise group, and a third group of no exercise. Aerobic, but not resistance exercise, was effective in reducing liver fat in adolescent girls with obesity, independent of weight loss or calorie restriction. Though, a major limitation of both studies was that, at baseline, very few children had sufficient liver fat to be characterized as having NAFLD, since only 12 boys and five girls had hepatic fat fraction ≥5.0 %.
Another group of investigators, Van Der Heijden et al. also performed two separate studies on children, not based on sex of the participants, but on the type of exercise, namely aerobic [33] or resistance [34] exercise. In the first study evaluating aerobic exercise [33], fifteen children with obesity were compared to 14 children with normal weight. Both groups were provided a 30-minute aerobic exercise program twice a week for 12 weeks, which did not lead to weight loss. It was found that children in the obese group had a decrease in the hepatic fat accumulation from 9% to 6%, measured by MRS. However, no significant change in ALT was observed. In addition, no significant changes were observed in any parameter in lean participants. In the second study on resistance training, twelve Hispanic adolescents with obesity performed a 1-h session exercising all major muscle groups, twice a week, for 12 weeks. Despite improvement in several metabolic parameters, such as hepatic insulin sensitivity and glucose production rate, no changes were observed in hepatic fat content. The authors provided no data on ALT levels.
In a RCT by de Piano et al. [35] the effects of aerobic training with aerobic plus resistance training in adolescents with obesity and fatty liver diagnosed by ultrasound, were compared. After one year of follow-up, it was observed that the aerobic plus resistance training was more effective in improving ALT levels along with other noninvasive biomarkers of metabolic derangement, such as insulin, homeostasis model assessment-insulin resistance (HOMA-IR), adiponectin, and agouti-related peptide. Nonetheless, no follow-up ultrasound was performed.
A more recent nonrandomized study was conducted by Labayen et al. [36]. A total of 116 children with overweight or obesity (10.6 ± 1.1 years) and hepatic steatosis on MRI were recruited. For 22 weeks, participants followed a lifestyle and psycho-education program alone, or in combination with a supervised exercise intervention consisting of 90-min high-intensity aerobic workouts, three times a week. At the end of the intervention, the hepatic fat was re-evaluated by MRI and was found to be reduced only in the exercise group, regardless of baseline value and any change in total body adiposity.
Dietary plus physical activity interventions
Most of the studies carried out to evaluate lifestyle changes in children and adolescents with NAFLD included both diet and physical activity programs (Table 1). As early as in 1994, Vajro et al. [37] first observed that, in children with obesity, persistent ALT increase, and a “bright” liver on ultrasound, a combined program of nutrition and exercise leading to weight loss could be beneficial. Another early study by Tazawa et al. [38] comprised 73 children aged 6–14 years with obesity and elevated ALT. The authors did not apply a strict dietary program, but they adjusted participants’ diet according to each one’s food preferences and advised that they reduce their daily caloric intake by 20%. In addition, increased physical activity was recommended but without a detailed structured exercise program, for three months. The authors observed weight loss in 36/73 children and ALT normalization in 20/73. This ALT reduction was observed mostly in children with weight reduction (17/20), but, unexpectedly, also in some participants with weight gain (3/20).
Ten years later, in 2006, Nobili et al. [39] published the only study so far comprising children with biopsy-proven NAFLD. In this uncontrolled study, 84 children with overweight/obesity, elevated aminotransferases and NAFLD were enrolled. Increased liver fibrosis was identified in 49 (58.3%) patients at baseline, with obesity and age being independent risk factors of fibrosis. All children followed a 12-month program of lifestyle intervention consisting of one-hour nutritional counseling sessions, the prescription of a balanced diet adjusted to individual preferences, and an exercise program. More specifically, a low calorie diet (25–30 Kcal/kg/d) comprised by 50–60% carbohydrate, 25–30% fat, and 15–20% protein was prescribed. In addition, all participants followed a three-time per week aerobic exercise program with 30–45 min-sessions. Children that completed the 12-month program (57/84) showed a significant decrease in body weight (from mean 60.9 to mean 56 kg), along with a significant ALT reduction (from mean 62 to mean 33 IU/L). Among these 57 patients, 52 had body mass index (BMI) ≥ 85th percentile for age and sex at baseline, of whom, most had an improved ultrasound at the end of the study. More specifically, liver echogenicity on ultrasound completely resolved in 5/52 patients, improved in 41/52 patients, and showed no change in 6/52 patients. Nonetheless, post treatment liver biopsy was not performed in any of the participants.
Three more recent trials comprised patients that were diagnosed with NAFLD by liver MRI or MRS. The first by Pozzato et al. [40] comprised 25 children with obesity, nine of whom (36%) were diagnosed with hepatic steatosis by MRI. Mean ALT levels at baseline were 31 IU/L, which were not very increased, albeit above the upper limit of normal. The latter is 22 IU/L for adolescent girls, and 26 IU/L for adolescent boys according to the National Health and Nutrition Examination Survey for adolescents [41] and more recent studies [42]. Participants followed a 1-year nutrition-behavior intervention based on balanced diet and physical exercise. After the intervention, prevalence of hepatic steatosis dropped down to 7.7% from 34.6% at baseline, while no significant decrease in ALT levels was observed. Regarding body weight, at the end of the study participants had a mean decrease in BMI z-score of 0.26 (0.11–0.41). Importantly, this change was accompanied by a decrease in central adiposity with a waist circumference reduction of 1.46 (0.34–2.60) cm. The other study by Koot et al. [43] evaluated children with NAFLD by MRS. In this study, 55 children (8–18 years) with severe obesity and hepatic steatosis were non-randomly assigned to three intervention groups, namely the inpatient treatment group, the ambulatory treatment group, and the usual care group. After six months, 43, 29 and 22% of children, respectively, had no signs of hepatic steatosis. The respective percentages for serum ALT normalization were 41, 33 and 6%. At the end of the six-month period, the BMI z-score change was greater in the inpatient group (−0.37 [−0.5 to − 0.2]) compared both to the ambulatory (− 0.16 [−0.3 to − 0.04]) and the control group (0.06 [−0.01 to 0.13]). Treatment effects were sustained at 1.5 years follow-up in the first two groups. The authors concluded that the intensity of the intervention (inpatient vs ambulatory) does not significantly increase the treatment success rate. The third study, by Chan et al. [44] also used MRS to identify children with intrahepatic triglyceride content ≥5%. Fifty-two children were randomly assigned to either a dietitian-led lifestyle modification program group or a conventional pediatrician-led consultation group. After 52 weeks of follow-up, a reduction of the intra-hepatic triglyceride content to 2–3% was observed in both groups. Regarding body weight, both groups showed a reduction in BMI z-score at 16 weeks of intervention, but this reduction persisted only for the pediatrician-led group at the end of the study. The authors observed that the more the parents and pediatricians were involved, the longer the results of the intervention were sustained.
Many of the studies involving both diet and exercise interventions comprised children that were diagnosed with NAFLD based on high ALT levels and/or abnormal ultrasound findings. Wang et al. [45] performed an RCT with 76 children/adolescents with obesity, high ALT levels and steatosis on ultrasound that were randomized to a control group without any intervention (Group 1), to a group of children with hypocaloric diet and aerobic exercise (Group 2), or to a group receiving vitamin E supplement of 100 IU/day (Group 3). After one month, aspartate aminotransferase (AST), ALT, HOMA-IR and BMI improved in Groups 2 and 3, but not in Group 1. Between Groups 2 and 3, a greater reduction was observed in the camp group compared to the vitamin E group. Another study by Grønbæk et al. [46] comprised 117 children with obesity, 43% of whom had liver steatosis on ultrasound, and 58% increased LFTs. A 10-week weight loss camp program was implemented, and data were collected from the children at the end of the 10-week period, and 12 months later. A 10% weight loss was observed overall, with hepatic steatosis dropping to 30% along with a decrease in ALT levels in all children. In an uncontrolled study by Campos et al. [47] 18 post-pubertal adolescents with obesity and NAFLD on ultrasound, followed nutritional counseling once a week and 1 h of combined aerobic and resistance training, three times a week. After one year, the mean weight loss observed was 11 ± 7.2 kg. Mean ALT levels decreased from 37.2 ± 22.1 at baseline to 27.5 ± 15.0 IU/L at the end of the study (p = 0.05). In addition, the prevalence of NAFLD diagnosed by ultrasound, dropped from 100% to 33%. Devore et al. [48] recruited 83 children with chronic ALT elevation, who were followed up for one year in a gastroenterology clinic with 30-min consultation on nutrition and exercise every three months. Only 39/83 patients (47%) completed the program, showing statistically significant decrease in mean BMI z-score, as well as in both ALT and AST. These results, however, should be interpreted with caution, because of the low percentage of completion rate.
One of the largest studies to date was conducted in a tertiary center for children with severe obesity [49]. Lefere et al. recruited 204 patients (median age, 14 years) with severe obesity (mean BMI z-score, +2.8). NAFLD was diagnosed by ultrasonography in 71.1% of these patients, while 32.8% had presumable fibrosis stage (F) ≥2 in transient elastography. All participants were enrolled in an intensive lifestyle therapy with caloric restriction, physical activity program, education regarding healthy lifestyle, and psychosocial support. After six months, liver fibrosis improved in 75% of patients with baseline fibrosis. After one year, these changes persisted, and in 35 patients, fibrosis resolved completely. Serum ALT levels decreased significantly but changes in ALT were not greater in those with fibrosis regression. More specifically, ALT change in those with resolution of fibrosis was −13 IU/L (+1 to −28) vs −28 IU/L (−7 to −72) in those without resolution of fibrosis (p = 0.100). One of the major drawbacks of the study is the low percentage of completion rate, thus its results should also be cautiously interpreted.
Two other studies with combined diet and exercise interventions in children and adolescents, focused mainly on changes in vascular structure and function. However, since they present hepatic outcomes as well, they were also included in this review. The first, by Pacifico et al. [50] enrolled 135 children with obesity and NAFLD based on ultrasound. In addition, 52 children underwent hepatic MRI for steatosis estimation. Fifteen subjects were lost to follow-up. The other 120 followed a 1-year intervention program with a hypocaloric diet and a 60-min physical exercise, five days a week. At the end of the study period, a significant decrease in the BMI-standard deviation score (SDS) was observed (mean −0.34, −0.30 to −0.40), along with a decrease in mean ALT levels from 54 to 37 IU/L, and a significant decrease in hepatic fat content measured by hepatic MRI. The second study by Sanches et al. [51] comprised 131 adolescents with obesity, out of whom, 33 were diagnosed with NAFLD determined by ultrasound. All subjects followed a one-year interdisciplinary therapy of diet, exercise, and psychological support. At the end of the study, a decrease in BMI was observed, from 39.5 to 34.6 kg/m2, together with a decrease in the mean ALT levels from 27 to 21 IU/L. However, no follow-up ultrasound was performed.
Dietary supplements: antioxidants
Vitamin E has been known to have antioxidant, anti-inflammatory, and anti-apoptotic properties. Therefore, it has been studied as a supplement in adult patients with NAFLD and NASH and has been shown to be effective in some studies [15, 52,53,54,55], while others showed no improvement, especially regarding the level of fibrosis [14, 56, 57]. However, it should be highlighted that the duration of all relevant studies was possibly short to show improvement in a hard endpoint like hepatic fibrosis [58]. On the other hand, concerns have been raised due to possible adverse effects of the long-term administration of high-dose vitamin E in adults [59]. Therefore, current adult guidelines recommend that vitamin E supplementation may be used in selected patients with NASH and F ≥ 2 for up to 2 years [60].
In pediatric populations with NAFLD, several studies have been conducted to identify the possible effect of vitamin E supplementation (Table 2). A study by Wang et al. [45] compared three groups of children with obesity and NAFLD, aged 10–17, for one month. Group 1 was the control group, group 2 comprised children in a summer camp that followed a strict lifestyle intervention and children in group 3 received oral vitamin E at a dose of 100 mg/d. The study showed that vitamin E supplementation decreased ALT in Group 2 and 3 compared to the control group; however, the reduction in ALT was greater in the children of the lifestyle intervention group than vitamin E group (88.58 ± 39.99 vs 63.69 ± 27.05, p = 0.040, respectively). In a large study by Nobili et al. [61] with a longer follow-up period of 24 months, the addition of alpha-tocopherol (a vitamin E form) 600 IU/day plus ascorbic acid (vitamin C) 500 mg/day to lifestyle intervention was investigated in children with biopsy-proven NAFLD. Importantly, the effects of the intervention were evaluated by liver biopsy, looking for the grade of steatosis, hepatocyte ballooning, and lobular inflammation in liver histology at 24 months. Secondary end points included changes in LFTs, body weight, and indices of insulin sensitivity on an oral glucose tolerance test. The study showed that the efficacy of the combination of vitamin E and vitamin C was similar to the efficacy of lifestyle intervention alone, since primary and secondary end points were similar for both groups at the end of the intervention period. A noteworthy finding was that ALT normalized in more children in the placebo compared to the antioxidant group (22/28 vs 13/25, respectively, p < 0.05). Another study showed that vitamin E led to significant reduction in ALT (>50 percent from baseline or even normalization) in 38% of children with NASH in a "real world" setting [62]. Furthermore, the combined administration of vitamin E and the antioxidant hydroxytyrosol improved steatosis grade in 40 adolescents with NAFLD compared to the placebo group [63]. In another RCT (TONIC trial) [64], vitamin E supplementation was compared to metformin. More specifically, 173 children and adolescents (aged 8–17 years) with biopsy-confirmed NAFLD, were randomized to daily dosing of 800 IU of vitamin E, 1000 mg of metformin, or placebo for 96 weeks. The study showed that neither vitamin E, nor metformin were superior to placebo regarding the primary outcome, which was a reduction by ≥50% of the baseline ALT level or an ALT level ≤40 IU/L, at every 12-week visit from 48 to 96 weeks of treatment. More specifically, only 15/58 (26%) of the vitamin E group, and 9/57 (16%) of the metformin group met the primary outcome at 96 weeks, compared to 10/58 (17%) of the placebo group (p = 0.26 and p = 0.83, respectively). Similarly, no statistical significance was identified among the three groups regarding hepatocellular ballooning, NAFLD activity score, and other histological features on follow-up liver biopsy. What is interesting though, is the fact that, among children with NASH, NASH resolved at 96 weeks in more children in the vitamin E group (58%) compared to the placebo (28%; p = 0.006) or to the metformin group (41%). Akcam et al. [65] also compared a 6-month metformin or vitamin E supplement in addition to exercise, and nutritional counseling in adolescents with obesity and NAFLD. Metformin treatment was superior to vitamin E in improving metabolic syndrome components. However, no change was observed in ALT levels in any group. Of note, no follow-up ultrasound was performed in this study. Another small study by Vajro et al. [13] allocated 28 children with obesity, NAFLD and high LFTs either to placebo, or to vitamin E supplementation. The interesting finding was that vitamin E supplementation was effective in ALT normalization in those children with minimal adherence to dietary and physical activity recommendations. Indeed, there was a poor compliance to lifestyle interventions (13/28 participants, 46%), compared to the 100% compliance to vitamin E supplementation. The authors suggested that vitamin E could be considered as an effective approach in such patients. Even earlier was a study by Lavine et al. [66] who showed that 4 to 10 months of daily oral vitamin E administration to 11 children with obesity and NASH led to normalization of their AST and ALΤ levels.
Another antioxidant with anti-inflammatory properties that has been investigated in children with NAFLD is ginger. Indeed, Kamari et al. [67] examined the effect of adding ginger to an anti-inflammatory diet low in processed food in 160 children (8–11 years of age) with obesity and NAFLD. They found that both BMI and ALT levels improved in the ginger and ginger-with-anti-inflammatory-diet groups compared to controls (for BMI p = 0.04 in both cases, and for ALT p = 0.004 and <0.001, respectively). Similarly, a significant reduction in liver fat accumulation was identified for both intervention groups. This reduction was greater in the ginger-with-anti-inflammatory-diet group (one-degree reduction of steatosis in 82.5% of participants, and two-degree reduction of steatosis in 17.5%).
Among the nutraceutical compounds, curcumin, the most frequently used polyphenol with anti-inflammatory and antifibrotic properties, has been shown to be of value in the context of NAFLD, both in basic and clinical studies [68, 69]. All relevant clinical studies, though, comprised adult patients. There is only one randomized placebo-controlled clinical study with children by Ismail et al [70], which showed that the daily administration of 500 mg curcumin to obese children for 4 weeks, lead to a decrease in their insulin resistance.
Dietary supplements: probiotics
There is evidence suggesting that gut microbiota may play crucial role in NAFLD development. Indeed, since the liver receives almost 70% of its blood supply from the intestines via the portal circulation, bacteria products, such as lipopolysaccharides and endotoxins can increase hepatic inflammation and oxidative stress [71].
It is, therefore, rational that studies with probiotics and gut microbiota modifiers have been conducted both in adult and pediatric populations with NAFLD (Table 2) [72, 73]. Vajro et al. [74] demonstrated that children with obesity, persisting hypertransaminasemia and ultrasonographic NAFLD that were treated for 8 weeks with the probiotic Lactobacillus rhamnosus strain GG had lower ALT levels compared to placebo treated children. Alisi et al. [75] showed that children with biopsy-proven NAFLD that were supplemented with a mixture of eight strains of bacteria had improved liver ultrasound findings after 8 weeks. In another study by Famouri et al. [76] children with obesity and NAFLD that were treated with a daily mixture of four probiotics (Lactobacillus acidophilus, Lactobacillus rhamnosus, Bifidobacterium lactis, and Bifidobacterium bifidum), were more likely to decrease ALT levels and normalize ultrasound findings compared to the placebo group. Unfortunately, the small number of the relevant RCTs [74, 75], their small sample sizes, the differences in the probiotic strains used, the short follow-up and the lack of paired liver biopsies render the results insecure. Especially regarding follow-up, it is known that discontinuation of probiotic supplementation is usually followed by a rapid rebound to baseline microbiota composition, rendering studies with longer follow-up necessary [77].
Dietary supplements: polyunsaturated fatty acids
NASH severity and modified gene expression have been shown to be associated with decreased polyunsaturated fatty acids (PUFAs) hepatocyte content [78]. In addition, epidemiological studies show an inverse relationship between PUFAs intake and the risk of NAFLD and NASH development [79]. Therefore, dietary ω3 PUFA supplements, such as docosahexaenoic (DHA) and eicosapentaenoic acid (EPA), have been investigated for the management of NAFLD in adults. Some clinical trials and meta-analyses support a possible beneficial role of PUFA supplementation in improving LFTs [56, 79,80,81]. However, other studies did not provide favorable results of PUFAs on hepatic histology of patients with NAFLD [82]. Thus, PUFAs do not seem to be beneficial in adult patients with NAFLD [83].
Regarding studies in pediatric populations, seven trials have been conducted so far (Table 2). Nobili et al. [84] compared the effect of DHA supplementation on liver fat content, in children with biopsy-proven NAFLD. More specifically, 250 or 500 mg DHA were administered to 60 children with NAFLD for 6–24 months and were compared to the placebo group. Children in both DHA groups demonstrated a decrease in liver fat content as detected by ultrasonography after 6 months of treatment. ALT did not significantly change after treatment. In a 24-month extension of this study [85], the difference between DHA and placebo groups persisted. In addition, ALT levels were lower in the DHA 250 mg than placebo group, after the 12th month onwards. However, no follow-up biopsy was performed. Three subsequent RCTs were published on the topic, albeit with conflicting results. More specifically, Janczyk et al. [86] examined 76 children with overweight/obesity and NAFLD that were randomized to receive either omega-3 fatty acids (DHA and EPA, 450−1300 mg/day) or placebo (omega-6 sunflower oil). After six months, no difference was found in ALT levels or the liver steatosis on ultrasound between the two groups. However, AST and gamma-glutamyl transferase (GGT) levels were lower in the intervention compared to the placebo group. Boyraz et al. [87] examined 108 children with obesity and NAFLD, randomized into two groups, one receiving 1000 mg EPA/DHA supplementation daily and the other placebo. Both groups underwent a lifestyle intervention. At the end of the 12-month observation period, both groups showed improvement, but the EPA/DHA group had significantly greater rate of ALT decrease compared to the placebo group (39.2% to 14.2% vs 38.4% to 28.8%, respectively, p = 0.01). In addition, the rates of children with steatosis decreased more significantly in the EPA/DHA group (56 patients before to 18 patients after intervention) compared to the control group (52 to 31, respectively). In another study, by Pacifico et al. [88] it was shown that hepatic fat measured by MRI decreased after 6 months of DHA supplementation to children with obesity and biopsy-proven NAFLD compared to the placebo group, despite similar reduction in ALT. Zöhrer et al. [89] also compared placebo vs a mixture of PUFAs with additional antioxidant molecules (namely, DHA with choline and vitamin E) along with lifestyle modification in an RCT with 43 children with biopsy-proven NASH. A significant decrease in severe steatosis in the treatment group (50% to 5%, p = 0.001) was observed on ultrasound. Importantly, a follow-up biopsy only in the intervention group showed significant improvement in steatosis, ballooning, and NASH. Finally, Spahis et al. [90] demonstrated that 6 months of 2 g daily n-3 PUFA supplementation in 20 male children/adolescents with NAFLD resulted in decreased Fatty Liver Index, a non-invasive index of steatosis, ALT levels and ALT/AST ratio, indicating beneficial effect on liver steatosis.
Based on the existing studies, definite conclusion on the effect of PUFAs administration in children and adolescents with NAFLD cannot be drawn. Longer-term studies with paired liver biopsies and hard endpoints, i.e., resolution of NASH and/or improvement of hepatic fibrosis are necessary to clarify any effect of PUFA in children/adolescent NAFLD.
Discussion
The current critical review included all trials that have evaluated the efficacy of lifestyle interventions in children and/or adolescents with MASLD. Such interventions include dietary changes, programs of resistance and/or aerobic exercise, or a combination of both. In addition, studies on dietary supplements, such as vitamin E, probiotics, and PUFAs, were also included. Overall, studies on diet alone have shown some improvement in pediatric MASLD, especially when it is accompanied by weight loss. However, no definite conclusion as to which is the best dietary approach, can be drawn. Data on exercise alone are scarce but suggest some improvement in liver steatosis in children affected by obesity. Most studies have examined the combination of diet and exercise, suggesting a beneficial effect on laboratory or imaging surrogate markers of childhood MASLD. Studies on dietary supplements have shown contradictory results, which are further characterized by high heterogeneity in their endpoints and lack of paired liver biopsies in most of them.
Regarding studies on dietary modifications alone for the management of pediatric MASLD, five trials have been included in this review. All focused on carbohydrate or fat intake reduction, either compared to each other, or compared to a usual diet. Regarding carbohydrate reduction, a special focus on fructose can be observed. Indeed, excessive dietary fructose consumption has been linked to a higher risk of MASLD and hepatic fibrosis development, possibly through increased de novo lipogenesis [91, 92]. Two studies examined whether a low fructose diet can improve MASLD in children, with conflicting results [23, 25]. Other monosaccharides or disaccharides can be involved in MASLD pathogenesis, and a low-free sugar diet was shown to considerably improve hepatic steatosis compared to usual diet [27]. However, no definitive conclusion can be drawn if a carbohydrate- or a fat-restricted diet is more beneficial for children with MASLD, since the results are conflicting [26, 28]. It seems that the main drive of improvement of MASLD is weight loss, while the diet macronutrients and micronutrients seem to be of secondary importance, if any [93]. Indeed, even if MASLD can sometimes be diagnosed in lean subjects [94], obesity is a major risk factor identified in studies in children [95, 96]. Therefore, weight loss, together with the improvement in several of the metabolic syndrome parameters [97], could be, at least in part, responsible for the amelioration of MASLD in obese children after various dietary interventions. Future studies comprising normal weight children with MASLD who do not require weight loss could be of help to determine the best type of diet, although, in lean MASLD the underlying pathophysiology and risk factors may be different (e.g., the genetic factors are more prominent) [98, 99].
Regarding physical activity, indirect evidence on MASLD improvement comes from population studies linking decreased physical activity, sedentary behavior, and inadequate cardiorespiratory fitness with a higher risk of MASLD in children [100, 101]. Physical activity guidelines for the general pediatric population may differ somehow from country to country, but they generally advocate for a daily average of ≥60 min of moderate or vigorous intensity combination of aerobic and resistance exercise, every day of the week [102]. Relevant recommendations have been published by NASPGHAN also for children with MASLD [11]. However, no robust data exist on the possible beneficial effects of exercise on hepatic function in such children. Relevant studies conducted so far and included in this review comprise mostly children with obesity that followed a structured aerobic and/or resistance exercise program and managed to lose weight [31,32,33,34,35]. However, some, but not all, of these children had MASLD at baseline and no trial has been conducted comprising children with biopsy-proven MASLD, more specifically with paired liver biopsy. A more recent trial by Labayen et al. [36] focused specifically on the effects of exercise when added to a family-based lifestyle intervention program in children with obesity and hepatic steatosis. This is the first study showing that exercise, as an adjunct to a multicomponent intervention program, can improve MASLD and hepatic function. More such studies, especially RCTs, are needed to establish the importance of exercise in children with MASLD.
Many of the studies included in this review examined the combined effects of diet and exercise. More specifically, a total of 13 studies were identified, comprising 959 children and adolescents, most of whom were diagnosed with MASLD at baseline [37,38,39,40, 43,44,45,46,47,48,49,50,51]. The diagnosis was mainly based on elevated ALT levels and/or abnormal ultrasonographic findings. Duration of intervention varied between one month and one year and the completion rate was between 38.7% and 100%. The efficacy of interventions was estimated based on ALT level reduction, intrahepatic fat change estimated by ultrasound, MRI, or MRS, or fibrosis determined by transient or magnetic resonance elastography. Follow-up liver biopsy was performed in only one of the studies [39]. Most studies showed an improvement in these parameters, suggesting a beneficial effect of a structured, combined intervention program that leads to weight loss. However, no definite conclusions can be drawn regarding the ideal dietary type, as commented above for the studies with diet alone, or the exact type and duration of exercise. What seems unequivocal though, is the beneficial effect of weight loss on pediatric MASLD. Indeed, in all studies included in this review, weight loss was accompanied by improvement in LFTs and/or by decreased hepatic fat content. Lifestyle interventions have been shown to have good effectiveness in weight loss in children, but they are difficult to implement for long-term [103,104,105].
Apart from diet and exercise interventions, dietary supplements have gained attention lately as a lifestyle approach for children with MASLD. Vitamin E, having antioxidant, anti-apoptotic, and anti-inflammatory properties, has been evaluated as a supplement in adult patients with MASLD and MASH, with certain benefits [15]. In children with MASLD, eight studies have been conducted to date with vitamin E [13, 45, 61,62,63,64,65,66]. The number of children included in these studies is considerable (551 in total), but these studies are characterized by heterogeneity, a general lack of paired liver biopsies, and by the fact that vitamin E doses are usually much lower than those proposed for adults with MASLD, so definite conclusion on the effect of vitamin E on pediatric MASLD cannot be drawn. Indeed, vitamin E supplementation was shown to improve only some histological findings in a minority of children. In addition, concerns have been raised by findings of increased hemorrhagic stroke and prostate cancer risk in adults receiving vitamin E in high doses [106, 107], although extrapolation of these findings in children is not easy.
To date, three studies have examined the possible effect of probiotics supplementation to children with MASLD [74,75,76]. Their results may warrant further studies on probiotics in MASLD, but to date definite conclusion cannot be made. Definite limitation of these studies are their small sample sizes, the differences in the probiotic strains used, and, above all, the short-term follow-up, Finally, seven studies examined the effects of PUFAs to children with MASLD [84,85,86,87,88,89,90]. Some, but not all, of these studies showed an improvement in LFTs, e.g., normalization of ALT levels and/or improved ultrasonographic or MRI findings. However, these results should not be overestimated, until larger studies with paired liver biopsies clarify the effect of PUFAs on MASLD histology, if any.
Limitations of the study
Despite being a comprehensive critical review of the current literature, this study has some limitations, mainly related to the heterogeneity of the data included. More specifically, an inherent difficulty of studies on pediatric MASLD is the way the disease is defined in order, not only, to select the correct population for any given intervention, but also, to reliably evaluate the outcome. Indeed, liver biopsy is the current gold standard for MASLD diagnosis and for severity assessment, namely the presence of hepatic steatosis, inflammation, and, most importantly, fibrosis, which is the main histological predictor of morbidity and mortality [108]. However, because of its invasiveness, biopsy was performed only in a few studies, while several others were based on various laboratory or imaging surrogate markers of the disease, either for the recruitment procedure or for the follow-up [109]. ALT measurement was frequently applied because it is inexpensive and easily available, but it has low sensitivity and specificity in both adults [110] and children [11]. According to the most recent NASPGHAN Clinical Practice Guideline for the Diagnosis and Treatment of Nonalcoholic Fatty Liver Disease in Children [11], ALT increased to more than twice the upper limit, after the exclusion of other causes of fatty liver, in overweight or obese children older than 10 years indicates NAFLD with 88% sensitivity, but only 26% specificity. This means that studies based solely on ALT levels as inclusion criteria were subjected to misclassification bias [111]. Similarly, ALT change as an endpoint evaluating the efficacy of intervention, may not necessarily reflect histological improvement. Newer biomarkers, such as increased fibroblast growth factor 21 [112], and newer techniques, such as high-resolution metabolomics [113], seem to be promising alternatives. However, no studies included in this review used such surrogate markers in pediatric populations with MASLD. Regarding imaging modalities, abdominal ultrasound was extensively used. Having a low cost, good safety profile, and high accessibility, ultrasound remains the imaging technique of choice for fatty liver screening, with a sensitivity and specificity of 84.8% (95% confidence interval; 79.5–88.9), and 93.6% (87.2–97.0), respectively [114, 115]. However, sensitivity and specificity of the ultrasound are lower in obese individuals, i.e., the majority of MASLD patients [116]. MRI, MRS and MRI-PDFF are more accurate methods to evaluate liver fat, but they are more expensive and less accessible than ultrasound [116] and were therefore rarely applied in the studies included. Imaging methods used to evaluate liver fibrosis include transient elastography, share wave elastography, and magnetic resonance elastography, all of which were also rarely used [117]. Further to the above difficulties, the relatively low completion rate observed in several of the included studies (Tables 1 and 2), further decrease the reliability of the studies’ results and make their comparison even more difficult.
Conclusions
In conclusion, lifestyle modifications, including diet and exercise are considered to be beneficial for children and adolescents with MASLD, and therefore are included in the relevant guidelines [10, 11]. Even if the scientific evidence for these recommendations is not robust, the increasing prevalence of obesity and NAFLD and the associated cardiometabolic risk, in conjunction with the absence of a definite treatment, make these lifestyle measures essential in the management of this vexing pediatric health problem. Certainly, well-organized RCTs that will include children with biopsy-proven MASLD, and paired liver biopsies will contribute to clarify and quantify diet and exercise effects on pediatric MASLD. Regarding the various dietary supplements such as vitamin E, probiotics and PUFAs, existing data do not favor their use in children with MASLD. However, larger, and better methodological studies may shed light on the efficacy of some of them in the future, especially vitamin E.
References
M.E. Rinella, J.V. Lazarus, V. Ratziu, S.M. Francque, A.J. Sanyal, F. Kanwal et al. A multi-society Delphi consensus statement on new fatty liver disease nomenclature. J. Hepatol. 0, 45 (2023)
E.L. Anderson, L.D. Howe, H.E. Jones, J.P.T. Higgins, D.A. Lawlor, A. Fraser, The prevalence of non-alcoholic fatty liver disease in children and adolescents: a systematic review and meta-analysis. PLoS One 10, e0140908 (2015)
A.E. Feldstein, P. Charatcharoenwitthaya, S. Treeprasertsuk, J.T. Benson, F.B. Enders, P. Angulo, The natural history of non-alcoholic fatty liver disease in children: a follow-up study for up to 20 years. Gut. 58, 1538–1544 (2009)
J.B. Schwimmer, P.E. Pardee, J.E. Lavine, A.K. Blumkin, S. Cook, Cardiovascular risk factors and the metabolic syndrome in pediatric nonalcoholic fatty liver disease. Circulation. 118, 277–283 (2008)
M.L. Geurtsen, S. Santos, J.F. Felix, L. Duijts, M.W. Vernooij, R. Gaillard et al. Liver fat and cardiometabolic risk factors among school‐age children. Hepatology. 72, 119–129 (2020)
Y.L. Liao, G.Y. Zhu, C. Chang, Non-alcoholic fatty liver disease increases the risk of cardiovascular disease in young adults and children: a systematic review and meta-analysis of cohort studies. Front. Cardiovasc. Med. 10, 1291438 (2024)
E.L. Yu, J.B. Schwimmer, Epidemiology of pediatric nonalcoholic fatty liver disease. Clin. Liver Dis. 17, 196 (2021)
A.K. Sahota, W.L. Shapiro, K.P. Newton, S.T. Kim, J. Chung, J.B. Schwimmer, Incidence of nonalcoholic fatty liver disease in children: 2009-2018. Pediatrics. 146, e20200771 (2020)
X. Zhang, M. Wu, Z. Liu, H. Yuan, X. Wu, T. Shi et al. Increasing prevalence of NAFLD/NASH among children, adolescents and young adults from 1990 to 2017: a population-based observational study. BMJ Open 11, e042843 (2021)
P. Vajro, S. Lenta, P. Socha, A. Dhawan, P. McKiernan, U. Baumann et al. Diagnosis of nonalcoholic fatty liver disease in children and adolescents: position paper of the ESPGHAN Hepatology Committee. J. Pediatr. Gastroenterol. Nutr. 54, 700–713 (2012)
M.B. Vos, S.H. Abrams, S.E. Barlow, S. Caprio, S.R. Daniels, R. Kohli et al. NASPGHAN clinical practice guideline for the diagnosis and treatment of nonalcoholic fatty liver disease in children: recommendations from the Expert Committee on NAFLD (ECON) and the North American Society of Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN). J. Pediatr. Gastroenterol. Nutr. 64, 319–334 (2017)
B.J. Perumpail, A.A. Li, N. John, S. Sallam, N.D. Shah, W. Kwong et al. The role of vitamin E in the treatment of NAFLD. Diseases 6, 86–96 (2018)
P. Vajro, C. Mandato, A. Franzese, E. Ciccimarra, S. Lucariello, M. Savoia et al. Vitamin E treatment in pediatric obesity-related liver disease: a randomized study. J. Pediatr. Gastroenterol. Nutr. 38, 48–55 (2004)
H. El Hadi, R. Vettor, M. Rossato, Vitamin E as a treatment for nonalcoholic fatty liver disease: reality or myth? Antioxidants. 7(1), 12 (2018)
K. Sato, M. Gosho, T. Yamamoto, Y. Kobayashi, N. Ishii, T. Ohashi et al. Vitamin E has a beneficial effect on nonalcoholic fatty liver disease: a meta-analysis of randomized controlled trials. Nutrition. 31, 923–930 (2015)
M. Rahimlou, H. Ahmadnia, A. Hekmatdoost, Dietary supplements and pediatric non-alcoholic fatty liver disease: Present and the future. World J. Hepatol. 7, 2597 (2015)
Y. Park, S.A. Smith-Warner, X. Zhang, Y.J. Park, H. Kim, H. Park et al. Association between use of vitamin and mineral supplement and non-alcoholic fatty liver disease in hypertensive adults. Sci. Rep. 13, 1–13 (2023)
L.L. Wang, P.H. Zhang, H.H. Yan, Functional foods and dietary supplements in the management of non-alcoholic fatty liver disease: a systematic review and meta-analysis. Front. Nutr. 10, 1014010 (2023)
A.F.G. Cicero, A. Colletti, S. Bellentani, Nutraceutical approach to Non-Alcoholic Fatty Liver Disease (NAFLD): the available clinical evidence. Nutrients. 10, 1153 (2018)
M.E. Rinella, B.A. Neuschwander-Tetri, M.S. Siddiqui, M.F. Abdelmalek, S. Caldwell, D. Barb et al. AASLD practice guidance on the clinical assessment and management of nonalcoholic fatty liver disease. Hepatology. 77, 1797–1835 (2023)
Y. Xing, J. Fan, H.J. Wang, H. Wang, Comparison of MAFLD and NAFLD Characteristics in Children. Children. 10, 560 (2023)
M.J. Page, J.E. McKenzie, P.M. Bossuyt, I. Boutron, T.C. Hoffmann, C.D. Mulrow et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372, 71 (2021)
M.B. Vos, M.B. Weber, J. Welsh, F. Khatoon, D.P. Jones, P.F. Whitington et al. Fructose and oxidized low-density lipoprotein in pediatric nonalcoholic fatty liver disease: a pilot study. Arch. Pediatr. Adolesc. Med. 163, 674–675 (2009)
S.S. Gidding, B.A. Dennison, L.L. Birch, S.R. Daniels, M.W. Gilman, A.H. Lichtenstein et al. Dietary recommendations for children and adolescents: a guide for practitioners: consensus statement from the American Heart Association. Circulation. 112, 2061–2075 (2005)
R. Jin, J.A. Welsh, N.A. Le, J. Holzberg, P. Sharma, D.R. Martin et al. Dietary fructose reduction improves markers of cardiovascular disease risk in hispanic-American Adolescents with NAFLD. Nutrients. 6, 3187 (2014)
M. Ramon-Krauel, S.L. Salsberg, C.B. Ebbeling, S.D. Voss, R.V. Mulkern, M.M. Apura, et al. A low-glycemic-load versus low-fat diet in the treatment of fatty liver in obese children.Childhood Obes. 9, 252 (2013).
J.B. Schwimmer, P. Ugalde-Nicalo, J.A. Welsh, J.E. Angeles, M. Cordero, K.E. Harlow et al. Effect of a low free sugar diet vs usual diet on nonalcoholic fatty liver disease in adolescent boys: a randomized clinical trial. JAMA. 321, 256–265 (2019)
A.M. Goss, S. Dowla, M. Pendergrass, A. Ashraf, M. Bolding, S. Morrison et al. Effects of a carbohydrate-restricted diet on hepatic lipid content in adolescents with non-alcoholic fatty liver disease: a pilot, randomized trial. Pediatr. Obes. 15(7), e12630 (2020)
K. Hallsworth, G. Fattakhova, K.G. Hollingsworth, C. Thoma, S. Moore, R. Taylor et al. Resistance exercise reduces liver fat and its mediators in non-alcoholic fatty liver disease independent of weight loss. Gut. 60, 1278–1283 (2011)
E. Bacchi, C. Negri, G. Targher, N. Faccioli, M. Lanza, G. Zoppini et al. Both resistance training and aerobic training reduce hepatic fat content in type 2 diabetic subjects with nonalcoholic fatty liver disease (the RAED2 Randomized Trial). Hepatology. 58, 1287–1295 (2013)
S.J. Lee, F. Bacha, T. Hannon, J.L. Kuk, C. Boesch, S. Arslanian, Effects of aerobic versus resistance exercise without caloric restriction on abdominal fat, intrahepatic lipid, and insulin sensitivity in obese adolescent boys: a randomized, controlled trial. Diabetes. 61, 2787 (2012)
S.J. Lee, A.R. Deldin, D. White, Y.M. Kim, I. Libman, M. Rivera-Vega et al. Aerobic exercise but not resistance exercise reduces intrahepatic lipid content and visceral fat and improves insulin sensitivity in obese adolescent girls: a randomized controlled trial. Am. J. Physiol. Endocrinol. Metab. 305(10), E1222–E1229 (2013)
G.J. Van Der Heijden, Z.J. Wang, Z.D. Chu, P.J.J. Sauer, M.W. Haymond, L.M. Rodriguez et al. A 12-week aerobic exercise program reduces hepatic fat accumulation and insulin resistance in obese, Hispanic adolescents. Obesity 18, 384–390 (2010)
G.J. Van Der Heijden, Z.J. Wang, Z. Chu, G. Toffolo, E. Manesso, P.J.J. Sauer et al. Strength exercise improves muscle mass and hepatic insulin sensitivity in obese youth. Med. Sci. Sports Exercise 42, 1973–1980 (2010)
A. De Piano, M.T. De Mello, P.D.L. Sanches, P.L. Da Silva, R.M.S. Campos, J. Carnier et al. Long-term effects of aerobic plus resistance training on the adipokines and neuropeptides in nonalcoholic fatty liver disease obese adolescents. Eur. J. Gastroenterol. Hepatol. 24, 1313–1324 (2012)
I. Labayen, M. Medrano, L. Arenaza, E. Máz, M. Osés, V. Martínez-Vizcáno et al. Effects of exercise in addition to a family-based lifestyle intervention program on hepatic fat in children with overweight. Diabetes Care 43, 306–313 (2020)
P. Vajro, A. Fontanella, C. Perna, G. Orso, M. Tedesco, A. De Vincenzo, Persistent hyperaminotransferasemia resolving after weight reduction in obese children. J. Pediatr. 125, 239–241 (1994)
Y. Tazawa, H. Noguchi, F. Nishinomiya, G. Takada, Effect of weight changes on serum transaminase activities in obese children. Acta Paediatr. Jpn 39, 210–214 (1997)
V. Nobili, M. Marcellini, R. Devito, P. Ciampalini, F. Piemonte, D. Comparcola et al. NAFLD in children: a prospective clinical-pathological study and effect of lifestyle advice. Hepatology. 44, 458–465 (2006)
C. Pozzato, E. Verduci, S. Scaglioni, G. Radaelli, M. Salvioni, A. Rovere et al. Liver fat change in obese children after a 1-year nutrition-behavior intervention. J. Pediatr. Gastroenterol. Nutr. 51, 331–335 (2010)
J.B. Schwimmer, W. Dunn, G.J. Norman, P.E. Pardee, M.S. Middleton, N. Kerkar et al. SAFETY study: alanine aminotransferase cutoff values are set too high for reliable detection of pediatric chronic liver disease. Gastroenterology. 138(4), 1357–1364 (2010)
S. Bussler, M. Vogel, D. Pietzner, K. Harms, T. Buzek, M. Penke et al. New pediatric percentiles of liver enzyme serum levels (alanine aminotransferase, aspartate aminotransferase, γ-glutamyltransferase): Effects of age, sex, body mass index, and pubertal stage. Hepatology. 68, 1319–1330 (2018)
B.G.P. Koot, O.H. Van Der Baan-Slootweg, S. Vinke, A.E. Bohte, C.L.J. Tamminga-Smeulders, P.L.M. Jansen et al. Intensive lifestyle treatment for non-alcoholic fatty liver disease in children with severe obesity: inpatient versus ambulatory treatment. Int. J. Obes. 40, 51–57 (2016)
D.F.Y. Chan, H.K. So, S.C.N. Hui, R.S.M. Chan, A.M. Li, M.M. Sea et al. Dietitian-led lifestyle modification programme for obese Chinese adolescents with non-alcoholic fatty liver disease: a randomized controlled study. Int. J. Obes. 42, 1680–1690 (2018)
C.L. Wang, L. Liang, J.F. Fu, C.C. Zou, F. Hong, J.Z. Xue et al. Effect of lifestyle intervention on non-alcoholic fatty liver disease in Chinese obese children. World J. Gastroenterol. 14, 1598 (2008)
H. Grønbæk, A. Lange, N.H. Birkebæk, P. Holland-Fischer, J. Solvig, A. Hørlyck et al. Effect of a 10-week weight loss camp on fatty liver disease and insulin sensitivity in obese Danish children. J. Pediatr. Gastroenterol. Nutr. 54, 223–228 (2012)
R.M.S. Campos, A. De Piano, P.L. Da Silva, J. Carnier, P.L. Sanches, F.C. Corgosinho et al. The role of pro/anti-inflammatory adipokines on bone metabolism in NAFLD obese adolescents: effects of long-term interdisciplinary therapy. Endocrine. 42, 146–156 (2012)
S. Devore, R. Kohli, K. Lake, L. Nicholas, K. Dietrich, W.F. Balistreri et al. A multidisciplinary clinical program is effective in stabilizing BMI and reducing transaminase levels in pediatric patients with NAFLD. J. Pediatr. Gastroenterol. Nutr. 57, 119–123 (2013)
S. Lefere, E. Dupont, A. De Guchtenaere, S. Van Biervliet, S. Vande Velde, X. Verhelst et al. Intensive lifestyle management improves steatosis and fibrosis in pediatric nonalcoholic fatty liver disease. Clin. Gastroenterol. Hepatol. 20, 2317–2326.e4 (2022)
L. Pacifico, M. Arca, C. Anania, V. Cantisani, M. Di Martino, C. Chiesa, Arterial function and structure after a 1-year lifestyle intervention in children with nonalcoholic fatty liver disease. Nutr. Metab. Cardiovasc. Dis. 23, 1010–1016 (2013)
P.L. Sanches, A. De Piano, R.M.S. Campos, J. Carnier, M.T. De Mello, N. Elias et al. Association of nonalcoholic fatty liver disease with cardiovascular risk factors in obese adolescents: the role of interdisciplinary therapy. J. Clin. Lipidol. 8, 265–272 (2014)
M.A. Pervez, D.A. Khan, A.U.R. Slehria, A. Ijaz, Delta-tocotrienol supplementation improves biochemical markers of hepatocellular injury and steatosis in patients with nonalcoholic fatty liver disease: a randomized, placebo-controlled trial. Complement. Ther. Med. 52, 102494 (2020)
E. Magosso, M.A. Ansari, Y. Gopalan, I.L. Shuaib, J.W. Wong, N.A.K. Khan et al. Tocotrienols for normalisation of hepatic echogenic response in nonalcoholic fatty liver: A randomised placebo-controlled clinical trial. Nutr. J. 12, 1–8 (2013)
M.Y. Wang, K. Prabahar, M.A. Găman, J.L. Zhang, Vitamin E supplementation in the treatment on nonalcoholic fatty liver disease (NAFLD): Evidence from an umbrella review of meta-analysis on randomized controlled trials. J. Dig. Dis. 24, 380–389 (2023)
A. Vadarlis, C. Antza, D.R. Bakaloudi, I. Doundoulakis, G. Kalopitas, M. Samara et al. Systematic review with meta-analysis: the effect of vitamin E supplementation in adult patients with non-alcoholic fatty liver disease. J. Gastroenterol. Hepatol. 36, 311–319 (2021)
J. Karedath, H. Javed, F.A. Talpur, B. Lal, A. Kumari, H. Kivan et al. Effect of Vitamin E on clinical outcomes in patients with non-alcoholic fatty liver disease: a meta-analysis. Cureus. 14(12), e32764 (2022)
F. Bril, D.M. Biernacki, S. Kalavalapalli, R. Lomonaco, S.K. Subbarayan, J. Lai et al. Role of Vitamin E for nonalcoholic steatohepatitis in patients with type 2 diabetes: a randomized controlled trial. Diabetes Care 42, 1481–1488 (2019)
G. Mintziori, S.A. Polyzos, Emerging and future therapies for nonalcoholic steatohepatitis in adults. Expert Opin. Pharmacother. 17, 1937–1946 (2016)
E.R. Miller, R. Pastor-Barriuso, D. Dalal, R.A. Riemersma, L.J. Appel, E. Guallar, Meta-analysis: high-dosage vitamin E supplementation may increase all-cause mortality. Ann. Intern. Med. 142(1), 37–46 (2005)
G. Marchesini, C.P. Day, J.F. Dufour, A. Canbay, V. Nobili, V. Ratziu et al. EASL-EASD-EASO clinical practice Guidelines for the management of non-alcoholic fatty liver disease. J. Hepatol. 64, 1388–1402 (2016)
V. Nobili, M. Manco, R. Devito, V. Di Ciommo, D. Comparcola, M.R. Sartorelli et al. Lifestyle intervention and antioxidant therapy in children with nonalcoholic fatty liver disease: a randomized, controlled trial. Hepatology. 48, 119–128 (2008)
T. Yodoshi, S. Orkin, A.C. Arce-Clachar, K. Bramlage, W. Su, L. Fei et al. Identifying predictors of response to Vitamin E for the treatment of pediatric nonalcoholic steatohepatitis. J. Parenter. Enteral. Nutr. 44, 1301–1307 (2020)
V. Nobili, A. Alisi, A. Mosca, A. Crudele, S. Zaffina, M. Denaro et al. The antioxidant effects of hydroxytyrosol and Vitamin E on pediatric nonalcoholic fatty liver disease, in a clinical trial: a new treatment? Antioxid. Redox. Signal. 31, 127–133 (2019)
J.E. Lavine, J.B. Schwimmer, M.L. Van Natta, J.P. Molleston, K.F. Murray, P. Rosenthal et al. Effect of Vitamin E or metformin for treatment of nonalcoholic fatty liver disease in children and adolescents: the TONIC randomized controlled trial. JAMA. 305, 1659–1668 (2011)
M. Akcam, A. Boyaci, O. Pirgon, S. Kaya, S. Uysal, B.N. Dundar, Therapeutic effect of metformin and vitamin E versus prescriptive diet in obese adolescents with fatty liver. Int. J. Vitam. Nutr. Res. 81, 398–406 (2011)
J.E. Lavine, Vitamin E treatment of nonalcoholic steatohepatitis in children: a pilot study. J. Pediatr. 136, 734–738 (2000)
N. Kamari, M. Moradinazar, M. Qasemi, T. Khosravy, M. Samadi, H. Abdolahzad, Combination of the effect of ginger and anti‐inflammatory diet on children with obesity with nonalcoholic fatty liver disease: a randomized clinical trial. Food Sci. Nutr. 11, 1846 (2023)
N.A. Zabihi, M. Pirro, T.P. Johnston, A. Sahebkar, Is there a role for curcumin supplementation in the treatment of non-alcoholic fatty liver disease? The data suggest yes. Curr. Pharm. Des. 23, 969–982 (2017)
M. Guariglia, F. Saba, C. Rosso, E. Bugianesi, Molecular mechanisms of curcumin in the pathogenesis of metabolic dysfunction associated steatotic liver disease. Nutrients. 15, 5053–5060 (2023)
N.M.I. Nagwa, R. Samer, A.A. El Baky, W.K. Hashem, I. Alshaymaa, Effect of oral curcumin administration on insulin resistance, serum resistin and fetuin-A in obese children: Randomized placebo-controlled study. Res. J. Pharm. Biol. Chem. Sci. 5, 887–896 (2014)
J. Aron-Wisnewsky, M.V. Warmbrunn, M. Nieuwdorp, K. Clément, Nonalcoholic fatty liver disease: modulating gut microbiota to improve severity? Gastroenterology. 158, 1881–1898 (2020)
V. Nobili, S. Cucchiara, The use of probiotics in pediatric nonalcoholic fatty liver disease: teachable moment or missed opportunity? J. Pediatr. Gastroenterol. Nutr. 64, 336–337 (2017)
L. Liu, P. Li, Y. Liu, Y. Zhang, Efficacy of probiotics and synbiotics in patients with nonalcoholic fatty liver disease: a meta-analysis. Dig. Dis. Sci. 64, 3402–3412 (2019)
P. Vajro, C. Mandato, M.R. Licenziati, A. Franzese, D.F. Vitale, S. Lenta et al. Effects of Lactobacillus rhamnosus strain GG in pediatric obesity-related liver disease. J. Pediatr. Gastroenterol. Nutr. 52, 740–743 (2011)
A. Alisi, G. Bedogni, G. Baviera, V. Giorgio, E. Porro, C. Paris et al. Randomised clinical trial: the beneficial effects of VSL#3 in obese children with non-alcoholic steatohepatitis. Aliment Pharmacol. Ther. 39, 1276–1285 (2014)
F. Famouri, Z. Shariat, M. Hashemipour, M. Keikha, R. Kelishadi, Effects of probiotics on nonalcoholic fatty liver disease in obese children and adolescents. J. Pediatr. Gastroenterol. Nutr. 64, 413–417 (2017)
C.A. Lozupone, J.I. Stombaugh, J.I. Gordon, J.K. Jansson, R.Knight, Diversity, stability and resilience of the human gut microbiota. Nature. 489, 220 (2012).
B.M. Arendt, E.M. Comelli, D.W.L. Ma, W. Lou, A. Teterina, T. Kim et al. Altered hepatic gene expression in nonalcoholic fatty liver disease is associated with lower hepatic n-3 and n-6 polyunsaturated fatty acids. Hepatology. 61, 1565–1578 (2015)
X.T. Lu, Y.D. Wang, T.T. Zhu, H.L. Zhu, Z.Y. Liu, Dietary fatty acids and risk of non-alcoholic steatohepatitis: a national study in the United States. Front. Nutr. 9, 952451 (2022)
D.B. Jump, K.A. Lytle, C.M. Depner, S. Tripathy, Omega-3 polyunsaturated fatty acids as a treatment strategy for nonalcoholic fatty liver disease. Pharmacol. Ther. 181, 108–125 (2018)
K. Musa-Veloso, C. Venditti, H.Y. Lee, M. Darch, S. Floyd, S. West et al. Systematic review and meta-analysis of controlled intervention studies on the effectiveness of long-chain omega-3 fatty acids in patients with nonalcoholic fatty liver disease. Nutr. Rev. 76, 581–602 (2018)
A.J. Sanyal, M.F. Abdelmalek, A. Suzuki, O.W. Cummings, M. Chojkier, No significant effects of ethyl-eicosapentanoic acid on histologic features of nonalcoholic steatohepatitis in a phase 2 trial. Gastroenterology. 147(2), 377–84.e1 (2014)
S.A. Polyzos, E.S. Kang, C. Boutari, E.J. Rhee, C.S. Mantzoros, Current and emerging pharmacological options for the treatment of nonalcoholic steatohepatitis. Metabolism. 111S, 154203 (2020)
V. Nobili, G. Bedogni, A. Alisi, A. Pietrobattista, P. Risé, C. Galli et al. Docosahexaenoic acid supplementation decreases liver fat content in children with non-alcoholic fatty liver disease: double-blind randomised controlled clinical trial. Arch. Dis. Child 96, 350–353 (2011)
V. Nobili, A. Alisi, C. Della Corte, P. Risé, C. Galli, C. Agostoni et al. Docosahexaenoic acid for the treatment of fatty liver: randomised controlled trial in children. Nutr. Metab. Cardiovasc. Dis. 3, 1066–1070 (2013)
W. Janczyk, D. Lebensztejn, A. Wierzbicka-Rucińska, A. Mazur, J. Neuhoff-Murawska, P. Matusik et al. Omega-3 Fatty acids therapy in children with nonalcoholic Fatty liver disease: a randomized controlled trial. J. Pediatr. 166, 1358–1363.e3 (2015)
M. Boyraz, Ö. Pirgon, B. Dündar, F. Çekmez, N. Hatipoğlu, Long-term treatment with n-3 polyunsaturated fatty acids as a monotherapy in children with nonalcoholic fatty liver disease. J. Clin. Res. Pediatr. Endocrinol. 7, 121–127 (2015)
L. Pacifico, E. Bonci, M. Di Martino, P. Versacci, G. Andreoli, L.M. Silvestri et al. A double-blind, placebo-controlled randomized trial to evaluate the efficacy of docosahexaenoic acid supplementation on hepatic fat and associated cardiovascular risk factors in overweight children with nonalcoholic fatty liver disease. Nutr. Metab. Cardiovasc. Dis. 25, 734–741 (2015)
E. Zöhrer, A. Alisi, J. Jahnel, A. Mosca, C. Della Corte, A. Crudele et al. Efficacy of docosahexaenoic acid-choline-vitamin E in paediatric NASH: a randomized controlled clinical trial. Appl. Physiol. Nutr. Metab. 42, 948–954 (2017)
S. Spahis, F. Alvarez, N. Ahmed, J. Dubois, R. Jalbout, M. Paganelli et al. Non-alcoholic fatty liver disease severity and metabolic complications in obese children: impact of omega-3 fatty acids. J. Nutr. Biochem. 58, 28–36 (2018)
M.F. Abdelmalek, A. Suzuki, C. Guy, A. Unalp-Arida, R. Colvin, R.J. Johnson et al. Increased fructose consumption is associated with fibrosis severity in patients with nonalcoholic fatty liver disease. Hepatology. 51, 1961–1971 (2010)
X. Ouyang, P. Cirillo, Y. Sautin, S. McCall, J.L. Bruchette, A.M. Diehl et al. Fructose consumption as a risk factor for non-alcoholic fatty liver disease. J. Hepatol. 48, 993–999 (2008)
S.A. Polyzos, J. Kountouras, C.S. Mantzoros, Obesity and nonalcoholic fatty liver disease: from pathophysiology to therapeutics. Metabolism. 92, 82–97 (2019)
A.Y. Wang, J. Dhaliwal, M. Mouzaki, Lean non-alcoholic fatty liver disease. Clin. Nutr. 38, 975–981 (2019)
Q. Pang, J.Y. Zhang, S.D. Song, K. Qu, X.S. Xu, S.S. Liu et al. Central obesity and nonalcoholic fatty liver disease risk after adjusting for body mass index. World J. Gastroenterol. 21, 1650 (2015)
V. Cuzmar, G. Alberti, R. Uauy, A. Pereira, C. García, F. De Barbieri et al. Early obesity: risk factor for fatty liver disease. J. Pediatr. Gastroenterol. Nutr. 70, 93–98 (2020)
A. Serbis, V. Giapros, A. Galli-Tsinopoulou, E. Siomou, Metabolic syndrome in children and adolescents: is there a universally accepted definition? Does it Matter? Metab. Syndr. Relat. Disord. 18, 462–470 (2020)
J.K. DiStefano, G.S. Gerhard, NAFLD in normal weight individuals. Diabetol. Metab. Syndr. 14, 45 (2022)
E.J. Kim, H.J. Kim, Nonalcoholic fatty liver disease in obese and nonobese pediatric patients. Korean J. Pediatr. 62, 30 (2019)
J.L. Trilk, A. Ortaglia, S.N. Blair, M. Bottai, T.S. Church, R.R. Pate, Cardiorespiratory fitness, waist circumference, and alanine aminotransferase in youth. Med. Sci. Sports Exercise 45, 722–727 (2013)
L. Gerber, M. Otgonsuren, A. Mishra, C. Escheik, A. Birerdinc, M. Stepanova et al. Non-alcoholic fatty liver disease (NAFLD) is associated with low level of physical activity: a population-based study. Aliment Pharmacol. Ther. 36, 772–781 (2012)
A.M. Parrish, M.S. Tremblay, S. Carson, S.L.C. Veldman, D. Cliff, S. Vella et al. Comparing and assessing physical activity guidelines for children and adolescents: a systematic literature review and analysis. Int. J. Behav. Nutr. Phys. Activity 17, 1–22 (2020)
B. Li, S. Gao, W. Bao, M. Li, Effectiveness of lifestyle interventions for treatment of overweight/obesity among children in China: a systematic review and meta-analysis. Front. Endocrinol. 13, 972954 (2020)
S.L. Samuels, P. Hu, K.R. Maciejewski, F. Li, J. Dziura, M. Savoye et al. Real-world effectiveness of the Bright Bodies healthy lifestyle intervention for childhood obesity. Obesity. 31, 203–213 (2023)
A. Ek, M. Brissman, K. Nordin, K. Eli, P. Nowicka, A long-term follow-up of treatment for young children with obesity: a randomized controlled trial. Int. J. Obes. 47, 1152–1160 (2023)
L. E, B. J, Y. S, S. P, P. J, A. JM, et al. Effects of long-term vitamin E supplementation on cardiovascular events and cancer: a randomized controlled trial. JAMA. 293, 1338–1347 (2005)
E.L. Abner, F.A. Schmitt, M.S. Mendiondo, J.L. Marcum, R.J. Kryscio, Vitamin E and all-cause mortality: a meta-analysis. Curr. Aging Sci. 4, 158 (2011)
E. Makri, A. Goulas, S.A. Polyzos, Epidemiology, pathogenesis, diagnosis and emerging treatment of nonalcoholic fatty liver disease. Arch. Med. Res. 52, 25–37 (2021)
M. Mouzaki, S.C. Ling, R.A. Schreiber, B.M. Kamath, Management of pediatric nonalcoholic fatty liver disease by academic hepatologists in canada: a nationwide survey. J. Pediatr. Gastroenterol. Nutr. 65, 380–383 (2017)
S. Verma, D. Jensen, J. Hart, S.R. Mohanty, Predictive value of ALT levels for non-alcoholic steatohepatitis (NASH) and advanced fibrosis in non-alcoholic fatty liver disease (NAFLD). Liver Int. 33, 1398–1405 (2013)
J.B. Schwimmer, K.P. Newton, H.I. Awai, L.J. Choi, M.A. Garcia, L.L. Ellis et al. Paediatric gastroenterology evaluation of overweight and obese children referred from primary care for suspected non-alcoholic fatty liver disease. Aliment Pharmacol. Ther. 38, 1267–1277 (2013)
L. He, L. Deng, Q. Zhang, J. Guo, J. Zhou, W. Song et al. Diagnostic value of CK-18, FGF-21, and related biomarker panel in nonalcoholic fatty liver disease: a systematic review and meta-analysis. Biomed. Res. Int. 2017, 9729107 (2017)
R.D. Khusial, C.E. Cioffi, S.A. Caltharp, A.M. Krasinskas, A. Alazraki, J. Knight-Scott et al. Development of a plasma screening panel for pediatric nonalcoholic fatty liver disease using metabolomics. Hepatol. Commun. 3, 1311 (2019)
R. Hernaez, M. Lazo, S. Bonekamp, I. Kamel, F.L. Brancati, E. Guallar et al. Diagnostic accuracy and reliability of ultrasonography for the detection of fatty liver: a meta-analysis. Hepatology. 54, 1082 (2011)
C.M. Lee, E.L. Yoon, A. Nakajima, M. Yoneda, H. Toyoda, S. Yasuda et al. A reappraisal of the diagnostic performance of B-Mode ultrasonography for mild liver steatosis. Am. J. Gastroenterol. 118, 840–847 (2023)
S.A. Polyzos, C.S. Mantzoros, Necessity for timely noninvasive diagnosis of nonalcoholic fatty liver disease. Metabolism. 63, 161–167 (2014)
Q. Yu, Y. Liu, P. Hu, F. Gao, G. Huang, Performance of imaging techniques in non-invasive diagnosis of non-alcoholic fatty liver disease in children: a systematic review and meta-analysis. Front. Pediatr. 10, 837116 (2022)
Funding
Open access funding provided by HEAL-Link Greece.
Author information
Authors and Affiliations
Contributions
Conceptualization, A.S. and D.N.K.; Methodology, A.S., S.A.Po., S.A.Pa., D.N.K.; Validation, S.A.Po., S.A.Pa., E.S., D.N.K.; Investigation, A.S., S.A.Po., S.A.Pa., E.S., D.N.K.; Data Curation, A.S., S.A.Po., D.N.K.; Writing – Original Draft Preparation, A.S., S.A.Po., D.N.K.; Writing – Review & Editing, S.A.Po., S.A.Pa., E.S., D.N.K.; Visualization, A.S.; Supervision, S.A.Po., E.S., D.N.K.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Serbis, A., Polyzos, S.A., Paschou, S.A. et al. Diet, exercise, and supplements: what is their role in the management of the metabolic dysfunction-associated steatotic liver disease in children?. Endocrine 85, 988–1006 (2024). https://doi.org/10.1007/s12020-024-03783-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-024-03783-7