Abstract
Purpose
To evaluate how self-care maintenance, self-care monitoring, and self-care management affect glycated haemoglobin in type 2 diabetes mellitus patients and to set cut-off points of the Self-Care of Diabetes Inventory scales using glycated haemoglobin as outcome of interest.
Methods
A secondary analysis of a previous multicentre observational cross-sectional study was conducted. Overall, 540 adults with type 2 diabetes mellitus confirmed diagnosis were involved. Socio-demographic and clinical data were collected. Self-care maintenance, self-care monitoring, and self-care management were measured by the Self-Care of Diabetes Inventory. Linear regression models were performed to assess the relationship between self-care maintenance, self-care monitoring, and self-care management and glycated haemoglobin. Receiver operating characteristics curves were carried out to identify the best cut-off score for each self-care scale considering glycated haemoglobin >7% as outcome of interest.
Results
Self-care monitoring and self-care management were associated to glycated haemoglobin in both patients without (self-care monitoring p = 0.0008; self-care management p = 0.0178) and with insulin therapy (self-care monitoring p = 0.0007; self-care management p = 0.0224). Self-care maintenance was associated to glycated haemoglobin in patients without insulin therapy (p = 0.0118). Cut-off scores providing the best performance were 70 points for self-care maintenance and self-care monitoring, and 60 points for self-care management.
Conclusions
Self-care maintenance, self-care monitoring, and self-care management differently affect glycated haemoglobin in patients with type 2 diabetes mellitus. Clinicians could implement tailored interventions to improve glycaemic control considering the lacking area of self-care.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Diabetes is one of the most relevant public health challenges [1, 2], affecting 463 million people worldwide [3]. Type 2 diabetes mellitus (T2DM) accounts for more than 90% of diabetes cases [4]. T2DM is associated with higher rate of cardiovascular disease [5] and leads to serious microvascular and macrovascular complications [3, 6, 7]. These cause blindness, lower limb amputation, kidney failure, and further disabling consequences, significantly compromising the quality of life, or leading to premature death [5, 8,9,10]. Many of these complications can be prevented by performing adequate self-care behaviours [11, 12].
Self-care was defined as “a process of maintaining health through health-promoting practices and managing illness” [13, 14]. Self-care includes self-care maintenance, self-care monitoring, and self-care management. Self-care maintenance comprises those behaviours aimed at maintaining physical and emotional stability. In diabetes, it means for example adherence to medications, diet, and physical activity recommendations. Self-care monitoring includes behaviours to monitor changes in the body and recognise signs and symptoms. In diabetes, it comprises blood glucose and blood pressure monitoring, and symptom of hypo- or hyperglycaemia recognition. Self-care management is the process of responding to those changes when they occur. In diabetes, this is for example to manage episodes of hypo- or hyperglycaemia [13,14,15]. Self-care in diabetes is associated with improved glycaemic control [7, 11, 16]. Glycated haemoglobin (HbA1c) is the main indicator of long-term glycaemic control because it is able to reflect the cumulative glycaemic trend of the last 2–3 months [17, 18]. Higher HbA1c was associated with higher risk of diabetes complications, coronary heart disease, and stroke [17]. Reduction in HbA1c levels was associated with a decrease in the risk of microvascular complications and diabetes mortality [19].
Several studies assessed the association between one or more specific self-care behaviours (i.e. exercise, diet, foot care, adherence to medication) and HbA1c [7, 11, 16, 20,21,22,23,24]. However, the dynamic and complexity of self-care as a process were never taken into account while studying the relationship between self-care and glycaemic control. Furthermore, the association between self-care maintenance, self-care monitoring, and self-care management and HbA1c was never assessed before. Having this knowledge could be relevant for several reasons. First, it could help clinicians in identifying patients at risk of poor glycaemic control, according to their self-care levels. Second, it could allow to personalise interventions to improve self-care and glycaemic control: self-care maintenance, for example, requires motivation while self-care monitoring and self-care management require skills and problem-solving abilities respectively [14]. Third, it could deepen the overall understanding of the phenomenon of self-care and its relationship with T2DM patients’ clinical outcomes.
The primary objective of this study was to assess the associations between self-care maintenance, self-care monitoring, and self-care management and HbA1c in T2DM patients. To do so, the Self-Care of Diabetes Inventory (SCODI) has been used because it was specifically developed to measure these three concepts [15]. It was also shown to be a psychometrically sound tool to measure self-care in the T2DM population [25, 26]. However, cut-off scores defining adequate or inadequate self-care of the SCODI scales by objective external criteria have not been defined yet. Thus, the secondary aim of this study was to estimate cut-off scores of self-care maintenance, self-care monitoring, and self-care management scales using HbA1c as the outcome of interest.
Methods
This study is a secondary analysis of a previous multicentre observational cross-sectional study [26]. No further data have been collected for this study. Ethical approval was obtained by the Institutional Review Boards of participating centres. Signed informed consent was obtained from all study participants. Study procedures were conducted according to the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Declaration of Helsinki [27].
Sample
A consecutive sample of 540 T2DM patients was recruited in six outpatient diabetes clinics in the North of Italy during outpatient visits, as described in the parent study [26]. Briefly, inclusion criteria were: confirmed diagnosis of T2DM according to guidelines criteria [28] and age ≥ 18 years. Exclusion criteria were: first visit to the diabetes centre; time since the diagnosis of diabetes <1 year; inability to read the study questionnaire; documented cognitive impairment; types of diabetes different from type 2 (as type 1 diabetes, gestational diabetes, or impaired glucose tolerance) [28].
Measurement
Socio-demographic data including gender, age, occupational status, family income, school education, and family support were collected. Clinical data such as years from T2DM diagnosis, body mass index (BMI), presence of comorbidities, presence of diabetes microvascular complications (diabetic retinopathy, diabetic kidney disease, diabetic foot, diabetic neuropathy), and last available value of glycated haemoglobin (HbA1c) were collected by reviewing medical records. Standardised criteria from clinical guidelines were used to verify the T2DM diagnosis and to assess the presence of comorbidities [28].
The SCODI is the self-report tool used to measure self-care maintenance, self-care monitoring, and self-care management as main variables of this study [15]. The SCODI was developed based on the Middle Range Theory of Self-Care of Chronic Illness [14] and it was demonstrated to be a valid and reliable measure of diabetes self-care [15]. Briefly, the self-care maintenance scale measures adherence to main diabetes treatments (i.e. medication, diet exercise). The self-care monitoring scale includes body listening behaviours, such as blood glucose or blood pressure monitoring and symptom recognition behaviours. The self-care management scale includes those behaviours performed by patients to manage symptoms, high or low blood glucose levels, and health problems when they occur. Furthermore, the SCODI allows to measure self-care confidence that is known to be a strong determinant of self-care [14, 15, 26, 29]. Self-care confidence was defined as the degree of confidence a patient has in her/his ability to perform adequate self-care [14]. In this study, self-care confidence was used to adjust the association between self-care behaviours and HbA1c, as better described below. A five-points Likert type scale measures every item of the SCODI. All the SCODI scales provide a 0–100 standardised score where higher scores mean better self-care. Until now, a cut-off of 70 points has been used to classify self-care maintenance, self-care monitoring, self-care management, and self-care confidence as adequate (≥70) or inadequate (<70), as per previous similar studies and tools [15, 30,31,32].
Statistical analysis
Socio-demographic and clinical data were described with frequencies and percentages when variables were categorical and with median and interquartile range when continuous. Patients were stratified according to whether they had insulin treatment because of the differences in their clinical history and self-care behaviours [33]. Moreover, we found a significant interaction between insulin treatment and self-care in the linear regression models on HbA1c. Comparisons of socio-demographic and clinical characteristics between patients with and without insulin treatment were performed using χ2 test or Mann–Whitney U test, as appropriate.
To investigate the association between self-care maintenance, self-care monitoring, and self-care management and HbA1c, linear regression models were adopted, after checking on the linearity assumption. Quadratic and cubic terms were added among the regressors in case of departure from linearity and the likelihood ratio test (LRT) was used to test the overall significance. The associations were adjusted for the following covariates: gender, age, low income, school education, occupation, family support, years from diagnosis of diabetes, number of comorbidities, BMI, self-care confidence, and education in diabetes over the last year. The HbA1c value was considered as percentage in the models and also converted in mmol/mol for descriptive purposes.
Receiver operating characteristics (ROC) curve was applied out to identify the best cut-off score by Youden method for each self-care scale using HbA1c as gold standard and considering a value >7% as inadequate [18]. The area under the ROC curve (AUC), as the measure of the ability of each self-care scale to distinguish between adequate and inadequate HbA1c, was also calculated. Moreover, sensitivity and specificity of the best cut-off score were calculated for each scale and compared with the commonly used threshold score of 70 points.
Results
Socio-demographic and clinical data of the patients, overall and divided according to the presence or not of insulin treatment, are shown in Table 1 together with self-care scales scores. The overall sample of 540 T2DM patients was mostly composed by men (58%; n = 311) aged 60 years or more (77%; n = 415), retired (75%; n = 402) and with a low level of education (none, elementary or middle school: 83%; n = 448). Almost half of the sample (47%; n = 252) have had T2DM for at least 10 years, and the vast majority (87%; n = 469) had at least one comorbidity. Only a small proportion of patients (6%; n = 32) had received education about self-management in diabetes over the last year. Most of the patients (69%; n = 370) were taking oral glucose-lowering medications, the remaining part (31%; n = 170) were taking also insulin. HbA1c blood level was mostly (58%; n = 311) over the typically suggested glycaemic goal of 7% (53 mmol/mol) [18] (median = 7.2% (55 mmol/mol)), and the BMI mostly (77%; n = 417) pointed out overweight (BMI ≥ 25) (median = 28.1). Almost 40% of the sample had at least one diabetes complication (39%; n = 209), whose the most frequent was retinopathy (22%; n = 119). Patients under insulin treatment were typically older (p = 0.025), had diabetes for longer (p < 0.001), were more frequently retired (p = 0.033) and had more comorbidities (p < 0.001) than those without insulin. Furthermore, they had higher levels of HbA1c (p < 0.001) and more complications (p < 0.001) than patients without insulin therapy (Table 1).
Accounting 70 points as the cut-off score, only self-care maintenance (median = 81.3; Q1–Q3 = 72.9–89.6) and self-care confidence (median = 79.6; Q1–Q3 = 66.9–93.2) were adequate in most of the patients, respectively, in 80% (n = 432) and 70% (n = 377). Self-care monitoring was adequate in half of the patients (median = 70.6) and self-care management scores were mostly low (median = 59.4). Self-care monitoring (p < 0.001) and self-care confidence (p = 0.023) scores were better for patients under insulin treatment than for the others.
The presence of insulin therapy was shown to be a modifier of the effect of self-care monitoring (LRT between model without and model with an interaction term of insulin therapy with self-care monitoring p = 0.041) and self-care management (LRT between model without and model with interaction p = 0.001) on HbA1c, showing that their effect was different in the two subgroups. Thus, we stratified the sample by insulin therapy, including also self-care maintenance for homogeneity (LRT between model without and model with interaction p = 0.144). We did not find any other variable as modifier of the effect of self-care on HbA1c. As showed in Fig. 1, HbA1c was inversely correlated with self-care. In patients without insulin therapy, for each increment of ten points of self-care maintenance, HbA1c percentage decreased by 0.09 (beta = −0.009; 95% CI = −0.016 to −0.002) and for each increment of ten points of self-care monitoring, HbA1c decreased by 0.08 (beta = −0.008; 95% CI = −0.012 to −0.003). Self-care management had a quadratic relationship with HbA1c (LRT p = 0.0178): the curve showed very stable values of HbA1c up to about 55 points score, beyond which the concentration of HbA1c was slowly reduced by the increase in the self-care management scores. For patients under insulin treatment, there was no significant relationship between self-care maintenance and HbA1c (LRT p = 0.1231). We found a cubic relationship between self-care monitoring and HbA1c (LRT p = 0.0007): from 40 to 80 points in self-care monitoring score, HbA1c blood level was progressively reduced; from 80 to 100 points the relationship seemed to reverse its trend. Finally, self-care management had a linear relationship with HbA1c: for each increment of ten points in self-care management, HbA1c measured as a percentage decreased by 0.13 (beta = −0.013; 95% CI = −0.024 to −0.002). The results of univariate models are shown in Tables 5, 6, and 7 in Supplementary Material.
When adjusting for relevant covariates, the association between self-care maintenance and HbA1c in patients without insulin therapy became not significant (p = 0.2000) (Table 2). Presence of family support (p = 0.0383), years from diagnosis (p < 0.0001), BMI (p = 0.0080), and self-care confidence (p = 0.0024) resulted significantly associated with the outcome. For patients under insulin treatment, only age (p = 0.0303) and presence of family support (p = 0.0168) showed a statistically significant association with HbA1c (Table 2).
Self-care monitoring in patients without insulin therapy was associated with HbA1c (p = 0.0432) together with lack of occupation (p = 0.0494), presence of family support (p = 0.0483), years from diagnosis (p = 0.0003), BMI (p = 0.0058), and self-care confidence (p = 0.0301). For patients with insulin therapy the cubic relationship between self-care monitoring and HbA1c was significant (LRT p = 0.0004), together with the association of age (p = 0.0095) and presence of family support (p = 0.0047) with HbA1c (Table 3).
Concerning self-care management in patients without insulin treatment, there was a significant quadratic relationship with HbA1c (LRT p = 0.0278). In the same model, lack of occupation (p = 0.0450), low level of education (p = 0.0463), presence of family support (p = 0.0309), years from diagnosis (p = 0.0007), BMI (p = 0.0034), and self-care confidence (p = 0.0005) were associated with HbA1c. For patients under insulin treatment, the HbA1c level was significantly influenced by self-care management (p = 0.0375), age (p = 0.0157), and presence of family support (p = 0.0098) (Table 4).
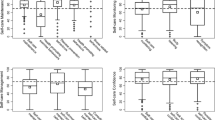
The ROC curves identifying best cut-offs of self-care scales with respect to suboptimal HbA1c (HbA1c > 7%) [18] are shown both for patients without and with insulin therapy in Fig. 2. The best cut-off for self-care maintenance scale in patients without insulin therapy was 76.04 points, with AUC of 0.578. For patients with insulin therapy, it was not meaningful to identify a cut-off, because the association between self-care maintenance and HbA1c was not significant in the linear regression model. However, although it is not properly useful, we reported this cut-off in Fig. 2 for homogeneity. ROC curve of self-care monitoring scale, both in patients without and with insulin therapy showed best cut-off equal to 77.94 points, with AUC, respectively, of 0.608 and 0.627 (Table 8 in Supplementary Material). For self-care management scale in patients without insulin treatment, the best cut-off was 60.94, with AUC of 0.552. For patients with insulin therapy, the best cut-off was 56.94 and the AUC was 0.604. When compared with the 70 points cut-off—the one used by previous studies [15, 30,31,32]—best cut-off scores by Youden method had lower sensitivity than 70 for self-care maintenance in patients without insulin therapy (0.85 vs 0.73) and for self-care monitoring both in patient without (0.54 vs 0.42) and with insulin therapy (0.84 vs 0.75). For self-care management, sensitivity was higher using best cut-offs by Youden method both in patients without (0.52 vs 0.36) and with insulin therapy (0.81 vs 0.34). AUC, sensitivity, and specificity of the best cut-off scores compared to 70 points cut-off were shown in Table 8 in Supplementary Material for each self-care scale.
Discussion
The aims of this study were to evaluate how self-care maintenance, self-care monitoring, and self-care management affect HbA1c in T2DM patients and to identify cut-off scores of self-care scales using HbA1c as gold standard. To the best of our knowledge, this is the first study addressing these issues. We found that self-care maintenance, self-care monitoring, and self-care management differently affect glycaemic control in patients with T2DM. Self-care monitoring and self-care management are associated with HbA1c in both patients without and with insulin therapy. Self-care maintenance is associated with HbA1c in patients without insulin therapy. Furthermore, we found that cut-off scores providing the best sensitivity and specificity to identify suboptimal HbA1c (>7%) for the three self-care scales are different among the scales, and also different from the ones used in previous studies [15, 30,31,32]. These findings are relevant for several reasons. First, clinicians can identify patients at risk of poor glycaemic control, according to their self-care levels. Second, interventions to improve glycaemic control can be tailored, accounting for the area of self-care that is lacking. Finally, the cut-off scores we identified can be used in future research to identify inadequate self-care, according to the patients’ likelihood to have suboptimal glycaemic control.
We found that higher scores of self-care monitoring in patients not receiving insulin were associated with lower HbA1c. This is consistent with previous studies where interventions aimed to improve patients’ self-monitoring of blood glucose significantly reduced HbA1c [19, 34, 35]. However, explaining this finding, we need to consider that the self-care monitoring scale includes also weight monitoring [36, 37], blood pressure monitoring [38], feet examination, and symptom recognition that were shown to be relevant for T2DM patients. Interestingly, although these behaviours do not directly affect HbA1c, they probably support patients’ self-awareness [39], which contributes to guide self-care decision-making and, consequently, improves health outcomes [18, 19]. Higher self-care monitoring was also associated with lower HbA1c in patients under insulin treatment. Surprisingly, looking at the regression curve, after the score of about 80 points, we found that higher scores of self-care monitoring were progressively associated with increasing values of HbA1c. This pattern might reflect the cross-sectional nature of the study. In fact, it seems that these patients improved their self-care monitoring in response to their inadequate HbA1c, as also found in previous studies [40, 41]. Indeed, the HbA1c of patients under insulin treatment was significantly higher, and we argue that the perceived severity of their clinical situation was higher in these patients, leading to the improvement of self-care monitoring [42, 43].
Self-care management was also significantly associated with HbA1c in patients both without and with insulin therapy. In the first group we found an almost flat curve up to a self-care management of about 55, representing a probably low influence of poor self-care management on HbA1c. This could be due to the rare incidence of the signs and symptoms, measured by the self-care management scale, in this group of patients [44]. However, higher scores of self-care management showed an association with lower HbA1c [45]: according to the model, a patient with a 60 points score will have an HbA1c of 7.2%, while a patients with a 90 or 100 points score will have respectively an HbA1c of 6.9 and 6.7%. In patients under insulin treatment, we found a relevant inverse association both in univariate and in multivariate linear models. These patients had significantly worst HbA1c when compared to the other group and probably they experienced more signs and symptoms [33]. Therefore, the more patients were able to perform self-care management when signs and symptoms occurred, the more HbA1c level improved, as also reported in the literature [46, 47].
As per self-care maintenance, in the simple linear model we found a significant association with HbA1c in patients without insulin therapy, but not in patients taking insulin. When adjusting for other socio-demographic and clinical variables, the association was not significant in both groups. This is surprising because we expected self-care maintenance to be strongly associated with HbA1c, as the scale assesses the adherence to major diabetes treatments. However, the scale is multidimensional and investigates heterogeneous behaviours [15]. In fact, self-care maintenance concerns diet, physical activity, and medications, that directly influence HbA1c [48], but also oral hygiene, smoking, feet care, vaccinations, hand washing, and adherence to visits and check-ups, that have not a direct influence on HbA1c. Thus, as the self-care maintenance construct is so complex, future research should study it longitudinally to better understand if changes in self-care maintenance have an effect on HbA1c.
ROC curves showed that the best cut-off scores for the self-care maintenance, self-care monitoring, and self-care management scales to identify patients with suboptimal HbA1c should be different from the score of 70, used until now [15, 30,31,32]. However, this finding should be discussed according to the aim of the instrument and the area of its application. First, the SCODI was not developed with a diagnostic purpose for HbA1c, but to measure patients’ self-care behaviours. That is why we did not expect to find high AUCs, as our results showed. Second, for a clinical purpose, we believe that sensitivity is the most relevant parameter to consider because we would rather have more false-positive than false-negative cases, based on the HbA1c outcome. In fact, although false-positives might have good glycaemic control, they could benefit anyway from a more in-depth assessment of their knowledge, attitudes, and self-care [11]. Thus, based on our results, we recommend a cut-off score of 70 points for self-care maintenance and self-care monitoring, and a cut-off score of 60 points for self-care management. Again, these cut-off scores should be studied longitudinally in the future. However, our findings add relevant information because they are based on an external objective criterion never tested before for the SCODI’s scales.
Limitations and strengths
The cross-sectional nature of this study represents its main limitation, because it does not allow to determine if self-care behaviours put in place by patients are the cause or the effect of HbA1c levels. Another weakness of the study is not having considered patients’ haemoglobin level: it could affect HbA1c independently of glycaemic control, especially in patients with renal failure [49]. However, not having collected this information, we have performed a sensitivity analysis excluding the 75 patients with diabetic kidney disease and we have verified that our results did not undergo any significant change. Although the study was conducted in one country, the main socio-demographic and clinical characteristics of the sample were comparable to those in the international literature [50]. Moreover, sample size was quite large and the recruitment was consecutive. To the best of our knowledge, this was the first study investigating the relationship between self-care and HbA1c taking into account the complexity of the self-care process as defined by the Middle Range Theory of Self-care of Chronic Illness [14] and using a theoretically grounded psychometrically sound measure [15] for this purpose.
Conclusions
Measuring self-care and supporting patients to improve self-care is relevant for achieving good health outcomes in diabetes. Knowing how self-care maintenance, self-care monitoring, and self-care management affect HbA1c has implications both for clinical practice and research. Clinically, patients with inadequate self-care monitoring and self-care management should be considered at high risk of inadequate glycaemic control. Therefore, interventions should be administered to them to improve their clinical condition. Even if self-care maintenance was not associated with patients’ glycaemic control, patients with inadequate self-care maintenance require further assessment according to the complexity of this part of the self-care process. Further research should: assess the association between self-care maintenance, self-care monitoring, and self-care management and HbA1c by longitudinal designs, also using other instruments than the SCODI; estimate prospectively the best cut-off scores of the SCODI scales assessing changes in HbA1c over time; and develop and test interventions to improve HbA1c through tailored self-care maintenance, self-care monitoring, and self-care management support.
References
B. Zhou, Y. Lu, K. Hajifathalian et al. Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4·4 million participants. Lancet 387, 1513–1530 (2016). https://doi.org/10.1016/S0140-6736(16)00618-8
L. Chen, D.J. Magliano, P.Z. Zimmet, The worldwide epidemiology of type 2 diabetes mellitus - present and future perspectives. Nat. Rev. Endocrinol. 8, 228–236 (2011). https://doi.org/10.1038/nrendo.2011.183
International Diabetes Federation, IDF Diabetes Atlas, 9th edn. (International Diabetes Federation, Brussels, 2019)
S. Chatterjee, K. Khunti, M.J. Davies, Type 2 diabetes. Lancet 389, 2239–2251 (2017). https://doi.org/10.1016/S0140-6736(17)30058-2
World Health Organization, Global Report on Diabetes. (World Health Organization, Geneva, 2016)
M.J. Fowler, Microvascular and macrovascular complications of diabetes. Clin. Diabetes 26, 77–82 (2008). https://doi.org/10.2337/diaclin.26.2.77
American Association of Diabetes Educators, AADE guidelines for the practice of diabetes self-management education and training (DSME/T). Diabetes Educ. 35, 85S–107S (2009). https://doi.org/10.1177/0145721709352436
J. Visaria, N.N. Iyer, A. Raval et al. Incidence and prevalence of microvascular and macrovascular diseases and all-cause mortality in type 2 diabetes mellitus: a 10-year study in a US commercially insured and medicare advantage population. Clin. Ther. 41, 1522–1536.e1 (2019). https://doi.org/10.1016/j.clinthera.2019.05.012
M. Tabesh, J.E. Shaw, P.Z. Zimmet et al. Association between type 2 diabetes mellitus and disability: What is the contribution of diabetes risk factors and diabetes complications? J. Diabetes 10, 744–752 (2018). https://doi.org/10.1111/1753-0407.12659
L.M. Jaacks, K.R. Siegel, U.P. Gujral, K.M.V. Narayan, Type 2 diabetes: a 21st century epidemic. Best Pract. Res. Clin. Endocrinol. Metab. 30, 331–343 (2016). https://doi.org/10.1016/j.beem.2016.05.003
M.A. Powers, J. Bardsley, M. Cypress et al. Diabetes self-management education and support in type 2 diabetes: a joint position statement of the American Diabetes Association, the American Association of diabetes educators, and the Academy of nutrition and dietetics. Clin. Diabetes 34, 70–80 (2016). https://doi.org/10.2337/diaclin.34.2.70
M. Song, Diabetes mellitus and the importance of self-care. J. Cardiovasc. Nurs. 25, 93–98 (2010). https://doi.org/10.1097/JCN.0b013e3181c5a364
B. Riegel, T. Jaarsma, C.S. Lee, A. Strömberg, Integrating symptoms into the middle-range theory of self-care of chronic illness. Adv. Nurs. Sci. 42, 206–215 (2019). https://doi.org/10.1097/ANS.0000000000000237
B. Riegel, T. Jaarsma, A. Strömberg, A middle-range theory of self-care of chronic illness. Adv. Nurs. Sci. 35, 194–204 (2012). https://doi.org/10.1097/ANS.0b013e318261b1ba
D. Ausili, C. Barbaranelli, E. Rossi, et al, Development and psychometric testing of a theory-based tool to measure self-care in diabetes patients: The Self-Care of Diabetes Inventory. BMC Endocr. Disord. 17, (2017). https://doi.org/10.1186/s12902-017-0218-y
J.K.T. Tshiananga, S. Kocher, C. Weber et al. The effect of nurse-led diabetes self-management education on glycosylated hemoglobin and cardiovascular risk factors: a meta-analysis. Diabetes Educ. 38, 108–123 (2012). https://doi.org/10.1177/0145721711423978
S.I. Sherwani, H.A. Khan, A. Ekhzaimy et al. Significance of HbA1c test in diagnosis and prognosis of diabetic patients. Biomark Insights 11, 95–104 (2016). https://doi.org/10.4137/BMI.S38440
American Diabetes Association, 6. Glycemic targets: standards of medical care in diabetes-2019. Diabetes Care 42, S61–S70 (2019). https://doi.org/10.2337/dc19-S006
O. Schnell, H. Alawi, T. Battelino et al. Self-monitoring of blood glucose in type 2 diabetes: recent studies. J. Diabetes Sci. Technol. 7, 478–488 (2013). https://doi.org/10.1177/193229681300700225
T.A. Deakin, C.E. McShane, J.E. Cade, R. Williams, Group Based Training for Self-management Strategies in People with Type 2 Diabetes Mellitus. In: A. Steinsbekk, (ed) Cochrane Database of Systematic Reviews. (John Wiley & Sons, Ltd, Chichester, 2005). p CD003417
R. Carpenter, T. Di Chiacchio, K. Barker, Interventions for self-management of type 2 diabetes: an integrative review. Int. J. Nurs. Sci. 6, 70–91 (2019). https://doi.org/10.1016/j.ijnss.2018.12.002
American Diabetes Association, 5. Lifestyle management: standards of medical care in diabetes-2019. Diabetes Care 42, S46–S60 (2019). https://doi.org/10.2337/dc19-S005
Y. Lu, J. Xu, W. Zhao, H.-R. Han, Measuring self-care in persons with type 2 diabetes: a systematic review. Eval. Health Prof. 39, 131–184 (2016). https://doi.org/10.1177/0163278715588927
J. Caro-Bautista, F.J. Martín-Santos, J.M. Morales-Asencio, Systematic review of the psychometric properties and theoretical grounding of instruments evaluating self-care in people with type 2 diabetes mellitus. J. Adv. Nurs. 70, 1209–1227 (2014). https://doi.org/10.1111/jan.12298
D. Ausili, C. Barbaranelli, B. Riegel, Generalizability of the self-care of diabetes inventory across cultures and languages: Italy and the United States. Eval. Heal. Prof. (2019). https://doi.org/10.1177/0163278719840689
D. Ausili, E. Rossi, P. Rebora et al. Socio-demographic and clinical determinants of self-care in adults with type 2 diabetes: a multicentre observational study. Acta Diabetol. 55, 691–702 (2018). https://doi.org/10.1007/s00592-018-1135-x
World Medical Association, World medical association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 310, 2191–2194 (2013). https://doi.org/10.1001/jama.2013.281053
American Diabetes Association, Standards of Medical care in Diabetes-2016. Diabetes Care. 39, S1–S112 (2016)
E. Vellone, L. Pancani, A. Greco et al. Self-care confidence may be more important than cognition to influence self-care behaviors in adults with heart failure: testing a mediation model. Int. J. Nurs. Stud. 60, 191–199 (2016). https://doi.org/10.1016/j.ijnurstu.2016.04.016
B. Riegel, C.S. Lee, V.V. Dickson, B. Carlson, An update on the self-care of heart failure index. J. Cardiovasc. Nurs. 24, 485–497 (2009). https://doi.org/10.1097/JCN.0b013e3181b4baa0
D. Ausili, P. Rebora, S. Di Mauro et al. Clinical and socio-demographic determinants of self-care behaviours in patients with heart failure and diabetes mellitus: a multicentre cross-sectional study. Int. J. Nurs. Stud. 63, 18–27 (2016). https://doi.org/10.1016/j.ijnurstu.2016.08.006
R. Caruso, P. Rebora, F. Dellafiore et al. Clinical and socio-demographic determinants of inadequate self-care in adults with type 1 diabetes mellitus: the leading role of self-care confidence. Acta. Diabetol. 56, 151–161 (2019). https://doi.org/10.1007/s00592-018-1259-z
S. Erpeldinger, M.B. Rehman, C. Berkhout et al. Efficacy and safety of insulin in type 2 diabetes: meta-analysis of randomised controlled trials. BMC Endocr. Disord. 16, 39 (2016). https://doi.org/10.1186/s12902-016-0120-z
International Diabetes Federation, Self-monitoring of blood glucose in non-insulin treated type 2 diabetes. (International Diabetes Federation, Brussels, 2009)
M. Cypress, D. Tomky, Using self-monitoring of blood glucose in noninsulin-treated type 2 diabetes. Diabetes Spectr. 26, 102–106 (2013). https://doi.org/10.2337/diaspect.26.2.102
A. Gummesson, E. Nyman, M. Knutsson, M. Karpefors, Effect of weight reduction on glycated haemoglobin in weight loss trials in patients with type 2 diabetes. Diabetes Obes. Metab. 19, 1295–1305 (2017). https://doi.org/10.1111/dom.12971
J.P.H. Wilding, The importance of weight management in type 2 diabetes mellitus. Int. J. Clin. Pract. 68, 682–691 (2014). https://doi.org/10.1111/ijcp.12384
A. Grossman, E. Grossman, Blood pressure control in type 2 diabetic patients. Cardiovasc. Diabetol. 16, 3 (2017). https://doi.org/10.1186/s12933-016-0485-3
C.Y. Jurgens, Somatic awareness, uncertainty, and delay in care-seeking in acute heart failure. Res. Nurs. Health 29, 74–86 (2006). https://doi.org/10.1002/nur.20118
N. Iqbal, C. Morgan, H. Maksoud, I. Idris, Improving patients’ knowledge on the relationship between HbA1c and mean plasma glucose improves glycaemic control among persons with poorly controlled diabetes. Ann. Clin. Biochem. 45, 504–507 (2008). https://doi.org/10.1258/acb.2008.008034
H. Trivedi, L.J. Gray, S. Seidu et al. Self-knowledge of HbA1c in people with type 2 diabetes mellitus and its association with glycaemic control. Prim. Care Diabetes 11, 414–420 (2017). https://doi.org/10.1016/j.pcd.2017.03.011
P. Shabibi, M.S. Abedzadeh Zavareh, K. Sayehmiri et al. Effect of educational intervention based on the Health Belief Model on promoting self-care behaviors of type-2 diabetes patients. Electron Physician 9, 5960–5968 (2017). https://doi.org/10.19082/5960
S.O. Adejoh, Diabetes knowledge, health belief, and diabetes management among the Igala, Nigeria. SAGE Open 4, 215824401453996 (2014). https://doi.org/10.1177/2158244014539966
A. Gupta, A.K. Gupta, T.P. Singh, Occurrence of complications in newly diagnosed type 2 diabetes patients: a hospital based study. J. Indian Med. Assoc. 111, 245–247 (2013)
M. Captieux, G. Pearce, H.L. Parke et al. Supported self-management for people with type 2 diabetes: a meta-review of quantitative systematic reviews. BMJ Open 8, e024262 (2018). https://doi.org/10.1136/bmjopen-2018-024262
Rusdiana, M. Savira, R. Amelia, The effect of diabetes self-management education on Hba1c level and fasting blood sugar in type 2 diabetes mellitus patients in primary health care in binjai city of north Sumatera, Indonesia. Open Access Maced J. Med. Sci. 6, 715–718 (2018). https://doi.org/10.3889/oamjms.2018.169
C. Yuan, C.W.K. Lai, L.W.C. Chan et al. The effect of diabetes self-management education on body weight, glycemic control, and other metabolic markers in patients with type 2 diabetes mellitus. J. Diabetes Res. 2014, 789761 (2014). https://doi.org/10.1155/2014/789761
American Diabetes Association, Standards of medical care in diabetes-2019. Diabetes Care 42:S1–S193 (2019). https://doi.org/10.2337/dc19-Sint01
I.C. Kuo, H.Y.H. Lin, S.W. Niu, et al Anemia modifies the prognostic value of glycated hemoglobin in patients with diabetic chronic kidney disease. PLoS ONE 13, (2018). https://doi.org/10.1371/journal.pone.0199378
A. Nicolucci, K. Kovacs Burns, R.I.G. Holt et al. Diabetes attitudes, wishes and needs second study (DAWN2TM): cross-national benchmarking of diabetes-related psychosocial outcomes for people with diabetes. Diabet Med. 30, 767–777 (2013). https://doi.org/10.1111/dme.12245
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Fabrizi, D., Rebora, P., Luciani, M. et al. How do self-care maintenance, self-care monitoring, and self-care management affect glycated haemoglobin in adults with type 2 diabetes? A multicentre observational study. Endocrine 69, 542–552 (2020). https://doi.org/10.1007/s12020-020-02354-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02354-w