Abstract
Published articles reported controversial results about the association between leisure-time physical activity (LTPA) and risk of type 2 diabetes. A meta-analysis of prospective cohort studies was conducted to explore the effect of LTPA on the incidence of type 2 diabetes. PubMed and Embase databases were searched from its inception to June 13, 2014. Fixed or random effects models were used to calculate the pooled effect sizes based on between-study heterogeneity that was examined by the Q test and I 2 statistic. A total of eight studies, including 296,395 participants and 10,815 incident cases, were included in this study. Both high-level LTPA [high vs. low: hazard ratio (HR) 0.69, 95 % confidence interval (CI) 0.61–0.78] and moderate-level LTPA (moderate vs. low: HR 0.79, 95 % CI 0.70–0.89) were associated with decreased incidence of type 2 diabetes. In conclusion, LTPA was significantly associated with decreased risk of diabetes; high-level LTPA is more beneficial in decreasing the incidence of type 2 diabetes than moderate-level LTPA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The number of patients with diabetes worldwide has more than doubled during the past 20 years [1]. The economic cost of diabetes is enormous and is destined to increase with the increasing number of diabetes. In 2010, global health expenditure attributed to diabetes was estimated to be $376 billion, which made up 12 % of all global health expenditure, and by 2030, the estimated global health expenditure attributed to diabetes is expected to increase by 30–34 % from 2010, reaching $490–893 billion [2]. Besides, complications of diabetes, particularly renal and cardiovascular diseases, substantially increase the risk of subsequent severe illness and death [3].
Physical activity is one of the most important modifiable factors in the primary prevention of non-infectious chronic diseases. The overall incidence of diabetes could be reduced by 58 % by physical activities as well as diet control in population at high risk for diabetes [4]. Leisure-time physical activity (LTPA) is an important component of physical activity and a widely accessible, inexpensive, effective intervention to control and prevent disease. Therefore, it is of practical importance to understand the association between LTPA and type 2 diabetes in taking measures to reduce the prevalence of type 2 diabetes.
Many prospective studies have investigated the relationship between LTPA and type 2 diabetes [5–12]. However, the findings have been inconsistent, and there has not been a systematic review of the relationship between LTPA and type 2 diabetes. A meta-analysis conducted in 2007 showed an inverse association between physical activity of moderate intensity and the risk of type 2 diabetes, but it did not distinguish the types of physical activity, and it focused on total physical activity instead [13]. In addition, many articles exploring the association between physical activity and type 2 diabetes have been published since 2007; thus it is necessary to update the study results. We systematically reviewed the literature to determine the relationship between LTPA and type 2 diabetes.
Methods
The meta-analysis of observational studies in epidemiology guidelines were followed for the current study [14].
Search strategy
The PubMed and Embase databases were searched from its inception to June 13, 2014 to identify all relevant literature. MeSH terms and entry terms about the topic were used: (physical activity OR physical activities OR motor activity OR motor activities OR exercise OR exercises OR walking OR energy expenditure) AND (type 2 diabetes OR T2DM) AND (cohort study OR prospective study OR longitudinal study OR follow-up study). The subjects of studies were defined as humans, and the languages of articles were limited to English and Chinese, because the reviewers are fluent in both of these languages. Reference lists of all included studies and review articles were manually reviewed to identify additional studies.
Inclusion criteria
A study must meet the following criteria for inclusion in the analysis: (1) prospective cohort study; (2) exposure of interest being different levels of LTPA; (3) outcome of interest being type 2 diabetes; (4) study population comprising healthy people without history of type 2 diabetes; (5) analysis duly adjusted for confounding factors; and (6) hazard ratio (HR) or relative risk (RR) with 95 % confidence interval (CI; or data to calculate them) being reported. If multiple articles were published from the same cohort, the most informative report was included.
Based on the included studies, boundaries of different levels of LTPA were also summarized. Studies reporting different levels of LTPA with regard to boundaries were excluded.
Data extraction and quality assessment
The following items were extracted for each study: name of the first author, year of publication, study area (country), duration of follow-up, characteristics of cohort population, number of cases with type 2 diabetes, measurement of LTPA, adjustment for potential confounding factors, and estimates of associations. LTPA was categorized into three levels for studies that reported ≥3 levels of PA: the lowest category was defined as low-level LTPA (reference group), the highest category as high-level LTPA, and all categories in between were pooled to represent moderate-level LTPA [15]. LTPA was categorized into high level and low level for studies that reported two levels of LTPA. For each selected study, the HR (95 % CI) or RR (95 % CI) values for the high- versus the low-level LTPA group and for the moderate- versus the low-level LTPA group were extracted [16]. When multiple effect estimates for LTPA presented, lifetime LTPA data or the most recent LTPA data were used. The Newcastle-Ottawa Scale was used to assess the quality of included studies, as recommended by the Cochrane Non-Randomized Studies Methods Working Group [17]. Literature review, data extraction, and quality assessment were performed by two independent investigators (P.H. and H.H.). Any disagreement was settled by discussion.
Statistical analysis
The pooled HR with its corresponding 95 % CI was calculated by pooling the adjusted HR of each study to assess the association of LTPA with the risk of type 2 diabetes. Heterogeneity among studies was assessed using the Q test and the I 2 statistic [18]. I 2 describes the percentage of total variation because of between-study heterogeneity rather than chance. In the presence of substantial heterogeneity (I 2 > 50 %), the DerSimonian and Laird random effects model (REM) was adopted as the pooling method; otherwise, the inverse variance fixed effects model (FEM) was applied as the pooling method [19]. Since several studies only provided HRs of subgroups by sex or race, etc., the overall HR for each study was calculated using REM or FEM based on heterogeneity between subgroups. Meta-regression was conducted to explore the possible sources of between-study heterogeneity. Publication bias was estimated using funnel plot and modified Egger linear regression test [20]. All statistical analyses were performed with STATA version 11.0 (StataCorp LP, College Station, TX). All tests were 2-sided, and a P value <0.05 was considered statistically significant.
Results
Characteristics of studies
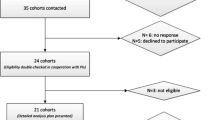
We identified 1789 potentially relevant articles, of which eight studies ultimately met the inclusion criteria (Figure S1 in the online supplement). The total population of the included studies was 296,395 persons, who were initially free from type 2 diabetes, and 10,815 persons developed type 2 diabetes during follow-up. The follow-up duration ranged from 5.1 to 28 years, and the median duration of follow-up was 10.4 years. All included studies reported the effect of high-level LTPA on risk of type 2 diabetes [5–12] and five reported the effect of moderate-level LTPA [5, 7–11]. One study involved men only [11], three involved women only [7–9]; two studies involved both men and women and reported sex-specific results [6, 12]; and two studies involved both men and women but did not report sex-specific results [5, 10]. Three studies defined type 2 diabetes as physician-diagnosed diabetes [7, 9, 11], one study defined type 2 diabetes as use of antidiabetic medication [8], two studies ascertained type 2 diabetes from a national or hospital medication registry [5, 10], one study defined type 2 diabetes by self-report [12], and one study defined type 2 diabetes by self-report or from hospital record [6]. Four studies were conducted in North America [7–9, 11] and four in Europe [5, 6, 10, 12]. Total stars (Table S3 in the online supplement) indicate the quality of the studies assessed by the Newcastle-Ottawa Scale and the maximum score was nine. One study was scored nine stars [12]; two studies were scored eight stars [5, 6]; two studies were scored seven stars [9, 11]; two studies were scored six stars [7, 8]; and one study was scored five stars in quality assessment [12]. The results of all included studies were adjusted for potential confounding factors (Table S1 in the online supplement). Other characteristics of included articles, such as statistics used to estimate HR, type 2 diabetes measurement, and definition of PA levels, are also provided in Table S2 in the online supplement. Boundaries of different levels of LTPAs are summarized in Table S4 in the online supplement; studies with a little difference in the levels of LTPA with regard to the boundary, such as reference 11, were not removed from analysis after discussion.
LTPA and risk of type 2 diabetes
The association between moderate-level LTPA and risk of type 2 diabetes compared with low-level LTPA is shown in Fig. 1. There was heterogeneity between five studies (P Q = 0.058; I 2 = 56.2 %), and REM was used. The overall result showed that moderate-level LTPA was associated with decreased risk of type 2 diabetes compared with the reference group with low-level LTPA (HR 0.79; 95 % CI, 0.70–0.89). Figure 2 showed the association between high-level LTPA and risk of type 2 diabetes compared with low-level LTPA. There was heterogeneity between eight studies examining high-level LTPA and risk of type 2 diabetes (P Q = 0.014; I 2 = 60.2 %); therefore, REM was used to pool the HR. The result of the meta-analysis showed that high-level LTPA decreased the risk of type 2 diabetes compared with low-level LTPA (HR 0.69; 95 % CI 0.61–0.78).
Although there is an overlap between the HR (95 % CI) of moderate-level LTPA and that of high-level LTPA, the HR of moderate-level LTPA is larger than that of high-level LTPA as a whole.
Exploration of the heterogeneity source
Exploratory univariate meta-regression was performed with the introduction of follow-up duration (≥10 vs. <10 years), study area (North America, Europe, and Oceania), definition of LTPA (MET h/week, kcal/week, h/week), publication year, and outcomes of estimation methods (HR, RR). The results of meta-regression indicated that the follow-up duration was the main source of heterogeneity in high-level LTPA (meta-regression coefficient, 0.26; 95 % CI 0.09–0.43; P = 0.01). However, no variable was identified to be the source of heterogeneity in moderate-level LTPA.
Publication bias evaluation
The shape of the funnel plot assessing publication bias was roughly symmetrical for high-level LTPA. No publication bias was detected by Egger test for high-level LTPA (P = 0.685) and moderate-level LTPA (P = 0.063).
Discussion
To the best of our knowledge, this is the first meta-analysis of prospective cohort studies investigating the association between LTPA and development of type 2 diabetes. This meta-analysis included eight studies with a total population of 296,395 and 10,815 diabetes cases identified during follow-up. The results of this study suggested that high-level LTPA might reduce the incidence of diabetes by 22–39 %, while moderate LTPA might reduce the incidence of type 2 diabetes by 11–30 %.
The mechanism between LTPA and type 2 diabetes is complex. LTPA may decrease the incidence of diabetes in several ways. One possible mechanism is through weight loss. LTPA aids in body weight loss, while obesity may increase the risk of type 2 diabetes through induction of insulin resistance [21]. Another potential mechanism may be increasing insulin sensitivity and glucose uptake after exercise. Physical activity was reported to increase insulin-stimulated glycogen synthesis by increasing the number of Glucose transporter 4 (GLUT-4) in the plasma membrane and the activity of hexokinase ΙΙ and glycogen synthase [22]. In addition, Park et al. found that exercise ameliorates glucose homeostasis via Ca2+ signals, which regulate GLUT-4 translocation [23]. It is also possible that people engaged in more LTPA may be more conscientious about their health and also eat healthier, while diet has been identified to be associated with type 2 diabetes [24, 25].
Previous studies and meta-analyses have also found that regular LTPA was associated with other diseases, including hypertension, cardiovascular disease as well as metabolic syndrome [16, 26, 27]. By comparing the results of these studies, we concluded that the effect of LTPA in preventing type 2 diabetes was more obvious than in the other diseases. Regular LTPA should be promoted to prevent diabetes as well as other chronic diseases.
This meta-analysis had several major strengths. First, all included studies were prospective cohort studies, which investigated the causal inference between LTPA and type 2 diabetes and provided a strong case of credibility due to their methodological strengths. Second, the statistical power of this study was considerably high because of the large sample size. Third, confounding bias was reduced, since all included studies were adjusted for confounding factors. There were also some limitations of this meta-analysis. First, only English and Chinese articles were searched for inclusion; eligible articles in other languages were not included in the analysis, which may influence the pooled estimated value. Second, possible bias from the pooling of HR and RR should be noted even if it was not significant in the meta-regression. HR was calculated by Cox proportional hazards models, while RR was estimated based on pooled logistic regression. Different statistical methods may result in the bias of the pooled result. Third, we were unable to determine a dose–response association between LTPA and the incidence of type 2 diabetes, since different units, such as MET h/week, kcal/week, h/week, were used to quantify physical activity.
In conclusion, the results of this meta-analysis suggested that LTPA was significantly associated with a decreased risk of type 2 diabetes, and high-level LTPA is more beneficial in decreasing the incidence of type 2 diabetes than moderate-level LTPA. Therefore, it is worthy of increasing LTPA as a widely accessible and inexpensive intervention to prevent type 2 diabetes.
References
P.Z. Zmmet et al., Diabetes: a 21st century challenge. Lancet Diabetes Endocrinol. 2(1), 56–64 (2014)
P. Zhang et al., Global healthcare expenditure on diabetes for 2010 and 2030. Diabetes Res. Clin. Pract. 87(3), 293–301 (2010)
H.H. Parving et al., Cardiorenal end points in a trial of aliskiren for type 2 diabetes. N. Engl. J. Med. 367(23), 2204–2213 (2012)
J. Tuomilehto et al., Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N. Engl. J. Med. 344(18), 1343–1350 (2001)
K. Waller et al., Leisure-time physical activity and type 2 diabetes during a 28 year follow-up in twins. Diabetologia 53(12), 2531–2537 (2010)
J. Joseph et al., Incidence of and risk factors for type-2 diabetes in a general population: the Tromso Study. Scand. J. Public Health. 38(7), 768–775 (2010)
J.S. Rana et al., Adiposity compared with physical inactivity and risk of type 2 diabetes in women. Diabetes Care 30(1), 53–58 (2007)
J. Hsia et al., Physical activity and diabetes risk in postmenopausal women. Am. J. Prev. Med. 28(1), 19–25 (2005)
A.R. Weinstein et al., Relationship of physical activity vs body mass index with type 2 diabetes in women. JAMA 292(10), 1188–1194 (2004)
G. Hu et al., Occupational, commuting, and leisure-time physical activity in relation to risk for Type 2 diabetes in middle-aged Finnish men and women. Diabetologia 46(3), 322–329 (2003)
F.B. Hu et al., Physical activity and television watching in relation to risk for type 2 diabetes mellitus in men. Arch. Intern. Med. 161(12), 1542–1548 (2001)
N. Haapanen et al., Association of leisure time physical activity with the risk of coronary heart disease, hypertension and diabetes in middle-aged men and women. Int. J. Epidemiol. 26(4), 739–747 (1997)
C.Y. Jeon et al., Physical activity of moderate intensity and risk of type 2 diabetes: a systematic review. Diabetes Care 30(3), 744–752 (2007)
D.F. Stroup et al., Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15), 2008–2012 (2000)
G.C. Wendel-Vos et al., Physical activity and stroke. A meta-analysis of observational data. Int. J. Epidemiol. 33(4), 787–798 (2004)
J. Li et al., Physical activity and risk of cardiovascular disease–a meta-analysis of prospective cohort studies. Int. J. Environ. Res. Public Health. 9(2), 391–407 (2012)
G.A. Wells et al., The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses (2013). http://www.ohri.ca/programs/clinical_epidemiology/nosgen.pdf. Accessed 1 Sept 2014
J.P. Higgins et al., Quantifying heterogeneity in a meta-analysis. Stat. Med. 21(11), 1539–1558 (2002)
J.P. Higgins et al., Measuring inconsistency in meta-analyses. BMJ 327(7414), 557–560 (2003)
R.M. Harbord et al., A modified test for small-study effects in meta-analyses of controlled trials with binary endpoints. Stat. Med. 25(20), 3443–3457 (2006)
J. Ye, Mechanisms of insulin resistance in obesity. Front. Med. 7(1), 14–24 (2013)
G. Perseghin et al., Increased glucose transport-phosphorylation and muscle glycogen synthesis after exercise training in insulin-resistant subjects. N. Engl. J. Med. 335(18), 1357–1362 (1996)
D.R. Park et al., Exercise ameliorates insulin resistance via Ca2+ signals distinct from those of insulin for GLUT4 translocation in skeletal muscles. Diabetes 64(4), 1224–1234 (2015)
K.A. Meyer et al., Carbohydrates, dietary fiber, and incident type 2 diabetes in older women. Am. J. Clin. Nutr. 71(4), 921–930 (2000)
M.B. Schulze et al., Glycemic index, glycemic load, and dietary fiber intake and incidence of type 2 diabetes in younger and middle-aged women. Am. J. Clin. Nutr. 80(2), 348–356 (2004)
P. Huai et al., Physical activity and risk of hypertension: a meta-analysis of prospective cohort studies. Hypertension 62(6), 1021–1026 (2013)
D. He et al., Association between leisure time physical activity and metabolic syndrome: a meta-analysis of prospective cohort studies. Endocrine 46(2), 231–240 (2014)
Acknowledgments
The study was supported by Risk Factor and Intervention Strategy of Life Expectancy in Shandong Province (2013WS0168).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Pengcheng Huai and Huiju Han have contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Huai, P., Han, H., Reilly, K.H. et al. Leisure-time physical activity and risk of type 2 diabetes: a meta-analysis of prospective cohort studies. Endocrine 52, 226–230 (2016). https://doi.org/10.1007/s12020-015-0769-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-015-0769-5