Abstract
Idiopathic pulmonary fibrosis (IPF) is a devastating disease characterized by obliteration of alveolar architecture, resulting in declining lung function and ultimately death. Pathogenic mechanisms remain unclear but involve a concomitant accumulation of scar tissue together with myofibroblasts activation. Microparticles (MPs) have been investigated in several human lung diseases as possible pathogenic elements, prognosis markers and therapeutic targets. We postulated that levels and cellular origins of circulating MPs might serve as biomarkers in IPF patients and/or as active players of fibrogenesis. Flow cytometry analysis showed a higher level of Annexin-V positive endothelial and platelet MPs in 41 IPF patients compared to 22 healthy volunteers. Moreover, in IPF patients with a low diffusing capacity of the lung for carbon monoxide (DLCO<40%), endothelial MPs (EMPs) were found significantly higher compared to those with DLCO>40% (p = 0.02). We then used EMPs isolated from endothelial progenitor cells (ECFCs) extracted from IPF patients or controls to modulate normal human lung fibroblast (NHLF) properties. We showed that EMPs did not modify proliferation, collagen deposition and myofibroblast transdifferentiation. However, EMPs from IPF patients stimulated migration capacity of NHLF. We hypothesized that this effect could result from EMPs fibrinolytic properties and found indeed higher plasminogen activation potential in total circulating MPs and ECFCs derived MPs issued from IPF patients compared to those isolated from healthy controls MPs. Our study showed that IPF is associated with an increased level of EMPs in the most severe patients, highlighting an active process of endothelial activation in the latter. Endothelial microparticles might contribute to the lung fibroblast invasion mediated, at least in part, by a fibrinolytic activity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Idiopathic pulmonary fibrosis (IPF) is a devastating lung disease characterized by progressive obliteration of normal alveolar architecture and replacement by fibrotic tissue. The result is declining lung function, progressive dyspnea and ultimately death within 3–5 years of diagnosis [1]. Precise pathogenic mechanisms are still largely debated but they involve a progressive accumulation of scar tissue and myofibroblasts activation following epithelial injuries of an unknown nature. IPF is also associated with a major pulmonary vascular remodeling, an aberrant angiogenesis with a vascular ablation associated to a decreased mobilization of endothelial progenitor cells [2,3,4]. These angiogenic abnormalities could largely contribute to gas exchange impairment.
The role of extracellular vesicles (EVs) in human pulmonary diseases both as pathogenic determinants and biomarkers is being actively investigated. The most studied EVs are circulating microparticles (MPs). They are defined by a diameter from 100 to 1000 nm, and are released by shedding from the surface of different cell types upon activation: endothelial cells, platelets, leukocytes or erythrocytes. Mechanisms regulating MPs formation include cytoskeleton remodeling and externalization of phosphatidylserine. Increased numbers of MPs have been documented in several lung diseases such as pulmonary arterial hypertension (PAH) [5], chronic obstructive pulmonary disease (COPD), asthma, lung cancer or parenchymal lung disease such as systemic sclerosis (SS) [6]. Moreover, specific MP populations and/or procoagulant properties might correlate with disease severity and/or lung function parameters in PAH [7, 8] or SS [9, 10]. More than just serving as a disease biomarker, evidence has accumulated showing that MPs are involved in several biological processes. Indeed, MPs can convey functional RNA species and proteins from one cell to another, an open up the area of horizontal transfer of bioactive molecules in cell-to-cell communication [11, 12].
To date, there are no available data assessing circulating MPs level and characterization in the setting of IPF. We investigated the number and cellular origin of circulating MPs in patients with this condition and describe endothelial microparticles (EMPs) as potential marker of disease severity. We then analyzed EMPs produced by endothelial progenitor cells (ECFCs) isolated from IPF patients or controls to decipher their potential involvement in fibrogenesis.
Methods and Patients
Study Populations
Study population consisted of 41 patients with recently diagnosed IPF (< 9 months) enrolled in the « COFI » French national cohort between 2008 and 2012. The study was approved by the local ethic committee Île-de-France II (registration number 2006 − 108). Controls were healthy volunteers (60–90 years old), clear of any pulmonary or cardiovascular disease and any history of cancer, enrolled in the VIMOPEIL cohort at the Clinical Investigation Center of European Hospital Georges Pompidou [13].
Quantification of Circulating MP Sub-populations
Collected blood was centrifuged twice at 1500 g for 15 min and platelet-poor-plasma was stored at − 80 °C, as previously described [14]. MPs was count by flow cytometry on a Gallios flow cytometer (Beckman & Coulter) as previously described [15, 16]. First, MPs were selected in an FSC/SSC gate calibrated using 0.1, 0.3, 0.5 and 0.9 µm FSC calibration beads (Megamix-Plus, Biocytex, France), following manufacturer recommendations for the cytometer settings as previously described [17]. 0.1 to 1 nm selected events were then analyzed depending on their fluorescence to classify their sub-population origin and quantify them, in presence of counting beads as an intern counting standard (Accucount, Spherotech). MPs were labeled in diluted plasma (1/10 in NaCl or 1/20 for CD62E labeling) using the following markers: annexin V-FITC (labeling PS, Beckman & Coulter), E-selectin/CD62e-FITC (R&D), CD31-PE (Beckman & Coulter), CD144-PE (Beckman & Coulter), platelet CD41-PC7 (Beckman & Coulter), monocyte CD14-PE (R&D systems) and neutrophil CD66b-FITC (Beckman & Coulter). MPs were selected by gating on FSC/SSC criteria MP sized events (gate calibrated using Megamix-Plus FSC, Biocytex). Data analysis used FlowJo software.
Endothelial Progenitor Cell Isolation and Vesicle Formation
Endothelial progenitor cells subtype used here were endothelial colony forming cells (ECFCs) known to be main vasculogenic cells in adults [18, 19]. ECFCs were isolated from whole peripheral blood collected on heparin from IPF patients and controls. Blood samples were diluted with PBS/EDTA 2 mM and centrifuged at 1200 g for 20 min, on density gradient (Histopaque, density of 1077, Sigma). Obtained mononuclear cells were washed twice in PBS/EDTA. Cells were sprayed on fibronectin at a density of 5 × 106 per well of 6 well-culture plate in a specific endothelial cell growth medium (EGM2, Lonza) added with 10% fetal calf serum (FCS). Whole blood and mononuclear cells were counted on Sysmex XN-Series™. Culture wells were screened twice a week, looking for ECFC growth. Each new colony was isolated and sprayed. EMPs were obtained in vitro by stimulation of cultured ECFC using TNF-α (R&D) as previously described [20]. Briefly, ECFCs were starved overnight in endothelial basal medium (EBM2) with 0.5% FBS before being stimulated with 25 ng/mL TNF-α during 24 h. Supernatant was then centrifuged twice at 1500 g for 15 min, then at 14,000 g for 2 min in order to eliminate cell debris and then stored at − 80 °C. To isolate EMPs from frozen conditioned medium, the obtained conditioned culture medium was centrifuged at 20,000 g for 90 min and then washed twice using MPs washing buffer (HEPES 10 mM, NaCl 140 mM, azide 0.01%). Control cord-blood ECFCs (so-called CB-EMPs) were obtained from cord blood mononuclear cells as previously described [21]. EMP quantification from ECFC was done by flow (annexin V – FITC, acoustic focusing cytometer Attune, Life Technologies TM) using the same settings methods and the same calibration beads as described above for Gallios quantification of circulating MPs (Beckman & Coulter) settings.
EMPs count is normalized before using them for fibroblast activation. Numbers of EMPs were normalized to cell numbers in each condition. After collection of supernatant, cells were trypsinized and viable cells counted (tryptan blue) for a normalization of EMPs to ECFC number in culture. In order to appreciate the EMPs quantitative ability after TNF-α activation of the three different sources of ECFC (healthy adults, cord blood and IPF patients), we choose to express this number of EMPs per 104 cells in percentage. Thus, we then normalized every single value to the basal mean value of the control group without activation by TNF-α. Numbers of EMPs were normalized to cell numbers in each condition.
Fibroblast Activation by EMPs Derived from ECFC
Fibroblast activation was performed with ECFC-derived MPs at the concentration of 2 × 106 AnnV+ MPs/mL for duration of 72 h. This concentration has been chosen because it corresponds to circulating concentration of EMPs in IPF patients. In proliferation tests, deposit collagen quantification, fibroblasts to myofibroblasts transdifferentiation and stress fiber formation, the amount was equivalent to 100 EMPs per target cell. For migration test in Boyden chamber model, the amount was equivalent to 80 EMPs per target cell.
Normal Human Lung Fibroblast (NHLF) Proliferation
NHLF (NHLF, Lonza) proliferation was studied by colorimetric paranitrophenylphosphatase (pNPP) activity method as previously described [22]. NHLF were seeded at a density of 20,000 cells per well of 12 well-culture plate in fibroblast growth medium (FGM2) containing 10% FCS. After an overnight starving to synchronize cell cycle and to eliminate MPs present in FCS, NHLF were activated with EMPs. Proliferation was evaluated by a daily count of cells, both microscopically using Kova slides and automatically, using Scepter cell counter (Merck Millipore). NHLF were incubated at 37 °C with 3 mg/mL pNPP solution for 90 min and pNPP reaction was inhibited with NaOH 1N. Absorbance was read at 405 nm.
Collagen Deposit by NHLF
Extracellular matrix, especially type I collagen (and type III) deposit and accumulation is a key phase observed in fibrotic tissue in IPF. To test the capacity of EMPs to induce collagen production and deposit in NHLF, cells were seeded in 6 well culture plates, starved (0.5% FCS overnight) and treated once, then at each medium change every 72 h, with 2 × 106 EMPs/mL. Supernatant was centrifuged twice at 1500 g for 15 min to eliminate cell debris. Collagen from basal lamina was extracted with cold acetic acid/pepsin overnight at 4 °C. Quantitation was realized using Sircol Soluble Collagen Assay (Biocolor), following manufacturer recommendations in extracted collagen and in cell culture supernatant.
Myofibroblast Differentiation of NHLF
Fibroblast to myofibroblasts differentiation is also a key phase in IPF. To test the ability of EMPs to induce NHLF differentiation into myofibroblasts, EZ slides culture chamber were seeded with NHLF in the presence or absence of 2 × 106EMPs/mL. Culture medium was changed every 72 h and supplied with EMPs. After a 6 days culture in vitro, cells were fixed with cold pure methanol on ice for 10 min. Differentiated NHLF were incubated with a mouse anti-human αSMA (Sigma), followed by incubation with anti-mouse IgG-FITC for 1 h at RT. After washing, slides were mounted using Vectashield mounting medium, staining cells nuclei with DAPI (Vector Laboratories).
NHLF Migration in Boyden Chamber
To test IPF-EMP effects on NHLF migration capacity, we used a Boyden chamber model with 8 µm pores transwells coated with 0.2% gelatin, under growth factor gradient density conditions (recombinant-fibroblast growth factor, added with 10% FCS) for chemoattraction. NHLF were treated once with 2 × 106 EMPs/mL during 5 days of culture, or untreated (control). Cells were trypsinized, washed with PBS and stained with 5 µM intra-vital fluorescent cell trace (Cell Trace CFSE, Life Technologies). They were then washed again and suspended in EBM2 at a density of 105 cells/mL. One hundred microliter of this suspension were dropped on the upper face of the transwell, the bottom face was inserted in 600 µL of chemoattractive medium in 24 well plate. After 5 h of incubation at 37 °C, cells were fixed with HBSS Mg + + Ca + + 1.1% glutaraldehyde. The permeable support was cut out and deposited on a slide. We used Vectashield mounting medium that contains DAPI (Vector Laboratories) to stain migrant cells nuclei. Cells were observed by fluorescence microscopy, using green filter for cell localization with CFSE coloration. Blue filter was also used for cell’s nucleus localization labeled with DAPI, as a counting control. Each support membrane was analyzed on 10 fields and the final result was a mean number of cells having migrated per surface unit. Support membrane surface was measured using image J.
Stress Fiber Formation in NHLF
The effect of EMPs on filamentous actin fiber (F-actin) formation in NHLF was analyzed. NHLF were overnight starved, cultured on EZ slides (Merck Millipore) and treated with 2 × 106 EMPs/mL for 15 and 30 min. They were fixed with cold pure methanol for 10 min and F-actin fibers were stained using phalloidin and observed by fluorescent microscopy using rhodamine filter. NHLF nuclei were stained with Vectashield mounting medium. F-actin fibers were quantified using Image J fluorescence image analysis.
Isolation of MPs from Plasma
Defrosted MPs were centrifuged first at 13,000 g, 2 min in order to eliminate cryoprecipitate debris. Supernatant plasma was centrifuged at 20,000 g, 90 min. The pellet was washed twice in washing buffer (HEPES 10 mM, NaCl 140 mM, azide 0.01%) and centrifuged again at 20,000 g, 90 min. Final pellet was suspended in 20 µL in the same buffer and then frozen at − 20 °C overnight before being stored at − 80 °C. MPs (10 µL) were lysed by five successive cycles of freezing/defrosting − 196 °C (in liquid nitrogen) and 37 °C. MP proteins were quantified using a NanoDrop® spectrophotometer, using BSA as standard (from 0.1 to 1 mg/mL).
Fibrinolytic Potential of MPs
EMP fibrinolytic potential was measured using zymography as a qualitative method and plasmin generation test as a quantitative one. For zymography, MPs were isolated from 8 mL of patients or healthy controls blood plasma with sodium dodecylsulphate-polyacrylamide gel electrophoresis (SDS–PAGE) 8%, pH 8.3 at 110 volts. After migration, the gel was rinsed twice 30 min in a 2.5% triton solution to eliminate SDS and then for 15 min in pure water. The gel was finally transferred onto a fibrin/agarose gel obtained by coagulation at 37 °C of 1 mg/mL bovine fibrinogen (Bovogen Biological, Australia) with 0.2u/mL bovine thrombin in type VII agarose (Sigma®). This gel was enriched with plasminogen (100 nM). The overlapped gels were incubated at 37 °C for 36 h. Zymography on lysed EMPs was also performed.
The second test was realized in 96 wells u-bottom microplates, containing 10 µL of MPs suspension, 1 µM of plasminogen and 0.75 mM plasmin chromogenic substrate (CBS, Stago), in a final volume of 60 µL of phosphate buffer. At 37 °C, MP plasminogen activators convert plasminogen to plasmin, which cleaves the CBS. The resulting paranitroaniline absorbs at 405 nm. Optical density was measured each 120 s during 12 h. We used u-PA as standard and positive control. Initial velocity determined the plasmin generation activity of MPs samples. We also realized the plasmin generation test by IPF-EMPs and CB-EMPs as described above. We used the same method to quantify ECFCs isolated EMPs plamin generation activity.
Measurement of Soluble u-PA and t-PA
Plasma levels of urokinase were measured with highly sensitive ELISAs as recommended by the manufacturer (reference DU-PA00, R&D Systems, Minneapolis, MN, USA). Plasma level of t-PA antigen was measured with Asserachrom® t-PA kit (Diagnostica Stago, Asnières-Sur-Seine, France).
Circulating Cell Transcriptome Analysis
Total circulating cells RNA was isolated from patients and controls whole blood using PAXgene blood RNA kit (Qiagen®) following the manufacturer procedures. RNA was quantified by measuring absorbance at 260 nm on NanoDrop ND-1000 (Labtech®). Reverse transcription to complementary DNA (cDNAs) was realized using QuantiTect Reverse Transcription kit (Qiagen®) following the manufacturer procedures. Taqman® technique was used for quantitative PCR for PLAT gene (t-PA gene, Hs00263492_m1, Applied®) and PLAU gene (u-PA gene, Hs01547054_m1, Applied®). GAPDH gene (4326317E, Applied®) was used to normalize results. Each well contained 5 µL of Master Mix (Universal PCR Master MIX, Applied®), 0,5 µL of GAPDH primer, 0,5 µL of interest gene primer, 2 µL of sample cDNAs and 2 µL of pure water. We performed 50 amplification cycles during 10 min at 90°, 15 s at 95° and 10 min at 60° on TaqMan 7900 HT FAST (Applied Biosystems®). Results were analyzed on SDS v2.3 software and were expressed as a normalized ratio regarding to the quantification Ct limit arbitrary fixed at 35.
Statistics
Data are shown as means ± SD. Intergroup comparisons were based on the Mann and Whitney nonparametric test. All statistical tests were performed using the Stat View software package (SAS, Cary, NC, USA). Differences with P < 0.05 were considered statistically significant.
Results
Endothelial Microparticles are Increased in Patients with Severe IPF
Study population consisted of 41 patients with IPF with a sex ratio of 5 (M/F) and a median age of 71 years. They were compared to 22 healthy controls aged 60 to 90 years.
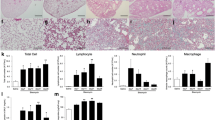
Flow cytometry analysis showed an increase of Annexin-V positive MPs in IPF patients compared to healthy volunteers (respectively with mean of 14,141 ± 336 vs 27,151 ± 4723, with a p = 0.02). This increased level was represented by endothelial E-selectin MPs and platelet MPs (PMPs) (E-selectin MPs in IPF patients vs healthy volunteers: 124 ± 47 vs 1032 ± 295, respectively, p = 0.0003; PMP in IPF and controls: 1550 ± 246 vs 7039 ± 2650, respectively, p = 0.001). We didn’t found any significant difference between CD31 and CD144 positive MPs (with respectively a p = 0.27 for CD144-MPs and 0.82 for CD31-MPs), in contrary of E-selectin MPs. CD14 positive monocyte MPs were decreased in IPF patients (705 ± 196 vs 230 ± 150 in IPF and controls, respectively, p = 0.01). No difference was observed in neutrophil MPs (p = 0.82) (Fig. 1). To confirm relevance of our results on EMPs and PMPs, we analyzed circulating MPs quantification in percentage of annexin-V positive MPs. PMPs represent 50% of annexin-V positive MPs while EMPs represent 1 to 10% of annexin-V positive MPs according to disease status. By expressing circulating MPs quantification in percentage of annexin-V positive MPs, we did not found any significant increase in PMPs (p = 0.73). The difference between controls and IPF patients is always clearly significant for E-selectin positive MPs while it becomes slightly significant for other EMPs subpopulations (CD144 and CD31 EMPs, both with a p = 0.04) as shown in Fig. 2a, confirming relevance of EMPs in IPF and pointing out a specific involvement of endothelial activation state in IPF. We then sought to determine whether circulating MP levels might reflect IPF severity as evaluated by one of its most relevant functional parameters i.e. the Diffusing capacity of the Lung for Carbon monoxide (DLCO). DLCO is a reliable guide to outcome and values of less than 40% predicted are generally indicative of advanced disease. EMPs markedly differed according to the DLCO threshold. Indeed, subjects with a DLCO < 40% predicted, i.e. the most severe ones, exhibited a significant increase in EMP counts compared to those with a DLCO > 40% predicted (Fig. 2b) with values of 7590 ± 2729 vs 2840 ± 1302 in DLCO < 40% and DLCO > 40%, respectively (p = 0.02). Conversely, no difference was observed for PMPs (Fig. 2c) or other MPs.
Quantification of circulating MPs in IPF. Left and center panels: cytograms for healthy controls (left) and IPF patients (center). Gray: negative control for annexin V labeling (a), or isotypic controls (b to e); Green: annexin V labeling (total MP, a) or specific antibodies for endothelium (Eselectin, b), platelets (CD41, c), monocytes (CD14, d) and neutrophils (CD66b, e). Right panel: quantitative analyses of MP counts. Open bars: healthy controls, closed bars: IPF patients.
EMPs are the main actor in circulating MPs in IPF. a E-selectin, CD144 and CD31 are all significantly increased in IPF compared to healthy controls when MPs count are expressed by percentage of annexin-V positive MPs. b Numbers of EMPs counted in IPF patients according to DLCO cut-off of 40%. Results are medians ± SEM (p = 0.02). c Numbers of PMPs counted in IPF patients according to DLCO cut-off of 40%. Results are medians ± SEM (p = 0.31)
EMPs Generated from IPF Patients-Endothelial Progenitor Cells Induce Fibroblast Migration Potential
ECFCs obtained from cord blood, whole blood of healthy volunteers or IPF patients were treated with TNF-α to induce EMPs release. Interestingly, all ECFC origins were able to give rise to a significant EMPs generation. In particular, EMPs from ECFCs derived from IPF patients were found threefold higher after TNF-α (Fig. 3a, p = 0.002). ECFC-derived EMPs were further used in vitro to assess their potential capacity to modulate the fibrogenic properties of NHLF (Fig. 3b). For this purpose, they were used at concentrations comparable to circulating EMPs counts found in IPF patients. Because increase after TNF-α was comparable in CB and PB-ECFC, we only used CB-EMPs derived ECFC as controls to activate fibroblast in our next experiments.
Vesicle formation ECFC isolated from cord blood, controls and IPF patients. a Histograms show the numbers of MPs generated from ECFCs upon TNF-alpha activation, quantified by flow cytometry. Respectively from the left to the right, cord blood ECFCs, healthy controls ECFCs and IPF patients ECFCs. In white, basal EMPs generation, in gray, TNF-alpha activated EMPs generation. b Potential effects mediated by EMPs secreted in vitro by TNF-alpha activation on ECFCs
EMPs addition to NHLF culture medium had no effect on cell viability (data not shown), nor on collagen deposition (Fig. 4a) or transdifferentiation potential into myofibroblasts (Fig. 4b). Conversely, NHLF pretreated with IPF-EMPs showed a significantly enhanced migratory capacity compared to those treated with control-EMPs (p = 0.0003) and controls (p < 0.0001) (Fig. 5a) when using a Boyden chamber. Furthermore, a significantly increased formation of F-actin fibers was observed in NHLF pretreated with IPF-EMPs compared to those treated with cord blood-EMPs (p = 0.03) and controls (p = 0.0004) (Fig. 5b), in line with a pro-migratory phenotype.
IPF-EMPs do not modify fibroblast collagen deposit and myofibroblast formation. a Collagen quantification in cell culture deposit ECM. b Fluorescence microscopy: Alpha-SMA staining shows no effects of MPE on fibroblast to myofibroblast transdifferentiation. Upper panel : CB-MPs treated NHLF; lower panel: IPF-MPs treated NHLF
IPF-EMPs induce a fibroblast promigratory phenotype. a IPF-EMPs treated NHLF display an increased migratory capacity in vitro. Cells are traced with intravital dye CFSE. b Increased F-actin fibers in fluorescence microscopy (stained with phalloidin) in IPF-EMPs treated NHLF supporting a promigratory phenotype
Microparticles from IPF Patients Have a Higher Plasmin Generation Potential
One of the potential mechanisms underlying cell migration is matrix proteolysis. We firstly describe global fibrinolytic potential in IPF patients by quantifying both urokinase-type plasminogen activator (u-PA) and tissue-plasminogen activator (t-PA) in platelet poor plama (PPP). We found higher circulating levels of both u-PA and t-PA (IPF vs controls, p = 0.01 and p = 0.03, respectively for u-PA and t-PA) (Fig. 6a). No differences between whole blood cells u-PA and t-PA mRNA levels were observed in (Fig. 6b). These data might suggest that the enhanced fibrinolytic protein levels observed in IPF patient’s plasma do involve MPs themselves and not an increased expression by circulating hematopoietic cells.
MP from IPF patients have an increased ability to generate plasmin. a Circulating levels of fibrinolysis mediators: healthy controls (white bars) and IPF patients (black bars). Both u-PA and t-PA are increased in IPF patients (left and right respectively). b mRNA levels of fibrinolysis mediators in whole blood circulating cells: in white healthy controls, in black IPF patients. u-PA and t-PA are not significantly different in IPF patients and controls. c Plasminogen activation detected with zymography in total circulating MPs. Right panel: IPF-MPs generate plasmin which lysis fibrin gel comparing to controls. Left panel: quantification of generated plasmin: IPF-MPs have increased plasminogen activation potential. d Plasminogen activation detected with zymography in EMPs derived from ECFCs. Right panel: IPF-ECFCs generate plasmin which lysis fibrin gel comparing to controls. Left panel: quantification of generated plasmin: IPF-ECFCs have increased plasminogen activation potential
EMPs have been shown to bear fibrinolytic properties; we thus explored the ability of MPs isolated from of IPF patients and controls plasma to generate plasmin. Figure 6c shows a significant increase in plasmin generation by total circulating MPs from IPF patients compared to healthy controls (p = 0.006), further confirmed by the zymography assay showing a largest MP fibrinolytic activity. Since we described that EMPs are linked to severity of the disease and are probably linked to a profibrotic phenotype, we quantified plasmin generation by EMPs derived from ECFCs from IPF patients compared to healthy control. As described in Fig. 6d, plasmin generation quantification shows that IPF-EMPs display a higher activity than CB-EMPs, suggesting that the total MPs plasmin generation activity is due to EMPs.
Discussion
We have demonstrated in this study that IPF is associated with an increase in circulating endothelial microparticles particularly in the most severe patients i.e. those with a low DLCO. This increase, in addition to being a marker of endothelial lesion and/or activation, might also reflect a pathogenic role of EMPs in the disease as we have shown that those isolated from endothelial progenitor cells from IPF patients could stimulate fibroblasts migration, at least in part through an increase in their plasmin generation capacity.
Microparticles have been largely shown to influence hemostasis, given their procoagulant potential due to the exposure of phosphatidylserine and tissue factor (TF) [23, 24] on their surface. More recently, they have been shown to have a fibrinolytic potential with a strong ability to generate plasmin [25]. An association between blood coagulation and pulmonary fibrosis is well recognized [26]. Based on the role of microparticles in blood coagulation, microparticles-bound TF (MP-TF) procoagulant activity has been previously quantified in subjects with diffuse parenchymal lung disease [27]. Increased levels of MPs have also been shown in the bronchoalveolar lavage fluid of patients with interstitial lung diseases, in particular IPF. However, circulating MPs have never been quantified so far in IPF patients. Therefore, we assessed circulating microparticles in a consistent number (n = 41) of IPF subjects in relation with their disease severity. The present study showed increased PMP and EMP counts in IPF patients compared to controls. PMP is the most abundant MP population in normal peripheral blood, accounting for around 70–90% of all MPs. They exhibit a strong procoagulant phenotype. A role for the activation of blood coagulation and thrombin receptor PAR-1-mediated signaling by FXa is now clear in IPF [28]. A contribution of locally synthesized FX to fibrotic responses to lung injury has been demonstrated [29]. Procoagulant MPs originating from platelets could be involved in these coagulation and profibrotic signals. We did not find any correlation between PMP counts and disease severity in our study. We hypothesize that circulating PMPs levels reflect more a consequence of the deregulation of hemostasis present in IPF than a true actor of its pathogenesis. One of the explanation could also be a technical point: however we used platelet-poor plasma according to recommendations [30], measurement of AnV + MPs and PMPs could result from the degranulation of the residual platelets to the defrosting of the residual platelet in platelet-poor plasma and be just artefactual in accordance to absence of clinical correlation.
In contrast, we showed that plasma levels of MPs of endothelial origin were largely increased in IPF, particularly so in advanced stages of the disease. These findings might suggest that an increased endothelial activation is associated to fibrotic processes. Indeed, IPF is associated with abnormal and heterogeneous vascular remodeling. This aberrant vascular architecture close to fibrotic areas [31] has been hypothesized to result from an imbalance between angiogenic growth factors. The endothelium plays a central role in pulmonary vascular regulation and endothelial dysfunction is increasingly viewed as critical for disease initiation and progression of IPF. Our group confirmed these data by showing an imbalance in circulating endothelial cells and their progenitors in IPF arguing for the presence of endothelial activation in IPF [2].
Experimental studies have demonstrated the ability of EMPs to promote vascular inflammation and angiogenesis, to interfere with coagulation pathways and to regulate vascular tone, thus pointing to a number of biologic mechanisms by which EMPs may contribute to tissue remodeling in IPF. In order to have enough material to assess potential EMPs profibrotic effects, we used those generated in vitro by endothelial progenitors, namely ECFCs (for endothelial colony forming cells), activation rather than EMPs isolated from patient’s plasma. MPs derived from ECFC are thought to reproduce most progenitor cells effects through a horizontal protein and RNAs transfer [32]. Endothelial progenitor cell-derived MPs have been described as vectors of remodeling process [33, 34]. We generated ECFC MPs upon TNF-α activation [20] and firstly showed that ECFCs from IPF patients had an enhanced ability to generate MPs. We then used the latter to activate normal lung fibroblasts and showed that IPF-EMPs exhibited enhancing effects on NHLF migratory capacity in vitro.
MPs, and in general microvesicles, may play a role in intercellular communication by acting as signaling complexes that directly stimulate target cells, transfer receptors between cells, deliver proteins to the target cells and mediate a horizontal transfer of genetic information. Migration is largely dependent on enzymatic functions derived from matrix metalloproteinases (MMPs) and plasmin. Since MPs has been described as vectors of fibrinolytic activity, we focused our attention on the ability of circulating MPs from IPF patients to generate plasmin. Circulating MPs display indeed a range of plasmin generation in various pathological conditions and this activity is partially generated by endothelial MPs, supporting blood fibrinolytic activity. Their surface plasminogen activation is a functional feature that differs between healthy and diseased subjects [25, 35]. Our results show that this activity is significantly increased in IPF patients and that a pro-fibrinolytic and a plasmin proteolytic activity might be mediated by EMPs in this disease. Plasmin generation systems have been shown to enhance fibroblasts migration [36, 37]. It is clear that MP composition drives these effects. EMPs ability to induce migration might also modulate fibrocytes migration to the lung. Fibrocytes are a distinct population of blood-born cells that co-express hematopoietic cell antigens (CD45+) and fibroblasts markers (collagen 1+). They contribute to lung fibrogenesis in several interstitial pneumonitis such as IPF [38] and scleroderma [39]. Attenuation of fibroblasts homing in mouse models directly correlates with a reduction in pulmonary fibrosis [40, 41] and we have previously described a key role for fibroblasts in IPF-associated aberrant vascular remodeling [42]. Increased EMPs which we have shown here to be markedly elevated in IPF might play a role in fibroblasts migration to the lung and therefore contribute to local fibrogenesis. Our study has several limitations. First of all, we compared MPs generation capacities between IPF-ECFC and healthy controls-ECFC (including those isolated from healthy adult donors and from cord blood). Healthy adult donors ECFC are difficult to obtain and more than that, as others and we previously described [13, 18, 43, 44], number of ECFC and their expansion properties are lower than cord blood ECFC. We described in Fig. 3a than despite these discrepancies in ECFC from healthy donors and cord blood ECFC, we have the same ability of both ECFC sources to form EMPs. Thus, we performed all functional analysis on fibroblast activation with CB-ECFC derived-EMPs. Moreover, circulating MPs should have been also a good positive control to activate fibroblasts. However, suspension of isolated MPs from peripheral blood would lead a stimulation of NHLF with all sub-populations of MPs and not only EMPs. Purifying EMPs from total circulating MPs is a tricky point with technical limitations. Moreover, due to the high amount of EMPs needed to perform these experiments, the volume of acceptable collected blood from IPF patients is not high enough. ECFC has been described to be a good reflect of vessel and a “liquid biopsy” of vessels in particular in pulmonary disease [3], thus we think it`s a good cell type to reproduce effect of pathological EMPs from patients with IPF or controls. Another limitation of our study is the absence of exploration of microvesicles subtypes according to size in plasma [45] or ECFC conditioned medium [46] as previously described.
Thus, our results indicate that according to the pathological environment associated to the donor health status, the properties of ECFC in term of tissue repair potential can be affected with significant alterations of EMPs properties. EMPs from ECFC isolated from patients with IPF could increase devastating fibrotic process because of higher fibrinolytic properties. We also can anticipate that EMPs from patients-derived ECFC can have some deleterious effect on vascular system and participate to endothelial lesion in IPF. Since extracellular vesicle has been proposed in regenerative medicine, we need to identify bioengineering strategies able to control the molecular composition and thereby to enhance the therapeutic potential of microvesicles.
In conclusion, this study has shown a marked increase in circulating endothelial MPs in IPF. EMPs might be key actors of pulmonary fibrogenesis in this disease through their fibrinolytic capacities and enhancing effects on fibroblasts migration. Their serial assessment during the follow-up and their analysis in relation with the development of IPF complications and outcome would help us to evaluate their potential value of biomarkers of disease severity.
References
Raghu, G., Rochwerg, B., Zhang, Y., Garcia, C. A. C., Azuma, A., Behr, J., et al. (2015). An official ATS/ERS/JRS/ALAT clinical practice guideline: treatment of idiopathic pulmonary fibrosis. An update of the 2011 clinical practice guideline. American Journal of Respiratory and Critical Care Medicine, 192(2), e3–19.
Smadja, D. M., Mauge, L., Nunes, H., d’Audigier, C., Juvin, K., Borie, R., et al. (2013). Imbalance of circulating endothelial cells and progenitors in idiopathic pulmonary fibrosis. Angiogenesis, 16(1), 147–157.
Toshner, M., Voswinckel, R., Southwood, M., Al-Lamki, R., Howard, L. S. G., Marchesan, D., et al. (2009). Evidence of dysfunction of endothelial progenitors in pulmonary arterial hypertension. American Journal of Respiratory and Critical Care Medicine, 180(8), 780–787.
Malli, F., Koutsokera, A., Paraskeva, E., Zakynthinos, E., Papagianni, M., Makris, D., et al. (2013). Endothelial progenitor cells in the pathogenesis of idiopathic pulmonary fibrosis: an evolving concept. PloS One, 8(1), e53658.
Amabile, N., Guignabert, C., Montani, D., Yeghiazarians, Y., Boulanger, C. M., & Humbert, M. (2013). Cellular microparticles in the pathogenesis of pulmonary hypertension. The European Respiratory Journal, 42(1), 272–279.
Nieri, D., Neri, T., Petrini, S., Vagaggini, B., Paggiaro, P., & Celi, A. (2016). Cell-derived microparticles and the lung. European Respiratory Review: an Official Journal of European Respiratory Society, 25(141), 266–277.
Bakouboula, B., Morel, O., Faure, A., Zobairi, F., Jesel, L., Trinh, A., et al. (2008). Procoagulant membrane microparticles correlate with the severity of pulmonary arterial hypertension. American Journal of Respiratory and Critical Care Medicine, 177(5), 536–543.
Amabile, N., Heiss, C., Real, W. M., Minasi, P., McGlothlin, D., Rame, E. J., et al. (2008). Circulating endothelial microparticle levels predict hemodynamic severity of pulmonary hypertension. American Journal of Respiratory and Critical Care Medicine, 177(11), 1268–1275.
Iversen, L. V., Ullman, S., Østergaard, O., Nielsen, C. T., Halberg, P., Karlsmark, T., et al. (2015). Cross-sectional study of soluble selectins, fractions of circulating microparticles and their relationship to lung and skin involvement in systemic sclerosis. BMC Musculoskeletal Disorders, 16, 191.
Nomura, S., Inami, N., Ozaki, Y., Kagawa, H., & Fukuhara, S. (2008). Significance of microparticles in progressive systemic sclerosis with interstitial pneumonia. Platelets, 19(3), 192–198.
Ratajczak, J., Wysoczynski, M., Hayek, F., Janowska-Wieczorek, A., & Ratajczak, M. Z. (2006). Membrane-derived microvesicles: important and underappreciated mediators of cell-to-cell communication. Leukemia, 20(9), 1487–1495.
Ratajczak, M. Z., & Ratajczak, J. (2016). Horizontal transfer of RNA and proteins between cells by extracellular microvesicles: 14 years later. Clinical and Translational Medicine, 5(1), 7.
Mauge, L., Sabatier, F., Boutouyrie, P., D’Audigier, C., Peyrard, S., Bozec, E., et al. (2014). Forearm ischemia decreases endothelial colony-forming cell angiogenic potential. Cytotherapy, 16(2), 213–224.
Evrard, S. M., d’Audigier, C., Mauge, L., Israël-Biet, D., Guerin, C. L., Bieche, I., et al. (2012). The profibrotic cytokine transforming growth factor-β1 increases endothelial progenitor cell angiogenic properties. Journal of Thrombosis and Haemostasis, 10(4), 670–679.
Amabile, N., Cheng, S., Renard, J. M., Larson, M. G., Ghorbani, A., McCabe, E., et al. (2014). Association of circulating endothelial microparticles with cardiometabolic risk factors in the Framingham Heart Study. European Heart Journal, 35(42):2972–2979.
Empana, J.-P., Boulanger, C. M., Tafflet, M., Renard, J. M., Leroyer, A. S., Varenne, O., et al. (2015). Microparticles and sudden cardiac death due to coronary occlusion. The TIDE (Thrombus and Inflammation in Sudden Death) study. European Heart Journal. Acute Cardiovascular Care, 4(1), 28–36.
Poncelet, P., Robert, S., Bouriche, T., Bez, J., Lacroix, R., & Dignat-George, F. (2016). Standardized counting of circulating platelet microparticles using currently available flow cytometers and scatter-based triggering: forward or side scatter? Cytometry Part A: the Journal of the International Society for Analytical Cytology, 89(2), 148–158.
Yoder, M. C., Mead, L. E., Prater, D., Krier, T. R., Mroueh, K. N., Li, F., et al. (2007). Redefining endothelial progenitor cells via clonal analysis and hematopoietic stem/progenitor cell principals. Blood, 109(5), 1801–1809.
Silvestre, J. S., Smadja, D. M., & Levy, B. I. (2013). Postisch-emic revascularization: from cellular and molecular mechanisms to clinical applications. Physiological Reviews, 93, 1743–1802.
Sapet, C., Simoncini, S., Loriod, B., Puthier, D., Sampol, J., Nguyen, C., et al. (2006). Thrombin-induced endothelial microparticle generation: identification of a novel pathway involving ROCK-II activation by caspase-2. Blood, 108(6):1868–1876.
Smadja, D. M., Bièche, I., Silvestre, J.-S., Germain, S., Cornet, A., Laurendeau, I., et al. (2008). Bone morphogenetic proteins 2 and 4 are selectively expressed by late outgrowth endothelial progenitor cells and promote neoangiogenesis. Arteriosclerosis, Thrombosis, and Vascular Biology, 28(12), 2137–2143.
Smadja, D. M., Levy, M., Huang, L., Rossi, E., Blandinières, A., Israel-Biet, D., et al. (2015). Treprostinil indirectly regulates endothelial colony forming cell angiogenic properties by increasing VEGF-A produced by mesenchymal stem cells. Thrombosis and Haemostasis, 114(4), 735–747.
Sabatier, F., Roux, V., Anfosso, F., Camoin, L., Sampol, J., & Dignat-George, F. (2002). Interaction of endothelial microparticles with monocytic cells in vitro induces tissue factor-dependent procoagulant activity. Blood, 99(11):3962–3970.
Abid Hussein, M. N., Böing, A. N., Biró, E., Hoek, F. J., Vogel, G. M. T., Meuleman, D. G., et al. (2008). Phospholipid composition of in vitro endothelial microparticles and their in vivo thrombogenic properties. Thrombosis Research, 121(6), 865–871.
Lacroix, R., Plawinski, L., Robert, S., Doeuvre, L., Sabatier, F., Martinez de Lizarrondo, S., et al. (2012). Leukocyte- and endothelial-derived microparticles: a circulating source for fibrinolysis. Haematologica, 97(12), 1864–1872.
Crooks, M. G., & Hart, S. P. (2015). Coagulation and anticoagulation in idiopathic pulmonary fibrosis. European Respiratory Review: an Official Journal of European Respiratory Society, 24(137), 392–399.
Novelli, F., Neri, T., Tavanti, L., Armani, C., Noce, C., Falaschi, F., et al. (2014). Procoagulant, tissue factor-bearing microparticles in bronchoalveolar lavage of interstitial lung disease patients: an observational study. PloS One, 9(4), e95013.
Lin, C., Borensztajn, K., & Spek, C. A. (2017). Targeting coagulation factor receptors - protease-activated receptors in idiopathic pulmonary fibrosis. Journal of Thrombosis and Haemostasis, 15(4), 597–607.
Scotton, C. J., Krupiczojc, M. A., Königshoff, M., Mercer, P. F., Lee, Y. C. G., Kaminski, N., et al. (2009). Increased local expression of coagulation factor X contributes to the fibrotic response in human and murine lung injury. The Journal of Clinical Investigation, 119(9), 2550–2563.
Cointe, S., Judicone, C., Robert, S., Mooberry, M. J., Poncelet, P., Wauben, M., et al. (2017). Standardization of microparticle enumeration across different flow cytometry platforms: results of a multicenter collaborative workshop. Journal of Thrombosis and Haemostasis, 15(1), 187–193.
Renzoni, E. A., Walsh, D. A., Salmon, M., Wells, A. U., Sestini, P., Nicholson, A. G., et al. (2003). Interstitial vascularity in fibrosing alveolitis. American Journal of Respiratory and Critical Care Medicine, 167(3), 438–443.
Ratajczak, J., Kucia, M., Mierzejewska, K., Marlicz, W., Pietrzkowski, Z., Wojakowski, W., et al. (2013). Paracrine proangiopoietic effects of human umbilical cord blood-derived purified CD133 + cells–implications for stem cell therapies in regenerative medicine. Stem Cells and Development, 22(3), 422–430.
Wang, J., Chen, S., Ma, X., Cheng, C., Xiao, X., Chen, J., et al. (2013). Effects of endothelial progenitor cell-derived microvesicles on hypoxia/reoxygenation-induced endothelial dysfunction and apoptosis. Oxidative Medicine and Cellular Longevity, 2013, 572729.
Bitzer, M., Ben-Dov, I. Z., & Thum, T. (2012). Microparticles and microRNAs of endothelial progenitor cells ameliorate acute kidney injury. Kidney International, 82(4), 375–377.
Doeuvre, L., & Angles-Cano, E. (2009). Cell-derived microparticles unveil their fibrinolytic and proteolytic function. Medical Science, 25(1), 37–44.
Gobin, A. S., & West, J. L. (2002). Cell migration through defined, synthetic ECM analogs. FASEB Journal: an Official Publication Federation American Society Experimental Biology, 16(7), 751–753.
Warejcka, D. J., Narayan, M., & Twining, S. S. (2011). Maspin increases extracellular plasminogen activator activity associated with corneal fibroblasts and myofibroblasts. Experimental Eye Research, 93(5), 618–627.
Strieter, R. M., Keeley, E. C., Hughes, M. A., Burdick, M. D., & Mehrad, B. (2009). The role of circulating mesenchymal progenitor cells (fibrocytes) in the pathogenesis of pulmonary fibrosis. Journal of Leukocyte Biology, 86(5), 1111–1118.
Ruehl, M., Muche, M., Freise, C., Erben, U., Neumann, U., Schuppan, D., et al. (2011). Hydroxyproline-containing collagen analogs trigger the release and activation of collagen-sequestered proMMP-2 by competition with prodomain-derived peptide P33-42. Fibrogenesis Tissue Repair, 4(1), 1.
Phillips, R. J., Burdick, M. D., Hong, K., Lutz, M. A., Murray, L. A., Xue, Y. Y., et al. (2004). Circulating fibrocytes traffic to the lungs in response to CXCL12 and mediate fibrosis. The Journal of Clinical Investigation, 114(3), 438–446.
Moore, B. B., Murray, L., Das, A., Wilke, C. A., Herrygers, A. B., & Toews, G. B. (2006). The role of CCL12 in the recruitment of fibrocytes and lung fibrosis. American Journal of Respiratory Cell and Molecular Biology, 35(2), 175–181.
Smadja, D. M., Dorfmüller, P., Guerin, C. L., Bieche, I., Badoual, C., Boscolo, E., et al. (2014). Cooperation between human fibrocytes and endothelial colony-forming cells increases angiogenesis via the CXCR4 pathway. Thrombosis and Haemostasis, 112(5), 1002–1013.
Smadja, D. M., Bièche, I., Emmerich, J., Aiach, M., & Gaussem, P. (2006). PAR-1 activation has different effects on the angiogenic activity of endothelial progenitor cells derived from human adult and cord blood. Journal of Thrombosis and Haemostasis, 4(12), 2729–2731.
Ingram, D. A., Mead, L. E., Tanaka, H., Meade, V., Fenoglio, A., Mortell, K., et al. (2004). Identification of a novel hierarchy of endothelial progenitor cells using human peripheral and umbilical cord blood. Blood, 104(9):2752–2760.
Nadaud, S., Poirier, O., Girerd, B., Blanc, C., Montani, D., Eyries, M., et al. (2013). Small platelet microparticle levels are increased in pulmonary arterial hypertension. European Journal of Clinical Investigation, 43(1), 64–71.
Simoncini, S., Chateau, A.-L., Robert, S., Todorova, D., Yzydorzick, C., Lacroix, R., et al. (2017). Biogenesis of pro-senescent microparticles by endothelial colony forming cells from premature neonates is driven by SIRT1-dependent epigenetic regulation of MKK6. Scientific Reports, 7(1), 8277.
Acknowledgements
This work was supported by grants of Chancellerie des Universities (Legs Poix) and Coeny-maeva charitable foundation.
Nour C. Bacha is supported by a grant from « Fonds de dotation pour la Recherche en Santé Respiratoire ».
We thank the technicians and engineers of hematology department of Georges Pompidou hospital, in particular Sebastien Bertil, Alexandre Kisaoglou, Florence Desvard, Nadège Ochat and Yann Burnel.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Declaration of Interest
Authors declare no conflict of interest related to this work.
Rights and permissions
About this article
Cite this article
Bacha, N.C., Blandinieres, A., Rossi, E. et al. Endothelial Microparticles are Associated to Pathogenesis of Idiopathic Pulmonary Fibrosis. Stem Cell Rev and Rep 14, 223–235 (2018). https://doi.org/10.1007/s12015-017-9778-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-017-9778-5