Abstract
Cholesterol oxidation product, 3β-hydroxy-5-oxo-5,6-secocholestan-6-al (cholesterol 5,6-secosterol, ChSeco or Atheronal-A), formed at inflammatory sites, has been shown to promote monocyte differentiation into macrophages and cause elevated expression of macrophage scavenger receptors. Since inflammation is a key event at all stages of atherosclerotic plaque formation, the pro-inflammatory actions of ChSeco in human THP-1 monocytes and mouse J774 macrophages were investigated in the present study by employing ELISA, qRT-PCR, and functional assays. An increase in the secretion of interleukin-8 and platelet-derived growth factor (PDGF) isoform AA and, to a limited extent, PDGF isoform BB was observed into the culture medium of THP-1 monocytes exposed to ChSeco. However, no changes were seen in the secretion of tumor necrosis factor-alpha. In J774 macrophages treated with ChSeco, there was an upregulation of gene expression of several pro-inflammatory cytokines and their receptors. Concomitantly, there was down-regulation of gene expression of interleukin-1ß, interleukin-10, and lymphotoxin-beta. An increase in the release of interleukin-18 and chemokine (C–C motif) ligand-20 from J774 macrophages (which corroborated well with their gene expression profiles) and increased binding of THP-1 monocytes to ChSeco-exposed human aortic endothelial cells were observed. The results of the present study, for the first time, demonstrate the pro-inflammatory action of ChSeco and suggest the underlying pro-atherogenic mechanisms. These could be mediated through enhanced monocyte recruitment into the sub-endothelial space and subsequent proliferation of smooth muscle cells under the influence of monocyte-derived PDGF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cholesterol secoaldehyde (3β-hydroxy-5-oxo-5,6-secocholestan-6-al, ChSeco or Atheronal-A; Fig. 1) is an oxysterol known to be formed in reactions of ozone with cholesterol [1, 2] and when cholesterol-5α-hydroperoxide undergoes Hock cleavage [3]. Because of its wide-spread occurrence in the arterial plaque [4] and other areas of inflammation [5] and because of its cytotoxic effects in various mammalian cell types including immune cells [6,7,8,9,10,11,12], ChSeco and its aldolized product, 3β-hydroxy-5β-hydroxy-B-norcholestan-6β-carboxaldehyde (Atheronal-B; Fig. 1), have raised much concern and interest [13,14,15,16,17,18,19,20]. While early studies focused largely on ozone-specific oxidation of cholesterol to be the primary source of ChSeco [1, 4, 7, 21,22,23], recent studies suggest that this oxysterol is formed in vivo mainly as a result of singlet oxygen-mediated oxidation of cholesterol and the subsequent Hock cleavage of the product cholesterol-5α-hydroperoxide [3, 12, 24, 25].
Possible routes for the formation of ChSeco (Atheronal-A) and Atheronal-B (aldolized ChSeco) in vivo: A pathway involving direct reactions of ozone in the breathing air with cholesterol in the epithelial lung lining fluids (tracheobronchial surface fluid and alveolar and small airway lining fluid) at the air-lung interface; and B pathway involving singlet oxygen-mediated oxidations of cholesterol at inflammatory sites in most extrapulmonary tissues and organs
We have previously shown that ChSeco is cytotoxic to mouse J774 macrophages and that the cell death at low concentrations of ChSeco conforms to several characteristic features of apoptosis mediated by the mitochondrial pathway but not involving the reactive oxygen species (ROS) as mediators [6]. Based on these observations, and the fact that Atheronal-B has been shown to be pro-atherogenic in that it promotes maturation of monocytes to macrophages and causes upregulation of endothelial adhesion molecules and macrophage scavenger receptor, a suggestion has been put forth that ChSeco formed in vivo contributes to the initiation, progression, and culmination of atherosclerotic plaques as these processes are critically dependent on macrophage apoptosis [6, 20]. In view of these reports, we, in the present study, investigated the inflammatory actions of ChSeco in vitro by determining the inflammatory cytokine release and gene expression in human THP-1 monocytes and mouse J774 macrophages using ELISA and RT-PCR. Additionally, we examined the adhesion of THP-1 monocytes to human aortic endothelial cells (HAECs) previously exposed to sub-cytotoxic concentrations of ChSeco. The results demonstrated the inflammatory potential of ChSeco and a possible pro-atherogenic role(s) for this unique oxysterol. It is suggested that ChSeco contributes to atherogenesis by enhancing the recruitment of monocytes into the sub-endothelial space and by facilitating the proliferation of smooth muscle cells through increased production of monocyte-derived PDGF.
Materials and methods
Chemicals, cell lines, and reagents
All chemicals were procured from Sigma-Aldrich (St. Louis, MO) unless otherwise specified. Fetal bovine serum (FBS) was from Atlanta Biologicals (Lawrenceville, GA); BCA protein assay kit from Pierce Biotechnology (Rockford, IL); 5-(and-6)-chloromethyl-2,7-dichloro-dihydrofluorescein (CMH2DCFDA) from Invitrogen (Carlsbad, CA); CellTiter 96 Aqueous One (MTS/PMS) reagent for measurement of cell viability from Promega (Madison, WI); ELISA kits specific for human monocyte chemo-attractant protein-1 (MCP-1) from R&D Systems (Minneapolis, MN), tumor necrosis factor-alpha (TNF-α) from BD Bioscience (San Jose, CA); and chemokine (C–C motif) ligand-20 (CCL-20), interleukin-8 (IL-8), and interleukin-18 (IL-18) from MBL (Nagoya, Japan); RNeasy mini kit from Qiagen (Valencia, CA); cytoselect leukocyte-endothelium adhesion assay kit from Cell Biolabs (San Diego, CA); and cDNA synthesis kit from SuperArray (Frederick, MD). Culture plates (24- and 96-well) and 25 cm2 culture flasks were purchased from Corning (Acton, MA). Mouse J774 macrophages, human acute monocytic leukemia THP-1 cells (THP-1 monocytes), and human aortic endothelial cells (HAECs) were purchased from ATCC (Rockville, MD).
Cholesterol secoaldehyde was synthesized by ozonation of cholesterol in mixed solvents of methanol and dichloromethane (1/1, v/v) as described in previous publications [9, 26]. Stock solutions of ChSeco were prepared in DMSO at a concentration of 20 mM and stored in small aliquots at −80 °C until use.
Cell culture
Mouse J774 macrophages were maintained in DMEM containing 4 mM L-glutamine,1.5 g/L sodium bicarbonate, 4.5 g/L glucose, and 10% FBS. THP-1 monocytes were cultured in RPMI-1640 supplemented with 0.05 mM 2-mercaptoethanol and 10% FBS. HAECs were cultured in Ham’s F12K medium supplemented with 2 mM L-glutamine, 1.5 g/L sodium bicarbonate, 0.1 mg/mL heparin, 0.03 mg/mL ECGS and 10% (v/v) FBS. Cell lines were maintained at 37 ± 0.5 °C in 5% CO2/95% humidified air. All treatments, including exposure to ChSeco, were performed in a medium that contained a low serum supplement (i.e., 2% FBS).
Cell viability and proliferation
THP-1 monocytes, seeded in 24-well culture plates (3 × 104 cells/well; volume: 500 μL), were exposed to ChSeco or un-oxidized cholesterol (control) for 24 h. At the end of the incubation period, the MTS/PMS reagent (10 μL) was added to each well and incubated for 3 h [8, 11]. The extent of MTS reduction was then measured at 490 nm using a BioTek EL 800 microplate reader (Winooski, VT). Background absorbance from wells that contained cholesterol or ChSeco in DMEM but without cells was subtracted. THP-1 monocytes exposed to vehicle (untreated control) were set to 100% and changes in viability of THP-1 monocytes exposed to ChSeco or cholesterol were measured relative to the corresponding untreated controls.
Measurement of intracellular ROS
Intracellular ROS was measured based on the hydrolysis 5-(and-6)-chloromethyl-2,7-dichlorodihydrofluorescein diacetate (CMH2DCFDA) and subsequent oxidation of 5-(and-6)-chloromethyl-2,7-dichlorodihydrofluorescein (CMH2DCF) to a fluorescent compound, 5-(and-6)-chloromethyl-2,7-dichlorofluorescein (CMDCF). THP-1 monocytes (1 × 105/well) in 24-well plates were incubated with 10 µM CMH2DCFDA in Krebs-Ringer-HEPES (KRH) buffer at 37 ˚C for 30 min. Following a brief wash, THP-1 monocytes were exposed to ChSeco (0–100 µM) in KRH buffer. The time-course of appearance of CMDCF was measured at excitation and emission wavelengths of 485 and 538 nm (respectively) using a SpectraMax Gemini EM fluorescence microplate reader (Molecular Devices; Sunnyvale, CA). THP-1 monocytes treated with vehicle, but no ChSeco were used as the negative control, and menadione (25 or 50 µM)-exposed cells served as the positive control.
Quantification of cytokine (protein) expression
Human THP-1 monocytes in 24-well plates (1 × 105 cells/well) were cultured in the absence or presence of ChSeco (30 μM) or LPS (10 ng/mL; positive control) for up to 24 h. Cell-free supernatants were collected at 2, 6, 18, and 24 h and stored at −70 °C until assayed. The concentrations of MCP-1, TNF-α, IL-8, PDGF (AA and BB isoforms) in culture supernatants were quantified using commercially available ELISA kits. In each case, a standard curve was established using known amounts of authentic cytokines. The ELISA kits used were specific for the measurement of human (natural as well as recombinant) cytokines with little or no cross-reactivity with cytokines (or growth factors) from non-human species.
Mouse J774 macrophages (1 × 106/well) in 24-well plates were cultured in the absence or presence of ChSeco (10–15 μM) or LPS (50 ng/mL; positive control) for 24 h. The concentrations of IL-18 and CCL-20 in the cell-free supernatants were quantified using commercially available, mouse-specific ELISA kits.
Quantification of cytokine and their receptor (gene) expression
Mouse J774 macrophages, grown in 25 cm2 flasks, were exposed to 0 (control) or 15 µM ChSeco for 4, 16, and 24 h. The total RNA was isolated using the RNeasy mini kit (Qiagen). The quality of RNA was ascertained by formaldehyde-denaturing gel electrophoresis (1.2%) and UV absorbance at 260 and 280 nm. Approximately 2 μg of total RNA was reverse transcribed with random hexamer primers using the first-strand synthesis kit (SuperArray). The cDNA (10-fold diluted) was used in a two-step RT-PCR (quantitative) assay, with a single-reporter measurement using the ABI-Prism SDS 7900 HT Fast RT-PCR system (Applied Biosystems; Foster City, CA). The RT² Profiler PCR array for mouse inflammatory cytokine and receptors (SuperArray) contained the necessary primer pairs for the amplification. The RT-PCR methodology used here allows simultaneous detection of 86 genes related to inflammation along with five housekeeping genes. The threshold cycle (Ct) for each well was calculated using the instrument’s software (SDS version 2.1). The resulting threshold cycle values for all wells were analyzed using the excel spreadsheet tool provided by the manufacturer. Values were expressed as fold change in expression relative to the untreated control group(s).
Monocyte-endothelial cell adhesion assay
Adhesion of THP-1 monocytes to HAECs, previously exposed to ChSeco, was measured using a cytoselect leukocyte-endothelium adhesion assay kit. For this, HAECs grown to confluence in gelatin-coated 96-well plates were exposed to either ChSeco (0–15 µM) or IL-8 (50 ng/mL; positive control) for 4 h. The medium was removed after the exposure period, and the HAECs were washed twice with PBS. A suspension of THP-1 monocytes (5 × 105) labeled with leuko tracker in a final volume of 200 μL was added to each well and incubated for 1 h at 37 °C. Non-adherent THP-1 monocytes were removed by washing (thrice) with buffer. The THP-1 monocytes adhered to HAECs were lysed and the fluorescence was measured at excitation and emission wavelengths of 480 and 520 nm, respectively, using a SpectraMax Gemini EM spectrofluorimeter. The fluorescence intensity of the control HAECs that were not exposed to ChSeco was set at 1 and the values of fluorescence associated with ChSeco exposed HAECs were expressed relative to this control.
Statistical analysis
Data are presented as ±SD of at least three independent experiments performed in duplicates. Data analysis was done using GraphPad Prism software and comparison was made between untreated and ChSeco-treated cells as well as by means of unpaired Student’s t-test and their significance was established by ANOVA. A difference of p < 0.05 was considered statistically significant.
Results
ChSeco induces upregulation of IL-8 and PDGF-AA but not TNF-α, MCP-1, and PDGF-BB in THP-1 monocytes
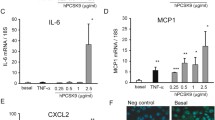
When THP-1 monocytes were exposed to ChSeco (30 µM), there was a time-dependent increase in the level of IL-8 in the culture medium (Fig. 2A). The concentration of IL-8 in the culture medium of cells exposed to ChSeco for 24 h was typically 176 ± 8 pg/mL. This value of IL-8 was about one-third of what was observed in culture supernatants of THP-1 monocytes exposed to LPS (10 ng/mL) for 24 h (539 ± 28 pg/mL; positive control) (Fig. 2B). In all these cases, control THP-1 monocytes that were not exposed to ChSeco showed negligible release of IL8 into the medium.
Secretion of IL-8 and TNF-α by THP-1 monocytes exposed to ChSeco. THP-1 monocytes (1 × 105/well) in 24-well plates were treated with either ChSeco (5–30 µM) or LPS (10 ng/mL; positive control). Cell-free supernatants were collected at 24-h time period after ChSeco or LPS treatment. IL-8 (A, B) and TNF-α (C) were determined using commercially available ELISA kits as described in the Methods section. Results are expressed as pg of IL-8 (or TNF-α) released per mL medium. Values are the average of three independent experiments performed in duplicates. The comparison was made between LPS-treated and ChSeco-exposed cells. *p < 0.05 indicates significance with respect to the untreated controls
Human THP-1 monocytes, with or without exposure to ChSeco (30 μM) for periods up to 24 h, did not show any evidence of TNF-α release into the culture medium (Fig. 2C). While it was observed that the concentration of TNF-α in these cultures was below the detection limit, we further confirmed the validity of the ELISA assay by exposing THP-1 monocytes to LPS (10 ng/mL; positive control). It was observed that, within 4 h of exposure to LPS, there was a substantial release of TNF-α into the medium (1155 ± 128 pg/mL) by THP-1 monocytes, the level of which declined thereafter (Fig. 2C).
There was a substantial increase in the level of PDGF-AA in the culture medium of THP-1 monocytes that were exposed to ChSeco (30 µM) (79 ± 25.3 pg/mL) when compared to vehicle-only-exposed THP-1 monocytes (18 ± 5.6 pg/mL) (Fig. 3A). Nevertheless, we did not observe significant differences in the release of PDGF-BB dimmer into the culture medium of THP-1 monocytes that were exposed to ChSeco (9 ± 2.6 pg/mL) as against the respective controls (5 ± 3.6 pg/mL) (Fig. 3B). We did not detect MCP-1 in the culture supernatants of THP-1 monocytes that were exposed to ChSeco (30 μM) or LPS (10 ng/mL) for periods up to 24 h.
Secretion of PDGF-AA and PDGF-BB by THP-1 monocytes exposed to ChSeco. THP-1 monocytes (1 × 105 /well) in 24-well plates were treated with ChSeco (30 µM) for 24 h. A PDGF-AA and B PDGF-BB in the culture medium were quantitatively determined using commercially available human ELISA kits as described in the Methods section. Values are the average of three independent experiments in duplicate wells. *P < 0.001 is significant for ChSeco treatment against the untreated controls
ChSeco reduces the viability of THP-1 monocytes
Exposure of THP-1 monocytes to ChSeco for 24 h resulted in a significant decrease in cell viability as determined by the extent of reduction of MTS to MTS formazan by viable cells in a PMS-assisted reaction (Fig. 4). The extent of ChSeco-induced loss of cell viability was found to be dose-dependent with an IC50 value of 16 ± 2.2 μM. In comparison, exposure of THP-1 monocytes to un-oxidized cholesterol did not result in a significant change in the cell viability or proliferation (Fig. 4).
Loss of viability in THP-1 monocytes exposed to ChSeco. THP-1 monocytes (3 × 104/well) in 24-well culture plates at 70% confluence were exposed to varying concentrations of ChSeco and un-oxidized cholesterol for 24 h. At the end of the incubation period, cell viability was assessed using MTS/PMS reagent (Cell Titer 96 Aqueous One reagent) as described in the Methods section. The viability of cells exposed to vehicle (untreated control) was set to 100% and the percentage viability in ChSeco-treated cultures was expressed relative to the controls. Values are average of quadruplicate measurements from three independent experiments
ChSeco does not induce the generation of intracellular peroxides in THP-1 monocytes
THP-1 monocytes exposed to ChSeco (0–30 µM) did not generate ROS over a period of 8 h (Fig. 5). In comparison, menadione (50 μM), a strong inducer of ROS, caused THP-1 monocytes to generate intracellular peroxides. Practically no DCF fluorescence was observed in control cultures that contained ChSeco but devoid of THP-1 monocytes.
Generation of intracellular reactive oxygen species in human THP-1 monocytes exposed to ChSeco. THP-1 monocytes were exposed to ChSeco (30 µM) or menadione (50 µM; positive control) and the generation of ROS was measured by uptake, hydrolysis, and subsequent oxidation of CMH2DCFDA to CMDCF. ** p < 0.01 versus untreated controls. Data presented are mean ± SD of three independent experiments
ChSeco upregulates inflammatory gene expression in mouse J774 macrophages
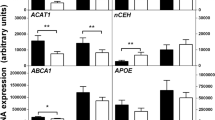
To confirm the inflammatory potential of ChSeco, we performed a quantitative real-time PCR array analysis of genes associated with inflammation. The profiling of gene expression in mouse J774 macrophages was performed at 4, 16, and 24 h following exposure to ChSeco (Table 1). It was found that, at 4 h, there was significant upregulation of CCL8, CCL20, CCR1, and CCR8 (p < 0.05; a change in gene expression of ≥2-fold relative to vehicle control was considered significant). At 16 h of ChSeco treatment, there were 28 genes that were found to be differentially regulated (p < 0.05 for those with fold change of ≥+2 or ≤−2). Out of these 28 genes, 25 genes (BCL6, CASP1, CCL1, CCL8, CCL11, CCL17, CCL20, CCL25, CCR1, CCR2, CCR3, CCR8, CXCL12, IL16, IL18, IL1R1, IL1R2, IL2RG, IL3R, IL6ST, LTA, SPP1, TGFB1, TNFRSF1A, and TOLLIP) were upregulated and 3 genes (IL1B, IL10, and LTA) downregulated relative to the untreated controls. At 24 h of treatment with ChSeco, there were18 genes that were found to be differentially regulated (p < 0.05 for those with fold change of ≥+2 or ≤−2); out of 18 genes, 15 genes (BLR1, CASP1, CCL8, CCL17, CCL20, CCR1, CCR2, CCR3, IL13, IL16, IL18, IL1R1, ILR2RG, LTA, and TOLLIP) were upregulated and 3 genes (IL1B, IL10, and LTB) downregulated relative to the vehicle control. Among the various genes upregulated, IL18 and CCL20 were the two most highly expressed genes at 16 h with an overall fold increase of 4.3 and 8.0, respectively (i.e., relative to the untreated, vehicle only-exposed controls).
ChSeco induces the release of IL-18 but not CCL-20 in J774 macrophages
Further, to confirm the results of gene expression at protein expression/synthesis level, we measured by ELISA the concentrations of IL-18 and CCL-20 in the culture supernatants of J774 macrophages that were exposed to ChSeco (0, 10, or 15 μM) or LPS (10 ng/mL; positive control) for 24 h. The concentration of IL-18 in culture supernatants of J774 macrophages that were not exposed to ChSeco was 68 ± 0.2 pg/ mL (Fig. 6A). This value was found to be much higher in culture supernatants of J774 macrophages exposed to either 10 (137 ± 24.5 pg/mL) or 15 μM ChSeco (214 ± 22.4 pg/mL) (Fig. 6A). As anticipated, exposure to LPS showed the highest level of expression of IL-18 (270 ± 25.0 pg/mL). In all these assays, we did not detect any significant release of CCL-20 into the culture medium (Fig. 6B).
Secretion of A IL-18 and B CCL-20 by mouse J774 macrophages exposed to ChSeco. Macrophages (1 × 106 /well) in 24-well plates were exposed to ChSeco (0, 10, or 15 μM) or LPS (50 ng/mL; positive control) for 0–24 h. IL-18 in the culture medium was determined at 24 h following the incubation with ChSeco (0–15 μM) or LPS (50 ng/mL). CCL20 in the culture medium was determined at 0, 4, 16, and 24 h following the incubation with 15 μM ChSeco. Both IL-18 and CCL-20 were determined using commercially available mouse-specific ELISA kits as described in the Methods section. Values are mean ± SD of three independent experiments. *p < 0.05 indicates significance with respect to the untreated control
Pretreatment of HAECs with ChSeco facilitate adhesion to THP-1 monocytes
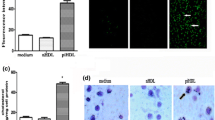
We examined the possibility that ChSeco induces the expression of cell adhesion molecules on HAECs and thereby facilitates the binding of THP-1 monocytes. For this, we exposed HAECs to various low concentrations of ChSeco for 2 h, and thereafter ChSeco-containing medium was removed and the HAECs were co-incubated with THP-1 monocytes for 4 h. Compared to the untreated HAECs, there was 2.0 (±0.33)-fold increase in the adhesion of THP-1 monocytes to HAECs previously exposed to ChSeco (15 µM) (Fig. 7). HAECs exposed to IL8 (50 ng/mL; positive control) increase their adhesion to THP-1 monocytes by 5.3 (±1.2)-fold.
Adhesion of human THP-1 monocytes to HAECs. HAECs were cultured in gelatin-coated 96-well cell culture plates for 24 h. At confluence, the cells were exposed to ChSeco (0 or 15 µM) and IL8 (50 ng/mL; positive control) for 4 h. The adhesion of leuko tracker dye-labeled THP-1 monocytes to HAECs was determined by a fluorescent spectrophotometer. *p < 0.05 versus untreated control. Values presented are mean ± SEM of three separate experiments
Discussion
According to the “response to injury” hypothesis, a loss or alteration(s) in the physiological function of the endothelium initiates the process of atherogenesis [27,28,29]. Accordingly, the adhesion of circulating monocytes to the vascular endothelium is often considered to be one of the earliest steps in this process [27, 30, 31]. Both endothelial cells and adherent monocytes are known to secrete pro-inflammatory cytokines which increase the expression of adhesion molecules and thereby facilitate binding and subsequent transmigration of circulating leukocytes into the sub-endothelial space. In this study, we show that human THP-1 monocytes when exposed to ChSeco, release IL-8 and PDGF-AA, but not TNF-α, in a time- and/or dose-dependent manner (Figs. 2 and 3). IL-8 is a chemo-attractant protein with known mitogenic and pro-inflammatory properties. Both PDGF isoforms AA and BB have been shown to elicit mitogenic responses in smooth muscle cells present in the atherosclerotic plaques [32, 33]. The observation that ChSeco promotes the release of not only IL8 but also PDGF-AA and, to a limited extent, PDGF-BB by THP-1 monocytes, suggests that ChSeco could play a direct role in the induction of inflammation and an indirect role in smooth muscle cell proliferation. Several investigators have reported a similar pro-inflammatory potential with other oxysterols that are present in oxidized LDL [34,35,36,37].
The pro-inflammatory potential of ChSeco was further confirmed by studies of protein and gene expression in mouse J774 macrophages. Unlike THP-1 monocytes, J774 macrophages exposed to ChSeco had increased release of IL-18 and CCL-20, the latter being known as macrophage inhibitory protein-3-alpha (MIP-3-α). Both IL-18 and CCL-20 are known for their chemo-attractant properties and recruit immune cells to the site of inflammation [38,39,40]. An increased expression of IL-18 (protein) alone was suggested to be a good predictor of cardiovascular risk [41, 42]. While this is the case, in the present study, we show that IL10 (gene expression) was downregulated (Table 1). IL-10 is an anti-inflammatory cytokine [43], its lowered gene expression, as observed by us, may result in lowered protein expression. The combined effect of increased IL-18 expression and lowered IL-10 expression could therefore be potentially detrimental.
The gene expression studies using RT-PCR (Table 1) are corroborated by protein expression of pro-inflammatory cytokines and their receptors (Figs. 2, 3, and 6). Of particular interest in the present work is the increased expression of the IL1R1 gene. It has been shown that in the IL1R1 knockout mouse which has lowered expression of the corresponding receptor protein, there was evidence of reduced atherosclerotic plaque formation [44, 45]. Although we do not have data on IL1R1, by analogy it is possible that increased expression of IL1R1 by ChSeco may promote atherosclerotic plaque formation.
Caspase -1 which is responsible for the maturation and release of IL-1β and IL-18 in the inflammasome pathway [46, 47] was found to be over-expressed at the gene level in ChSeco-treated J774 macrophages. This suggests the possibility of inflammasome signaling, which, again, is in agreement with increased expression of IL18 in ChSeco-treated J774 macrophages.
The reasons for an apparent lack of expression of TNF-α in ChSeco-exposed monocytes are not clear. TNF-α is a known inducer of adhesion molecules and is considered to be a marker of cardiovascular events [48, 49]. In many cell types, under conditions of oxidative stress, TNF-α has been shown to be expressed through activation of the NF-kB pathway [50, 51]. In the present study, THP-1 monocytes exposed to ChSeco failed to induce the production of intracellular ROS and this could be a reason for the lack of TNF-α expression.
In studies, where THP-1 monocytes were co-incubated with HAECs previously exposed to a sub-cytotoxic level of ChSeco, there was evidence of increased cell-to-cell adhesion (Fig. 7). This raises the possibility that ChSeco induces the expression of adhesion molecules in HAECs which act as ligands for the binding of THP-1 monocytes. The increased expression of adhesion molecules could result from the direct action of ChSeco on HAECs. Alternatively, it is possible that ChSeco induces the secretion of pro-inflammatory cytokines, and these, in turn, act on HACEs causing increased expression of adhesion molecules.
The concentration of ChSeco in the human atheromatous plaque was found to be as high as 60 μM [4, 9]. This value is 2- to 3-fold higher than the IC50 values of ChSeco observed in immune and non-immune cell types [6, 52]. Apart from being cytotoxic to monocytes and macrophages, ChSeco at sub-cytotoxic concentrations is a potent inducer of pro-inflammatory cytokines and adhesion molecules. These attributes make ChSeco or any other oxysterol as an important contributor to early as well as late events in atherosclerotic plaque formation.
In conclusion, the present study, for the first time, demonstrates that low, biologically relevant concentrations of ChSeco and, by inference its aldolized product, Atheronal-B, can up-regulate the gene as well as protein expression profiles of several inflammatory cytokines in human THP-1 monocytes and mouse J774 macrophages. Together with the fact ChSeco is cytotoxic monocytes and macrophages, the increased adhesion of THP-1 monocytes to HAECs previously exposed to sub-cytotoxic levels of ChSeco, suggests that this unique oxysterol may have significant roles to play in early as well as late stages of atherosclerosis.
Abbreviations
- Atheronal-B:
-
3-hydroxy-5-hydroxy-B-norcholestan-6-carboxaldehyde
- BCL:
-
B-cell lymphoma protein
- ChSeco:
-
3β-hydroxy-5-oxo-5,6-secocholestan-6-al (cholesterol secoaldehyde or Atheronal-A)
- CASP:
-
caspase
- CCL:
-
chemokine (C–C motif) ligand
- CCR:
-
chemokine receptor
- CMH2DCFDA:
-
5-(and-6)-chloromethyl-2, 7-dichlorodihydro-fluorescein diacetate
- CMDCFDA:
-
5-(and-6)-chloromethyl-2,7-dichlorodihydro-fluorescein
- CMDCF:
-
5-(and-6)-chloromethyl-2,7-dichlorofluorescein
- CXCL:
-
chemokine (C–X–C motif) ligand
- HAECs:
-
human aortic endothelial cells
- IL:
-
interleukin
- LTA:
-
lymphotoxin-alpha
- MCP:
-
monocyte chemo-attractant protein
- PDGF:
-
platelet-derived growth factor
- ROS:
-
reactive oxygen species
- TNFα:
-
tumor necrosis factor-alpha
- TNFRSF:
-
tumor necrosis factor receptor superfamily
- TOLLIP:
-
toll interacting protein
References
Wang, K., Bermudez, E., & Pryor, W. A. (1993). The ozonation of cholesterol: separation and identification of 2,4-dinitrophenylhydrazine derivatization products of 3 beta-hydroxy-5-oxo-5,6-secocholestan-6-al. Steroids, 58, 225–229.
Smith, L. L., Ezell, E. L., & Jaworski, K. (1986). On the ozonization of cholesterol 3-acyl esters in protic media. Steroids, 61, 401–406.
Brinkhorst, J., Nara, S. J. & Pratt, D. A. (2008). Hock cleavage of cholesterol 5alpha-hydroperoxide: an ozone-free pathway to the cholesterol ozonolysis products identified in arterial plaque and brain tissue. Journal of the American Chemical Society, 130, 12224–12225.
Wentworth, P., Jr, Nieva, J., Takeuchi, C., Galve, R., Wentworth, A. D., Dilley, R. B., DeLaria, G. A., Saven, A., Babior, B. M., Janda, K. D., Eschenmoser, A., & Lerner, R.A. (2003). Evidence for ozone formation in human atherosclerotic arteries. Science, 302, 1053–1056.
Zhang, Q., Powers, E. T., Nieva, J., Huff, M. E., Dendle, M. A., Bieschke, J., Glabe, C. G., Eschenmoser, A., Wentworth, P., Lerner, R. A. & Kelly, J.W. (2004). Metabolite-initiated protein misfolding may trigger Alzheimer’s disease. Proceedings of the National Academy of Sciences of the United States of America, 101, 4752–4757.
Gao, X., Raghavamenon, A. C., D’Auvergne, O., & Uppu, R. M. (2009). Cholesterol secoaldehyde induces apoptosis in J774 macrophages via mitochondrial pathway but not involving reactive oxygen species as mediators. Biochemical and Biophysical Research Communications, 389, 382–387.
Pulfer, M. K. & Murphy, R. C. (2004). Formation of biologically active oxysterols during ozonolysis of cholesterol present in lung surfactant. The Journal of Biological Chemistry, 279, 26331–26338.
Raghavamenon, A. C., Gernapudi, R., Babu, S., D’Auvergne, O., Murthy, S. N., Kadowitz, P. J., & Uppu, R. M. (2009). Intracellular oxidative stress and cytotoxicity in rat primary cortical neurons exposed to cholesterol secoaldehyde. Biochemical and Biophysical Research Communications, 386, 170–174.
Sathishkumar, K., Haque, M., Perumal, T. E., Francis, J., & Uppu, R. M. (2005). A major ozonation product of cholesterol, 3beta-hydroxy-5-oxo-5,6-secocholestan-6-al, induces apoptosis in H9c2 cardiomyoblasts. FEBS Letters, 579, 6444–6450.
Sathishkumar, K., Xi, X., Martin, R., & Uppu, R. M. (2007). Cholesterol secoaldehyde, an ozonation product of cholesterol, induces amyloid aggregation and apoptosis in murine GT1-7 hypothalamic neurons. Journal of Alzheimer’s Disease, 11, 261–274.
Sathishkumar, K., Gao, X., Raghavamenon, A. C., Parinandi, N., Pryor, W. A., & Uppu, R. M. (2009). Cholesterol secoaldehyde induces apoptosis in H9c2 cardiomyoblasts through reactive oxygen species involving mitochondrial and death receptor pathways. Free Radical Biology & Medicine, 47, 548–558.
Raghavamenon, A. C., Gao, X., Atkins-Ball, D. S., Varikuti, S., Parinandi, N. L., & Uppu, R. M. (2020). ‘Ozone-specific’ oxysterols and neuronal cell signaling. In L. Berliner & N. Parinandi (Eds.), Measuring Oxidants and Oxidative Stress in Biological Systems. Biological Magnetic Resonance, 34, 109–122.
Bosco, D. A., Fowler, D. M., Zhang, Q., Nieva, J., Powers, E. T., Wentworth, P., Jr., Lerner, R. A., & Kelly, J. W. (2006). Elevated levels of oxidized cholesterol metabolites in Lewy body disease brains accelerate alpha-synuclein fibrilization. Nature Chemical Biology, 2, 249–253.
Cygan, N. K., Scheinost, J. C., Butters, T. D., & Wentworth, P., Jr, (2011). Adduction of cholesterol 5,6-secosterol aldehyde to membrane-bound myelin basic protein exposes an immunodominant epitope. Biochemistry, 50, 2092–2100.
Drahl, C. (2009). Probing for in-body ozone. Chemical & Engineering News, 87, 40–42.
Nieva, J., Shafton, A., Altobell, L.J., 3rd., Tripuraneni, S., Rogel, J. K., Wentworth, A. D., Lerner, R. A., & Wentworth, P., Jr. (2008). Lipid-derived aldehydes accelerate light chain amyloid and amorphous aggregation. Biochemistry, 47, 7695–7705.
Nieva, J., Song, B. D., Rogel, J. K., Kujawara, D., Altobel, L., Izharrudin, A., Boldt, G. E., Grover, R. K., Wentworth, A. D. & Wentworth, P., Jr. (2011). Cholesterol secosterol aldehydes induce amyloidogenesis and dysfunction of wild-type tumor protein p53. Chemistry & Biology, 18, 920–927.
Scheinost, J. C., Wang, H., Boldt, G. E., Offer, J. & Wentworth, P., Jr. (2008). Cholesterol secosterol-induced aggregation of methylated amyloid-beta peptides–insights into aldehyde-initiated fibrillization of amyloid-beta. Angewandte Chemie. International Edition in English, 47, 3919–3922.
Scheinost, J. C., Witter, D. P., Boldt, G. E., Offer, J. & Wentworth, P., Jr. (2009). Cholesterol secosterol adduction inhibits the misfolding of a mutant prion protein fragment that induces neurodegeneration. Angewandte Chemie. International Edition in English, 48, 9469–9472.
Takeuchi, C., Galve, R., Nieva, J., Witter, D. P., Wentworth, A. D., Troseth, R. P., Lerner, R. A., & Wentworth, P., Jr, (2006). Proatherogenic effects of the cholesterol ozonolysis products, atheronal-A and atheronal-B. Biochemistry, 45, 7162–7170.
Babior, B. M., Takeuchi, C., Ruedi, J., Gutierrez, A., & Wentworth, P., Jr. (2003). Investigating antibody-catalyzed ozone generation by human neutrophils. Proceedings of the National Academy of Sciences of the United States of America, 100, 3031–3034.
Pryor, W. A., Wang, K., & Bermudez, E. (1992). Cholesterol ozonation products as biomarkers for ozone exposure in rats. Biochemical and Biophysical Research Communications, 188, 618–623.
Wentworth, P., Jr., McDunn, J. E., Wentworth, A. D., Takeuchi, C., Nieva, J., Jones, T., Bautista, C., Ruedi, J. M., Gutierrez, A., Janda, K. D., Babior, B.M., Eschenmoser, A., & Lerner, R.A. (2002). Evidence for antibody-catalyzed ozone formation in bacterial killing and inflammation. Science, 298, 2195–2199.
Tomono, S., Miyoshi, N., Sato, K., Ohba, Y., & Ohshima, H. (2009). Formation of cholesterol ozonolysis products through an ozone-free mechanism mediated by the myeloperoxidase-H2O2-chloride system. Biochemical and Biophysical Research Communications, 383, 222–227.
Uemi, M., Ronsein, G. E., Miyamoto, S., Medeiros, M. H., & Di Mascio, P. (2009). Generation of cholesterol carboxyaldehyde by the reaction of singlet molecular oxygen [O2 (1Delta(g))] as well as ozone with cholesterol. Chemical Research in Toxicology, 22, 875–884.
Sathishkumar, K., Raghavamenon, A. C., Ganeshkumar, K., Telaprolu, R., Parinandi, N. L., & Uppu, R. M. (2010). Simultaneous analysis of expression of multiple redox- sensitive and apoptotic genes in hypothalamic neurons exposed to cholesterol secoaldehyde. Methods in Molecular Biology, 610, 263–284.
Kaperonis, E. A., Liapis, C. D., Kakisis, J. D., Dimitroulis, D., & Papavassiliou, V. G. (2006). Inflammation and atherosclerosis. European Journal of Vascular and Endovascular Surgery, 31, 386–393.
Ross, R.(1999). Atherosclerosis an inflammatory disease. American Heart Journal, 138, S419–420.
Ross, R.(1999). Atherosclerosis – An inflammatory disease. New England Journal of Medicine, 340, 115–126.
Fan, J. & Watanabe, T. (2003). Inflammatory reactions in the pathogenesis of atherosclerosis. Journal of Atherosclerosis and Thrombosis, 10, 63–71.
Libby, P., Ridker, P. M., & Maseri, A. (2002). Inflammation and atherosclerosis. Circulation, 105, 1135–1143.
Matsui, T. (1993). [PDGF system in vascular smooth muscle cell proliferation]. Nihon Rinsho. Japanese Journal of Clinical Medicine, 51, 1656–1662.
Myllarniemi, M., Calderon, L., Lemstrom, K., Buchdunger, E., & & Hayry, P. (1997). Inhibition of platelet-derived growth factor receptor tyrosine kinase inhibits vascular smooth muscle cell migration and proliferation. FASEB Journal, 11, 1119–1126.
Brown, A. J. & Jessup, W. (1999). Oxysterols and atherosclerosis. Atherosclerosis, 142, 1–28.
Dushkin, M., Schwartz, Y., Volsky, N., Musatov, M., Vereschagin, E., Ragino, J., Perminova, O., & Kozlov, V. (1998). Effects of oxysterols upon macrophage and lymphocyte functions in vitro. Prostaglandins & Other Lipid Mediators, 55, 219–236.
Liu, Y., Hulten, L. M., & Wiklund, O. (1997). Macrophages isolated from human atherosclerotic plaques produce IL-8, and oxysterols may have a regulatory function for IL-8 production. Arteriosclerosis, Thrombosis, and Vascular Biology, 17, 317–323.
Prunet, C., Montange, T., Vejux, A., Laubriet, A., Rohmer, J. F., Riedinger, J. M., Athias, A., Lemaire-Ewing, S., Neel, D., & Petit, J. M., Steinmetz, E., Brenot, R,, Gambert, P., Lizard, G. (2006). Multiplexed flow cytometric analyses of pro- and anti-inflammatory cytokines in the culture media of oxysterol-treated human monocytic cells and in the sera of atherosclerotic patients. Cytometry A, 69, 359–373.
Ohsuzu, F.(2004). The roles of cytokines, inflammation and immunity in vascular diseases. Journal of Atherosclerosis and Thrombosis, 11, 313–321.
Reape, T. J. & Groot, P. H. (1999). Expression and cellular localization of the CC chemokines PARC and ELC in human atherosclerotic plaques. Atherosclerosis, 147, 213–225.
Ruth, J. H., Park, C. C., Amin, M. A., Lesch, C., Marotte, H., Shahrara, S., & Koch, A. E. (2010). Interleukin-18 as an in vivo mediator of monocyte recruitment in rodent models of rheumatoid arthritis. Arthritis Research & Therapy, 12, R118.
Kretowski, A. & Kinalska, I. (2003). Serum levels of interleukin-18-a potential marker of cardiovascular death-could be determined by genetic predisposition. Circulation, 107, e206–207.
Blankenberg, S., Tiret, L., Bickel, C., Peetz, D., Cambien, F., Meyer, J., & Rupprecht, H. J. (2002). Interleukin-18 is a strong predictor of cardiovascular death in stable and unstable angina. Circulation, 106, 24–30.
Mallat, Z., Besnard, S., Duriez, M., Deleuze, V., Emmanuel, F., Bureau, M. F., Soubrier, F. & Esposito, B. (1999). Protective Role of Interleukin-10 in Atherosclerosis. Circulation Research, 85, 17–24.
Chamberlain, J., Evans, D., King, A., Dewberry, R., Dower, S., Crossman, D. & Francis, S. (2006). Interleukin-1beta and signaling of interleukin-1 in vascular wall and circulating cells modulates the extent of neointima formation in mice. The American Journal of Pathology, 168, 1396–1403.
Chamberlain, J., Francis, S., Brookes, Z., Shaw, G., Graham, D., Alp, N. J., Dower, S., & Crossman, D. C. (2009). Interleukin-1 regulates multiple atherogenic mechanisms in response to fat feeding. PLoS One, 4, e5073.
Mariathasan, S., Newton, K., Monack, D. M., Vucic, D., French, D. M., Lee, W. P., Roose-Girma, M., Erickson, S., & Dixit, V. M. (2004). Differential activation of the inflammasome by caspase-1 adaptors ASC and Ipaf. Nature, 430, 213–218.
Thornberry, N. A., Bull, H. G., Calaycay, J. R., Chapman, K. T., Howard, A. D., Kostura, M. J., Miller, D. K., Molineaux, S. M., Weidner, J. R. & Aunins, J. (1992). A novel heterodimeric cysteine protease is required for interleukin-1 beta processing in monocytes. Nature, 356, 768–774.
Collins, T., Read, M. A., Neish, A. S., Whitley, M. Z., Thanos, D. & Maniatis, T. (1995). Transcriptional regulation of endothelial cell adhesion molecules: NF-Kappa B and cytokine-inducible enhancers. FASEB Journal, 9, 899–909.
Ogiwara, F., Takahashi, M. & Ikeda, U. (2004). Inflammmatory markers and cytokines in cardiovascular diseases. Rinsho Byori. The Japanese Journal of Clinical Pathology, 52, 686–692.
Bowie, A. & O’Neill, L. A. (2000). Oxidative stress and nuclear factor-kappaB activation: a reassessment of the evidence in the light of recent discoveries. Biochemical Pharmacology, 59, 13–23.
Schutze, S., Potthoff, K., Machleidt, T., Berkovic, D., Wiegmann, K., & Kronke, M. (1992). TNF activates NF-kappa B by phosphatidylcholine-specific phospholipase C-induced “acidic” sphingomyelin breakdown. Cell, 71, 765–776.
Gao, X. (2009). Cytotoxicity and inflammatory potential of cholesterol secoaldehyde: a cell-based mechanistic study of a putative ozone-specific oxysterol with implications for cardiovascular disease. PhD. Dissertation. Southern University.
Acknowledgements
The authors acknowledge the support from the National Institutes of Health (NIH) through the National Institute of General Medical Science (NIGMS) Grant 5 P2O GM103424-17 and the US Department of Education (US DoE; Title III, HBGI Part B grant number P031B040030). Its contents are solely the responsibility of authors and do not represent the official views of NIH, NIGMS, or US DoE.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gao, X., Raghavamenon, A.C., Atkins-Ball, D.S. et al. Atherogenic oxoaldehyde of cholesterol induces innate immune response in monocytes and macrophages. Cell Biochem Biophys 79, 649–658 (2021). https://doi.org/10.1007/s12013-021-01004-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-021-01004-w