Abstract
Lead is a ubiquitous and neurotoxic heavy metal particularly harmful to children, who are more susceptible than adults to its toxic effects. The prevalence of lead poisoning and iron deficiency (ID) is high in socioeconomically vulnerable child populations, negatively affecting neurocognitive development in children. Although numerous studies have shown the association between blood lead levels (BLL) and ID, the issue remains controversial. Here, we aimed to identify the association between BLL and iron nutritional status in children. We conducted an analytical cross-sectional study of healthy children aged 1–6 y attending periodic health checks in primary healthcare units from La Plata and its surroundings, Buenos Aires, Argentina, between 2012 and 2017. We performed anthropometric evaluations and determined BLL, hemoglobin (Hb) and serum ferritin levels. Blood lead levels ≥ 5 µg/dL were defined as elevated BLL; ferritin levels < 12 ng/ml were considered ID; Hb levels < 11 g/dL (< 11.5 g/dL for children ≥ 5 y) were defined as anemia. Data were analysed using Mann Whitney test, Student´s t-test, chi-square test and logistic regression. The R package (v. 4.2.2.) was used for the statistical analysis of data. The sample included 392 children (mean age, 2.4 ± 1.4 y; 44.6% females). The prevalence of elevated BLL, ID and anemia was 8.7%, 26.3% and 31.8%, respectively. We found a significant association between elevated BLL and ID (odds ratio [OR], 95% confidence interval [CI]: 3.16 (1.50, 6.63)). The prevalence of elevated BLL was 16.2% and 5.8% in children with and without ID, respectively (p = 0.003). We also found association between elevated BLL and anemia (OR 95% CI: 3.03 (1.49, 6.29)). In conclusion, blood lead levels ≥ 5 µg/dL were significantly associated with ID and anemia in children aged 1–6 years.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lead is a toxic metal widely distributed in the Earth´s crust. Currently, children are exposed to lead through particles dispersed in the air, food, water, dust and soil [1]. Blood lead levels (BLL) have markedly decreased in the last 20 years, not only in population groups from developed countries but also from developing countries, including Argentina [2,3,4]. However, such BLL are still worrying, considering there is no safe blood lead threshold value below which lead has no adverse/toxic health effects [5].
Iron deficiency (ID) is the most common nutritional disorder worldwide and the main cause of anemia in infants, having a high prevalence in developing countries [6]. Lead poisoning and ID are highly prevalent in socioeconomically vulnerable child populations, negatively affecting the neurocognitive development of children [7,8,9,10,11]. Additionally, very low lead concentrations have been associated with negative developmental outcomes in children [12].
The epidemiological association between iron deficiency and lead poisoning has been examined by Wong in a review [13]. Divalent metal transporter 1 (DMT1) is one of the mechanisms believed to be involved in lead absorption in the small intestine, as well as the primary iron transporter. In the state of ID, the expression of DMT1 increases. This positive regulation during deficiency could explain the increased lead absorption by intestinal cells and the higher lead levels in individuals with ID [14].
Differences in BLL between children with and without ID living in contaminated environments are well-documented [15, 16]. However, while some studies observe such an association [17,18,19,20], others do not when lead concentrations are low [21, 22].
In order to gain insight into the issue of lead exposure and iron status in children from Argentina exposed to lowly contaminated environments, we analysed the relationship between BLL and iron nutritional status in children aged 1 to 6 years.
Materials and Methods
We conducted an analytical cross-sectional study of healthy children aged 1–6 y performing periodic health checks at the Health Observatory of the Instituto de Desarrollo e Investigaciones Pediátricas (IDIP), La Plata Children Hospital, and in primary healthcare units from La Plata and its surroundings, Buenos Aires, Argentina, from March 2012 to March 2017. Subjects who met the following criteria were excluded: children with chronic disease diagnosis, acute and/or infectious disease at the moment of the study, genetic syndrome, neurological background, moderate or acute malnutrition, or whose parents or tutors refused to participate in this study. We used convenience sampling. Sample size was calculated to detect a difference of 1.2 µg/dL between children with and without ID, assuming a 95% confidence interval (CI), an 80% power of the test, and a standard deviation (SD) of 2.4 µg/dL according to a previous study [3]. The estimated minimum sample size was 126 children (n = 63 each group). Nevertheless, considering that around 33% of children have ID, at least 192 children were included to ensure the number of children with ID.
Blood was collected by venipuncture to determine BLL, serum ferritin, C-reactive protein (CRP) and hemoglobin (Hb) levels. To measure BLL, heparanized blood was diluted (1:5) in 15% nitric acid (Merck, Argentina) and then centrifuged. The supernatant was analysed by atomic absorption spectroscopy (283.3 nm wave length) in a Varian Agilent 240Z AA 120 Programmable Sample Dispenser with Zeeman Effect background correction (Mulgrave, Victoria, Australia). The limits of detection (LOD) and quantification (LOQ) were 0.8 and 2.7 µg/dL, respectively. Blood lead levels ≥ 5.0 µg/dL were defined as elevated BLL [23]. Ferritin was determined by chemiluminescence in an Access Beckman Coulter analyser, considering ferritin levels < 12 ng/ml as ID. In case of elevated CRP (≥ 5 mg/L), the threshold value for ID was ferritin < 30 ng/mL [24]. Hemoglobin determinations were performed using a hematological counter (ABX Pentra 60, Montpellier, France). Values of Hb < 11 and < 11.5 g/dL for children < 5 and ≥ 5 years, respectively, were defined as anemia [25]. Iron deficiency anemia (IDA) was considered when Hb < 11 and < 11.5 g/dL for children < 5 and ≥ 5 years, respectively, and ferritin levels < 12 ng/ml.
Weight and height were assessed using standard methods. Weight was measured with a Tanita UM-061 digital electronic scale (0.1 g precision) (Tanita Corporation of America Inc., Illinois, USA) and height was measured with a portable SECA stadiometer (0.5 cm precision; SECA, United Kingdom). Weight-for-age (W/A), height-for-age (H/A) and body mass index (BMI) were determined and evaluated using the World Health Organization (WHO) Child Growth Standards [26].
Sources of lead exposure in children were collected using a questionnaire administered by trained staff. Sociodemographic information such as the child’s age and sex, the geographic location of the family house, family composition, parental employment status, parental level of education, housing conditions (building material, floor type, presence and/or location of a bathroom, number of rooms), access to water and health services were recorded. Based on these data, we developed the unmet basic needs (UBNs) indicator according to the methodology described by the National Statistics and Censuses Institute of Argentina (Instituto Nacional de Estadísticas y Censos, INDEC) [27]. Determinants of external lead exposure included presence of gas station (fuel distribution), car repair and/or paint shop, smithy, bus stops, high traffic roads, dirt roads, garbage dumps or polluted streams less than 100 m away.
We used the Kolmogorov-Smirnov test to analyse the normality of variables. Ferritin and BLL concentrations were expressed a geometric means (GM) and 95% CI considering their log normal distribution. In case of BLL < LOD, mean values were adjusted with the extrapolation method based on linear regression [28]. The rest of the variables were expressed as means ± standard deviations (SD) if they had a normal distribution, and as medians (P25; P75) in case of non-parametric data. Children were divided into two categories according to their age (< 2 and ≥ 2 y) taking into account the higher prevalence of ID in younger children and the increased lead exposure due to physiological, biological and behavioral patterns such as exploring the environment during the oral stage (hand-to-mouth), pica habits and frequent contact with the ground. Student´s t-test or Mann-Whitney test were used to compare quantitative variables by age and sex, and chi-square test was used to study the association between BLL ≥ 5 µg/dL and ID or anemia. Odds ratios (OR, 95% CI) were determined using logistic regression. The multivariate logistic regression model was used to adjust for confounding variables (sex and age of children < 2 y). The R package (v. 4.2.2) was used for the statistical analysis of data. In all cases, p < 0.05 was considered statistically significant.
Results
A total of 392 children (mean age, 2.4 ± 1.4 y; 44.6% female) were enrolled. The sociodemographic and anthropometric characteristics of the study sample are detailed in Table 1. From the total sample, 79.6% reported having at least one source of external lead exposure: living < 100 m from car repair/paint shops (38.1%), bus stops (35.2%), high traffic roads (31.6%), polluted streams (31%) and garbage dumps (26.2%).
Biochemical parameters are detailed in Table 2. From the total number of children, 8.7% had elevated BLL, 26.3% had ID and 31.8% were anemic.
Table 3 depicts BLL, ferritin and Hb mean values and the prevalence of elevated BLL, ID and anemia according to the age of children (< and ≥ 2 y). Whereas ferritin and Hb levels were lower in children < 2 y, the prevalence of elevated BLL, ID and anemia was higher as compared with children ≥ 2 y. Mean BLL levels did not differ between groups. The analysis of the variables by sex did not result in significant differences (data not shown).
Results of the comparison of ferritin and Hb according to BLL < or ≥ 5 µg/dL are shown in Fig. 1. Mean ferritin levels were lower in children with elevated BLL (95% CI): 12.41 ng/mL (9.37, 16.43) compared with BLL < 5 µg/dL (18.24 ng/mL (17.07, 19.48), p = 0.010). Likewise, median Hb values (reported as median (P25, P75)) were lower in children with elevated BLL (10.9 g/dL (10.6, 11.6) vs. 11.5 g/dL (10.9, 12.0); p = 0.001).
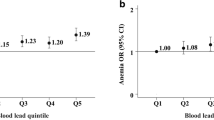
Results of the adjusted and unadjusted logistic regression models used to determine the association between elevated BLL, ID and anemia are presented in Table 4. We found a significant association between elevated BLL and ID (p = 0.003). The prevalence of elevated BLL was 16.2% in children with ID and 5.8% in children without ID. Similarly, bivariate analysis showed a significant association between elevated BLL and anemia (p = 0.003).
Finally, the multivariate logistic regression model for elevated BLL adjusted by sex and age of the children confirmed the obtained associations (Table 4).
Discussion
In the present study, a direct association between elevated BLL (≥ 5 µg/dL) and ID was found in children aged 1–6 y exposed to low environmental lead poisoning. These associations remained even when data were adjusted by sex and age < 2 y.
Numerous reports have analysed the currently studied associations in varying child age-ranges, levels of environmental lead exposure, thresholds for elevated BLL and parameters to evaluate iron nutritional status. For instance, in agreement with the present findings, a study in Chinese children aged 0–5 y with low levels of lead exposure showed that blood lead concentrations were inversely associated with iron status [29]. Another report of children aged 1 through 12 y found that the prevalence of lead poisoning was higher in children with than without ID (3.4% vs. 1.1%) [30]. A longitudinal study of 1,275 children followed-up from 9 to 42 months of age determined that children with ID were at higher risk of developing lead poisoning (OR: 4.12, 95% CI: 1.96; 8.65) than children with normal/adequate iron status [17]. On the other hand, and as opposed to the present results, a recent study of children between 0.54 and 14.87 y did not find a significant association between BLL and trace elements such as iron, probably due to the relatively low lead levels and the adequate iron status of the children analysed [31].
In addition to the higher proportion of children with elevated BLL and ID, our data revealed that ferritin and Hb levels were markedly lower in children with elevated BLL, which coincided with studies performed in Brazil [19], Pakistan [20], and India [32]. In line with our findings, a recent systematic review of 58 studies in pediatric populations (0–15 y) from 1974 to 2021 concluded that elevated BLL could be related to low iron deposits and higher risk of anemia [33]. Similarly, a meta-analysis demonstrated that the risk of developing IDA was higher among children with BLL > 10 µg/dL than in children with lower BLL (OR: 2.75 (95% CI, 1.10–6.85 µg/L; p = 0.0303) [34].
This study is one among few carried out in Argentina evaluating the association between BLL and iron status in a child population without evident clinical signs or symptoms of lead poisoning, performing periodic health checks. Such association is particularly relevant in younger children undergoing nervous system development, considering that most research has found association of ID and lead poisoning with child cognitive development and behaviour [35, 36].
Nevertheless, the current study has some limitations. First, results correspond to a sample of children performing health checks in the public health system of a region of the province of Buenos Aires, Argentina, which cannot be extrapolated to the general population. Secondly, since this is a cross-sectional study, causality cannot be inferred. Third, although the indicators used to define ID are readily accessible, they may prove insufficient. Finally, we did not evaluate dietary lead intake as an important source of lead in children, as it has been reported in other studies [37, 38].
Bearing in mind that there is no safe blood lead threshold value below which lead has no adverse effects on neurodevelopment, prevention strategies should not be discontinued, particularly in vulnerable populations. Furthermore, considering the high ID prevalence currently found, the individual risk of lead poisoning once the iron status of children has been determined should be evaluated, just like the presence of anemia during health checks to prevent the combined effects of ID and lead poisoning on child cognitive development and behavior.
Conclusion
BLL ≥ 5 µg/dL was significantly associated with ID and anemia in children aged 1–6 years.
References
World Health Organization (2010) Childhood lead poisoning. Geneva, World Health Organization. https://apps.who.int/iris/handle/10665/136571
Tsoi MF, Cheung CL, Cheung TT, Cheung BM (2016) Continual decrease in blood lead level in americans: United States National Health Nutrition and Examination Survey 1999–2014. Am J Med 129:1213–1218
Martins E, Varea A, Hernández K, Sala M, Girardelli A, Fasano V, Disalvo L (2016) Niveles De plombemia en niños de 1 a 6 años en la región de La Plata, Argentina: Identificación De factores de riesgo de exposición al plomo. Arch Argent Pediatr 114(6):543–548
Martínez SA, Simonella L, Hansen C, Rivolta S, Cancela LM, Virgolini MB (2013) Blood lead levels and enzymatic biomarkers of environmental lead exposure in children in Cordoba, Argentina, after the ban of leaded gasoline. Hum Exp Toxicol 32(5):449–463
Centers for Disease Control and Prevention (CDC) (2012) CDC response to Advisory Committee on Childhood Lead Poisoning Prevention recommendations in ‘‘Low level lead exposure harms children: a renewed call for primary prevention.’’ [on line]. US Department of Health and Human Services, CDC, Atlanta, GA. http://www.cdc.gov/nceh/lead/acclpp/cdc_response_lead_exposure_recs.pdf
De Benoist ME, Egli I, Cogswell M (2008) Worldwide Prevalence of Anaemia 1993–2005:WHO Global Database of Anaemia. Technical Report. World Health Organization, Geneva
Pivina L, Semenova Y, Doşa MD, Dauletyarova M, Bjørklund G (2019) Iron Deficiency, cognitive functions, and Neurobehavioral disorders in Children. J Mol Neurosci 68(1):1–10
Carter RC, Jacobson JL, Burden MJ, Acrimony-Sivan R, Dodge NC, Angelilli ML et al (2010) Iron deficiency anemia and cognitive function in infancy. Pediatrics 126(2):e427–434
McCann JC, Ames BN (2007) An overview of evidence for a causal relation between iron deficiency during development and deficits in cognitive or behavioral function. Am J Clin Nutr 85(4):931–945
Koller K, Brown T, Spurgeon A, Levy L (2004) Recent developments in low-level lead exposure and intellectual impairment in children. Environ Health Perspect 112(9):987–994
Lanphear BP, Hornung R, Khoury J, Yolton K, Baghurst P, Bellinger DC et al (2005) Low-level environmental lead exposure and children’s intellectual function: an international pooled analysis. Environ Health Perspect 113(7):894–899
Jusko TA, Henderson CR, Lanphear BP, Cory-Slechta DA, Parsons PJ, Canfield RL (2008) Blood lead concentrations < 10 microg/dL and child intelligence at 6 years of age. Environ Health Perspect 116(2):243–248
Kwong WT, Friello P, Semba RD (2004) Interactions between iron deficiency and lead poisoning: epidemiology and pathogenesis. Sci Total Environ 330:21–37
Garrick MD, Singleton ST, Vargas F, Kuo HC, Zhao L, Knöpfel M et al (2006) DMT1: which metals does it transport? Biol Res 39(1):79–85
Bradman A, Eskenazi B, Sutton P, Athanasoulis M, Goldman LR (2001) Iron deficiency associated with higher blood lead in children living in contaminated environments. Environ Health Perspect 109:1079–1084
Muwakkit S, Nuwayhid I, Nabulsi M, al Hajj R, Khoury R, Mikati M et al (2008) Iron deficiency in young Lebanese children: association with elevated blood lead levels. J Pediatr Hematol Oncol 30:382–386
Wright RO, Tsaih SW, Schwartz J, Wright RJ, Hu H (2003) Association between iron deficiency and blood lead level in a longitudinal analysis of children followed in an urban primary care clinic. J Pediatr 142:9–14
Zimmermann MB, Muthayya S, Moretti D, Kurpad A, Hurrel RF (2006) Iron fortification reduces blood lead levels in children in Bangalore. India Pediatr 117:2014–2021
Rondó PH, Carvalho Mde F, Souza MC, Moraes F (2006) Lead, hemoglobin, zinc protoporphyrin and ferritin concentrations in children. Rev Saude Publica 40(1):71–76
Shah F, Kazi TG, Afridi HI, Baig JA, Khan S, Kolachi NF et al (2010) Environmental exposure of lead and iron deficit anemia in children age ranged 1–5 years: a cross sectional study. Sci Total Environ 408(22):5325–5330
Serwint JR, Damokosh AI, Berger OG, Chisolm JJ Jr, Gunter EW, Jones RL et al (1999) No difference in iron status between children with low and moderate lead exposure. J Pediatr 135:108–110
Hammad TA, Sexton M, Langenberg P (1996) Relationship between blood lead and dietary iron intake in preschool children. A cross-sectional study. Ann Epidemiol 6(1):30–33
Centers for Disease Control and Prevention (CDC) (2012) CDC response to Advisory Committee on Childhood Lead Poisoning Prevention recommendations in ‘‘Low level lead exposure harms children: a renewed call for primary prevention.’’ [on line] Atlanta, GA: US Department of Health and Human Services, CDC. http://www.cdc.gov/nceh/lead/acclpp/cdc_response_lead_exposure_recs.pdf
World Health Organization (2011) Serum ferritin concentrations for the assessment of iron status and iron deficiency in populations. Vitamin and Mineral. WHO, Geneva (Switzerland), Nutrition Information System (WHO/NMH/NHD/MNM/112)
Organización Mundial de la Salud (2011) Concentraciones de hemoglobina para diagnosticar la anemia y evaluar su gravedad. Ginebra, Organización Mundial de la Salud, (WHO/NMH/NHD/MNM/11.1) http://www.who.int/vmnis/indicators/haemoglobin_es.pdf
De Onis M, Onyango AW, Borghi E, Garza C, Yang H (2007) Comparison of the World Health Organization (WHO) child growth standards and the National Center for Health Statistics/WHO international growth reference: implications for child health programmes. Public Health Nutr 9(7):42–47
Instituto Nacional de Estadística y Censos. Mapa de necesidades básicas insatisfechas 2001. Buenos Aires: INDEC (2003) [Accessed on: June 10th, 2016]. http://www.indec.gov.ar/micro_sitios/webcenso/aquisecuenta/Aqui7.pdf
Croghan CW, Egeghy PP (2003) Methods of dealing with values below the limit of detection using SAS. Presented at Southeastern SAS User Group, St. Petersburg, FL, September 22–24
Guo Y, Deng YH, Ke HJ, Wu JL (2021) Iron Status in relation to low-level lead exposure in a large Population of children aged 0–5 years. Biol Trace Elem Res 199(4):1253–1258
Yip R, Dallman PR (1984) Developmental changes in erythrocyte protoporphyrin: roles of iron deficiency and lead toxicity. J Pediatr 104(5):710–713
Martínez-Hernanz Á, González-Estecha M, Blanco M, Fuentes M, Ordóñez-Iriarte JM, Palazón-Bru I et al (2020) Blood lead in children and associations with trace elements and sociodemographic factors. J Trace Elem Med Biol 58:126424
Tripathi RM, Raghunath R, Mahapatra S, Sadasivan S (2001) Blood lead and its effect on cd, Cu, Zn, Fe and hemoglobin levels of children. Sci Total Environ 277(1–3):161–168
Słota M, Wąsik M, Stołtny T, Machoń-Grecka A, Kasperczyk S (2022) Effects of environmental and occupational lead toxicity and its association with iron metabolism. Toxicol Appl Pharmacol 434:115794
Farkhondeh T, Mansouri B, Binkowski LJ, Błaszczyk M, Pirsaheb M, Azadi NA et al (2022) Blood lead concentrations in children with iron deficiency anemia: a systematic review and meta-analysis. Environ Sci Pollut Res Int 29(3):3199–3212
Kordas K (2010) Iron, lead, and children’s behavior and cognition. Annu Rev Nutr 30:123–148
Wasserman G, Graziano JH, Factor-Litvak P, Popovac D, Morina N, Musabegovic A et al (1992) Independent effects of lead exposure and iron deficiency anemia on developmental outcome at age 2 years. J Pediatr 121(5 Pt 1):695–703
European Food Safety Authority (2012) Lead dietary exposure in the European population. EFSA J 10(7):2831
Martins E, Malpeli A, Asens D, Telese L, Fasano V, Vargas V et al (2018) Contribution of diet to lead exposure among children aged 1 to 7 years in La Plata, Buenos Aires. Arch Argent Pediatr 116(1):14–20
Funding
This study received funding from IDIP.
Author information
Authors and Affiliations
Contributions
L.D. and A.V. contributed to the first draft, the study design, investigation and final writing. N.M. and M.S. participated in the investigation and the final writing of the manuscript. M.V.F. participated in study design, statistical analysis and final writing. H.F.G. was in charge of supervising and administering the project and participated in the final writing of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
The study protocol was approved by the Institutional Research Review Board of IDIP. The study results were communicated to parents/tutors. Children whose BLL were ≥ 5 g/dL were referred to the Toxicology Service for follow-up.
Consent to Participate
Written informed consent was signed by all the participating parents and/or tutors and attested by a witness.
Conflict of Interest
The authors declare they have nothing to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Disalvo, L., Varea, A., Matamoros, N. et al. Blood Lead Levels and Their Association with Iron Deficiency and Anemia in Children. Biol Trace Elem Res (2024). https://doi.org/10.1007/s12011-024-04163-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12011-024-04163-y