Abstract
Lead is a heavy metal abundant in nature that causes haematological imbalances, and hepatic and renal dysfunction, and this imbalance has been linked to oxidative stress. Several reports have shown that natural products are implicated in ameliorating metal poisonings. Ginkgo biloba is a flavonoid-rich natural herbal supplement with several pharmacological properties. The present study investigated effect of Ginkgo biloba supplement (GBS) on lead-induced toxicity. Animals were given a lead dose of 25 mg/kg for 14 days orally and then given Ginkgo biloba supplements of 50 mg/kg and 100 mg/kg orally for 14 days. Animals given GBS had significantly improved haematological and rheological parameters. GBS showed a protective impact in terms of improved kidney and liver histology, anti-oxidant enzyme activity (CAT, SOD, GSH, and MDA), organ function indices, and a lower rate of erythrocyte osmotic fragility. Conclusively, Ginkgo biloba supplementation attenuated lead toxicity by normalization of haematological imbalances, and hepatic and renal dysfunction as well as maintaining erythrocyte membrane integrity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The basic role of blood, which is a crucial unique circulatory tissue, is to maintain homeostasis. Blood is made up of cells suspended in a fluid intercellular material (plasma). Red blood cells, white blood cells, and leucocytes are useful in monitoring feed toxicity, especially with feed elements that affect the blood and farm animal health [1]. The study of the flow properties of blood and its constituents (plasma and formed elements such as erythrocytes, white blood cells, and platelets) is known as hemorheology [2]. Basic features of blood flow include haematocrit, plasma and whole blood viscosity, plasma proteins, and erythrocyte deformability and aggregation [3]. For example, blood viscosity is related to haemoconcentration but inversely proportional to flow rate [4]. This means that substances that increase blood components while decreasing plasma could raise blood viscosity, lowering flow rate and affecting tissue perfusion leading to cell damage [4, 5]. There is evidence that both genetic and environmental factors play important roles in hemorheological changes [6]. However, environmental factors have been significantly implicated in some interorgan blood-related diseases [6]. There is mounting evidence suggesting that blood flow indices are important variables in appropriate tissue perfusion and changes in these variables play a key role in disease processes [7].
Lead (Pb) is a non-biodegradable, pervasive contaminant that poses a serious threat to human health. It is spread naturally, but industrial activity has drastically increased their concentrations in the environment [8,9,10]. Lead is emitted by industries such as smelting and mining, battery manufacture, pigment manufacturing, and ceramic manufacturing. The risk of human exposure has doubled as a result of increased emissions of this metal into the environment and its non-biodegradability [11]. However, due to their prevalence in food, air, and tobacco leaves, the most common routes of Pb exposure include ingestion and inhalation [8,9,10,11]. It is important to mention here that the World Health Organization (WHO) Model Lists of environmental pollutant recommends lead as one of the top 5 environment toxicants [12]. Lead has additionally been listed second on the priority list of harmful compounds by the US Agency for Toxic Substances and Disease Registry (ATSDR) [13]. Lead poisoning has a variety of negative impacts on the body, including brain, kidneys, liver, blood homeostasis, and immune system toxicity [14, 15]. The liver, kidneys, and brain, on the other hand, show higher vulnerability to lead-induced toxicity [16]. While lead is conjugated in the liver and eliminated through the kidneys, its accumulation in the liver and kidneys causes morphological changes in both organs [17]. Several bodies of evidence have shown that oxidative stress is one of the key mechanisms of lead-induced toxicity [17,18,19,20]. Other mechanisms include binding to oxygen, nitrogen, and sulphur ligands, which may affect a variety of enzymes and proteins [18, 21], interaction with bioelements [22,23,24], and induction of apoptosis as well as release of pro-inflammatory cytokines [25,26,27,28].
Previous studies have shown that natural products have been used to mitigate metal-related toxicity [29]. Polyphenols, flavonoids, vitamins, and other bioactive components have all been linked to a reduction in the negative effects of lead poisoning including lead-induced neurotoxicity because of their ability to downregulate pro-oxidative factors and upregulation of anti-oxidant enzymes [29]. In animal models, many herbs, such as Bacopa monniera, Allium sativum, Coriandrum sativum, and others, have been shown to reduce lead poisoning [30,31,32]. Furthermore, some active agents extracted from natural products such as naringenin, silymarin, ascorbic acid, and tannic acid have also been shown to be effective in inhibiting lead-induced organ damage including haematological and biochemical abnormalities [33,34,35,36,37].
Ginkgo biloba supplement (GBS) is a popular commercial medical herb derived from the green leaves of the ginkgo tree, which is one of the oldest surviving plant species [38]. It is known to contain secondary metabolites, and its pharmacological potential is attributed to the abundance of flavonoid glycosides (kaempferol, quercetin, myricetin, apigenin, isorhamnetin, luteolin, and tamarixetin) and terpene trilactones (ginkgolides A, B, C, J, M, K, L, P, and Q, as well as bilobalide) [39,40,41]. In vivo experiments have shown that GBS increases blood flow and block platelet activating factor. It protects the cell membrane from free radical damage and protects against myocardial and brain ischemia/reperfusion injury [42]. GBS is commonly utilized in the clinical treatment of cardiovascular and neurological diseases including Alzheimer’s disease, labyrintopathies [43], and Parkinson’s disease [44]. Additionally, GBS has also been shown to demonstrate hepatoprotective, anti-inflammatory, and antioxidant properties [44,45,46,47,48]. However, the effect of GBS on lead-induced hepato-renal damage and hemorheological changes remains unknown. Hence, the study was designed to investigate the protective effects of GBS on lead-induced hepato-renal damage and hemorheological changes in male Wistar rats.
Materials and Methods
Chemicals
Gingko biloba supplement was purchased from Mason Vitamins, INC, Miami Lakes, USA. Lead acetate (Pb), thiobarbituric acid, hydrogen peroxide, trichloroacetic acid, and glutathione were purchased from Sigma-Aldrich, St Louis, MO, USA. All other chemicals used were of analytical grade.
Animals
Twenty (20) male Wistar rats weighing between 150 and 200 g were used for this study. The study was done in the PAMO University of Medical Sciences, Port-Harcourt, Rivers State, Nigeria. During the experiment, the rats were kept in conventional laboratory settings (temperature 25 °C, relative humidity 35–60%, 12-h light–dark cycle) and had free access to regular rat chow and drinking water. The study was approved, and the protocol followed strictly to the guidelines set forth by the University Ethical Committee on Animal Experimentation (PUMS-AREC/028), which follows the “Principle of Laboratory Animal Care” (NIH Publication No. 85–23).
Study Design and Experimental Procedure
Ginkgo biloba supplements contain 24–28% flavonoids, 5–12% terpene lactones (2.8–6.0% ginkgolides A, B, and C, with at least 1.3% ginkgolides B and 2.6–5.6% bilobalide), and less than 5 ppm ginkgolic acids in standardized form. Commercial manufacturers isolated the active components from G. biloba leaves. Ginkgo biloba and lead acetate were each given orally for 14 days after being dissolved in distilled water. After 1 week of acclimatization, rats were randomly divided into four groups and given the following treatments: group 1 (control) received water (10 mL/kg), group 2 received 25 mg/kg b.wt of lead acetate for 14 days, and groups 3 and 4 received 50 mg/kg and 100 mg/kg of Ginkgo biloba supplement for 14 days. The doses of Ginkgo biloba supplement [49] and lead acetate [50, 51] chosen were based on the findings of prior studies and reports. The animals were anesthetized (Ketamin 70 mg/kg), and euthanized by cervical dislodgement, and the blood, kidney, and liver tissues were harvested; some were preserved at 4 °C while some were preserved in 10% neutral-buffered formalin (Fig. 1).
Haematology and Rheological Variables
Blood was obtained from anesthetized animals via heart puncture and placed in EDTA-coated bottles. An automated haematology analyser was used to determine the haematological parameters (ABX Micros 60 from Horiba ABX, France). RBC, PCV, haemoglobin white blood cell (WBC), and other haematological indicators such as lymphocytes and platelet count were all measured. Osmotic fragility was done according to the methods of Oyewale, [52]. Whole blood viscosity was estimated using the method described by Reid and Ugwu [53] and the flow rate was expressed as flow per minute. Plasma fibrinogen concentration was estimated by clot weight according to the method of Ingram [54].
Biochemical Assay
The concentrations of creatinine and urea for renal function, as well as alanine aminotransferase (ALT), aspartate aminotransferase (AST), and alkaline phosphatase (ALP) activities for liver injury markers in the plasma, were determined using a Randox test kit according to the protocol described by Reitman and Frankel [55].
Preparation of Tissue for Antioxidant Assay
The kidney and liver tissues were removed after euthanasia. Harvested tissues were homogenized in 10% w/v phosphate buffer (0.1 M, pH 7.4), and centrifuged at 10,000 rpm for 10 min at 4 °C, and the supernatants were immediately frozen and preserved at 10 °C for antioxidant experiments. Catalase (CAT), glutathione (GSH), superoxide dismutase (SOD), and malondialdehyde (MDA) assays were performed on the liver and kidney supernatants using various kits according to Beer and Sizer [56], McCord and Fridovich [57], and Ohkawa et al. [58] protocols, respectively.
Histology
The organs were fixed in 10% neutral-buffered formalin, dehydrated in increasing concentrations of ethanol, cleaned with xylene, and then embedded in paraffin. Haematoxylin and eosin were used to stain 2-μm sections of liver and kidney paraffin blocks, respectively. A light microscope was used to capture the stained slides at 400 magnifications, and the resulting histomicrograph was examined for histoarchitectural changes as previously described by Asiwe et al. [59].
Statistical Analysis
All data was analysed using one-way analysis of variance (ANOVA) in GraphPad prism 7.0 (GraphPad Software, San Diego, CA) and expressed as mean standard error of mean (SEM). Multiple group comparisons were done using the Tukey post hoc test. Two-way ANOVA was used for osmotic fragility, and p < 0.05 was regarded statistically significant.
Results
Ginkgo biloba Supplement (GBS) Alleviates Haematological Alterations in Male Wistar Rats Treated with Lead Acetate
The effect of GBS on haematological variables in lead-treated rats is shown in Fig. 2. Exposure of rats to lead acetate daily for 14 days caused a significant (p < 0.05) decrease in RBC, Hb, PCV, lymphocyte, and platelets. Treatment with GBS (50 and 100 mg/kg, p.o.) significantly (p < 0.05) increased the mean value of these variables RBC [F(3,12) = 32.9, p < 0.0001] Hb [F(3,12) = 6.42, p = 0.0077] PCV [F(3,12) = 16.3, p = 0.0002], lymphocyte [F(3,12) = 20.1, p < 0.0001], and platelet [F(3,12) = 36.7, p < 0.0001] when compared with lead-treated animals. However, WBC showed a significant (p < 0.05) increase in both lead-treated and GBS-treated animals [F(3,12) = 11.2, p = 0.0009] when compared with the control animals as shown in Fig. 2(A–F).
Ginkgo biloba supplement alleviates haematological alterations in male Wistar rats treated with lead acetate: (A) red blood cell, (B) haemoglobin concentration, (C) packed cell volume, (D) white blood cell, (E) lymphocyte, (F) platelet. All values are expressed as mean ± standard error of mean (n = 5), *p < 0.05 when compared with the control group while #p < 0.05 was significant when compared with the lead group (one-way ANOVA followed by Tukey post hoc test). GBS, Ginkgo biloba supplement
Ginkgo biloba Supplement Reduces Hyperfibrinogenemia, Clotting Time, and Erythrocyte Osmotic Fragility in Male Wistar Rats Exposed to Lead Acetate
As presented in Fig. 3(A–D), GBS reduced the clotting time (Fig. 3B) and fibrinogen (Fig. 3C) level significantly (p < 0.05) when compared with the marked increase caused by lead exposure [F (3,12) = 130, p < 0.0001 and F (3,12) = 91.2, p < 0.0001] respectively. However, both lead and GBS (50 and 100 mg/kg) showed a significant (p < 0.05) increase in blood flow rate/viscosity (Fig. 3A) when compared with control animals [F(3,12) = 40.1, p < 0.0001]. Two-way ANOVA revealed a significant (p < 0.05) difference in the interaction between treatment groups [F (15,72) = 324, p < 0.0001] and column factor [F (3,72) = 596, p < 0.0001] as GBS reduces the percentage haemolysis at 0.3, 0.5, 0.7, and 0.9 concentrations of sodium chloride as shown in Fig. 3D.
Ginkgo biloba supplement reduces hyperfibrinogenemia, clotting time, and erythrocyte osmotic fragility in male Wistar rats exposed to lead acetate: (A) viscosity, (B) clotting time, (C) fibrinogen, (D) erythrocyte osmotic fragility. All values are expressed as mean ± standard error of mean (n = 5), *p < 0.05 when compared with the control group while #p < 0.05 was significant when compared with the lead group (one-way ANOVA followed by Tukey post hoc test). GBS, Ginkgo biloba supplement
Ginkgo biloba Supplement Alleviates Liver Damage and Improves Renal Functions in Male Wistar Rats Exposed to Lead Acetate
Following the exposure of animals to lead acetate, Fig. 4 shows the effects of GBS on liver and renal function markers. There was a significant (p < 0.05) increase in AST [F(3,12) = 28.2, p < 0.0001], ALT [F(3,12) = 18.8, p < 0.0001], ALP [F(3,12) = 9.41, p = 0.0018], urea [F(3,12) = 34, p < 0.0001), and creatinine [F(3,12) = 48.6, p < 0.0001] when compared with control groups. However, treatment with GBS (50 and 100 mgkg, p.o.) significantly (p < 0.05) reduced these elevated liver enzymes (Fig. 4A–C) and renal markers (Fig. 4D–E) when compared with the lead-treated groups.
Ginkgo biloba supplement alleviates liver damage and improves renal functions in male Wistar rats exposed to lead acetate: (A) aspartate aminotransferase (AST), (B) alanine aminotransferase (ALT), (C) alkaline phosphatase (ALP), (D) urea, (E) creatinine. All values are expressed as mean ± standard error of mean (n = 5), *p < 0.05 when compared with the control group while #p < 0.05 was significant when compared with the lead group (one-way ANOVA followed by Tukey post hoc test). GBS, Ginkgo biloba supplement
Ginkgo biloba Supplement Improves Endogenous Antioxidant Enzymes in the Kidney and Liver of Male Wistar Rats Exposed to Lead Acetate
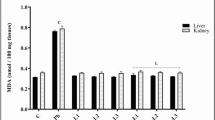
Table 1 indicates the activity of lipid peroxidation (MDA level), catalase (CAT), glutathione (GSH), and superoxide dismutase (SOD) in the kidney tissue of lead-induced renal toxicity. There was significant (p < 0.05) decrease in SOD, CAT, and GSH in lead-treated group; however, treatment with Ginkgo biloba supplement elevated the levels of these enzyme in a dose-dependent manner. There was increase in MDA in the lead group suggesting increased lipid peroxidation. However, 50 mg of GBS improves lipid membrane by decreasing kidney MDA levels. Also, lead treatment caused a significant (p < 0.05) decrease in the weight of the kidney when compared with control group; however, GBS (50 and 100 mg/kg, p.o.) did not reverse the effect caused by lead compared with lead-treated group (Table 1). The endogenous antioxidant enzyme (CAT and SOD) in the liver was significantly (p < 0.05) increased in GBS-treated animals when compared with lead-treated group (Table 2). However, liver GSH level was significantly (p < 0.05) increased by Ginkgo biloba supplementation. There was significant increase in MDA (lipid peroxidation) in lead-treated group when compared to the control group. However, treatment with GBS (50 and 100 mg/kg) prevented the lipid peroxidation by significantly reducing liver MDA level. The weight of the liver reduced in lead group when compared with control while GBS increased the weight significantly when compared with lead-exposed group as shown in Table 2.
Ginkgo biloba Supplement Protects Against Lead-Induced Liver and Kidney Histoarchitectural Alterations in Male Wistar Rats
As represented in Fig. 5, rats exposed to lead acetate had histoarchitectural alterations as moderate atrophy of hepatic cords and single necrosis of hepatocytes was observed. However, treatment with Ginkgo biloba supplement (50 and 100 mg/kg) improved the histoarchitecture of hepatocytes (Liver plate B, C and D). The kidney also showed glomerular and tubular atrophy and random tubular epithelial coagulation necrosis in lead-exposed animals. Treatment with GBS restored the kidney tissue to its normal histoarchitecture (kidney plate B, C, and D).
Ginkgo biloba supplement protects against lead-induced liver and kidney histoarchitectural alterations in male Wistar rats: (A) control, (B) lead, (C) 50 mg/kg of GBS after lead exposure, (D) 100 mg/kg of GBS after lead exposure. Arrows indicate significant lesion. GBS, Ginkgo biloba supplement. (H&E × 400)
Discussion
Lead poisoning is one of the most dangerous heavy metal poisonings for both humans and animals. Lead toxicity is a major source of concern for public health professionals all around the world. Lead toxicity manifests itself in a variety of organ systems, including the brain, liver, kidneys, and lungs [18]. Herbal medicine supplements, on the other hand, can be used to prevent lead toxicity. Natural remedies have been used to treat a variety of disorders since the dawn of time, and food supplement usage has recently gotten a lot of attention as a way to cope with liver and kidney toxicity. Ginkgo biloba contains a variety of bioactive chemicals that have the ability to heal tissue injuries while also controlling oxidative and inflammatory processes. In the study, GBS significantly attenuated lead-induced haematological, haemorheological, hepatic, and renal imbalances in male Wistar rat.
As previously reported by Andjelkovic et al. [60], treatment of rats with lead resulted in a considerable fall in RBC count, Hb concentration, and % PCV, indicating normocytic normochromic anaemia. This anaemia could be caused by the suppressive impact of lead on the haematopoietic organ, which affects erythropoiesis, or it could be caused by lead binding to RBCs, which increases erythrocyte membrane fragility, resulting in rapid erythrocyte destruction (Fig. 2A–C). Furthermore, because lead has the potential to resist divalent cations like iron, it could be linked to diminished haemoglobin synthesis, which could be produced by the suppression of aminolevulinic acid dehydratase (ALAD) or improper iron metabolism [61,62,63]. Treatment with Ginkgo biloba supplement, on the other hand, appears to have haematinic potential, since Hb concentration and RBC count were significantly enhanced, resulting in increased packed cell volume. The major functions of the white blood cell and its differentials are to fight infections, defend the body against invasion by foreign organisms through phagocytosis, and produce or at the very least transport and distribute antibodies in the immune response. The impact of lead on the immune system varies depending on the type of lead, the route of administration, the dose, the duration of exposure, the age of the host, and genetic susceptibility [64, 65]. Immunosuppression has been reported as a result of chronic high-level lead exposure [66, 67]. Surprisingly, exposure to a low dose of lead in this study resulted in a large increase in WBC count and a decrease in lymphocytes, implying that lead has a negative influence on body physiology. This change could be due to the body’s ability to adapt to local environmental and disease-causing situations. Isaac et al. [68] have shown lead to have immunostimulating effects, resulting in leukocytosis and lymphocytopenia, both of which imply bone marrow toxicity and a significant risk of lymphoproliferative neoplasm formation [64, 66, 69]. GBS was unable to modulate this condition in this current study, which was ascribed to the duration of the experiment, since the results indicated the possibility of immunomodulation. Blood platelets are also involved in the clotting process. Low platelet concentration indicates that the clotting process could take longer time, resulting in significant blood loss in the event of an injury [68]. Treatment with GBS, on the other hand, significantly increased platelet count while also reducing clothing time, suggesting that Ginkgo biloba may play a role in platelet aggregation. Fibrinogen is a glycoprotein produced in the liver that aids in the synthesis of fibrin, which causes blood clots. The presence of hyperfibrinogenemia in lead-exposed animals suggests the likelihood of thrombosis. GBS, on the other hand, improved this condition and eliminated the risk of thrombosis and inflammation. The osmotic fragility of lead-exposed rats revealed that rats given Ginkgo biloba supplement (GBS) considerably improved erythrocyte osmotic resistance to hypotonic stress (0.3, 0.5, 0.7, and 0.9% NaCl concentrations) (Fig. 3D). The findings show that GBS protect red blood cells from hypotonic stress. This protective effect has been attributed to flavonoids (quercetin and triterpenes), which are important ingredients of Ginkgo biloba [70, 71]. This work, on the other hand, contradicts Abdel-Baieth [72], who claimed that Ginkgo biloba leaf extract increased red cell osmotic fragility in hypotonic media.
The administration of lead acetate to rats resulted in a rise in ALP, AST, and ALT serum concentrations (Fig. 4A–C), as described in earlier investigations [62, 73, 74]. Lead disrupts the cytoskeleton, causing membrane rupture and lysis, resulting in a rise in the quantity of these biochemicals in the blood [62]. Ginkgo biloba supplementation significantly reduced ALT, AST, and ALP in serum in the current study, which is consistent with prior research [75]. By inhibiting the pro-inflammatory cytokine NF-кB, GBS has been shown to improve liver architecture and function in carbon tetrachloride (CCl4)–treated Wistar rats, suggesting a powerful hepatoprotective action of GBS [76]. In terms of kidney function markers, lead-treated rats showed a considerable rise in serum urea and creatinine levels, which was also observed in prior investigations [15, 61]. Increased protein breakdown, which raises ammonia level and, in turn, serum urea concentrations, is caused by oxidative stress [77]. Accordingly, the breakdown of the renal cell brush border epithelia caused by free radicals rendered the cells impermeable to urea and creatinine [78]. There is an increase in the levels of these kidney indicators in blood due to limited or no tubular absorption of urea and creatinine by the renal tubules. GBS considerably reduced the levels of urea and creatinine in the current investigation. This could be attributed to Ginkgo biloba’s strong antioxidant potential, which counteracts the oxidative insults produced in the kidneys as a result of lead acetate–induced toxicity, suggesting Ginkgo’s nephro-protective potential against lead poisoning (Fig. 4D–E).
Lead has been shown to cause oxidative damage to membrane lipids by increasing peroxidation [17]. Liver and kidney cells suffer from uncontrolled peroxidation because liver and kidney are the most affected organs due to ingestion and/or inhalation exposure [79]. It causes a loss of membrane integrity, which leads to cell death [80]. Lead acetate caused a considerable rise in lipid peroxidation in the present investigation, as measured by a significant increase in MDA concentration in the liver and kidney homogenate, which is consistent with prior research [80]. However, GBS significantly reduced lipid peroxidase in both organs (Tables 1 and 2), which could be related to Ginkgo biloba’s anti-oxidative nature and its ability to scavenge free radicals [81]. Anti-oxidant enzymes stored in the body neutralize free radicals produced during oxidative stress. Lead acetate reduced the activities of CAT, SOD, and GSH in both liver and kidney tissues in the current experiment, making tissues vulnerable to oxidative stress, as previously reported [82]. These anti-oxidant enzymes feature active sites that act as targets for harmful heavy metals such as lead, mercury, and cadmium, resulting in decreased enzymatic activity. The sulfhydryl groups of these enzymes have a high affinity for lead, which causes them to lose their activity [83]. The GBS treatment has been shown to restore DNA damage caused by stannous chloride poisoning’s high oxidative environment [83]. The histological analysis demonstrated that Ginkgo biloba supplementation restored architectural alterations caused by lead treatment (Figs. 5). Lead, as previously stated, causes oxidative stress in the liver and kidney, resulting in pathological alterations [15, 84]. Lead is taken up by proximal tubular cells, according to studies on its transit in the kidney [85]. Renal tubular damage is also caused by high levels of lead, with glomerular and tubular shrinkage as well as random tubular epithelial coagulation necrosis [86, 87]. In injured renal tissue with necrosis in the parenchyma, tubular dilatations, and hyperemic situations, GBS has been shown to offer protection to histological integrity [88]. At higher dosage of GBS, the histological type of kidney injury was shown to be significantly reduced. Our findings matched those of [84], who found that ginger therapy had similar effects. According to prior studies, lead exposure resulted in moderate hepatic cord atrophy and a single hepatocyte necrosis [15, 62]. Because the liver is the first organ exposed to lead and plays a substantial role in lead accumulation, biotransformation, and removal, these pathological characteristics are commonly seen in lead intoxication [62]. In this study, GBS treatment resulted in significant recovery of hepatic and renal architectures following lead exposure as evidenced by the histological observation. However, further investigations are needed to confirm the particular involvement of the signalling mechanisms employed by Ginkgo biloba in the cytoarchitectural protection of the liver and kidney.
Conclusion
The results of this study showed that treatment with Ginkgo biloba supplement significantly ameliorated lead toxicity by normalization of haematological indices and modulation of haemorheological factors as well as maintaining erythrocyte membrane integrity. It also improved liver and renal functions by protecting the tissues against oxidative damage and histoarchitectural alterations caused by lead acetate intoxication. However, the findings from this study therefore suggest that supplementation with Ginkgo biloba might be a viable therapeutic approach for reducing lead-induced changes and oxidative damage–induced haematological imbalance and organ damage in lead toxicity.
Data Availability
All data are available upon request.
References
Oyawoye BM, Ogunkunle HN (2004) Biochemical and haematological reference values in normal experimental animals. Masson, New York, pp 212–218
Baskurt OK, Meiselman HJ (2003) Blood Rheology and hemodynamics. Semin Thromb Hemost 29(5):435–450
Rabai, M., (2012). In vitro hemorheological studies focusing on erythrocyte deformability and aggregation [Ph.D. thesis], University of Pecs, Hungary.
Chang HY, Li X, Karniadakis GE (2017) Modeling of biomechanics and biorheology of red blood cells in type 2 diabetes mellitus. Biophys J 113(2):481–490
Sloop GD, De Mast Q, Pop G, Weidman JJ, St Cyr JA., (2020). The role of blood viscosity in infectious diseases. Cureus 12(2): e7090.
Olafedehan, C.O., Obun, A.M., Yusuf, M.K., Adewumi, O.O., Oladefedehan, A.O., Awofolaji, A.O., Adeniji, A. A. (2010). Effects of residual cyanide in processed cassava peal meals on haematological and biochemical indices of growing rabbits (p.212). Proceedings of 35th Annual Conference of Nigerian Society for Animal Production.
Mohan A, Srinivasan V, Deepa R, Mohan V (2001) Lipoprotein(a): role in diabetes and its vascular complications. JAPI 49:1100–1105
Järup L, Åkesson A (2009) Current status of cadmium as an environmental health problem. Toxicol Appl Pharmacol 238:201–208
Casas SJ, Sordo J (2006) Lead chemistry, analytical aspects, environmental impact and health effects. Elsevier, Amsterdam The Netherlands, p 9780444529459
Satarug S, Garrett SH, Sens MA, Sens DA (2010) Cadmium, environmental exposure, and health outcomes. Environ Health Perspect 118:182–190
Tchounwou PB, Yedjou CG, Patlolla AK, Sutton DJ (2012) Heavy metal toxicity and the environment. EXS 2012(101):133–164
WHO (2010). Action is needed on chemicals of major public health concern. Public Health Environmental 2010, pp. 1–4. Available online: https://www.who.int/ipcs/assessment/public_health/chemicals_phc/en/ (accessed on 26 September 2018).
ATSDR Substance Priority List ATSDR. Available online: https://www.atsdr.cdc.gov/spl/ (accessed on 26 September 2018).
Assi MA, Hezmee MNM, Haron AW, Sabri MYM, Rajion MA (2016) The detrimental effects of lead on human and animal health. Veterinary World 9(6):660–671
Offor SJ, Mbagwu HO, Orisakwe OE (2017) Lead induced hepato- renal damage in male albino rats and effects of activated charcoal. Front Pharmacol 8:107
Jackie T, Haleagrahara N, Chakravarthi S (2011) Antioxidant effects of Etlingera elatior flower extract against lead acetate induced perturbations in free radical scavenging enzymes and lipid peroxidation in rats. BMC Res Notes 4(1):67
Flora G, Gupta D, Tiwari A (2012) Toxicity of lead: A review with recent updates. Interdiscip Toxicol 5:47–58
Matovic´, V., Buha, A., Dukic´-C´ osic´, D., Bulat, Z., (2015) Insight into the oxidative stress induced by lead and/or cadmium in blood, liver and kidneys. Food Chem Toxicol 78:130–140
Flora, S.J.S., Agrawal, S., (2017). Arsenic, cadmium, and lead; Academic Press: Cambridge, MA, USA, 2017; ISBN 9780128042397.
Matovic´, V., Buha, A., Bulat, Z., Dukic´-C´ osic´, D., ukic´-C´ osic´, D. (2011) Cadmium toxicity revisited: focus on oxidative stress induction and interactions with zinc and magnesium. Arh Hig Rada Toksikol 62:65–76
Nieboer E, Richardson DHS (1980) The replacement of the nondescript term “heavy metals” by a biologically and chemically significant classification of metal ions. Environ Pollut 1:3–26
Djukic´-C´ osic´, D., Ninkovic´, M., Malicˇevic´, Ž., Plamenac-Bulat, Z., Matovic´, V. (2006) Effect of supplemental magnesium on the kidney levels of cadmium, zinc, and copper of mice exposed to toxic levels of cadmium. Biol Trace Elem Res 114:281–292
Bulat ZP, Djukic´-C´ osic´, D., Malicˇevic´, Ž., Bulat, P., Matovic´, V. (2008) Zinc or magnesium supplementation modulates Cd intoxication in blood, kidney, spleen, and bone of rabbits. Biol Trace Elem Res 124:110–117
Bulat Z, Dukic´-C´ osic´, D., Antonijevic´, B., Buha, A., Bulat, P., Pavlovic´, Z. Matovic´, V. (2017) Can zinc supplementation ameliorate cadmium-induced alterations in the bioelement content in rabbits? Arh Hig Rada Toksikol 2017(68):38–45
Rani A, Kumar A, Lal A, Pant M (2014) Cellular mechanisms of cadmium-induced toxicity: a review. Int J Environ Health Res 24:378–399
Waisberg M, Joseph P, Hale B, Beyersmann D (2003) Molecular and cellular mechanisms of cadmium carcinogenesis. Toxicology 192:95–117
Joseph P (2009) Mechanisms of cadmium carcinogenesis. Toxicol Appl Pharmacol 238:272–279
Ahmed YF, Eldebaky HAA, Mahmoud KGM, Nawito M (2012) Effects of lead exposure on DNA damage and apoptosis in reproductive and vital organs in female rabbits. Glob Vet 9:401–408
Atuadu V, Ben-Azu B, Oyem J, Esom E, Mba C, Nebo K, Ezemeka G, Anibeze C. Adansonia digitata L. leaf extract attenuates lead-induced cortical histoarchitectural changes and oxidative stress in the prefrontal cortex of adult male Wistar rats. Drug Metab Pers Ther. 2020 Oct 21:/j/dmdi.ahead-of-print/dmdi-2020–0116/dmdi-2020–0116.xml. doi: https://doi.org/10.1515/dmdi-2020-01.
Sharma A, Sharma V, Kansal L (2010) Amelioration of lead-induced hepatotoxicity by Allium sativum extracts in Swiss albino mice. Libyan Journal of Medicine 5(1):4621
Velaga MK, Basuri CK, Robinson TKS, Yallapragada PR, Rajanna S, Rajanna B (2014) Ameliorative effects of Bacopa monniera on lead-induced oxidative stress in different regions of rat brain. Drug Chem Toxicol 37(3):357–364
Velaga MK, Yallapragada PR, Williams D, Rajanna S, Bettaiya R (2014) Hydroalcoholic seed extract of Coriandrum sativum (Coriander) alleviates lead-induced oxidative stress in different regions of rat brain. Biol Trace Elem Res 159(1–3):351–363
Harisa GI (2014) Mitigation of lead-induced neurotoxicity by the naringin: erythrocytes as neurons substitute markers. Biol Trace Elem Res 159(1–3):99–106
Nam SM, Seo JS, Go TH, Nahm SS, Chang BJ (2019) Ascorbic acid supplementation prevents the detrimental effects of prenatal and postnatal lead exposure on the purkinje cell and related proteins in the cerebellum of developing rats. Biol Trace Elem Res 190(2):446–456
Shalan MG, Mostafa MS, Hassouna MM, El-Nabi SEH, El-Refaie A (2005) Amelioration of lead toxicity on rat liver with vitamin C and silymarin supplements. Toxicology 206(1):1–15
Winiarska-Mieczan A, Krusiński R, Kwiecien M (2013) Tannic acid influence on lead and cadmium accumulation in the hearts and lungs of rats. Advances in Clinical and Experimental Medicine: Official Organ Wroclaw Medical University 22(5):615–620
Zargar R, Raghuwanshi P, Rastogi A, Koul LA, Khajuria P, Ganai AW, Kour S (2016) Protective and ameliorative effect of sea buckthorn leaf extract supplementation on lead induced hematobiochemical alterations in wistar rats. Veterinary World 9(9):929
Jacobs BP, Browner WS (2000) Ginkgo biloba: a living fossil. Am J Med 108:341–342
Singh B, Kaur P, Gopichand C, Singh BD, Ahuja PS (2008) Biology and chemistry of Ginkgo biloba. Fitoterapia 79:401–418
Liao HJ, Zheng YF, Li HY, Peng GP (2011) Two new ginkogolides from leaves of Ginkgo biloba. Planta Med 77:1818–1821
Ude C, Schubert-Zsilavecz M, Wurglics M (2013) Ginkgo biloba extracts: a review of the pharmacokinetics of the active ingredients. Clin Pharmacokinet 52(9):727–749
Zhang WR, Hayashi T, Kitagawa H (2000) Protective effect of ginkgo extract on rat brain with transient middle cerebral artery occlusion. Neurol Res 22:517–521
Luo Y (2001) Ginkgo biloba neuroprotection: therapeutic implications in Alzheimer’s disease. J Alzheimers Dis 3:401–407
Adebayo O.G., Ben‑Azu B., Ajayi A.M., Wopara I Aduema W., Kolawole T.A., Umoren E.B., Onyeleonu I Ebo O.T., Ajibo D.N., Akpotu A.E., (2021). Gingko biloba abrogate lead-induced neurodegeneration in mice hippocampus: involvement of NF-kB expression, myeloperoxidase activity and pro-inflammatory mediators. Biological trace element research, 1–14.
Ding J, Yu J, Wang C (2005) Ginkgo biloba extract alleviates liver fibrosis induced by CCl4 in rats. Liver Int 25:1224–1232
He SX, Luo JY, Wang YP (2006) Effects of extract from Ginkgo biloba on carbon tetrachloride-induced liver injury in rats. World J Gastroenterol 12:3924–3928
Sener G, Omurtag GZ, Sehirli O (2006) Protective effects of Ginkgo biloba against acetaminophen-induced toxicity in mice. Mol Cell Biochem 283:39–45
Naik SR, Panda VS (2007) Antioxidant and hepatoprotective effects of Ginkgo biloba phytosomes in carbon tetrachloride-induced liver injury in rodents. Liver Int 27:393–399
Mesquita TRR, de Jesus ICG, dos Santos JF, de Almeida GKM, de Vasconcelos CML, Guatimosim S, Macedo FN, dos Santos RV, de Menezes-Filho JER, Miguel-dos-Santos R, Matos PTD, Scalzo S, Santana-Filho VJ, Albuquerque-Júnior RLC, Pereira-Filho RN, Lauton-Santos S (2017) Cardioprotective action of Ginkgo biloba extract against sustained-adrenergic stimulation occurs via activation of M2/NO pathway. Front Pharmacol 8:220
Insha Amin Ishraq Hussain Muneeb U. Rehman Bilal Ahmad Mir Showkat Ahmad Ganaie Sheikh Bilal Ahmad Manzoor Ur Rahman Mir Syed Showkeen Muzamil Azher Arafah Parvaiz Ahmad (2020). Zingerone prevents lead-induced toxicity in liver and kidney tissues by regulating the oxidative damage in Wistar rats. J Food Biochem.00: e13241.
Udefa A.L., Amama E.A., Archibong E.A., Nwangwa J.N., Adama S., Inyang V.U., Inyaka G.U., Aju G.J., Okpa S., Inah I.O., (2020). Antioxidant, anti-inflammatory and anti-apoptotic effects of hydro-ethanolic extract of Cyperus esculentus L. (tigernut) on lead acetate-induced testicular dysfunction in Wistar rats. Biomedicine & Pharmacotherapy 129 (2020) 110491.
Oyewale JO (1992) Effects of temperature and pH on osmotic fragility of erythrocytes of the domestic fowl (Gallus domesticus) and guinea fowl (Numida maleagridis). Res Vet Sci 52(1):1–4
Reid HL, Ugwu AC (1987) A simple technique for rapid determination of plasma viscosity. Nig J Physiol Sci 3:45–48
Ingram GIC (1952) The determination of plasma fibrinogen by the clot-weight method. Biochem J 51(5):583–585
Reitman S, Frankel S (1957) A colorimetric method for the glutamic–pyruvate transaminase. Am J Clin Pathol 28:56–63
Beers RF, Sizer JW (1952) A spectrophotometric method for measuring the breakdown of hydrogen peroxide by catalase. J Biol Chem 195:133–140
McCord JM, Fridovich I (1969) Superoxide dismutase. An enzymic function for erythrocuprein (hemocuprein). J Biol Chem 244:6049–6055
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95:351–358
Asiwe JN, Anachuna KK, Moke EG, Sanusi KO, Okonofua DE, Omeru O, Fasanmade AA (2021) High dietary salt intake alleviates fasting blood glucose in streptozotocin-induced diabetic male Wistar rats. Thai J Pharm Sci 45(3):172–177
Andjelkovic M, Buha Djordjevic A, Antonijevic E, Antonijevic B, Stanic M, Kotur Stevuljevic J, Spasojevic-Kalimanovska V, Jovanovic M, Boricic N, Wallace D, Bulat Z (2019) Toxic effect of acute cadmium and lead exposure in rat blood, liver, and kidney. Int J Environ Res Public Health 16:274
Yuan G, Dai S, Yin Z (2014) Sub-chronic lead and cadmium co-induce apoptosis protein expression in liver and kidney of rats. Int J Clin Exp Pathol 7(6):2905
Abdel-Moneim AM, El-Toweissy MY, Ali AM (2015) Curcumin ameliorates lead induced hemato-biochemical alterations and renal oxidative damage in a rat model. Biol Trace Elem Res 168:206–220
El-Boshy ME, Refaat B, Qasem AH, Khan A, Ghaith M, Almasmoum H, Mahbub A, Almaimani RA (2019) The remedial effect of Thymus vulgaris extract against lead toxicity-induced oxidative stress, hepatorenal damage, immunosuppression, and haematological disorders in rats. Environ Sci Pollut Res Int 26:22736–22746
Aprioku JS, Obianime AW (2014) Evaluation of the effects of Citrus aurantifolia (lime) juice in lead-induced hematological and testicular toxicity in rats. Pharmacologia 5:36–41
Fenga C, Gangemi S, Di Salvatore V, Falzone L, Libra M (2017) Immunological effects of occupational exposure to lead. Mol Med Rep 15:3355–3360
Lawrence DA (1995) Posited mechanisms of metal immunotoxicity. Hum Exp Toxicol 14:114–116
Ercal N, Neal R, Treeratphan P, Lutz PM, Hammond TC, Dennery PA, Spitz DR (2000) A role for oxidative stress in suppressing serum immunoglobulin levels in lead-exposed Fisher 344 rats. Arch Environ Contam Toxicol 39:251–256
Isaac, L.J., Abah, G., Akpan, B., Ekaette, I.U. (2013). Haematological properties of different breeds and sexes of rabbits (p.24–27). Proceedings of the 18th Annual Conference of Animal Science Association of Nigeria.
Alwaleedi SA (2016) Hematobiochemical changes induced by lead intoxication in male and female albino mice. Nat J Physiol Pharm Pharmacol 6:46
Chan PC, Xia Q, Fu PP (2007) Ginkgo biloba leave extract: biological, medicinal, and toxicological effects. J Environ Sci Health C Environ Carcinog Ecotoxicol Rev 25:211–244
He J, Lin J, Li J, Zhang JH, Sun XM, Zeng CM (2008) Dual effects of Ginkgo biloba leaf extract on human red blood cells. Nordic Pharmacol Soc 104:138–144
Abdel Baieth HE (2009) Evaluation of Ginkgo biloba extract on hematological changes affected with hazards of electromagnetic field exposure. Inte J Biomed Sci 5:229–236
Azab A (2014) Hepatoprotective effect of sesame oil against lead induced liver damage in albino mice: Histological and biochemical studies. American Journal of Biological Sciences 2(6–2):1–11
Ibrahim NM, Eweis EA, El-Beltagi HS, Abdel-Mobdy YE (2012) Effect of lead acetate toxicity on experimental male albino rat. Asian Pac J Trop Biomed 20(1):41–46
Mani V, Arivalagan S, Islam Siddique A, Namasivayam N (2017) Antihyperlipidemic and antiapoptotic potential of zingerone on alcohol induced hepatotoxicity in experimental rats. Chem Biol Interact 272:197–206
Cheong, K. O., Shin, D.-S., Bak, J., Lee, C., Kim, K. W., Je, N. K., Moon, J.O. (2016). Hepatoprotective effects of zingerone on carbon tetrachloride-and dimethylnitrosamine induced liver injuries in rats.Archives of Pharmacal Research, 39(2), 279–291.
Siu ER, Mruk DD, Porto CS, Cheng CY (2009) Cadmium-induced testicular injury. Toxicol Appl Pharmacol 238(3):240–249
Hasanein P, Ghafari-Vahed M, Khodadadi I (2017) Effects of isoquinoline alkaloid berberine on lipid peroxidation, antioxidant defense system, and liver damage induced by lead acetate in rats. Redox Reports 22(1):42–50
Tohma, H., Gülçin, İ., Bursal, E., Gören, A. C., Alwasel, S. H., & Köksal, E. (2017). Antioxidant activity and phenolic compounds of ginger (Zingiber officinale Rosc.) determined by HPLC-MS/MS. Journal of Food Measurement and Characterisation, 11(2), 556–566.
Laamech, J., El-Hilaly, J., Fetoui, H., Chtourou, Y., Gouitaa, H., Tahraoui, A., & Lyoussi, B. (2017). Berberis vulgaris L. effects on oxidative stress and liver injury in lead-intoxicated mice. Journal of Complementary and Integrative Medicine, 14(1), 1–14.
Rajan I, Narayanan N, Rabindran R, Jayasree PR, Manish KPR (2013) Zingerone protects against stannous chloride induced and hydrogen peroxide-induced oxidative DNA damage in vitro. Biol Trace Elem Res 155(3):455–459
Reddy YA, Chalamaiah M, Ramesh B, Balaji G, Indira P (2014) Ameliorating activity of ginger (Zingiber officinale) extract against lead induced renal toxicity in male rats. J Food Sci Technol 51(5):908–914
Vander AJ, Mouw DR, Cox J, Johnson B (1979) Lead transport by renal slices and its inhibition by tin. American Journal of Renal Physiology 236(4):F373–F378
Ekong EB, Jaar BG, Weaver VM (2006) Lead-related nephrotoxicity: a review of the epidemiologic evidence. Kidney Int 70(12):2074–2084
Kandemir FM, Yıldırım S, Caglayan C, Kucukler S, Eser G (2019) Protective effects of zingerone on cisplatin-induced nephrotoxicity in female rats. Environ Sci Pollut Res 26(22):22562–22574
Adeyemi O, Ajayi JO, Olajuyin AM, Oloyede OB, Oladiji AT, Oluba OM, Adebayo EA (2009) Toxicological evaluation of the effect of water contaminated with lead, phenol and benzene on liver, kidney and colon of Albino rats. Food Chemistry and Toxicology 47(4):885–887
Renugadevi J, Prabu SM (2010) Cadmium-induced hepatotoxicity in rats and the protective effect of naringenin. Exp Toxicol Pathol 62(2):171–181
Acknowledgements
The authors appreciate the technical assistance rendered during this study by Mr. Kingsley Etim of Department of Physiology and Mr. Saviour Inegbenehi of Department of Biochemistry, PAMO University Medical Sciences, Port Harcourt.
Author information
Authors and Affiliations
Contributions
JNA conceptualised the experiments. BRB, AEA, and 1AO managed the animal experiment; JNA, LCA, HE, and BRB managed the laboratory assays; JNA and TMED and EOA wrote the first draft of the manuscript. All authors read and approved the final draft and submission of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights
The institution, PAMO University of Medical Sciences Animal Research Ethics Committee which agreed with the “Guide to the care and use of laboratory animals in research and teaching” as prescribed in NIH publications volume 25 No.28 revised in 1996 approved the use of animal for this study with approval number PUMS-AREC/028.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asiwe, J.N., Daubry, T.M.E., Okon, I.A. et al. Ginkgo biloba Supplement Reverses Lead (II) Acetate–Induced Haematological Imbalances, Hepatic and Renal Dysfunctions in Male Wistar Rat. Biol Trace Elem Res 200, 5134–5144 (2022). https://doi.org/10.1007/s12011-022-03098-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-022-03098-6