Abstract
Purpose of review
The purpose of this review is to detail the advanced echocardiographic studies that evaluated outcomes in pediatric PH using these advanced imaging techniques: (1) right heart size and function (using 2D and 3D echocardiography), (2) myocardial mechanics, and (3) right ventricular (RV) to pulmonary arterial coupling.
Recent findings
Advanced echocardiographic imaging tools in pediatric PH include RV/left ventricular ratio, 3D echocardiographic assessment of RV volumes and ejection fraction, right atrial and RV strain, and RV-pulmonary arterial coupling ratio that allow for evaluation of clinical outcomes in this patient population. The right atrial to RV axis provides insights to RV diastolic function that has been poorly understood in pediatrics. The RV-pulmonary arterial coupling ratio helps us understand the mechanics of the RV response to afterload.
Summary
The advanced imaging tools provide clinical outcome evaluation in pediatric PH patients and provide insight into the RA-RV axis and the RV-pulmonary circulatory unit.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Echocardiography is the most important noninvasive tool that is used as a routine assessment of pediatric pulmonary hypertension (PH) [1••, 2••, 3, 4•, 5, 6•]. It is used in screening as well as for continued follow-up and medication management [7•]. Conventional imaging includes assessment of anatomy in two-dimensions (2D), hemodynamics via Doppler echocardiography, and qualitative and quantitative evaluation of right ventricular (RV) and left ventricular (LV) function [3, 4•, 5, 7•, 8•, 9••, 10]. The advanced imaging tools in echocardiography include evaluation of right heart size and function, myocardial mechanics, and RV to pulmonary arterial (PA) coupling ratio [11,12,13, 14•, 15]. In recent years, different echocardiography parameters have been identified to be useful in identifying high-risk patients who are likely to develop adverse clinical outcomes [14•, 16•, 17, 18•, 19]. In this review, we will discuss the echocardiographic studies that evaluated outcomes in pediatric PH using these advanced imaging techniques: (1) right heart size and function (using 2D and 3D echocardiography), (2) myocardial mechanics, and (3) RV to PA coupling.
Right heart size and function using 2D and 3D echocardiography
Echocardiographic assessment of right heart size and function can be performed by 2D and 3D echocardiography based on the recent adult and pediatric guidelines [9••, 20••]. Ryan et al. in 1985 derived the eccentricity index to differentiate between volume overload and pressure overload and found that LV deformation of the interventricular septum was greatest in end-systole in patients with RV pressure overload [21]. Eccentricity index > 1 has been shown to correlate well with invasive measurements of pulmonary artery pressure and to be a predictor of adverse outcome in adults [21]. Based on the concept of eccentricity index and septal shift, a RV/LV ratio in end systole to incorporate the RV in pediatric PH patients was derived (Fig. 1a) [22•]. This study compared 80 normal pediatric patients with 84 abnormal pediatric PH patients. RV/LV ratio in end-systole was higher in PH patients compared to controls and RV/LV correlated with hemodynamic measurements in catheterization within 48 h of cardiac catheterization [22•]. RV/LV > 1 was associated with an increased risk for an adverse event including initiation of intravenous prostacyclin therapy, atrial septostomy, death, or transplantation [22•]. For every increase of 0.1 units in RV/LV ratio, the hazard increased by 10% [22•].
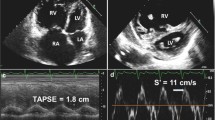
Advanced echocardiographic imaging in pediatric pulmonary hypertension. a The right ventricular (RV)/left ventricular (LV) ratio. b Three-dimensional imaging of the RV: volumes, ejection fraction, and strain are shown in the pediatric pulmonary hypertension patient. c Right atrial function: ɛS = reservoir function, ɛE = conduit function, and ɛA = pump function. d Sans equation simplifies the RV-pulmonary arterial coupling ratio (Ees/Ea) into a volumetric method of stroke volume (SV)/end-systolic volume (ESV).
With the advent of 3D echocardiography, RV volumes and function (Fig. 1b) can be measured more accurately to encompass the difficult geometric RV shape. RV volumes and function have been shown to correlate well to cardiac magnetic resonance imaging (CMRI) with some underestimation of RV volumes [9••, 23, 24•]. Both normal values of RV volumes and function have been reported in adults and pediatrics [25, 26•]. Emerging studies have confirmed the prognostic value of 3D-derived RV volumes and ejection fraction (EF) in patients with PH and RV dysfunction [14•, 27•]. In a study with 96 pediatric PH patients compared to 40 normal controls, the PH patients had higher RV volumes and lower RVEF compared to controls [14•]. The RVEF had the highest area under the curve (0.83, with sensitivity of 90% and specificity of 67% with a RVEF cut-off value of 43%) [14•]. And when comparing to conventional indices of RV function such as tricuspid annular plane systolic excursion (TAPSE), the RV volumes and EF were prognostic in evaluating clinical outcomes whereas TAPSE was not prognostic [14•]. Nagata et al. found similar results in adult studies that RVEF was independently associated with cardiac outcomes in patients with diverse backgrounds and that RVEF offered incremental value over clinical risk factors and other conventional echocardiographic parameters for predicting future adverse outcomes [27•].
Right heart myocardial mechanics
Speckle tracking has become a clinical standard for assessing RV systolic function from a RV-focused apical view. Strain measures myocardial deformation whereas its time derivative, strain rate, defines the rate of deformation of myocardium over time. RV regional and global strain can be measured. Normal values of adult and pediatric RV strain have also been reported [9••, 28, 29, 30•, 31]. In 575 adult patients with known or suspected PH, Fine et al. demonstrated that RV strain was a strong predictor of survival even after adjusting for pulmonary artery pressures, pulmonary vascular resistance, and right atrial pressure [32•]. RV longitudinal systolic strain provided incremental prognostic valve over conventional clinical and echocardiographic variables [32•]. Hardegree et al. showed that RV free wall longitudinal strain can be used as a quantitative assessment of RV systolic function in adult PH patients and that an improvement of RV systolic strain ≥ 5% while on therapy was found to be an independent predictor of improved survival [33]. Okumura et al. subsequently demonstrated in pediatric idiopathic pulmonary artery hypertension (PAH) that RV global longitudinal strain may be a more sensitive parameter to detect early RV dysfunction and may be better at predicting outcomes [18•]. They demonstrated that if the RV strain does not improve over time after treatment, these patients have worse outcomes [18•]. Interestingly, similar to RV strain, TAPSE was worse in non-survivors but the difference in TAPSE over time between the survivors and non-survivors was not as divergent as between RV strain in a 5-year follow-up [18•]. RV strain can also be derived from 3D echocardiography acquisitions with the post-processing software demonstrating RV longitudinal free-wall and septal strain (Fig. 1b) [14•, 34]. Vitarelli et al. demonstrated that in chronic PH, both 2D and 3D strain parameters were better associated with RV failure hemodynamics than conventional echocardiographic indices [34]. In our pediatric PH patients, RV longitudinal free-wall strain was prognostic of adverse clinical outcomes [14•].
Right atrial (RA) mechanics can also be studied with speckle tracking echocardiography. The components of RA function can be studied and provide insight into RV diastolic function. There are three components to RA function: reservoir, conduit, and pump function (Fig. 1c). The reservoir function is maximal atrial filling, the conduit function is passive emptying of the RA to the RV, and the pump function is the active RA emptying into the RV also known as atrial kick [35•]. Interaction of RA-RV strain can be studied and are interrelated. Mendes et al. demonstrated that in normal patients with normal RV strain where there is high ventricular deformation, there is high atrial deformation as the RV pulls down on the RA [36]. With low RV deformation, there is low atrial strain [36]. Querejeta Roca et al. studied RA function in patients with PAH and found that RA reservoir and passive conduit functions are impaired in PAH, independent of RA size and pressure, and likely reflect RV failure and overload [37•]. In adult studies of 108 idiopathic PAH patient, D’Alto et al. demonstrated that patients with worse reservoir function have worse prognosis [38]. In our study with 66 pediatric PH patients compared to 36 normal controls, all phases of the RA function were depressed in PH patients and that RA reservoir, pump function, and minimum volumes were predictors of adverse clinical events [16•]. This study highlights the difference between pathophysiologic difference between adults and children [16•]. In adults, the pump function is more affected at the time of the diagnosis but it is more preserved in children. This preservation of atrial contractile function is important in maintaining RV filling as the RV gets stiffer and less compliant through disease progression. Similar pediatric study showed that the active right atrial emptying fraction predicts reduced survival in PAH patients [39•]. Assessment of atrial size and function may allow for assessment of RV diastolic function as traditional echocardiographic indices for RV diastolic function in pediatrics are still poorly validated [40]. RA function also allows for understanding of RA-RV interactions in pediatric PH; however, RA function cannot be used in the setting atrial level shunts or significant tricuspid regurgitation. Currently, RA function needs to be standardized as the tools of speckle tracking to evaluate RA function are taken from left atrial strain and normal pediatric values are still lacking.
Right ventricular pulmonary arterial coupling
The relationship between RV contractility and RV afterload is often referred to as RV-PA coupling. The main cause of mortality in PH is right ventricular (RV) failure with inability of the RV to maintain cardiac output with increasing arterial afterload, thus decoupling of the ventricular-pulmonary circulatory system [41••, 42]. From invasive pressure-volume loop analysis, the most widely accepted index of RV-PA coupling uses the ratio between ventricular elastance (Ees; a measure of contractility) to arterial elastance (Ea; a measure of afterload) [43••, 44]. The optimal RV-PA coupling allows for flow ejection at a minimal energy cost and corresponds to an Ees/Ea ratio of 1.5 to 2.0 [43••]. In patients with PH, the RV adapts to the increase in pulmonary arterial afterload by increasing Ees to preserve Ees/Ea [45]. Surrogates of Ees/Ea ratio using noninvasive methods such as the ratio between RV systolic pulmonary artery pressure (sPAP) and RV end-systolic area, TAPSE/sPAP, or RV strain/sPAP have been proposed [46, 47, 48•, 49]. Guazzi et al. demonstrated that the ratio of TAPSE/sPAP correlates with invasive coupling index of Ees/Ea and with compliance, representing an independent predictor of worse outcome in heart failure with preserved EF [50]. However, this TAPSE/sPAP is difficult to use in children because the noninvasive estimation of sPAP is based on Doppler velocity of tricuspid regurgitation by Bernoulli’s equation, an approach in pediatric patients that may at times imprecisely correlate with cardiac catheterization pressures [51]. Others have proposed using pulmonary acceleration time (PAAT) to replace sPAP in the TAPSE/sPAP ratio as PAAT has been demonstrated as a reliable estimate of invasive PAP in the absence of reliable tricuspid regurgitation [52•]. The ratio of TAPSE/PAAT as a surrogate of Ees/Ea warrants future investigation in children [53].
Another estimate of RV-PA coupling ratio is the noninvasive volumetric estimate proposed by Sanz [54•]. In this method, the coupling ratio is further simplified for pressure and expressed as stroke volume (SV)/end-systolic volume (ESV) (Fig. 1d) [54•]. This SV/ESV derived from CMRI has been demonstrated in adults with PH as an independent predictor of outcome and has been shown to be more sensitive than RV EF to changes in function early in the disease [55]. In 17 pediatric PH patients, Truong et al. demonstrated the feasibility of SV/ESV ratio from CMRI and found correlation to cardiac catheterization evaluation of the RV-PA coupling ratio using the single beat method [56•]. The volumetric estimate of the RV-PA coupling using SV/ESV ratio can be derived from 3D echocardiography as 3D echocardiography is readily available and more cost effective. This SV/ESV ratio has been shown in adults with PH to correlate with right heart catheterization-CMRI-derived RV-PA coupling ratio [57•]. Their study suggests further evaluation of outcomes using this volumetric estimate of RV-PA coupling ratio in the future [57•]. We have embarked on the study using SV/ESV derived from 3D echocardiography to evaluate pediatric PH patients compared to controls and have found a prognostic value of this SV/ESV ratio to adverse clinical events [58].
Conclusion
The advanced imaging tools available to evaluated pediatric PH patients provide insight into the RA-RV axis and the RV-PA coupling. 3D echocardiography provides volumetric and functional assessment that allows for quantitative assessment of the right heart without geometric assumptions. Myocardial mechanics using speckle tracking imaging provide assessment of the RA and RV function and provide further insights into the diastolic function of the right heart that have been poorly understood in the pediatric PH patients. Lastly, the RV-PA coupling ratio further illustrates the interaction of the RV to the vasculature in the pulmonary circulatory unit. These advances are crucial in delineating the outcomes in pediatric PH patients and to the understanding of the RV to pulmonary unit in children with PH.
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
••Abman SH, Hansmann G, Archer SL, Ivy DD, Adatia I, Chung WK, et al. Pediatric Pulmonary Hypertension: Guidelines From the American Heart Association and American Thoracic Society. Circulation. 2015;132(21):2037–99 An important guideline in pediatric pulmonary hypertension.
••Ivy DD, Abman SH, Barst RJ, Berger RM, Bonnet D, Fleming TR, et al. Pediatric pulmonary hypertension. J Am Coll Cardiol. 2013;62(25 Suppl):D117–26 An important update in pediatric pulmonary hypertension.
Bossone E, Ferrara F, Grunig E. Echocardiography in pulmonary hypertension. Curr Opin Cardiol. 2015;30(6):574–86.
•D’Alto M, Bossone E, Opotowsky AR, Ghio S, Rudski LG, Naeije R. Strengths and weaknesses of echocardiography for the diagnosis of pulmonary hypertension. Int J Cardiol, 2018;263:177–83.Important in describing the strength and weakness of echocardiography in pulmonary hypertension.
D’Alto M, Romeo E, Argiento P, Di Salvo G, Badagliacca R, Cirillo AP, et al. Pulmonary arterial hypertension: the key role of echocardiography. Echocardiography. 2015;32(Suppl 1):S23–37.
•Kasprzak JD, Huttin O, Wierzbowska-Drabik K, Selton-Suty C. Imaging the Right Heart-Pulmonary Circulation Unit: The Role of Ultrasound. Heart Fail Clin. 2018;14(3):361–76 Describes echocardiography in right heart and pulmonary circulation unit.
•Jone PN, Ivy DD. Echocardiography in pediatric pulmonary hypertension. Front Pediatr. 2014;2:124 Summary of echocardiography in pediatric pulmonary hypertension.
•Koestenberger M, Friedberg MK, Nestaas E, Michel-Behnke I, Hansmann G. Transthoracic echocardiography in the evaluation of pediatric pulmonary hypertension and ventricular dysfunction. Pulm Circ. 2016;6(1):15–29 Summary of echocardiography in pediatric pulmonary hypertension.
••Rudski LG, Lai WW, Afilalo J, Hua L, Handschumacher MD, Chandrasekaran K, et al. Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. J Am Soc Echocardiogr. 2010;23(7):685–713 quiz 86–8 An important guideline in right heart echocardiographic evaluation in adults.
Ploegstra MJ, Roofthooft MT, Douwes JM, Bartelds B, Elzenga NJ, van de Weerd D, et al. Echocardiography in pediatric pulmonary arterial hypertension: early study on assessing disease severity and predicting outcome. Circ Cardiovasc Imaging. 2015;8(1).
Ferrara F, Gargani L, Ostenfeld E, D’Alto M, Kasprzak J, Voilliot D, et al. Imaging the right heart pulmonary circulation unit: Insights from advanced ultrasound techniques. Echocardiography. 2017;34(8):1216–31.
Rengier F, Melzig C, Derlin T, Marra AM, Vogel-Claussen J. Advanced imaging in pulmonary hypertension: emerging techniques and applications. Int J Card Imaging. 2018.
Jone PN, Patel SS, Cassidy C, Ivy DD. Three-dimensional Echocardiography of Right Ventricular Function Correlates with Severity of Pediatric Pulmonary Hypertension. Congenit Heart Dis. 2016;11(6):562–9.
•Jone PN, Schafer M, Pan Z, Bremen C, Ivy DD. 3D echocardiographic evaluation of right ventricular function and strain: a prognostic study in pediatric pulmonary hypertension. Eur Heart J Cardiovasc Imaging. 2018;19:1026–33 Prognostic study in pediatric pulmonary hypertension using 3D echocardiography and strain.
Kubba S, Davila CD, Forfia PR. Methods for Evaluating Right Ventricular Function and Ventricular-Arterial Coupling. Prog Cardiovasc Dis. 2016;59(1):42–51.
•Jone PN, Schafer M, Li L, Craft M, Ivy DD, Kutty S. Right Atrial Deformation in Predicting Outcomes in Pediatric Pulmonary Hypertension. Circ Cardiovasc Imaging. 2017;10(12) Prognostic study in pediatric pulmonary hypertension using right atria strain.
Alkon J, Humpl T, Manlhiot C, McCrindle BW, Reyes JT, Friedberg MK. Usefulness of the right ventricular systolic to diastolic duration ratio to predict functional capacity and survival in children with pulmonary arterial hypertension. Am J Cardiol. 2010;106(3):430–6.
•Okumura K, Humpl T, Dragulescu A, Mertens L, Friedberg MK. Longitudinal assessment of right ventricular myocardial strain in relation to transplant-free survival in children with idiopathic pulmonary hypertension. J Am Soc Echocardiogr. 2014;27(12):1344–51 Prognostic study in pediatric pulmonary hypertension using right ventricular strain.
Kassem E, Humpl T, Friedberg MK. Prognostic significance of 2-dimensional, M-mode, and Doppler echo indices of right ventricular function in children with pulmonary arterial hypertension. Am Heart J. 2013;165(6):1024–31.
••Simpson J, Lopez L, Acar P, Friedberg MK, Khoo NS, Ko HH, et al. Three-dimensional Echocardiography in Congenital Heart Disease: An Expert Consensus Document from the European Association of Cardiovascular Imaging and the American Society of Echocardiography. J Am Soc Echocardiogr. 2017;30(1):1–27 An important guideline in assessment of right ventricular volume and function in pediatrics.
Ryan T, Petrovic O, Dillon JC, Feigenbaum H, Conley MJ, Armstrong WF. An echocardiographic index for separation of right ventricular volume and pressure overload. J Am Coll Cardiol. 1985;5(4):918–27.
•Jone PN, Hinzman J, Wagner BD, Ivy DD, Younoszai A. Right ventricular to left ventricular diameter ratio at end-systole in evaluating outcomes in children with pulmonary hypertension. J Am Soc Echocardiogr. 2014;27(2):172–8 Prognostic study in pediatric pulmonary hypertension using new index of RV/LV ratio.
Shimada YJ, Shiota M, Siegel RJ, Shiota T. Accuracy of right ventricular volumes and function determined by three-dimensional echocardiography in comparison with magnetic resonance imaging: a meta-analysis study. J Am Soc Echocardiogr. 2010;23(9):943–53.
•Muraru D, Spadotto V, Cecchetto A, Romeo G, Aruta P, Ermacora D, et al. New speckle-tracking algorithm for right ventricular volume analysis from three-dimensional echocardiographic data sets: validation with cardiac magnetic resonance and comparison with the previous analysis tool. Eur Heart J Cardiovasc Imaging. 2016;17(11):1279–89 Important study in validating 3D echocardiography to cardiac magnetic resonance imaging.
Maffessanti F, Muraru D, Esposito R, Gripari P, Ermacora D, Santoro C, et al. Age-, body size-, and sex-specific reference values for right ventricular volumes and ejection fraction by three-dimensional echocardiography: a multicenter echocardiographic study in 507 healthy volunteers. Circ Cardiovasc Imaging. 2013;6(5):700–10.
•Laser KT, Karabiyik A, Korperich H, Horst JP, Barth P, Kececioglu D, et al. Validation and Reference Values for Three-Dimensional Echocardiographic Right Ventricular Volumetry in Children: A Multicenter Study. J Am Soc Echocardiogr. 2018;31(9):1050–63 Important study to establish pediatric normal right ventricular volumes and function.
•Nagata Y, Wu VC, Kado Y, Otani K, Lin FC, Otsuji Y, et al. Prognostic Value of Right Ventricular Ejection Fraction Assessed by Transthoracic 3D Echocardiography. Circ Cardiovasc Imaging. 2017;10(2) Incremental value of right ventricular ejection fraction using 3D echocardiography.
Morris DA, Krisper M, Nakatani S, Kohncke C, Otsuji Y, Belyavskiy E, et al. Normal range and usefulness of right ventricular systolic strain to detect subtle right ventricular systolic abnormalities in patients with heart failure: a multicentre study. Eur Heart J Cardiovasc Imaging. 2017;18(2):212–23.
Muraru D, Onciul S, Peluso D, Soriani N, Cucchini U, Aruta P, et al. Sex- and Method-Specific Reference Values for Right Ventricular Strain by 2-Dimensional Speckle-Tracking Echocardiography. Circ Cardiovasc Imaging. 2016;9(2):e003866.
•Levy PT, Sanchez Mejia AA, Machefsky A, Fowler S, Holland MR, Singh GK. Normal ranges of right ventricular systolic and diastolic strain measures in children: a systematic review and meta-analysis. J Am Soc Echocardiogr. 2014;27(5):549–60 e3 Describes normal right ventricular strain in pediatrics.
Levy PT, El-Khuffash A, Patel MD, Breatnach CR, James AT, Sanchez AA, et al. Maturational Patterns of Systolic Ventricular Deformation Mechanics by Two-Dimensional Speckle-Tracking Echocardiography in Preterm Infants over the First Year of Age. J Am Soc Echocardiogr. 2017;30(7):685–98 e1.
•Fine NM, Chen L, Bastiansen PM, Frantz RP, Pellikka PA, Oh JK, et al. Outcome prediction by quantitative right ventricular function assessment in 575 subjects evaluated for pulmonary hypertension. Circ Cardiovasc Imaging. 2013;6(5):711–21 Prognostic study in pulmonary hypertension using right ventricular strain.
Hardegree EL, Sachdev A, Villarraga HR, Frantz RP, McGoon MD, Kushwaha SS, et al. Role of serial quantitative assessment of right ventricular function by strain in pulmonary arterial hypertension. Am J Cardiol. 2013;111(1):143–8.
Vitarelli A, Mangieri E, Terzano C, Gaudio C, Salsano F, Rosato E, et al. Three-dimensional echocardiography and 2D-3D speckle-tracking imaging in chronic pulmonary hypertension: diagnostic accuracy in detecting hemodynamic signs of right ventricular (RV) failure. J Am Heart Assoc. 2015;4(3):e001584.
•Gaynor SL, Maniar HS, Prasad SM, Steendijk P, Moon MR. Reservoir and conduit function of right atrium: impact on right ventricular filling and cardiac output. Am J Physiol Heart Circ Physiol. 2005;288(5):H2140–5 Important concepts of atrial function and the impact it has to the right ventricular filling pressure.
Mendes L, Cardim N. Right atrial function with speckle tracking echocardiography: Do we really need it? Rev Port Cardiol. 2017;36(12):901–4.
•Querejeta Roca G, Campbell P, Claggett B, Solomon SD, Shah AM. Right Atrial Function in Pulmonary Arterial Hypertension. Circ Cardiovasc Imaging. 2015;8(11):e003521 discussion e. Prognostic study in pulmonary hypertension using right atrial strain.
D’Alto M, D’Andrea A, Di Salvo G, Scognamiglio G, Argiento P, Romeo E, et al. Right atrial function and prognosis in idiopathic pulmonary arterial hypertension. Int J Cardiol. 2017;248:320–5.
•Kumar S, Vadlamudi K, Kaddoura T, Bobhate P, Goot BH, Elgendi M, et al. Active right atrial emptying fraction predicts reduced survival and increased adverse events in childhood pulmonary arterial hypertension. Int J Cardiol. 2018;271:306–11 Prognostic study in pediatric pulmonary hypertension using right atrial function.
Mertens LL. Right Atrial Contractile Function in Pediatric Pulmonary Hypertension: A Novel Marker for Disease Severity? Circ Cardiovasc Imaging. 2017;10(12).
••Vonk Noordegraaf A, Westerhof BE, Westerhof N. The Relationship Between the Right Ventricle and its Load in Pulmonary Hypertension. J Am Coll Cardiol. 2017;69(2):236–43 An important concept and mechanism of right ventricular function in relation to afterload in pulmonary hypertension.
Vonk Noordegraaf A, Haddad F, Bogaard HJ, Hassoun PM. Noninvasive imaging in the assessment of the cardiopulmonary vascular unit. Circulation. 2015;131(10):899–913.
••Vonk-Noordegraaf A, Haddad F, Chin KM, Forfia PR, Kawut SM, Lumens J, et al. Right heart adaptation to pulmonary arterial hypertension: physiology and pathobiology. J Am Coll Cardiol. 2013;62(25 Suppl):D22–33 Describes mechanism of right ventricular function in relation to afterload in pulmonary hypertension.
Naeije R, Brimioulle S, Dewachter L. Biomechanics of the right ventricle in health and disease (2013 Grover Conference series). Pulm Circ. 2014;4(3):395–406.
Kuehne T, Yilmaz S, Steendijk P, Moore P, Groenink M, Saaed M, et al. Magnetic resonance imaging analysis of right ventricular pressure-volume loops: in vivo validation and clinical application in patients with pulmonary hypertension. Circulation. 2004;110(14):2010–6.
Claessen G, La Gerche A, Voigt JU, Dymarkowski S, Schnell F, Petit T, et al. Accuracy of Echocardiography to Evaluate Pulmonary Vascular and RV Function During Exercise. JACC Cardiovasc Imaging. 2016;9(5):532–43.
Pratali L, Allemann Y, Rimoldi SF, Faita F, Hutter D, Rexhaj E, et al. RV contractility and exercise-induced pulmonary hypertension in chronic mountain sickness: a stress echocardiographic and tissue Doppler imaging study. JACC Cardiovasc Imaging. 2013;6(12):1287–97.
•Guazzi M, Bandera F, Pelissero G, Castelvecchio S, Menicanti L, Ghio S, et al. Tricuspid annular plane systolic excursion and pulmonary arterial systolic pressure relationship in heart failure: an index of right ventricular contractile function and prognosis. Am J Physiol Heart Circ Physiol. 2013;305(9):H1373–81 This study uses a new noninvasive index of right ventricular-pulmonary arterial ratio to evaluate patients with heart failure.
Iacoviello M, Monitillo F, Citarelli G, Leone M, Grande D, Antoncecchi V, et al. Right ventriculo-arterial coupling assessed by two-dimensional strain: A new parameter of right ventricular function independently associated with prognosis in chronic heart failure patients. Int J Cardiol. 2017;241:318–21.
Guazzi M, Dixon D, Labate V, Beussink-Nelson L, Bandera F, Cuttica MJ, et al. RV Contractile Function and its Coupling to Pulmonary Circulation in Heart Failure With Preserved Ejection Fraction: Stratification of Clinical Phenotypes and Outcomes. JACC Cardiovasc Imaging. 2017;10(10 Pt B):1211–21.
Groh GK, Levy PT, Holland MR, Murphy JJ, Sekarski TJ, Myers CL, et al. Doppler echocardiography inaccurately estimates right ventricular pressure in children with elevated right heart pressure. J Am Soc Echocardiogr. 2014;27(2):163–71.
•Levy PT, Patel MD, Groh G, Choudhry S, Murphy J, Holland MR, et al. Pulmonary Artery Acceleration Time Provides a Reliable Estimate of Invasive Pulmonary Hemodynamics in Children. J Am Soc Echocardiogr. 2016;29(11):1056–65 Describes pulmonary acceleration time can estimate invasive pulmonary hemodynamics in children.
Levy PT, El Khuffash A, Woo KV, Singh GK. Right Ventricular-Pulmonary Vascular Interactions: An Emerging Role for Pulmonary Artery Acceleration Time by Echocardiography in Adults and Children. J Am Soc Echocardiogr. 2018;31(8):962–4.
•Sanz J, Garcia-Alvarez A, Fernandez-Friera L, Nair A, Mirelis JG, Sawit ST, et al. Right ventriculo-arterial coupling in pulmonary hypertension: a magnetic resonance study. Heart. 2012;98(3):238–43 First study that uses the volumetric estimate of right ventricular- pulmonary arterial coupling ratio.
Vanderpool RR, Pinsky MR, Naeije R, Deible C, Kosaraju V, Bunner C, et al. RV-pulmonary arterial coupling predicts outcome in patients referred for pulmonary hypertension. Heart. 2015;101(1):37–43.
•Truong U, Patel S, Kheyfets V, Dunning J, Fonseca B, Barker AJ, et al. Non-invasive determination by cardiovascular magnetic resonance of right ventricular-vascular coupling in children and adolescents with pulmonary hypertension. J Cardiovasc Magn Reson. 2015;17:81 First pediatric study that uses the volumetric estimate of right ventricular- pulmonary arterial coupling ratio to correlate to cardiac catheterization measurements.
•Aubert R, Venner C, Huttin O, Haine D, Filippetti L, Guillaumot A, et al. Three-Dimensional Echocardiography for the Assessment of Right Ventriculo-Arterial Coupling. J Am Soc Echocardiogr. 2018;31(8):905–15 First study that uses 3D echocardiography to assess right ventricular to pulmonary arterial coupling ratio and compared it to invasive hemodynamic measurements.
Jone PN, Schäfer M, Pan Z, Ivy DD. Right ventricular-arterial coupling ratio derived from 3-dimensional echocardiography predicts outcomes in pediatric pulmonary hypertension. Circ Cardiovasc Imaging. 2019;12(1):e008176.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pediatric and Congenital Heart Disease
Rights and permissions
About this article
Cite this article
Jone, PN., Ivy, D.D. Comprehensive Noninvasive Evaluation of Right Ventricle-Pulmonary Circulation Axis in Pediatric Patients with Pulmonary Hypertension. Curr Treat Options Cardio Med 21, 6 (2019). https://doi.org/10.1007/s11936-019-0710-y
Published:
DOI: https://doi.org/10.1007/s11936-019-0710-y