Abstract
Purpose of Review
This review aims to summarize (i) the latest evidence on cranial neural crest cells (CNCC) contribution to craniofacial development and ossification; (ii) the recent discoveries on the mechanisms responsible for their plasticity; and (iii) the newest procedures to ameliorate maxillofacial tissue repair.
Recent Findings
CNCC display a remarkable differentiation potential that exceeds the capacity of their germ layer of origin. The mechanisms by which they expand their plasticity was recently described. Their ability to participate to craniofacial bone development and regeneration open new perspectives for treatments of traumatic craniofacial injuries or congenital syndromes.
Summary
These conditions can be life-threatening, require invasive maxillofacial surgery and can leave deep sequels on our health or quality of life. With accumulating evidence showing how CNCC-derived stem cells potential can ameliorate craniofacial reconstruction and tissue repair, we believe a deeper understanding of the mechanisms regulating CNCC plasticity is essential to ameliorate endogenous regeneration and improve tissue repair therapies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The craniofacial skeleton is a crucial component of vertebrate development. It is the structure that protects the brain, and it is essential for respiration, food intake and communication. Additionally, the craniofacial skeleton shapes our face, which is one major definition of our very self. Given its essential functions, congenital craniofacial syndromes – which represent a third of all congenital malformations within the human population [1] – or traumatic injuries to the head skeleton – can have a profound impact on our health and quality of life. When available, treatments of such syndromes or trauma require heavy maxillo-facial surgeries and reconstruction. Regenerative medicine has made tremendous progress in developing treatments and procedures to enhance craniofacial tissue repair in patients. Most commonly used procedures include autologous bone transplantation [2, 3], bone tissue engineering techniques [4, 5] including bone distraction – whereby new bone is generated by applying stress (stretching) to the endogenous bone tissue [6] – and more recently stem cell-based therapies [7, 8]. However, these techniques present the risk of generating unsuitable structures (with ectopic bone formation), relatively poor integration of the new graft or cells within the existing bone and the surrounding soft tissues and they are limited by the size of tissue to replace. Stem cell-based therapy bears an additional risk of genetic and epigenetic mutations which can promote tumor formation [9••, 10, 11].
The repair of severely damaged or missing bones should ideally occur through the induction of an endogenous regenerative response, alleviating the need to harvest tissue from the patient or a donor, and avoiding additional issues such as rejection of the tissue transplant. Moreover, endogenous regeneration results in the formation of a structure (i) similar in pattern to the original anatomy and (ii) better integrated within the native tissues including the surrounding muscles, nerves, and vasculature. Data from regenerative species show that controlled cell dedifferentiation is an essential determinant to insure an adequate endogenous regenerative response [12,13,14]. Understanding how cell plasticity is regulated is then crucial to enhance tissue resident stem cells mobilization and expansion, reduce the tumorigenic risks and altogether promote an efficient endogenous regeneration.
The majority of craniofacial bones derive from cranial neural crest cells (CNCC) – a transient stem cell-like population arising in the most rostral part of the embryo soon after gastrulation [15, 16]. Within the ectoderm lineage, at the border between the neural plate and the surface ectoderm, CNCC are induced as an epithelial cell type [17, 18], that subsequently undergoes an epithelial-to-mesenchymal transition (EMT). CNCC then delaminate from the dorsal epithelium and migrate dorso-ventrally through the embryo to populate various locations in the craniofacial complex where they differentiate into diverse cell types [17, 19]. CNCC present an extraordinary differentiation potential since they generate not only ectoderm derivatives, such as neurons, glia and melanocytes, but also give rise to cells canonically associated with the mesoderm such as bones, cartilage and smooth muscles – also referred to as ectomesenchyme [17, 20] (Fig. 1). Thus, CNCC “break” the rules set during gastrulation as they generate derivatives that extend beyond the potential of their germ layer of origin [21]. This unique differentiation potential can be explained by the fact that CNCC express pluripotency programs at the onset of their development [22, 23]. Furthermore, it was recently shown that CNCC are able to reactivate Oct4 and the associated pluripotency programs [24•, 25••] during their formation. Together, these studies suggest that a deeper understanding of how CNCC regulate the expression of pluripotency programs could unveil new strategies to stimulate cell plasticity in vivo during post-natal tissue repair. Future regenerative therapies will need to recapitulate these processes to enhance endogenous regeneration and ameliorate craniofacial tissue repair.
In this review we will briefly summarize how CNCC contribute to craniofacial bone development and highlight the newest findings regarding transcriptional regulation of ossification. We will focus on the recent discovery on the origin of CNCC remarkable plasticity and finally, we will question how this plasticity could be used to enhance craniofacial bone regeneration and discuss on the latest procedures enhancing craniofacial bone healing.
Given the limitation of words, we will only focus on the cranial neural crest, even though accumulating evidence suggest that the trunk neural crest could also have a skeletogenic capacity in vivo [26].
Neural Crest Contribution to the Craniofacial Skeleton
During embryogenesis bone can either form via the endochondral ossification process, where mesenchymal progenitors form a cartilaginous template that is gradually replaced by bone tissue, or intramembranous ossification, during which mesenchymal cells directly differentiate into osteoblasts, with no cartilaginous intermediate. Intramembranous bones are predominant in the head forming the cranial vault together with most bones of the face. The intramembranous ossification process starts in utero and ends at different postnatal times depending on the type of bone. For example, the skull bones are not fully ossified at birth allowing the postnatal growth and development of the brain. The cells that take part in the endochondral and intramembranous ossification processes to build the skeleton – the chondrocytes and osteoblasts – are primarily of mesodermal origin. Yet, some facial bones, as well as the endocranium, are derived from CNCC [16]. Development of the craniofacial skeleton requires the precise differentiation of CNCC into osteoblasts or chondrocytes. Following CNCC migration and colonization of the facial prominences and branchial arches, CNCC aggregate, condense, and differentiate into a common osteochondral progenitor and then into more differentiated chondrocytes or osteoblasts [27]. The molecular regulations orchestrating craniofacial ossification were recently reviewed in great details [28]. Harmonious craniofacial ossification requires the precise action of CNCC intrinsic transcription factors such as SOX9, RUNX2 and MSX1/2 in association with extrinsic inputs that include fibroblast growth factor (FGF), Wingless-related integration site (WNT) and Transforming growth factor/Bone morphogenetic protein (TGFβ/BMP) signaling pathways (Fig. 1). Thus, gene expression and signaling pathways must be specifically activated and terminated in the correct location at the proper developmental time to ensure a bona fide craniofacial development. Recent studies further exemplified that inaccurate regulation of gene expression in CNCC leads to severe craniofacial defect. A mouse model constitutively activating the activin A receptor type I (ACVR1) to enhance BMP signaling in CNCC results in ectopic cartilage formation in the craniofacial region [29•]. The study further showed that the increased BMP signaling inhibits autophagy via the mTORC1 pathway and blocks the autophagic degradation of β-catenin, causing CNCC to adopt a chondrogenic identity. This phenotype was then rescued by inhibiting mTORC1 signaling to reactivate the Wnt/β-catenin signaling pathway [29•]. mTORC1 was also shown to mediate the function of the acetyltransferase GCN5 – a highly conserved enzyme and potent activator of chondrocyte maturation – during craniofacial development [30]. Interestingly in this context, GCN5 is not acting as an epigenetic regulator but probably via direct activation of mTORC1 pathway [30]. Epigenetic regulation also plays a role in the CNCC ossification. In fact, inhibition of KMT2D function – a histone methylase which mutations are associated with Kabuki syndrome congenital craniofacial disorder – in the neural crest lineage alters osteochondral progenitor differentiation and results in craniofacial hypoplasia [31]. We have also demonstrated a link between the epigenetic modulator Ten eleven translocation enzyme 1 (TET1) and chondrogenic differentiation [32]. Loss of TET1 expression impairs chondrogenesis via tissue-specific changes in 5-hydroxymethylcytosine (5hmC) landscape and reduces the expression of cartilage markers. It remains to be established if this mechanism has a direct impact on CNCC. A recent breakthrough study found that in the neural crest lineage, mutation of the tumor suppressor Brca1 resulted in neonatal death of the mutant animals which presented with a cleft palate and reduced skull due to the reduction in size of craniofacial bones. The reduction in bones size was not due to osteogenic differentiation but by a strong defect in osteogenic proliferation and survival due to an increased DNA damage in skeletogenic precursor cells as demonstrated by the inhibition of p53 which is sufficient to rescue the Brca1 mutant phenotype in vivo [33].
Balance between osteogenesis and chondrogenesis is essential for correct development of the craniofacial skeleton. Using mice deficient for Yap and Taz in the neural crest lineage it was demonstrated this pathway promotes osteogenic genes expression while repressing chondrogenic fate via the action of the Wnt/β-catenin pathway. The Yap/Taz signaling pathway is thus involved in regulating this equilibrium and resulting mutants presented with cranial bone defects and ectopic cartilage formation [34•]. Gene regulatory networks orchestrating bone and cartilage formation and differentiation have been and are still being dissected and characterized in great details [35] which represent a great resource to find potential new strategies to stimulate osteo- and chondrogenesis during bone repair. Nevertheless, the mechanisms conferring CNCC its remarkable plasticity – with their capacity to generate cell types that extend beyond their ectoderm germ layer origin – was only recently uncovered and needs to be explored in more depth.
Origin of CNCC Cellular Plasticity
CNCC have a much broader differentiation potential than their ectodermal lineage of origin and have been challenging the three-germ layer theory for almost a century (history of neural crest biology has recently been reviewed in [36]). Several pieces of evidence have demonstrated and confirmed the contribution of CNCC in the formation of the cranial cartilage and bone, but many key questions are still open, primarily concerning the mechanisms through which these cells reach their final skeletogenic fate.
Pioneer studies using fluorescent intracellular dye to label single pre-migratory neural crest cells to follow their fate after migration in early embryos demonstrated CNCC plasticity in vivo [37,38,39,40]. These experiments also revealed that pre-migratory neural crest cells are composed of a mixture of multipotent and more restricted subpopulations. More recently, studies perform in avian and Xenopus embryos showed a subpopulation of pre-migratory CNCC expresses pluripotency factor genes such as Nanog, Klf4, and Oct4 supporting the notion of CNCC exceptional potency [23]. In situ hybridization performed in Xenopus embryos showed neural crest specifiers genes are co-expressed with pluripotency markers [22], suggesting pluripotency program is retained from the blastula stage into the CNCC lineage. Moreover, when derived from blastula-stage embryos, animal pole-derived explants could generate all three germ layers under defined culture conditions. Yet, this potential was lost when explants were taken later during development as gastrula-stage cells have already undergone lineage commitment. However, when converting gastrula-derived explants to neural plate border identity (through the over-expression of Pax3 and Zic1), explants reacquired the capacity to form ectoderm, mesoderm as well as endoderm – even though neural crest cells do not endogenously form endodermal derivatives [22].
In contrast, a single-cell RNA-sequencing (scRNA-seq) study investigating 136,966 single-cell transcriptomes obtained from 10 early Xenopus developmental stages failed to uncover a cluster of cells with enriched expression of pluripotency markers [41]. Though one can argue that the sequencing technique used for the experiment was not sensitive enough to detect the retention of a pluripotency programs in neural plate border cells at low transcriptional levels. Alternatively, this approach does not detect non-transcriptional regulation, such as epigenetic modifications of enhancers regulating the expression of genes responsible for the increase in CNCC differentiation potential. Along the same line, a recent study identified miR-302 as a post-transcriptional regulator of CNCC plasticity. This miRNA appears to maintain chromatin accessibility, to directly target Sox9 and expand the period of ectomesenchyme specification and enlarge CNCC developmental potential [42•]. Recent data obtained in Xenopus and mouse embryos showed pluripotency programs are in fact reactivated during CNCC formation [24•, 25••]. Careful analysis of Oct4 spatiotemporal expression in mouse embryos revealed that – in late neurula embryo – Oct4 is not expressed in the developing head-folds. Yet, it is reactivated later, in the most anterior part of the embryo following somitogenesis, demonstrating that rather than being maintained from the epiblast, pluripotency programs are transiently reactivated in the prospective CNCC following head-folds formation. Moreover, this transient re-expression of pluripotency programs was shown to be essential for CNCC to expand their differentiation potential as inhibition of Oct4 reactivation at the onset on CNCC induction severely impairs facial ectomesenchyme specification and survival, directly linking the reactivation of pluripotency programs with CNCC cellular potential expansion [25••]. In addition, analysis of Oct4+ CNCC open chromatin landscape confirmed that regulatory elements controlling expression of mesenchymal genes such as Pdgfra or Mef2c are already accessible in pre-migratory CNCC – 8 to 12 hours before any transcripts coding for these mesenchymal specification genes are being detected in migratory CNCC – confirming previous epigenetics profiling experiments that identified regulatory elements contribute to neural crest cell fate decisions [25••, 43,44,45]. Furthermore, the transcription factor TFAP2α was shown to physically interacts with the OCT4-SOX2 dimer to modify its chromatin binding from pluripotency to CNCC enhancers and thus regulate developmental potential of this population [46]. Together, these studies suggest that CNCC differentiation programs are already primed before EMT, allowing CNCC to adapt to future environmental cues they may encounter during and after their migration to issue a correct craniofacial development.
Neural Crest Cells and Bone Regeneration
In mammals, bone tissue has an excellent repair capacity, however its ability to heal large defects remains limited [47]. Thus, stimulating endogenous regeneration is necessary to treat severe craniofacial tissue injuries to alleviate the need of tissue transplantation from the patient or a donor and avoid additional complications such as transplant or scaffold rejection.
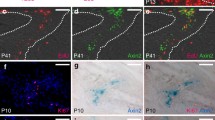
Skeletal stem cells (SSC) are the common tissue-resident progenitor cells giving rise to bone, cartilage, and stromal elements during bone regeneration [48,49,50]. A subpopulation of SSC with high regenerative potential has been recently identified in the periosteum and efficiently contribute to the endochondral ossification process during fracture repair [51, 52]. Accumulating evidence suggest that bone regeneration relies on SSC recapitulating developmental programs to ensure the repair process [53,54,55,56]. For example, following femoral fracture, SSC are mobilized and display increased proliferation, viability, and enhanced osteogenic function. Moreover, a recent report shows that enriched 3D-hydrogel transplantation induces expansion of the Msx1+ skeletal stem cells and enhanced bone regeneration in a model of calvaria injury [53]. Transcriptome analysis of the injury-responsive mouse SSC showed a striking overlap between molecular programs active during long bone development and regeneration, such as BMP and Hedgehog signaling [54]. However, one can argue these signals are pivotal hubs that are used in various tissue and contexts. Similarly, SSC were shown to play a significant role in mandibular repair during distraction osteogenesis – a procedure consisting in cutting and separating bone, to allow bone repair process to fill in the gap [55]. Moreover, it has been shown that, during the repair process, SSC reactivate neural crest transcriptional programs which enhances bone formation and tissue repair [56] (Fig. 2). While both long and craniofacial bone regeneration rely on the reactivation of developmental programs for efficient repair, CNCC-derived bones regenerate better compared to mesoderm-derived long bones [57, 58]. However, it is still unclear whether this is due to the lack of expression of the Hox genes in anterior craniofacial bones [57, 58] or to the ability of the craniofacial SSC to more efficiently reactivate developmental programs than long bone SSC is still unclear.
Deeper understanding of the molecular mechanisms mobilizing SSC and stimulating cell potency could then be translated to ameliorate craniofacial endogenous regenerative responses, tissue repair and healing (Fig. 2). Up to date, the ability of adjuvant therapies to enhance endogenous bone repair has been studied using various animal models. During mandibular distraction, treatment with deferoxamine was shown to accelerate bone consolidation in rats [59] by chelating iron, which results in the stimulation of the hypoxia inducible factor 1-α (HIF-1α) pathway – a master regulator of cellular response to hypoxia [60, 61]. Using a rat model of mandibular distraction osteogenesis, another study demonstrated that activating the stromal cell–derived factor-1 (SDF1)/chemokine receptor-4 (CXCR4) pathway promoted migration of endogenous mesenchymal stem cells to the distraction site [62]. However, this study did not determine the contribution of the recruited mesenchymal stem cells to the distraction regeneration but still represent a promising avenue to explore since the SDF1 signaling is also involved in CNCC migration [63] during embryogenesis.
Homologous and heterologous bone transplantation are one of the most common surgical procedures utilized for damaged bone repair. However, many limitations and challenging post-operative complications can occur with this procedure, such as site infection or immunologic reaction. Thus, alternative treatments for repair and regeneration need to be explored. For example, chondrocytes from other sources could be harvested and expanded in vitro [64] alone or in combination with bioengineering tools such as biomimetic hydrogels [65]. These cells can be then grafted on the site of bone regeneration to contribute to bone repair. In fact, chondrocytes harvested from tibia fracture calli can efficiently repair craniofacial bone fractures [66]. Another possible strategy focuses on nasal cartilage biopsies that can be harvested under local anesthesia, with minimal donor site morbidity [67]. Such biopsies have been shown to be a good source of nasal chondrocytes that display a better proliferation and chondrogenic capacity than articular chondrocytes ex vitro and in vivo [68, 69] and have a superior ability to integrate the surrounding tissue when implanted to repair cartilage defects (reviewed in [70]). These represent a source of easily accessible material in relatively abundant quantity and are promising avenue to further explore in the future (Fig. 2).
Conclusion
The craniofacial skeleton represents one major derivative of the cranial neural crest [16, 71]. Because of the crucial functions of this structure, any defects, either injury or disease-associated, have an enormous impact on quality of life. While bone is a tissue with very efficient regenerative capacities, about 10% of bone fractures are unable to self-repair [72] and will require transplantation or stem-cell therapies. Regenerative medicine has made tremendous progresses in developing treatments and procedures to increase tissue repair in patients. Nevertheless, it is essential to find new ways to stimulate endogenous regeneration to overcome the limitations of autologous and heterologous transplantations, including graft rejection. Stimulating the endogenous repair also results in the formation of a better integrated structure within surrounding tissues and similar in pattern to the original. Understanding the role of the mesenchymal niche and the developmental program(s) that activate and guide the CNCC-driven osteogenesis is fundamental to ameliorate and therapeutically target bone repair. CNCC contribution to this process has been demonstrated and validated by recent studies that have also pointed out the extreme plasticity of the cells [25••] although further investigations are needed to define their exact fate. Re-expression of pluripotency programs is a peculiar developmental event that CNCC activate but it would be interesting to know whether the cells are reactivating this process during bone repair. Several studies of SSC contribution to bone repair demonstrated the importance of recapitulating developmental processes in post-natal bone repair processes. Characterizing the gene regulatory networks governing bone development and the mechanisms controlling SSC potential within their niche represent fundamental goals in the fields of developmental biology, stem cell research and regenerative medicine. Furthermore, understanding the molecular regulations of cell plasticity during development will be essential to enhance SSC expansion, stimulate tissue resident stem cells and reduce the tumorigenic risks of stem cell transplantation. This knowledge will be essential to establish prototype procedures aiming at enhancing endogenous regenerative responses during tissue repair. It will likely lead to protocols increasing the viability and adaptability of stem-cell or tissue transplants, which will ameliorate autograft integration and overall repair process. Translating this knowledge will allow to engineer better regenerative therapies for humans suffering traumatic injuries or congenital syndromes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Gilbert-Barness E. Teratogenic causes of malformations. Ann Clin Lab Sci. 2010. Spring;40(2):99–114. https://pubmed.ncbi.nlm.nih.gov/20421621/.
Ho-Shui-Ling A, Bolander J, Rustom LE, Johnson AW, Luyten FP, Picart C. Bone regeneration strategies: engineered scaffolds, bioactive molecules and stem cells current stage and future perspectives. Biomaterials. 2018;180:143–62. https://doi.org/10.1016/j.biomaterials.2018.07.017.
Neovius E, Engstrand T. Craniofacial reconstruction with bone and biomaterials: review over the last 11 years. J Plast Reconstr Aesthetic Surg JPRAS. 2010;63(10):1615–23. https://doi.org/10.1016/j.bjps.2009.06.003.
Aghali AM. Poly(ethylene glycol) and Co-polymer Based-Hydrogels for Craniofacial Bone Tissue Engineering. In: Li B, Webster T, editors. Orthopedic Biomaterials: Advances and Applications. Cham: Springer International Publishing; 2017. p. 225–46. https://doi.org/10.1007/978-3-319-73664-8_9.
Dang M, Saunders L, Niu X, Fan Y, Ma PX. Biomimetic delivery of signals for bone tissue engineering. Bone Res. 2018;6:25. https://doi.org/10.1038/s41413-018-0025-8.
McCarthy JG, Stelnicki EJ, Mehrara BJ, Longaker MT. Distraction osteogenesis of the craniofacial skeleton. Plast Reconstr Surg. 2001;107(7):1812–27. https://doi.org/10.1097/00006534-200106000-00029.
Dupont KM, Sharma K, Stevens HY, Boerckel JD, García AJ, Guldberg RE. Human stem cell delivery for treatment of large segmental bone defects. Proc Natl Acad Sci U S A. 2010;107(8):3305–10. https://doi.org/10.1073/pnas.0905444107.
Jeon OH, Panicker LM, Lu Q, Chae JJ, Feldman RA, Elisseeff JH. Human iPSC-derived osteoblasts and osteoclasts together promote bone regeneration in 3D biomaterials. Sci Rep. 2016;6:26761. https://doi.org/10.1038/srep26761.
•• Glaeser JD, et al. Neural crest-derived mesenchymal progenitor cells enhance cranial allograft integration. Stem Cells Transl Med. 2021;10(5):797–809. https://doi.org/10.1002/sctm.20-0364. This study shows that using neural crest-derived mesenchymal cells enhances allograft efficiency by ameliorating the integration of the bone transplant. It also shows how to harness neural crest-derived cells potential during cranial bone regeneration.
Luo J, et al. Infiltrating bone marrow mesenchymal stem cells increase prostate cancer stem cell population and metastatic ability via secreting cytokines to suppress androgen receptor signaling. Oncogene. 2014;33(21):2768–78. https://doi.org/10.1038/onc.2013.233.
Zhang T, Lee YW, Rui YF, Cheng TY, Jiang XH, Li G. Bone marrow-derived mesenchymal stem cells promote growth and angiogenesis of breast and prostate tumors. Stem Cell Res Ther. 2013;4(3):70. https://doi.org/10.1186/scrt221.
Gerber T, et al. Single-cell analysis uncovers convergence of cell identities during axolotl limb regeneration. Science. 2018;362(6413):eaaq0681. https://doi.org/10.1126/science.aaq0681.
McCusker CD, Athippozhy A, Diaz-Castillo C, Fowlkes C, Gardiner DM, Voss SR. Positional plasticity in regenerating Amybstoma mexicanum limbs is associated with cell proliferation and pathways of cellular differentiation. BMC Dev Biol. 2015;15:45. https://doi.org/10.1186/s12861-015-0095-4.
Vieira WA, McCusker CD. Regenerative models for the integration and regeneration of head skeletal tissues. Int J Mol Sci. 2018;19(12):3752. https://doi.org/10.3390/ijms19123752.
Le Douarin N, Kalcheim C. The Neural Crest, 2nd ed. In Developmental and Cell Biology Series. Cambridge: Cambridge University Press; 1999. https://doi.org/10.1017/CBO9780511897948.
Noden DM, Trainor PA. Relations and interactions between cranial mesoderm and neural crest populations. J Anat. 2005;207(5):575–601. https://doi.org/10.1111/j.1469-7580.2005.00473.x.
Simões-Costa M, Bronner ME. Establishing neural crest identity: a gene regulatory recipe. Development. 2015;142(2):242–57. https://doi.org/10.1242/dev.105445.
Theveneau E, Mayor R. Neural crest migration: interplay between chemorepellents, chemoattractants, contact inhibition, epithelial-mesenchymal transition, and collective cell migration. Wiley Interdiscip Rev Dev Biol. 2012;1(3):435–45. https://doi.org/10.1002/wdev.28.
Soldatov R, et al. Spatiotemporal structure of cell fate decisions in murine neural crest. Science. 2019;364(6444). https://doi.org/10.1126/science.aas9536.
Le Douarin NM, Creuzet S, Couly G, Dupin E. Neural crest cell plasticity and its limits. Development. 2004;131(19):4637–50. https://doi.org/10.1242/dev.01350.
Perera SN, Kerosuo L. On the road again: Establishment and maintenance of stemness in the neural crest from embryo to adulthood. Stem Cells. 2021;39(1):7–25. https://doi.org/10.1002/stem.3283.
Buitrago-Delgado E, Nordin K, Rao A, Geary L, LaBonne C. NEURODEVELOPMENT. Shared regulatory programs suggest retention of blastula-stage potential in neural crest cells. Science. 2015;348(6241):1332–5. https://doi.org/10.1126/science.aaa3655.
Lignell A, Kerosuo L, Streichan SJ, Cai L, Bronner ME. Identification of a neural crest stem cell niche by Spatial Genomic Analysis. Nat Commun. 2017;8(1):1830. https://doi.org/10.1038/s41467-017-01561-w.
• Scerbo P, Monsoro-Burq AH. The vertebrate-specific VENTX/NANOG gene empowers neural crest with ectomesenchyme potential. Sci Adv. 2020;6(18):eaaz1469. https://doi.org/10.1126/sciadv.aaz1469. This study shows pluripotency factors are reactivated during neural crest formation in Xenopus.
•• Zalc A, et al. Reactivation of the pluripotency program precedes formation of the cranial neural crest. Science. 2021; 371(6529). https://doi.org/10.1126/science.abb4776. This study demonstrates the re-expression of pluripotency programs is necessary for the expansion of cranial neural crest cells differentiation potential in mammals.
Rodrigues-Da-Silva MA, de Espindola da Silveira G, Taufer CR, Calloni GW. The mesenchymal potential of trunk neural crest cells. Int J Dev Biol. 2022;66(4–5–6):317–31. https://doi.org/10.1387/ijdb.220032gc.
Bhatt S, Diaz R, Trainor PA. Signals and switches in mammalian neural crest cell differentiation. Cold Spring Harb Perspect Biol. 2013;5(2). https://doi.org/10.1101/cshperspect.a008326.
Dash S, Trainor PA. The development, patterning and evolution of neural crest cell differentiation into cartilage and bone. Bone. 2020;137:115409. https://doi.org/10.1016/j.bone.2020.115409.
• Yang J, et al. Augmented BMP signaling commits cranial neural crest cells to a chondrogenic fate by suppressing autophagic β-catenin degradation. Sci Signal. 2021;14(665):eaaz9368. https://doi.org/10.1126/scisignal.aaz9368. This study shows how the coordinated action of BMP signaling and autophagy regulates cell fate decision during craniofacial development.
Pezoa SA, Artinger KB, Niswander LA. GCN5 acetylation is required for craniofacial chondrocyte maturation. Dev Biol. 2020;464(1):24–34. https://doi.org/10.1016/j.ydbio.2020.05.006.
Shpargel KB, Mangini CL, Xie G, Ge K, Magnuson T. The KMT2D Kabuki syndrome histone methylase controls neural crest cell differentiation and facial morphology. Development. 2020;147(21):dev187997. https://doi.org/10.1242/dev.187997.
Smeriglio P, Grandi FC, Taylor SEB, Zalc A, Bhutani N. TET1 directs chondrogenic differentiation by regulating SOX9 dependent activation of Col2a1 and acan in vitro. JBMR Plus. 2020;4(8):e10383. https://doi.org/10.1002/jbm4.10383.
Kitami K, Kitami M, Kaku M, Wang B, Komatsu Y. BRCA1 and BRCA2 tumor suppressors in neural crest cells are essential for craniofacial bone development. PLoS Genet. 2018;14(5):1007340. https://doi.org/10.1371/journal.pgen.1007340.
• Zhao X, et al. Yap and Taz promote osteogenesis and prevent chondrogenesis in neural crest cells in vitro and in vivo. Sci Signal. 2022;15(757):eabn9009. https://doi.org/10.1126/scisignal.abn9009. This study identifies a mechanism controlling the proper balance between osteogenesis and chondrogenesis during craniofacial bones development.
Liao J, et al. Gene regulatory network from cranial neural crest cells to osteoblast differentiation and calvarial bone development. Cell Mol Life Sci. 2022;79(3):158. https://doi.org/10.1007/s00018-022-04208-2.
Kelsh RN, Camargo Sosa K, Farjami S, Makeev V, Dawes JHP, Rocco A. Cyclical fate restriction: a new view of neural crest cell fate specification. Development. 2021;148(22):dev176057. https://doi.org/10.1242/dev.176057.
Bronner-Fraser M, Fraser SE. Cell lineage analysis reveals multipotency of some avian neural crest cells. Nature. 1988;335(6186):161–4. https://doi.org/10.1038/335161a0.
Collazo A, Bronner-Fraser M, Fraser SE. Vital dye labelling of Xenopus laevis trunk neural crest reveals multipotency and novel pathways of migration. Development. 1993;118(2):363–76. https://doi.org/10.1242/dev.118.2.363.
Serbedzija GN, Bronner-Fraser M, Fraser SE. Vital dye analysis of cranial neural crest cell migration in the mouse embryo. Development. 1992;116(2):297–307. https://doi.org/10.1242/dev.116.2.297.
Serbedzija GN, Bronner-Fraser M, Fraser SE. Developmental potential of trunk neural crest cells in the mouse. Development. 1994;120(7):1709–18. https://doi.org/10.1242/dev.120.7.1709.
Briggs JA, et al. The dynamics of gene expression in vertebrate embryogenesis at single-cell resolution. Science. 2018; 360(6392). https://doi.org/10.1126/science.aar5780.
• Keuls RA, Oh YS, Patel I, Parchem RJ. Post-transcriptional regulation in cranial neural crest cells expands developmental potential. Proc Natl Acad Sci USA. 2023;120(6):e2212578120. https://doi.org/10.1073/pnas.2212578120. This study shows post-transcriptional are also regulating cranial neural crest cells differentiation potential.
Rada-Iglesias A, Bajpai R, Swigut T, Brugmann SA, Flynn RA, Wysocka J. A unique chromatin signature uncovers early developmental enhancers in humans. Nature. 2011;470(7333):279–83. https://doi.org/10.1038/nature09692.
Minoux M, et al. Gene bivalency at Polycomb domains regulates cranial neural crest positional identity. Science. 2017;355(6332):31. https://doi.org/10.1126/science.aal2913.
Williams RM, et al. Reconstruction of the global neural crest gene regulatory network in vivo. Dev Cell. 2019;51(2):255-276 e7. https://doi.org/10.1016/j.devcel.2019.10.003.
Hovland AS, et al. Pluripotency factors are repurposed to shape the epigenomic landscape of neural crest cells. Dev Cell. 2022; S1534580722006360. https://doi.org/10.1016/j.devcel.2022.09.006.
Kiernan C, Knuth C, Farrell E. Chapter 6 - Endochondral Ossification: Recapitulating Bone Development for Bone Defect Repair. In: Stoddart MJ, Craft AM, Pattappa G, Gardner OFW, editors. Developmental Biology and Musculoskeletal Tissue Engineering. Boston: Academic Press; 2018. p. 125–48. https://doi.org/10.1016/B978-0-12-811467-4.00006-1.
Robey PG, Kuznetsov SA, Riminucci M, Bianco P. Skeletal (‘mesenchymal’) stem cells for tissue engineering. Methods Mol Med. 2007;140:83–99. https://doi.org/10.1007/978-1-59745-443-8_5.
Chan CKF, et al. Identification and specification of the mouse skeletal stem cell. Cell. 2015;160(1–2):285–98. https://doi.org/10.1016/j.cell.2014.12.002.
Chan CKF, et al. Identification of the human skeletal stem cell. Cell. 2018;175(1):43-56.e21. https://doi.org/10.1016/j.cell.2018.07.029.
Duchamp de Lageneste O, et al. Periosteum contains skeletal stem cells with high bone regenerative potential controlled by Periostin. Nat Commun. 2018;9(1):773. https://doi.org/10.1038/s41467-018-03124-z.
Julien A, et al. Skeletal stem/progenitor cells in periosteum and skeletal muscle share a common molecular response to bone injury. J Bone Miner Res Off J Am Soc Bone Miner Res. 2022;37(8):1545–61. https://doi.org/10.1002/jbmr.4616.
Zhang X, et al. Msx1+ stem cells recruited by bioactive tissue engineering graft for bone regeneration. Nat Commun. 2022;13(1):5211. https://doi.org/10.1038/s41467-022-32868-y.
Marecic O, et al. Identification and characterization of an injury-induced skeletal progenitor. Proc Natl Acad Sci. 2015;112(32):9920–5. https://doi.org/10.1073/pnas.1513066112.
Fang TD, et al. Creation and characterization of a mouse model of mandibular distraction osteogenesis. Bone. 2004;34(6):1004–12. https://doi.org/10.1016/j.bone.2004.02.011.
Ransom RC, et al. Mechanoresponsive stem cells acquire neural crest fate in jaw regeneration. Nature. 2018;563(7732):514–21. https://doi.org/10.1038/s41586-018-0650-9.
Leucht P, Kim J-B, Amasha R, James AW, Girod S, Helms JA. Embryonic origin and Hox status determine progenitor cell fate during adult bone regeneration. Development. 2008;135(17):2845–54. https://doi.org/10.1242/dev.023788.
Wang KC, Helms JA, Chang HY. Regeneration, repair and remembering identity: the three Rs of Hox gene expression. Trends Cell Biol. 2009;19(6):268–75. https://doi.org/10.1016/j.tcb.2009.03.007.
Donneys A, et al. Deferoxamine expedites consolidation during mandibular distraction osteogenesis. Bone. 2013;55(2):384–90. https://doi.org/10.1016/j.bone.2013.04.005.
Wang GL, Jiang BH, Rue EA, Semenza GL. Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci. 1995;92(12):5510–4. https://doi.org/10.1073/pnas.92.12.5510.
Iyer NV, et al. Cellular and developmental control of O2 homeostasis by hypoxia-inducible factor 1α. Genes Dev. 1998;12(2):149–62. https://doi.org/10.1101/gad.12.2.149.
Cao J, et al. Recruitment of exogenous mesenchymal stem cells in mandibular distraction osteogenesis by the stromal cell-derived factor-1/chemokine receptor-4 pathway in rats. Br J Oral Maxillofac Surg. 2013;51(8):937–41. https://doi.org/10.1016/j.bjoms.2013.05.003.
Theveneau E, et al. Collective chemotaxis requires contact-dependent cell polarity. Dev Cell. 2010;19(1):39–53. https://doi.org/10.1016/j.devcel.2010.06.012.
Smeriglio P, et al. Collagen VI enhances cartilage tissue generation by stimulating chondrocyte proliferation. Tissue Eng Part A. 2015;21(3–4):840–9. https://doi.org/10.1089/ten.TEA.2014.0375.
Smeriglio P, et al. Comparative potential of juvenile and adult human articular chondrocytes for cartilage tissue formation in three-dimensional biomimetic hydrogels. Tissue Eng Part A. 2015;21(1–2):147–55. https://doi.org/10.1089/ten.TEA.2014.0070.
Wong SA, et al. Chondrocyte-to-osteoblast transformation in mandibular fracture repair. J Orthop Res Off Publ Orthop Res Soc. 2021;39(8):1622–32. https://doi.org/10.1002/jor.24904.
Lan MY, Park JP, Jang YJ. Donor site morbidities resulting from conchal cartilage harvesting in rhinoplasty. J Laryngol Otol. 2017;131(6):529–33. https://doi.org/10.1017/S0022215117000639.
Rotter N, et al. Age-related changes in the composition and mechanical properties of human nasal cartilage. Arch Biochem Biophys. 2002;403(1):132–40. https://doi.org/10.1016/S0003-9861(02)00263-1.
Wolf F, Haug M, Farhadi J, Candrian C, Martin I, Barbero A. A low percentage of autologous serum can replace bovine serum to engineer human nasal cartilage. Eur Cell Mater. 2008;15:1–10. https://doi.org/10.22203/ecm.v015a01.
Li T, Chen S, Pei M. Contribution of neural crest-derived stem cells and nasal chondrocytes to articular cartilage regeneration. Cell Mol Life Sci CMLS. 2020;77(23):4847–59. https://doi.org/10.1007/s00018-020-03567-y.
Jiang X, Iseki S, Maxson RE, Sucov HM, Morriss-Kay GM. Tissue origins and interactions in the mammalian skull vault. Dev Biol. 2002;241(1):106–16. https://doi.org/10.1006/dbio.2001.0487.
Sheen JR, Garla VV. Fracture Healing Overview. In StatPearls. Treasure Island: StatPearls Publishing, 2022. Accessed: Feb. 28, 2023. [Online]. Available: http://www.ncbi.nlm.nih.gov/books/NBK551678/.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
Piera Smeriglio and Antoine Zalc declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Smeriglio, P., Zalc, A. Cranial Neural Crest Cells Contribution to Craniofacial Bone Development and Regeneration. Curr Osteoporos Rep 21, 624–631 (2023). https://doi.org/10.1007/s11914-023-00804-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-023-00804-8