Abstract
Purpose of Review
Many mechanical load-bearing joints of the body are prone to posttraumatic osteoarthritis (PTOA), including the knee joint and temporomandibular joint (TMJ). Early detection of PTOA can be beneficial in prevention or alleviating further progression of the disease.
Recent Findings
Various mouse models, similar to those used in development of novel diagnosis strategies for early stages of OA, have been proposed to study early PTOA. While many studies have focused on OA and PTOA in the knee joint, early diagnostic methods for OA and PTOA of the TMJ are still not well established. Previously, we showed that fluorescent near-infrared imaging can diagnose inflammation and cartilage damage in mouse models of knee PTOA. Here we propose that the same approach can be used for early diagnosis of TMJ-PTOA.
Summary
In this review, we present a brief overview of PTOA, application of relevant mouse models, current imaging methods available to examine TMJ-PTOA, and the prospects of near-infrared optical imaging to diagnose early-stage TMJ-OA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Articular cartilage is a smooth layer of connective tissue present at the diarthrodial surfaces of joints such as the knee, hip, and temporomandibular joints [1•, 2,3,4]. Arthritis is a degenerative chronic disorder that causes damage to articular cartilage and surrounding tissues in joints.
The early diagnosis and treatment of osteoarthritis (OA) is a key factor in preventing the degradation of cartilage and subsequent lack of joint movement [5]. However, understanding the etiology of OA is vital for development of an effective diagnostic method. One of the extensively studied synovial joints is the knee joint as it undergoes continuous bone remodeling and cartilage maintenance during the normal course of mechanical loading from daily activities [6].
Similar to the knee joint, the temporomandibular joint (TMJ) bears comparable mechanical loading and hence undergoes similar degenerative processes [7,8,9,10,11]. It is noteworthy that PTOA of TMJ (TMJ-PTOA) varies in reported prevalence due to different criteria used for diagnosis [12,13,14]. TMJ-PTOA can occur either unilaterally or bilaterally and is more commonly reported in women than men [15,16,17]. Gonadal hormones have been associated with differences in pain perception, and the female hormone estrogen may increase sensitivity to pain in women. In support of this hypothesis, estrogen receptor polymorphisms have been correlated with different levels of pain in TMJ-OA in women [18]. TMJ-PTOA is generally recognized after the onset of pain and due to this reason only about 3–7% of patients seek medical attention, after considerable damage to the cartilage of TMJ has already developed [19, 20]. Thus, it is of utmost importance to diagnose TMJ-PTOA in early stages before the onset of symptomatic pain.
Different imaging modalities that are used to diagnose TMJ-PTOA include panoramic radiographs, arthrography, TMJ tomograms, ultrasonography, radionuclide examination, cone beam computer tomography (CBCT), and magnetic resonance imaging (MRI). In this report, we are reviewing the current technology in orthopedic research for the PTOA knee joint with the purpose of translating the applications to the TMJ. We present a brief overview of TMJ and the imaging techniques available to diagnose TMJ-PTOA. Moreover, prospects of developing more sensitive imaging techniques to detect TMJ-PTOA at an early stage are suggested.
Posttraumatic Osteoarthritis in Knee Joint
The type of OA that occurs after injury or insult to an already affected joint is known as “posttraumatic OA (PTOA)” [21, 22]. It has been estimated that knee OA is most common in women over the age of 60 with a prevalence of about 14–42% [23]. In the USA, 12% of all OA cases fall under the category of PTOA. This percentage is likely to increase due to current lack of diagnosis following a traumatic injury [24]. It should be emphasized that trauma increases the risk of developing knee OA 5-fold compared with a 1.7-fold increased risk due to obesity, which is considered a major risk factor [25,26,27]. Moreover, joints are more prone to develop PTOA due to trauma affecting joint tissues in addition to cartilage, such as ligaments and menisci [25, 28]. For instance, 50–70% of patients with either anterior cruciate ligament (ACL) or meniscal damage develop PTOA 10–15 years post-injury [28,29,30,31].
The annual health-care cost of PTOA in the USA was estimated to be 3 billion USD in 2006 [24]. The expected cost of a patient is 13 thousand USD only for the operative procedure and hospital stay [32,33,34]. Indirect costs, such as disability and reduced work productivity, are excluded from these estimates. Furthermore, PTOA is common in young adults after injury, increasing the duration of disability and resulting in higher economic cost [35]. In addition, the cost of managing PTOA in individuals who develop this complication after injury is greater than those who do not develop OA due to an injury [36]. Thus, the issue of high health-care cost associated with PTOA needs urgent attention. It is vital to develop advanced diagnostic methods to detect early-stage PTOA that will aid in reducing the economic cost of PTOA treatment.
Mouse Models of PTOA in Knee Joint
PTOA mouse models serve as excellent candidates to mimic the changes occurring in human joints after an injury [37]. Five criteria (Table 1) have been set forth to establish an “ideal” animal model of OA [38••, 39]:
To date, there is no mouse model of OA that may be regarded as “ideal.” However, multiple mouse models have been suggested to approximately mimic PTOA in humans. Two types of PTOA mouse models are broadly accepted: (A) Invasive models that are established by either surgical or chemical means, and (B) non-invasive models that are developed by the application of mechanical load without disrupting the joint integrity. Here we shall briefly review the non-invasive models.
Non-invasive PTOA Mouse Models
Non-invasive mouse models are more appropriate than invasive models to study the early stages of PTOA [38••]. First, the injuries produced by non-invasive techniques progress in the same manner and time frames as human injury [40]. This is important in the development of diagnostic and therapeutic strategies for early stages of OA that can either help in impeding or inhibiting the PTOA. Furthermore, non-invasive models exhibit damage to the structural components of the joints that are reflective of injury due to mechanical stress in humans. In addition, these types of models are simple, easy to implement, and require less technical expertise in comparison to the invasive models. These features minimize intra-sample variation, making the non-invasive animal models close to ideal.
Fracture of Tibial Plateau
The first non-invasive model, introduced in 2007, is based on intra-articular fracture (IAF) of the proximal tibia [41]. This model mimics high-impact force traumatic injuries in humans such as those occurring during frontal automobile collisions. The blunt impact to articular cartilage causes fragmentation of articular surfaces, fracture of subchondral bone, joint displacement, and leakage of blood and marrow into the joint space. To mimic blunt trauma in C57BL/6 mice, articular fracture of the tibial plateau was induced by first positioning the lower limb at approximately 90° flexion in a custom-made cradle. Subsequently, a 10 N compressive preload was applied to the proximal tibia using a mounted wedge-shaped indenter to a target compressive force of 55 N at a rate of 20 N/s [36, 38••].
A shortcoming of this model is that it cannot be used to study low-impact non-contact injuries that generally lead to PTOA such as anterior cruciate ligament (ACL) rupture or meniscus tear. Moreover, the fracture severity varies between samples and hence, cautions are needed to include possible variables into the analysis. Even with allowances for fracture severity, variability of this model serves as a limitation of this method [38••].
Cyclic Compression of Tibia
Cyclic compression of the tibia is the most common non-invasive method of PTOA [42]. Oscillatory loading is applied to the hind limbs such that loads are transmitted through the articular joint, resulting in damage to the cartilage tissue. The first model was introduced by Poulet and his colleagues in CBA mice by applying a 9 N compressive load every 10 s with a total of 40 cycles for each loading sequence. The loading was performed three days per week [43].
The first and foremost benefit of the cyclic compression model is its adjustability to study the course of OA development [38••]. The severity of joint degradation can be controlled by altering either the compressive force or loading time. Nonetheless, the severity achieved through this model is always mild, making this model an ideal method of choice to study the course of OA occurring at a very early stage. Furthermore, the reproducibility of this model is high, with little variation among the individual animals. In addition, the data obtained after the application of cyclic compression is a direct consequence of the mechanical loading. This helps in determining the exact impact of mechanical loading on the joint, rather than secondary factors causing the joint damage such as in fracture of the tibial plateau [44]. We evaluated this model in different strains of mice and found that the reproducibility of mild cartilage damage remains consistent with little to no variation among the individual animals (data not shown).
ACL Rupture Model
This model utilizes the feature of rupturing the ACL by over-compression of the tibia [45]. This procedure mimics an acute injury model and can be used to observe the changes associated with ACL rupture in humans. The model was constructed in 10-week-old C57BL/6 mice by application of a single compressive target force of 12 N with a loading rate of 1 mm/s. Injury can be noted as an audible click when the compressive load is released [38••]. Similar to cyclic compression of the tibia, the results obtained from this model are reproducible with a predictable feature of joint degeneration.
Temporomandibular Joint
The inferior articular surfaces of the TMJ are formed by the mandibular condyle and the superior surfaces by the glenoid fossa or mandibular fossa as well as articular eminence of the temporal bone [46, 47]. It has morphological features similar to other synovial joints, including articular disks, articular surfaces, fibrous joint capsules, synovial fluid, synovial membranes, and ligaments. As such, TMJ is essentially a hinge joint allowing backward and forward movement translationally in addition to a gliding motion.
The unique feature that distinguishes TMJ from other synovial joints is the presence of strong fibrocartilage instead of the weaker hyaline cartilage at the articular surface. The primary difference between hyaline and fibrocartilage is the high content of either collagen type II (Col2) or collagen type I (Col1), respectively [48]. This compositional difference gives rise to numerous dense collagen fibers on the articular surfaces of TMJ rather than the less dense hyaline cartilage [49]. In addition, the amount of Col1 in the mandibular condyle is less compared to the other synovial joints [50]. Furthermore, the cartilage of the mandibular condyle is a secondary cartilage and is derived from cranial neural crest (CNC) cells [51,52,53].
Mouse Models of TMJ-PTOA
Animal models of TMJ-PTOA are similar to other PTOA models and include both invasive and non-invasive techniques. The invasive models of PTOA are either surgically or chemically induced while the non-invasive methods are mechanically induced [54]. The choice of method depends on the outcome under consideration. Chemically induced models can help to study pain, surgically induced models help to study degenerative changes, and mechanically loaded models help to study structural and functional changes [55]. Only the non-invasive mechanical models will be discussed here.
Non-invasive Mouse Models of TMJ-PTOA
Three mouse models of TMJ mechanical loading have been introduced [56]. Of these, the altered functional loading and mastication-based models are less invasive than the forced mouth opening model.
Altered Functional Loading Model
An altered functional loading model results from feeding mice a soft pellet diet and trimming their incisors every other day for 4–6 weeks. This contrasts with loading control animals that are fed a standard hard pellet diet without incisor trimming [57]. The decreased load in the experimental animals resulted in reduced thickness of the TMJ articular cartilage. Furthermore, analysis of mRNA levels showed that expression of SRY-box containing gene 9 (Sox9) and Col2 genes decreased. The reduced expression of Col2 in the altered mechanical loading group was also observed by immunolabelling. It is well established that SOX9 directly regulates the expression of Col2 [58]. Therefore, the results of this study suggest that altered mechanical loading through trimming of incisors and a soft diet can produce significant changes in the TMJ cartilage.
Mastication-Based Model
This model was established in mice by inserting a unilateral anterior crossbite prosthesis and varying the size of food pellets in the diet [59]. Use of the prosthesis increased demands on the TMJ during mastication. The animals with the prosthetic device that had been given a large pellet diet showed hypocellularity, loss of proteoglycans, and decreased expression of Col2 at the 3-week follow-up compared to those with the prosthesis and small pellet diet.
Forced Mouth Opening Model
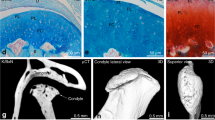
This mouse model is based upon continuous opening of the mouth in anesthetized animals for 1 h a day up to 5 days [60]. Examination of this model tested a hypothesis that forced mouth opening would cause increased anabolism in the condyles of mandibular cartilage. A force of 0.5 N resulted in increased expression of Sox9 and Col2 genes with a concomitant increase in the thickness of subchondral bone. Further application of this model in transgenic mouse lines expressing fluorescent reporters under control of collagen gene promoters demonstrated increased expression of Col1, Col2, and Col10 genes in the cartilage of the TMJ [61]. These results indicate that loading of TMJ by forced mouth opening causes remodeling of TMJ to balance the changes due to altered mechanical loading. Figure 1 illustrates the use of this technique to test the impact of rebamipide (a gastroprotective agent) on cartilage degeneration in TMJ-OA [62].
Establishing a TMJ-OA model. The TMJs of C57BL/6 WT mice were subjected to jaw-opening devices that were applied to the interincisal teeth to hold the mandible in the maximal opened position. The mechanical stress was applied for 3 h per day for 5 days. Mice in the rebamipide treatment groups received the drug for 4 weeks. Mice were under general anesthesia during the procedure. Somnopentyl was administered via intraperitoneal route at a concentration of 50 mg/kg to induce anesthesia [62,63,64]. Note: This figure was modified/adapted from “Izawa T. et. al, 2016, PLoSOne, 11(4):e0154107 E.” and Tanaka et al. J Dent Res 87(4):296–307, 2008
Imaging Modalities for TMJ-PTOA
Abnormalities in the TMJ can be visualized using both invasive and non-invasive techniques. Here we introduce a brief description of the techniques available to examine and diagnose TMJ-PTOA.
X-ray Examination
Radiographic examination of the TMJ has been a method of choice for decades [65, 66]. Although this technique is cost-effective and provides lower radiation exposure than some imaging modalities, it cannot deliver the three-dimensional detail of more advanced methods. Some authors have even argued that standard X-ray at times did not correlate with the clinical features of the disease [67]. Yet, to date X-ray examination is still being used in clinics owing to advances in panoramic projection. However, the morphology of bone may appear blurred due to the surrounding tissues [68]. In addition, radiography is not a suitable method to examine the non-bony structures such as the cartilage tissue. Further disadvantages of radiographs include lack of information on joint effusions and superimposed images of structures. In spite of its limitations, conventional X-ray is often useful as an initial technique in examination of the TMJ.
Arthrography
The arthrography technique is an invasive method to examine the TMJ that was introduced in clinics in 1970 [69]. This method entails injection of a radiopaque contrast agent into the TMJ with the aid of an arthroscope. Analysis depends on the manner in which the contrast agent flows into the joint. Furthermore, there is a risk of allergic reaction, infection, and radiation to the patient due to the use of the contrast reagent. This technique has now been abrogated due to the introduction of MRI [12].
Computerized Tomography
The CT method is useful in examining both bone and soft tissues of the TMJ. CT is used to diagnose fractures of condyles, disc dislocation, ankylosis, erosions, infection, tumors, congenital anomalies, and degeneration of bone [68, 70]. CT is more likely to be recommended if pathology of bone is suspected through MRI. Thus, CT has some advantages over MRI in terms of acquiring bone details and three-dimensional (3D) evaluation of traumatic injury, congenital problems, and postsurgical examination [12].
Magnetic Resonance Imaging
The power of MRI lies in the fact that it provides high-resolution images and high tissue contrast with an additional benefit of no side effects. MRI also provides detailed anatomical and functional details of the TMJ in both open and closed mouths [19]. The accuracy of MRI has been found to be 60–100% in examining bone degeneration and 73–95% in assessment of disc dislocation. Additionally, MRI can reveal the pathology of other soft tissues such as that of chewing muscles [68]. In contrast to radiographs, MRI changes seem to correlate with the clinical symptoms of TMJ-OA [71,72,73]. However, the use of MRI has been inhibited by the high cost, and detection of TMJ disorders at an early stage of the disease is still a challenge.
Ultrasound
The use of ultrasound is without doubt the least expensive modality, is easy to perform, and is a readily available technique for examination of the TMJ. This technique can be used to evaluate joint effusion, cartilage tissue, and disk displacement. Furthermore, this technique can be performed in real time, allowing examinations during mouth movement. However, despite its numerous advantages, ultrasonography cannot be used solely to diagnose TMJ-PTOA due to the limitation in distinguishing disk displacement with or without reduction [70].
Target-Specific Near-Infrared Imaging of TMJ-PTOA (Fig. 2)
More recently, the use of near-infrared optical imaging has become a notable method for detecting joint damage [74]. We and others have shown that using either fluorescent probes or targeted nanosomes (nano-sized liposomes) that are guided by monoclonal antibodies specific for the markers of cartilage damage can help in the diagnosis of damaged cartilage tissue surfaces [42, 75]. We have developed specific methodology using in vivo image scanning (IVIS) that can detect either inflammation or cartilage damage in arthritic joints [76]. For instance, targeted nanosomes may carry monoclonal antibodies that can detect exposed type II collagen on the surface of the cartilage. In this way, nanosomes can either deliver a detection probe or a therapeutic drug to the damaged surface. The advantage of this technique is its excellent capability to detect OA at an early stage [77, 78••].
Schematic diagram of antibody-targeted nanosome binding onto damaged cartilage in a post-traumatic osteoarthritis (PTOA) mouse model. Shown in the graphical abstract is a schematic diagram of our targeted nanosomes in a PTOA mouse model (PEG: polyethylene glycol). Cupped loading cells engage the distal femur on top and the ankle below. A force of 9 N is applied sinusoidally at 0.07 Hz for 40 cycles. The targeted nanosome technology can simultaneously be used for early detection of cartilage damage in the knee joint. This imaging technique can also detect inflammation in the TMJ using an IVIS imaging system (left picture in lower panel). (Red line indicates current application and red dot line indicates future application). Note: This figure was modified/adapted from “Cho et al. 2015 Nanomedicine: NBM, 11:939-946”
In a similar manner, we expect that the IVIS imaging approach can be used with or without targeted nanosomes to detect inflammatory changes and cartilage damage at the early stages of TMJ-PTOA. In our preliminary examination, we have already observed changes in the cartilage tissue of OA associated with arthritic mice (Fig. 2). We hypothesize that more specific targeted nanosomes generated against the cartilage tissue of TMJ will aid detection of early-stage TMJ-PTOA. As a result, TMJ-PTOA can be identified before the onset of pain symptoms, which helps prevent the tissue degeneration at the TMJ. In addition, this technique comes with the benefit of being easy to apply in clinics with minimal side effects.
Conclusion
The current diagnostic measures available to detect TMJ-PTOA, in spite of their many advantages, have a common limitation of not detecting OA at its early stages. Many mouse models that mimic various clinical cases of knee OA have been developed, but there are limited models and diagnostic techniques that can detect TMJ-PTOA at an early stage. In this aspect, we suggest applying the IVIS method by developing either targeted nanosomes or using fluorescence probes to detect the pathological changes that occur at an early stage of TMJ-PTOA. Once such an approach is established, it easily could be translated into clinical settings both for diagnostic and therapeutic purposes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
• Kim DG, et al. Sex dependent mechanical properties of the human mandibular condyle. J Mech Behav Biomed Mater. 2017;71:184–91 This study shows the mechanical behavior of the cartilage-subchondral bone and it is related to the subchondral bone properties including tissue mineral density and trabecular morphological parameters.
Decker RS, Koyama E, Pacifici M. Articular cartilage: structural and developmental intricacies and questions. Curr Osteoporos Rep. 2015;13(6):407–14.
Sophia Fox AJ, Bedi A, Rodeo SA. The basic science of articular cartilage: structure, composition, and function. Sports Health. 2009;1(6):461–8.
Buckwalter JA, Mankin HJ. Articular cartilage: tissue design and chondrocyte-matrix interactions. Instr Course Lect. 1998;47:477–86.
Chu CR, Williams AA, Coyle CH, Bowers ME. Early diagnosis to enable early treatment of pre-osteoarthritis. Arthritis Res Ther. 2012;14(3):212.
Yokota H, Leong DJ, Sun HB. Mechanical loading: bone remodeling and cartilage maintenance. Curr Osteoporos Rep. 2011;9(4):237–42.
Quinn JH, Bazan NG. Identification of prostaglandin E2 and leukotriene B4 in the synovial fluid of painful, dysfunctional temporomandibular joints. J Oral Maxillofac Surg. 1990;48(9):968–71.
Holmlund A, et al. Concentrations of neuropeptides substance P, neurokinin A, calcitonin gene-related peptide, neuropeptide Y and vasoactive intestinal polypeptide in synovial fluid of the human temporomandibular joint. A correlation with symptoms, signs and arthroscopic findings. Int J Oral Maxillofac Surg. 1991;20(4):228–31.
Herring SW. TMJ anatomy and animal models. J Musculoskelet Neuronal Interact. 2003;3(4):391–4 discussion 406-7.
Kim DG, Jeong YH, Kosel E, Agnew AM, McComb DW, Bodnyk K, et al. Regional variation of bone tissue properties at the human mandibular condyle. Bone. 2015;77:98–106.
Coogan JS, Kim DG, Bredbenner TL, Nicolella DP. Determination of sex differences of human cadaveric mandibular condyles using statistical shape and trait modeling. Bone. 2018;106:35–41.
Bag AK, et al. Imaging of the temporomandibular joint: an update. World J Radiol. 2014;6(8):567–82.
Ohrbach R, Dworkin SF. The Evolution of TMD Diagnosis: Past, Present, Future. J Dent Res. 2016;95(10):1093–101.
Dworkin SF, LeResche L. Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomandib Disord. 1992;6(4):301–55.
Boyan BD, Tosi LL, Coutts RD, Enoka RM, Hart DA, Nicolella DP, et al. Addressing the gaps: sex differences in osteoarthritis of the knee. Biol Sex Differ. 2013;4(1):4.
LeResche L. Epidemiology of temporomandibular disorders: implications for the investigation of etiologic factors. Crit Rev Oral Biol Med. 1997;8(3):291–305.
Zhao YP, Zhang ZY, Wu YT, Zhang WL, Ma XC. Investigation of the clinical and radiographic features of osteoarthrosis of the temporomandibular joints in adolescents and young adults. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;111(2):e27–34.
Kang SC, Lee DG, Choi JH, Kim ST, Kim YK, Ahn HJ. Association between estrogen receptor polymorphism and pain susceptibility in female temporomandibular joint osteoarthritis patients. Int J Oral Maxillofac Surg. 2007;36(5):391–4.
Aiken A, Bouloux G, Hudgins P. MR imaging of the temporomandibular joint. Magn Reson Imaging Clin N Am. 2012;20(3):397–412.
Guralnick W, Kaban LB, Merrill RG. Temporomandibular-joint afflictions. N Engl J Med. 1978;299(3):123–9.
Anderson DD, Marsh JL, Brown TD. The pathomechanical etiology of post-traumatic osteoarthritis following intraarticular fractures. Iowa Orthop J. 2011;31:1–20.
Lotz MK, Kraus VB. New developments in osteoarthritis. Posttraumatic osteoarthritis: pathogenesis and pharmacological treatment options. Arthritis Res Ther. 2010;12(3):211.
Lawrence RC, Felson DT, Helmick CG, Arnold LM, Choi H, Deyo RA, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part II. Arthritis Rheum. 2008;58(1):26–35.
Brown TD, Johnston RC, Saltzman CL, Marsh JL, Buckwalter JA. Posttraumatic osteoarthritis: a first estimate of incidence, prevalence, and burden of disease. J Orthop Trauma. 2006;20(10):739–44.
Muthuri SG, McWilliams DF, Doherty M, Zhang W. History of knee injuries and knee osteoarthritis: a meta-analysis of observational studies. Osteoarthr Cartil. 2011;19(11):1286–93.
Gelber AC, et al. Joint injury in young adults and risk for subsequent knee and hip osteoarthritis. Ann Intern Med. 2000;133(5):321–8.
Gelber AC, Hochberg MC, Mead LA, Wang NY, Wigley FM, Klag MJ. Body mass index in young men and the risk of subsequent knee and hip osteoarthritis. Am J Med. 1999;107(6):542–8.
Lohmander LS, Englund PM, Dahl LL, Roos EM. The long-term consequence of anterior cruciate ligament and meniscus injuries: osteoarthritis. Am J Sports Med. 2007;35(10):1756–69.
Neuman P, Englund M, Kostogiannis I, Friden T, Roos H, Dahlberg LE. Prevalence of tibiofemoral osteoarthritis 15 years after nonoperative treatment of anterior cruciate ligament injury: a prospective cohort study. Am J Sports Med. 2008;36(9):1717–25.
Lohmander LS, Östenberg A, Englund M, Roos H. High prevalence of knee osteoarthritis, pain, and functional limitations in female soccer players twelve years after anterior cruciate ligament injury. Arthritis Rheum. 2004;50(10):3145–52.
Roos H, Adalberth T, Dahlberg L, Lohmander LS. Osteoarthritis of the knee after injury to the anterior cruciate ligament or meniscus: the influence of time and age. Osteoarthr Cartil. 1995;3(4):261–7.
Lubowitz JH, Appleby D. Cost-effectiveness analysis of the most common orthopaedic surgery procedures: knee arthroscopy and knee anterior cruciate ligament reconstruction. Arthroscopy. 2011;27(10):1317–22.
Gianotti SM, Marshall SW, Hume PA, Bunt L. Incidence of anterior cruciate ligament injury and other knee ligament injuries: a national population-based study. J Sci Med Sport. 2009;12(6):622–7.
Parkkari J, Pasanen K, Mattila VM, Kannus P, Rimpela A. The risk for a cruciate ligament injury of the knee in adolescents and young adults: a population-based cohort study of 46 500 people with a 9 year follow-up. Br J Sports Med. 2008;42(6):422–6.
Yelin E, Callahan LF. The economic cost and social and psychological impact of musculoskeletal conditions. National Arthritis Data Work Groups. Arthritis Rheum. 1995;38(10):1351–62.
Losina E, Walensky RP, Reichmann WM, Holt HL, Gerlovin H, Solomon DH, et al. Impact of obesity and knee osteoarthritis on morbidity and mortality in older Americans. Ann Intern Med. 2011;154(4):217–26.
Little CB, Hunter DJ. Post-traumatic osteoarthritis: from mouse models to clinical trials. Nat Rev Rheumatol. 2013;9(8):485–97.
•• Christiansen BA, et al. Non-invasive mouse models of post-traumatic osteoarthritis. Osteoarthr Cartil. 2015;23(10):1627–38 This review discusses in detail the non-invasive animal models of post-traumatic osteoarthritis. The article covers findings of studies utilizing different methods to induce joint injury. The articles illustrates the significance of non-invasive models to study PTOA at various stages.
Kuyinu EL, Narayanan G, Nair LS, Laurencin CT. Animal models of osteoarthritis: classification, update, and measurement of outcomes. J Orthop Surg Res. 2016;11:19.
Anderson DD, Chubinskaya S, Guilak F, Martin JA, Oegema TR, Olson SA, et al. Post-traumatic osteoarthritis: improved understanding and opportunities for early intervention. J Orthop Res. 2011;29(6):802–9.
Furman BD, Strand J, Hembree WC, Ward BD, Guilak F, Olson SA. Joint degeneration following closed intraarticular fracture in the mouse knee: a model of posttraumatic arthritis. J Orthop Res. 2007;25(5):578–92.
Cho H, et al. Study of osteoarthritis treatment with anti-inflammatory drugs: cyclooxygenase-2 inhibitor and steroids. Biomed Res Int. 2015;2015:595273.
Poulet B, Hamilton RW, Shefelbine S, Pitsillides AA. Characterizing a novel and adjustable noninvasive murine joint loading model. Arthritis Rheum. 2011;63(1):137–47.
Wu P, Holguin N, Silva MJ, Fu M, Liao W, Sandell LJ. Early response of mouse joint tissue to noninvasive knee injury suggests treatment targets. Arthritis Rheumatol. 2014;66(5):1256–65.
Christiansen BA, Anderson MJ, Lee CA, Williams JC, Yik JHN, Haudenschild DR. Musculoskeletal changes following non-invasive knee injury using a novel mouse model of post-traumatic osteoarthritis. Osteoarthr Cartil. 2012;20(7):773–82.
Alomar X, Medrano J, Cabratosa J, Clavero JA, Lorente M, Serra I, et al. Anatomy of the temporomandibular joint. Semin Ultrasound CT MR. 2007;28(3):170–83.
Piette E. Anatomy of the human temporomandibular joint. An updated comprehensive review. Acta Stomatol Belg. 1993;90(2):103–27.
Vos LM, Kuijer R, Huddleston Slater JJR, Bulstra SK, Stegenga B. Inflammation is more distinct in temporomandibular joint osteoarthritis compared to the knee joint. J Oral Maxillofac Surg. 2014;72(1):35–40.
Hinton RJ, Serrano M, So S. Differential gene expression in the perichondrium and cartilage of the neonatal mouse temporomandibular joint. Orthod Craniofacial Res. 2009;12(3):168–77.
Benjamin M, Ralphs JR. Biology of fibrocartilage cells. Int Rev Cytol. 2004;233:1–45.
Shen G, Darendeliler MA. The adaptive remodeling of condylar cartilage---a transition from chondrogenesis to osteogenesis. J Dent Res. 2005;84(8):691–9.
Merida-Velasco JR, et al. Development of the human temporomandibular joint. Anat Rec. 1999;255(1):20–33.
Liang W, et al. Observing the development of the temporomandibular joint in embryonic and post-natal mice using various staining methods. Exp Ther Med. 2016;11(2):481–9.
Xu L, Polur I, Lim C, Servais JM, Dobeck J, Li Y, et al. Early-onset osteoarthritis of mouse temporomandibular joint induced by partial discectomy. Osteoarthr Cartil. 2009;17(7):917–22. https://doi.org/10.1016/j.joca.2009.01.002.
Almarza AJ, Brown BN, Arzi B, Ângelo DF, Chung W, Badylak SF, et al. Preclinical animal models for temporomandibular joint tissue engineering. Tissue Eng Part B Rev. 2018;24(3):171–8.
Poulet B. Non-invasive loading model of murine osteoarthritis. Curr Rheumatol Rep. 2016;18(7):40.
Chen J, Sorensen KP, Gupta T, Kilts T, Young M, Wadhwa S. Altered functional loading causes differential effects in the subchondral bone and condylar cartilage in the temporomandibular joint from young mice. Osteoarthr Cartil. 2009;17(3):354–61.
Bell DM, Leung KKH, Wheatley SC, Ng LJ, Zhou S, Wing Ling K, et al. SOX9 directly regulates the type-II collagen gene. Nat Genet. 1997;16(2):174–8.
Liu YD, Liao LF, Zhang HY, Lu L, Jiao K, Zhang M, et al. Reducing dietary loading decreases mouse temporomandibular joint degradation induced by anterior crossbite prosthesis. Osteoarthr Cartil. 2014;22(2):302–12.
Sobue T, Yeh WC, Chhibber A, Utreja A, Diaz-Doran V, Adams D, et al. Murine TMJ loading causes increased proliferation and chondrocyte maturation. J Dent Res. 2011;90(4):512–6.
Utreja A, Dyment NA, Yadav S, Villa MM, Li Y, Jiang X, et al. Cell and matrix response of temporomandibular cartilage to mechanical loading. Osteoarthr Cartil. 2016;24(2):335–44.
Izawa T, Mori H, Shinohara T, Mino-Oka A, Hutami IR, Iwasa A, et al. Rebamipide attenuates mandibular condylar degeneration in a murine model of TMJ-OA by mediating a chondroprotective effect and by downregulating RANKL-mediated osteoclastogenesis. PLoS One. 2016;11(4):e0154107.
Tanaka E, Detamore MS, Mercuri LG. Degenerative disorders of the temporomandibular joint: etiology, diagnosis, and treatment. J Dent Res. 2008;87(4):296–307.
Tung JT, Arnold CE, Alexander LH, Yuzbasiyan-Gurkan V, Venta PJ, Richardson DW, et al. Evaluation of the influence of prostaglandin E2 on recombinant equine interleukin-1beta-stimulated matrix metalloproteinases 1, 3, and 13 and tissue inhibitor of matrix metalloproteinase 1 expression in equine chondrocyte cultures. Am J Vet Res. 2002;63(7):987–93.
Gynther GW, Tronje G, Holmlund AB. Radiographic changes in the temporomandibular joint in patients with generalized osteoarthritis and rheumatoid arthritis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996;81(5):613–8.
Solberg WK, Woo MW, Houston JB. Prevalence of mandibular dysfunction in young adults. J Am Dent Assoc. 1979;98(1):25–34.
Katzberg RW. Temporomandibular joint imaging. Radiology. 1989;170(2):297–307.
Tvrdy P. Methods of imaging in the diagnosis of temporomandibular joint disorders. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2007;151(1):133–6.
Westesson PL, Bronstein SL. Temporomandibular joint: comparison of single- and double-contrast arthrography. Radiology. 1987;164(1):65–70.
Vilanova JC, Barceló J, Puig J, Remollo S, Nicolau C, Bru C. Diagnostic imaging: magnetic resonance imaging, computed tomography, and ultrasound. Semin Ultrasound CT MR. 2007;28(3):184–91.
Jung YW, Park SH, On SW, Song SI. Correlation between clinical symptoms and magnetic resonance imaging findings in patients with temporomandibular joint internal derangement. J Korean Assoc Oral Maxillofac Surg. 2015;41(3):125–32.
Koos B, Twilt M, Kyank U, Fischer-Brandies H, Gassling V, Tzaribachev N. Reliability of clinical symptoms in diagnosing temporomandibular joint arthritis in juvenile idiopathic arthritis. J Rheumatol. 2014;41(9):1871–7.
Lamot U, Strojan P, Surlan Popovic K. Magnetic resonance imaging of temporomandibular joint dysfunction-correlation with clinical symptoms, age, and gender. Oral Surg Oral Med Oral Pathol Oral Radiol. 2013;116(2):258–63.
Cho H, Bhatti FUR, Lee S, Brand DD, Yi AK, Hasty KA. In vivo dual fluorescence imaging to detect joint destruction. Artif Organs. 2016;40(10):1009–13.
Lim NH, Vincent TL, Nissim A. In vivo optical imaging of early osteoarthritis using an antibody specific to damaged arthritic cartilage. Arthritis Res Ther. 2015;17:376.
Cho H, Kim BJ, Park SH, Hasty KA, Min BH. Noninvasive visualization of early osteoarthritic cartilage using targeted nanosomes in a destabilization of the medial meniscus mouse model. Int J Nanomedicine. 2018;13:1215–24.
Cho H, Bhatti FUR, Yoon TW, Hasty KA, Stuart JM, Yi AK. Non-invasive dual fluorescence in vivo imaging for detection of macrophage infiltration and matrix metalloproteinase (MMP) activity in inflammatory arthritic joints. Biomed Opt Express. 2016;7(5):1842–52.
•• Cho H, et al. Detection of early cartilage damage using targeted nanosomes in a post-traumatic osteoarthritis mouse model. Nanomedicine. 2015;11(4):939–46 This study describes that use of fluorescent labeled anti type II collagen antibody can detect early cartilage damage in a mouse model of osteoarthritis. This detection method may also prove to be useful for targeted delivery of drugs in the future.
Funding
H.C. was supported by grants from Arthritis Foundation (Discovery Award), and Oxnard Foundation (Medical Research Award).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
FB, AK, BSL, TD, DK, HC declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any original studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Craniofacial Skeleton
Rights and permissions
About this article
Cite this article
Bhatti, FUR., Karydis, A., Lee, B.S. et al. Understanding Early-Stage Posttraumatic Osteoarthritis for Future Prospects of Diagnosis: from Knee to Temporomandibular Joint. Curr Osteoporos Rep 19, 166–174 (2021). https://doi.org/10.1007/s11914-021-00661-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-021-00661-3