Abstract
Purpose of Review
Osteogenesis is a complex process involving the specification of multiple progenitor cells and their maturation and differentiation into matrix-secreting osteoblasts. Osteogenesis occurs not only during embryogenesis but also during growth, after an injury, and in normal homeostatic maintenance. While much is known about osteogenesis-associated regulatory genes, the role of microRNAs (miRNAs), which are epigenetic regulators of protein expression, is just beginning to be explored. While miRNAs do not abrogate all protein expression, their purpose is to finely tune it, allowing for a timely and temporary protein down-regulation.
Recent Findings
The last decade has unveiled a multitude of miRNAs that regulate key proteins within the osteogenic lineage, thus qualifying them as “ostemiRs.” These miRNAs may endogenously target an activator or inhibitor of differentiation, and depending on the target, may either lead to the prolongation of a progenitor maintenance state or to early differentiation. Interestingly, cellular identity seems intimately coupled to the expression of miRNAs, which participate in the suppression of previous and subsequent differentiation steps. In such cases where key osteogenic proteins were identified as direct targets of miRNAs in non-bone cell types, or through bioinformatic prediction, future research illuminating the activity of these miRNAs during osteogenesis will be extremely valuable.
Summary
Many bone-related diseases involve the dysregulation of transcription factors or other proteins found within osteoblasts and their progenitors, and the dysregulation of miRNAs, which target such factors, may play a pivotal role in disease etiology, or even as a possible therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Birth defects that affect the skeleton account for 5% of all infant deaths. In survivors, skeletal defects can result in lifelong burdens ranging from stunted growth and malformations to poor bone density and the need for surgery. The key to understanding normal and abnormal bone formation, in addition to finding possible treatments for bone disorders, lies in studying the genetic regulation of osteogenesis. Recent advances in genomics have led to the discovery of endogenous small RNA molecules, known as microRNAs (miRNAs, miRs), which regulate genetic expression at the transcript level through degradation or a translational halt of the target transcript. Understanding how miRNAs contribute to the regulation of osteogenesis may provide insights into the molecular causality of skeletal defects and disorders.
Faulty Osteogenesis as the Root Cause of Skeletal Defects
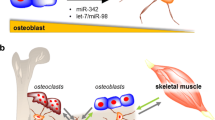
Osteogenesis describes the process of bone formation during early development, bone homeostasis in adults, and bone remodeling after an injury. Osteoblasts, the cells that secrete a bone-specific extracellular matrix (ECM), which later becomes calcified and mineralized (Fig. 1), is derived from progenitor cells of a distinct germ layer origin in the embryo. Vertebrae and some craniofacial bones are derived from paraxial mesoderm, while the appendicular skeleton, or long bones, are derived from lateral plate mesoderm [5]. The majority of the craniofacial bones and cartilage however are derived from cranial neural crest cells (NCCs).
Osteogenesis in the long bones and from cranial neural crest cells. In the lateral mesoderm-derived long bones, osteoblasts are created through three different processes: (i) in the perichondrium, they are directly differentiated from mesenchymal cells; (ii) in trabecular bone, they are also created from mesenchymal cells, but with influence from hypertrophic chondrocytes; (iii) trabecular osteoblasts, according to recent lineage tracing evidence, may also derive from transdifferentiating hypertrophic chondrocytes [1,2,3,4]. In contrast, neural crest-derived craniofacial bone is differentiated from cranial neural crest cells that specify at the neural plate border, which later delaminate and become migratory. Through intramembranous ossification, these crest-derived progenitors first differentiate into mesenchyme, which directly converts into pre-osteoblasts without a cartilage intermediate. Developmental trajectory is denoted by encircled numbers
Independent of their origin, bone progenitor cells condense at sites of future skeletal element formation. These condensations are composed of loosely packed mesenchymal cells, which during endochondral ossification differentiate into chondrocytes, undergo hypertrophy, apoptosis, and are later replaced by osteoblasts [5] (Fig. 1). Recent lineage-tracing experiments ended a decade long debate whether the cartilage anlage was necessary for mesodermal progenitors to differentiate into osteoblasts. That it was dispensable was demonstrated by showing that a subset of collagen X expressing hypertrophic chondrocytes survive and can directly transdifferentiate into osteoblasts [1,2,3,4] (Fig. 1), a hypothesis that had long been fueled by the fact that these transitory chondrocytes begin to express Runt-related factor 2 (Runx2) [6,7,8], a master osteogenic transcription factor (TF) [9•]. In contrast, during intramembranous ossification or dermal bone formation, progenitor cells of neural crest cell origin differentiate directly into osteoblasts (reviewed in [10]) (Fig. 1). In cases where mesenchymal cells commit directly to the osteogenic lineage, they first form pre-osteoblasts, which have the ability to proliferate expansively [11]. Osteocytes, the terminally matured osteoblasts, are fully surrounded by ECM and communicate with each other through dendritic processes to sense mechanical stimuli and regulate mineral homeostasis [12•].
Dysregulation of any event during osteogenesis can result in a wide array of skeletal disorders and diseases. While cleft lip and palate may be visibly apparent immediately at birth [13], others, such as osteogenesis imperfecta (OI) or brittle bone disease, present a variety of symptoms from loose joints to weak bones, which cause dysmorphism and premature death later in life [14]. Some rarer diseases, such as fetal skeletal dysplasia, exhibit stunted bone growth, poor mineralization, and limb agenesis [15]. The underlying causes may be genetic, including mutations in genes such as collagen and fibroblast growth factor receptors, or may be environmental such as in the case of phosphate or vitamin D metabolism deficiency [15].
Transcriptional Control of Osteogenesis
The etiology of skeletal malformations is often associated with the misregulation of the genes coding for ECM proteins or master transcription factors. In osteogenesis, master lineage regulatory TFs include Runx2, also known as Core-binding factor α1, and Osterix (Osx) [16]. RUNX2 controls the promoters of all major osteoblast ECM genes, including Col1a1 (type I collagen), Spp1 (osteopontin), Ibsp (bone sialoprotein, BSP), and Bglap (osteocalcin, OCN), the transcription of which contributes to the establishment of an osteoblast phenotype [9•, 17]. Consequently, disrupted Runx2 results in a complete lack of bone [6]. Furthermore, mutations in RUNX2 that diminish protein activity can lead to cleidocranial dysostosis [18], a disease characterized by absent parietal bones and delayed skull ossification [19].
As a central mediator of osteogenesis, RUNX2 executes signals from the Wnt, bone morphogenetic protein (BMP), and fibroblast growth factor (FGFs) signaling pathways [16, 20,21,22]. In Runx2 expressing cells, Osx is responsible for their final commitment to mature osteoblasts [23]. OSX works partially through activating the Wnt signaling pathway [24], downstream of which transcription of Runx2 is activated [25]. Thus, it appears that Runx2 and Osx work in a feed-forward loop that implements the osteogenic phenotype [26•].
microRNAs in Disease Etiology and Development
The molecular underpinnings of osteogenic gene expression have been extensively studied in a variety of model organisms [26•], but only recently have we started to explore the critical roles that miRNAs play in their regulation. After the first miRNA, lin-4, was discovered in Caenorhabditis elegans [27•], it was subsequently found that miRNAs were highly conserved throughout the animal kingdom, as well as in plants [28,29,30]. Furthermore, genetic studies in animal models demonstrated that miRNAs play crucial roles in animal development [31, 32] and disease etiology [33, 34]. Instead of representing all-or-nothing on/off switches, miRNAs fine-tune gene expression by dampening protein expression epigenetically through binding to the 3′ UTR of mRNA transcripts [35]. Accelerated deadenylation and subsequent decapping destabilizes these mRNAs [36], ultimately reducing protein abundance.
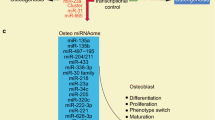
Usually found throughout intergenic regions of the genome, miRNA genes often cluster together, such that they can be transcribed as poly-cistronic transcripts [37] (Fig. 2). Polymerase II transcription generates a stem-loop structure containing the primary miRNA (pri-miRNA), which can range in size from hundreds of nucleotides up to kilobases [47]. The pri-miRNA then adopts a secondary stem loop structure, which undergoes nuclear cleavage by a multiprotein complex. The core components of this complex are the RNase III enzyme Drosha and the dsRNA-binding domain protein DGCR8 (DiGeorge syndrome chromosomal [or critical] region 8) [48]. The resulting hairpin-shaped pre-miRNA, which is about 65 nucleotides long, contains a 2-nt 3′ overhang that is recognized by exportin-5, allowing nuclear export via a Ran-GTP-dependent mechanism [40]. microRNAs, which are encoded in introns and are part of the primary mRNA transcript, are processed by the spliceosome, which also produces a pre-miRNA that is then shuttled into the cytoplasm for further processing via the same mechanism [38, 39].
microRNA biogenesis and target recognition. miRNAs encoded in intergenic regions can be transcribed between exons or as polycistronic miRNAs by RNA polymerase II/III [37]. Single transcribed miRNAs are spliced out of the exons by the spliceosome into a hairpin structure known as pre-miRNAs, while polycistronic miRNAs are known as pri-miRNAs before being processed to single pre-miRNAs by DROSHA and DGCR8 proteins [38, 39]. The pre-miRNAs are then exported from the nucleus via Exportin-5 [40]. The hairpin loop of the pre-miRNA is then cleaved off by Dicer, forming a miRNA duplex [41], and loaded onto the RNA induced silencing complex (RISC) via Argonaut proteins [42, 43]. The miRNA along with RISC is then loaded onto the target mRNA transcript and can halt transcription [43] or cause degradation by exonuclease activity [44,45,46]
Next, the pre-miRNA is cleaved by cytoplasmic Dicer to produce the mature ~19–25 nt miRNA duplex [41]. The miRNA strand with the lower relative thermodynamic stability of base-pairing at its 5′ end is then loaded onto an Argonaut protein and incorporated into the RNA-induced silencing complex (RISC). This results in a mature miRNA, which is then directed to the 3′ UTR of the target mRNAs [42]. Based on partial complementarity, the mRNA targets are then blocked from being translated [43] or directed to the cellular 5′-to-3′ mRNA decay pathway. There, mRNAs are first deadenylated, decapped, and ultimately degraded by the cytoplasmic 5′-to-3′ exonuclease XRN1 [44,45,46].
Based on these mechanisms, the regulatory nature of miRNAs is multifold. Due to the partial complementarity described above, one miRNA may have several target sites in the 3′UTR of a single mRNA, and one 3′UTR has tens to hundreds of different binding sites for different miRNAs. Thus, multiple co-expressed miRNAs may act in concert to ensure that the expression of a specific mRNA is repressed as efficiently as possible. In addition, because one miRNA has multiple distinct mRNA targets, a down-regulated miRNA may offset the up-regulation of another in the control of a common target mRNA. Given these considerations, it appears that the complexity of osteogenesis is compounded by miRNA expression as well as by any feedback regulation that may exist between the microRNAs and their targets, a few examples of which will be discussed in this review.
Of the hundreds of miRNAs confirmed to exist, a subset of them associated with terminal osteoblast differentiation and acquisition of osteogenic identity from already committed progenitors have been designated “ostemiR” [49•]. This review discusses the role of microRNAs during early and late specification of progenitor cells with a particular emphasis on osteogenic potential in the craniofacial skeleton. In addition to the known ostemiRs (Table 1), we also discuss miRNAs that silence proteins associated with osteogenesis in non-bone tissues.
microRNAs that Control Osteoblast Identity and Homeostasis
Osteoblasts secrete a variety of unique proteins that comprise an extremely specialized ECM. A subset of these serve as a scaffold upon which mineral is deposited in a final maturation step, while others impart structural flexibility to withstand compressive and tensile stress. Any microRNA targeting the mRNAs for the non-collagenous glycoproteins and proteoglycans such as osteonectin, BSP, and OCN, which are all implicated in calcification of the ECM [80], would execute an important control over matrix mineralization. Consequently, the osteonectin-targeting miR-29a and -29c appear to play a role in osteoblast maturation and indeed, their expression levels increase during late osteogenesis [50]. Similarly, miR-125b, which directly targets the OCN mRNA, Bglap, is highly expressed in primary human osteoblasts isolated from human trabecular bone and thus is implicated in normal bone homeostasis [52].
In bone, vitamin D bound to its receptor, VDR, participates in the mineralization process, and disruption to the VDR pathway can lead to mineralization defects such as those found in Rickets [81]. The importance of miR-125b in osteoblast identity is further illustrated in the fact that exogenous miR-125b blocked differentiation, while in contrast, its inhibition indirectly yielded higher ALP activity [82]. Furthermore, in breast and prostate cancer, which often metastasize to bone [83], down-regulation of miR-125b results in increased expression of its target Vdr [53], again demonstrating the importance of miR-125b in osteogenesis. While the only currently reported miRNAs directly targeting the bone-type Alpl are miR-204/211 [54], 16 additional conserved miRNA binding sites are predicted in its 3′UTR (microrna.org). Since expression of ALP not only maintains, but also initiates matrix mineralization, thusly associating with earlier stages of osteogenesis, the miRNAs post-transcriptionally regulating this enzyme may be expressed by mesenchymal stem cell as was indeed confirmed for miR-204 [71•].
Once fully embedded in the matrix, osteoblasts take on new functions as they terminally differentiate into osteocytes, which sense and respond to mechanical stimulation in a bone-anabolic manner. This response is mediated by cyclooxygenase-2 (COX2) [84, 85], which produces proliferation-stimulating prostaglandins [86]. While no Cox2-regulating microRNAs have been identified in the context of osteoblasts or mechanical loading, miR-101a and miR-199a down-regulate Cox2 in early mouse embryos during implantation [55]. Identified in several miRNA screens, miR-199a associates with osteoblast differentiation [87, 88], suggesting that its identification as an ostemiR may be linked to its control of Cox2. Additionally, while not directly linked to Cox2, miR-218, miR-191*, miR-3010a, and miR-33 were recently identified in MC3T3-E1 osteoblastic cells to be responsive to mechanical strain [89].
miRNAs Expressed at the Preosteoblast Stage
Prior to matrix calcification, proliferating osteoprogenitors secrete OPN [90], encoded by Spp1. While several microRNAs have been associated with Spp1 regulation (i.e., miR-541 [49•]; miR-21 [91]), no miRNA directly silencing Spp1 has been identified in osteoblasts or their precursors. However, miR-299-5p targets Spp1 in breast cancer cells [57] and miR-127-5p targets Spp1 in chondrocytes [58] and thus they may also do so in pre-osteoblasts.
The non-collagenous component of the ECM constitutes only a small portion. In fact, over 90% of the secreted ECM proteins are collagenous fibrils, primarily those of type I collagen. Since collagen is so abundant, it is not surprising that perturbation of collagen production is a root cause of OI [92, 93]. Any miRNA regulating collagen genes may thus not only be important for normal osteogenesis, but their misregulation could potentially be implicated in the etiology of OI. For example, miR-29b directly regulates Col1a1, Col1a2, and Col3a1 in hepatic cells [59], but this has not yet been replicated in cells of the osteogenic lineage. Secretion of ECM proteins decreases in association with prolonged differentiation, and the function of miR-29b in osteoblasts could be to suppress the expression of collagen proteins allowing the collagen fibril matrix to mature for mineral deposition [94]. Consequently, the expression of miRNAs similar to miR-29b would be expected to be higher as osteoblasts transition to the calcification step.
Rat mesenchymal stem cells overexpressing miR-21 exhibit enhanced performance in a fracture healing model in vivo [91]. The pro-osteogenic effect of miR-21 may occur through an indirect regulation of Col1a1, since miR-21 indirectly causes elevated expression of Col1a1 and in turn deposition of type I collagen, in a murine model of lung fibrosis [95]. Interestingly, recombinant COL1A1 positively regulates miR-21 expression, illustrating an unknown mechanistic feedback loop between protein and miRNA that likely prevents complete transcript shut-off [95]. miR-21 is also increased by the pro-osteogenic TGFβ and BMPs, but surprisingly not through transcriptional control, but rather through enhanced processing of the pri-miRNA [96•]. The designation of miR-21 as an ostemiR is however controversial, because miR-21 is up-regulated in most types of cancer [97].
Another ECM protein produced in pre-osteoblasts is fibronectin, an adhesion protein, which binds to integrins to influence cell proliferation and tissue development [98, 99]. Although miR-200b and miR-377 regulate fibronectin in kidney proximal tubular cells and in diabetic neuropathy respectively, a role for these miRNAs in osteogenesis remains to be determined [60, 61]. Interestingly, miR-377 is expressed during osteogenic differentiation of human dental pulp stem cells [100] and is up-regulated in response to contact of human osteoblast-like MG-63 cells with osteo-inductive biomaterials used for surgical bone restoration [101, 102].
microRNAs Associated with the Mesenchymal State and Mesenchymal Commitment
Mesenchymal stem or stromal cells (MSCs) have the potential to generate skeletal as well as connective tissue [103]. Markers that define MSC identity have been agreed on by the International Society for Cellular Therapy to include the surface expression of CD90, CD73, and CD105 [104]. In terms of microRNAs however, none are known to directly target the corresponding mRNAs during osteogenesis. The only existing evidence comes from cancer cell lines, in which miR-422 targets Nt5e (codes for CD73) [62] and miR-370 negatively regulates Eng (codes for CD105) [63].
Another surface glycoprotein shared by MSCs is CD44, which functions in adhesion and migration and binds hyaluronan and OPN [105]. In both human renal and prostate cancer cells, CD44 has been identified as a direct target of miR-34a [64], a miRNA that promotes osteogenesis in human adipose-derived stem cells [106]. In addition, the 3′UTR of CD146, which has been associated with a higher potential for osteogenic differentiation [107], is directly targeted by miR-329 in endothelial cells [65]. Also, in endothelial cells, expression of Vcam1, which encodes the cell-cell adhesion molecule CD106 and reduces the migratory ability of MSCs [108], is controlled by miR-126 [109]. However, again, direct regulation has yet to be confirmed in osteoblasts or their precursors. Potentiating the MSC state is miR-140-5p, which inhibits osteogenic lineage commitment and is commonly enriched in undifferentiated human MSCs from various tissue sources [110]. In zebrafish, injection of miR-140-5p phenocopies Bmp2 repression, resulting in aberrant embryonic bone development (short stature, curved trunk, craniofacial malformations) and confirming a direct relationship between the two [111, 112].
For expression of pre-osteoblastic matrix genes to occur, which turn MSCs into pre-osteoblasts and later mature osteoblasts, the master TFs RUNX2 and OSX must be genetically activated. miR-125b, a miRNA identified in MSCs throughout many genetic screens [100, 113], is predicted to target Osx. However, a relationship has not been confirmed beyond the finding of reduced Osx mRNA [114]. In contrast, miR-143 [66, 67], miR-145 [66], miR-214 [68], and miR-637 [69] suppress osteogenic differentiation by directly targeting Osx. Due to the ability of miR-322 to directly target Tob2, which normally helps to degrade Osx, Osx mRNA is stabilized, allowing osteoblast differentiation to occur [70].
Genetic manipulation of Runx2 in vivo indicated that its expression is both necessary and sufficient for mesenchymal cell differentiation towards the osteoblast lineage [115, 116]. Discovered as endogenous attenuators of Runx2 expression, which prevent cells from differentiating into osteoblasts, the inhibition of miR-23a, miR-34c, miR-628-3p miR-137, miR-204, miR-205, miR-338-3p, miR-433, miR-375, and miR-135 promoted osteoblast differentiation along with an increase in bone-specific markers [56, 71•, 72,73,74,75,76,77, 79, 117]. A recent publication bioinformatically identified additional microRNAs predicted to target Runx2 [118]. These include miR-141, miR-200a, and miR-200b, whose expression is expected to be down-regulated as differentiation progresses, but remain high in mesenchymal cells thus representing MSC markers. Alternatively, a microRNA may qualify as an ostemiR if its expression is up-regulated and it targets inhibitors of RUNX2, as is the case for miR-129-5p, which targets the signal transducer and activator of transcription 1 [119] that normally sequesters RUNX2 in the cytoplasm to prevent its nuclear activity [78].
In the nucleus, RUNX2 may regulate transcription not only of genes, but also of miRNAs, such as the pro-osteogenic miR-690 [88] and miR-1192 [120]. In contrast, RUNX2 represses the promoter of the miR23a~27a~24–2 cluster [76]. The consequence of this negative feed-forward loop is to cause depression of special AT-rich sequence-binding protein 2 (Satb2), a scaffold protein that increases RUNX2 activity to promote differentiation. This is an interesting example of a cluster, in which all three miRNAs share Satb2 as a common target, but only one of them, miR-23a, targets Runx2, the attenuation of which seems to fine tune the pace of progression of the osteoblast phenotype rather than switching it off completely.
Two miRNAs that directly target Satb2, miR-34b and miR-34c, were shown to affect osteoblast proliferation and differentiation in vivo [79]. SATB2 itself has recently been implicated as a major osteogenic TF, since Satb2 −/− mice exhibit craniofacial abnormalities [121]. Satb2 is expressed in cells of the osteoblast lineage in developing mice [121] and was reported to function both upstream and downstream of RUNX2 and OSX [121,122,123,124]. Due to its participation in regulatory feedback loops together with RUNX2 and miRNAs, this implicates Satb2 in the acquisition of an osteoprogenitor fate from both the NC and the mesoderm-derived progenitor cells.
One such feedback loop comprises miR-31, whereby in bone marrow MSCs, RUNX2 occupies and activates transcription from the miR-31 promoter, which in turn lowers Satb2 mRNA and protein expression [123]. While a more recent paper suggests the same feedback loop directs dental follicle cells towards osteogenesis [125], neither of the two studies provides evidence for the direct binding of miR-31 to the 3′UTR of Satb2. Other studies place SATB2 upstream of RUNX2 protein and under inflammatory conditions, TNFα-activated miR-33-5p can reduce RUNX2 by directly targeting Satb2 [124].
Due to the negative regulation of their target transcripts, it would be expected that any miRNA targeting Satb2 directly would be down-regulated to induce osteogenic commitment. miR-205, for instance, exhibits this expression pattern during bone marrow MSC differentiation, and its inhibition promotes osteogenesis [77]. However, this is another example of a miRNA for which Satb2 regulation is predicted, but has not yet been experimentally confirmed.
microRNAs Involved in Neural Crest Induction and Differentiation
Some osteomiRs participate in the direct conversion of a mesenchymal cell into an osteoblast, such as in the cases of intramembranous ossification or in the perichondrium. Yet others, which are not discussed here, may modulate endochondral bone formation through tuning chondrogenic differentiation from mesenchymal cells. In addition, microRNAs may also take part in the newly discovered transdifferentiation of hypertrophic chondrocytes into osteoblasts [1,2,3,4].
The general importance of microRNAs in the specification of neural crest cell (NCC)-derived bone in the skull, which is formed via intramembranous ossification, became apparent in conditional knockouts of Dgcr8 (which processes nuclear miRNAs) in cranial NCCs [126, 127•]. Although the role of individual miRNAs during NCC development has not been thoroughly analyzed, miRNAs likely contribute to the intricate, multi-step process of craniofacial cartilage and bone formation. This developmental process is controlled by a number of transcription factors that interact in a so-called gene-regulatory network (GRN), governed by feedback loops and repetitive gene expression (Table 2, see also [128•]). However, virtually nothing is known about the miRNAs governing most of the genes in the GRN that regulate NCC specification and development.
The classical theory of NCC specification proposes a partition of a dorsal subset of neuroepithelial cells from the neural tube as the source for NCCs [130]. More recently, it has been proposed that specification occurs during gastrulation and is initiated by neural plate border specifier genes such as Pax7 [131•, 132]. Originally identified as being required for muscle cell differentiation, homeostasis, and repair [133], Pax7 is targeted directly by miR-431 in muscle satellite cells, the overexpression of which increases myogenic differentiation [134]. Thus, misexpression of miR-431 could negatively impact NCC development.
Once the expression of neural plate border specifiers is initiated, Pax7 engages with other border specifiers such as Gbx2, Zic1/3, and Tfap2, in a mutual cross regulatory network (reviewed in [128•]). Only one silencing miRNA has been identified each for Zic3 and Tfap2 mRNAs, namely, miR-564 [135] and miR-214 [136], respectively. Since the cross-regulation of border specifier genes ensures the stabilization of NCC identity, allowing for continued expression of this gene set through subsequent developmental stages, it is highly likely that the misexpression of regulatory miRNAs would disrupt this network. In addition, the neural plate border genes not only control genes within their own network, but also inhibit neural transcription factors (and vice versa) to sharply define cellular identity in the border region [137]. Hence, overexpression of the neural specifiers Sox2/3, which can occur through an absence of microRNA control (i.e., miR-126 [138]), would result in the repression of NCC identity.
Presumptive NCCs reside at the junction between the neural plate and the preplacodal ectoderm and begin to express of a set of NCC specifier genes, among them Snai1/2, FoxD3, and Sox10 [127•]. The only miRNA identified to regulate Foxd3, miR-429, is currently only known to participate in skin pigmentation [139]. In human hepatocellular carcinoma, FOXD3 activates miR-137 transcription, which decreases proliferation and migration in tumor cells [117]. The role of miR-137 in hepatocellular carcinoma may mirror a similar role in NCCs to slow down proliferation and migration and ultimately maintain or expand the NCC pool.
Following specification, NCCs undergo delamination and leave the neural tube, where they migrate dorsolaterally and differentiate into diverse cell types. This progression requires frequent switches between epithelial and mesenchymal states [140,141,142] similarly observed in cancer metastasis and involves the same reiterated use of a TF machinery including TWIST1 and MSX1/2 [143,144,145,146]. Interestingly, Twist1, which is downregulated by miR-1271 in pancreatic cancer cells [147], is a NCC-specifier gene [128•], which is also necessary for maintaining NCCs after migration, facilitating the formation of craniofacial bone [148]. In turn, Msx1/2 are expressed at the plate border as well as in migrating NCCs, which later re-express Msx2 as well as Dlx5/6 as they transition into mesenchymal osteoprogenitors [149, 150]. Due to their co-regulation of RUNX2 [151], deficiencies in Msx1/2 cause severe cranioskeletal abnormalities, and deletion of both Msx1 and Msx2 cause late gestation lethality [152]. miR-322 indirectly increases Msx2 expression [70] and therefore it is possible that this regulatory mechanism occurs during the migration of NCCs. In turn, the Dlx5 silencing miR-141 and miR-200a [150] may control both the early induction as well as the differentiation of NCCs.
Due to the limited information available on miRNAs that regulate NCC development, we conducted an elementary search for predicted miRNAs using the published GRN and the miRanda algorithm (microRNA.org). Additional helpful hypothetical lists of candidate miRNAs with potential involvement in NC development can be found in a recent review [153]. In total, 201 candidate miRNAs were identified (Table 2), 126 of which (62.7%) targeted more than 1 GRN gene and 25 of which targeted more than 5 genes (Fig. 3). Four of these miRNAs are predicted to silence 10 of the 22 GRN genes across multiple steps of NCC development (Fig. 3 and Table 2). These, we consider the most powerful miRNAs as they may possess the potential to completely block the NC developmental program. Of the 120 candidate miRNAs that specifically target NC specifiers, 8 target 5 or more mRNAs, possibly explaining the co- and inter-regulation of neural crest specifier genes that is necessary to maintain the NC in an undifferentiated state [154]. Intriguingly, seven of these overlap with miRNAs that regulate multiple stages, except for miR-489, which seems specific to neural crest specifiers.
microRNAs potentially implicated in neural crest osteogenesis. Candidate miRNAs predicted to target neural crest GRN genes categorized according to the potential stages of neural crest development they may regulate. Candidate microRNAs that are predicted to target genes in the neural crest gene regulatory network (adopted from [128•]) were assembled with the miRanda algorithm available at microRNA.org [129] and categorized according to the expression of their targets during neural crest development. Based on mouse miRNAs, only conserved microRNAs with a good miRSVR score were taken into account
One of the miRNAs potentially regulating nine different GRN genes is miR-1192, a miRNA induced by RUNX2. This interesting coincidence suggests that once a cell has committed to a specific lineage, it ensures it does not revert back in developmental time. Moreover, 15 of the candidate GRN miRNAs target Runx2, Osx, and/or Satb2, which could be interpreted as a safeguard that helps lock-in a specific cell fate. For instance, considering that miR-204 expression would block the neural plate border state and simultaneously prevent Runx2 expression, it may therefore be expressed by NCCs to preserve NCC identity. A slightly different scenario may occur with miR-217, which targets both border and NC specifier genes. Here, additional targeting of Runx2 may take place in a more mature osteoblast to block all prior cell states.
Conclusion
This review discussed the different stages of osteogenesis bringing together different miRNAs and their targets, the disruption of which may potentially cause severe malformations or deformities. Interestingly, cellular identity is intimately coupled to the expression of miRNAs suppressing previous and subsequent differentiation steps. miRNAs may promote osteogenic differentiation and matrix mineralization through targeting genes with functions in osteoclastogenesis and chondrogenesis and/or signaling, and thus may also qualify as ostemiRs. Although some miRNA target identification has occurred in non-bone cell types, or by bioinformatic prediction, future research illuminating the activity of these miRNAs during (NC-) osteogenesis will be extremely valuable.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Park J, Gebhardt M, Golovchenko S, Perez-Branguli F, Hattori T, Hartmann C, et al. Dual pathways to endochondral osteoblasts: a novel chondrocyte-derived osteoprogenitor cell identified in hypertrophic cartilage. Biol Open. 2015;4(5):608–21.
Yang G, Zhu L, Hou N, Lan Y, Wu XM, Zhou B, et al. Osteogenic fate of hypertrophic chondrocytes. Cell Res. 2014;24(10):1266–9.
Yang L, Tsang KY, Tang HC, Chan D, Cheah KS. Hypertrophic chondrocytes can become osteoblasts and osteocytes in endochondral bone formation. Proc Natl Acad Sci U S A. 2014;111:12097–102.
Zhou X, von der Mark K, Henry S, Norton W, Adams H, de Crombrugghe B. Chondrocytes transdifferentiate into osteoblasts in endochondral bone during development, postnatal growth and fracture healing in mice. PLoS Genet. 2014;10:e1004820.
Gilbert SF. Osteogenesis: the development of bones. Dev Biol 10th ed. Sunderland: Sinauer Associates, Inc.; 2014. P. 432.
Komori T, Yagi H, Nomura S, Yamaguchi A, Sasaki K, Deguchi K, et al. Targeted disruption of Cbfa1 results in a complete lack of bone formation owing to maturational arrest of osteoblasts. Cell. 1997;89:755–64.
Otto F, Thornell AP, Crompton T, Denzel A, Gilmour KC, Rosewell IR, et al. Cbfa1, a candidate gene for cleidocranial dysplasia syndrome, is essential for osteoblast differentiation and bone development. Cell. 1997;89:765–71.
Inada M, Yasui T, Nomura S, Miyake S, Deguchi K, Himeno M, et al. Maturational disturbance of chondrocytes in Cbfa1-deficient mice. Dev Dyn. 1999;214:279–90.
• Ducy P, Zhang R, Geoffroy V, Ridall AL, Karsenty G. Osf2/Cbfa1: a transcriptional activator of osteoblast differentiation. Cell. 1997;89:747–54. This paper was the first to identify and clone Runx2 , also known as Cbfa1 , identifying it as a master activator of osteoblast differentiation by showing transcription of osteoblastic genes in non-osteoblastic cells.
Keller KC, zur Nieden NI. Osteogenesis from pluripotent stem cells: neural crest or mesodermal origin? In: Kallos MS, editor. Embryonic stem cells—differentiation and pluripotent alternatives, InTech; 2011. p. 323–48.
Huang B, Wang Y, Wang W, Chen J, Lai P, Liu Z, et al. mTORC1 prevents preosteoblast differentiation through the notch signaling pathway. PLoS Genet. 2015;11(8):e1005426.
• Bonewald LF. The amazing osteocyte. J Bone Miner Res. 2011;26(2):229–38. A comprehensive review on the function of osteocytes in bone, including a historic view on how osteocytogenesis was discovered to be an active process.
Shkoukani MA, Chen M, Vong A. Cleft lip—a comprehensive review. Front Pediatr Frontiers Media SA. 2013;1:53.
Trejo P, Rauch F. Osteogenesis imperfecta in children and adolescents—new developments in diagnosis and treatment. Osteoporos Int. 2016;27(12):3427–37.
Barkova E, Mohan U, Chitayat D, Keating S, Toi A, Frank J, et al. Fetal skeletal dysplasias in a tertiary care center: radiology, pathology, and molecular analysis of 112 cases. Clin Genet. 2015;87:330–7.
Nakashima K, Zhou X, Kunkel G, Zhang Z, Deng JM, Behringer RR, et al. The novel zinc finger-containing transcription factor osterix is required for osteoblast differentiation and bone formation. Cell. 2002;108:17–29.
Ducy P, Karsenty G. Two distinct osteoblast-specific cis-acting elements control expression of a mouse osteocalcin gene. Mol Cell Biol. 1995;15:1858–69.
Quack I, Vonderstrass B, Stock M, Aylsworth AS, Becker A, Brueton L, et al. Mutation analysis of core binding factor a1 in patients with cleidocranial dysplasia. Am J Hum Genet. 1999;65:1268–78.
Mundlos S. Cleidocranial dysplasia: clinical and molecular genetics. J Med Genet. 1999;36:177–82.
Woei Ng K, Speicher T, Dombrowski C, Helledie T, Haupt LM, Nurcombe V, et al. Osteogenic differentiation of murine embryonic stem cells is mediated by fibroblast growth factor receptors. Stem Cells Dev. 2007;16:305–18.
Åberg T, Wang X-P, Kim J-H, Yamashiro T, Bei M, Rice R, et al. Runx2 mediates FGF signaling from epithelium to mesenchyme during tooth morphogenesis. Dev Biol. 2004;270:76–93.
Zhang YW, Yasui N, Ito K, Huang G, Fujii M, Hanai J, et al. A RUNX2/PEBP2alpha a/CBFA1 mutation displaying impaired transactivation and Smad interaction in cleidocranial dysplasia. Proc Natl Acad Sci. 2000;97:10549–54.
Sinha KM, Zhou X. Genetic and molecular control of osterix in skeletal formation. J Cell Biochem. 2013;114:975–84.
Niger C, Luciotti MA, Buo AM, Hebert C, Ma V, Stains JP. The regulation of runt-related transcription factor 2 by fibroblast growth factor-2 and connexin43 requires the inositol polyphosphate/protein kinase Cδ cascade. J Bone Miner Res NIH Public Access. 2013;28:1468–77.
Gaur T, Lengner CJ, Hovhannisyan H, Bhat RA, Bodine PVN, Komm BS, et al. Canonical WNT signaling promotes osteogenesis by directly stimulating Runx2 gene expression. J Biol Chem. 2005;280:33132–40.
• Karsenty G. Transcriptional control of skeletogenesis. Annu Rev Genomics Hum Genet. 2008;9:183–96. This review highlights many of the important transcriptional activators and repressors during differentiation of mesenchymal tissue into the osteochondral lineage and discusses the interaction between the two master osteogenic transcription factors RUNX2 and OSX.
• Lee R, Feinbaum R, Ambros V. The C. elegans heterochronic gene lin-4 encodes small RNAs with antisense complementarity to lin-14. Cell. 1993;75:843–54. This paper was the first to identify a small non-coding RNA molecule found to bind to the 3′UTR of a target mRNA, which suggested a translation regulation.
Reinhart BJ, Slack FJ, Basson M, Pasquinelli AE, Bettinger JC, Rougvie AE, et al. The 21-nucleotide let-7 RNA regulates developmental timing in Caenorhabditis elegans. Nature. 2000;403:901–6.
Reinhart BJ, Weinstein EG, Rhoades MW, Bartel B, Bartel DP. MicroRNAs in plants. Genes Dev. 2002;16:1616–26.
Chen X. A microRNA as a translational repressor of APETALA2 in Arabidopsis flower development. Science. 2004;303:2022–5.
Johnston RJ, Hobert O. A microRNA controlling left/right neuronal asymmetry in Caenorhabditis elegans. Nature. 2003;426:845–9.
Li X, Carthew RW. A microRNA mediates EGF receptor signaling and promotes photoreceptor differentiation in the drosophila eye. Cell. 2005;123:1267–77.
Heimberg AM, Sempere LF, Moy VN, Donoghue PCJ, Peterson KJ. MicroRNAs and the advent of vertebrate morphological complexity. Proc Natl Acad Sci. 2008;105:2946–50.
Ardekani AM, Naeini MM. The role of microRNAs in human diseases. Avicenna J Med Biotechnol. 2010;2:161–79.
Pasquinelli AE. MicroRNAs and their targets: recognition, regulation and an emerging reciprocal relationship. Nat Rev Genet. 2012;13:271–82.
Wu L, Fan J, Belasco JG. MicroRNAs direct rapid deadenylation of mRNA. Proc Natl Acad Sci. 2006;103:4034–9.
Wahid F, Shehzad A, Khan T, Kim YY. MicroRNAs: synthesis, mechanism, function, and recent clinical trials. Biochim Biophys Acta. 1803;2010:1231–43.
Lin SL, Miller JD, Ying SY. Intronic microRNA (miRNA). J Biomed Biotechnol. 2006;2006:1–13.
Ruby JG, Jan CH, Bartel DP. Intronic microRNA precursors that bypass Drosha processing. Nature. 2007;448:83–6.
Bohnsack MT, Czaplinski K, Gorlich D. Exportin 5 is a RanGTP-dependent dsRNA-binding protein that mediates nuclear export of pre-miRNAs. RNA. 2004;10:185–91.
Sontheimer EJ. Assembly and functions of RNA silencing complexes. Nat Rev Mol Cell Biol. 2005;6:127–38.
Ha M, Kim VN. Regulation of microRNA biogenesis. Nat Rev Mol Cell Biol. 2014;15:509–24.
Olsen PH, Ambros V. The lin-4 regulatory RNA controls developmental timing in Caenorhabditis elegans by blocking LIN-14 protein synthesis after the initiation of translation. Dev Biol. 1999;216:671–80.
Wu L, Fan J, Belasco JG. MicroRNAs direct rapid deadenylation of mRNA. Proc Natl Acad Sci U S A. 2006;103(11):4034–9.
Eulalio A, Rehwinkel J, Stricker M, Huntzinger E, Yang SF, Doerks T, et al. Target-specific requirements for enhancers of decapping in miRNA-mediated gene silencing. Genes Dev. 2007;21(20):2558–70.
Eulalio A, Huntzinger E, Nishihara T, Rehwinkel J, Fauser M, Izaurralde E. Deadenylation is a widespread effect of miRNA regulation. RNA. 2009;15(1):21–32.
Cai X, Hagedorn CH, Cullen BR. Human microRNAs are processed from capped, polyadenylated transcripts that can also function as mRNAs. RNA. 2004;10:1957–66.
Denli AM, Tops BBJ, Plasterk RHA, Ketting RF, Hannon GJ. Processing of primary microRNAs by the microprocessor complex. Nature. 2004;432:231–5.
• Eguchi T, Watanabe K, Hara ES, Ono M, Kuboki T, Calderwood SK, et al. OstemiR: a novel panel of microRNA biomarkers in osteoblastic and osteocytic differentiation from mesenchymal stem cells. PLoS One. 2013;8:e58796. This paper reveals a number of miRNAs differentially expressed during osteoblastic and osteocytic differentiation denoted “ostemiRs,” which have been proposed to affect osteogenic differentiation, stemness as well as other important processes.
Kapinas K, Kessler CB, Delany AM. miR-29 suppression of osteonectin in osteoblasts: regulation during differentiation and by canonical Wnt signaling. J Cell Biochem. 2009;108:216–24.
Zhou X, Luan X, Chen Z, Francis M, Gopinathan G, Li W, et al. MicroRNA-138 inhibits periodontal progenitor differentiation under inflammatory conditions. J Dent Res. 2016;95:230–7.
Laxman N, Rubin C-J, Mallmin H, Nilsson O, Pastinen T, Grundberg E, et al. Global miRNA expression and correlation with mRNA levels in primary human bone cells. RNA. 2015;21:1433–43.
Mohri T, Nakajima M, Takagi S, Komagata S, Yokoi T. MicroRNA regulates human vitamin D receptor. Int J Cancer. 2009;125:1328–33.
Chen Q, Liu W, Sinha KM, Yasuda H, de Crombrugghe B. Identification and characterization of microRNAs controlled by the osteoblast-specific transcription factor Osterix. PLoS One. 2013;8:e58104.
Chakrabarty A, Tranguch S, Daikoku T, Jensen K, Furneaux H, Dey SK. MicroRNA regulation of cyclooxygenase-2 during embryo implantation. Proc Natl Acad Sci. 2007;104:15144–9.
Li Z, Hassan MQ, Volinia S, van Wijnen AJ, Stein JL, Croce CM, et al. A microRNA signature for a BMP2-induced osteoblast lineage commitment program. Proc Natl Acad Sci. 2008;105:13906–11.
Shevde LA, Metge BJ, Mitra A, Xi Y, Ju J, King JA, et al. Spheroid-forming subpopulation of breast cancer cells demonstrates vasculogenic mimicry via hsa-miR-299-5p regulated de novo expression of osteopontin. J Cell Mol Med. 2010;14:1693–706.
Tu M, Li Y, Zeng C, Deng Z, Gao S, Xiao W, et al. MicroRNA-127-5p regulates osteopontin expression and osteopontin-mediated proliferation of human chondrocytes. Sci Rep. 2016;6:25032.
Sekiya Y, Ogawa T, Yoshizato K, Ikeda K, Kawada N. Suppression of hepatic stellate cell activation by microRNA-29b. Biochem Biophys Res Commun. 2011;412:74–9.
Tang O, Chen X-M, Shen S, Hahn M, Pollock CA. MiRNA-200b represses transforming growth factor-β1-induced EMT and fibronectin expression in kidney proximal tubular cells. Am J Physiol Renal Physiol. 2013;304:1266–73.
Wang Q, Wang Y, Minto AW, Wang J, Shi Q, Li X, et al. MicroRNA-377 is up-regulated and can lead to increased fibronectin production in diabetic nephropathy. FASEB J. 2008;22:4126–35.
Bonnin N, Armandy E, Carras J, Ferrandon S, Foy J-P, Saintigny P, et al. MiR-422a promotes loco-regional recurrence by targeting NT5E/CD73 in head and neck squamous cell carcinoma. Oncotarget. 2016; doi:10.18632/oncotarget.9829.
Chen XP, Chen YG, Lan JY, Shen ZJ. MicroRNA-370 suppresses proliferation and promotes endometrioid ovarian cancer chemosensitivity to cDDP by negatively regulating ENG. Cancer Lett. 2014;353:201–10.
Yu G, Li H, Wang J, Gumireddy K, Li A, Yao W, et al. miRNA-34a suppresses cell proliferation and metastasis by targeting CD44 in human renal carcinoma cells. J Urol. 2014;192:1229–37.
Wang P, Luo Y, Duan H, Xing S, Zhang J, Lu D, et al. MicroRNA 329 suppresses angiogenesis by targeting CD146. Mol Cell Biol. 2013;33:3689–99.
Liu H, Lin H, Zhang L, Sun Q, Yuan G, Zhang L, et al. miR-145 and miR-143 regulate odontoblast differentiation through targeting Klf4 and Osx genes in a feedback loop. J Biol Chem. 2013;288:9261–71.
Li E, Zhang J, Yuan T, Ma B. MiR-143 suppresses osteogenic differentiation by targeting Osterix. Mol Cell Biochem. 2014;390:69–74.
Shi K, Lu J, Zhao Y, Wang L, Li J, Qi B, et al. MicroRNA-214 suppresses osteogenic differentiation of C2C12 myoblast cells by targeting Osterix. Bone. 2013;55:487–94.
Zhang J, Fu W, He M, Wang H, Wang W, Yu S, et al. MiR-637 maintains the balance between adipocytes and osteoblasts by directly targeting osterix. Mol Biol Cell. 2011;22:3955–61.
Gámez B, Rodríguez-Carballo E, Bartrons R, Rosa JL, Ventura F. MicroRNA-322 (miR-322) and its target protein Tob2 modulate Osterix (Osx) mRNA stability. J Biol Chem. 2013;288:14264–75.
• Huang J, Zhao L, Xing L, Chen D. MicroRNA-204 regulates Runx2 protein expression and mesenchymal progenitor cell differentiation. Stem Cells. 2010;28:357–64. This paper demonstrates the direct binding of miR-204 to the 3′UTR of Runx2 within the osteogenic lineage to inhibit osteogenesis and promote adipogenesis.
Kim E-J, Kang I-H, Lee JW, Jang W-G, Koh J-T. MiR-433 mediates ERRγ-suppressed osteoblast differentiation via direct targeting to Runx2 mRNA in C3H10T1/2 cells. Life Sci. 2013;92:562–8.
Chen H, Ji X, She F, Gao Y, Tang P. miR-628-3p regulates osteoblast differentiation by targeting RUNX2: possible role in atrophic non-union. Int J Mol Med Spandidos Publications. 2017;39:279–86.
Liu H, Sun Q, Wan C, Li L, Zhang L, Chen Z. MicroRNA-338-3p regulates osteogenic differentiation of mouse bone marrow stromal stem cells by targeting Runx2 and Fgfr2. J Cell Physiol. 2014;229:1494–502.
Du F, Wu H, Zhou Z, Liu YU. microRNA-375 inhibits osteogenic differentiation by targeting runt-related transcription factor 2. Exp Ther Med. 2015;10:207–12.
Hassan MQ, Gordon JAR, Beloti MM, Croce CM, van Wijnen AJ, Stein JL, et al. A network connecting Runx2, SATB2, and the miR-23a~27a~24-2 cluster regulates the osteoblast differentiation program. Proc Natl Acad Sci. 2010;107:19879–84.
Hu N, Feng C, Jiang Y, Sekiya Q, Liu H. Regulative effect of mir-205 on osteogenic differentiation of bone mesenchymal stem cells (BMSCs): possible role of SATB2/Runx2 and ERK/MAPK pathway. Int J Mol Sci. 2015;16:10491–506.
Kim S, Koga T, Isobe M, Kern BE, Yokochi T, Chin YE, et al. Stat1 functions as a cytoplasmic attenuator of Runx2 in the transcriptional program of osteoblast differentiation. Genes Dev. 2003;17:1979–91.
Wei J, Shi Y, Zheng L, Zhou B, Inose H, Wang J, et al. miR-34s inhibit osteoblast proliferation and differentiation in the mouse by targeting SATB2. J Cell Biol. 2012;197:509–21.
Brennan-Speranza TC, Conigrave AD. Osteocalcin: an osteoblast-derived polypeptide hormone that modulates whole body energy metabolism. Calcif Tissue Int. 2015;96:1–10.
van Leeuwen J, van Driel M, van den Bemd G, Pols HA. Vitamin D control of osteoblast function and bone extracellular matrix mineralization. Crit Rev Eukaryot Gene Expr. 2001;11:199–226.
Mizuno Y, Yagi K, Tokuzawa Y, Kanesaki-Yatsuka Y, Suda T, Katagiri T, et al. miR-125b inhibits osteoblastic differentiation by down-regulation of cell proliferation. Biochem Biophys Res Commun. 2008;368:267–72.
Yin JJ, Pollock CB, Kelly K. Mechanisms of cancer metastasis to the bone. Cell Res. 2005;15:57–62.
Forwood MR. Inducible cyclo-oxygenase (COX-2) mediates the induction of bone formation by mechanical loading in vivo. J Bone Miner Res. 1996;11:1688–93.
Wadhwa S, Choudhary S, Voznesensky M, Epstein M, Raisz L, Pilbeam C. Fluid flow induces COX-2 expression in MC3T3-E1 osteoblasts via a PKA signaling pathway. Biochem Biophys Res Commun. 2002;297:46–51.
Greenhough A, Smartt HJM, Moore AE, Roberts HR, Williams AC, Paraskeva C, et al. The COX-2/PGE2 pathway: key roles in the hallmarks of cancer and adaptation to the tumour microenvironment. Carcinogenesis. 2009;30:377–86.
Okamoto H, Matsumi Y, Hoshikawa Y, Takubo K, Ryoke K, Shiota G. Involvement of microRNAs in regulation of osteoblastic differentiation in mouse induced pluripotent stem cells. PLoS One. 2012;7:e43800.
Yu S, Geng Q, Pan Q, Liu Z, Ding S, Xiang Q, et al. MiR-690, a Runx2-targeted miRNA, regulates osteogenic differentiation of C2C12 myogenic progenitor cells by targeting NF-kappaB p65. Cell Biosci. 2016;6:10.
Guo Y, Wang Y, Liu Y, Liu Y, Zeng Q, Zhao Y, et al. MicroRNA-218, microRNA-191*, microRNA-3070a and microRNA-33 are responsive to mechanical strain exerted on osteoblastic cells. Mol Med Rep. 2015;12:3033–8.
Sodek J, Ganss B, McKee MD. Osteopontin. Crit Rev Oral Biol Med. 2000;11:279–303.
Sun C, Huang F, Liu X, Xiao X, Yang M, Hu G, et al. miR-21 regulates triglyceride and cholesterol metabolism in non-alcoholic fatty liver disease by targeting HMGCR. Int J Mol Med. 2015;35:847–53.
Tsipouras P, Myers JC, Ramirez F, Prockop DJ. Restriction fragment length polymorphism associated with the pro alpha 2(I) gene of human type I procollagen. Application to a family with an autosomal dominant form of osteogenesis imperfecta. J Clin Invest. 1983;72:1262–7.
Byers PH, Shapiro JR, Rowe DW, David KE, Holbrook KA. Abnormal alpha 2-chain in type I collagen from a patient with a form of osteogenesis imperfecta. J Clin Invest. 1983;71:689–97.
Kalajzic I, Staal A, Yang W-P, Wu Y, Johnson SE, Feyen JHM, et al. Expression profile of osteoblast lineage at defined stages of differentiation. J Biol Chem. 2005;280:24618–26.
Li C, Nguyen HT, Zhuang Y, Lin Y, Flemington EK, Guo W, et al. Post-transcriptional up-regulation of miR-21 by type I collagen. Mol Carcinog. 2011;50:563–70.
• Davis BN, Hilyard AC, Lagna G, Hata A. SMAD proteins control DROSHA-mediated microRNA maturation. Nature. 2008;454:56–61. This paper highlights the fact that signaling cascades cannot only activate the transcription of microRNAs through downstream transcription factors but also by affecting microRNA processing.
Kawakita A, Yanamoto S, Yamada S-I, Naruse T, Takahashi H, Kawasaki G, et al. MicroRNA-21 promotes oral cancer invasion via the Wnt/β-catenin pathway by targeting DKK2. Pathol Oncol Res. 2014;20:253–61.
Lenselink EA. Role of fibronectin in normal wound healing. Int Wound J. 2015;12:313–6.
Liu F, Lv Q, Du WW, Li H, Yang X, Liu D, et al. Specificity of miR-378a-5p targeting rodent fibronectin. Biochim Biophys Acta. 1833;2013:3272–85.
Vasanthan P, Govindasamy V, Gnanasegaran N, Kunasekaran W, Musa S, Abu Kasim NH. Differential expression of basal microRNAs’ patterns in human dental pulp stem cells. J Cell Mol Med. 2015;19:566–80.
Palmieri A, Pezzetti F, Brunelli G, Martinelli M, Scapoli L, Arlotti M, et al. Medpor regulates osteoblast’s microRNAs. Biomed Mater Eng. 2008;18:91–7.
Palmieri A, Pezzetti F, Brunelli G, Martinelli M, Lo Muzio L, Scarano A, et al. Anorganic bovine bone (Bio-Oss) regulates miRNA of osteoblast-like cells. Int J Periodontics Restorative Dent. 2010;30:83–7.
Vodyanik MA, Yu J, Zhang X, Tian S, Stewart R, Thomson JA, et al. A mesoderm-derived precursor for mesenchymal stem and endothelial cells. Cell Stem Cell. 2010;7:718–29.
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The international society for cellular therapy position statement. Cytotherapy. 2006;8:315–7.
Spaeth EL, Labaff AM, Toole BP, Klopp A, Andreeff M, Marini FC. Mesenchymal CD44 expression contributes to the acquisition of an activated fibroblast phenotype via TWIST activation in the tumor microenvironment. Cancer Res. 2013;73:5347–59.
Fan J, Im CS, Guo M, Cui Z-K, Fartash A, Kim S, et al. Enhanced osteogenesis of adipose-derived stem cells by regulating bone morphogenetic protein signaling antagonists and agonists. Stem Cells Transl Med. 2016;5:539–51.
Harkness L, Zaher W, Ditzel N, Isa A, Kassem M. CD146/MCAM defines functionality of human bone marrow stromal stem cell populations. Stem Cell Res Ther. 2016;7:4.
Nishihira S, Okubo N, Takahashi N, Ishisaki A, Sugiyama Y, Chosa N. High-cell density-induced VCAM1 expression inhibits the migratory ability of mesenchymal stem cells. Cell Biol Int. 2011;35:475–81.
Harris TA, Yamakuchi M, Ferlito M, Mendell JT, Lowenstein CJ. MicroRNA-126 regulates endothelial expression of vascular cell adhesion molecule 1. Proc Natl Acad Sci. 2008;105:1516–21.
Hwang S, Park S-K, Lee HY, Kim SW, Lee JS, Choi EK, et al. miR-140-5p suppresses BMP2-mediated osteogenesis in undifferentiated human mesenchymal stem cells. FEBS Lett. 2014;588:2957–63.
Niu T, Liu N, Zhao M, Xie G, Zhang L, Li J, et al. Identification of a novel FGFRL1 microRNA target site polymorphism for bone mineral density in meta-analyses of genome-wide association studies. Hum Mol Genet. 2015;24:4710–27.
Gan S, Huang Z, Liu N, Su R, Xie G, Zhong B, et al. MicroRNA-140-5p impairs zebrafish embryonic bone development via targeting BMP-2. FEBS Lett. 2016;590:1438–46.
Yu X, Cohen DM, Chen CS. miR-125b is an adhesion-regulated microRNA that protects mesenchymal stem cells from anoikis. Stem Cells. 2012;30:956–64.
Chen S, Yang L, Jie Q, Lin Y-S, Meng G-L, Fan J-Z, et al. MicroRNA-125b suppresses the proliferation and osteogenic differentiation of human bone marrow-derived mesenchymal stem cells. Mol Med Rep. 2014;9:1820–6.
Karsenty G, Wagner EF. Reaching a genetic and molecular understanding of skeletal development. Dev Cell. 2002;2:389–406.
Komori T. Regulation of osteoblast differentiation by transcription factors. J Cell Biochem. 2006;99:1233–9.
Liu L-L, Lu S-X, Li M, Li L-Z, Fu J, Hu W, et al. FoxD3-regulated microRNA-137 suppresses tumour growth and metastasis in human hepatocellular carcinoma by targeting AKT2. Oncotarget. 2014;5:5113–24.
Farina NH, Zingiryan A, Akech JA, Callahan CJ, Lu H, Stein JL, et al. A microRNA/Runx1/Runx2 network regulates prostate tumor progression from onset to adenocarcinoma in TRAMP mice. Oncotarget. 2016; doi:10.18632/oncotarget.11992.
Xiao WZ, Gu XC, Hu B, Liu XW, Zi Y, Li M. Role of microRNA-129-5p in osteoblast differentiation from bone marrow mesenchymal stem cells. Cell Mol Biol. 2016;62:95–9.
Yu S, Geng Q, Ma J, Sun F, Yu Y, Pan Q, et al. Heparin-binding EGF-like growth factor and miR-1192 exert opposite effect on Runx2-induced osteogenic differentiation. Cell Death Dis. 2013;4:e868.
Dobreva G, Chahrour M, Dautzenberg M, Chirivella L, Kanzler B, Fariñas I, et al. SATB2 is a multifunctional determinant of craniofacial patterning and osteoblast differentiation. Cell. 2006;125:971–86.
Tang W, Li Y, Osimiri L, Zhang C. Osteoblast-specific transcription factor Osterix (Osx) is an upstream regulator of Satb2 during bone formation. J Biol Chem. 2011;286:32995–3002.
Deng Y, Wu S, Zhou H, Bi X, Wang Y, Hu Y, et al. Effects of a miR-31, Runx2, and Satb2 regulatory loop on the osteogenic differentiation of bone mesenchymal stem cells. Stem Cells Dev. 2013;22:2278–86.
Mi W, Shi Q, Chen X, Wu T, Huang H. miR-33a-5p modulates TNF-α-inhibited osteogenic differentiation by targeting SATB2 expression in hBMSCs. FEBS Lett. 2016;590:396–407.
Ge J, Guo S, Fu Y, Zhou P, Zhang P, Du Y, et al. Dental follicle cells participate in tooth eruption via the RUNX2-miR-31-SATB2 loop. J Dent Res. 2015;94:936–44.
Le Douarin NM, Dupin E. Multipotentiality of the neural crest. Curr Opin Genet Dev. 2003;13:529–36.
• Nie X, Wang Q, Jiao K. Dicer activity in neural crest cells is essential for craniofacial organogenesis and pharyngeal arch artery morphogenesis. Mech Dev. 2011;128:200–7. This paper signifies the importance of miRNA regulation within neural crest cells during early craniofacial development, with no defects in the migration of cranial and cardia neural crest cells, but to subsequent development.
• Simões-Costa M, Bronner ME. Establishing neural crest identity: a gene regulatory recipe. Development. 2015;142:242–57. This review highlights the complex genetic regulations and pathways, identified as the gene regulatory network, in which neural crest cells undergo in order to become specified, maintained, migratory, and further differentiated.
Betel D, Wilson M, Gabow A, Marks DS, Sander C. The microRNA.org resource: targets and expression. Nucleic Acids Res. 2008;36:D149–53.
Crane JF, Trainor PA. Neural crest stem and progenitor cells. Annu Rev Cell Dev Biol. 2006;22:267–86.
• Basch ML, Bronner-Fraser M, García-Castro MI. Specification of the neural crest occurs during gastrulation and requires Pax7. Nature. 2006;441:218–22. This paper challenged the prior notion that neural crest specification occurs after gastrulation and introduced Pax7 as a border specifier gene.
Monsoro-Burq AH. PAX transcription factors in neural crest development. Semin Cell Dev Biol. 2015;44:87–96.
Sambasivan R, Yao R, Kissenpfennig A, Van Wittenberghe L, Paldi A, Gayraud-morel B, et al. Pax7-expressing satellite cells are indispensable for adult skeletal muscle regeneration. Development. 2011;4333:3647–56.
Wu R, Li H, Zhai L, Zou X, Meng J, Zhong R, et al. MicroRNA-431 accelerates muscle regeneration and ameliorates muscular dystrophy by targeting Pax7 in mice. Nat Commun. 2015;6:7713.
Yang B, Jia L, Guo Q, Ren H, Hu D, Zhou X, et al. MiR-564 functions as a tumor suppressor in human lung cancer by targeting ZIC3. Biochem Biophys Res Commun. 2015;467:690–6.
Penna E, Orso F, Cimino D, Vercellino I, Grassi E, Quaglino E, et al. miR-214 coordinates melanoma progression by upregulating ALCAM through TFAP2 and miR-148b downmodulation. Cancer Res. 2013;73:4098–111.
Pieper M, Ahrens K, Rink E, Peter A, Schlosser G. Differential distribution of competence for panplacodal and neural crest induction to non-neural and neural ectoderm. Dev. 2012;139:1175–87.
Otsubo T, Akiyama Y, Hashimoto Y, Shimada S, Goto K, Yuasa Y. MicroRNA-126 inhibits sox2 expression and contributes to gastric carcinogenesis. PLoS One. 2011;6
Yan B, Liu B, Zhu C-D, Li K-L, Yue L-J, Zhao J-L, et al. MicroRNA regulation of skin pigmentation in fish. J Cell Sci. 2013;126:3401–8.
Duband JL, Monier F, Delannet M, Newgreen D. Epithelium-mesenchyme transition during neural crest development. Acta Anat. 1995;154:63–78.
Shook D, Keller R. Mechanisms, mechanics and function of epithelial-mesenchymal transitions in early development. Mech Dev. 2003;120:1351–83.
Thiery JP, Sleeman JP. Complex networks orchestrate epithelial-mesenchymal transitions. Nat Rev Mol Cell Biol. 2006;7:131–42.
Vincentz JW, Firulli BA, Lin A, Spicer DB, Howard MJ, Firulli AB. Twist1 controls a cell-specification switch governing cell fate decisions within the cardiac neural crest. PLoS Genet. 2013;9:e1003405.
MacKenzie A, Ferguson MW, Sharpe PT. Hox-7 expression during murine craniofacial development. Development. 1991;113:601–11.
Takahashi K, Nuckolls GH, Takahashi I, Nonaka K, Nagata M, Ikura T, et al. Msx2 is a repressor of chondrogenic differentiation in migratory cranial neural crest cells. Dev Dyn. 2001;222:252–62.
McCusker C, Cousin H, Neuner R, Alfandari D. Extracellular cleavage of cadherin-11 by ADAM metalloproteases is essential for Xenopus cranial neural crest cell migration. Mol Biol Cell. 2009;20:78–89.
Liu H, Wang H, Liu X, Yu T. miR-1271 inhibits migration, invasion and epithelial-mesenchymal transition by targeting ZEB1 and TWIST1 in pancreatic cancer cells. Biochem Biophys Res Commun. 2016;472:346–52.
Bildsoe H, Loebel DAF, Jones VJ, Chen Y-T, Behringer RR, Tam PPL. Requirement for Twist1 in frontonasal and skull vault development in the mouse embryo. Dev Biol. 2009;331:176–88.
Davideau JL, Demri P, Hotton D, Gu TT, MacDougall M, Sharpe P, et al. Comparative study of MSX-2, DLX-5, and DLX-7 gene expression during early human tooth development. Pediatr Res. 1999;46:650–6.
Itoh T, Nozawa Y, Akao Y. MicroRNA-141 and -200a are involved in bone morphogenetic protein-2-induced mouse pre-osteoblast differentiation by targeting distal-less homeobox 5. J Biol Chem. 2009;284:19272–9.
Shirakabe K, Terasawa K, Miyama K, Shibuya H, Nishida E. Regulation of the activity of the transcription factor Runx2 by two homeobox proteins, Msx2 and Dlx5. Genes Cells. 2001;6:851–6.
Ishii M, Han J, Yen H-Y, Sucov HM, Chai Y, Maxson RE. Combined deficiencies of Msx1 and Msx2 cause impaired patterning and survival of the cranial neural crest. Development. 2005;132:4937–50.
Mayanil CS. Transcriptional and epigenetic regulation of neural crest induction during neurulation. Dev Neurosci. 2013;35:361–72.
Sauka-Spengler T, Bronner-Fraser M. A gene regulatory network orchestrates neural crest formation. Nat Rev Mol Cell Biol. 2008;9:557–68.
Acknowledgments
We apologize to the authors of many excellent research studies who we could not cite here due to space constraints. This work was supported by a grant from the National Institute of Dental and Craniofacial Research of the National Institutes of Health (R01 DE025330-01A1) and a grant from the Tobacco Related Disease Research Program (25IP-0018, award no. 392351) to NzN.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Steven R. Sera and Nicole I. zur Nieden declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Skeletal Development
Rights and permissions
About this article
Cite this article
Sera, S.R., zur Nieden, N.I. microRNA Regulation of Skeletal Development. Curr Osteoporos Rep 15, 353–366 (2017). https://doi.org/10.1007/s11914-017-0379-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-017-0379-7