Abstract
Purpose of Review
Patient navigation promotes access to timely treatment of chronic diseases by eliminating barriers to care. Patient navigation programs have been well-established in improving screening rates and diagnostic resolution. This systematic review aimed to characterize the multifaceted role of patient navigators within the realm of cancer treatment.
Recent Findings
A comprehensive electronic literature review of PubMed and Embase databases was conducted to identify relevant studies investigating the role of patient navigators in cancer treatment from August 1, 2009 to March 27, 2023.
Summary
Fifty-nine articles were included in this review. Amongst studies focused on cancer treatment initiation, 70% found a significant improvement in treatment initiation amongst patients who were enrolled in patient navigation programs, 71% of studies focused on treatment adherence demonstrated significant improvements in treatment adherence, 87% of studies investigating patient satisfaction showed significant benefits, and 81% of studies reported a positive impact of patient navigators on quality care indicators. Three palliative care studies found beneficial effects of patient navigation. Thirty-seven studies investigated disadvantaged populations, with 76% of them concluded that patient navigators made a positive impact during treatment. This systematic review provides compelling evidence supporting the value of patient navigation programs in cancer treatment. The findings suggest that patient navigation plays a crucial role in improving access to care and optimizing treatment outcomes, especially for disadvantaged cancer patients. Incorporating patient navigation into standard oncology practice can reduce disparities and improve the overall quality of cancer care.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The intricate nature of cancer care can pose significant challenges for patients, leading to gaps in understanding, delays in treatment, and disparities in healthcare access. Patient navigation is a community-based intervention designed to increase access to care and eliminate barriers patients may face [1]. Beginning in the 1990s, patient navigation programs emerged as a promising approach to support patients through the cancer care continuum by providing personalized assistance and guidance to improve patient outcomes and reduce racial healthcare disparities [1]. Since then, these programs have emerged as a critical strategy aimed at addressing challenges and optimizing the patient journey through the complexities of cancer diagnosis, treatment, and survivorship. The roles of patient navigators are constantly evolving and expanding, with the Center for Disease Control and American Cancer Society dedicating more broader definitions regarding their use in healthcare [2, 3].
The cancer care continuum is a comprehensive framework that outlines the various stages and elements involved in care for individuals affected by cancer [4]. Specifically, the “treatment” phase of the continuum is the time period between diagnosis and survivorship which includes curative-intent therapies, disease-control therapies, and symptom management [5]. Types of cancer treatment may include surgery, chemotherapy, radiation therapy, hormonal therapy, targeted therapy, and immunotherapy (Fig. 1). This continuum is designed to ensure a coordinated approach to managing cancer throughout a patient’s journey. The benefits of patient navigation have been thoroughly documented in phases of screening and diagnostic resolution [6]. However, there is a paucity of literature evaluating the efficacy of patient navigation on cancer treatment as a whole [7,8,9,10,11,12]. We conducted a systematic review to characterize the role of patient navigation in cancer treatment, focusing on treatment initiation, treatment adherence, quality indicators, palliative care, and patient satisfaction. The findings of this review could have important implications for cancer care providers, policymakers, and patients, for future implementation of navigation programs that improve cancer care delivery and patient outcomes.
Methods
Data Sources
A comprehensive electronic literature review of PubMed and Embase databases was conducted to identify relevant studies investigating the role of patient navigators in cancer treatment. Search terms were devised in coordination with a librarian to ensure pertinent literature, balance between specificity and inclusivity, and maintain a strong focus on patient navigation and cancer treatment. The following MeSH terms were used for PubMed: (("Neoplasms"[Mesh]) OR (cancer patient*[tiab])) AND (("Patient Navigation"[Mesh]) OR (patient navigat*[tiab])). The search term used for Embase was as follows: ('patient'/exp OR patient) AND ('navigator'/exp OR navigator) AND cancer AND [01–08-2009]/sd NOT [24–03-2023]/sd AND [2009–2023]/py.
We also summarized ongoing clinical trials for patient navigation in cancer treatment through the National Cancer Institute’s (NCI) clinicaltrials.gov. This search was filtered with the following: condition—cancer, terms—navigation, study status—not yet recruiting, recruiting, and enrolling by invitation. The search was conducted on March 24, 2023.
Inclusion and Exclusion Criteria
Studies were selected for inclusion in this systematic review if they were published between the dates of August 1, 2009 to March 24, 2023. Articles included all cancer patients that received cancer treatment and had a patient navigation intervention group studied. Empirical research, randomized controlled trials, cohort studies, case–control studies, and observational studies were included. Studies also had to be published in English. Studies were excluded if they were published before 8/1/2009 or after 3/24/2023. Studies that did not implement patient navigation or were not directly related to the role of patient navigators in cancer treatment were excluded. Non-empirical studies, including reviews, commentaries, or editorials were excluded. Case studies presenting individual patient cases without broader empirical analysis were also excluded. Clinical trials were included if they focused on patient navigation during the cancer “treatment” phase defined by the Cancer Care Continuum [5].
Study Selection
After removing duplicates with Excel string matching across titles, the titles and abstracts of the remaining records were screened independently by two reviewers (M.C. and V.W.) for relevance to the research question and adherence to the inclusion and exclusion criteria. Full-text articles were retrieved for records that met the initial screening criteria. The full-text articles were then assessed by the reviewers (M.C. and V.W.) for final inclusion in the systematic review.
Quality Assessment
The methodological quality of the included studies was assessed using the 2018 version of the Mixed Methods Appraisal Tool (MMAT) [13]. The MMAT includes specific criteria for assessing the quality of various study designs, such as randomized controlled trials, cohort studies, case–control studies, and observational studies. This quality assessment aimed to evaluate the validity and reliability of the included studies and inform the interpretation of their findings.
Data Synthesis
A narrative synthesis approach was used to summarize and analyze the findings of the included studies. Themes related to the impact of patient navigators on treatment initiation, treatment adherence, patient satisfaction, quality indicators, and palliative care were identified and discussed. Secondary themes included the country the study was performed in, the types of cancer patients had, and whether the study had a focused on a disadvantaged population such as racial minorities, socioeconomically challenged, and underinsured. The synthesis aimed to provide a comprehensive overview of the role of patient navigators in cancer treatment across different contexts and populations.
Results
Study Selection
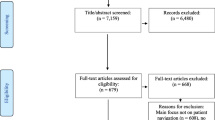
A total of 2229 articles were identified through the PubMed and Embase databases. Duplicates were removed and 1934 articles remained (Fig. 2). Of the remaining 1934 articles, 1876 were excluded based on inapplicable results or not meeting inclusion criteria. 1008 were not relevant to patient navigation during cancer treatment, 761 did not have a full text or were conference abstracts only, 92 were reviews, 10 were editorials, notes, or cover letters, 4 were limited case studies, and 2 were not written in English. Fifty-nine total articles were included in this review, with thirty-seven of them investigating disadvantaged groups.
Treatment Initiation
Twenty-three articles focused on the impact of patient navigators on the time between diagnosis and treatment initiation. Of these, 70% (n = 16) reported a significant reduction in time to treatment with patients that received navigation. These positive outcomes were observed across various cancer types, including eight breast, three lung, one head and neck, one hematologic, one pancreatic, one gastrointestinal, and one multiple cancer studies [14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29]. Eight breast and one gastrointestinal cancer study focused on disadvantaged populations [14,15,16,17,18,19,20,21, 25]. The remaining studies either showed no significant difference or increased time to treatment between patient navigation groups and control groups [30,31,32,33,34,35,36]. A comprehensive overview of these findings is presented in Table 1.
Treatment Adherence
Seventeen articles delved into the impact of patient navigators in treatment adherence, measuring the extent to which patients adhered to treatment plans and attended appointments throughout their cancer journey. A total of 71% (n = 12) demonstrated a significant improvement of treatment adherence with navigation compared to the control group [37,38,39,40,41,42,43,44,45,46,47,48]. This was evident across multiple types of cancer, including five breast, three cervical, one osteosarcoma, one lymphoma, and two multiple cancer studies. Eight of these twelve studies focused on vulnerable populations, distributed amongst three breast, three cervical, one lymphoma, and one multiple cancer studies [37, 39, 41,42,43,44, 47, 48]. Five articles discovered no difference in treatment adherence between patients that received patient navigation and those who did not [25, 34, 49,50,51]. A comprehensive overview of these findings is presented in Table 2.
Patient Satisfaction
Fifteen articles assessed patient satisfaction or quality of life, which explored the contentment of patients with their care during the treatment process. Thirteen out of the fifteen studies (87%) demonstrated high rates of satisfaction with their navigator [18, 26, 30, 36, 50, 52,53,54,55,56,57,58,59]. Many of these studies encompassed several different cancers, ranging from breast, cervical, colorectal, prostate, head and neck, melanoma, gynecologic, and hematologic malignancies. Five of these studies, investigating all cancers and breast cancer, were done on disadvantaged groups [18, 36, 50, 58]. Two articles found no significant difference in satisfaction with patient navigation during treatment [60, 61]. A comprehensive overview of these findings can be found in Table 3.
Quality of Care
Eleven studies investigated the quality of patient navigation interventions by assessing adherence to various healthcare quality metrics such as hospitalizations, emergency department visits, financial assistance, or standard quality indicators tailored to different cancers. Nine (81%) of studies reported a positive impact of navigation on quality care indicators, which included four breast, one lymphoma, and four all-encompassing cancers studies [55, 56, 62,63,64,65,66,67,68]. Within these studies, two focused on breast cancer, one on lymphoma, and one involved all cancer types that targeted disadvantaged populations [56, 62, 64, 68]. Two studies found no improvement in cost of care or other healthcare assistance between navigated patients and the control [32, 69]. A comprehensive overview of these findings can be found in Table 4.
Palliative Care
There were three articles that investigated the role of patient navigation in palliative care for cancer patients during treatment. Two studies discovered an increase in compliance for advanced directive completion, in addition to increased supportive care efforts [70, 71]. The third study determined that navigators benefited family caregivers with decreased anxiety and improving their quality of life during treatment [72]. A comprehensive overview of these findings can be found in Table 5.
Ongoing Clinical Trials
Table 6 lists ongoing clinical trials for patient navigation during cancer treatment. Eighteen trials were identified with our search.
Discussion
This systematic review examined the role of patient navigation during cancer treatment and demonstrated that patient navigation programs can improve patient outcomes and can reduce inequities in treatment based on non-medical factors. Patient navigation programs can decrease time to initiate treatment, increase patient adherence to treatment, and improve patient satisfaction and quality of care. Many of these studies focus on high-risk groups (i.e., minority or low-income populations), which further highlights the impact of these programs.
Thirty-seven of the fifty-nine articles (63%) focused on vulnerable healthcare populations. Within these thirty-seven studies, twenty-eight (76%) of them had positive conclusions regarding the role of patient navigators during cancer treatment. Eight of the sixteen studies that found significant improvement in treatment initiation for navigated patients were studies focused on disadvantaged patients [14,15,16,17,18,19,20,21, 25] Eight of the twelve studies that observed enhanced treatment adherence rates were done in disadvantaged populations as well [37, 39, 41,42,43,44, 47, 48]. Marginalized populations often struggle navigating the complex healthcare system and experience many barriers that lead to them not receiving the care that they need. With the help of patient navigators, they get to work closely with underserved patients and personalize a plan with their healthcare team to ensure that the treatment regimen is viable for the patient. These navigators can assist patients from different backgrounds throughout their cancer journey and help improve abandonment rates, treatment delays, and lead to better health outcomes.
Although the research is limited on the impact navigators have on palliative care, the three articles identified in this review consistently highlight favorable outcomes linked to the utilization of navigation services. The studies have demonstrated increased emotional and psychosocial support for both the patient and their family members. Patient navigators possess the capacity to assist patients in navigating the complex and challenging journey of managing a cancer diagnosis, relieving suffering, and providing support near the end of life through education, care coordination, and advance care planning. Given these promising effects but limited data, more research is necessary to understand the potential impact patient navigation programs hold in palliative care.
Our clinical trial search contained themes similar to our literature review. One trial utilized a culturally sensitive and personalized smartphone app, in addition to patient navigation, to assess change in adherence to endocrine hormone therapy amongst breast cancer patients [76]. The mobile app augments the patient navigation intervention by providing at-home educational content to patients in terms of potential side effects, management of symptoms, self-care skills etc. Another study utilizes text message navigation to provide patients with guidance while considering convenience for patients [87]. The American Cancer Society also recently launched their ACE CARES app which provides services for patients throughout their cancer journey [91]. Providing valuable information and navigation for cancer patients just at their fingertips could immensely improve their cancer journey. It could facilitate easier communication with their healthcare team and be more convenient overall for the patient. Digital literacy among users will need to be considered, and more research will be needed to fully understand its implementation and benefits for navigation.
It is notable that a significant proportion of the reviewed studies primarily focused on the impact of patient navigators in breast cancer care. While these studies provide valuable insights into the potential benefits of patient navigation, there exists a notable gap in the representation of other cancer types. This overrepresentation of breast cancer calls for increased attention to other cancer types to ensure a comprehensive understanding of the role of patient navigators across diverse oncological landscapes. The intricacies of treatment regimens, patient experiences, and healthcare disparities can vary substantially among different cancer populations. Diversifying the scope of investigation would not only provide a more nuanced understanding of the impact of patient navigators but also shed light on tailored strategies that could benefit patients facing less frequently studied cancers.
The recent decision by the Centers for Medicare and Medicaid Services (CMS) to reimburse patient navigation services for cancer patients is a significant step forward in enhancing the quality of care for individuals grappling with cancer [92]. Previously, navigation services were not billable, meaning that hospitals had to fund these services themselves. Now hospitals can use reimbursement codes for patient navigation services for cancer patients. This makes it more feasible for hospitals to allocate resources towards patient navigation. The decision not only recognizes the value of patient navigation in improving healthcare outcomes but also aligns with the broader healthcare trends of emphasizing patient-centered care and value-based reimbursement models. By reimbursing these services, CMS encourages healthcare providers to invest in comprehensive patient care and promotes a holistic approach to cancer treatment.
There are limitations to this review. Unpublished works and conference abstracts were not included, which may have created a potential for a lack of all-encompassing information. However, our search criteria was broad and allowed us to evaluate many publications. By limiting studies to English, there may be a lack of generalizability for international patient navigation programs. Studies that implemented patient navigation with cancer patients but not during their cancer treatment timeline were excluded. These studies may provide insight on the benefits of patient navigation, but this review was specifically focused on the duration of cancer treatment.
Conclusion
In conclusion, this systematic review suggests compelling evidence supporting the role of patient navigators in cancer treatment. The studies in this review revealed how patient navigation can improve treatment initiation, adherence, quality of care, and patient satisfaction for many cancer patients, especially in disadvantaged populations. With upcoming policy changes improving the cost-effectiveness of these programs it is our hope that more widespread adoption may take place, and subsequently more patients will benefit from these valuable services.
Data Availability
No datasets were generated or analyzed during the current study.
References
Freeman HP, Rodriguez RL. History and principles of patient navigation. Cancer. 2011;117(S15):3537–40.
Patient navigation in cancer care. [cited 2024 Feb 19]. Available from: https://www.cancer.org/cancer/patient-navigation.html.
Patient navigation | CDC. 2023 [cited 2024 Feb 19]. Available from: https://www.cdc.gov/cancer/community-resources/interventions/patient-navigation.htm.
Hopkins J, Mumber MP. Patient navigation through the cancer care continuum: an overview. J Oncol Pract. 2009;5(4):150–2.
Cancer Control Continuum | Division of Cancer Control and Population Sciences (DCCPS). [cited 2023 Aug 18]. Available from: https://cancercontrol.cancer.gov/about-dccps/about-cc/cancer-control-continuum.
Ali-Faisal SF, Colella TJF, Medina-Jaudes N, Benz SL. The effectiveness of patient navigation to improve healthcare utilization outcomes: a meta-analysis of randomized controlled trials. Patient Educ Couns. 2017;100(3):436–48.
Roland KB, Milliken EL, Rohan EA, DeGroff A, White S, Melillo S, et al. Use of community health workers and patient navigators to improve cancer outcomes among patients served by federally qualified health centers: a systematic literature review. Health Equity. 2017;1(1):61–76.
Tho PC, Ang E. The effectiveness of patient navigation programs for adult cancer patients undergoing treatment: a systematic review. JBI Database Syst Rev Implement Rep. 2016;14(2):295–321.
Baik SH, Gallo LC, Wells KJ. Patient navigation in breast cancer treatment and survivorship: a systematic review. J Clin Oncol. 2016;34(30):3686–96.
Dalton M, Holzman E, Erwin E, Michelen S, Rositch AF, Kumar S, et al. Patient navigation services for cancer care in low-and middle-income countries: A scoping review. PLoS ONE. 2019;14(10): e0223537.
Harun A, Harrison JD, Young JM. Interventions to improve patient participation in the treatment process for culturally and linguistically diverse people with cancer: a systematic review. Asia Pac J Clin Oncol. 2013;9(2):99–109.
Ruiz-Pérez I, Rodríguez-Gómez M, Pastor-Moreno G, Escribá-Agüir V, Petrova D. Effectiveness of interventions to improve cancer treatment and follow-up care in socially disadvantaged groups. Psychooncology. 2019;28(4):665–74.
Hong Q, Pluye P, Fàbregues S, Bartlett G, Boardman F, Cargo M, et al. Mixed Methods appraisal tool (MMAT), version 2018. Registration of Copyright (#1148552), Canadian Intellectual Property Office, Industry Canada.
Haideri NA, Moormeier JA. Impact of patient navigation from diagnosis to treatment in an urban safety net breast cancer population. J Cancer. 2011;2:467–73.
Dudley DJ, Drake J, Quinlan J, Holden A, Saegert P, Karnad A, et al. Beneficial effects of a combined navigator/promotora approach for Hispanic women diagnosed with breast abnormalities. Cancer Epidemiol Biomarkers Prev. 2012;21(10):1639–44.
Mireles-Aguilar T, Tamez-Salazar J, Muñoz-Lozano JF, Lopez-Martinez EA, Romero C, Platas A, et al. Alerta Rosa: Novel Alert and navigation breast cancer program in Nuevo Leon, Mexico, for reducing health system interval delays. Oncologist. 2018;23(12):1461–6.
Ramirez A, Perez-Stable E, Penedo F, Talavera G, Carrillo JE, Fernández M, et al. Reducing time-to-treatment in underserved Latinas with breast cancer: the six cities study: Latina breast cancer patient navigation. Cancer. 2014;120(5):752–60.
Rohsig V, Silva P, Teixeira R, Lorenzini E, Maestri R, Saraiva T, et al. Nurse navigation program: outcomes from a breast cancer center in Brazil. Clin J Oncol Nurs. 2019;23(1):E25-31.
Tamez-Salazar J, Mireles-Aguilar T, De La Garza-Ramos C, Garcia-Garcia M, Ferrigno AS, Platas A, et al. Prioritization of patients with abnormal breast findings in the Alerta Rosa navigation program to reduce diagnostic delays. Oncologist. 2020;25(12):1047–54.
Perez‐Bustos AH, Orozco‐Urdaneta M, Erazo R, Cordoba‐Astudillo P, Gallo D, Muñoz‐Zuluaga C, et al. A patient navigation initiative to improve access to breast cancer care in Cali, Colombia. Cancer Rep. 2022 [cited 2023 Aug 18];5(9). Available from: https://onlinelibrary.wiley.com/doi/10.1002/cnr2.1564.
Vieira CM, Diniz PHC, Dizon DS, Nogueira-Rodrigues A. Patient navigation (PN) support to timely access to radiotherapy in the Brazilian public health system. Support Care Cancer. 2023;31(3):182.
Kunos C, Olszewski S, Espinal E. Impact of nurse navigation on timeliness of diagnostic medical services in patients with newly diagnosed lung cancer. J Community Support Oncol. 2015;219–24.
Zibrik K, Laskin J, Ho C. Implementation of a lung cancer nurse navigator enhances patient care and delivery of systemic therapy at the British Columbia Cancer Agency, Vancouver. J Oncol Pract. 2016;12(3):e344–9.
Hunnibell LS, Rose MG, Connery DM, Grens CE, Hampel JM, Rosa M, et al. Using nurse navigation to improve timeliness of lung cancer care at a Veterans Hospital. Clin J Oncol Nurs. 2012;16(1):29–36.
Muñoz R, Farshidpour L, Chaudhary U, Fathi A. Multidisciplinary Cancer care model: a positive association between oncology nurse navigation and improved outcomes for patients with cancer. Clin J Oncol Nurs. 2018;22(5):E141–5.
Gordils-Perez J, Schneider S, Gabel M, Trotter K. Oncology Nurse navigation: development and implementation of a program at a comprehensive cancer center. Clin J Oncol Nurs. 2017;21(5):581–8.
Enomoto LM, Fenstermaker J, Desnoyers RJ, Pasche BC, Blackstock AW, Howerton RM, et al. Oncology navigation decreases time to treatment in patients with pancreatic malignancy. Ann Surg Oncol. 2019;26(5):1512–8.
Ohlstein JF, Brody-Camp S, Friedman S, Levy JM, Buell JF, Friedlander P. Initial experience of a patient navigation model for head and neck cancer. JAMA Otolaryngol Neck Surg. 2015;141(9):804.
Burhansstipanov L, Krebs LU, Dignan MB, Jones K, Harjo LD, Watanabe-Galloway S, et al. Findings from the native navigators and the Cancer Continuum (NNACC) Study. J Cancer Educ. 2014;29(3):420–7.
Koh C, Nelson JM, Cook PF. Evaluation of a patient navigation program. Clin J Oncol Nurs. 2011;15(1):41–8.
Battaglia TA, Gunn CM, Bak SM, Flacks J, Nelson KP, Wang N, et al. Patient navigation to address sociolegal barriers for patients with cancer: A comparative-effectiveness study. Cancer. 2022;128(S13):2623–35.
Wagner EH, Ludman EJ, Aiello Bowles EJ, Penfold R, Reid RJ, Rutter CM, et al. Nurse navigators in early cancer care: a randomized, controlled trial. J Clin Oncol. 2014;32(1):12–8.
Freund KM, Battaglia TA, Calhoun E, Darnell JS, Dudley DJ, Fiscella K, et al. Impact of patient navigation on timely cancer care: the patient navigation research program. JNCI J Natl Cancer Inst. 2014 [cited 2023 Aug 18];106(6). Available from: https://academic.oup.com/jnci/article-lookup/doi/10.1093/jnci/dju115.
Dockery LE, Motwani A, Ding K, Doescher M, Dvorak JD, Moore KN, et al. Improving cancer care for American Indians with cervical cancer in the Indian Health Service (IHS) system — Navigation may not be enough. Gynecol Oncol. 2018;149(1):89–92.
Serrell EC, Hansen M, Mills G, Perry A, Robbins T, Feinberg M, et al. Prostate cancer navigation: initial experience and association with time to care. World J Urol. 2019;37(6):1095–101.
Vilchis H, Onstad LE, Benavidez R, Castillo R, Bush N, Sanchez J, et al. Una Mano amiga: pilot test of a patient navigator program for Southwest New Mexico. J Cancer Educ. 2019;34(1):173–9.
Fouad M, Wynn T, Martin M, Partridge E. Patient navigation pilot project: results from the Community Health Advisors in Action Program (CHAAP). Ethn Dis. 2010;20(2):155–61.
Ko NY, Darnell JS, Calhoun E, Freund KM, Wells KJ, Shapiro CL, et al. Can Patient navigation improve receipt of recommended breast cancer care? Evidence from the National Patient Navigation Research Program. J Clin Oncol. 2014;32(25):2758–64.
Petereit D, Omidpanah A, Boylan A, Kussman P, Baldwin D, Banik D, et al. A multi-faceted approach to improving breast cancer outcomes in a rural population, and the potential impact of patient navigation. S D Med J S D State Med Assoc. 2016;69(6):268–73.
Benn CA, Ramdas Y, Netcare Breastcare Centre of Excellence, Milpark Hospital, Johannesburg, South Africa, Van Den Bergh B, Netcare Breastcare Centre of Excellence, Milpark Hospital, Johannesburg, South Africa, Bannerman NL, et al. Colour Coding Navigation: “Triage” techniques to improve compliance in breast cancer patients requiring primary chemotherapy. Eur J Breast Health. 2020;16(4):262–6.
Čačala SR, Farrow H, Makhanya S, Couch DG, Joffe M, Stopforth L. The value of navigators in breast cancer management in a South African Hospital. World J Surg. 2021;45(5):1316–22.
Luckett R, Pena N, Vitonis A, Bernstein MR, Feldman S. Effect of patient navigator program on no-show rates at an academic referral colposcopy clinic. J Womens Health. 2015;24(7):608–15.
Dessources K, Hari A, Pineda E, Amneus MW, Sinno AK, Holschneider CH. Socially determined cervical cancer care navigation: an effective step toward health care equity and care optimization. Cancer. 2020;126(23):5060–8.
Salcedo M, Gowen R, Rodriguez A, Fisher-Hoch S, Daheri M, Guerra L, et al. Addressing high cervical cancer rates in the Rio Grande Valley along the Texas-Mexico border: a community-based initiative focused on education, patient navigation, and medical provider training/telementoring. Perspect Public Health. 2023;143(1):22–8.
Gaston CL, Taleon K, Barsales K, Dimayuga C, Estanislao J, Fajardo P, et al. The effect of a patient navigator on treatment abandonment and follow-up for high grade osteosarcoma patients in the Philippine General Hospital. Asian Pac J Cancer Prev. 2021;22(9):2873–7.
Percac-Lima S, Cronin PR, Ryan DP, Chabner BA, Daly EA, Kimball AB. Patient navigation based on predictive modeling decreases no-show rates in cancer care: Targeted Navigation Decreases No-Show Rates. Cancer. 2015;121(10):1662–70.
Koffi KG, Silué DA, Laurent C, Boidy K, Koui S, Compaci G, et al. AMAFRICA, a patient-navigator program for accompanying lymphoma patients during chemotherapy in Ivory Coast: a prospective randomized study. BMC Cancer. 2019;19(1):1247.
Guadagnolo BA, Boylan A, Sargent M, Koop D, Brunette D, Kanekar S, et al. Patient navigation for American Indians undergoing cancer treatment: utilization and impact on care delivery in a regional healthcare center. Cancer. 2011;117(12):2754–61.
Ell K, Vourlekis B, Xie B, Nedjat-Haiem FR, Lee PJ, Muderspach L, et al. Cancer treatment adherence among low-income women with breast or gynecologic cancer: a randomized controlled trial of patient navigation. Cancer. 2009;115(19):4606–15.
Fiscella K, Whitley E, Hendren S, Raich P, Humiston S, Winters P, et al. Patient navigation for breast and colorectal cancer treatment: a randomized trial. Cancer Epidemiol Biomarkers Prev. 2012;21(10):1673–81.
Bickell NA, Geduld AN, Joseph KA, Sparano JA, Kemeny MM, Oluwole S, et al. Do community-based patient assistance programs affect the treatment and well-being of patients with breast cancer? J Oncol Pract. 2014;10(1):48–54.
Gabitova G, Burke NJ. Improving healthcare empowerment through breast cancer patient navigation: a mixed methods evaluation in a safety-net setting. BMC Health Serv Res. 2014;14(1):407.
Jean-Pierre P, Winters PC, Clark JA, Warren-Mears V, Wells KJ, Post DM, et al. Do better-rated navigators improve patient satisfaction with cancer-related care? J Cancer Educ. 2013;28(3):527–34.
Berezowska A, Passchier E, Bleiker E. Evaluating a professional patient navigation intervention in a supportive care setting. Support Care Cancer. 2019;27(9):3281–90.
Mir O, Ferrua M, Fourcade A, Mathivon D, Duflot-Boukobza A, Dumont S, et al. Digital remote monitoring plus usual care versus usual care in patients treated with oral anticancer agents: the randomized phase 3 CAPRI trial. Nat Med. 2022;28(6):1224–31.
Lee T, Ko I, Lee I, Kim E, Shin M, Roh S, et al. Effects of nurse navigators on health outcomes of cancer patients. Cancer Nurs. 2011;34(5):376–84.
Berezowska A, Passchier E, Bleiker E. Professional patient navigation in a hospital setting: a randomized controlled trial. Support Care Cancer. 2021;29(4):2111–23.
Guadagnolo BA, Cina K, Koop D, Brunette D, Petereit DG. A Pre-post survey analysis of satisfaction with health care and medical mistrust after patient navigation for American Indian cancer patients. J Health Care Poor Underserved. 2011;22(4):1331–43.
Fillion L, De Serres M, Cook S, Goupil RL, Bairati I, Doll R. Professional patient navigation in head and neck cancer. Semin Oncol Nurs. 2009;25(3):212–21.
Post DM, McAlearney AS, Young GS, Krok-Schoen JL, Plascak JJ, Paskett ED. Effects of patient navigation on patient satisfaction outcomes. J Cancer Educ. 2015;30(4):728–35.
Wells KJ, Winters PC, Jean-Pierre P, Warren-Mears V, Post D, Van Duyn MAS, et al. Effect of patient navigation on satisfaction with cancer-related care. Support Care Cancer. 2016;24(4):1729–53.
Chen F, Mercado C, Yermilov I, Puig M, Ko CY, Kahn KL, et al. Improving breast cancer quality of care with the use of patient navigators. Am Surg. 2010;76(10):1043–6.
Weber JJ, Mascarenhas DC, Bellin LS, Raab RE, Wong JH. Patient navigation and the quality of breast cancer care: an analysis of the breast cancer care quality indicators. Ann Surg Oncol. 2012;19(10):3251–6.
Castaldi M, Safadjou S, Elrafei T, McNelis J. A Multidisciplinary patient navigation program improves compliance with adjuvant breast cancer therapy in a public hospital. Am J Med Qual. 2017;32(4):406–13.
Raj A, Ko N, Battaglia TA, Chabner BA, Moy B. Patient navigation for underserved patients diagnosed with breast cancer. Oncologist. 2012;17(8):1027–31.
Winget M, Holdsworth L, Wang S, Veruttipong D, Zionts D, Rosenthal EL, et al. Effectiveness of a lay navigation program in an Academic Cancer Center. JCO Oncol Pract. 2020;16(1):e75-83.
Todd Yezefski MD, Jordan Steelquist BA, Kate Watabayashi BA, Dan Sherman MA, Veena Shankaran MD. Impact of trained oncology financial navigators on patient out-of-pocket spending. 2018 [cited 2023 Aug 18];24. Available from: https://www.ajmc.com/view/impact-of-trained-oncology-financial-navigators-on-patient-outofpocket-spending.
Hu B, Boselli D, Pye LM, Chen T, Bose R, Symanowski JT, et al. Equal access to care and nurse navigation leads to equitable outcomes for minorities with aggressive large B-cell lymphoma. Cancer. 2021;127(21):3991–7.
Lee Stirling S, Etland C, Connelly CD, Calero P, Ecoff L. Oncology nurse navigator effect on emergency department visits and hospital admissions of adults with cancer post-outpatient chemotherapy. Oncol Nurs Forum. 2022;49(6):595–612.
Soto-Perez-de-Celis E, Chavarri-Guerra Y, Ramos-Lopez WA, Alcalde-Castro J, Covarrubias-Gomez A, Navarro-Lara Á, et al. Patient navigation to improve early access to supportive care for patients with advanced cancer in resource-limited settings: a randomized controlled trial. Oncologist. 2021;26(2):157–64.
Fink RM, Kline DM, Siler S, Fischer SM. Apoyo con Cariño: a qualitative analysis of a palliative care-focused lay patient navigation intervention for Hispanics with advanced cancer. J Hosp Palliat Nurs. 2020;22(4):335–46.
Dionne-Odom JN, Azuero A, Taylor RA, Dosse C, Bechthold AC, Currie E, et al. A lay navigator-led, early palliative care intervention for African American and rural family caregivers of individuals with advanced cancer (Project Cornerstone): results of a pilot randomized trial. Cancer. 2022;128(6):1321–30.
Impact Of Nurse Navigation Program on Outcomes in Patients With GI Cancers - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04602611.
Patient Navigation to Improve Patient Centered Cancer Care - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT03226405.
pCHIP: Prostate Cancer Health Impact Program - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04293406.
Improving Adherence to EHT Among Breast Cancer Patients - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT02850939.
Assessment of Financial Difficulty in Participants With Chronic Lymphocytic Leukemia and Multiple Myeloma - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT03870633.
Addressing Cancer-Related Financial Toxicity in Rural Oncology Care Settings - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04931251.
Navigation on Head and Neck Radiotherapy - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04857749.
Navigate - Improving Survival in Vulnerable Lung Cancer Patients - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT05053997.
Telehealth Based Synchronous Navigation to Improve Molecularly-Informed Care for Patients With Lung Cancer. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT05790460.
Financial Navigation Program to Improve Understanding and Management of Financial Aspects of Cancer Care for Patients and Their Spouses - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04960787.
Cancer Financial Experience - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT05018000.
Translating Research Into Practice - ClinicalTrials.gov. Accessed March 24, 2023. https://clinicaltrials.gov/study/NCT03514433.
Multi-Site Trial of Navigation vs Treatment as Usual for Delays in Starting Adjuvant Therapy. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT05793151.
Rural Lung and Head and Neck Cancer Intervention - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04916990.
Mobile intervention to improve adherence of oral anti-cancer medications among acute myeloid leukemia patients, the txt4AML Study - ClinicalTrials.gov. [cited 2023 Mar 24]. Available from: https://clinicaltrials.gov/study/NCT05595135?cond=Cancer&intr=navigation&term=txt4aml&rank=1.
A Multilevel Intervention to Improve Timely Cancer Detection and Treatment Initiation - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04141449.
Assessing the Impact of a Financial Navigation Program for Patients With Multiple Myeloma -ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT05448196.
Navigation vs Usual Care for Timely Adjuvant Therapy for Patients With Locally Advanced HNSCC - ClinicalTrials.gov. Accessed March 25, 2023. https://clinicaltrials.gov/study/NCT04030130.
ACS CARESTM. [cited 2024 Jan 9]. Available from: https://www.cancer.org/support-programs-and-services/acs-cares.html.
Calendar Year (CY) 2024 Medicare Physician Fee Schedule Final Rule | CMS. [cited 2023 Dec 5]. Available from: https://www.cms.gov/newsroom/fact-sheets/calendar-year-cy-2024-medicare-physician-fee-schedule-final-rule#:~:text=CY%202024%20PFS%20Ratesetting%20and%20Conversion%20Factor&text=CMS%20is%20also%20finalizing%20significant,2023%20conversion%20factor%20of%20%2433.89.
Author information
Authors and Affiliations
Contributions
Matthew Chen—conceptualization, writing—original draft preparation, writing—review and editing, methodology, data curation, formal analysis and investigation. Victoria Wu—writing—original draft preparation, writing—review and editing, methodology, data curation. Richard Hoehn—conceptualization, writing—review and editing. Derek Falk: writing – review and editing. Chesley Cheatham: writing—review and editing. Jennifer Cullen: writing – review and editing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, M., Wu, V.S., Falk, D. et al. Patient Navigation in Cancer Treatment: A Systematic Review. Curr Oncol Rep 26, 504–537 (2024). https://doi.org/10.1007/s11912-024-01514-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11912-024-01514-9