Abstract
Most drugs used in standard regimens for acute lymphoblastic leukemia (ALL) were developed more than 30 years ago. Since that time, several new drugs have been developed and incorporated into ALL treatment. In spite of this, novel therapeutic approaches are still needed to improve outcomes for high-risk or relapsed ALL. This manuscript discusses newer treatment strategies, including purine nucleoside analogs, monoclonal antibodies, antibody drug conjugates, mammalian target of rapamycin (mTOR) inhibitors, proteasome inhibitors, histone deacetylase (HDAC) inhibitors, hypomethylating agents, spleen tyrosine kinase inhibitors, Bruton’s tyrosine kinase (BTK) inhibitors, Janus kinase-signal transducer and activator of transcription (JAK-STAT) inhibitors, anti-programmed cell death protein (anti-PD-1) antibodies, mitogen-activated protein kinase (MEK) inhibitors, CXCR4 antagonists, poly (ADP-ribose) polymerase (PARP) inhibitors, and FMS-like tyrosine kinase 3 (FLT3) inhibitors. Additionally, this manuscript discusses the impact of diagnostic approaches on management of ALL. Specifically, minimal residual disease is increasingly felt to be important and will likely dramatically impact the care of ALL patients in the near future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Approximately 6000 new cases of acute lymphoblastic leukemia (ALL) are diagnosed in the USA annually. About 60% of these cases occur in children and adolescents younger than 20 years of age, with cure rates approaching 90% [1,2,3]. The remaining percentage will develop relapsed/refractory (R/R) disease, and the survival rate remains poor for this group [4•]. Adult ALL portends a dimmer prognosis. Pediatric-based remission induction regimens have allowed most younger adults to achieve complete remission (CR), but 20–30% will relapse and the five-year OS rate is only 40–50% [5].
Nearly all medications used as the standard of care for pediatric ALL were developed prior to the 1980s. In the 1990s, the Berlin-Frankfurt-Münster (BFM) regimen was developed [6]. In the early 2000s, imatinib was incorporated into treatment for those with Philadelphia chromosome-positive (Ph+) ALL. In the 2000s, nelarabine was approved for relapsed T cell ALL and the addition of rituximab to hyperfractionated cyclophosphamide, vincristine, and doxorubicin, alternating with high-dose methotrexate and cytarabine (hyper-CVAD), was found to improve outcomes in adult B-ALL [7•]. It has since been incorporated into standard therapy for CD20-positive (CD20+) B-ALL. Additionally, young adults have superior outcomes when treated with pediatric-like ALL protocols, compared to standard adult chemotherapy regimens [8]. Despite these advances in treatment modalities, there remains an unmet need for novel therapeutic approaches in the R/R setting in both pediatric ALL and in the adult population [9].
Previous sections in this journal have addressed pediatrics, Ph+ALL, stem cell transplantation (SCT) and chimeric antigen receptor T cell (CAR T) therapy. This section explores novel therapeutic strategies that are being studied in either preclinical or mostly early clinical settings. Ongoing ALL clinical trials are discussed below and summarized in Tables 1 and 2; most have not been published. Discussion of active trials studying post-transplant maintenance therapy will be deferred.
Purine Nucleoside Analog: Nelarabine
Nelarabine is a purine nucleoside analog that is metabolized to arabinosylguanine nucleotide triphosphate (araGTP); araGTP incorporates into DNA and inhibits DNA synthesis, resulting in apoptosis. Nelarabine has been studied in the past two decades and was approved in 2005 as third-line treatment of T cell leukemia/lymphoma. Several trials are currently evaluating the role of nelarabine in first-line or risk-adapted chemotherapy regimens. A phase II French study is evaluating nelarabine incorporated into consolidation and maintenance therapy in high-risk T cell ALL (NCT02619630). As part of a larger ALL trial evaluating chemotherapy optimization in ALL, a phase III study will investigate the use of nelarabine as consolidation therapy in T-ALL (NCT02881086).
Anti-CD20 Monoclonal Antibodies and Related Drug Conjugates: Rituximab, Ofatumumab, and Obinutuzumab
CD20 is a protein expressed on the surface of B cells and the main interest in CD20 stems from its near-ubiquitous expression in B cell lymphomas. In leukemia, however, CD20 is expressed on only 30–50% of precursor B cell lymphoblasts [10]. Monoclonal antibodies (mAb) currently being used or studied in ALL include rituximab, ofatumumab, and obinutuzumab.
Rituximab binds to CD20 and rapidly eliminates B cells through complement-dependent cytotoxicity, antibody-dependent cellular cytotoxicity (ADCC), and stimulation of apoptosis. Rituximab improved CR rates and OS when combined with standard induction and consolidation chemotherapy in patients with CD20+ ALL [10]. The GRAALL-2005 study evaluated the addition of rituximab to chemotherapy in patients with Ph-negative (Ph-), CD20+ B cell ALL. Rituximab was given during induction, salvage re-induction, consolidation, late intensification, and maintenance) [11]. Its addition improved 2-year event-free survival (EFS) and 2-year OS (65 vs. 52%; P = 0.038 and 74 vs. 63%; P = 0.018, respectively) when censored for SCT [12]. Of all patients who underwent SCT, the rituximab group had longer EFS and OS (hazard ratio (HR) 0.59; P = 0.02 and HR 0.55; P = 0.02, respectively) [11].
Ofatumumab is a fully human, type I anti-CD20 mAb targeting the small-loop epitope on CD20, with more complement-dependent cytotoxicity than rituximab. Ofatumumab is currently approved for chronic lymphocytic leukemia (CLL) [13]. A phase II trial combined ofatumumab with hyper-CVAD in newly diagnosed ALL patients. Interim results showed the 3-year CR rate was 78% and the 3-year OS was 68%. Three-year OS was slightly longer in CD20-negative (CD20-) patients compared to CD20+ ones but this was not statistically significant [14]. A current phase II trial assesses the combination of ofatumumab and augmented BFM in patients with precursor B ALL/lymphoblastic lymphoma (NCT02419469).
Obinutuzumab is a humanized type II anti-CD20 mAb. In contrast to type I anti-CD20 antibodies rituximab and ofatumumab, obinutuzumab has less complement-dependent cytotoxicity, less ADCC and little direct cytotoxicity [15]. Preclinical investigations showed obinutuzumab-induced cell death in rituximab-sensitive or rituximab-resistant precursor B-ALL in xenografted mice [16]. Future studies investigating obinutuzumab for precursor B-ALL are warranted.
Anti-CD19 Monoclonal Antibodies and Related Drug Conjugates: Blinatumomab, Denintuzumab Mafodotin, and ADCT-402
CD19 is a protein expressed on the surface of B cells throughout their lifecycle and works with other surface molecules to direct downstream signaling. Approximately 80% of ALL lymphoblasts express high levels of CD19 [17].
Blinatumomab is the first FDA-approved bispecific T cell engager (BiTE) antibody, linking two single-chain antibodies which bind CD3 and CD19. When the BiTE molecule binds to CD3 on T cells and CD19 on B cells, inflammatory cytokine release and T cell proliferation occur, leading to redirected lysis of CD19+ cells [18]. Blinatumomab was approved for the treatment of R/R Ph- ALL in 2014 and continues to be studied in different contexts of ALL. The phase III TOWER trial evaluated blinatumomab against standard chemotherapy in R/R ALL. Interim results demonstrated a nearly doubled median OS with blinatumomab compared to standard therapy (7.7 vs. 4 months) [19]. CR rate was also higher with blinatumomab compared to standard chemotherapy (39 vs. 19%) and the study was stopped early for efficacy. Future usage of blinatumomab is likely to increase and current studies are investigating its use in the frontline and R/R setting in different subtypes of ALL (NCT02143414, NCT02003222, and NCT02807883). Challenges with blinatumomab administration include 4-week continuous infusion cycles. Side effects include cytokine release syndrome and neurologic toxicities, requiring close monitoring during infusion.
Denintuzumab mafodotin is an antibody drug conjugate (ADC) linking an anti-CD19 antibody to monomethyl auristatin F (MMAF), a cytotoxic agent. Once internalized, MMAF causes cell cycle arrest and leads to apoptosis [20]. A phase I study evaluated denintuzumab mafodotin in patients with R/R B-ALL and other hematologic malignancies. Of those treated with weekly dosing, 22% of patients had a CR or partial remission (PR). Of those treated every 21 days, 35% had a CR (though some had incomplete platelet or blood recovery) [21].
ADCT-402 is an ADC linking a humanized anti-CD19 antibody to a cytotoxic pyrrolobenzodiazepine dimer. Upon binding and internalization, the cytotoxic dimer cross-links and inhibits DNA replication, inhibiting proliferation of CD19-expressing tumor cells. In vitro and in vivo testing demonstrated anti-tumor activity at varying degrees of CD19 expression, though the effect was less potent in CD19- cell lines [22]. A phase I trial evaluating ADCT-402 in patients with R/R B cell ALL is ongoing (NCT02669264).
CAR T cell therapy for ALL is discussed in a previous section.
Anti-CD22 Monoclonal Antibodies and Related Drug Conjugates: Inotuzumab Ozogamicin, Moxetumomb Pasudotox, Coltuximab Ravtansine, and Epratuzumab
CD22 is a B cell lineage antigen expressed on mature B-cells, some immature B-cells, and 90% of lymphoblasts in pre-B-ALL [10, 23]. Upon cross linking of B cell antigen receptor by the antigen, CD22 is rapidly phosphorylated and modulates B cell activation and function, mediating apoptosis in subsets of B cells.
Inotuzumab ozogamicin is an ADC consisting of cytotoxic agent calicheamicin linked to an anti-CD22 antibody [24]. When inotuzumumab ozogamicin binds to CD22 and is internalized, calicheamicin induces DNA breakage [25]. The phase III INO-VATE ALL study evaluated inotuzumab ozogamicin in R/R CD22+ ALL [26]. The CR rate, PFS, and median OS was higher with inotuzumab ozogamicin group compared to standard chemotherapy arm (80.7 vs. 29.4%; P < 0.001, 5.0 vs. 1.8 months; P < 0.001 and 7.7 vs. 6.7 months; P = 0.04). Inotuzumab ozogamicin is currently being studied with combination chemotherapy in R/R patients (NCT01925131) and older patients (NCT01371630). Inotuzumab ozogamicin is also being studied in combination with bendamustine, fludarabine with or without rituximab as conditioning therapy with an allogeneic SCT (NCT01664910). At this time, inotuzumab ozogamicin remains available only for compassionate use in the USA.
Moxetumomab pasudotox (MP) is a recombinant immunoconjugate composed of an anti-CD22 immunoglobulin variable domain fused to a fragment of a Pseudomonas exotoxin. Once MP binds to CD22 and internalizes, the bacterial exotoxin catalyzes the apoptosis cascade [27]. MP is currently being investigated in ALL (phase I/II study in R/R ALL (NCT01891981)).
Coltuximab ravtansine (SAR3419) is an ADC linked to cytotoxic maytansinoid (DM4) linked to an anti-CD19 antibody. Upon internalization, DM4 inhibits microtubule assembly and tubulin polymerization, leading to cell cycle arrest. Coltuximab ravtansine is being investigated in several trials for non-Hodgkin lymphoma, but the phase II study for R/R ALL was terminated early due to low clinical response rate [28].
Epratuzumab is an anti-CD22 mAb that is internalized after binding to CD22. Epratuzumab transfers proteins that are associated with B cell receptor (BCR) to effector cells. Thus, while epratuzumab targets CD22-expressing B cells, overall B cell destruction is reduced. In a phase II Children’s Oncology Group (COG) trial, epratuzumab was added to standard re-induction chemotherapy for first relapse of pre-B cell ALL. The addition of epratuzumab was well tolerated, but the rates of achieving CR the second time (CR2) was not better than historical controls [29]. A phase II is assessing CR2 rates of R/R ALL treated with epratuzumab, cytarabine, and clofarabine (NCT00945815).
Anti-CD52 Monoclonal Antibodies: Alemtuzumab
CD52 is expressed in 36–66% of leukemia cells [30]. Alemtuzumab is a recombinant mAb directed against CD52; the proposed mechanism is lysis of leukemia cells expressing CD52 by ADCC [31]. Due to severe side effects of lymphopenia prolonged immunosuppression and lack of robust efficacy data in multiple small trials, alemtuzumab not frequently used for ALL [10]. A current trial is evaluating alemtuzumab in combination with recombinant human IL-15 for patients with R/R acute or chronic adult T cell leukemia (NCT02689453).
MTOR Inhibitors: Everolimus, Temsirolimus, and Sirolimus
The PI3K/Akt/mTOR signaling pathway is observed to be aberrantly activated in a variety of malignancies, including T cell ALL and pre-B-ALL [32]. Constitutive activation may also play a role in chemotherapy resistance. Phosphorylation and activation of PI3K/Akt pathway promotes cell growth and metabolism. Mammalian target of rapamycin (mTOR) is a serine/threonine kinase that is a downstream target of Akt that exists in two protein complexes: mTORC1 and mTORC2.
Everolimus, temsirolimus, and sirolimus inhibit mTOR kinase activity by binding to intracellular protein FKBP-1, forming a complex that inhibits mTOR signaling. Murine models and human cell line studies have demonstrated downregulated mTORC1 and mTORC2 activity, decreased phosphorylation of enzymes in Akt and mTOR signaling, and increased apoptosis in pre-B-ALL cell lines treated with everolimus [32,33,34]. An Italian study found a synergistic effect when everolimus was combined with Akt inhibitor MK-2206 [32]. Such findings provide strong rationale for the investigation of mTOR inhibition in ALL, particularly in the setting of resistance to chemotherapeutic drugs.
A single-institution phase I/II trial testing everolimus in combination with hyper-CVAD for R/R ALL in pediatric patients showed that the combination was well tolerated. The CR and PR rates were 25 and 8%, respectively [35].
Ongoing trials include National Cancer Institute (NCI) phase II trial studying temsirolimus in R/R ALL and other malignancies (NCT00084916), phase I COG study ADVL1114 exploring temsirolimus in combination with intensive re-induction therapy for R/R ALL (NCT01403415), phase I trial evaluating sirolimus and corticosteroids in R/R ALL (NCT00874562), phase I trial studying everolimus with multi-agent re-induction chemotherapy in pediatric relapsed ALL (NCT01523977), phase I trial studying temsirolimus with etoposide, cyclophosphamide, and dexamethasone for relapsed pediatric ALL (NCT01614197), and NCI-sponsored multi-center phase II trial with TORC1/2 inhibitor sapanisertib in R/R ALL in adults (NCT02484430). Results from all these trials are pending.
Proteasome Inhibitors: Bortezomib, Carfilzomib, and Ixazomib
Nuclear factor kappa-B (NF-ΚB) is a transcriptional activator with anti-apoptotic properties which plays a role in a variety of malignancies. Proteasome inhibitors inactivate NF-ΚB and impair tumor growth [4•]. Bortezomib is a reversible 26S proteasome inhibitor that showed preclinical activity against ALL, but minimal single-agent activity [36,37,38]. Preclinical studies demonstrated synergy between bortezomib and the combination of dexamethasone, asparaginase, vincristine, doxorubicin, and cytarabine [39].
A phase I Therapeutic Advances in Childhood Leukemia & Lymphoma (TACL) study showed bortezomib was well tolerated in combination with re-induction chemotherapy in R/R pediatric ALL [40]. The phase II expansion of the TACL study found an overall response rate of 73%. B-precursor subtypes responded better than T cell subtypes (80 vs. 0%, though only two of the 22 patients had T cell subtype) [38].
The phase II AALL07P1 COG study investigated the efficacy of bortezomib with re-induction chemotherapy vincristine, prednisone, pegasparagase, and doxorubicin for relapsed ALL. The CR rate was 69% in pre-B-ALL (n = 61) and 65% in T cell ALL (n = 17) [41]. A phase II study investigating bortezomib with re-induction chemotherapy in adults is recruiting (NCT01769209) while another phase II trial is investigating the same question in pediatric and young adult patients (NCT02535806). A randomized phase III COG study (AALL1231) is studying combination chemotherapy with or without bortezomib for younger patients with newly diagnosed T cell ALL or stage II-IV T cell lymphoblastic lymphoma (NCT02112916). Bortezomib has also been investigated in combination with other classes of drugs, including epigenetic-targeting agents such as histone deacetylases (HDAC) inhibitors.
Carfilzomib achieves a higher degree of proteasome inhibition compared to bortezomib with fewer off-target effects. A phase I study of carfilzomib for treatment of AML or ALL was completed in 2014 and results are pending (NCT01137747). The maximum tolerated dose of carfilzomib combined with hyper-CVAD is being studied in a phase I study (NCT02293109). In addition, the safety and tolerability of carfilzomib with re-induction therapy for relapsed ALL are being evaluated as well (NCT02303821).
Ixazomib, the newest proteasome inhibitor that is also orally administered, is being studied in a phase I trial, in combination with chemotherapy for ALL (NCT02228772).
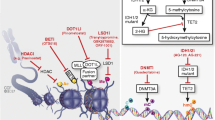
Epigenetic Targeting: HDAC Inhibitors—Belinostat, Vorinostat, and Panobinostat
The silencing of tumor suppressor genes can lead to oncogenesis in leukemias. Histone acetyltransferases and HDACs add and remove acetyl groups to and from lysine residues on histones. Net deacetylation results in suppressed transcription of tumor suppressor genes [4•]. HDAC inhibitors block cellular proliferation, promote differentiation, and induce apoptosis.
A phase I trial evaluating the safety of vorinostat, an HDAC inhibitor, showed anti-tumor activity in 17% of patients with hematologic malignancies, but most did not have ALL [42]. A newer phase I study of vorinostat and decitabine with solid tumors or relapsed leukemias was completed (NCT00275080); results are pending. A phase II study of vorinostat and decitabine with chemotherapy for relapsed ALL was terminated due to toxicity (NCT01483690).
Belinostat, another HDAC inhibitor, and bortezomib were studied in a phase I trial in multiple tumor types, including recurrent adult T cell leukemia/lymphoma (NCT00348985); results for this study are pending. Panobinostat, the newest HDAC inhibitor, has been studied in a phase I trial (NCT01321346) in multiple malignancy types in children and adults; results are pending. An ongoing phase II study is investigating the addition of panobinostat, bortezomib, and liposomal vincristine to salvage therapy for relapsed T-ALL in children and young adults (NCT02518750).
Epigenetic Targeting: DNMT Inhibitors (Hypomethylating Agents)—Azacitidine and Decitabine
DNA methyltransferase (DNMT) inhibition has been investigated as a therapeutic strategy in order to undo or decrease the repression of regulatory genes. Azacitidine and decitabine are cytosine analogs that are incorporated into nucleic acids and promote degradation of DNMTs, thus restoring normal gene differentiation and proliferation.
In vitro studies of relapsed ALL, cell samples treated with DNMT inhibitors with and without HDAC inhibitors showed restoration of normal gene expression [43]. A phase I TACL trial studied azacitidine in combination with chemotherapy for relapsed ALL or AML. This drug combination was well tolerated [44]. A pilot TACL study of decitabine and vorinostat combined with chemotherapy for relapsed pediatric ALL was initiated but was terminated due to toxicity (NCT01483690).
BTK Inhibitors: Ibrutinib
The BCR signaling pathway plays an essential role in B cell development and function, which includes the Bruton’s tyrosine kinase (BTK). Preclinical studies have investigated the activity of ibrutinib, an oral selective irreversible inhibitor of BTK, in B cell ALL. Mouse xenograft models and human ALL cell line studies found that ibrutinib suppressed pre-BCR-positive ALL proliferation both in vitro and in vivo [45, 46]. These data provide a rationale for clinical testing of ibrutinib in B-ALL with active pre-BCR signaling, either as a single agent or in combination with other therapies. While ibrutinib has been added to the armamentarium of therapies in CLL, it has yet to play a distinct role in ALL. A phase II trial of ibrutinib in R/R B cell ALL was terminated in 2016 due to slow accrual (NCT02129062). A phase II study of ibrutinib and blinatumomab in adult patients with R/R B cell ALL is planned but not yet open to recruitment (NCT02997761).
BCL2 Inhibitors: Navitoclax and Venetoclax
The B cell lymphoma-2 (BCL-2) proteins tightly regulate cell death. Evasion of cell death by malignant cells and the regulation of apoptosis have become an intense area of drug development over the last several years. BCL-2 inhibitors block the binding of BCL-2 to anti-apoptotic proteins, triggering cell death. Navitoclax (ABT-263) is a BCL-2 inhibitor which showed responses in patient-derived xenograft models of B cell precursor, T-ALL, and MLL-mutated ALL [47]; however, dose-limiting thrombocytopenia has limited the progress of navitoclax in pediatric ALL trials. A second-generation, selective BCL-2 inhibitor venetoclax (ABT-199) has demonstrated activity against ALL in xenograft models [48]. While it has shown promise in the treatment of CLL and studies in other B cell malignancies are underway (e.g., NCT02419560), venetoclax has yet to be tested in ALL.
JAK-STAT Inhibitors
The Janus kinase-signal transducer and activator of transcription (JAK-STAT) cell signaling pathway regulates gene transcription. JAK1/2/3 are tyrosine kinases, and mutations in these, especially JAK2, have been implicated in myeloproliferative neoplasms. Even in the absence of JAK mutations, aberrant over-activation of this signaling pathway has been described in other malignancies such as Ph-like ALL.
Xenograft models studied showed decreased leukemia burden with ruxolitinib, a selective JAK1/2 inhibitor [49]. Most of the cell lines had mutations in JAK2 or cytokine receptor-like factor 2 (CRLF2). A phase II COG study is evaluating ruxolitinib with multi-agent chemotherapy in children with newly diagnosed JAK-mutated or CRLF2-rearranged B cell ALL (NCT02723994).
Since amplification of the JAK-STAT signaling pathway has implicated in Ph-like ALL, studies are also evaluating the use of ruxolitinib, compared to tyrosine kinase inhibitors like dasatinib, in combination with chemotherapy, in this subtype of ALL. A phase I study is evaluating the addition of ruxolitinib to dasatinib plus dexamethasone in Ph+ALL (NCT02494882). A phase II study is underway to assess the response rates of Ph-like ALL to either ruxolitinib or dasatinib in combination with chemotherapy (NCT02420717).
PD-1 Inhibitors: Nivolumab
Presentation of peptides by major histocompatibility complex (MHC) enables native T cells to recognize tumor-specific antigens [50]. Malignant cells evade immunosurveillance as they lack expression of costimulatory molecules and induce anergy. Nivolumab is a human IgG4 monoclonal antibody against anti-programmed cell death protein-1 (PD-1); nivolumab dampens T cell anergy and allows immunosurveillance of malignant cells to take place. Nivolumab has been approved for treatment of non-small cell lung cancer, melanoma, and relapsed Hodgkin lymphoma. Little is known about the role of nivolumab in ALL. A phase I study is recruiting patients to investigate nivolumab plus dasatinib in patients with R/R Ph+ALL (NCT02819804). A phase I study is investigating blinatumomab, nivolumab with or without ipilimumab in patients with poor-risk R/R CD19+ precursor B cell ALL (NCT02879695).
MEK Inhibitors
Ras pathway mutations are common, occurring in 40% of relapsed pediatric ALL cases [51]. Kirsten rat sarcoma (KRAS) and neuroblastoma RAS (NRAS) gene mutations identified at the time of diagnosis have no prognostic significance in ALL, but if developed during frontline treatment, patients are more likely to have chemoresistant disease and poorer OS.
Mitogen-activated protein kinase (MEK) inhibition with selumetinib showed in vitro and in vivo activity in RAS-mutated ALL cell samples [51]. Combined MEK and PI3K/AKT inhibition was also studied, which showed cytotoxicity in T-ALL cell samples [52]. Despite this information, further studies of MEK inhibitors in ALL are lacking. Pimasertib, a MEK1/2 inhibitor, was investigated in a variety of hematologic malignancies including ALL, but this phase II study was terminated due to low probability of clinical benefit (NCT00957580). Trametinib has been investigated in other hematologic malignancies but has not yet been investigated in ALL.
PARP Inhibitors: Veliparib
Poly (ADP-ribose) polymerase (PARP) is a single-strand break sensing protein and PARP inhibitors have been shown to be cytotoxic to cancer cells but preventing the repair of DNA damage in malignant cells. Preclinical studies showed anti-proliferative effects on human cell lines in patients with adult T cell leukemia/lymphoma by inducing apoptosis [53].
A phase I, multi-center study is evaluating veliparib and temozolomide in patients with acute leukemia, including multiple subtypes of ALL (NCT01139970). Another phase I study is evaluating veliparib and topotecan with or without carboplatin with various hematologic malignancies including R/R ALL (NCT00588991). A phase I/II trial is evaluating veliparib, bendamustine, and rituximab in the setting of multiple malignancies, including R/R ALL (NCT01326702).
FLT3 Inhibitors: Midostaurin, Quizartinib, and Lestaurtinib
FMS-like tyrosine kinase 3 (FLT3) has long been recognized as a target in leukemia, as the receptor is overexpressed on most blast cells and certain leukemias have high rates of FLT3 mutations. Despite this, no FLT3 inhibitors have been incorporated into routine treatment for leukemia yet.
Midostaurin, a multi-target protein kinase inhibitor with anti-FLT3 activity was investigated in R/R MLL-arranged ALL and FLT3-positive AML. This phase I/II study was terminated due to poor accrual (NCT00866281). Quizartinib, an anti-FLT3 TKI, was investigated in R/R childhood ALL or AML in a TACL study (NCT01411267). Lestaurtinib, an inhibitor of FLT3, JAK2, and other tyrosine kinases, is currently being studied in a laboratory biomarker study in infants (NCT01150669). A phase III study evaluating combination chemotherapy with and without lestaurtinib in young children is ongoing (NCT00557193).
Risk Assessments Impacting Therapeutic Strategy: Minimal Residual Disease
Recent studies have demonstrated that minimal residual disease (MRD) measured during treatment constitutes the single most important prognostic indicator [54]. High levels of MRD are associated worse prognosis. The preeminent theory is that MRD measurement can be used to tailor treatment by identifying high-risk patients who require more intensity therapy, while sparing low- or standard-risk patients of unnecessary treatment-related morbidities [54].
A large, multi-national, randomized trial (AIEOP-BFM-ALL 2000) investigated the use of MRD in childhood ALL. Patients underwent MRD testing on days 33 and 78 of induction therapy. MRD negative patients were randomized to standard delayed intensification or reduced-intensity delayed intensification. The 4-year cumulative incidence of relapse, disease-free survival and OS were not statistically different [55].
The recent National Comprehensive Cancer Network guidelines for ALL state MRD testing is an essential aspect of following patients after morphologic CR is achieved [56]. There are commercially available tests for MRD assessments, but MRD testing is still not yet fully incorporated. Barriers to the routine incorporation of MRD testing into clinical care include different study techniques, lack of availability, difficult implementation, cost, turn-around time, and standardization of definitions/levels even within the US [57].
Conclusion
At the University of Virginia, younger, fit patients with ALL are treated with the augmented BFM, hyper-CVAD, or CALGB 10403 regimens. Rituximab and dasatinib are added for CD20+ and Ph+ALL, respectively. Higher-risk patients undergo allogeneic SCT in first-CR. In older or less fit patients, treatments are individualized. Vincristine, steroids, and low-dose anthracyclines are administered for four weekly infusions as induction therapy. Zoster and Pneumocystis pneumonia prophylaxis are used for all patients. For R/R disease, treatments depend on the ALL subtype. Nelarabine and blinatumomab are utilized for R/R T- and B-ALL, respectively. In Ph+ disease, mutation testing is performed for TKI resistance. If relapse occurs within 1 year of achieving remission, then re-induction is with a different regimen; re-induction therapy with the same regimen is considered if relapse occurs after 1 year.
Significant strides have been made in the last few decades in the treatment of pediatric and adult ALL. Multiple novel therapeutic strategies have emerged and focus on specific aspects of ALL. Enhanced understanding of the complexities of cellular signaling pathways has led to exploration of other treatment strategies. MRD is also readily becoming a routine aspect of following patients in remission to prognosticate their relapse risk, with a high potential to impact treatment. There is a gradual but inevitable shift towards personalization of management for ALL patients, which mirrors the shift in the oncologic treatment landscape at large.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Inaba H, Greaves M, Mullighan CG. Acute lymphoblastic leukaemia. Lancet. Elsevier Ltd; 2013;381(9881):1943–55.
Pui C-H. Recent research advances in childhood acute lymphoblastic leukemia. J Formos Med Assoc. Formosan Medical Association & Elsevier; 2010;109(11):777–87.
Hunger SP, Lu X, Devidas M, et al. Improved survival for children and adolescents with acute lymphoblastic leukemia between 1990 and 2005: a report from the children’s oncology group. J Clin Oncol. 2012;30(14):1663–9.
• Annesley CE, Brown P. Novel agents for the treatment of childhood acute leukemia. Ther Adv Hematol. 2015;6(2):61–79. This reference provides high-yield information regarding drugs with newer mechanisms of action being investigated, some of which were not able to be mentioned within the scope of our manuscript.
Gökbuget N, Stanze D, Beck J, et al. Outcome of relapsed adult lymphoblastic leukemia depends on response to salvage chemotherapy, prognostic factors, and performance of stem cell transplantation. Blood. 2012;120(10):2032–41.
Seibel NL. Acute lymphoblastic leukemia: an historical perspective. Am Soc Hematol Educ Progr. 2008;365
• Thomas DA, Faderl S, O’Brien S, Bueso-Ramos C, Cortes J, Garcia-Manero G, et al. Chemoimmunotherapy with hyper-CVAD plus rituximab for the treatment of adult Burkitt and Burkitt-type lymphoma or acute lymphoblastic leukemia. Cancer. 2006;106(7):1569–80. This reference provides useful information regarding mechanisms of action being studied. Specifically, it contains detailed discussion regarding monoclonal antibodies and their increasingly important role in the care of ALL.
DeAngelo DJ, Stevenson KE, Dahlberg SE, Silverman LB, Couban S, Supko JG, et al. Long-term outcome of a pediatric-inspired regimen used for adults aged 18–50 years with newly diagnosed acute lymphoblastic leukemia. Leukemia. Nature Publishing Group; 2015;29(3):526–34.
Papadantonakis N, Advani AS. Recent advances and novel treatment paradigms in acute lymphocytic leukemia. Ther Adv Hematol. 2016;7(5):252–69.
Jabbour E, Brien SO, Ravandi F, et al. Monoclonal antibodies in acute lymphoblastic leukemia. Blood. 2015;125(26):4010–6.
Maury S, Chevret S, Thomas X, et al. Rituximab in B-lineage adult acute lymphoblastic leukemia. N Engl J Med. 2016;375:1044–53.
Jabbour E, Kantarjian H. Immunotherapy in adult acute lymphoblastic leukemia: the role of monoclonal antibodies. Blood Adv. 2016;1(3):260–4.
Thomas DA, Brien SO, Jorgensen JL, et al. Prognostic significance of CD20 expression in adults with de novo precursor B-lineage acute lymphoblastic leukemia prognostic significance of CD20 expression in adults with de novo precursor B-lineage acute lymphoblastic leukemia. Blood. 2014;113(25):6330–7.
Sasaki K, Kantarjian HM, Ravandi F, et al. Frontline ofatumumab in combination with hyper-CVAD for adult patients with CD-20 positive acute lymphoblastic leukemia (ALL): interim result of a phase II clinical trial. In: American Society of Hematology Annual Meeting & Exposition. 2016. p. Abstract 2783.
Beers SA, French RR, Chan HTC, et al. Antigenic modulation limits the efficacy of anti-CD20 antibodies: implications for antibody selection. Blood. 2010;115(25):5191–201.
Awasthi A, Ayello J, Van de Ven C, et al. Obinutuzumab (GA101) compared to rituximab significantly enhances cell death and antibody-dependent cytotoxicity and improves overall survival against CD20+ rituximab-sensitive/−resistant Burkitt lymphoma (BL) and precursor B-acute lymphoblastic leukaemia. Br J Haematol. 2015;171(5):763–75.
Tedder TF. CD19: a promising B cell target for rheumatoid arthritis. Nat Rev Rheumatol. Nature Publishing Group; 2009;5(10):572–7.
Amgen. Blincyto (R) [package insert]. California, USA. 2014. p. 19.
Topp MS, Stein A, Nicola Gökbuget N et al. Blinatumomab nearly doubles survival in acute lymphoblastic leukemia. In: 2016 European Hematology Association Congress. 2016. p. Abstr S149.
Van Epps HA, Heiser R, Cao A, et al. Denintuzumab mafodotin stimulates immune responses and synergizes with CD20 antibodies to heighten anti-tumor activity in preclinical models of non-hodgkin lymphoma. In: American Society of Hematology Annual Meeting & Exposition. 2016. p. Abstract 4177.
Fathi AT, Borate U, Deangelo DJ, et al. A phase 1 study of denintuzumab mafodotin (SGN-CD19A) in adults with relapsed or refractory B-lineage acute leukemia (B-ALL) and highly aggressive lymphoma. Blood. 2015;126(23):1328.
Zammarchi F, Williams DG, Adams L, et al. Pre-clinical development of Adct-402, a novel pyrrolobenzodiazepine (PBD)-based antibody drug conjugate (ADC) targeting CD19-expressing B-cell malignancies. Blood. 2015;126(23):1564.
Sullivan-Chang L, O’Donnell RT, Tuscano JM. Targeting CD22 in B-cell malignancies: current status and clinical outlook. BioDrugs. 2013;27(4):293–304.
Shah N, Stevenson M, Yuan C, et al. Characterization of CD22 expression in acute lymphoblastic leukemia. Pediatr. 2015;62:964–9.
DiJoseph JF, Armellino DC, Boghaert ER, et al. Antibody-targeted chemotherapy with CMC-544: a CD22-targeted immunoconjugate of calicheamicin for the treatment of B-lymphoid malignancies. Blood. 2004;103(5):1807–14.
Kantarjian HM, DeAngelo DJ, Stelljes M, et al. Inotuzumab ozogamicin versus standard therapy for acute lymphoblastic leukemia. N Engl J Med. 2016;375(8):740–53.
Kreitman RJ, Pastan I. Antibody fusion proteins: anti-CD22 recombinant immunotoxin moxetumomab pasudotox. Clin Cancer Res. 2011;17(20):6398–405.
Kantarjian HM, Lioure B, Kim SK, et al. A phase II study of coltuximab ravtansine (SAR3419) monotherapy in patients with relapsed or refractory acute lymphoblastic leukemia. Clin Lymphoma Myeloma Leuk. 2016;16(3):139–45.
Raetz E, Cairo M, Borowitz M, et al. Re-induction chemoimmunotherapy with epratuzumab in relapsed acute lymphoblastic leukemia (ALL): phase II results from Children’s oncology group (COG) study ADVL04P2. Pediatr Blood Cancer. 2015;62:1171–5.
Hu Y, Turner MJ, Shields J, Gale MS, Hutto E, Roberts BL, et al. Investigation of the mechanism of action of alemtuzumab in a human CD52 transgenic mouse model. Immunology. 2009;128:260–70.
Genzyme Corporation. Campath (R) [package insert]. Massachusetts, USA. 2009. p. 1–2.
Neri LM, Cani A, Martelli AM, et al. Targeting the PI3K/Akt/mTOR signaling pathway in B-precursor acute lymphoblastic leukemia and its therapeutic potential. Leukemia. 2014;28(4):739–48.
Brown VI, Fang J, Alcorn K, et al. Rapamycin is active against B-precursor leukemia in vitro and in vivo, an effect that is modulated by IL-7-mediated signaling. Proc Natl Acad Sci U S A. 2003;100(25):15113–8.
Teachey DT, Obzut DA, Cooperman J, et al. The mTOR inhibitor CCI-779 induces apoptosis and inhibits growth in preclinical models of primary adult human ALL. Clin Oncol. 2006;107(3):1149–55.
Daver N, Boumber Y, Kantarjian H, et al. A phase I/II study of the mTOR inhibitor everolimus in combination with hyperCVAD chemotherapy in patients with relapsed/refractory acute lymphoblastic leukemia. Clin Cancer Res. 2015;21(12):2704–14.
Cortes J, Thomas D, Koller C, et al. Phase I study of bortezomib in refractory or relapsed acute leukemias phase I study of bortezomib in refractory or relapsed acute leukemias. Clin Cancer Res. 2004;10:3371–6.
Horton TM, Pati D, Plon SE, et al. A phase 1 study of the proteasome inhibitor bortezomib in pediatric patients with refractory leukemia: a Children’s Oncology Group study. Clin Cancer Res. 2007;13(5):1516–22.
Messinger YH, Gaynon PS, Sposto R, et al. Bortezomib with chemotherapy is highly active in advanced B-precursor acute lymphoblastic leukemia : therapeutic advances in childhood Bortezomib with chemotherapy is highly active in advanced B-precursor acute lymphoblastic leukemia: therapeutic advance. Blood. 2012;120(2):285–90.
Horton TM, Gannavarapu A, Blaney SM, et al. Bortezomib interactions with chemotherapy agents in acute leukemia in vitro. Cancer Chemother Pharmacol. 2006;58(1):13–23.
Messinger Y, Gaynon P, Raetz E, et al. Phase I study of bortezomib combined with chemotherapy in children with relapsed childhood acute lymphoblastic leukemia (ALL): a report from the therapeutic advances in childhood leukemia (TACL) consortium. Pediatr Blood Cancer. 2010;55:254–9.
Horton T, Lu X., O’Brien M, et al. Bortezomib reinduction therapy to improve response rates in pediatric ALL in first relapse: a Children’s Oncology Group (COG) study (AALL07P1). In: ASCO Annual Meeting. 2013. p. Abstract 10003.
Garcia-Manero G, Yang H, Bueso-ramos C, et al. Phase 1 study of the histone deacetylase inhibitor vorinostat (suberoylanilide hydroxamic acid [SAHA]) in patients with advanced leukemias and myelodysplastic syndromes. Blood. 2008;111(3):1060–6.
Bhatla T, Wang J, Morrison DJ, et al. Epigenetic reprogramming reverses the relapse-specific gene expression signature and restores chemosensitivity in childhood B-lymphoblastic leukemia. Blood. 2012;119(22):5201–10.
Sun W, Gaynon PS, Sposto R, et al. A phase 1 study of azacitidine (AZA) in combination with fludarabine and cytarabine in relapse/refractory childhood leukemia: a Therapeutic Advances in Childhood Leukemia & Lymphoma (TACL) study. Blood2. 2014;124(21):3764.
Kim E, Koehrer S, Rosin NY, et al. Activity of bruton’s tyrosine kinase (BTK) inhibitor ibrutinib (PCI-32765) in B-cell acute lymphoblastic leukemia (B-ALL). Blood. 2012;120(21):2569.
Kim E, Koehrer S, Rosin NY, et al. Brutonʼs tyrosine kinase inhibitor ibrutinib interferes with constitutive and induced pre-B cell receptor signaling in B-cell acute lymphoblastic leukemia. Blood. 2013;122(21):1399.
Suryani S, Carol H, Chonghaile TN, Frismantas V, Sarmah C, High L, et al. Cell and molecular determinants of in vivo efficacy of the BH3 mimetic ABT-263 against pediatric acute lymphoblastic leukemia xenografts. Clin Cancer Res. 2014;20(17):4520–31.
Suryani S, Evans K, Richmond J, Robbins A, Bracken L, Kurmasheva R, et al. Evaluation of the Bcl-2 inhibitor ABT-199 in xenograft models of acute lymphoblastic leukemia by the pediatric preclinical testing program. In: AACR Annual Meeting. 2015. p. Abstr nr 3276.
Maude S, Tasian S, Vincent T, et al. Targeting JAK1/2 and mTOR in xenograft models of Ph-like acute lymphoblastic leukemia. Blood. 2012;120(17):3510–8.
Batlevi CL, Matsuki E, Brentjens RJ, Younes A. Novel immunotherapies in lymphoid malignancies. Nat Rev Clin Oncol [Internet]. 2015;13:25–40.
Irving J, Matheson E, Minto L, et al. Ras pathway mutations are prevalent in relapsed childhood acute lymphoblastic leukemia and confer sensitivity to MEK inhibition. Blood. 2014;124(23):3420–30.
Canté-Barrett K, Spijkers-Hagelstein JAP, Buijs-Gladdines JGCAM, et al. MEK and PI3K-AKT inhibitors synergistically block activated IL7 receptor signaling in T-cell acute lymphoblastic leukemia. Leukemia [Internet]. Nature Publishing Group; 2016;30:1832–43.
Bai XT, Moles R, Chaib-Mezrag H, et al. Small PARP inhibitor PJ-34 induces cell cycle arrest and apoptosis of adult T-cell leukemia cells. J Hematol Oncol Journal of Hematology & Oncology. 2015;8(117):1–12.
Pui C-H, Pei D, Raimondi SC, Coustan-Smith E, Jeha S, Cheng C, et al. Clinical impact of minimal residual disease in children with different subtypes of acute lymphoblastic leukemia treated with response-adapted therapy. Leukemia. Nature Publishing Group; 2016;(August):1–28.
Schrappe M, Zimmermann M, Möricke A, et al. Reduced intensity delayed intensification in standard-risk patients defined by minimal residual disease in childhood acute lymphoblastic leukemia: Results of an International Randomized Trial in 1164 Patients (Trial AIEOP- BFM ALL 2000). In: American Society of Hematology Annual Meeting & Exposition. 2016. p. Plenary 4.
National Comprehensive Cancer Network. Acute lymphoblastic leukemia (Version 2.2016) [Internet].
Van Dongen JJM, Van Der Velden VHJ, Bruggemann M, et al. Minimal residual disease diagnostics in acute lymphoblastic leukemia: need for sensitive, fast, and standardized technologies. Blood. 2015;125(26):3996–4009.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Acute Lymphocytic Leukemias
Rights and permissions
About this article
Cite this article
Man, L.M., Morris, A.L. & Keng, M. New Therapeutic Strategies in Acute Lymphocytic Leukemia. Curr Hematol Malig Rep 12, 197–206 (2017). https://doi.org/10.1007/s11899-017-0380-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11899-017-0380-3