Abstract
Purpose of Review
The purpose of this review is to provide an update on lamin A/C (LMNA)-related cardiomyopathy and discuss the current recommendations and progress in the management of this disease. LMNA-related cardiomyopathy, an inherited autosomal dominant disease, is one of the most common causes of dilated cardiomyopathy and is characterized by steady progression toward heart failure and high risks of arrhythmias and sudden cardiac death.
Recent Findings
We discuss recent advances in the understanding of the molecular mechanisms of the disease including altered cell biomechanics, which may represent novel therapeutic targets to advance the current management approach, which relies on standard heart failure recommendations. Future therapeutic approaches include repurposed molecularly directed drugs, siRNA-based gene silencing, and genome editing.
Summary
LMNA-related cardiomyopathy is the focus of active in vitro and in vivo research, which is expected to generate novel biomarkers and identify new therapeutic targets. LMNA-related cardiomyopathy trials are currently underway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mutations in the lamin A/C gene (LMNA) cause laminopathies, a heterogeneous group of inherited disorders including muscular dystrophies and cardiomyopathy [1, 2], the latter characterized by progressive heart failure (HF), complicated by life-threatening arrhythmias, which eventually leads to death or heart transplant [3, 4, 5•]. LMNA encodes a nucleoskeletal intermediate filament dimerizing protein with complex cellular functions, including maintaining nuclear structural integrity, regulating gene expression, mechanosensing, and mechanotransduction through the lamina-associated proteins [6,7,8,9,10,11]. In humans, LMNA mutations frequently lead to a signature dysrhythmia that includes conduction disease, ventricular arrhythmias (ventricular tachycardia and ventricular fibrillation), and sudden cardiac death [4, 12], and indeed, LMNA is a major cause of arrhythmogenic cardiomyopathy (ACM) [13••].
A series of investigations have independently shown that defects of nuclear lamina due to LMNA mutations [7, 8, 14] affect mechanotransduction and mechanosensing in cardiomyocytes [15] leading to altered gene expression and cell dysregulation spanning from the nuclear lamina to the cell-cell junction. These mechanisms and the link to cardiac pump dysfunction are still incompletely understood, but their elucidation is critical for the development of novel therapies. In fact, currently, there are no specific therapies for LMNA-related cardiomyopathy, and the guidelines for cardiac dysfunction follow general recommendations for treatment of heart failure and prevention of ventricular arrhythmias and sudden cardiac death [16]. However, as discussed below, active research is ongoing to develop novel treatments though high-throughput drug discovery, repurposed molecularly directed drugs for mutation-specific altered gene pathways, siRNA-based gene silencing for malignant gene mutations, and genome editing.
Molecular Mechanisms Involved in the Pathogenesis of LMNA Cardiomyopathy
The paucity of human heart tissue from dilated cardiomyopathy (DCM) patients with identified LMNA mutations has hindered research discovery of the molecular mechanisms responsible for the pathogenesis of DCM. Subsequently, the lack of cellular targets has hampered the development of effective drug treatments for DCM patients with LMNA mutations. Therefore, several murine models with LMNA mutations (Table 1) have been generated to bridge the gap between genotype and phenotype and are aimed to unravel the pathogenic signaling pathways affecting DCM patients with LMNA mutations in order to facilitate the development of therapeutic treatments for LMNA-related DCM.
In Vivo LMNA Mouse Models
Thus far, majority of the molecular mechanisms associated with LMNA cardiomyopathy were discovered using the LmnaH222P/H222P mice [17]. Studies from hearts of male LmnaH222P/H222P mice at early stages before the onset of cardiac disease showed upregulation of mitogen-activated protein kinase (c-Jun N-terminal kinase (JNK), p38α and extracellular signal-regulated kinases 1 and 2 (ERK1 and 2), protein kinase B (AKT)/mammalian target of rapamycin complex 1 (mTORC1), and transforming growth factor-β (TGF-β) signaling. However, WNT/β-catenin signaling was downregulated in the hearts of LmnaH222P/H222P mice at a later age. The findings from LmnaH222P/H222P mice, where ERK1/2, AKT/mTORC1, TGF-β, and WNT/β-catenin signaling were involved in the pathogenesis of DCM, have been corroborated in human heart samples diagnosed with LMNA cardiomyopathy [18,19,20].
A second LMNA mouse line, homozygous for the LmnaN195K/N195K mutation, develops cardiac arrhythmias resembling DCM patients with conduction system disease [21]. The LMNA N195K mutation was identified from autosomal dominant Emery-Dreifuss muscular dystrophy (EDMD) patient, but the LmnaN195K/WT mice have indistinguishable phenotype as wild-type mice. Interestingly, when bred to homozygosity, the homozygous LmnaN195K/N195K mice die postnatally at 12 weeks old due to cardiac arrhythmia with minimal involvement of skeletal muscle. The cause of death of the mutant LmnaN195K/N195K mice was due to the mislocalization of CX43, CX40 and Hf1b/Sp4 in the heart of these mice. Moreover, expression levels of desmin were reduced at the intercalated disc and z-lines. Collectively, findings from the LmnaN195K/N195K mouse model are suggestive of defective mechanosignaling caused by the mutant LMNAN195K in the heart.
Recently, a cardiac-specific inducible transgenic mouse model expressing LmnaD300N, a mutation identified from a patient with DCM, has been generated and identified the activation of the DNA damage response/TP53 pathways as the causative mechanisms of the disease [22•]. In this mouse model, cell cycle, apoptosis, and senescence-associated secretory phenotype were dysregulated and echoed the activation of TGF-β resulting in increased myocardial fibrosis in the heart. Moreover, retinoblastoma expression was significantly downregulated resulting in dysregulation of E2F/CDKN2A/MDM2 to activate DDR/TP53 pathways. Therefore, the DDR/TP53 pathways could potentially be therapeutic targets for LMNA cardiomyopathy.
Other LMNA mouse models have been investigated [23,24,25]: Myh6-LmnaE82K and LmnaL530P/L530P showed cardiac remodeling [26]. The LMNA E82K is a DCM causing variant and involved in the activation of Fas and mitochondrial pathways responsible for apoptosis. Although the LmnaL530P/L530P mice showed enlarged heart and fibrosis, molecular mechanisms responsible for the cardiac phenotype remain to be determined.
In Vitro LMNA Models
Several in vitro studies on LMNA mutations (∆K32, E161K, R190W, N195K and M371K) showed defective structural assembly and restoration after stress, but no molecular mechanisms have been provided to explain the observed phenotype [27, 28].
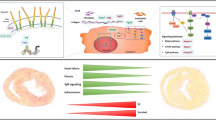
In summary, the data from LMNA mouse models and in vitro cellular models strongly suggests that mutant LMNA causes gene expression and structural defects in the heart (Fig. 1). However, the direct molecular mechanisms caused by LMNA mutations remained largely unknown. Moreover, the fact that LMNA regulates transcription factors such as Wnt and Hf1b/Sp4, the involvement of LMNA in cardiac development particularly in determining cell fate is yet to be determined.
Biophysical and Biomechanical Characteristics of Laminopathies
In 1999, it was realized for the first time that a mutation in the nuclear lamin A/C was causing (EDMD) [29]. Since then, more than 450 disease-associated lamin mutations have been discovered. Why are lamins, type V intermediate filaments specific to the nucleus, so important for their contribution in these diseases? Undoubtedly, lamins (i) provide structural support to the nucleus (indeed, they are called molecular shock absorber) and control nuclear size and stiffness [30,31,32]. (ii) They also contribute to cytoskeletal/nucleus coupling (through the LINC protein complex) [33], (iii) chromatin organization [34], (iv) DNA replication [35], and (v) transcriptional regulation [34]. As far as their mechanical roles are concerned, lamins control nuclear elasticity and deformation, and they play major role in mechanotransduction and mechanosignaling, i.e., the cell ability to react to mechanical stimuli. Being alpha-helix-based intermediate filament, lamins, in contrast to actin filaments and microtubules, withstand much larger strains of up to several hundred percent and therefore, they offer structural support under rapid, large and severe deformation. Furthermore, Ackbarow et al. [36] have shown that in the presence of a macroscopic defect, the structure and properties of the lamin alpha-helix allow shape changes which effectively protect the protein network against catastrophic failure. However, at the nano scale, the mechanisms of the damaging effects of LMNA pathogenic mutations on the lamin network are incompletely understood [37, 38].
Recently, it has been envisioned that the nucleus itself could be seen as a mechanosensor, which modulates gene expression in response to mechanical disturbances [39]. Therefore, external forces that are transferred through the cytoskeleton to the nucleus create a deformation but at the same time, based on lamin composition, can modify chromatin organization and transcriptional activity. For instance, the physical organization and location of heterochromatin inside the nucleus can change, such as the highly condensed heterochromatin normally positioned at the outer nucleus border and mostly silent is moved toward the inside increasing gene activation. Other effects might be triggered since the mechanical properties of the nucleus are primarily determined by the nuclear interior and the nuclear lamina. The elastic nuclear lamina is the major load-bearing element; however, the nuclear interior also plays a role. Chromatin is more viscoelastic in nature but any modifications in chromatin structure and organization can also affect the mechanical properties of the nucleus. At the same time, characteristic mechanical stresses can induce altered phosphorylation in nuclear envelope proteins [40]. Reduced tension leads to an increased lamin A/C phosphorylation, while increased tension produces decreased lamin A/C phosphorylation. An example is the application of shear stresses to isolated nuclei which caused the immunoglobulin (Ig) domain of lamin A to unfold, exposing a previously buried cysteine residue [41].
Force-induced stretching of nuclear membranes might be another mechanism triggered by impaired mechanotransduction. Since the nuclear lamina is much stiffer than the nuclear membrane, it protects the nuclear membrane from experiencing large mechanical forces. This “shock-absorber” function can therefore significantly modulate the stretch response of the nuclear membrane altering the distribution and organization of membrane-bound proteins [40, 42]. The aforementioned results demonstrate the relevance and the direct role of nuclear lamins in modulating transcriptional activity, nuclear and cytoskeletal organization.
In the presence of LMNA mutations, not only the nucleus and cell mechanical properties might change but also the adhesion properties at the level of outer cell membrane can be altered. For example, atomic force microscopy (AFM) and steered molecular dynamics (SMD) have been used to study three lamin mutations: Glu161Lys (E161K, rs28933093), Asp192Gly (D192G, rs57045855), and Asn195Lys (N195K, rs28933091) [32, 43•, 44•]. All three mutations cause a profound change in cardiomyocytes biomechanics leading to (i) increased nuclear stiffness, (ii) altered cellular viscoelasticity associated with modifications of the actin microfilaments network but also (iii) nearly complete loss of cell membrane work of adhesion. These findings indicate that lamins and lamina-associated proteins form a unique functional mechanical and mechanosensing entity that extends from the nucleo-skeleton to the cell membrane and which becomes destabilized by changes in any of its component elements. Furthermore, these biomechanical experiments predict that LMNA D192G will be the most damaging, followed by N195K and E161K. Remarkably, these biomechanical findings are in good agreement with clinical findings and even though genotype-phenotype correlation was evaluated in an extremely limited population, data suggest that the most severe outcome is associated with the D192G variant, while the mildest with the E161K [43•].
The aforementioned evidence indicates that nuclear configuration and deformability, as well as force transmission between the cytoskeleton and nucleus, play critical roles in activating or modulating cellular mechanotransduction signaling. These properties are particularly important in the cardiac and skeletal muscle, tissues exposed to high levels of mechanical stresses. The identification of quantifiable biomechanical alterations in laminopathies and the possibility to rescue them with therapeutic compounds make cell biomechanics and attractive biomarker for drug developments.
LMNA Phenotypes
LMNA mutations can cause a variety of different diseases that may present in a variety of combinations (Table 2) [45]. In the heart, laminopathies may cause DCM or cardiac conduction disease, and these two disorders can be present independently or overlap. LMNA-related DCM is typically characterized by left ventricular enlargement, systolic and diastolic dysfunction, and can involve the right ventricle mimicking arrhythmogenic right ventricular cardiomyopathy [51]. Conduction disease can range from atrioventricular block to atrial standstill. Supraventricular arrhythmias are frequent [52], as are ventricular arrhythmias which associate with increased risk of sudden cardiac death [4, 5•]. Thromboembolism may also be associated with LMNA-DCM [53].
LMNA mutations can cause multisystem involvement including neuromuscular, metabolic, and aging processes. Moreover, different types of muscular dystrophies are associated with LMNA, such as Emery-Dreyfuss muscular dystrophy (the autosomal dominant form EDMD2, and the recessive form EDMD3), limb-girdle muscular dystrophy (LGMD1B), and the pediatric LMNA-related congenital muscular dystrophy. LMNA-related metabolic disorders include partial lipodystrophy, insulin resistance, and hypertriglyceridemia (FPLD2) and the Malouf syndrome. Other disorders include the axonal Charcot-Marie-Tooth neuropathy (CMT2B1), skeletal abnormalities, such as brachydactyly, short stature, and heart-hand syndrome-Slovenian type. Finally, LMNA mutations can cause the premature aging Hutchinson–Gilford progeria syndrome (HGPS) and the adult-onset progeria Atypical Werner’s syndrome [45].
The understanding of the pleomorphic features of laminopathies is important from the diagnostic standpoint. In evaluating a patient with DCM, the possibility of multisystem involvement, in particular neuromuscular disease, due to LMNA mutations must be considered. An accurate skeletal muscle evaluation (CK elevation, rigidity of the spine, contractures of the elbows and Achilles tendons [54]) and the presence of atrioventricular block, supraventricular and ventricular arrhythmias, insulin resistance, and lipodystrophy can raise the clinical suspicion of a laminopathy.
Genetics of Laminopathies
LMNA mutations are inherited in an autosomal dominant manner, seen as multiple affected family members across generations, with age-related penetrance. The evaluation of DCM starts with an accurate family history, which by current guidelines should include three or more generations [13••, 47, 48]. Genetic testing should be offered to patients with DCM, in particular patients with family history of DCM, conduction disease, or sudden cardiac death, and patients with a “red flag” phenotype suspicious for laminopathies. Family cascade screening should include clinical testing with ECG and echocardiogram. If a LMNA pathogenic or likely pathogenic variant is identified according to current genetic guidelines [55], at-risk first-degree relatives should be tested to allow appropriate management. The pathogenic role of a novel LMNA variant may be difficult to assess, and in this case, the availability of the family for segregation analysis may add significant informativity [56]. The pre-test probability for a LMNA mutation rises from 5 to 8% in the DCM population to 33% when the DCM phenotype is associated with family history of DCM and conduction disease [52, 57, 58].
The type of LMNA mutation may modify the risk disease progression and arrhythmias. Non-missense mutations (ins-del/truncating, or mutations affecting splicing) are an established risk factor for malignant ventricular arrhythmias and risk of sudden cardiac death: Heterozygous truncating LMNA mutations appear to have a higher arrhythmia risk than missense variants [4, 59]; indeed, they are considered among the criteria for ICD for prevention of SCD in the AHA/ACC guidelines [50]. However, in laminopathies, the majority of reported variants are missense mutations, and their association with the prognosis is still poorly defined. In a recent analysis of LMNA mutation reported in the literature, Captur et al. [60•] found that missense mutations upstream of the nuclear localization sequence were associated with a worse prognosis.
While some of the LMNA missense variant are recurrent and therefore more frequent, such as p.Glu161Lys, providing some insights into their pathogenic effect, most of the missense variants are “private” and unique to a patient or a family, therefore very rare, making the assessment of genotype-phenotype association difficult. Another challenge in assessing the pathogenic effect of LMNA missense variants is the significant phenotype variability found even within families carrying the same mutation, probably due to the modifier effect that environmental and epigenetic factors can have on LMNA gene expressivity.
Management of LMNA-Related Cardiomyopathy
Lifestyle Modifications
Highly dynamic competitive sports for 10 years or more were found to be independent predictors of sudden cardiac death and equivalents in patients with LMNA mutations in a small series [61]. In general, there is lack of information in this regard, and the current guidelines, based on expert opinion (class III; level of evidence C), recommend that symptomatic athletes with DCM (without specifying the cause of DCM) should not participate in most competitive sports, with the possible exception of low-intensity (class 1A) sports [62].
There is little information concerning the risk of pregnancy in LMNA carriers. A small study reported a favorable outcome in early stages of cardiomyopathy and in absence of heart failure [63]. In limited studies on symptomatic DCM and in patients with family history of DCM, the prognosis appears to be poor, although some benefit has been reported with the “BOARD therapy regime” (prolactin blocker bromocriptine (BR), oral heart failure drugs, anticoagulation, diuretics) [64, 65]. A multicenter study on pregnancy in DCM is currently in progress to evaluate the risks and prognosis question in this patient population (ClinicalTrials.gov Identifier: NCT03235063).
Medical Therapy for Myocardial Dysfunction
The current management of LMNA-related cardiomyopathy follows general recommendations for the treatment of heart failure, including beta-blockers, ACE inhibitors, or angiotensin-receptor blockers, although the specific efficacy in this population is unknown (Table 2) [49, 66]. In terminal stages of heart failure, LMNA carriers may require advanced therapies such as heart transplantation or ventricular assist devices.
Therapy for Arrhythmias and Prevention of Sudden Cardiac Death
The frequent occurrence of conduction disease may require permanent pacing. The recent AHA/ACC/HRS guidelines for the prevention of sudden cardiac death [50] and the new 2019 HRS guidelines on arrhythmogenic cardiomyopathy [13••] identify the LMNA carrier status as a high-risk condition and recommend an implantable cardioverter-defibrillator even in absence of significant left ventricular dysfunction (left ventricular ejection fraction < 45%) when other predictors of life-threatening ventricular arrhythmias are present (non-sustained ventricular tachycardia, male gender, truncation mutation). For supraventricular and ventricular arrhythmias refractory to medical management, catheter ablation may be used in experienced centers (Table 2).
Recent Advances in LMNA Therapy
Advanced strategies to develop novel treatments include high-throughput drug discovery and repurposed molecularly directed drugs. Indeed, activation of the mTOR pathway was reported in LMNA-associated DCM, and, in animal models, inhibition of mTOR by temsirolimus or rapamycin was shown to rescue the DCM phenotype [67, 68]. Mitogen-activated protein kinase (MAPK) signaling is increased in LMNA-associated DCM, leading to the discovery of compounds aimed at reducing this signaling, such as Selumetinib (Array BioPharma) [69]. Recently, encouraging results were reported from a phase 2 registrational trial on A797 (Array Biopharma), an oral, selective p38 MAPK inhibitor in LMNA-associated DCM [70], and this compound is now in phase 3 clinical trial. Remarkably, there is a significant overlap in the activation of important signaling pathways (MAPK and p38, Wnt/β-catenin and mTOR, Cx43, TGFB) in LMNA, which offers opportunities for the development of novel treatments.
Other novel experimental strategies include antisense oligonucleotide therapy (siRNAs) targeting exon 11 for the treatment of progeria which aims at reducing prelamin A/progerin in favor of the alternative splicing of lamin C [71].
Finally, two recent papers report favorable results in vitro and in vivo of genome editing by CRISPR/Cas9-technology for Hutchinson–Gilford progeria syndrome, which is caused by a LMNA point mutation, in most cases a c.1824C > T; p.Gly608Gly, which activates a cryptic splice site in exon 11. Santiago-Fernández et al. Beyret et al. independently showed progerin reduction and improved the progeria phenotype in a HGPS mice model by introducing frameshift mutations with CRISPR/Cas9 technology using an adeno-associated virus 9 (AAV9) delivery vectors [72•, 73•]. Advantage of genome editing technology is the persistence of the effect compared to antisense oligonucleotides. Although off-target effects need still to be addressed, it is noteworthy to emphasize that genome editing therapies for other diseases have now entered in clinical trials, and that the HGPS gene editing model could be recapitulated in other malignant LMNA missense variants.
Conclusion
LMNA-related cardiomyopathy is one of the most common causes of dilated cardiomyopathy and is characterized by progression toward heart failure and high risk of arrhythmias and sudden cardiac death. The possible multiorgan involvement should prompt a careful examination of potential carriers and raise red flags suspicious of LMNA mutation carriers. While the current therapies are aiming at containing the progression of myocardial remodeling and the risk of life-threatening arrhythmias, investigators are exploring novel technologies to correct the gene defect or the molecular mechanisms causing the disease phenotype.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Mestroni L, Brun F, Spezzacatene A, Sinagra G, Taylor MR. Genetic causes of dilated cardiomyopathy. Prog Pediatr Cardiol. 2014;37:13–8.
Sweet ME, Taylor MRG, Mestroni L. Diseases of the nuclear membrane. In: Jeffries JL, Blaxall B, Robbins J, Towbin JA, editors. Cardioskeletal myopathies in children and young adults. London: Academic Press; 2017. p. 233–48.
Brodsky GL, Muntoni F, Miocic S, Sinagra G, Sewry C, Mestroni L. Lamin A/C gene mutation associated with dilated cardiomyopathy with variable skeletal muscle involvement. Circulation. 2000;101:473–6.
van Rijsingen IA, Arbustini E, Elliott PM, Mogensen J, Hermans-van Ast JF, van der Kooi AJ, et al. Risk factors for malignant ventricular arrhythmias in lamin a/c mutation carriers a European cohort study. J Am Coll Cardiol. 2012;59:493–500.
• Kumar S, Baldinger SH, Gandjbakhch E, Maury P, Sellal JM, Androulakis AF, et al. Long-term arrhythmic and nonarrhythmic outcomes of lamin A/C mutation carriers. J Am Coll Cardiol. 2016;68:2299–307 Important multicenter study that confirmed the prognostic effect of LMNA mutations.
Corne TD, Sieprath T, Vandenbussche J, Mohammed D, Te Lindert M, Gevaert K, et al. Deregulation of focal adhesion formation and cytoskeletal tension due to loss of A-type lamins. Cell Adhes Migr. 2016:1–17.
Osmanagic-Myers S, Dechat T, Foisner R. Lamins at the crossroads of mechanosignaling. Genes Dev. 2015;29:225–37.
Fedorchak GR, Kaminski A, Lammerding J. Cellular mechanosensing: getting to the nucleus of it all. Prog Biophys Mol Biol. 2014;115:76–92.
Nikolova V, Leimena C, McMahon AC, Tan JC, Chandar S, Jogia D, et al. Defects in nuclear structure and function promote dilated cardiomyopathy in lamin A/C-deficient mice. J Clin Invest. 2004;113:357–69.
Lammerding J, Schulze PC, Takahashi T, Kozlov S, Sullivan T, Kamm RD, et al. Lamin A/C deficiency causes defective nuclear mechanics and mechanotransduction. J Clin Invest. 2004;113:370–8.
Chandar S, Yeo LS, Leimena C, Tan JC, Xiao XH, Nikolova-Krstevski V, et al. Effects of mechanical stress and carvedilol in lamin A/C-deficient dilated cardiomyopathy. Circ Res. 2010;106:573–82.
van Berlo JH, de Voogt WG, van der Kooi AJ, van Tintelen JP, Bonne G, Yaou RB, et al. Meta-analysis of clinical characteristics of 299 carriers of LMNA gene mutations: do lamin A/C mutations portend a high risk of sudden death? J Mol Med (Berl). 2005;83:79–83.
•• Towbin JA, McKenna WJ, Abrams DJ, Ackerman MJ, Calkins H, Darrieux FCC, Daubert JP, de Chillou C, DePasquale EC, Desai MY, Estes NAM, 3rd, Hua W, Indik JH, Ingles J, James CA, John RM, Judge DP, Keegan R, Krahn AD, Link MS, Marcus FI, McLeod CJ, Mestroni L, Priori SG, Saffitz JE, Sanatani S, Shimizu W, Peter van Tintelen J, Wilde AAM and Zareba W. 2019 HRS expert consensus statement on evaluation, risk stratification, and management of arrhythmogenic cardiomyopathy. Heart rhythm. 2019. Important new guidelines intriducing the concept of arrhythmogenic cardiomyopathy spanning from ARVC to dilated cardiomyopathy and including LMNA-reated cardiomyopathy.
Dahl KN, Ribeiro AJS, Lammerding J. Nuclear shape, mechanics, and mechanotransduction. Circ Res. 2008;102:1307–18.
Moncayo-Arlandi J, Brugada R. Unmasking the molecular link between arrhythmogenic cardiomyopathy and Brugada syndrome. Nat Rev Cardiol. 2017;14:744–56.
Corrado D, Link MS, Calkins H. Arrhythmogenic right ventricular cardiomyopathy. N Engl J Med. 2017;376:61–72.
Arimura T, Helbling-Leclerc A, Massart C, Varnous S, Niel F, Lacene E, et al. Mouse model carrying H222P-Lmna mutation develops muscular dystrophy and dilated cardiomyopathy similar to human striated muscle laminopathies. Hum Mol Genet. 2005;14:155–69.
Le Dour C, Macquart C, Sera F, Homma S, Bonne G, Morrow JP, et al. Decreased WNT/beta-catenin signalling contributes to the pathogenesis of dilated cardiomyopathy caused by mutations in the lamin a/c gene. Hum Mol Genet. 2017;26:333–43.
Muchir A, Reilly SA, Wu W, Iwata S, Homma S, Bonne G, et al. Treatment with selumetinib preserves cardiac function and improves survival in cardiomyopathy caused by mutation in the lamin A/C gene. Cardiovasc Res. 2012;93:311–9.
Chatzifrangkeskou M, Le Dour C, Wu W, Morrow JP, Joseph LC, Beuvin M, et al. ERK1/2 directly acts on CTGF/CCN2 expression to mediate myocardial fibrosis in cardiomyopathy caused by mutations in the lamin A/C gene. Hum Mol Genet. 2016;25:2220–33.
Mounkes LC, Kozlov SV, Rottman JN, Stewart CL. Expression of an LMNA-N195K variant of A-type lamins results in cardiac conduction defects and death in mice. Hum Mol Genet. 2005;14:2167–80.
• Chen SN, Lombardi R, Karmouch J, Tsai JY, Czernuszewicz G, Taylor MRG, et al. DNA damage response/TP53 pathway is activated and contributes to the pathogenesis of dilated cardiomyopathy associated with LMNA (lamin A/C) mutations. Circ Res. 2019;124:856–73 Recent study on LMNA D300N unraveling the activation of the DNA damage response as a cause of cardiomyopathy.
Cattin ME, Bertrand AT, Schlossarek S, Le Bihan MC, Skov Jensen S, Neuber C, et al. Heterozygous LmnadelK32 mice develop dilated cardiomyopathy through a combined pathomechanism of haploinsufficiency and peptide toxicity. Hum Mol Genet. 2013;22:3152–64.
Lu D, Lian H, Zhang X, Shao H, Huang L, Qin C, et al. LMNA E82K mutation activates FAS and mitochondrial pathways of apoptosis in heart tissue specific transgenic mice. PLoS One. 2010;5:e15167.
Wang Y, Herron AJ, Worman HJ. Pathology and nuclear abnormalities in hearts of transgenic mice expressing M371K lamin A encoded by an LMNA mutation causing Emery-Dreifuss muscular dystrophy. Hum Mol Genet. 2006;15:2479–89.
Mounkes LC, Kozlov S, Hernandez L, Sullivan T, Stewart CL. A progeroid syndrome in mice is caused by defects in A-type lamins. Nature. 2003;423:298–301.
Zwerger M, Jaalouk DE, Lombardi ML, Isermann P, Mauermann M, Dialynas G, et al. Myopathic lamin mutations impair nuclear stability in cells and tissue and disrupt nucleo-cytoskeletal coupling. Hum Mol Genet. 2013;22:2335–49.
Bhattacharjee P, Banerjee A, Banerjee A, Dasgupta D, Sengupta K. Structural alterations of Lamin a protein in dilated cardiomyopathy. Biochemistry. 2013;52:4229–41.
Bonne G, Di Barletta MR, Varnous S, Becane HM, Hammouda EH, Merlini L, et al. Mutations in the gene encoding lamin A/C cause autosomal dominant Emery-Dreifuss muscular dystrophy. Nat Genet. 1999;21:285–8.
Cattin ME, Muchir A, Bonne G. ‘State-of-the-heart’ of cardiac laminopathies. Curr Opin Cardiol. 2013;28:297–304.
Zwerger M, Roschitzki-Voser H, Zbinden R, Denais C, Herrmann H, Lammerding J, et al. Altering lamina assembly reveals lamina-dependent and -independent functions for A-type lamins. J Cell Sci. 2015;128:3607–20.
Lanzicher T, Martinelli V, Puzzi L, Del Favero G, Codan B, Long CS, et al. The cardiomyopathy lamin A/C D192G mutation disrupts whole-cell biomechanics in cardiomyocytes as measured by atomic force microscopy loading-unloading curve analysis. Sci Rep. 2015;5:13388.
Alam SG, Lovett D, Kim DI, Roux KJ, Dickinson RB, Lele TP. The nucleus is an intracellular propagator of tensile forces in NIH 3T3 fibroblasts. J Cell Sci. 2015;128:1901–11.
Harr JC, Luperchio TR, Wong X, Cohen E, Wheelan SJ, Reddy KL. Directed targeting of chromatin to the nuclear lamina is mediated by chromatin state and A-type lamins. J Cell Biol. 2015;208:33–52.
Cobb AM, Murray TV, Warren DT, Liu Y, Shanahan CM. Disruption of PCNA-lamins A/C interactions by prelamin A induces DNA replication fork stalling. Nucleus. 2016;7:498–511.
Ackbarow T, Sen D, Thaulow C, Buehler MJ. Alpha-helical protein networks are self-protective and flaw-tolerant. PLoS One. 2009;4:e6015.
Lammerding J, Wolf K. Nuclear envelope rupture: actin fibers are putting the squeeze on the nucleus. J Cell Biol. 2016;215:5–8.
Kirby TJ, Lammerding J. Emerging views of the nucleus as a cellular mechanosensor. Nat Cell Biol. 2018;20:373–81.
Wang N, Tytell JD, Ingber DE. Mechanotransduction at a distance: mechanically coupling the extracellular matrix with the nucleus. Nat Rev Mol Cell Biol. 2009;10:75–82.
Guilluy C, Osborne LD, Van Landeghem L, Sharek L, Superfine R, Garcia-Mata R, et al. Isolated nuclei adapt to force and reveal a mechanotransduction pathway in the nucleus. Nat Cell Biol. 2014;16:376–81.
Swift J, Ivanovska IL, Buxboim A, Harada T, Dingal PC, Pinter J, et al. Nuclear lamin-A scales with tissue stiffness and enhances matrix-directed differentiation. Science. 2013;341:1240104.
Stephens AD, Banigan EJ, Adam SA, Goldman RD, Marko JF. Chromatin and lamin A determine two different mechanical response regimes of the cell nucleus. Mol Biol Cell. 2017;28:1984–96.
• Laurini E, Martinelli V, Lanzicher T, Puzzi L, Borin D, Chen SN, Long CS, Lee P, Mestroni L, Taylor MRG, Sbaizero O and Pricl S. Biomechanical defects and rescue of cardiomyocytes expressing pathologic nuclear lamins. Cardiovascular research. 2018. Study showing the biomechanical defects in different LMNA mutations and their rescue by p38 inhibitor A797.
Lanzicher T, Martinelli V, Long CS, Del Favero G, Puzzi L, Borelli M, et al. AFM single-cell force spectroscopy links altered nuclear and cytoskeletal mechanics to defective cell adhesion in cardiac myocytes with a nuclear lamin mutation. Nucleus. 2015;6:394–407.
Captur G, Arbustini E, Bonne G, Syrris P, Mills K, Wahbi K, et al. Lamin and the heart. Heart. 2018;104:468–79.
Paldino A, De Angelis G, Merlo M, Gigli M, Dal Ferro M, Severini GM, et al. Genetics of dilated cardiomyopathy: clinical implications. Curr Cardiol Rep. 2018 Aug 13;20:83.
Hershberger RE, Givertz MM, Ho CY, Judge DP, Kantor PF, McBride KL, et al. Genetic evaluation of cardiomyopathy-a Heart Failure Society of America Practice guideline. J Card Fail. 2018;24:281–302.
Hershberger RE, Givertz MM, Ho CY, Judge DP, Kantor PF, McBride KL, et al. Genetic evaluation of cardiomyopathy: a clinical practice resource of the American College of Medical Genetics and Genomics (ACMG). Genet Med. 2018;20:899–909.
Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Colvin MM, et al. 2016 ACC/AHA/HFSA focused update on new pharmacological therapy for heart failure: an update of the 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines and the Heart Failure Society of America. J Am Coll Cardiol. 2016;68:1476–88.
Al-Khatib SM, Stevenson WG, Ackerman MJ, Bryant WJ, Callans DJ, Curtis AB, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: executive summary. Circulation. 2018;138:e210–71.
Quarta G, Syrris P, Ashworth M, Jenkins S, Zuborne Alapi K, Morgan J, et al. Mutations in the lamin A/C gene mimic arrhythmogenic right ventricular cardiomyopathy. Eur Heart J. 2012;33:1128–36.
Taylor MR, Fain PR, Sinagra G, Robinson ML, Robertson AD, Carniel E, et al. Mestroni L and familial dilated cardiomyopathy registry research G. natural history of dilated cardiomyopathy due to lamin A/C gene mutations. J Am Coll Cardiol. 2003;41:771–80.
van Rijsingen IA, Bakker A, Azim D, Hermans-van Ast JF, van der Kooi AJ, van Tintelen JP, et al. Lamin A/C mutation is independently associated with an increased risk of arterial and venous thromboembolic complications. Int J Cardiol. 2013;168:472–7.
Brown CA, Lanning RW, McKinney KQ, Salvino AR, Cherniske E, Crowe CA, et al. Novel and recurrent mutations in lamin A/C in patients with Emery-Dreifuss muscular dystrophy. Am J Med Genet. 2001;102:359–67.
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405–24.
Captur G, Bilinska Z, Arbustini E. Lamin missense mutations-the spectrum of phenotype variability is increasing. Eur J Heart Fail. 2018;20:1413–6.
Karkkainen S, Helio T, Miettinen R, Tuomainen P, Peltola P, Rummukainen J, et al. A novel mutation, Ser143Pro, in the lamin A/C gene is common in finnish patients with familial dilated cardiomyopathy. Eur Heart J. 2004;25:885–93.
Arbustini E, Pilotto A, Repetto A, Grasso M, Negri A, Diegoli M, et al. Autosomal dominant dilated cardiomyopathy with atrioventricular block: a lamin A/C defect-related disease. J Am Coll Cardiol. 2002;39:981–90.
Hasselberg NE, Edvardsen T, Petri H, Berge KE, Leren TP, Bundgaard H, et al. Risk prediction of ventricular arrhythmias and myocardial function in lamin A/C mutation positive subjects. Europace. 2014;16:563–71.
• Captur G, Arbustini E, Syrris P, Radenkovic D, O'Brien B, McKenna WJ, et al. Lamin mutation location predicts cardiac phenotype severity: combined analysis of the published literature. Open Heart. 2018;5:e000915 This study showed that LMNA mutations upstream of the nuclear localization signal or C-terminal tail domain associate with a more severe cardiac phenotype.
Pasotti M, Klersy C, Pilotto A, Marziliano N, Rapezzi C, Serio A, et al. Long-term outcome and risk stratification in dilated cardiolaminopathies. J Am Coll Cardiol. 2008;52:1250–60.
Maron BJ, Udelson JE, Bonow RO, Nishimura RA, Ackerman MJ, Estes NA 3rd, et al. American Heart Association E, Arrhythmias Committee of Council on Clinical Cardiology CoCDiYCoC, Stroke Nursing CoFG, translational B and American College of C. Eligibility and Disqualification recommendations for competitive athletes with cardiovascular abnormalities: task force 3: hypertrophic cardiomyopathy, arrhythmogenic right ventricular cardiomyopathy and other cardiomyopathies, and myocarditis: a scientific statement from the American Heart Association and American College of Cardiology. Circulation. 2015;132:e273–80.
Palojoki E, Kaartinen M, Kaaja R, Reissell E, Karkkainen S, Kuusisto J, et al. Pregnancy and childbirth in carriers of the lamin A/C-gene mutation. Eur J Heart Fail. 2010;12:630–3.
Van Tintelen JP, Pieper PG, Van Spaendonck-Zwarts KY, Van Den Berg MP. Pregnancy, cardiomyopathies, and genetics. Cardiovasc Res. 2014;101:571–8.
Bondue A, Arbustini E, Bianco A, Ciccarelli M, Dawson D, De Rosa M, et al. Complex roads from genotype to phenotype in dilated cardiomyopathy: scientific update from the Working Group of Myocardial Function of the European Society of Cardiology. Cardiovasc Res. 2018;114:1287–303.
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, et al. ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37:2129–200.
Ramos FJ, Chen SC, Garelick MG, Dai DF, Liao CY, Schreiber KH, et al. Rapamycin reverses elevated mTORC1 signaling in lamin A/C-deficient mice, rescues cardiac and skeletal muscle function, and extends survival. Sci Transl Med. 2012;4:144ra103.
Choi JC, Muchir A, Wu W, Iwata S, Homma S, Morrow JP, et al. Temsirolimus activates autophagy and ameliorates cardiomyopathy caused by lamin A/C gene mutation. Sci Transl Med. 2012;4:144ra102.
Wu W, Muchir A, Shan J, Bonne G, Worman HJ. Mitogen-activated protein kinase inhibitors improve heart function and prevent fibrosis in cardiomyopathy caused by mutation in lamin A/C gene. Circulation. 2011;123:53–61.
MacRae C, Taylor MRG, Mestroni L, Moses JR, Ashley EA, Wheeler MT, et al. Phase 2 study of A797, an oral, selective p38 mitogen-activated protein kinase inhibitor, in patients with lamin A/C-related dilated cardiomyopathy. Eur Heart J. 2016;37:1011.
Lee JM, Nobumori C, Tu Y, Choi C, Yang SH, Jung HJ, et al. Modulation of LMNA splicing as a strategy to treat prelamin A diseases. J Clin Invest. 2016;126:1592–602.
• Santiago-Fernandez O, Osorio FG, Quesada V, Rodriguez F, Basso S, Maeso D, et al. Development of a CRISPR/Cas9-based therapy for Hutchinson-Gilford progeria syndrome. Nat Med. 2019;25:423–6 Recent pre-clinical study using genome editing to correct LMNA-relate progeria.
• Beyret E, Liao HK, Yamamoto M, Hernandez-Benitez R, Fu Y, Erikson G, et al. Single-dose CRISPR-Cas9 therapy extends lifespan of mice with Hutchinson-Gilford progeria syndrome. Nat Med. 2019;25:419–22 Similar recent pre-clinical study using genome editing to correct LMNA-relate progeria.
Varga R, Eriksson M, Erdos MR, Olive M, Harten I, Kolodgie F, et al. Progressive vascular smooth muscle cell defects in a mouse model of Hutchinson-Gilford progeria syndrome. Proc Natl Acad Sci U S A. 2006;103:3250–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Suet Nee Chen, Orfeo Sbaizero, and Luisa Mestroni declare that they have no conflict of interest.
Matthew RG Taylor reports grants from Array Biopharma.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Myocardial Disease
Rights and permissions
About this article
Cite this article
Chen, S.N., Sbaizero, O., Taylor, M.R.G. et al. Lamin A/C Cardiomyopathy: Implications for Treatment. Curr Cardiol Rep 21, 160 (2019). https://doi.org/10.1007/s11886-019-1224-7
Published:
DOI: https://doi.org/10.1007/s11886-019-1224-7