Abstract
Although differences diminish with age, outcomes are overall worse for women compared to men who present with suspected acute coronary syndrome. The reasons for this discrepancy are multifactorial, including sex-related differences in atherosclerosis biology and fluid dynamics, as well as a premature conclusion by providers that chest pain must be noncardiac in the absence of obstructive coronary artery disease. In this review of existing literature, we explore the diverse differential diagnosis in this unique set of patients. Especially in women with persistent symptoms, absence of occlusive disease should prompt consideration for subangiographic plaque disruption, epicardial or microvascular endothelial dysfunction, transient neurohormonal imbalance predisposing to Takotsubo cardiomyopathy or spontaneous coronary artery dissection, underlying systemic inflammatory conditions, thromboembolic disease, myocarditis, and sequelae of congenital heart disease. As always, a thorough history and attentive physical exam will help guide further work-up, which in many cases may warrant noninvasive imaging, such as contrast-enhanced echocardiography, cardiac magnetic resonance imaging, or positron emission tomography, with their respective means of measuring myocardial perfusion and myocardial tissue pathology. Lastly, intracoronary imaging such as intravascular ultrasound and optical coherence tomography and invasive diagnostic methods such as coronary reactivity testing continue to add to our understanding that what appear to be atypical presentations of ischemic heart disease in women may in fact be typical presentations of pathologic cousin entities that remain incompletely defined.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In this review of recent literature, we hope to address the following three questions as they relate to suspected ischemic heart disease among women. Are outcomes after ST elevation myocardial infarction (STEMI), non-ST elevation myocardial infarction (NSTEMI), and unstable angina (UA) worse in women compared to those in men? What is the pathophysiology of acute coronary syndrome (ACS) in women despite nonobstructive coronary artery disease by angiography? Lastly, what is the role of intracoronary and noninvasive imaging modalities and other diagnostic methods in the evaluation of women with this common presentation? In answering these questions, we hope to help centralize discussions begun in parallel, highlight the gravity of this clinical presentation, and implore our colleagues to utilize advanced modalities at their disposal to search for an underlying etiology.
Review of the Literature
Acute Coronary Syndrome Outcomes
Studies have reported somewhat mixed results comparing outcomes in women and men after acute coronary syndrome. In a single-institution study of 1197 patients presenting with NSTEMI ACS, women and men experienced similar treatment with percutaneous coronary intervention (PCI), as well as similar in-hospital and 9-month event-free survival [1]. While mortality and combined endpoints of death, myocardial infarction (MI), and target vessel revascularization were higher at 5 years in 1425 women who received PCI compared to men, female sex was not an independent predictor of outcomes after multivariate analysis took into account age and comorbidities [2]. In a 30-day mortality assessment of 136,247 patients presenting with ACS, Berger et al. found higher overall mortality in women, though again that difference disappeared after multivariate analysis [3]. Lawesson et al. followed 2132 STEMI patients younger than 46 years for a year and discovered that women had higher multivariable-adjusted in-hospital mortality, but long-term mortality was equal [4].
An overwhelming majority of large database studies however have concluded that outcomes are overall worse for women after ACS. Of 2382 patients presenting with ACS, Zdzienicka et al. compared 152 presenting without typical symptoms to those with typical symptoms [5]. The former subgroup was predominantly women, with higher in-hospital mortality rates in those presenting with NSTEMI treated conservatively [5]. The American College of Cardiology-National Cardiovascular Data Registry showed that white women presenting with stable angina had a 1.34-fold higher risk adjusted odds ratio for in-hospital mortality as compared to men, which may be attributed to lower utilization of aspirin, elective PCI, and glycoprotein IIb/IIIa inhibitors [6].
An analysis of the Global Registry of Acute Coronary Events compared outcomes of 7638 women and 19,117 men presenting with ACS and found that despite a higher prevalence of normal coronary arteries or mild coronary disease, women were more likely to experience death, MI, stroke, and rehospitalization at 6 months, even after adjustment for age and extent of disease [7]. In an exploratory analysis of 1127 patients, extent of nonobstructive disease detected by coronary computed tomography angiography (CCTA) was a predictor of mortality in women, but not in men [8].
Lee et al. compared outcomes in 1961 women and 8593 men and found higher in-hospital and 6-month mortality rates in women with STEMI and NSTEMI, as well as after PCI [9]. A French prospective, multicenter registry including 64,932 patients with suspected ACS found that women were more likely to be diagnosed with NSTEMI or UA, more likely to have angiographically normal coronary arteries after a diagnosis of both STEMI and NSTEMI, and less likely to undergo PCI or coronary artery bypass grafting (CABG) [10]. Mortality within 24 hours after PCI was also higher in women [10].
Perhaps the most influential on our current understanding of sex-based differences in MI presentation is an observational study of more than 1.1 million patients analyzed by the National Registry of Myocardial Infarction investigators [11]. Their findings were consistent with many of the aforementioned studies in that women were more likely to present without chest pain and had higher mortality compared to men in the same age group [11]. However, sex differences with regard to chest pain on presentation and mortality dissipated with age [11]. Unique to this study by Canto et al. is the stratification of patients by symptom presentation and age, which may explain some of the heterogeneity in the studies discussed above.
Pathophysiology
More interesting perhaps than apparent or actual gender bias is the surfacing of a still incompletely defined umbrella entity, that of ischemic heart disease with nonobstructive coronary arteries which appears to affect both women and men, but with a clear predilection for women. Moreover, persistent symptoms despite a negative angiogram portend a poorer prognosis. In a subanalysis of 673 participants from the Women’s Ischemia Syndrome Evaluation (WISE) study, Johnson et al. found that women with nonobstructive coronary disease but persistent chest pain at one year had more than twice the number of cardiovascular events, including MIs, strokes, heart failure, and cardiovascular-related death compared to women without persistent symptoms [12]. This provides justification for further diagnostic evaluation in this particularly high-risk group of women [12].
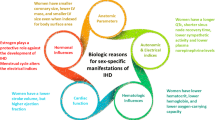
The diagnostic evaluation of nonobstructive coronary disease should include consideration of the following potential etiologies: subangiographic atherosclerotic disease, endothelial dysfunction, neurohormonal imbalance, inflammatory disease, thromboembolic disease, myocarditis, and rarely, sequelae of congenital heart disease [13–15]. Before expounding, inherent differences in plaque development between women and men must be reviewed.
Plaque Development
Yahagi et al. describe plaque rupture, erosion, and calcified nodules as the three underlying mechanisms for luminal thrombus causing ACS [16•]. Overall, plaque erosion is more common in women and plaque rupture is more common in men [16•]. Plaque rupture is more frequent in women over 50, and plaque erosion is more common in women younger than 50 [16•, 17]. This parallels a previous finding that thin-cap fibroatheromas in women occur most commonly after age 50 and with total cholesterol over 210 mg/dL [17].
With regard to plaque progression, Virmani et al. showed that erythrocyte-derived cholesterol that accumulates in the necrotic core of atherosclerotic plaques is a trigger for destabilization [18]. Virmani et al. hypothesized that vasospasm may contribute to the pathophysiology of plaque erosion as a basis for ACS, as the media layer tends to be thicker at these sites than at sites of rupture [17]. They found that calcification is uncommon in vulnerable plaques and is directly proportional to age with a 10-year lag in women as compared to men, though this difference is attenuated by the eighth decade [17].
There are dramatic sex differences not only in plaque biology but in fluid dynamics and endothelial shear stress that contribute to coronary atherosclerosis development in women, and vary with hormonal milieu [19•]. Mechanisms related to coronary flow differential have been offered as an explanation as to why anginal equivalent and atypical symptoms more commonly plague women [19•]. The relatively low estrogen state after menopause accelerates the development of atherosclerosis by contributing to the shift in both endothelial function and predominant plaque type during a woman’s lifetime [16•, 19•].
Mechanisms of plaque progression and destabilization are more variable in women compared to men, and thus, the angiographic appearance of atherosclerosis may be at best different and at worst falsely reassuring. See Fig. 1.
A 56-year-old woman with no cardiovascular risk factors presenting with fatigue and dyspnea on exertion is found to have non-ST elevation myocardial infarction and new left ventricular systolic dysfunction, and undergoes coronary angiography. a Angiography demonstrates moderate disease in the proximal to mid-segment of her left anterior descending coronary artery. b Qualitative assessment suggests an intermediate lesion. c Intravascular ultrasound (IVUS) however reveals significant stenosis, with a minimal luminal area of 2.7 mm2. d With intra-aortic balloon pump support in place, percutaneous stent implantation is pursued and post-dilation IVUS confirms restoration of a luminal area consistent with a large-caliber vessel. e Angiography displays satisfactory post-intervention results
In Search of an Etiology
Subangiographic Atherosclerotic Disease
One reason that nonobstructive disease leads to worse outcomes in women is plaque disruption undetected by angiography alone. A study by Iqbal et al. showed underlying plaque disruption by intravascular ultrasound (IVUS) in 38 % of women with MI but <50 % angiographic disease [20]. Reynolds et al. performed IVUS and cardiac magnetic resonance imaging (CMR) on 50 women presenting with MI but <50 % angiographic stenosis [21]. Again, IVUS demonstrated plaque disruption in 38 %, suggesting that angiography alone may frequently miss high-risk atherosclerotic disease [21].
What constitutes high-risk atherosclerotic disease in women is still not fully clear. Khuddus et al. performed IVUS on 100 women with suspected ischemia but without significant coronary artery disease by angiography and found a high prevalence of atherosclerosis with positive remodeling and preserved lumen size [22]. After treatment of the culprit lesion, 697 patients with ACS underwent quantitative coronary analysis (QCA), grayscale IVUS, and proprietary radiofrequency virtual histology IVUS (Volcano Corporation, San Diego, CA) [23]. Lansky et al. found that women had less extensive disease by angiographic and IVUS measures [23]. Women had overall smaller lumens, as well as less necrotic core and calcium, and less plaque rupture [23].
Endothelial Dysfunction
Endothelial dysfunction is an umbrella entity and includes frank vasospasm or impaired vasodilation on an epicardial level as well as coronary dysfunction on a microvascular level.
Epicardial vasospasm, or Prinzmetal angina, may be underdiagnosed in women and is characterized by intermittent increased vascular tone causing a reduction in lumen diameter [24]. Nitrates during angiography can dramatically reverse the heightened tone and confirm the diagnosis. Vasospasm can also be seen in cocaine toxicity, and an appropriate level of suspicion for concomitant substance abuse is important.
In recent years, a number of studies set the stage for the emergence of coronary microvascular dysfunction (CMD), which was largely borne out of “cardiac syndrome X” (CSX), coined in 1973 by Harvey Kemp [25]. Agrawal et al. draw a distinction between CSX and types of CMD which are associated with microvascular angina and coronary slow flow phenomenon [26]. These entities however may exist on a continuum and warrant better characterization.
In a retrospective cohort study of 32,856 patients with suspected ischemic heart disease, 23.3 % of women and 7.1 % of men had angiographically normal arteries, and of this subgroup, women were four times more likely to be readmitted to the hospital for ACS or chest pain requiring catheterization [27]. Similarly, Berger et al. found that 30-day mortality was higher in women diagnosed with STEMI, NSTEMI, and UA after adjustment for covariates, despite a 2-fold higher prevalence of nonobstructive disease in women with NSTEMI or UA [3]. A study by Lønnebakken et al. assessed segmental wall motion and perfusion with contrast echocardiography just prior to coronary angiography for NSTEMI [28]. They found that women had the same extent of myocardial ischemia determined by contrast echocardiography as men, but less prevalent angiographic disease [28]. These studies not only exposed a rather dramatic gender bias; they challenged traditional thinking that CSX and CMD are benign [26].
Investigators from the WISE study performed coronary reactivity testing (CRT) on a subgroup of 293 symptomatic women with nonobstructive coronary disease and followed them for a mean of 5.4 years [29]. CRT with escalating doses of adenosine, acetylcholine infusion, and nitroglycerin was safe and furthermore abnormal in half the population studied [29]. Murthy et al. reported that the presence of CMD defined by coronary flow reserve (CFR) <2.0 was noted to be highly prevalent in 813 women and 405 men with negative rest/stress positron emission tomography (PET) myocardial perfusion imaging (MPI) [30]. Worse outcomes are associated with CMD, and as such, a definitive diagnosis based on an empiric assessment of coronary reactivity or coronary flow may be warranted.
In an effort to establish a diagnosis of CMD noninvasively, Michelsen et al. measured digital reactive hyperemia index (RHI) in 322 women with angina but <50 % angiographic stenosis [31]. They found that RHI was unable to identify individuals with CMD as determined by coronary flow velocity reserve (CFVR) [31].
Evidence to support various treatments for CMD is limited at this time [26]. A recent systematic review included only 84 patients, suggesting that the search for suitable therapies for this entity is just beginning [32]. Nitric oxide modulators, angiotensin-converting enzyme inhibitors, estrogens, and transcutaneous electrical nerve stimulation have been shown to offer benefit [33]. No benefit was seen with alpha-blockers, statins, and calcium-channel blockers, and data is generally lacking for beta-blockers, nitrates, and anti-anginals [33]. A randomized, double-blind, placebo-controlled study of ranolazine for patients with CMD confirmed by CRT or myocardial perfusion reserve index (MPRI) showed no differences by treatment arm [34]. An ongoing randomized, controlled trial seeks to evaluate the phosphodiesterase-5 inhibitor udenafil as a potential treatment for CMD [35]. Results are pending.
Neurohormonal Imbalance
Another high-risk subset of patients presenting with suspected ischemic heart disease and found to have nonobstructive coronary arteries may have stress-induced left ventricular dysfunction, or Takotsubo cardiomyopathy. An observational series found significantly higher plasma catecholamine levels in patients with stress-related dysfunction compared with nonstress-related Killip class III MI [36]. A report from the SWEDEHEART registry showed that short- and long-term mortality in patients diagnosed with Takotsubo cardiomyopathy was comparable to patients with NSTEMI and STEMI [37]. A report by the International Takotsubo Registry showed that physical triggers, acute neurologic or psychiatric diseases, high troponin levels, and a low ejection fraction on admission were independent predictors for in-hospital complications [38].
A single-center retrospective review stratified 345 patients diagnosed with Takotsubo cardiomyopathy by trigger: post-operative period, emotional distress, no identifiable trigger, or medical illness, of which the lattermost conferred the worst prognosis [39]. The patient population studied was 91 % women with a mean age of 72 ± 12 years [39]. In a systematic review including 1109 patients, 86 % were women with a mean age of 59–76 years [40]. A recent review described the proposed pathophysiologic mechanisms underlying Takotsubo, including metabolic downregulation, excessive afterload and heightened left ventricular wall stress, CMD, regional cardiac catecholamine release, and beta2-adrenoceptor/Gi-dependent cardiodepression [41].
In addition to Takotsubo cardiomyopathy, spontaneous coronary artery dissection (SCAD) can present as STEMI, NSTEMI, UA, or sudden cardiac death. It predominantly affects women with mean age 42 to 52 [42]. SCAD is commonly seen in a clinical context associated with hormonal excess or disequilibrium, such as peripartum status, and after episodes of extreme exercise or emotion, as well as comorbid with connective tissue disease and systemic vasculopathy, i.e., fibromuscular dysplasia [42, 43].
In the acute setting, if coronary blood flow is preserved, a conservative strategy is preferred, whereas frank occlusion or hemodynamic instability warrant PCI or CABG [42]. In 6 of 13 cases of pregnancy-associated SCAD, IVUS or optical coherence tomography (OCT) helped confirm the diagnosis and guide management [44]. The rate of PCI failure may be high in these patients, so inpatient monitoring is appropriate regardless of the initial treatment strategy pursued [42]. Repeat pregnancy and hormonal therapy is discouraged in patients with peripartum coronary dissection, and comprehensive screening with imaging of the vasculature has also been recommended to rule out extracoronary vascular abnormalities in all patients presenting with SCAD [42].
Inflammatory Disease
Myocardial ischemia is not uncommon in chronic inflammatory conditions such as systemic lupus erythematosus (SLE), systemic sclerosis (SS), and rheumatoid arthritis (RA) [45]. Patients with SLE, anginal chest pain, and nonobstructive coronary disease by angiography underwent stress CMR MPI, which was abnormal in 44 % [46]. In addition to accelerated epicardial atherosclerosis, CMD is an increasingly recognized complication in these patients. Kakuta et al. performed Doppler echocardiography to estimate CFVR and found a significantly higher prevalence of CMD in patients with SLE (67 %), SS (76 %), and RA (63 %) compared to the control group (26 %) [47].
Thromboembolic Disease
Though not considered to be a traditional thrombophilic disorder, an elevated lipoprotein(a) (Lp(a)) level is a well-established, independent, causal, and genetic risk factor for the development of cardiovascular disease [48]. Lp(a) is the primary carrier of oxidized phospholipids throughout the bloodstream and, in concert with oxidative stress, chronic inflammation, and abnormalities of lipoprotein metabolism, is a key player in the development of atherosclerosis [49].
An elevated Lp(a) level begins to aggregate cardiovascular risk shortly after birth and has been associated with cerebrovascular events and deep vein thrombosis in childhood, as well as MI in early adulthood [48]. A statement by the European Atherosclerosis Society Consensus Panel recommends that a child with even moderate hypercholesterolemia should be genetically tested for familial hypercholesterolemia and inherited elevation of Lp(a), as this has prognostic value [50]. Target LDL-C for children older than 10 years with familial hypercholesterolemia should be less than 130 mg/dL [50].
Women are overrepresented in the category of patients who remain undiagnosed until after sustaining recurrent thrombosis-related events or procedures [48]. Extrapolated global prevalence of Lp(a) levels considered to be in the atherogenic range is estimated at 1.5 billion [48]. Monoclonal antibodies to PCSK9 have been shown to lower both LDL-C and Lp(a), but their impact on cardiovascular outcomes is still under investigation [50].
Other thrombophilic disorders leading to spontaneous coronary thrombosis constitute a rare cause of ischemia or infarction.
In a study of 1776 patients who presented with acute MI, 2.9 % were diagnosed with coronary artery embolism [51]. Of these cases, underlying atrial fibrillation was the embolic source in 73 % [51]. Kaplan-Meier analysis demonstrated higher incidence of cardiac death in the patients who suffered MI due to coronary embolism compared to a propensity score-matched cohort [51].
In addition to atrial fibrillation, septic emboli from endocarditis may infarct myocardial tissue as with any other organ. Left-sided cardiac tumors may be a nidus for thrombus formation and lead to coronary embolism.
Myocarditis
In a meta-analysis on MI in the setting of nonobstructive coronary arteries, Pasupathy et al. determined an overall prevalence of approximately 6 % [52]. Women were overrepresented in this group relative to the population with MI and obstructive coronary artery disease [52]. Pooled analysis of patients who underwent subsequent CMR imaging revealed an ultimate diagnosis of myocarditis in 33 %, true MI in 24 %, and no abnormality by CMR in 26 % [52].
Another meta-analysis by Tornvall et al. examined 556 patients, 49 % women, presenting with acute MI and nonobstructive coronary disease by angiography [53]. Subsequent CMR imaging revealed myocarditis again in 33 %, which was more common in younger people with high CRP, as well as true MI in 21 % [53]. Given that myocarditis is highly prevalent in this special population, checking CRP and searching for the typical enhancement pattern by CMR may be high yield. Making this diagnosis is important as it would end other reasonable diagnostic inquiries.
Sequelae of Congenital Heart Disease
Rarely, narrowing of the coronary arteries from sequelae of congenital heart disease can present as angina or ACS [54]. Coronary artery lumen may be distorted due to external compression from a plethoric pulmonary artery in the case of atrial septal defect and resultant pulmonary hypertension [54] or due to lateral compression in the case of anomalous coronary artery related to intramural intussusception of the vessel in the aortic root wall [55, 56].
The Role of Imaging
Intracoronary Imaging
IVUS is based on the concept of piezoelectric crystals emitting sound waves which interact with adjacent tissue and are transmitted back to the transducer, producing an image [57]. IVUS provides reasonable image resolution at 100–200 μm and can penetrate tissue beyond 5 mm, which allows for excellent plaque and endothelial wall definition [57]. The most common uses currently for IVUS surround PCI, such as assessment of minimal luminal area to determine significance of a plaque, identification of appropriate landing zones, and confirmation of adequate stent expansion [58].
IVUS has been used widely in the research setting; it has demonstrated blunted coronary vasoreactivity in NSTEMI [59] and has been used to characterize atypical atherosclerosis in angiographically nonobstructive disease [20–22]. It has also shown that appropriate treatment knows no gender bias. Among 978 patients who participated in serial assessment of atheroma progression, IVUS revealed that the rates of plaque progression or regression were not significantly different between women and men in the setting of aggressive risk factor modification [60]. Similarly, neither IVUS nor OCT demonstrated significant differences in plaque characteristics between 115 women and 268 men referred for evaluation of stable coronary artery disease, with the exception of greater plaque burden in men [61].
IVUS can be particularly useful when SCAD is suspected and has been shown to be valuable as a prognostic tool for patients with coronary artery disease. Nicholls et al. found a direct relationship between the burden of atherosclerosis, disease progression, and adverse cardiovascular events in a study involving 4137 patients [62]. The prognostic value of IVUS in ACS however is yet to be determined [58].
OCT is a newer technology that is similar to IVUS, but utilizes light instead of sound waves [57]. Blood distorts OCT imaging, so either saline or contrast must fill the coronary artery during image acquisition, which introduces variability that could limit its use [57]. In comparison to IVUS, what OCT loses in tissue penetration of only 1–2.5 mm, it makes up for in image resolution at 15–20 μm [57]. The precise role for OCT in the clinical setting is yet to be determined, but multiple studies have confirmed its ability to characterize plaque type, especially thin-cap fibroatheromas, with extremely high specificity [58]. Bogale et al. performed OCT on patients presenting with NSTEMI and angiographically intermediate disease [63]. As a result, they identified and stented atherosclerotic lesions with unstable features in 62 % of patients evaluated, though follow-up data was unavailable [63].
Prati et al. identified 31 patients, 84 % male, who presented with STEMI ultimately attributed to intact fibrous cap, as determined by OCT following aspiration thrombectomy [64]. After a median follow-up of 753 days, there was no difference in symptoms between the 12 who were treated with thrombectomy and dual antiplatelet therapy alone and the 19 who underwent aspiration thrombectomy followed by stent implantation [64]. Only one patient in the latter group required additional revascularization [64].
In a thorough review, Kanwar et al. incorporated recent data from IVUS and OCT studies into our understanding of ACS associated with intact fibrous cap [65]. It remains unclear whether the systematic use of intracoronary imaging in patients without evidence of plaque rupture can both guide management in the acute setting and improve outcomes, but with the research momentum surrounding both IVUS and OCT, these questions could be answered soon.
Noninvasive Imaging
Noninvasive imaging has shown promising results in the investigation of microvascular dysfunction. Shufelt et al. compared adenosine CMR in 53 women with CMD confirmed by CRT to age- and estrogen-matched controls [66]. They found that women with proven CMD had lower MPRI in the subendocardium and subepicardium [66]. A similar study by Thomson et al. performed vasodilator stress CMR in women with CRT-confirmed CMD and concluded that an MPRI threshold of 1.84 predicted abnormal CRT with a sensitivity of 73 % and a specificity of 74 % [67••].
PET MPI is a well-established means for diagnosing CMD [19•]. A review of the role of nuclear cardiology in the diagnosis of women with ischemic heart disease recommended PET assessment of CFR over single-photon emission computed tomography (SPECT) and conventional PET, which rely on relative perfusion distribution [68]. Such traditional interpretation methods are inadequate for diagnosing CMD. Unfortunately, limited availability of PET with CFR limits its use for this particular application [69].
Rinkevich et al. compared dipyridamole stress myocardial contrast echocardiography in women with exertional angina and abnormal stress tests to age-matched controls with no coronary artery disease [70]. They found that the stress to rest ratio of mean microbubble velocity was significantly lower in the study group, which confirmed abnormal autoregulation on the microvascular level [70].
These studies have been conducted in highly selected and small samples of women, thus limiting their generalizability and applicability in day-to-day practice.
Future Directions
Women with suspected ischemic heart disease who are found to have nonobstructive coronary artery disease comprise a special high-risk population. When the underlying etiology is not immediately evident, it is imperative that clinicians search for a diagnosis guided by a thorough history and physical exam, especially when symptoms persist. In many instances, diagnostic methods such as CFR and CRT as well as advanced imaging modalities such as IVUS, OCT, CMR, PET, and contrast echocardiography may be useful and appropriate. We propose an algorithm to assist the diagnostic work-up in the clinical setting; see Fig. 2.
Further research is needed to more diligently define the aforementioned distinct entities, and probably others, which are often grouped together in large-scale population studies such that subtle but meaningful differences are obscured.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Elkoustaf RA, Mamkin I, Mather JF, Murphy D, Hirst JA, Kiernan FJ, et al. Comparison of results of percutaneous coronary intervention for non-ST-elevation acute myocardial infarction or unstable angina pectoris in men versus women. Am J Cardiol. 2006;98(2):182–6.
Perl L, Bental T, Assali A, Vaknin-Assa H, Lev E, Kornowski R, et al. Impact of female sex on long-term acute coronary syndrome outcomes. Coron Artery Dis. 2015;26(1):11–6.
Berger JS, Elliott L, Gallup D, Roe M, Granger CB, Armstrong PW, et al. Sex differences in mortality following acute coronary syndromes. JAMA. 2009;302(8):874–82.
Lawesson SS, Stenestrand U, Lagerqvist B, Wallentin L, Swahn E. Gender perspective on risk factors, coronary lesions and long-term outcome in young patients with ST-elevation myocardial infarction. Heart. 2010;96(6):453–9.
Zdzienicka J, Siudak Z, Zawislak B, Dziewierz A, Rakowski T, Dubiel J, et al. Patients with non-ST-elevation myocardial infarction and without chest pain are treated less aggressively and experience higher in-hospital mortality. Kardiol Pol. 2007;65(7):769–75. discussion 776–7.
Shaw LJ, Shaw RE, Merz CN, Brindis RG, Klein LW, Nallamothu B, et al. Impact of ethnicity and gender differences on angiographic coronary artery disease prevalence and in-hospital mortality in the American College of Cardiology-National Cardiovascular Data Registry. Circulation. 2008;117(14):1787–801.
Dey S, Flather MD, Devlin G, Brieger D, Gurfinkel EP, Steg PG, et al. Sex-related differences in the presentation, treatment and outcomes among patients with acute coronary syndromes: the Global Registry of Acute Coronary Events. Heart. 2009;95(1):20–6.
Shaw LJ, Min JK, Narula J, Lin F, Bairey-Merz CN, Callister TQ, et al. Sex differences in mortality associated with computed tomographic angiographic measurements of obstructive and nonobstructive coronary artery disease: an exploratory analysis. Circ Cardiovasc Imaging. 2010;3(4):473–81.
Lee CY, Hairi NN, Wan Ahmad WA, Ismail O, Liew HB, Zambahari R, et al. Are there gender differences in coronary artery disease? The Malaysian National Cardiovascular Disease Database - Percutaneous Coronary Intervention (NCVD-PCI) Registry. PLoS One. 2013;8(8), e72382.
Isorni MA, Blanchard D, Teixeira N, le Breton H, Renault N, Gilard M, et al. Impact of gender on use of revascularization in acute coronary syndromes: the national observational study of diagnostic and interventional cardiac catheterization (ONACI). Catheter Cardiovasc Interv. 2015;86(2):E58–65.
Canto JG, Rogers WJ, Goldberg RJ, Peterson ED, Wenger NK, Vaccarino V, et al. Association of age and sex with myocardial infarction symptom presentation and in-hospital mortality. JAMA. 2012;307(8):813–22.
Johnson BD, Shaw LJ, Pepine CJ, Reis SE, Kelsey SF, Sopko G, et al. Persistent chest pain predicts cardiovascular events in women without obstructive coronary artery disease: results from the NIH-NHLBI-sponsored Women’s Ischaemia Syndrome Evaluation (WISE) study. Eur Heart J. 2006;27(12):1408–15.
Beltrame JF. Assessing patients with myocardial infarction and nonobstructed coronary arteries (MINOCA). J Intern Med. 2013;273(2):182–5.
Niccoli G, Scalone G, Crea F. Acute myocardial infarction with no obstructive coronary atherosclerosis: mechanisms and management. Eur Heart J. 2015;36(8):475–81.
Pasupathy S, Tavella R, Beltrame JF. The what, when, who, why, how and where of myocardial infarction with non-obstructive coronary arteries (MINOCA). Circ J. 2015;80(1):11–6.
Yahagi K, Davis HR, Arbustini E, Virmani R. Sex differences in coronary artery disease: pathological observations. Atherosclerosis. 2015;239(1):260–7. This excellent review highlights sex differences in plaque biology and mechanisms of acute coronary syndrome, complete with beautiful histopathologic illustrations.
Virmani R, Burke AP, Farb A, Kolodgie FD. Pathology of the vulnerable plaque. J Am Coll Cardiol. 2006;47(8 Suppl):C13–8.
Virmani R, Kolodgie FD, Burke AP, Finn AV, Gold HK, Tulenko TN, et al. Atherosclerotic plaque progression and vulnerability to rupture: angiogenesis as a source of intraplaque hemorrhage. Arterioscler Thromb Vasc Biol. 2005;25(10):2054–61.
Patel MB, Bui LP, Kirkeeide RL, Gould KL. Imaging microvascular dysfunction and mechanisms for female–male differences in CAD. J Am Coll Cardiol Img. 2016;9(4):465–82. Recently published in an issue dedicated to imaging ischemic heart disease in women, this excellent review highlights how sex differences in fluid dynamics and endothelial shear stress contribute to the development of atherosclerosis and microvascular dysfunction in women.
Iqbal SN, Feit F, Mancini GB, Wood D, Patel R, Pena-Sing I, et al. Characteristics of plaque disruption by intravascular ultrasound in women presenting with myocardial infarction without obstructive coronary artery disease. Am Heart J. 2014;167(5):715–22.
Reynolds HR, Srichai MB, Iqbal SN, Slater JN, Mancini GB, Feit F, et al. Mechanisms of myocardial infarction in women without angiographically obstructive coronary artery disease. Circulation. 2011;124(13):1414–25.
Khuddus MA, Pepine CJ, Handberg EM, Bairey Merz CN, Sopko G, Bavry AA, et al. An intravascular ultrasound analysis in women experiencing chest pain in the absence of obstructive coronary artery disease: a substudy from the National Heart, Lung and Blood Institute-Sponsored Women’s Ischemia Syndrome Evaluation (WISE). J Interv Cardiol. 2010;23(6):511–9.
Lansky AJ, Ng VG, Maehara A, Weisz G, Lerman A, Mintz GS, et al. Gender and the extent of coronary atherosclerosis, plaque composition, and clinical outcomes in acute coronary syndromes. JACC Cardiovasc Imaging. 2012;5(3 Suppl):S62–72.
Keller KB, Lemberg L. Prinzmetal’s angina. Am J Crit Care. 2004;13(4):350–4.
Kemp Jr HG. Left ventricular function in patients with the anginal syndrome and normal coronary arteriograms. Am J Cardiol. 1973;32(3):375–6.
Agrawal S, Mehta PK, Bairey Merz CN. Cardiac syndrome X: update 2014. Cardiol Clin. 2014;32(3):463–78.
Humphries KH, Pu A, Gao M, Carere RG, Pilote L. Angina with “normal” coronary arteries: sex differences in outcomes. Am Heart J. 2008;155(2):375–81.
Lønnebakken MT, Staal EM, Nordrehaug JE, Gerdts E. Usefulness of contrast echocardiography for predicting the severity of angiographic coronary disease in non-ST-elevation myocardial infarction. Am J Cardiol. 2011;107(9):1262–7.
Wei J, Mehta PK, Johnson BD, Samuels B, Kar S, Anderson RD, et al. Safety of coronary reactivity testing in women with no obstructive coronary artery disease: results from the NHLBI-sponsored WISE (Women’s Ischemia Syndrome Evaluation) study. JACC Cardiovasc Interv. 2012;5(6):646–53.
Murthy VL, Naya M, Taqueti VR, Foster CR, Gaber M, Hainer J, et al. Effects of sex on coronary microvascular dysfunction and cardiac outcomes. Circulation. 2014;129(24):2518–27.
Michelsen MM, Mygind ND, Pena A, Aziz A, Frestad D, Høst N, et al. Peripheral reactive hyperemia index and coronary microvascular function in women with no obstructive CAD, The iPOWER Study. J Am Coll Cardiol Img. 2016;9(4):411–7.
Marinescu MA, Löffler AI, Ouellette M, Smith L, Kramer CM, Bourque JM. Coronary microvascular dysfunction, microvascular angina, and treatment strategies. JACC Cardiovasc Imaging. 2015;8(2):210–20.
Löffler AI, Bourque JM. Coronary microvascular dysfunction, microvascular angina, and management. Curr Cardiol Rep. 2016;18(1):1.
Bairey Merz CN, Handberg EM, Shufelt CL, Mehta PK, Minissian MB, Wei J, et al. A randomized, placebo-controlled trial of late Na current inhibition (ranolazine) in coronary microvascular dysfunction (CMD): impact on angina and myocardial perfusion reserve. Eur Heart J. 2015;27.
Park SJ, Park JJ, Choi DJ, Chun EJ, Choi SI, Kim SM, et al. Understanding of chest pain in microvascular disease proved by cardiac magnetic resonance image (UMPIRE): study protocol for a randomized controlled trial. Trials. 2014;15:333.
Wittstein IS, Thiemann DR, Lima JA, Baughman KL, Schulman SP, Gerstenblith G, et al. Neurohumoral features of myocardial stunning due to sudden emotional stress. N Engl J Med. 2005;352(6):539–48.
Redfors B, Vedad R, Angerås O, Råmunddal T, Petursson P, Haraldsson I, et al. Mortality in takotsubo syndrome is similar to mortality in myocardial infarction—a report from the SWEDEHEART registry. Int J Cardiol. 2015;185:282–9.
Templin C, Ghadri JR, Diekmann J, Napp LC, Bataiosu DR, Jaguszewski M, et al. Clinical features and outcomes of takotsubo (Stress) cardiomyopathy. N Engl J Med. 2015;373(10):929–38.
Yerasi C, Koifman E, Weissman G, Wang Z, Torguson R, Gai J, et al. Impact of triggering event in outcomes of stress-induced (Takotsubo) cardiomyopathy. Eur Heart J Acute Cardiovasc Care. 2016.
Pelliccia F, Parodi G, Greco C, Antoniucci D, Brenner R, Bossone E, et al. Comorbidities frequency in Takotsubo syndrome: an international collaborative systematic review including 1109 patients. Am J Med. 2015;128(6), 654.e11-9.
Redfors B, Shao Y, Ali A, Omerovic E. Current hypotheses regarding the pathophysiology behind the takotsubo syndrome. Int J Cardiol. 2014;177(3):771–9.
Tweet MS, Gulati R, Hayes SN. What clinicians should know about spontaneous coronary artery dissection. Mayo Clin Proc. 2015;90(8):1125–30.
Saw J, Poulter R, Fung A. Intracoronary imaging of coronary fibromuscular dysplasia with OCT and IVUS. Catheter Cardiovasc Interv. 2013;82(7):E879–83.
Cade JR, Szarf G, de Siqueira ME, Chaves Á, Andréa JC, Figueira HR, et al. Pregnancy-associated spontaneous coronary artery dissection: insights from a case series of 13 patients. Eur Heart J Cardiovasc Imaging. 2016.
Nussinovitch U, Shoenfeld Y. Atherosclerosis and macrovascular involvement in systemic sclerosis: myth or reality. Autoimmun Rev. 2011;10(5):259–66.
Ishimori ML, Martin R, Berman DS, Goykhman P, Shaw LJ, Shufelt C, et al. Myocardial ischemia in the absence of obstructive coronary artery disease in systemic lupus erythematosus. JACC Cardiovasc Imaging. 2011;4(1):27–33.
Kakuta K, Dohi K, Sato Y, Yamanaka T, Kawamura M, Ogura T, et al. Chronic inflammatory disease is an independent risk factor for coronary flow velocity reserve impairment unrelated to the processes of coronary artery calcium deposition. J Am Soc Echocardiogr. 2016;29(2):173–80.
Hung MY, Tsimikas S. What is the ultimate test that lowering lipoprotein(a) is beneficial for cardiovascular disease and aortic stenosis? Curr Opin Lipidol. 2014;25(6):423–30.
Fraley AE, Tsimikas S. Clinical applications of circulating oxidized low-density lipoprotein biomarkers in cardiovascular disease. Curr Opin Lipidol. 2006;17(5):502–9.
Wiegman A, Gidding SS, Watts GF, Chapman MJ, Ginsberg HN, Cuchel M, et al. Familial hypercholesterolaemia in children and adolescents: gaining decades of life by optimizing detection and treatment. Eur Heart J. 2015;36(36):2425–37.
Shibata T, Kawakami S, Noguchi T, Tanaka T, Asaumi Y, Kanaya T, et al. Prevalence, clinical features, and prognosis of acute myocardial infarction attributable to coronary artery embolism. Circulation. 2015;132(4):241–50.
Pasupathy S, Air T, Dreyer RP, Tavella R, Beltrame JF. Systematic review of patients presenting with suspected myocardial infarction and nonobstructive coronary arteries. Circulation. 2015;131(10):861–70.
Tornvall P, Gerbaud E, Behaghel A, Chopard R, Collste O, Laraudogoitia E, et al. Myocarditis or “true” infarction by cardiac magnetic resonance in patients with a clinical diagnosis of myocardial infarction without obstructive coronary disease: a meta-analysis of individual patient data. Atherosclerosis. 2015;241(1):87–91.
Fabris E, Kilic ID, Caiazzo G, Serdoz R, Foin N, Sinagra G, et al. Nonatherosclerotic coronary artery narrowing. JACC Cardiovasc Imaging. 2016;9(3):317–20.
Taylor AJ, Byers JP, Cheitlin MD, Virmani R. Anomalous right or left coronary artery from the contralateral coronary sinus: “high-risk” abnormalities in the initial coronary artery course and heterogeneous clinical outcomes. Am Heart J. 1997;133:428–35.
Angelini P. Coronary artery anomalies: an entity in search of an identity. Circulation. 2007;115(10):1296–305.
Johnson PM, Patel J, Yeung M, Kaul P. Intra-coronary imaging modalities. Curr Treat Options Cardiovasc Med. 2014;16(5):304.
Groves EM, Seto AH, Kern MJ. Invasive testing for coronary artery disease: FFR, IVUS, OCT, NIRS. Heart Fail Clin. 2016;12(1):83–95.
Puri R, Nicholls SJ, Nissen SE, Brennan DM, Andrews J, Liew GY, et al. Coronary endothelium-dependent vasoreactivity and atheroma volume in subjects with stable, minimal angiographic disease versus non-ST-segment-elevation myocardial infarction: an intravascular ultrasound study. Circ Cardiovasc Imaging. 2013;6(5):674–82.
Nicholls SJ, Wolski K, Sipahi I, Schoenhagen P, Crowe T, Kapadia SR, et al. Rate of progression of coronary atherosclerotic plaque in women. J Am Coll Cardiol. 2007;49(14):1546–51.
Bharadwaj AS, Vengrenyuk Y, Yoshimura T, Baber U, Hasan C, Narula J, et al. Multimodality intravascular imaging to evaluate sex differences in plaque morphology in stable CAD. J Am Coll Cardiol Img. 2016;9(4):400–7.
Nicholls SJ, Hsu A, Wolski K, Hu B, Bayturan O, Lavoie A, et al. Intravascular ultrasound-derived measures of coronary atherosclerotic plaque burden and clinical outcome. J Am Coll Cardiol. 2010;55(21):2399–407.
Bogale N, Lempereur M, Sheikh I, Wood D, Saw J, Fung A. Optical coherence tomography (OCT) evaluation of intermediate coronary lesions in patients with NSTEMI. Cardiovasc Revasc Med. 2015.
Prati F, Uemura S, Souteyrand G, Virmani R, Motreff P, Di Vito L, et al. OCT-based diagnosis and management of STEMI associated with intact fibrous cap. JACC Cardiovasc Imaging. 2013;6:283–7.
Kanwar SS, Stone GW, Singh M, Virmani R, Olin J, Akasaka T, Narula J. Acute coronary syndromes without coronary plaque rupture. Nat Rev Cardiol. 2016.
Shufelt CL, Thomson LE, Goykhman P, Agarwal M, Mehta PK, Sedlak T, et al. Cardiac magnetic resonance imaging myocardial perfusion reserve index assessment in women with microvascular coronary dysfunction and reference controls. Cardiovasc Diagn Ther. 2013;3(3):153–60.
Thomson LE, Wei J, Agarwal M, Haft-Baradaran A, Shufelt C, Mehta PK, et al. Cardiac magnetic resonance myocardial perfusion reserve index is reduced in women with coronary microvascular dysfunction. A National Heart, Lung, and Blood Institute-sponsored study from the Women’s Ischemia Syndrome Evaluation. Circ Cardiovasc Imaging. 2015;8(4). This original study showed that noninvasive measurement of myocardial perfusion reserve index by cardiac magnetic resonance imaging can detect coronary microvascular dysfunction.
Esteves FP, Travin MI. The role of nuclear cardiology in the diagnosis and risk stratification of women with ischemic heart disease. Semin Nucl Med. 2014;44(6):423–38.
Kuruvilla S, Kramer CM. Coronary microvascular dysfunction in women: an overview of diagnostic strategies. Expert Rev Cardiovasc Ther. 2013;11(11):1515–25.
Rinkevich D, Belcik T, Gupta NC, Cannard E, Alkayed NJ, Kaul S. Coronary autoregulation is abnormal in syndrome X: insights using myocardial contrast echocardiography. J Am Soc Echocardiogr. 2013;26(3):290–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Joanna M. Joly and Vera Bittner declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Management of Acute Coronary Syndromes
Glossary of Terms
- ACS
-
Acute coronary syndrome
- CABG
-
Coronary artery bypass grafting
- CCTA
-
Coronary computed tomography angiography
- CFR
-
Coronary flow reserve
- CFVR
-
Coronary flow velocity reserve
- CMD
-
Coronary microvascular dysfunction
- CMR
-
Cardiac magnetic resonance
- CRT
-
Coronary reactivity testing
- CSX
-
Cardiac syndrome X
- IVUS
-
Intravascular ultrasound
- Lp(a)
-
Lipoprotein(a)
- MI
-
Myocardial infarction
- MPI
-
Myocardial perfusion imaging
- MPRI
-
Myocardial perfusion reserve index
- NSTEMI
-
Non-ST elevation myocardial infarction
- OCT
-
Optical coherence tomography
- PCI
-
Percutaneous coronary intervention
- PET
-
Positron emission tomography
- QCA
-
Quantitative coronary analysis
- RA
-
Rheumatoid arthritis
- RHI
-
Reactive hyperemia index
- SCAD
-
Spontaneous coronary artery dissection
- SLE
-
Systemic lupus erythematosus
- SPECT
-
Single-photon emission computed tomography
- SS
-
Systemic sclerosis
- STEMI
-
ST elevation myocardial infarction
- UA
-
Unstable angina
Rights and permissions
About this article
Cite this article
Joly, J.M., Bittner, V. Advanced Imaging and Diagnostic Methods in the Assessment of Suspected Ischemic Heart Disease in Women. Curr Cardiol Rep 18, 84 (2016). https://doi.org/10.1007/s11886-016-0767-0
Published:
DOI: https://doi.org/10.1007/s11886-016-0767-0