Abstract
Lower urinary tract symptoms (LUTS) in men are due to bladder dysfunction or bladder outlet disorders such as benign prostatic enlargement and bladder neck or urethral sphincter dysfunction. Men with lower urinary tract symptoms prefer shared problem-solving and decision making during treatment planning. Urodynamic studies (UDS) in male LUTS (MLUTS) are useful for both diagnosis and prognosis. UDS help both the clinician and the patient in shared decision making regarding treatment of these men. The AUA/SUFU guidelines and EAU guidelines are helpful in cost-effective selection of patients with MLUTS for urodynamic evaluation. UDS are indicated in the subset of patients with MLUTS being considered for invasive and potentially morbid therapy. Uroflowmetry and post-void residual (PVR) volume measurement by bladder ultrasound scan are good screening tests in MLUTS. Urodynamic evidence of bladder outlet obstruction has been correlated with better outcomes following invasive therapy.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Lower urinary tract symptoms (LUTS) encompass abnormalities in urinary storage, emptying, and sometimes with post micturition symptoms. The term male LUTS (MLUTS) have varied etiological factors and typically include frequency, urgency, nocturia, as well as hesitancy, weak stream, and subjective sensation of incomplete emptying in a male aged over 50 years. MLUTS may be due to bladder dysfunction or bladder outlet disorders, the latter including benign prostatic enlargement (BPE) and dysfunction of bladder neck, urethral sphincter, or pelvic floor. A significant variation in the management of patients with MLUTS has been documented [1].
Although benign prostatic enlargement causing bladder outlet obstruction is one of the common conditions resulting in MLUTS, there is no correlation among patient symptoms, size of the prostate, and bladder outlet obstruction documented by urodynamic studies (UDS), indicating other causes for MLUTS (non-BPH MLUTS). The condition of MLUTS excludes men with neurogenic lower urinary tract conditions, genitourinary malignancy, UTI’s, genitourinary trauma, radiation injury to the lower urinary tract (LUT), or LUTS following pelvic or LUT surgery. Patients with non-BPH MLUTS may not always have bladder outlet obstruction on UDS. Patient bother plays a significant role in selecting such patients for further evaluation and management. In this article, we focus on the role of UDS in the contemporary evaluation and management of MLUTS. Pressure flow studies (PFSs) are also helpful to assess treatment outcomes.
Significance of Urodynamics in MLUTS
UDS helps both the clinician and the patient in shared decision making on treatment and is useful to monitor the effectiveness of treatment. UDS will facilitate early identification and treatment of adverse lower urinary tract features, thereby reducing or avoiding further morbidity, improve quality of life, and occasionally slowing disease progression. The UDS also helps to predict outcomes of conservative or active treatments and can help to minimize treatment failures.
The American Urological Association (AUA)/SUFU (Society of Urodynamics, Female Pelvic Mecidine and Urogenital Reconstruction) have published guidelines on the role of UDS in the evaluation of MLUTS [3••, 4•, 5•]. The 6th International Consultation on Urologic Diseases (ICUD) consensus (2005) and the 6th International Consultation on New Developments in Prostate Cancer & Prostate Diseases (2005) [6] provide clinically useful guidelines on the role of UDS in MLUTS and their place in the diagnostic algorithm and treatment of men with LUTS.
The AUA/SUFU Guidelines on Urodynamics in Adults [5•] suggest uroflowmetry for the initial diagnosis and ongoing management of MLUTS (grade C level of evidence). Multichannel filling cystometry does not have much evidence but can identify detrusor overactivity (DO) or poor compliance when invasive/irreversible treatments are being considered (expert opinion). The AUA/SUFU panel recommends pressure flow studies as standard (grade B evidence) when diagnosis of obstruction is important, e.g., while considering invasive therapy based on the observation that PFS-confirmed obstruction as a predictor of improved treatment outcomes. The urodynamic study should be discussed with the patient regarding benefits, shortcomings, and possible complications.
According to the AUA, guidelines on the Management of Benign Prostatic Hyperplasia (BPH) were initially presented in 1994 (updated in 2010) [4•], UDS is optional in those without clear cut obstructive symptoms and in whom minimally invasive or invasive treatments are considered. The European Association of Urology (EAU) published guidelines (“Assessment, Therapy and Follow-Up of Men with Lower Urinary Tract Symptoms Suggestive of Benign Prostatic Obstruction” (BPH Guidelines)] and updated in 2013 (“EAU Guidelines on the Treatment and Follow-up of Non-neurogenic Male Lower Urinary Tract Symptoms Including Benign Prostatic Obstruction”) [7•]. The EAU document is a symptom- and treatment-based approach without specific guidelines on the workup of patients with MLUTS.
Pressure flow studies (PFSs) are recommended if the initial evaluation, uroflow rate (>10 ml/s), and post void residual urine volume are not suggestive of bladder outlet obstruction as these may suggest non-obstructive etiological factors for MLUTS. UDS in this population plays a crucial role as bladder outlet procedures are less likely to benefit this patient subset. The PFSs are extremely important if invasive treatment is being considered and in those patients continuing to have LUTS following prior surgery [8].
Indications for Urodynamic Study
Useful patient populations where UDS are helpful in treatment decisions include patients with persistent LUTS following prior invasive treatment, younger patients with urinary retention [16], patients whose symptoms do not correlate with uroflowmetry, and/or post-void residual (PVR) urine volume, patients whose LUTS cause suspicion of neurologic cause for voiding dysfunction and those with confounding conditions that could potentially affect bladder function (diabetes mellitus, previous radiation or pelvic surgery, and previous spine surgery), patients with MLUTS and incontinence [9].
Urodynamic Evaluation of MLUTS
UDS should be performed after the basic evaluation (history, physical exam, digital rectal exam, urinalysis, PVR urine volume measurement, and/or renal ultrasound where indicated) and only after formulating the clinical questions to be answered. Reproduction of patients’ symptoms during UDS is crucial to define the pathophysiology of MLUTS, as the latter is essential for effective treatment of these patients. UDS become especially important when the treatment being considered is invasive, irreversible, and potentially morbid, or costly. UDS in MLUTS will facilitate identification of the specific condition(s) contributing to the patient’s symptoms. Clinician supervision during UDS ensures the study reproduces the patient’s symptoms [10••].
Per AUA guidelines, PVR volume measurement is useful in patients with LUTS to rule out significant urinary retention both initially and during follow up (Clinical Principle) [5•]. Uroflowmetry is useful for the initial and ongoing evaluation of MLUTS when an abnormality of voiding/emptying is suspected (evidence strength: Grade C) [5•]. Uroflowmetry by itself cannot distinguish underactive detrusor from bladder outlet obstruction. Some patients may have both [11]. In addition, a normal uroflow pattern does not always exclude bladder outlet obstruction.
Multichannel invasive urodynamic evaluation encompasses cystometry, pressure flow studies (PFSs), sphincter electromyography (EMG), urethral pressure profilometry (UPP), and video urodynamic study (VUDS). Invasive UDS testing usually involves the use of a double- or triple-lumen urethral catheter. The abdominal pressure sensor (e.g., rectal catheter) provides a measurement of abdominal pressure. The detrusor pressure is a subtracted value obtained by subtracting intra-abdominal pressure from the intravesical pressure.
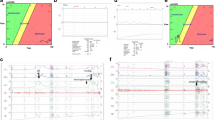
Cystometrogram (CMG) is the assessment of storage phase of the LUT function and includes bladder sensations, bladder capacity, and measurement of vesical or detrusor pressures during bladder filling. Involuntary detrusor contractions or detrusor overactivity (DO) and decreased detrusor compliance are documented during CMG (Fig. 1). As both these features could potentially affect treatment decision, it is important to correlate these features with patient-reported symptoms of urgency and/or urgency incontinence. DO occurs in over 50 % of men with BPH, and the prevalence of DO on PFSs has been shown to increase with increasing grades of obstruction to over 80 % in those with Schafer grade V obstruction [12]. Cystometric bladder capacity may be correlated with functional bladder capacity noted on frequency-volume charts.
Fifty-two-year-old male with increased urinary frequency, urgency, nocturia, weak urinary stream, incomplete bladder emptying, and straining on urination. Urodynamic study showing phasic detrusor overactivity during filling phase and normal pressure and low flow pattern during the voiding phase. Digital rectal exam revealing 20 g prostate
The parameters noted on UDS are very helpful in preoperative patient counseling. Decreased sensations and large capacity on preoperative UDS may suggest possible incomplete bladder emptying after bladder outlet procedures, whereas increased bladder sensations and decreased detrusor compliance may result in persistence of storage LUTS of frequency and urgency. Involuntary leak during UDS for MLUTS in a patient considering invasive treatment is a potential risk factor for persistence or sometimes worsening of this symptom after the bladder outlet procedure and such patients should be appropriately counseled. Detrusor contractility can be categorized as acontractile, underactive (Fig. 2), or normal [13]. An underactive detrusor can be differentiated from bladder outlet obstruction by PFSs as the latter measure detrusor pressure simultaneously with voiding, with a high pressure/low flow pattern typically confirming bladder outlet obstruction.
A 62-year-old man with diabetes mellitus, AUA symptom index 22. Weak urinary stream, on tamsulosin, digital rectal exam (DRE) 25 g prostate, maximum urinary flow rate on uroflowmetry, 9.5 ml/s, PVR 300 ml, voiding phase of the urodynamic study showing underactive detrusor with prominent abdominal straining
Absolute detrusor pressure cutoffs are not uniformly helpful to define bladder outlet obstruction [13]. Bladder contractility index is the objective quantification of detrusor contractility and is calculated as pdetQmax + 5Qmax. Contractility is grade as strong (BCI, ≥150), normal (BCI, 100–150), or weak (BCI, ≤100).
Abdominal straining during voiding phase of the PFSs may be correlated with hesitancy. Some patients may find it difficult to empty the bladder with the urodynamic catheter in situ. Recording of detrusor pressure during attempted voiding by such patients with or without fluoroscopy (the latter to assess the level of obstruction) may be helpful in this subset of patients with MLUTS.
Assessment of Bladder Outlet Obstruction
Various nomograms and formulas are used for bladder outlet obstruction including the ICS nomogram, Abrams-Griffiths Nomogram, and Schafer Nomogram [14]. Bladder outlet obstruction index (BOOI) also is useful to quantify bladder outlet obstruction and is calculated as pdetQmax – 2Qmax. A BOOI ≥40 indicates obstruction and an index ≤20 indicates no obstruction, with 20–40 suggesting an equivocal obstruction. Noninvasive techniques for making the diagnosis of obstruction are not accurate and not clinically useful [15••].
Detrusor sphincter dyssynergia or sphincter bradykinesia may be noted on sphincter EMG or fluoroscopy (on VUDS) and such patients need neurological assessment. LUTS in young males with dysfunctional voiding may be noted to have pseudo dyssynergia on EMG or fluoroscopy suggesting pelvic floor dysfunction as the cause of their LUTS.
VUDS is accomplished by radiologic imaging of the lower urinary tract during PFSs and is useful to document the anatomic location of the obstruction as bladder neck (primary bladder neck obstruction), in the prostatic urethra (BPH), in the membranous urethra (dysfunctional voiding), or anywhere along the urethra (urethral stricture). VUDS can also document vesicoureteral reflux and other anatomic abnormalities such as bladder diverticula or bladder stones.
Risks and Complications of Urodynamic Evaluation
UDS is a low-risk evaluation with good tolerability [16, 17]. Possible risks of UDS include patient discomfort, UTI, hematuria, and vasovagal syncope [18–20]. The AUA best practice recommends antimicrobial prophylaxis before UDS in patients with risk factors [21]. In those without risk factors, antimicrobial prophylaxis is not necessary if the pre procedural urine culture is sterile. A negative urinalysis, however, does not preclude the risk of post-procedural UTI. A Cochrane systematic review concluded that prophylactic antibiotics reduce bacteriuria after urodynamic studies but not symptomatic urinary tract infections [21].
When and How to Use Urodynamic Studies in Male LUTS?
In the current era of patient-centered health care delivery, it is important to take into consideration the patient’s goals for treatment and arrive at a reasonable diagnosis of the patient with MLUTS prior to formulating an effective treatment plan. UDS is a useful tool in this direction. Treatment strategies should be critically evaluated based on patient-reported outcomes and the patient’s perception of success. UDS is often used in the work up of MLUTS. Subjective improvement in LUTS and improvement in urodynamic parameters of bladder outlet obstruction (uroflow, detrusor voiding pressure, and post void residual volume) are used to gauge treatment success. Such yardsticks of treatment success enable us to compare contemporary treatment modalities for MLUTS. Urodynamic studies are helpful for patient counseling including treatment goals and anticipated outcomes.
Prediction of treatment success is of equal interest to patients, providers, and payers alike. Good correlation has been reported between urodynamic diagnoses and outcome of bladder outlet reduction procedures. Failure of bladder outlet procedures (e.g., transurethral resection of prostate) to improve MLUTS has been noted to be high in those without urodynamic evidence of bladder outlet reduction, those who had DO, and those who had detrusor underactivity. Tanaka et al. [22] noted 57 % of their MLUTS patient population had urodynamic evidence of obstruction, and these patients had better outcomes following transurethral resection of prostate (TURP), whereas the treatment was less efficacious in those without outlet obstruction but with DO. Machino and colleagues also reported poor outcomes in patients with equivocal obstruction coupled with DO [23]. Urodynamic evaluation can therefore help to avoid surgical failure in patients without documented outlet obstruction with possible DO. Van Venrooij et al. reported better symptom control in men with urodynamically documented outlet obstruction compared to unobstructed and equivocal men undergoing transurethral resection of the prostate [24]. Urodynamic parameters of outlet obstruction (Fig. 3) are helpful in setting treatment goals for symptom improvement in men choosing bladder outlet procedures.
A 69-year-old man with Parkinson’s disease, AUA symptom index 30 with weak urinary stream, subjective sensation of incomplete bladder emptying, increased daytime urinary frequency, nocturia, and urgency. Digital rectal exam revealed 35 g prostate. He is on tamsulosin and oxybutunin. Maximum urinary flow rate on complex Uroflowmetry, 6.5 ml/s. Pressure flow urodynamic study revealing high detrusor voiding pressure and low uroflow pattern with a postvoid residual volume of 250 ml indicating bladder outlet obstruction
Is Urodynamic Evaluation Cost Effective in MLUTS?
The costs for UDS evaluation should be weighed with overall cost of patient care. Cost benefits are achieved with accurate diagnosis, avoidance of inappropriate treatments, identifying those with non benign prostatic obstruction (BPO) MLUTS, avoidance of unnecessary medications/surgery, and detecting those with severe symptoms and proven outlet obstruction, as the latter benefit from early surgical intervention. The unequivocal surgical candidates may thus be counseled to avoid ineffective potentially long-term and costly medical therapy and inappropriate minimally invasive treatment options [25].
Conclusions
The outcomes for surgical outlet reduction are less than optimal for patients who do not demonstrate outlet obstruction on pressure flow urodynamic study. Urodynamics is an option to assess for any factors that influence treatment or patient counseling. By providing crucial parameters of lower urinary tract function, UDS are useful for an effective evaluation and management of men with LUTS and assist in the critical appraisal of contemporary treatments strategies in MLUTS. In the current era of shared decision making, they facilitate better patient counseling in more informed patients with care that meets treatment expectations and goals, especially in those considering potentially morbid invasive therapy. Pressure flow studies are therefore helpful to choose the surgical candidates likely to have better outcomes. VUDS are useful to identify the level of obstruction in younger men with LUTS. Large scale prospective studies encompassing urodynamic evaluation are becoming increasing significant in MLUTS due to the expanding treatment modalities in this patient population.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Wei JT, Calhoun E, Jacobsen SJ. Urologic diseases in America project: benign prostatic hyperplasia. J Urol. 2005;173(4):1256–61.
Andersson SO, Rashidkhani B, Karlberg L, et al. Prevalence of lower urinary tract symptoms in men aged 45–79 years: a population-based study of 40,000 Swedish men. Br J Urol. 2004;94(3):327–31.
Collins CW, Winters JC. AUA/SUFU Adult Urodynamics Guideline. A clinical review. Urol Clinics North Am. 2014;41:353–62. A total of 19 Guidelines Statements in each of the 4 lower urinary tract conditions were presented in this manuscript with each guideline statement discussed in the context of clinical cases.
McVary KT, Roehrborn CG, Avins AL, et al. Update on AUA guideline on the management of benign prostatic hyperplasia. J Urol. 2011;185(5):1793–803. The authors revised the 2003 version of the American Urological Association’s (AUA) Guideline on the management of benign prostatic hyperplasia (BPH) in this manuscript.
Winters JC, Dmochowski RR, Goldman HB, et al. Urodynamic studies in adults: AUA/SUFU guideline. J Urol. 2012;188 Suppl 6:2464–72. The manuscript is aimed to help the clinician in appropriate selection of urodynamic tests in common lower urinary tract symptoms following the basic clinical evaluation.
Abrams P, Chapple C, Khoury S, et al. Evaluation and treatment of lower urinary tract symptoms in older men. J Urol. 2009;181(4):1779–87.
Oelke M, Bachmann A, Descazeaud A, et al. EAU guidelines on the treatment and follow-up of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol. 2013;64(1):118–40. This is a summary of the 2013 edition of the European Association of Urology guidelines on the treatment and follow-up of male lower urinary tract symptoms.
McNicholas TA, Kirby RS, Lepor H. Evaluation and nonsurgical management of benign prostatic hyperplasia. In: Wein AJ, Kavoussi LR, Novick AC, et al., editors. Campbell-walsh urology. 10th ed. Philadelphia: Elsevier Saunders; 2012.
Thomas AW, Cannon A, Bartlett E, et al. The natural history of lower urinary tract dysfunction in men: minimum 10-year urodynamic follow-up of transurethral resection of prostate for bladder outlet obstruction. J Urol. 2005;174(5):1887–91.
Lenherr SM, Clemens JQ. Urodynamics: with a focus on appropriate indications. Urol Clin North Am. 2013;40(4):545–57. An excellent review on contemporary indications and techniques for adult urodynamic testing incorporating specific clinical questions and appropriate urodynamic studies addressing the questions along with a discussion on testing pitfalls and appropriate troubleshooting.
Chancellor M. Bladder outlet obstruction versus impaired detrusor contractility: the role of outflow. J Urol. 1991;145(4):810–2.
Oelke M, Baard J, Wijkstra H, et al. Age and bladder outlet obstruction are independently associated with detrusor overactivity in patients with benign prostatic hyperplasia. Eur Urol. 2008;54(2):419–26.
Abrams P, Cardozo L, Fall M, Standardisation Subcommittee of the International Continence Society, et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn. 2002;21:167–78.
Griffiths D, Hbfner K, Van Mastrigt R, et al. Standardization of terminology of lower urinary tract function: Pressure-flow studies of voiding, urethral resistance, and urethral obstruction. International Continence Society Subcommittee on Standardization of Terminology of Pressure-Flow Studies. Neurourol Urodyn. 1997;16:1–18.
Mehdizadeh JL, Leach GE. Role of invasive urodynamic testing in benign prostatic hyperplasia and male lower urinary tract symptoms. Urol Clin North Am. 2009;36(4):431–41. The manuscript addresses the controversy of the role of urodynamic studies in BPH/LUTS notwithstanding the additional information that urodynamic studies provide regarding bladder function and outlet obstruction. The authors discuss the role of urodynamic studies in BPH/LUTS, review best practice guidelines and current literature, and provide recommendations for their use in clinical practice.
Scarpero HM, Padmanabhan P, Xue X, et al. Patient perception of videourodynamic testing: a questionnaire based study. J Urol. 2005;173(2):555–9.
Ku JH, Kim SW, Kim HH, et al. Patient experience with a urodynamic study: a prospective study in 208 patients. J Urol. 2004;171(6):2307–10.
Liao L, Schaefer W. Within-session reproducibility and variability of urethral resistance and detrusor contractility in pressure-flow studies in men with lower urinary tract symptoms. Curr Urol. 2009;3(1):19–28.
Tammela TL, Schäfer W, Barrett DM, et al. Repeated pressure-flow studies in the evaluation of bladder outlet obstruction due to benign prostatic enlargement. Finasteride Urodynamics Study Group. Neurourol Urodyn. 1999;18(1):17–24.
Rosier PF, de la Rosette JJ, Koldewijn EL, et al. Variability of pressure-flow analysis parameters in repeated cystometry in patients with benign prostatic hyperplasia. J Urol. 1995;153(5):1520–5.
Foon R, Toozs-Hobson P, Latthe P. Prophylactic antibiotics to reduce the risk of urinary tract infections after urodynamic studies. Cochrane Datab Syst Rev. 2012;10:CD008224.
Tanaka Y, Masumori N, Itoh N, et al. Is the short-term outcome of transurethral resection of the prostate affected by preoperative degree of bladder outlet obstruction, status of detrusor contractility or detrusor overactivity? Int J Urol. 2006;13((11):1398–404.
Machino R, Kakizaki H, Ameda K, et al. Detrusor instability with equivocal obstruction: a predictor of unfavorable symptomatic outcomes after transurethral prostatectomy. Neurourol Urodyn. 2002;21(5):444–9.
Van Venrooij GE, van Melick HH, Boon TA. Comparison of outcomes of transurethral prostate resection in urodynamically obstructed versus selected urodynamically unobstructed or equivocal men. J Urol. 2003;62(4):672–6.
DiSantostefano R, Biddle A, Lavelle J. An evaluation of the economic costs and patient-related consequences of treatments for benign prostatic hyperplasia. Br J Urol. 2006;97:1007–16.
Compliance with Ethics Guidelines
Conflict of Interest
Hari S.G.R. Tunuguntla and Jaspreet Parihar declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Voiding Dysfunction Evaluation
Rights and permissions
About this article
Cite this article
Tunuguntla, H.S.G.R., Parihar, J. Urodynamics in Male Lower Urinary Tract Symptoms. Curr Bladder Dysfunct Rep 10, 125–131 (2015). https://doi.org/10.1007/s11884-015-0299-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11884-015-0299-2