Abstract
Since the advent of percutaneous coronary intervention, enormous advances have been made in the treatment of coronary artery disease. Angioplasty and bare metal stents were plagued by high rates of restenosis leading to repeat revascularization procedures. Examination of the underlying pathophysiology of restenosis led to the development of drug-eluting stents to reduce neointimal hyperplasia. However, as restenosis rates declined, length of dual antiplatelet therapy use and risk of long-term stent thrombosis associated with drug-eluting stents increased. Subsequent generations have improved each facet of stent design. Novel alloys maintain durability and reduce strut thickness to increase deliverability, biocompatible polymers decrease the inflammatory response and improve drug elution kinetics, and new generations of drugs predictably inhibit restenosis. Developments on the horizon include stents with bioabsorbable polymers and platforms. The purpose of this review is to assess the evolution of stent design and the evidence behind each generation and to peer into the future of stent technology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The advent of percutaneous coronary intervention (PCI) revolutionized the treatment of coronary artery disease and acute coronary syndrome. Since the first balloon angioplasty (PTCA) in 1977 and the first implantation of a coronary stent in 1984, PCI has consistently evolved over time with the introduction of new devices, techniques, and adjunctive pharmacotherapy.
The efficacy of PTCA was primarily limited by the high rate of restenosis, which occurred in as many as half of all revascularizations within the first year. Restenosis in the setting of PTCA was mediated by both elastic recoil, which led to acute closure in 5 to 10 % of patients, and subsequent proliferation of smooth muscle cells at the site of endothelial damage incurred by balloon inflations [1]. The first balloon-expandable Palmaz-Schatz stent, approved for use in coronary arteries by the US Food and Drug Administration in 1994, was designed to provide a scaffold that would increase the acute gain in lumen diameter compared with PTCA alone and, thereby, reduce the rate of clinically relevant restenosis following PCI.
While more effective than PTCA, bare metal stents (BMS) did not eliminate restenosis. Estimates on the restenosis rates following BMS placement varied, ranging from 11 to 40 %, with higher rates noted particularly in longer lesions and small-caliber vessels [2]. Both mechanical and biologic processes contributed to restenosis following BMS implantation. For example, experimental models demonstrated recruitment of inflammatory cells at the site of endothelial damage from balloon inflations, which led to subsequent neointimal hyperplasia and neovascularization. The acute stretch during stent deployment further exacerbated this process.
Over the following decade, various stent designs were developed to increase deliverability and durability and reduce the inflammatory reaction and neointimal hyperplasia post-stent implantation. Investigators hypothesized that antiproliferative drugs could be delivered locally via a polymer release mechanism in high enough concentrations to reduce neointimal hyperplasia but at a slow enough rate to avoid systemic toxicity. It was this insight that allowed creation of drug-eluting stents (DES), which became widely available for use in the USA in April 2003.
Drug-Eluting Stent Design
Each DES has three components—platform, polymer, and drug. Over the past decade, biomedical engineers periodically reexamined each component to improve on overall stent design and achieve the ideal characteristics of flexibility, trackability, radial strength, and biocompatibility (Table 1).
Stent Platform
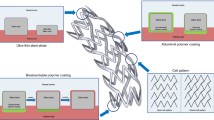
Stent platforms are tubular, trellis-like open frameworks with DES diameters ranging from 2.25 to 4.0 mm2 and lengths ranging from 8 to 38 mm. The open framework of stents led to a variety of cellular designs, including coils, mesh, and slotted tube. The tube design was considered superior due to smaller strut width and less gaps between struts, which increased radial strength and decreased plaque prolapse. The tube design was further improved with open versus closed cell patterns that, in turn, drove key stent selection factors. Open cell designs provided less metal surface area, greater conformability, and greater side branch access, while closed cell designs provided greater radial strength, more uniform drug concentration, and less plaque or tissue prolapse.
Other key factors that influenced stent platform design included number of struts, number of links connecting struts, and strut thickness, all of which positively correlated with rate of restenosis but increased radial strength. Finally, the materials used in stent platforms were chosen primarily based on their biocompatibility and thromboresistant properties, which influenced durability, another key factor in stent design.
Polymer
Prior to the introduction of DES, heparin-coated stents were evaluated in an attempt to help reduce restenosis rate, but multiple trials found no benefit with these compared to BMS [3, 4]. Since in-stent restenosis following BMS placement was mediated by neointimal hyperplasia and smooth muscle proliferation over time, simply adding an anticoagulant directly to the stent was an inadequate preventive mechanism. Not only did the drug need to be improved upon, but a polymer was also needed to encase the drug and permit modifications in release kinetics to ensure a steady local concentration after deployment. To be successful, polymers required two characteristics: predictable drug release over a targeted period of time and minimization of local inflammation [5].
Drug
In search of the ideal antiproliferative drug, three characteristics needed to be met: (1) wide therapeutic window, (2) lipophilic properties, and (3) long enough tissue retention time such that the endothelium could regrow after PCI-induced injury without a neointimal hyperplasia pattern. Two major classes of drugs were discovered and used to coat DES. One belongs to the rapamycin family (−“limus” drugs) and has an immunosuppressive mechanism of action. These macrolide antibiotics bind to the cytosolic FK-binding protein and inhibit the mammalian target of rapamycin (mTOR). mTOR inhibition upregulates p27, which, in turn, inhibits the CDK-cyclin complexes responsible for cell cycle progression from the gap 1 to the synthesis phase. The other, paclitaxel, has an antiproliferative mechanism of action and binds to the β-subunit of the tubulin heterodimer, which, in turn, inhibits the mitogen-activated protein kinase responsible for microtubule depolymerization. As a result, inappropriately stable microtubules are created, which inhibit spindle formation and mitosis.
First-Generation DES
The first generation of DES comprised of the Cypher sirolimus-eluting stent (SES) and the Taxus paclitaxel-eluting stent (PES) on a stainless steel platform with relatively thick struts (SES 140 μm, PES 132 μm). The polymer on SES eluted ~80 % of the drug in the first month, while the polymer on PES eluted ~10 % of the drug in the first 10 days and sequestered the rest indefinitely.
First-Generation DES Versus BMS
Initial studies demonstrated a significant reduction in lumen loss at 6 months with SES versus BMS, which translated into improvement in clinical outcomes in subsequent large randomized clinical trials (Table 2) [6, 7]. The Sirolimus-Eluting Stent in De-Novo Native Coronary Lesions (SIRIUS) trial randomized 1058 patients to either SES or BMS. At 9 months, the rate of target lesion revascularization (TLR) was significantly lower in the SES group (4.1 % SES vs. 16.6 % BMS, p < 0.001) [8]. This benefit extended out to 5 years, such that the SES group experienced a 14.8 % absolute reduction in TLR compared with BMS and similar rates of safety endpoints, including death, nonfatal myocardial infarction (MI), and stent thrombosis (ST) [9].
Studies evaluating PES versus BMS showed similar results. The Treatment of De Novo Coronary Disease Using a Single Paclitaxel Eluting Stent (TAXUS IV) study demonstrated significant reductions in ischemia-driven target vessel revascularization (TVR) with PES versus BMS at 9-month follow-up in 1314 randomized patients undergoing PCI (4.7 vs. 12.1 %, p < 0.001) [10]. This benefit also persisted 5 years post-randomization, with TVR rates of 16.9 % (PES) versus 27.4 % (BMS) (p < 0.001) and similar rates of death, MI, and ST [11].
Comparison of First-Generation DES
Few direct SES versus PES comparisons have been performed. The Sirolimus-Eluting Versus Paclitaxel-Eluting Stents for Coronary Revascularization (SIRTAX) trial randomized 1012 patients to either SES or PES and demonstrated a significantly lower rate of major adverse cardiovascular events (MACE) in the SES (6.2 %) versus PES (10.8 %) groups at 9-month follow-up, a difference that was driven primarily by TLR (4.8 vs. 8.3 %, p = 0.03) [12]. The larger Sirolimus- Versus Paclitaxel Eluting Stents in De Novo Coronary Artery Lesions (REALITY) and Scandinavian Organization on Randomized Trials with Clinical Outcome II (SORT OUT II) trials, however, demonstrated numerically lower, but not statistically significant, rates of clinical outcomes with SES versus PES at 1-year and 18-month follow-up, respectively [13, 14].
The introduction of DES radically disrupted PCI procedures. While the superiority of first-generation DES over BMS in the reduction of TVR was established, the delay in the endothelialization process raised concerns of increased risk of ST, a potentially catastrophic event [15, 16]. Syntheses of the available data demonstrated significant reductions in TLR and definite ST with SES versus PES in two different meta-analysis reports [17, 18]. Although mortality rates were not significantly different between SES and PES, there was a significant increase in very late ST and a trend towards higher risk of late MI with PES [17, 18]. While patient- and lesion-specific factors contributed to the increased risk of ST, additional DES-specific factors, including development of late malapposition, hypersensitivity to drug coating or polymer, and inflammatory response to strut thickness, were also described [19]. Furthermore, rates of TVR were significantly reduced with DES but remained clinically relevant. Together, these findings led to investigations into how to further improve on DES design [20].
Second-Generation DES
Growing data suggested a positive correlation between stent strut thickness and the reactive inflammatory process, which led to subsequent increased rates of restenosis and risk of the maladaptive remodeling that contributes to ST [21–23]. As such, second-generation stents took a rapamycin derivative, given the suggestion of superiority over paclitaxel, and encased it in a new more thromboresistant fluoropolymer on a platform made from the novel alloy cobalt chromium (CoCr). Compared to stainless steel, CoCr has less nickel and thinner stent struts, which decreased the local inflammatory response and increased radiopacity and conformability without sacrificing radial strength. This change in platform design led to the development of the Xience V and Promus everolimus-eluting stents (EES-CoCr, strut thickness 81 μm) and the Endeavor zotarolimus-eluting stent (E-ZES, strut thickness 91 μm).
Second-Generation DES: EES-CoCr
The Clinical Evaluation of XIENCE V Everolimus Eluting Coronary Stent System in the Treatment of Patients with De Novo Coronary Artery Lesions III (SPIRIT III) trial randomized 1002 patients to EES-CoCr versus PES and demonstrated a significant 43 % relative reduction in composite MACE at 9 months with EES-CoCr, primarily due to fewer MIs and TLR procedures [24]. These outcomes persisted to 3 years, suggesting improved long-term safety and efficacy [25]. The SPIRIT IV trial demonstrated similar results in more complex coronary lesions at 9-month and 2-year follow-up [26, 27].
However, it remained unclear whether it was the rapamycin derivative, the CoCr platform with thinner struts, or some combination of both which had a beneficial effect on outcomes. To further delineate the underlying mechanism of benefit with EES-CoCr, the Comparison of Everolimus Eluting XIENCE V Stent with Paclitaxel Eluting TAXUS LIBERTE Stent in All Comers (COMPARE) trial compared EES-CoCr with the newer Taxus Liberte PES, which remained on the original stainless steel platform but had strut thickness comparable to second-generation DES. This study demonstrated a reduced rate of the composite outcome of death, MI, and TVR with EES-CoCr compared to Taxus Liberte PES (6 vs. 9 %, p = 0.02) at 1-year follow-up [28]. The benefit with EES-CoCr was maintained at 2-year follow-up despite a significantly lower percentage of dual antiplatelet therapy use in the EES-CoCr group and suggested, again, the superiority of rapamycin derivatives over paclitaxel [29].
The SORT OUT IV trial compared rapamycin derivatives on the second-generation CoCr versus first-generation stainless steel platforms, EES-CoCr versus SES. Although EES-CoCr was noninferior to SES on the primary composite endpoint of cardiac death, MI, definite ST, and TVR at both 9 months and 2 years, EES-CoCr was associated with a lower rate of definite ST at 2 years [30, 31•]. The Randomized Evaluation of Sirolimus Eluting Versus Everolimus Eluting Stent (RESET) trial demonstrated similar noninferiority of EES-CoCr to SES on TLR at 1 year, while a propensity score-matched analysis demonstrated significant reductions in MI, TVR, and definite ST with EES-CoCr compared to SES on median follow-up of 1.5 years [32, 33•]. A meta-analysis of trials comparing EES-CoCr versus SES, however, showed no significant difference in MACE or composite of definite and probable ST on median follow-up of 13 months [34]. Although, the difference between EES-CoCr and SES was not apparent on short-term follow-up, 3-year follow-up in the SORT OUT IV and the recently published Randomized Comparison of Everolimus Eluting Stents and Sirolimus Eluting Stent in Patients with ST Elevation MI (RACES-MI) trials demonstrated no significant difference in MACE but significant reductions in overall and very late definite ST [35, 36•].
Second-Generation DES: E-ZES
Polymer characteristics impact both stent restenosis and thrombosis. Releasing drug over too short a period may reduce the time needed to be on dual antiplatelet therapy but lead to an increased rate of restenosis, while longer elution times delay endothelialization but potentially increase the rate of long-term ST. E-ZES differed primarily from EES-CoCr in their polymer drug elution properties, such that the biopolymer in E-ZES was designed to rapidly elute 95 % of the drug over the first 2 weeks. EES-CoCr fluoropolymers, on the other hand, released 80 % of the drug in the first 30 days, similar to first-generation SES.
This change in drug elution properties did not translate into clinical benefit. The Randomized Trial to Evaluate the Safety and Efficacy of the Medtronic Drug Eluting Coronary Stent System Versus the Cypher Sirolimus Eluting Coronary Stent System in De Novo Coronary Artery Lesions (ENDEAVOR III) trial demonstrated significantly higher rates of in-segment late lumen loss at 8 months angiographic follow-up with E-ZES versus SES [37]. Although there was a lower rate of MACE with E-ZES, this was primarily driven by a lower rate of peri-procedural MI, a controversial endpoint [38]. At 3-year follow-up, there was no significant difference between rates of all TVR but a significantly higher rate of TVR with coronary artery bypass graft surgery in the E-ZES compared to the SES group [39]. In addition, the SORT OUT III trial demonstrated a higher rate of the composite outcome of cardiac death, MI, and TVR at 3-year follow-up in patients randomized to E-ZES versus SES (12.9 vs. 10.1 %, p = 0.022), despite a higher rate of very late ST in the SES group (0 % ZES vs. 1.1 % SES, p = 0.0005) [40].
Newer Second-Generation DES
Newer second-generation DES reflected a culmination of prior data that demonstrated the superiority of rapamycin derivative drugs over paclitaxel, the CoCr platform with its thinner struts over the stainless steel platform, and biocompatible fluoropolymers that elute the majority of drug over 1 to 2 months. Further modifications in design were made to allow for greater flexibility and technical deliverability in complex lesions. These changes led to the introduction of (1) the Xience Prime EES on the same CoCr platform but with wider U-shaped connecting links, (2) the Promus Element EES on a platinum chromium (PtCr) platform (EES-PtCr), and (3) the Resolute ZES (R-ZES) with a new biocompatible polymer that eluted drug at a rate similar to EES.
Newer Second-Generation DES: EES-CoCr and EES-PtCr
The newer PtCr platform was designed to increase deliverability, and the Prospective Randomized Evaluation of a Novel Everolimus Eluting Coronary Stent (PLATINUM) trial demonstrated noninferiority of EES-PtCr to EES-CoCr in target vessel-related cardiac death, target vessel-related MI, and ischemia-driven TLR at 1 year [41]. However, over time, several case reports emerged suggesting longitudinal stent deformation after deployment of EES-PtCr, which may be explained by stent platform design [42]. While the original SES had a rigid scaffold with six connectors and the Xience EES-CoCr platform had a multi-link geometry with three connectors per ring, the Promus Element EES-PtCr platform was comprised of a helical design with two connectors per ring. Stents with fewer connectors have greater flexibility and deliverability; however, this comes at the expense of longitudinal stability and strength [43]. Furthermore, the peaks of the helical design line up with the valleys of the neighboring ring, such that longitudinal compression force on the stent rings may cause them to nest and “shorten.” Reduced longitudinal integrity has been well described as a risk for intraprocedural stent deformation and, thus, possible ST, particularly in ostial and bifurcation lesions [44, 45].
Both the Xience Prime EES-CoCr and Promus Element EES-PtCr stents made minor changes, resulting in the currently used Xience Xpedition EES-CoCr and Promus Premiere EES-PtCr. Xience Xpedition EES-CoCr did not modify the stent design but rather the stent delivery system with a smoother transition at the balloon/stent interface and a thinner multi-layer delivery balloon. The Promus Premier EES-PtCr, on the other hand, modified its platform with the addition of more connectors in the proximal two segments of the stent to increase axial strength.
Newer Second-Generation DES: R-ZES
Similar to the Promus Element EES-PtCr, R-ZES is comprised of a helical design with two connectors per ring. However, the peaks of the helical design in R-ZES line up with the peaks of the neighboring ring, potentially providing greater longitudinal stability and strength than the original Promus Element EES-PtCr. In addition, with similar drug elution properties as EES polymers, R-ZES demonstrated significantly lower in-stent late lumen loss on 6- to 8-month angiographic follow-up and a trend towards a lower rate of TLR at 2-year follow-up compared to E-ZES [46•]. It is not surprising that subsequent comparisons were primarily made between R-ZES and newer second-generation EES.
Multiple large trials demonstrated no significant differences between R-ZES and EES-CoCr [47•]. The Randomized Controlled Trial in Second Generation Zotarolimus Resolute Stents versus Everolimus Xience V stents in Real World Patients (TWENTE) trial randomized patients with acute coronary syndromes or stable angina, the majority of which had complex coronary lesions, to R-ZES or EES-CoCr and found no significant difference in the primary composite endpoint of cardiac death, MI, and clinically indicated TVR [48•]. The Randomized Comparison of a Zotarolimus Eluting Stent with an Everolimus Eluting Stent for Percutaneous Coronary Intervention All-Comers (RESOLUTE AC) trial also showed no difference in the primary composite endpoint of cardiac death, target vessel MI, and clinically indicated TLR or overall ST at 1-year follow-up [49]. However, there was a significantly higher rate of definite ST with R-ZES compared to EES-CoCr (1.2 vs. 0.3 %, p = 0.01).
In the only randomized R-ZES versus EES-PtCr comparison, The Third Generation Zotarolimus Eluting and Everolimus Eluting Stents in All Comer Patients Requiring Percutaneous Coronary Intervention (DUTCH PEERS) trial, there was no significant difference in the composite of cardiac death, target vessel-related MI, and TVR or rate of definite ST over the 12-month follow-up [50•]. While more patients in the EES-PtCr group experienced longitudinal stent deformation (R-ZES 0 vs. EES-PtCr 9 patients, p = 0.002), these were not associated with any adverse clinical events.
Synthesis of Data on Currently Approved DES
The large number of trials performed to date can create some confusion with regard to optimal stent choice. While guidelines do not specify a specific stent as first-line choice, a comprehensive network meta-analysis of more than 50,000 patients in 49 randomized controlled trials demonstrated significantly lower odds of definite ST at 1-year follow-up with EES-CoCr when compared to BMS, SES, PES, E-ZES, and R-ZES [51•]. The report also demonstrated lower odds of ST at 2-year follow-up with EES-CoCr than BMS and PES. A subsequent meta-analysis demonstrated similar results in patients presenting with ST segment elevation MI [52]. A mixed treatment comparison of both short- and long-term outcomes further added to the body of data that demonstrated newer second-generation DES to perform extremely well, with a slight favor towards EER-CoCr [53•]. In the short term (~1 year), SES, EES-CoCr, and R-ZES had similar efficacy with a lower rate of TVR relative to BMS, PES, and E-ZES. EES-CoCr was also associated with the lowest rate of ST. Longer-term outcomes were similar, as EES-CoCr was associated with the lowest rate of TVR and MI at 3-year follow-up.
Next-Generation DES
Bioresorbable Polymers
The localized immune response and hypersensitivity reaction to durable polymers may contribute to the long-term risk of ST associated with DES [54]. As a result, several recent trials have investigated the safety and efficacy of DES with bioresorbable polymers, none of which are currently available for investigational or commercial use in the USA.
The Nobori biolimus-eluting stent with a bioresorbable polymer (BES) comprises of a stainless steel platform with a strut thickness of 120 μm, a polylactic acid polymer applied solely to the abluminal stent surface that dissolves into carbon dioxide and water after 6 to 9 months, and a semi-synthetic sirolimus analog with greater lipophilicity than sirolimus. The Limus Eluted from a Durable Versus Erodable Stent Coating (LEADERS) trial randomized 1707 patients to SES or BES [55•]. At 5 years, BES was noninferior to SES in the MACE composite of cardiac death, MI, and TVR. However, BES was associated with a significant reduction in MACE in patients with more complex coronary anatomy (BES 30.3 % vs. SES 22.7 %, p = 0.02) and in very late ST (BES 0.7 % vs. SES 2.5 %, p = 0.003). The randomized Abluminal Biodegradable Polymer Biolimus Eluting Stent Versus Durable Polymer Everolimus Eluting stent (COMPARE II) trial and Nobori Biolimus Eluting Versus Xience/Promus Everolimus Eluting Stent (NEXT) trial, however, demonstrated no significant difference in MACE or ST with BES compared to EES-CoCr at 12 months [56, 57].
Other DES with bioresorbable polymers include the Yukon PC Choice sirolimus-eluting stent with a bioresorbable polymer (SES-BP) and the SYNERGY everolimus-eluting stent with a bioresorbable polymer (EES-BP). While the SES-BP comprises of a stainless steel platform and the EES-BP of a PtCr platform, both of these stents have thinner struts (SES-BP 87 μm, EES-BP 71 μm) than BES. The Intracoronary Stenting and Angiographic Results: Test Efficacy of 3 Limus Eluting Stents (ISAR TEST 4) trial, however, demonstrated no significant difference in the primary composite of cardiac death, target vessel-related MI, or TLR at 3 years between the SES-BP, original first-generation SES, and EES-CoCr [58]. Similarly, in the Trial to Assess the Safety and Performance of the Evolution Everolimus-Eluting Monorail Coronary Stent System for Treatment of De Novo Atherosclerotic Lesion (EVOLVE), EES-BP was noninferior to the currently approved EES-PtCr at 6-month follow-up [59].
Not all of the evidence, however, suggested a benefit with use of a bioabsorbable polymer. The SORT OUT V trial randomized 1229 patients to BES or the original first-generation SES. Although BES was noninferior to SES with respect to MACE and TVR, there was an increased risk of ST with BES compared to SES at 1-year follow-up (0.7 vs. 0.2 %, p = 0.034) [60]. The Cobalt Chromium Stent with Antiproliferative for Restenosis II (COSTAR II) trial demonstrated a significantly higher rate of MACE with a paclitaxel-eluting stent composed of a bioresorbable polymer (PES-BP) compared to the original first-generation PES (11.0 vs. 6.9 %, p < 0.005), a finding primarily attributable to a higher rate in TVR [61]. A meta-analysis investigating over 250,000 patients from 126 randomized trials demonstrated that DES with bioresorbable polymers were associated with a lower rate of TVR when compared to first-generation but not newer-generation DES with durable polymers [62•]. Two subsequent meta-analyses demonstrated higher rates of MI and long-term ST with BES than EES-CoCr [63•, 64]. These data again suggested that EES-CoCr may still have the best combination of efficacy and safety and that it seems hard to improve on currently approved DES.
Bioresorbable Stents
The recognition that incomplete endothelialization of DES can persist even on long-term follow-up has led to investigations in bioresorbable stents. The first bioresorbable stents were implanted between 1998 and 2000, and 10-year follow-up data in 50 patients demonstrated one cardiac death, four MIs, and two definite stent thromboses, suggesting long-term safety [65•]. Only recently have bioresorbable stents undergone rigorous systematic evaluation. The Absorb EES has a bioresorbable polymer and a bioresorbable scaffold with a strut thickness of 150 μm made of poly(l-lactide) that starts to gradually disintegrate around 1 to 2 years and completely dissolves by 3 to 3.5 years. The recently completed Evaluation of the Absorb Everolimus Eluting Bioresorbable Vascular Scaffold System Against the Xience Everolimus Eluting Coronary Stent (ABSORB) II trial randomized 501 patients 2:1 to Absorb EES or Xience EES-CoCr. Although data are not yet available on the co-primary endpoints of vasomotion (change in mean lumen diameter before and after nitrate administration) and change in minimum lumen diameter at 2-year follow-up, there have been no significant safety concerns reported with the Absorb EES at 1-year follow-up [66]. However, given that Absorb EES received approval in Europe 4 years ago, data from a European multi-center registry of 1731 Absorb EES implanted in 1189 patients are available and demonstrate a somewhat high cumulative incidence of scaffold thrombosis at 30 days (1.5 %) and 6 months (2.1 %) [67]. The currently ongoing ABSORB III trial aimed at obtaining US approval will randomize ~2000 patients 2:1 to the Absorb EES or Xience EES-CoCr and evaluate the composite of cardiac death, target vessel MI, or clinically indicated TLR at 1-year follow-up.
Conclusions
The advancements made in the efficacy and safety of PCI technology are remarkable, and the rapid pace of development in this field and the pipeline of stent design have been exciting to watch. Improvements in stent platform, polymer, and drug have revolutionized the way we treat coronary disease and culminate in the currently approved and hard to improve upon the newest second-generation DES. Investigations into bioresorbable stents remain ongoing with the aim to reduce the need for long-term dual antiplatelet therapy while continuing to offer low short- and long-term risks of ST.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Agostoni P, Valgimigli M, Biondi-Zoccai GG, et al. Clinical effectiveness of bare-metal stenting compared with balloon angioplasty in total coronary occlusions: insights from a systematic overview of randomized trials in light of the drug-eluting stent era. Am Heart J. 2006;151:682–9.
Duckers HJ, Nabel EG, Serruys PW. Essentials of restenosis: for the interventional cardiologist. Totowa, NJ: Humana Press; 2007.
Wohrle J, Al-Khayer E, Grotzinger U, et al. Comparison of the heparin coated vs the uncoated Jostent—no influence on restenosis or clinical outcome. Eur Heart J. 2001;22:1808–16.
Mehran R, Nikolsky E, Camenzind E, et al. An Internet-based registry examining the efficacy of heparin coating in patients undergoing coronary stent implantation. Am Heart J. 2005;150:1171–6.
Sousa JE, Serruys PW, Costa MA. New frontiers in cardiology: drug eluting stents. Circulation. 2003;107:2274–9.
Morice MC, Serruys PW, Sousa JE, Fajadet J, Ban Hayashi E, Perin M, et al. Randomized Study with the Sirolimus-Coated Bx Velocity Balloon-Expandable Stent in the Treatment of Patients with de Novo Native Coronary Artery Lesions. A randomized comparison of a sirolimus-eluting stent with a standard stent for coronary revascularization. N Engl J Med. 2002;346:1773–80.
Kelbaek H, Thuesen L, Helqvist S, Kløvgaard L, Jørgensen E, Aljabbari S, et al. The Stenting Coronary Arteries in Non-stress/Benestent Disease (SCANDSTENT) trial. J Am Coll Cardiol. 2006;47:449–55.
Moses JW, Leon MB, Popma JJ, et al. Sirolimus-eluting stents versus standard stents in patients with stenosis in a native coronary artery. N Engl J Med. 2003;349:1315–23.
Weisz G, Leon MB, Holmes DR, et al. Five-year follow-up after sirolimus-eluting stent implantation. Results of the SIRIUS (Sirolimus-Eluting Stent in De-Novo Native Coronary Lesions) trial. J Am Coll Cardiol. 2009;53:1488–97.
Stone GW, Ellis SG, Cox DA, et al. A polymer-based, paclitaxel-eluting stent in patients with coronary artery disease. N Engl J Med. 2004;50:221–31.
Ellis SG, Stone GW, Cox DA, Hermiller J, O’Shaughnessy C, Mann T, et al. Long-term safety and efficacy with paclitaxel-eluting stents: 5-year final results of the TAXUS IV clinical trial (TAXUS IV-SR: Treatment of De Novo Coronary Disease Using a Single Paclitaxel-Eluting Stent). JACC Cardiovasc Interv. 2009;2:1248–59.
Windecker S, Remondino A, Eberli FR, Jüni P, Räber L, Wenaweser P, et al. Sirolimus-eluting and paclitaxel-eluting stents for coronary revascularization. N Engl J Med. 2005;353:653–62.
Morice MC, Colombo A, Meier B, Serruys P, Tamburino C, Guagliumi G, et al. Sirolimus- vs paclitaxel-eluting stents in de novo coronary artery lesions: the REALITY trial: a randomized controlled trial. JAMA. 2006;295(8):895–904.
Galløe AM, Thuesen L, Kelbaek H, Thayssen P, Rasmussen K, Hansen PR, et al. Comparison of paclitaxel- and sirolimus-eluting stents in everyday clinical practice: the SORT OUT II randomized trial. JAMA. 2008;299:409–16.
Stone GW, Moses JW, Ellis SG, Schofer J, Dawkins KD, Morice MC, et al. Safety and efficacy of sirolimus- and paclitaxel-eluting coronary stents. N Engl J Med. 2007;356:998–1008.
Daemen J, Wenaweser P, Tsuchida K, Abrecht L, Vaina S, Morger C, et al. Early and late coronary stent thrombosis of sirolimus-eluting and paclitaxel-eluting stents in routine clinical practice: data from a large two-institutional cohort study. Lancet. 2007;369:667–78.
Schömig A, Dibra A, Windecker S, Mehilli J, de Lezo Suárez J, Kaiser C, et al. A meta-analysis of 16 randomized trials of sirolimus-eluting stents versus paclitaxel-eluting stents in patients with coronary artery disease. J Am Coll Cardiol. 2007;50:1373–80.
Stettler C, Wandel S, Allemann S, Kastrati A, Morice MC, Schömig A, et al. Outcomes associated with drug-eluting and bare-metal stents: a collaborative network meta-analysis. Lancet. 2007;370:937–48.
Holmes Jr DR, Kereiakes DJ, Garg S, Serruys PW, Dehmer GJ, Ellis SG, et al. Stent thrombosis. J Am Coll Cardiol. 2010;56:1357–65.
Mauri L, Hsieh WH, Massaro JM, Ho KK, D’Agostino R, Cutlip DE. Stent thrombosis in randomized clinical trials of drug-eluting stents. N Engl J Med. 2007;356:1020–9.
Kastrati A, Mehilli J, Dirschinger J, Dotzer F, Schühlen H, Neumann FJ, et al. Intracoronary stenting and angiographic results: strut thickness effect on restenosis outcome (ISAR-STEREO) trial. Circulation. 2001;103:2816–21.
Yoshitomi Y, Kojima S, Yano M, Sugi T, Matsumoto Y, Saotome M, et al. Does stent design affect probability of restenosis? A randomized trial comparing Multilink stents with GFX stents. Am Heart J. 2001;142:445–51.
Pache J, Kastrati A, Mehilli J, Schühlen H, Dotzer F, Hausleiter J, et al. Intracoronary stenting and angiographic results: strut thickness effect on restenosis outcome (ISAR-STEREO-2) trial. J Am Coll Cardiol. 2003;41:1283–8.
Stone GW, Midei M, Newman W, Sanz M, Hermiller JB, Williams J, et al. Comparison of an everolimus-eluting stent and a paclitaxel-eluting stent in patients with coronary artery disease: a randomized trial. JAMA. 2008;299:1903–13.
Applegate RJ, Yaqub M, Hermiller JB, Sood P, Yu S, Doostzadeh J, et al. Long-term (three-year) safety and efficacy of everolimus-eluting stents compared to paclitaxel-eluting stents (from the SPIRIT III Trial). Am J Cardiol. 2011;107:833–40.
Stone GW, Rizvi A, Newman W, Mastali K, Wang JC, Caputo R, et al. Everolimus-eluting versus paclitaxel-eluting stents in coronary artery disease. N Engl J Med. 2010;362:1663–74.
Stone GW, Rizvi A, Sudhir K, Newman W, Applegate RJ, Cannon LA, et al. Randomized comparison of everolimus- and paclitaxel-eluting stents. 2-year follow-up from the SPIRIT (Clinical Evaluation of the XIENCE V Everolimus Eluting Coronary Stent System) IV trial. J Am Coll Cardiol. 2011;58:19–25.
Kedhi E, Joesoef KS, McFadden E, Wassing J, van Mieghem C, Goedhart D, et al. Second-generation everolimus-eluting and paclitaxel-eluting stents in real-life practice (COMPARE): a randomised trial. Lancet. 2010;375:201–9.
Smits PC, Kedhi E, Royaards KJ, Joesoef KS, Wassing J, Rademaker-Havinga TA, et al. 2-year follow-up of a randomized controlled trial of everolimus- and paclitaxel-eluting stents for coronary revascularization in daily practice. COMPARE (Comparison of the everolimus eluting XIENCE-V stent with the paclitaxel eluting TAXUS LIBERTÉ stent in all-comers: a randomized open label trial). J Am Coll Cardiol. 2011;58:11–8.
Jensen LO, Thayssen P, Christiansen EH, Tilsted HH, Maeng M, Hansen KN, et al. 2-year patient-related versus stent-related outcomes: the SORT OUT IV (Scandinavian Organization for Randomized Trials With Clinical Outcome IV) Trial. J Am Coll Cardiol. 2012;60:1140–7.
Jensen LO, Thayssen P, Hansen HS, Christiansen EH, Tilsted HH, Krusell LR, et al. Randomized comparison of everolimus-eluting and sirolimus-eluting stents in patients treated with percutaneous coronary intervention: the Scandinavian Organization for Randomized Trials with Clinical Outcome IV (SORT OUT IV). Circulation. 2012;125:1246–55. Demonstrated that second generation everolimus-eluting stents are noninferior to first generation sirolimus-eluting stents and that first generation stents may have a higher rate of long-term stent thrombosis.
Kimura T, Morimoto T, Natsuaki M, Shiomi H, Igarashi K, Kadota K, et al. Comparison of everolimus-eluting and sirolimus-eluting coronary stents: 1-year outcomes from the Randomized Evaluation of Sirolimus-eluting Versus Everolimus-eluting stent Trial (RESET). Circulation. 2012;126:1225–36.
Räber L, Jüni P, Nüesch E, Kalesan B, Wenaweser P, Moschovitis A, et al. Long-term comparison of everolimus-eluting and sirolimus-eluting stents for coronary revascularization. J Am Coll Cardiol. 2011;57:2143–51. Demonstrated that everolimus-eluting stents likely have a long-term benefit over sirolimus-eluting stents driven by decreased incidence of stent thrombosis.
de Waha A, Dibra A, Byrne RA, Ndrepepa G, Mehilli J, Fusaro M, et al. Everolimus-eluting versus sirolimus-eluting stents: a meta-analysis of randomized trials. Circ Cardiovasc Interv. 2011;4:371–7.
Jensen L, Thayssen P, Maeng M, et al. Three-year outcomes after revascularization with everolimus- and sirolimus-eluting stents from the SORT OUT IV trial. J Am Coll Cardiol Intv. 2014;7:840–8.
Di Lorenzo E, Sauro R, Varricchio A, et al. Randomized comparison of everolimus-eluting stents and sirolimus-eluting stent in patients with ST elevation myocardial infarction: RACES-MI trial. J Am Coll Cardiol Intv. 2014;7:849–56. Demonstrated that everolimus-eluting stents are as effective as sirolimus-eluting stents but safer due to associated decreased risk of ST.
Kandzari DE, Leon MB, Popma JJ, Fitzgerald PJ, O’Shaughnessy C, Ball MW, et al. Comparison of zotarolimus-eluting and sirolimus-eluting stents in patients with native coronary artery disease. J Am Coll Cardiol. 2006;48:2440–7.
Moussa ID, Klein LW, Shah B, Mehran R, Mack MJ, Brilakis ES, et al. Consideration of a new definition of clinically relevant myocardial infarction after coronary revascularization procedures: an expert consensus document from the Society for Cardiovascular Angiography and Interventions (SCAI). J Am Coll Cardiol. 2013;62:1563–70.
Eisenstein EL, Leon MB, Kandzari DE, Mauri L, Edwards R, Kong DF, et al. Long-term clinical and economic analysis of the Endeavor zotarolimus-eluting stent versus the cypher sirolimus-eluting stent: 3-year results from the ENDEAVOR III trial (Randomized Controlled Trial of the Medtronic Endeavor Drug [ABT-578] Eluting Coronary Stent System Versus the Cypher Sirolimus-Eluting Coronary Stent System in De Novo Native Coronary Artery Lesions). JACC Cardiovasc Interv. 2009;2:1199–207.
Maeng M, Tilsted HH, Jensen LO, Kaltoft A, Kelbæk H, Abildgaard U, et al. 3-year clinical outcomes in the randomized SORT OUT III superiority trial comparing zotarolimus- and sirolimus-eluting coronary stents. JACC Cardiovasc Interv. 2012;5:812–8.
Stone GW, Teirstein PS, Meredith IT, et al. The PLATINUM (A Prospective, Randomized, Multicenter Trial to Assess an Everolimus-Eluting Coronary Stent System [PROMUS Element] for the Treatment of up to Two De Novo Coronary Artery Lesions) trial. J Am Coll Cardiol. 2011;57:1700–8.
Williams P, Mamas M, Morgan K, El-Omar M, Clarke B, Bainbridge A, et al. Longitudinal stent deformation: a retrospective analysis of frequency and mechanisms. Euro Interv. 2012;8:267–74.
Orrniston JA et al. JACC: Cardiovasc Interv. 2011;4:1310–7.
Chalet Y, Panes F, Chevalier B, Monassier JP, Spaulding C, Lancelin B, et al. Should we avoid ostial implantations of Wiktor stents? Cathet Cardiovasc Diagn. 1994;32:376–9.
Leibundgut G, Gick M, Toma A, et al. Longitudinal compression of the platinum-chromium everolimus-eluting stent during coronary implantation: predisposing mechanical properties, incidence, and predictors in a large patient cohort. Cathet Cardiovasc Interv. 2013;81:E206–14.
Tada T, Byrne RA, Cassese S, King L, Schulz S, Mehilli J, et al. Comparative efficacy of 2 zotarolimus-eluting stent generations: resolute versus endeavor stents in patients with coronary artery disease. Am Heart J. 2013;165:80–6. Demonstrated that Resolute zotarolimus-eluting stents are superior with regards to restenosis rates compared to Endeavor zotarolimus-eluting stents due to improved drug release kinetics.
Park KW, Lee JM, Kang SH, Ahn HS, Yang HM, Lee HY, et al. Safety and efficacy of second-generation everolimus-eluting Xience V stents versus zotarolimus-eluting resolute stents in real-world practice: patient-related and stent-related outcomes from the multicenter prospective EXCELLENT and RESOLUTE-Korea registries. J Am Coll Cardiol. 2013;61:536–44. Demonstrated that everolimus-eluting stents and Resolute zotarolimus-eluting stents have similar safety and efficacy over 1 year follow up.
von Birgelen C, Basalus MW, Tandjung K, van Houwelingen KG, Stoel MG, Louwerenburg JH, et al. A randomized controlled trial in second-generation zotarolimus-eluting Resolute stents versus everolimus-eluting Xience V stents in real-world patients: the TWENTE trial. J Am Coll Cardiol. 2012;59:1350–61. Demonstrated that Resolute zotarolimus-eluting stents are noninferior to everolimus-eluting stents in a real world population of patients with complex lesions.
Serruys PW, Silber S, Garg S, van Geuns RJ, Richardt G, Buszman PE, et al. Comparison of zotarolimus-eluting and everolimus-eluting coronary stents. N Engl J Med. 2010;363:136–46.
von Birgelen C, Sen H, Lam MK, Danse PW, et al. Third-generation zotarolimus-eluting and everolimus-eluting stents in all-comer patients requiring a percutaneous coronary intervention (DUTCH PEERS): a randomised, single-blind, multicentre, non-inferiority trial. Lancet. 2014;383:413–23. Demonstrated, again, that Resolute zotarolimus-eluting stents and everolimus-eluting stents perform comparably with regards to safety and efficacy with no significant difference in rates of stent thrombosis.
Palmerini T, Biondi-Zoccai G, Della Riva D, Stettler C, Sangiorgi D, D’Ascenzo F, et al. Stent thrombosis with drug-eluting and bare-metal stents: evidence from a comprehensive network meta-analysis. Lancet. 2012;379:1393–402. Demonstrated that colbalt chromium everolimus-eluting stents have the lowest rate of stent thrombosis in this comparison of bare metal stent and various drug-eluting stents.
Palmerini T, Biondi-Zoccai G, Della Riva D, Mariani A, Sabaté M, Valgimigli M, et al. Clinical outcomes with drug-eluting and bare-metal stents in patients with ST-segment elevation myocardial infarction: evidence from a comprehensive network meta-analysis. J Am Coll Cardiol. 2013;62:496–504.
Bangalore S, Kumar S, Fusaro M, Amoroso N, et al. Short- and long-term outcomes with drug-eluting and bare-metal coronary stents: a mixed-treatment comparison analysis of 117 762 patient-years of follow-up from randomized trials. Circulation. 2012;125:2873–91. This metaanalysis evaluating the safety and efficacy of various drug-eluting stents and bare metal stents demonstrated that everolimus-eluting stents, sirolimus-eluting stents, and Resolute zotarolimus-eluting stents have the greatest efficacy and everolimus-eluting stents may be the safest.
Finn AV, Joner M, Nakazawa G, Kolodgie F, Newell J, John MC, et al. Pathological correlates of late drug-eluting stent thrombosis: strut coverage as a marker of endothelialization. Circulation. 2007;115:2435–41.
Serruys PW, Farooq V, Kalesan B, de Vries T, Buszman P, Linke A, et al. Improved safety and reduction in stent thrombosis associated with biodegradable polymer-based biolimus-eluting stents versus durable polymer-based sirolimus-eluting stents in patients with coronary artery disease: final 5-year report of the LEADERS (Limus Eluted From A Durable Versus ERodable Stent Coating) randomized, noninferiority trial. JACC Cardiovasc Interv. 2013;6:777–89. Demonstrated that biodegradable polymers may reduce the risk of very late stent thrombosis associated with first generation drug-eluting stents.
Smits PC, Hofma S, Togni M, Vázquez N, Valdés M, Voudris V, et al. Abluminal biodegradable polymer biolimus-eluting stent versus durable polymer everolimus-eluting stent (COMPARE II): a randomised, controlled, non-inferiority trial. Lancet. 2013;381:651–60.
Natsuaki M, Kozuma K, Morimoto T, Kadota K, Muramatsu T, Nakagawa Y, et al. Biodegradable polymer biolimus-eluting stent versus durable polymer everolimus-eluting stent: a randomized, controlled, noninferiority trial. J Am Coll Cardiol. 2013;62:181–90.
Byrne RA, Kastrati A, Kufner S, Massberg S, Birkmeier KA, Laugwitz KL, et al. Randomized, non-inferiority trial of three limus agent-eluting stents with different polymer coatings: the Intracoronary Stenting and Angiographic Results: Test Efficacy of 3 Limus-Eluting Stents (ISAR-TEST-4) Trial. Eur Heart J. 2009;30:2441–9.
Meredith IT, Verheye S, Dubois CL, Dens J, Fajadet J, Carrié D, et al. Primary endpoint results of the EVOLVE trial: a randomized evaluation of a novel bioabsorbable polymer-coated, everolimus-eluting coronary stent. J Am Coll Cardiol. 2012;59:1362–70.
Christiansen EH, Jensen LO, Thayssen P, Tilsted HH, Krusell LR, Hansen KN, et al. Biolimus-eluting biodegradable polymer-coated stent versus durable polymer-coated sirolimus-eluting stent in unselected patients receiving percutaneous coronary intervention (SORT OUT V): a randomised non-inferiority trial. Lancet. 2013;381:661–9.
Krucoff MW, Kereiakes DJ, Petersen JL, Mehran R, Hasselblad V, Lansky AJ, et al. A novel bioresorbable polymer paclitaxel-eluting stent for the treatment of single and multivessel coronary disease: primary results of the COSTAR (Cobalt Chromium Stent With Antiproliferative for Restenosis) II study. J Am Coll Cardiol. 2008;51:1543–52.
Bangalore S, Toklu B, Amoroso N, Fusaro M, Kumar S, Hannan EL, et al. Bare metal stents, durable polymer drug eluting stents, and biodegradable polymer drug eluting stents for coronary artery disease: mixed treatment comparison meta-analysis. BMJ. 2013;347:f6625. This meta-analysis evaluating bare metal stents, drug-eluting stents, and drug-eluting stents with bioresorbable polymers demonstrated that everolimus-eluting stents and Resolute zotarolimus-eluting stents have the best combination of safety and efficacy.
Navarese EP, Tandjung K, Claessen B, Andreotti F, Kowalewski M, Kandzari DE, et al. Safety and efficacy outcomes of first and second generation durable polymer drug eluting stents and biodegradable polymer biolimus eluting stents in clinical practice: comprehensive network meta-analysis. BMJ. 2013;347:f6530. Demonstrated that bioresorbable polymers have a significantly higher rate of myocardial infarction when compared to everolimus-eluting stents and Resolute zotarolimus-eluting stents.
Palmerini T, Biondi-Zoccai G, Della Riva D, Mariani A, Sabaté M, Smits PC, et al. Clinical outcomes with bioabsorbable polymer- versus durable polymer-based drug-eluting and bare-metal stents: evidence from a comprehensive network meta-analysis. J Am Coll Cardiol. 2014;63:299–307.
Nishio S, Kosuga K, Igaki K, Okada M, Kyo E, Tsuji T, et al. Long-term (>10 years) clinical outcomes of first-in-human biodegradable poly-l-lactic acid coronary stents: Igaki-Tamai stents. Circulation. 2012;125:2343–53. This 10 year investigation of bioresorbable stents demonstrated a good safety and efficacy profile with the stent struts mostly disappearing by 3 years follow-up.
Diletti R, Serruys PW, Farooq V, Sudhir K, Dorange C, Miquel-Hebert K, et al. ABSORB II randomized controlled trial: a clinical evaluation to compare the safety, efficacy, and performance of the Absorb everolimus-eluting bioresorbable vascular scaffold system against the XIENCE everolimus-eluting coronary stent system in the treatment of subjects with ischemic heart disease caused by de novo native coronary artery lesions: rationale and study design. Am Heart J. 2012;164:654–63.
Capodanno D, Gori T, Nef H, Latib A, Mehilli J, Lesiak M, Caramanno G, Naber C, Di Mario C, Colombo A, Capranzano P, Wiebe J, Araszkiewicz A, Geraci S, Pyxaras S, Mattesini A, Naganuma T, Münzel T, Tamburino C. Percutaneous coronary intervention with everolimus-eluting bioresorbable vascular scaffolds in routine clinical practice: early and midterm outcomes from the European multicentre GHOST-EU registry. EuroIntervention. 2014 Jul 18. [Epub ahead of print]
Rasmussen K, Maeng M, Kaltoft A, Thayssen P, Kelbaek H, Tilsted HH, et al. Efficacy and safety of zotarolimus-eluting and sirolimus-eluting coronary stents in routine clinical care (SORT OUT III): a randomised controlled superiority trial. Lancet. 2010;375:1090–9.
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
Gregory Katz, Bhisham Harchandani, and Binita Shah declare that they have no conflict of interest. Binita Shah was partially funded by an NIH grant (UL1 TR000038).
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Coronary Heart Disease
Rights and permissions
About this article
Cite this article
Katz, G., Harchandani, B. & Shah, B. Drug-Eluting Stents: the Past, Present, and Future. Curr Atheroscler Rep 17, 11 (2015). https://doi.org/10.1007/s11883-014-0485-2
Published:
DOI: https://doi.org/10.1007/s11883-014-0485-2