Abstract
Background
Anatomy educators are increasing their utilisation of radiology in anatomy education in line with growing requirements for undergraduate radiology competency and clinical need.
Aims
We aimed to evaluate student perceptions of radiology and to outline the technical and academic considerations underlying the integration of radiology into musculoskeletal practical anatomy sessions.
Materials and methods
The formal integration of radiology into anatomy practical sessions took place over a 5-week period during the lower limb musculoskeletal component of the anatomy course taught to first-year medical students. During practical sessions, students were required to rotate between aligned audio-visual radiology presentations, osteology/anatomical models, and prosection/dissection learning stations. After completing the course, students were invited to complete a survey to establish their opinions on radiology as a mode of learning and their satisfaction with radiological integration in anatomical practical sessions.
Results
Most students were not familiar with radiology prior to attending our university. All our students agreed or strongly agreed that learning to read radiographs in anatomy is important and most agreed that radiology is a valid assessment tool. Sixty percent stated that radiology facilitated their understanding of anatomy. The majority believed that radiology was best suited to clinically relevant anatomy and X-rays were their preferred learning tool.
Conclusions
The practical approach to integrating radiology into undergraduate musculoskeletal anatomy described here did not place strain on existing academic resources. Most students agreed that radiology should be increased in anatomy education and that learning to understand radiographs in anatomy was important for clinical practice.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
A comprehensive understanding of anatomy remains fundamental to preparing medical students for clinical practice, as it forms the foundation for the understanding of disease and treatment strategies [1–3]. Anatomy is traditionally taught in the first 2 years of preclinical training and is delivered by lectures, small group learning, cadaveric dissection, prosection, or combined approaches of these [4]. While cadaveric-based dissection/prosection teaching remains at the core of anatomy teaching [5–7], modern digital and pedagogical anatomy resources have assisted educators in promoting discipline-specific teaching [8–16]. In particular, technological advances in medical imaging are greatly enhancing diagnostics and radiology is gradually becoming an integral component of preclinical training [3, 8, 16–23]. For example, the rapid uptake of mobile technologies and their integration with pre-existing Picture Archiving and Communications Systems (PACS) has revolutionised the practice of radiology and access to diagnostic images among healthcare professionals. However, while the integration of radiology into academic anatomy teaching has been documented as early as 1950 [24], modern digital platforms have only recently facilitated its use in formal teaching and its amalgamation into curricula varies amongst institutions.
Radiology appears main-stream in the United States (US) (80 %), Canadian (92 %), Australian, and New Zealand (100 %)-based medical schools, which utilize at least some form of radiological imaging as part of their undergraduate curriculum [25–28]. Moreover, a survey of 21 British and Irish universities performed in 2002 showed that the majority of medical schools are delivering anatomy content via integrated curricula involving radiology [17]. However, the extent of radiology’s involvement in undergraduate curricula is often truncated, inconsistent, and its vertical integration varies widely. For example, the European Society of Radiology showed that only 26 % of 34 surveyed European countries integrated radiology into first-year medicine [29], while US medical schools devoted an average of just 5 % of teaching time to radiology [30]. Radiology, including X-ray, computed tomography (CT), magnetic resonance imaging (MRI), and ultrasound enhances student understanding of three-dimensional (3D) anatomy [2, 23, 31–36], demonstrates the immediate relevance of anatomical learning and bridges the gap between preclinical teaching and professional practice [37–39]. Moreover, incorporating radiology into undergraduate anatomy teaching prior to formal clinical training has been shown to enhance interpretation of vital radiographic material in clinical years [40–42]. The necessity for more formalised and consensus-led integration of radiology in anatomy education is recognised by both educators and clinicians alike [7, 43–49]. However, despite the perceived advantages, many anatomy departments are failing to consistently engage their anatomy syllabus with radiology components [29, 50, 51], which is most likely a result of increasing student demand, declining teaching resources and potentially paucity of radiology expertise [3, 8, 17–21]. In addition, some educators feel that anatomy teaching should exclusively focus on clinically relevant anatomy and the interpretation of radiographs [52, 53], while others suggest that a blended approach is necessary, where the traditional anatomy teaching should place greater emphasis on radiology [38, 54–58]. Moreover, the role of the radiologist in undergraduate anatomy education, proposed delivery methods or recommended time allocation to radiology teaching remain unclarified, especially in the context of specific modular anatomy components, such as musculoskeletal anatomy.
In this communication, we describe the formal integration of radiology into anatomy lower limb practical sessions, without placing strain on existing teaching resources. We evaluated student opinion of the integration of clinically relevant and structural/functional anatomy, X-ray, CT, MRI, and ultrasound radiology into undergraduate lower limb musculoskeletal anatomy laboratory sessions. The class concerned consisted of 181 students who were divided into 2 groups of 90 and 91 to attend practical sessions in the dissection theatre (DT) on consecutive days. The DT was separated into 10 learning stations. Each station comprised of a donor body, a display area for anatomical models, and a 36-inch monitor running an android operating system. Academic staff involved in the delivery of practical sessions consisted of four Anatomy Demonstrators and two Anatomy Lecturers. The musculoskeletal anatomy taught within our department currently consists of a 10-week semester, with 5 weeks each devoted to upper and lower limb anatomy. For the latter, the first four sessions pertained to one element of lower limb anatomy and involved integrating traditional approaches, including prosection, dissection, cross-sectional plates, plastic models, and osteology specimens with key radiology images that necessitated student interaction though identifying important anatomical features. The final practical was a revision session which involved the understanding of musculoskeletal pathologies. Our laboratory methods are described on a week-to-week basis and our findings are discussed in relation to current musculoskeletal anatomy teaching practices and the student learning experience.
Materials and methods
The integration of radiology into lower limb practical sessions
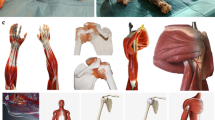
The study was performed over a 5-week period from weeks beginning 2nd November to 4th December 2015, during which students participated in 5 × 3-h practical anatomy sessions in the DT based on all aspects of lower limb musculoskeletal anatomy. In groups of eight and nine, students were assigned to each of the learning stations in the DT. Students were then divided into three groups of three individuals at each station, which were rotated every 45 min between three practical learning components; namely (1) a cadaver, (2) osteology/plastic models, and (3) an audio-visual (AV)-based radiology presentation (for samples of each learning component, see Fig. 1). A final 45 min was available after these rotation components for small group tutorials, which were delivered by anatomy staff. Prosections on one lower limb were performed in advance by staff, offering students the opportunity to dissect structures in the remaining lower limb during the cadaver component of the practical session. Radiology was integrated into practical classes through PowerPoint (Microsoft, version: 14.0.7166.5000) presentations displaying plain film X-rays, CT, MRI, angiography, and ultrasound. These were uploaded to monitors at each station. Students had the ability to control and progress the presentation using remote controllers for each monitor. Each presentation consisted on average ten slides incorporating various radiological modalities demonstrating lower limb structures relevant to each week’s learning objectives (Table 1). Content for the first 4 weeks consisted of non-pathological images of bones, muscles, tendons, ligaments, and vessels. Each image was first presented in an unlabelled format followed by a labelled version, and short answer questions were included with some of the slides. For example, an X-ray of the proximal femur included an arrow pointing to the lesser trochanter, students were asked to identify the bony prominence and to name the muscle attached to it. The final practical was dedicated to gross anatomy revision, and pathological images were included.
Sample presentation slides, anatomical specimen, and prosections from practical sessions 1–5. a Week 1 X-ray of the pelvis, including proximal femurs and accompanying questions. Osteology of human pelvis and prosection of gluteal region. b Week 2 MRI of the Knee and accompanying questions. Knee joint osteology and prosection of anterior knee, showing quadriceps muscles and patellar tendons. c Week 3 X-ray of the tibia and fibula and accompanying questions. Osteology of tibia and fibula and distal tibiofibular joint. Prosection of anterior and lateral compartments of leg. d Week 4 X-ray of the ankle/foot and accompanying legend. Osteology of the foot and sub-talar joints. Prosection of the anterior compartment of leg and foot. e Week 5 X-ray of the lower limb. Osteology of the lower limb. Prosection of anterior compartment muscles of thigh and leg
Evaluating the opinions of students toward radiology integration
After the final practical session, 181 first-year medical students were invited to complete an online anonymised survey to establish their attitudes towards the integration of radiology into lower limb anatomy. The survey was reviewed and approved by the local ethics committee of TCD. The survey instrument was a questionnaire consisting of ten independent, multiple choice questions that collected demographic data and sought to gauge student attitudes towards radiology and to measure their perceived benefit of radiology in anatomy education. Demographic questions determined the age range, gender, and region of origin of participants. Radiology questions were designed to determine (1) whether students had experience in radiology prior to attending our institution, (2) whether students enjoyed using radiology when learning anatomy, (3) whether radiology improved their understanding of anatomy during practical sessions, (4) which radiological modality they most preferred, (5) what type of anatomy was most enhanced by radiology, (6) whether radiology is a valid assessment tool in anatomy, and (7) their perceived importance of radiology for use in clinical practice. To analyse demographics and non-scalar survey responses, we tabulated data collected using Excel (version 14.0, Microsoft Corp., Redmond, WA). For scalar Likert data, Pearson’s Chi-squared (χ 2) tests were performed to assess significant deviations in preferences from chance deviations using the Statistical Package for Social Scientists (version 22, IBM Corp., Armonk, NY). Data were considered to be statistically different from chance expectations at p < 0.05.
Results
Demographics
One hundred and eighty-one first-year medical students were invited to complete an anonymised questionnaire. Eighty-nine students responded for a 49 % response rate. Forty-three percent of respondents were male and the majority were aged between 18 and 30 years of age (99 % of those surveyed) (Table 2). Seventy-two percent of respondents were European, while the remaining students originated from Asia, North America, Africa, and the Caribbean (Table 2).
Student opinion of radiology in practical anatomy education
Students were first asked whether or not they had experience of reading radiographs prior to attending our institution. The majority (84 %) stated that they had no prior experience in radiology (χ 2 = 40, df = 1, p < 0.0001) (Table 3). Students were then asked if they enjoyed radiological integration in anatomy practical sessions. The overall pooled distribution of preferences showed a significant deviation from chance (χ 2 = 50, df = 3, p < 0.0001), with 66 % stating that they enjoyed learning anatomy with radiology (p < 0.0001), while 32 % said that it depended on the topic (Table 3). Students were then asked if integrating radiology into anatomy practical sessions facilitated their understanding of anatomy. Students responses showed a significant deviation from chance expectations, indicating a clear preference in responses (χ 2 = 32, df = 2, p < 0.0001). These responses also mirrored the previous question in that 60 % agreed that radiology facilitated their learning, while 31 % stated that it depended on the topic (Table 3). Students were then asked their preferred radiological method for anatomy learning. Clear preferences were demonstrated in their responses (χ 2 = 115, df = 4, p < 0.0001). Interestingly, 66 % of students chose X-ray (p < 0.0001), while 17 % chose CT and 13 % chose MRI (Table 3). The remainder chose angiography (4 %) and ultrasound (1 %). Students were next asked which type of anatomy benefitted most from radiology integration. A clear preference was also observed in their responses (χ 2 = 155, df = 5, p < 0.0001). A significant majority (73 %) chose clinical anatomy (p > 0.0001), 20 % chose osteology with the remainder choosing neuroanatomy (4.8 %) or muscular anatomy (2.4 %). No students selected vascular anatomy (Table 3).
We next determined whether students agreed or disagreed that radiology was a valid assessment tool in anatomy education. Sixty-seven percent agreed or strongly agreed, while 27 % were neutral (χ 2 = 69, df = 4, p < 0.0001) (Fig. 2). Finally, we determined whether students agreed or disagreed that the ability to read radiographs is important for clinical practice. The overall pooled distribution of preferences showed a strongly significant deviation from chance expectation (χ 2 = 148, df = 4, p < 0.0001). Of all five choices, 94 % either “agreed” or “strongly agreed” with the statement, while “strongly agree” had the largest number of expressed preferences (70.2 %; p < 0.0001) (Fig. 2).
Student opinion on radiology in assessment and in clinical practice. a Student opinion significantly demonstrated that radiology is a valid assessment tool in anatomy education (p < 0.0001). b The majority of significantly students agreed or strongly agreed that learning radiology is important for clinical practice (p < 0.0001)
Discussion
Musculoskeletal injuries are amongst the foremost conditions observed in clinical practice [59, 60]. Findings from medical schools in the US, Canada, UK, and Ireland [48, 61–70] suggest that students are not adequately prepared in musculoskeletal medicine to meet clinical need partially due to a lack in undergraduate training, which is highlighted by the deficiencies in radiology understanding. Musculoskeletal anatomy is a major component of the anatomy curriculum at our university (an entire semester, year 1), yet the blending of radiology into existing anatomy teaching was seen as critical to advance our teaching in line with professional healthcare demand and students’ need [7]. In the past, our department typically delivered practical anatomy teaching, which entailed informal radiological integration into donor-led practical sessions, in which students in groups of ten were assigned to a cadaver and were afforded the opportunity to dissect body tissues horizontally aligned to lecture topics, under the direction of an anatomy demonstrator and/or academic. Through small group modular donor-led learning our approach was to formally integrate selected lower limb MRI, CT, X-ray, angiograms, and ultrasound radiographs with prosected cadaveric tissues, osteology specimen, and anatomical models. This mode of team-based learning is a productive strategy that does not require additional teaching resources, yet has yielded success in a variety of anatomy curricula [71–75]. Moreover, consensus-led opinion amongst educators, students, and clinicians has shown that cadaveric assimilation is the most appropriate to formally incorporate radiology into anatomy curricula [35, 43, 48, 76]. In our study, the synergy between donor and radiology was enhanced by preparing prosected lower limbs and displaying osteology/anatomical models that aligned to radiographs, thus increasing time efficiency at each station [77, 78] and reducing dissection time, which often needs to be instructor led. This strategy contributed to a highly significant overall mark increase (p < 0.0001) for the practical examination element of the musculoskeletal component of the module, when compared with the previous year.
A number of important considerations need to be addressed when designing a multi-modal practical anatomy course, which seeks to integrate prosection, radiology, and the traditional teaching; namely, who is to source, prepare, and deliver radiology teaching on a continuous basis, and what technical facilities are required? Moreover, the vast majority of students surveyed as part of our and another study [23] had no prior experience of radiology, which will necessitate image interpretation and elements of diagnostic teaching, requiring a dedicated expert radiology contribution. The solution depends on the teaching philosophies and staffing arrangements of the medical school in question. While some may aim to up-skill a member of academic staff, others may engage radiologists as academic staff or may utilize hospital-based teaching resources. We chose to employ a radiology career oriented medically qualified member of teaching demonstration staff, whose mandate was to implement and teach the radiology components into practical anatomy sessions. Furthermore, weekly presentations were enabled primarily by an inclusive digital interactive display at each station. Our teaching facilities have been modernised in recent years, and authors appreciate that digital displays are not ubiquitous in all DTs and alternative presentation tools may need to be developed.
We found that the vast majority of students had no experience of radiology prior to attending our University. Although student’s unfamiliarity with radiology represents an additional learning element, we found that they agreed that radiology is important for their profession, and that it should be utilized in examination periods to assess anatomical knowledge. This demonstrates an understanding of the benefits of radiological competence prior to clinical practice [79] and is reflected by the fact that 73 % of students felt that radiology was most suited to clinically relevant anatomy. We also report good student satisfaction with radiology and a positive perceived benefit in the context of anatomy education, which is in agreement with other studies [57, 76, 80–83]. However, up to a third of our respondents indicated that the benefits of radiology depended on the imaging modality and 65 % of students surveyed felt that X-rays were the best radiological modality for learning lower limb musculoskeletal anatomy, a finding previously reported for full body gross anatomy [76]. X-rays demonstrate bony landmarks on a 2D image, which are relatively easy to interpret and, therefore, useful for understanding osteology and points of muscle attachment, a key outcome in musculoskeletal anatomy. Less than 30 % of students preferred MRI and/or CT as a learning modality in anatomy, which may be related to the more complex nature of interpreting 3D structures and clinical issues [76]. A recent study outlining surgeons’ opinions of radiology in anatomy education found that CT and MRI were most beneficial [7], which indicates that these modalities may need to be more formally introduced, perhaps, in didactic or specialised lectures taught prior to their amalgamation into donor-led practical sessions, especially when considering their benefits in improving the spatial relationships between structures in gross and arthrology-based musculoskeletal anatomy [55, 84]. In addition, aligning prosected lower limb joints and osteology specimen with selected X-ray, MRI, and CT radiographs greatly supported student appreciation of arthrology, though multiple planes of view [43, 81, 84–87]; while the opportunity to dissect these structures consolidated their understanding of biological variations, function, neuro-vasculature, and age-related pathologies [6, 7, 11].
Conclusion
In this report, we detail the process of integrating radiology into lower limb donor-led musculoskeletal anatomy practical sessions delivered to first-year medical students. Student opinion of the integration of radiology in anatomy practical sessions was positive as a learning tool in lower limb anatomy, as an assessment resource, and as a link to clinical practice.
References
Schober A et al (2014) “Anatomy and imaging”: 10 years of experience with an interdisciplinary teaching project in preclinical medical education—from an elective to a curricular course. Rofo 186(5):458–465
Swamy M, Searle RF (2012) Anatomy teaching with portable ultrasound to medical students. BMC Med Educ 12:99
Caswell FR, Venkatesh A, Denison AR (2015) Twelve tips for enhancing anatomy teaching and learning using radiology. Med Teach 37(12):1067–1071
Ebert RH (1992) Flexner’s model and the future of medical education. Acad Med 67(11):737–742
Fitzharris TP (1998) Survey of gross anatomy courses in the United States and Canada. Anat Rec 253(6):162–166
Arraez-Aybar LA, Bueno-Lopez JL, Moxham BJ (2014) Anatomists’ views on human body dissection and donation: an international survey. Ann Anat 196(6):376–386
Sheikh AH et al (2016) Cadaveric anatomy in the future of medical education: what is the surgeons view? Anat Sci Educ 9(2):203–208
Older J (2004) Anatomy: a must for teaching the next generation. Surgeon 2(2):79–90
Marom A, Tarrasch R (2015) On behalf of tradition: an analysis of medical student and physician beliefs on how anatomy should be taught. Clin Anat 28(8):980–984
Davis CR et al (2014) Human anatomy: let the students tell us how to teach. Anat Sci Educ 7(4):262–272
Azer SA, Eizenberg N (2007) Do we need dissection in an integrated problem-based learning medical course? Perceptions of first- and second-year students. Surg Radiol Anat 29(2):173–180
Den Op Akker JW et al (2002) Giving color to a new curriculum: bodypaint as a tool in medical education. Clin Anat 15(5):356–362
Barry DS et al (2016) Anatomy education for the YouTube generation. Anat Sci Educ 9(1):90–96
Stirling A, Birt J (2014) An enriched multimedia eBook application to facilitate learning of anatomy. Anat Sci Educ 7(1):19–27
Pickering JD (2015) Anatomy drawing screencasts: enabling flexible learning for medical students. Anat Sci Educ 8(3):249–257
Jacobson S et al (2009) Creation of virtual patients from CT images of cadavers to enhance integration of clinical and basic science student learning in anatomy. Med Teach 31(8):749–751
Mitchell BS, Williams JE (2002) Trends in radiological anatomy teaching in the U.K. and Ireland. Clin Radiol 57(12):1070–1072
Drake RL et al (2009) Medical education in the anatomical sciences: the winds of change continue to blow. Anat Sci Educ 2(6):253–259
Cho MJ, Hwang YI (2013) Students’ perception of anatomy education at a Korean medical college with respect to time and contents. Anat Cell Biol 46(2):157–162
Topping DB (2014) Gross anatomy videos: student satisfaction, usage, and effect on student performance in a condensed curriculum. Anat Sci Educ 7(4):273–279
Mukhtar Y, Mukhtar S, Chadwick SJ (2009) Lost at sea: anatomy teaching at undergraduate and postgraduate levels. Med Educ 43(11):1078–1079
Sheikh AH et al (2016) Cadaveric anatomy in the future of medical education: What is the surgeons view? Anat Sci Educ 9:203–208
Murphy KP et al (2014) Medical student knowledge regarding radiology before and after a radiological anatomy module: implications for vertical integration and self-directed learning. Insights Imaging 5(5):629–634
Shanks SC (1950) The place of radiology in the undergraduate medical curriculum. Med Press 224(13):291–293
Craig S et al (2010) Review of anatomy education in Australian and New Zealand medical schools. ANZ J Surg 80(4):212–216
Grignon B, Oldrini G, Walter F (2016) Teaching medical anatomy: what is the role of imaging today? Surg Radiol Anat 38:253–260
Jack A, Burbridge B (2012) The utilisation of radiology for the teaching of anatomy in Canadian medical schools. Can Assoc Radiol J 63(3):160–164
Zafar AM (2009) Radiology: an underutilized resource for undergraduate curricula. Med Teach 31(3):266
Kourdioukova EV et al (2011) Analysis of radiology education in undergraduate medical doctors training in Europe. Eur J Radiol 78(3):309–318
Ganske I et al (2006) Teaching methods in anatomy courses in North American medical schools the role of radiology. Acad Radiol 13(8):1038–1046
Kondrashov P et al (2015) Impact of the clinical ultrasound elective course on retention of anatomical knowledge by second-year medical students in preparation for board exams. Clin Anat 28(2):156–163
Colucci PG et al (2015) Development and utilization of a web-based application as a robust radiology teaching tool (radstax) for medical student anatomy teaching. Acad Radiol 22(2):247–255
Murakami T et al (2014) An integrated teaching method of gross anatomy and computed tomography radiology. Anat Sci Educ 7(6):438–449
Phillips AW et al (2012) Improved understanding of human anatomy through self-guided radiological anatomy modules. Acad Radiol 19(7):902–907
Gunderman RB, Wilson PK (2005) Viewpoint: exploring the human interior: the roles of cadaver dissection and radiologic imaging in teaching anatomy. Acad Med 80(8):745–749
de Barros N et al (2001) The value of teaching sectional anatomy to improve CT scan interpretation. Clin Anat 14(1):36–41
Orsbon CP, Kaiser RS, Ross CF (2014) Physician opinions about an anatomy core curriculum: a case for medical imaging and vertical integration. Anat Sci Educ 7(4):251–261
Dettmer S et al (2010) Teaching surgery, radiology and anatomy together: the mix enhances motivation and comprehension. Surg Radiol Anat 32(8):791–795
Wijnen-Meijer M et al (2010) Vertical integration in medical school: effect on the transition to postgraduate training. Med Educ 44(3):272–279
Feigin DS et al (2007) Learning and retaining normal radiographic chest anatomy: does preclinical exposure improve student performance? Acad Radiol 14(9):1137–1142
Roche A et al (2009) Physical examination of the foot and ankle by orthopaedic and accident and emergency clinicians. Injury 40(2):136–138
Buckenham T (2013) Undergraduate anatomy teaching: whose responsibility? J Med Imaging Radiat Oncol 57(3):261–262
Gunderman RB et al (2003) The vital role of radiology in the medical school curriculum. AJR Am J Roentgenol 180(5):1239–1242
Heitkamp DE, Gunderman RB (2014) The interventional radiology/diagnostic radiology certificate: asking the hard questions. Radiology 273(2):322–325
Afaq A, McCall J (2002) Improving undergraduate education in radiology. Acad Radiol 9(2):221–223
Drake RL (1998) Anatomy education in a changing medical curriculum. Anat Rec 253(1):28–31
Pascual TN et al (2011) Undergraduate radiology education in the era of dynamism in medical curriculum: an educational perspective. Eur J Radiol 78(3):319–325
Mirsadraee S et al (2012) Radiology curriculum for undergraduate medical studies—a consensus survey. Clin Radiol 67(12):1155–1161
Marker DR et al (2010) Developing a radiology-based teaching approach for gross anatomy in the digital era. Acad Radiol 17(8):1057–1065
Samuel S, Shaffer K (2000) Profile of medical student teaching in radiology: teaching methods, staff participation, and rewards. Acad Radiol 7(10):868–874
Heptonstall NB, Ali T, Mankad K (2016) Integrating radiology and anatomy teaching in medical education in the UK—the evidence, current trends, and future scope. Acad Radiol 23(4):521–526
Bhangu A et al (2010) A three-year prospective longitudinal cohort study of medical students’ attitudes toward anatomy teaching and their career aspirations. Anat Sci Educ 3(4):184–190
McLachlan JC et al (2004) Teaching anatomy without cadavers. Med Educ 38(4):418–424
McLachlan JC, Patten D (2006) Anatomy teaching: ghosts of the past, present and future. Med Educ 40(3):243–253
Erkonen WE et al (1992) Effectiveness of teaching radiologic image interpretation in gross anatomy. A long-term follow-up. Invest Radiol 27(3):264–266
Chowdhury R, Wilson ID, Oeppen RS (2008) The departments of radiology and anatomy: new symbiotic relations? Clin Radiol 63(8):918–920
Arya R et al (2013) Making education effective and fun: stations-based approach to teaching radiology and anatomy to third-year medical students. Acad Radiol 20(10):1311–1318
Phillips AW, Smith SG, Straus CM (2013) The role of radiology in preclinical anatomy: a critical review of the past, present, and future. Acad Radiol 20(3):297–304 (e1)
Lipkind KL (1995) National hospital ambulatory medical care survey: 1993 outpatient department summary. Adv Data 268:1–12
Yelin EH, Felts WR (1990) A summary of the impact of musculoskeletal conditions in the United States. Arthritis Rheum 33(5):750–755
Freedman KB, Bernstein J (2002) Educational deficiencies in musculoskeletal medicine. J Bone Joint Surg Am 84-A(4):604–608
Pinney SJ, Regan WD (2001) Educating medical students about musculoskeletal problems. Are community needs reflected in the curricula of Canadian medical schools? J Bone Joint Surg Am 83-A(9):1317–1320
DiCaprio MR, Covey A, Bernstein J (2003) Curricular requirements for musculoskeletal medicine in American medical schools. J Bone Joint Surg Am 85-A(3):565–567
Craton N, Matheson GO (1993) Training and clinical competency in musculoskeletal medicine. Identifying the problem. Sports Med 15(5):328–337
Mulhall KJ, Masterson E (2002) The prevalence of musculoskeletal complaints in Irish general practice: implications for musculoskeletal training. Ir Med J 95(6):186
Booth A, Wise DI (1990) General practice training in musculoskeletal disorders. Br J Gen Pract 40(338):390
DiGiovanni BF et al (2014) Factors impacting musculoskeletal knowledge and clinical confidence in graduating medical students. J Bone Joint Surg Am 96(21):e185
Al-Nammari SS et al (2015) The inadequacy of musculoskeletal knowledge in graduating medical students in the United Kingdom. J Bone Joint Surg Am 97(7):e36
Day CS et al (2007) Musculoskeletal medicine: an assessment of the attitudes and knowledge of medical students at Harvard Medical School. Acad Med 82(5):452–457
Skelley NW et al (2012) Medical student musculoskeletal education: an institutional survey. J Bone Joint Surg Am 94(19):e146 (1–7)
Whelan A et al (2016) Student perceptions of independent versus facilitated small group learning approaches to compressed medical anatomy education. Anat Sci Educ 9(1):40–51
Nieder GL et al (2005) Team-based learning in a medical gross anatomy and embryology course. Clin Anat 18(1):56–63
Vasan NS, DeFouw DO, Holland BK (2008) Modified use of team-based learning for effective delivery of medical gross anatomy and embryology. Anat Sci Educ 1(1):3–9
Martinez EG, Tuesca R (2014) Modified team-based learning strategy to improve human anatomy learning: a pilot study at the Universidad del Norte in Barranquilla, Colombia. Anat Sci Educ 7(5):399–405
Huitt TW, Killins A, Brooks WS (2015) Team-based learning in the gross anatomy laboratory improves academic performance and students’ attitudes toward teamwork. Anat Sci Educ 8(2):95–103
Murphy KP et al (2015) Medical student perceptions of radiology use in anatomy teaching. Anat Sci Educ 8(6):510–517
Pabst R (2009) Anatomy curriculum for medical students: what can be learned for future curricula from evaluations and questionnaires completed by students, anatomists and clinicians in different countries? Ann Anat 191(6):541–546
Benninger B, Matsler N, Delamarter T (2014) Classic versus millennial medical lab anatomy. Clin Anat 27(7):988–993
Slanetz PJ, Kung J, Eisenberg RL (2013) Teaching radiology in the millennial era. Acad Radiol 20(3):387–389
Rizzolo LJ et al (2006) Design principles for developing an efficient clinical anatomy course. Med Teach 28(2):142–151
Shaffer K, Small JE (2004) Blended learning in medical education: use of an integrated approach with web-based small group modules and didactic instruction for teaching radiologic anatomy. Acad Radiol 11(9):1059–1070
Turmezei TD, Tam MD, Loughna S (2009) A survey of medical students on the impact of a new digital imaging library in the dissection room. Clin Anat 22(6):761–769
Kotze SH, Mole CG, Greyling LM (2012) The translucent cadaver: an evaluation of the use of full body digital X-ray images and drawings in surface anatomy education. Anat Sci Educ 5(5):287–294
Erkonen WE et al (1990) Gross anatomy instruction with diagnostic images. Invest Radiol 25(3):292–294
Bassett LW, Squire LF (1985) Anatomy instruction by radiologists. Invest Radiol 20(9):1008–1010
Lanier L, Kaude JV (1993) Radiologic anatomy–a credit course for first-year medical students. Acta Radiol 34(4):414–416
Clough RW, Lehr RP (1996) Testing knowledge of human gross anatomy in medical school: an applied contextual-learning theory method. Clin Anat 9(4):263–268
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest during the preparation of this manuscript or as part of its intended publication.
Rights and permissions
About this article
Cite this article
Davy, S., O’Keeffe, G.W., Mahony, N. et al. A practical description and student perspective of the integration of radiology into lower limb musculoskeletal anatomy. Ir J Med Sci 186, 409–417 (2017). https://doi.org/10.1007/s11845-016-1487-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-016-1487-6