Abstract
Background
The association between gastroesophageal reflux disease (GERD) and obesity is clearly defined. The incidence of erosive esophagitis (EE) and Barrett’s esophagus (BE) are as high as 26 and 6%, respectively. Gastric bypass (GBP) is considered the gold standard for obese patients with GERD. Evidence about the impact of GBP on EE and BE is not yet clear but more inspiring every day.
Methods
Obese patients operated by GBP with EE or BE were included for this study. Demographics, BMI, %EWL, and the evolution of EE and BE with pre and postoperative upper endoscopy were analyzed.
Results
In this study, 64 patients were included, 55 with EE and 9 with BE. The preoperative BMI was 44.29 km/m2 ± 3.5 and the %EWL was 78.5 ± 5.8 in the first year postoperative. Preoperatively, EE was distributed as follows: A: 54.5% (30), B: 34.5% (19), C: 9% (5), D: 2% (1). BE findings were the following: short segment (SSBE): 45% (4) and long segment (LSBE): 55% (5). Postoperatively, 80% of the patients with EE resolved their condition, 11% improved, 7% had no changes, and 2% worsened. From the patients with SSBE, 75% resolved their condition and 40% with LSBE resolved their condition after 24 months and no patient progressed to dysplasia.
Conclusion
Patients with EE had a statistically significant resolution after GBP. BE was improved or even resolved in many patients without acquiring significance but also without progression. Long-term surveillance data is necessary to define the certain evolution of EE and BE after GBP.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The association between GERD and obesity has been demonstrated among the literature with an incidence as high as 50–100% of obese patients while is only 8–26% in non-obese [1,2,3,4,5,6,7]. GERD is also associated with EE and BE as a pathophysiological risk factor [8, 9]. In bariatric patients, the incidence of EE and BE is 12–26% and 0.1–6%, respectively [6, 10,11,12,13].
The reasons that have classically explained the association between obesity and GERD are the increase of intraabdominal and intragastric pressure, the inversion of the gastroesophageal gradient, and the augmented incidence of hiatal hernia (HH) in the obese patients. On the other hand, non-obese patients that suffer from GERD have been more associated with a hypotensive inferior esophageal sphincter and to abnormal peristalsis of the esophagus [14, 15]. Since the pathophysiological mechanisms involved in GERD are different between obese and non-obese subjects, the approach is to be different as well. Obese patients with GERD might achieve better outcomes with a GBP than with an anti-reflux procedure (ARP). GERD recurrence, the low resolution of the disease, and even the progression of EE to BE and cancer have been reported in obese patients after ARP [16,17,18,19,20]. However, similar results between obese and non-obese patients after ARP could be also found in the literature [21,22,23,24,25,26,27,28] even with comparable resolution outcomes and/or endoscopic-histological regression in a variable rate in patients with EE and EB [16, 26,27,28].
Nevertheless, GBP seems to be an excellent option for obese patients with GERD and is being considered as the gold standard procedure by many authors [29,30,31,32,33]. Different studies would report a resolution of EE and BE between 36 and 62%, but the evidence might not be clear enough yet [6, 7, 34,35,36].
This report aims to assess the endoscopic and histological evolution of EE and BE after GBP in obese patients.
Methods
A retrospective analysis of a prospectively collected database of consecutive patients operated by GBP in Hospital Privado Universitario de Cordoba and Clinica Universitaria Reina Fabiola two tertiary care academic hospitals from Cordoba, Argentina, from January 2013 to April 2017 was conducted.
Demographics, BMI, and %EWL have been analyzed pre- and postoperatively. Upper endoscopy (UE) was performed to every patient preoperatively and after 12 months postoperatively. Los Angeles criteria were used for the evaluation of EE [37]. Biopsies were taken for histologic analysis following the Seattle criteria [38]. BE was classified as short segment (SSBE) when it was shorter than 3 cm and long segment (LSBE) when it was larger than 3 cm. Every patient with EE and BE received proton pump inhibitors (PPI) for 6 months after surgery. EE and BE resolution were established when normal epithelia were found in the esophageal gastric junction (EGJ) after BE or EE had been recorded.
All the procedures were performed in a standardized fashion by the same surgeon (FM). The patient was positioned with open legs, the primary surgeon on the right, the assistant on the left, and the camaraman in between legs. Four trocars and the Nathanson’s liver retractor were used. A 30–40 cc gastric pouch was constructed along the lesser curvature with a termino-lateral gastrojejunostomy using a 45 mm blue cartridge calibrated at 30 mm. The stapler stoma was closed using two planes of a 3–0 vycril running suture. A 60-cm-long biliopancreatic limb is anastomosed in a side-to-side fashion with a 120 cm alimentary (Roux) limb using a 45 mm white cartridge, and the stoma was closed with a vycril running suture. The Petersen and the mesenteric defect were closed using 2–0 ethibond. Routine dissection of the entire hiatus was not performed, even though, when a hiatal hernia was visible on preoperative studies or after dissection of the fundus and exposure of the left crus, it was repaired.
Results
During the study period, 115 GBP were analyzed, 40 of them were excluded from the study because of the absence of EE or BE. After that, 11 patients were also excluded for lacking clear endoscopy reports or biopsies in the postoperative control. For the final evaluation, 64 patients were included, 55 suffered from EE and 9 from BE.
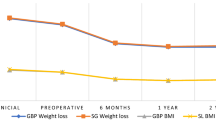
The mean age was 46.9 years, and 58.6% of the patients were females. Mean preoperative weight and BMI was 120 kg ± 11.5 and 44.29 kg/m2 ± 3.5. %EWL after 12 months from surgery was 78.5% ± 5.8 (Table 1).
Evolution of EE after GBP
Preoperatively, EE was evidenced in 55 patients. According to Los Angeles criteria, 54.5% [30] were grade A, 34.5% [19] grade B, 10% [5] grade C, and 2% [1] grade D. Postoperatively, 87% [26] of grade A patients resolved their condition with statistical significance (p = 0.001), 9% [3] remained without changes, and 3% [1] progressed to grade B. Grade B patients resolved in 84% [16] of the cases, improved to grade A in 10.5% [2] and 5.5% [1] remained without changes. Eighty percent [4] of the patients with grade C EE improved to grade A, and 20% [1] resolved the condition. Endoscopic resolution was found in the only patient with grade D EE.
Overall, out of 55 patients with EE preoperatively, 80% [39] resolved their condition, 11% [6] improved, 7% [4] remained without changes, and 2% [1] worsened from grade A to grade B. Finally, 91% (50) patients resolved or improved EE and 7% remained without changes. Only 1 patient had disease progression after surgery (Fig. 1).
Evolution of BE after GBP
BE esophagus was histologically diagnosed in 9 patients. The mean length was 3.5 cm (1–7 cm). SSBE was found in 45% [4] and LSBE in 55% [5]. These patients received more than one postoperative endoscopy (mean 1.6, range 1–3). After surgery, 75% [3] of the patients with SSBE resolved their condition and one patient remained without changes after 15 ± 6 months (p = NS) (Table 1). From the 5 patients with LSBE, 2 (40%) resolved the condition after 24 ± 3 months (p = NS), 2 patients shortened the length of the esophagitis, and one patient remained the same. The mean postoperative length was 2 cm (2–7 cm). Neither worsening nor progression to dysplasia was registered (Fig. 2).
Discussion
Since obesity is directly associated with GERD, it is also correlated with GERD consequences such as EE, BE, and esophagus adenocarcinoma [8, 9, 40]. Obese patients have a 3.3-fold higher prevalence of EE than non-obese and every 5 units of BMI increment, the risk of BE is 35% higher [40, 41]. Moreover, the incidence of EE and BE in obese patients submitted to bariatric surgery is 13–26% and 0.1–6% respectively [6, 10, 13].
As mentioned, the pathophysiological pathways related to GERD are different between obese and non-obese patients and this might have a great impact on its surgical approach.
Results of Antireflux Surgery in Obese Patients
Nowadays, the best surgical option for obese patients with GERD is a matter of debate. Results of ARP in the obese might be conflicting. Anvari et al. report no differences in surgical time, complications, and reoperations in 70 Nissen procedures in obese patients compared with the other reports [21]. Similar experiences have been published by other authors with complication rates, patient satisfaction, reoperations, or hiatal hernia recurrence in obese patients submitted to ARP similar to the general population. In these reports, authors do not consider obesity as a contraindication for ARP [21,22,23,24,25]. In addition to this, endoscopic and histologic resolution of EE and BE have also been reported in obese patients after ARP [26,27,28].
On the other hand, several authors showed a worse symptomatic control of GERD, with more recurrence of the disease and a relatively low regression of EE and BE. Even more, the progression of BE to dysplasia and esophageal cancer have been reported after ARP in the obese [16,17,18,19,20].
GBP seems to be an excellent option in patients with GERD and is being already considered the gold standard approach for this situation by some authors [29,30,31,32,33]. Anatomic modifications in GBP such as the creation of a small gastric pouch excluding most of the acid production and the Roux-en-Y configuration produce an improvement in GERD symptoms even without weight loss [38, 40]. Madalosso et al. prospectively evaluated 86 patients using Montreal classification and pH-meter and found a statistically significant decrease in typical symptoms of GERD and acid exposure of the esophagus after GBP [29]. The improvement of symptomatic control of GERD in obese with a reduction of PPI consumption after GBP have been reported by other authors as well [30, 31, 33]. Merrouche in a prospective cohort study evidenced a statistically significant improvement regarding symptoms, DeMeester score, manometry, and endoscopy findings after GBP in obese patients with GERD [42]. There are also many publications in the literature review that consider superior outcomes of GBP in this group of patients when comparing it to other surgical approaches among bariatric surgery [33, 39, 43, 44].
As mentioned before, EE incidence in the bariatric population is 13–26%. The presence of EE is considered a consequence of GERD by our team and GBP is offered to these patients. However, endoscopic surveillance after surgery is not widely reported. Overall, the existing reports in the literature show results that are similar to our experience. Braghetto, Csendes, and Czeczko have reported a postoperative remission as high as 100% [6, 35, 39]. In the experience of Madalosso et al., 22 patients out of 36 resolved EE after GBP, 5 improved the condition, 6 stayed the same and 3 worsened [29]. In a prospective cohort that included 130 patients, EE disappeared in 95% of the patients after 85 months of follow-up [45]. In our experience, 80% of the 55 patients resolved EE, 11% improved, 7% remained without changes and only one patient worsened (from A to B EE). Summarizing, 91% healed or improved EE, 7% remained the same, and 1 patient worsened. These results might be consistent enough to show the impressive benefit that GBP might offer to the obese patient with EE. Moreover, the clear association of EE and GERD might justify the extrapolation of this experience for the treatment of the obese patient with GERD and associated its conditions such as EE, extraesophageal symptoms, and even hiatal hernia. As a matter of fact, after the analysis of these results, GBP is the standard treatment for GERD in the severely obese population at our department. It seems that the direct strike to both basics pathophysiological issues, overweight and gastric acid emptying, provided by GBP result in an improvement of GERD in the obese that has not been reported by any other treatment.
BE is a consequence of EE where the squamous epithelium of the esophagus is replaced by intestinal metaplasia in an intention to heal the injury on the mucosa caused by the gastric acid reflux [6, 7]. This condition is recognized as premalignant for esophageal adenocarcinoma (EA) [7, 34, 46]. The incidence of EA in patients with BE increases by 0.1–0.3% per year [46]. In non-obese patients, EA incidence is 1.2% while in the obese reaches 6–7% [6, 10, 13]. A statistically significant association between BE, EA, and obesity have been reported where the risk of BE and EA is increased 12 and 16% for every point in the BMI in the obese [47]. Regarding BE in the obese, some reports showed a resolution of the condition after ARP, especially with SSBE [48, 49]. Even though, this type of surgery will not have any effect on obesity and progression rates to dysplasia or cancer might reach 7% [16,17,18,19]. Gorodner et al. pointed out this issue establishing that ARP might be an incomplete treatment for obese patients with GERD, especially when BE is evidenced [7]. Confirmation about BE resolution after GBP are scarce but promising, to our knowledge, there are no more than 5 publications that have expressly regarded this topic. Houghton et al. reported the evolution of 5 patients with BE that had a mean length of 6 cm (3–14 cm). Also, two of them had high-grade dysplasia and one undetermined dysplasia. After 34 months of follow-up, mean BE length decreased to 2 cm, dysplasia disappeared in two patients and improved to low grade in one. Complete remission of BE was observed in 40% of the patients and all of them evidenced improvement in length or dysplasia severity. The authors concluded that GBP should be the procedure of choice in obese with BE [36]. Andrew et al. studied 14 patients with SSBE and reported a resolution of 43% after GBP without progression to dysplasia in any case [34]. Gorodner et al. informed postoperative results in 11 patients with BE (9 SSBE and 2 LSBE) with 41 months of follow-up. They found a decrease in the mean length from 2.1 to 1.2 cm especially in SSBE, 36% of the patients resolved the condition and neither progression nor dysplasia was evidenced [7]. In the experience of Braghetto and Csendes, a resolution of 62% of the patients was reported. In another publication of the same group, they showed a resolution of 57% in SSBE and 20% in LSBE without progression in any case of both studies [6, 35]. Our experience showed similar results, the post-operative mean length improved from 3.5 to 2 cm, SSBE 75% of the patients achieved resolution and 40% in LSBE. Moreover, patients that did not resolve their condition showed improvement in length of BE and no progression or dysplasia was observed after surgery.
The present study did have some limitations. The retrospective study design might have decreased the quality of the data, and the sample size might have increased the likelihood of beta error. In addition, we did not perform functional studies neither evaluated the symptomatic association of our findings. On the other hand, there is little analysis about the esophagitis and Barrett esophagus evolution after GBP and this can be easily categorized following a standardized classification such as Los Angeles. Because of this consistent definition, the results might be more reliable than those from GERD symptom-based studies.
In the overall, most of the publications show encouraging results after GBP for both conditions EE and BE. The literature might be still scarce for the last, but length improvement, mean resolution of about 40% without progression or de novo dysplasia and even dysplasia improvement and resolution are promising results. Systematic endoscopic surveillance is still fundamental to establish the long term evolution of this particular group of patients.
Conclusion
In our experience, GBP promotes endoscopic and histologic improvement and/or the resolution of EE and BE in obese patients. No progression was recorded within a follow-up of 12 to 24 months. Long-term surveillance is necessary to determine the definite evolution in these patients.
References
Hong D, Khajanchee YS, Pereira N, et al. Manometric abnormalities and gastroesophageal reflux disease in the morbidly obese. Obes Surg. 2004;14:744–9.
Nelson LG, Gonzalez R, Haines K, et al. Amelioration of gastroesophageal reflux symptoms following roux-en-Y gastric bypass for clinically significant obesity. Am Surg. 2005;71:950–3.
El-Serag HB, Ergun GA, Pandolfino J, et al. Obesity increases oesophageal acid exposure. Gut. 2007;56:749–55.
Friedenberg FK, Xanthopoulos M, Foster GD, et al. The association between gastroesophageal reflux disease and obesity. Am J Gastroenterol. 2008;103:2111–22.
Corley DA, Kubo A. Body mass index and gastroesophageal reflux disease: a systematic review and meta-analysis. Am J Gastroenterol. 2006;101:2619–28.
Braghetto I, Korn O, Csendes A, et al. Laparoscopic treatment of obese patients with Gastroesophageal reflux disease and Barrett’s esophagus: a prospective study. Obes Surg. 2012;22:764–72.
Gorodner V, Buxhoeveden R, Clemente G, et al. Barrett’s esophagus after roux-en-Y gastric bypass: does regression occur? Surg Endosc. 2017;31:1849–54.
Koo JS, Lee SW, Park SM, et al. Abdominal obesity as a risk factor for the development of erosive esophagitis in subjects with a Normal Esophago-gastric junction. Gut Liver. 2009;3:276–84.
El-Serag H, Graham D, Satia J, et al. Obesity is an Independient risk factor for GERD symptoms and erosive esophagitis. Am J Gastroenterol. 2005;100:1243–50.
Csendes A, Burgos A, Smok G, et al. Endoscopic and histologic findings of the foregut in 426 patients with morbid obesity. Obes Surg. 2007;17:28–34.
Schigt A, Coblijn U, Lagarde S, et al. Is esophagogastroduodenoscopy before roux-en-Y gastric bypass or sleeve gastrectomy mandatory? Surg Obes Relat Dis. 2014;10:411–8.
Peromaa-Haavisto P, Victorzon M. Is routine preoperative upper GI endoscopy needed prior to gastric bypass? Obes Surg. 2013;23:736–9.
Muñoz R, Ibañez L, Salinas J, et al. Importance of routine preoperative upper GI endoscopy: why all patients should be evaluated? Obes Surg. 2009;19:427–31.
Fisichella PM, Patti MG. Gastroesophageal reflux disease and morbid obesity: is there a relation? World J Surg. 2009;33:2034–8.
Prachand VN, Alverdy JC. Gastroesophageal reflux disease and severe obesity: fundoplication or bariatric surgery? World J Gastroenterol. 2010;16:3757–61.
Morrow E, Bushyhead D, Wassenaar E, et al. The impact of laparoscopic anti-reflux surgery in patients with Barrett’s esophagus. Surg Endosc. 2014;28:3279–84.
Perez AR, Moncure AC, Rattner DW. Obesity adversely affects the outcome of antireflux operations. Surg Endosc. 2001;15:986–9.
Morgenthal CB, Lin E, Shane MD, et al. Who will fail laparoscopic Nissen fundoplication? Preoperative prediction of long-term outcomes. Surg Endosc. 2007;21:1978–84.
Braghetto I, Korn O, Valladares H, et al. Laparoscopic surgical treatment for patients with short- and long segment Barrett’s esophagus: which technique in which patient? Int Surg. 2011;96:95–103.
Tekin K, Toydemir T, Yerdel MA. Is laparoscopic antireflux surgery safe and effective in obese patients? Surg Endosc. 2012;26:86–95.
Anvari M, Bamehriz F. Outcome of laparoscopic Nissen fundoplication in patients with body mass index >or=35. Surg Endosc. 2006;20:230–4.
Winslow ER, Frisella MM, Soper NJ, et al. Obesity does not adversely affect the outcome of laparoscopic antireflux surgery (LARS). Surg Endosc. 2003;17:2003–11.
Chisholm JA, Jamieson GG, Lally CJ, et al. The effect of obesity on the outcome of laparoscopic antireflux surgery. J Gastrointest Surg. 2009;13:1064–70.
D'Alessio MJ, Arnaoutakis D, Giarelli N, et al. Obesity is not a contraindication to laparoscopic Nissen fundoplication. J Gastrointest Surg. 2005;9:949–54.
Fraser J, Watson DI, O’Boyle CJ, et al. Obesity and its effect on outcome of laparoscopic Nissen fundoplication. Dis Esophagus. 2001;14:50–3.
Broeders JA, Draaisma WA, Bredenoord AJ, et al. Long-term outcome of Nissen fundoplication in non-erosive and erosive gastro-oesophageal reflux disease. Br J Surg. 2010;97:845–52.
Oelschlager BK, Barreca M, Chang L, et al. Clinical and pathologic response of Barrett’s esophagus to laparoscopic antireflux surgery. Ann Surg. 2003;238:458–64.
O'Riordan JM, Byrne PJ, Ravi N, et al. Long-term clinical and pathologic response of Barrett’s esophagus after antireflux surgery. Am J Surg. 2004;188:27–33.
Madalosso CA, Gurski RR, Callegari-Jacques SM, et al. The impact of gastric bypass on gastroesophageal reflux disease in patients with morbid obesity: a prospective study based on the Montreal consensus. Ann Surg. 2010;251:244–8.
Nelson LG, Gonzalez R, Haines K, et al. Amelioration of gastroesophageal reflux symptoms following Roux-en-Y gastric bypass for clinically significant obesity. Am Surg. 2005;71:950–3.
Frezza EE, Ikramuddin S, Gourash W, et al. Schauer. Symptomatic improvement in gastroesophageal reflux disease (GERD) following laparoscopic Roux-en-Y gastric bypass. Surg Endosc. 2002;16(7):1027–31.
Perry Y, Courcoulas AP, Fernando HC, et al. Laparoscopic Roux-en-Y gastric bypass for recalcitrant gastroesophageal reflux disease in morbidly obese patients. JSLS. 2004;8:19–23.
Kindel TL, Oleynikov D. The improvement of gastroesophageal reflux disease and Barrett’s after bariatric surgery. Obes Surg. 2016;26:718–20.
Andrew B, Alley JB, Aguilar CE, et al. Barrett's esophagus before and after Roux-en-Y gastric bypass for severe obesity. Surg Endosc. 2018;32(2):930–6.
Csendes A, Burgos AM, Smok G, et al. Effect of gastric bypass on Barrett’s esophagus and intestinal metaplasia of the cardia in patients with morbid obesity. J Gastrointest Surg. 2006;10:259–64.
Houghton SG, Romero Y, Sarr MG. Effect of Roux-en-Y gastric bypass in obese patients with Barrett's esophagus: attempts to eliminate duodenogastric reflux. Surg Obes Relat Dis. 2008;4:1–4.
Lundell LR, Dent J, Bennett JR, et al. Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut. 1999;45:172–80.
Levine DS, Haggitt RC, Blount PL, et al. An endoscopic biopsy protocol can differentiate high-grade dysplasia from early adenocarcinoma in Barrett’s esophagus. Gastroenterology. 1993;105:40–50.
Barr AC, Frelich MJ, Bosler ME, et al. GERD and acid reduction medication use following gastric bypass and sleeve gastrectomy. Surg Endosc. 2017;31:410–5.
Stein DJ, El-Serag HB, Kuczynski J, et al. The association of body mass index with Barrett's oesophagus. Aliment Pharmacol Ther. 2005;22:1005–10.
Gorodner V, Viscido G, Signorini F, et al. Gastroesophageal reflux disease and morbid obesity: evaluation and treatment. Updat Surg. 2018 Aug 24;70:331–7. https://doi.org/10.1007/s13304-018-0579-4.
Merrouche M, Sabaté JM, Jouet P, et al. Gastro-esophagealreflux and esophageal motility disorders in morbidly obese patients before and after bariatric surgery. Obes Surg. 2007;17:894–900.
Pallati PK, Shaligram A, Shostrom VK, et al. Improvement in gastroesophageal reflux disease symptoms after various bariatric procedures: review of the Bariatric Outcomes Longitudinal Database. Surg Obes Relat Dis. 2014;10:502–7.
Jackson TD, Hutter MM. Morbidity and effectiveness of laparoscopic sleeve gastrectomy, adjustable gastric band, and gastric bypass for morbid obesity. Adv Surg. 2012;46:255–68.
Csendes A, Smok G, Burgos AM, et al. Prospective sequential endoscopic and histologic studies of the gastric pouch in 130 morbidly obese patients submitted to Roux-en-Y gastric bypass. Arq Bras Cir Dig. 2012;25:245–9.
Spechler SJ, Souza RF. Barrett’s esophagus. N Engl J Med. 2014;37:836–45.
Hofstetter WL, Peters JH, DeMeester TR, et al. Long-term outcome of antireflux surgery in patients with Barrett’s esophagus. Ann Surg. 2001;234:532–8.
Czeczko LE, Cruz MA, Klostermann FC, et al. Correlation between pre and postoperative upper digestive endoscopy in patients who underwent Roux-en-Y gastrojejunal bypass. Arq Bras Cir Dig. 2016;29:33–7.
Thrift AP, Shaheen NJ, Gammon MD, et al. Obesity and risk of esophageal adenocarcinoma and Barrett’s esophagus: a Mendelian randomization study. J Natl Cancer Inst. 2014;106:dju252.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Informed Consent
For this type of study, formal consent is not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Signorini, F., Viscido, G., Bocco, M.C.A. et al. Impact of Gastric Bypass on Erosive Esophagitis and Barret’s Esophagus. OBES SURG 30, 1194–1199 (2020). https://doi.org/10.1007/s11695-019-04333-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04333-1