Abstract
Background
Different bariatric surgeries have demonstrated different effectiveness for weight loss and glucose control in obese persons with diabetes, over a short follow-up time. The aim of this study was to compare weight loss, glucose control, and diabetes remission in individuals with type 2 diabetes, after three types of bariatric surgery: gastric banding (GB), sleeve gastrectomy (SG), and Roux-en-Y gastric bypass (RYGB), with 5 years follow-up.
Methods
A retrospective study was conducted on bariatric surgeries performed during 2002–2011 in a large nationwide healthcare organization.
Results
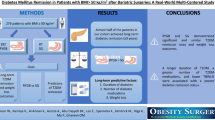
Of 2190 patients, 64.8 % were women. The operations performed were 1027 GB, 1023 SG, and 140 RYGB. Mean BMI ± SD at baseline, 1 year postoperatively, and 5 years postoperatively were 43.5 ± 6.18, 37.1 ± 6.35, and 35.5 ± 6.48 for GB; 43.6 ± 6.42, 34.4 ± 6.08, and 35.3 ± 6.7 for SG; and 42.8 ± 5.81, 32.8 ± 4.9, and 34.1 ± 5.09 for RYGB. Mean HbA1c ± SD at baseline, 1 year postoperatively, and 5 years postoperatively were 7.6 + 1.58, 6.5 + 1.22, and 6.8 + 1.48 for GB; 7.7 + 1.63, 6.4 + 1.18, and 6.7 + 1.57 for SG; and 8.0 + 1.78, 6.3 + 0.98, and 7.04 + 1.42 for RYGB. At 1 year follow-up, 53.2 % had achieved remission; at 5 years, 54.4 %. Remission rates at 5 years were similar for the three surgeries. Five-year remission was inversely associated with baseline HbA1c and with treatment with insulin at baseline and positively associated with BMI.
Conclusions
For all three surgeries, diabetes remission was higher than the baseline after 5 years; mean BMI and HbA1c decreased considerably during the first year postoperatively and remained lower than basal values throughout follow-up. Early improvements were greatest for RYGB, though the advantage over the other operations diminished with time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
About one in every seven persons in the world is obese, summing to over one half billion people [1]. About 347 million persons were estimated to have diabetes in the year 2008, which is more than double the number three decades before [2]. Despite the increases in obesity and diabetes, “diabetes remission” has emerged as a possibility, specifically in conjunction with bariatric surgery. The most recently issued guidelines of the American Diabetes Association include bariatric surgery as a treatment for adults with BMI >35 kg/m2 and with type 2 diabetes, “especially if diabetes or associated comorbidities are difficult to control with lifestyle and pharmacological therapy” [3]. Two recently published meta-analyses, with more than 1 year [4] and more than 2 years follow-up [5], concluded that bariatric surgery is more effective than conventional medical therapy for weight loss and glucose control in obese persons with diabetes. A retrospective review of medical records in the USA and the Swedish Obese Subjects prospective study showed such benefit to persist at a median of 6 years and 17.6 years, respectively [6, 7]. However, outcomes by type of surgery were not analyzed in these studies.
Gastric banding (GB), Roux-en-Y gastric bypass (RYGB), and sleeve gastrectomy (SG) are the three main bariatric procedures that are currently performed in Israel. RYGB has shown substantial weight loss and improvement in glucose control in a number of observational studies of diabetic patients [8, 9] and better outcomes than lifestyle modification and/or medical therapy alone in randomized trials [10, 11]. Most studies that have compared types of bariatric surgery in obese individuals with diabetes have investigated outcomes between only two types of procedures.
We conducted an observational study based on electronic medical records from a large nationwide healthcare organization, to compare weight loss and improvement in glucose control in individuals with type 2 diabetes, after RYGB, GB, and SG, with 5 years follow-up.
Methods
This is a retrospective study based on the electronic medical records of Clalit Health Services (CHS), the largest healthcare organization in Israel, insuring and providing care to over four million Israeli citizens (53 % of the total population). Members of CHS with diabetes who underwent bariatric surgery during the years 1999–2011 were included in this study. Follow-up data were accessed until December 2014. Data from the electronic database of CHS included demographic characteristics: sex, age, marital status, and socioeconomic status (low, medium, high), according to affiliation to local CHS clinics, and baseline and follow-up values of clinical parameters, including weight, height, calculated BMI, fasting glucose, HbA1c, creatinine, systolic and diastolic blood pressure, total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides.
The criteria for the performance of bariatric surgery in CHS are BMI >40, or >35 kg/m2 and at least one obesity-related risk factor. These are the same criteria issued by the US Department of Health and Human Services, National Institutes of Health, for bariatric surgery for severe obesity (http://www.niddk.nih.gov/health-information/health-topics/weight-control/bariatric-surgery-severe-obesity/Pages/bariatric-surgery-for-severe-obesity.aspx#a [accessed July 17, 2015]).
The main outcomes of this study were changes in BMI and in HbA1c and the achievement of diabetes remission, defined as HbA1c <6 %, without the use of a diabetes medication except metformin. This definition was used since at CHS we treat some prediabetic patients (HbA1c 5.7–6.4 %) with metformin, in line with the current ADA guidelines for Prevention or Delay of Type 2 Diabetes [12]. Outcomes were assessed at 1, 2, and 5 years postoperatively.
Rabin Medical Center Ethics Committee approved the study.
Statistical Analysis
A comparison between three groups of patients according to procedure (GB, SG, and RYGB) regarding demographic (age, gender, etc.) and clinical (lab results, BMI) parameters was performed using one-way analysis of variance (ANOVA) and chi-square test, as applicable. Whenever the ANOVA test was significant, pair-wise comparisons were performed using the Gabriel post hoc test.
Multivariate logistic regression models were applied to the data to study simultaneously the independent relationship between clinical factors and diabetes remission at 1, 2, and 5 years after surgery. These models predict the probability of remission as a function of the explanatory variables. The statistical significance level was set to 0.05 and the power analysis was set to 90 %. Statistical analysis was done by SPSS for Windows software, version 20.0 (Chicago, IL).
Results
A total of 13,425 members of CHS underwent bariatric surgery during the study period. Of them, 2190 (16 %) were with diabetes: 64.8 % women and 35.2 % men. The operations performed were 1027 GB, 1023 SG, and 140 RYGB (Fig. 1). Table 1 presents demographic and clinical characteristics of the patients at baseline according to type of surgery. A higher proportion of the men underwent SG and a higher proportion of the women underwent RYGB. Mean baseline HbA1c was higher for the RYGB group, and a higher proportion of these patients used insulin. For the three groups, 9 % of the patients were at remission from diabetes at baseline, indicating that they had been diagnosed with diabetes, but already met our study criteria for remission when they underwent bariatric surgery. No secondary revisions or conversions were performed in 87.5 % of the patients who underwent GB and in 94 % of those who underwent SG.
Weight Reduction
During the first year postoperatively, mean BMI + SD at baseline, 1 year postoperatively, and 5 years postoperatively were 43.5 ± 6.18, 37.1 ± 6.35 (14.5 % weight loss from baseline weight [WL]), and 35.5 ± 6.48 (18.2 % WL) for GB; 43.6 ± 6.42, 34.4 ± 6.08 (21.0 % WL), and 35.3 ± 6.7 (19.0 % WL) for SG; and 42.8 ± 5.81, 32.8 ± 4.91 (23.5 % WL), and 34.1 ± 5.09 (20.5 % WL) for RYGB (Fig. 2). During the first year of follow-up, mean BMI decreased by 10.1, 9.2, and 6.3 units, for RYGB, SG, and GB, respectively. At 5 years follow-up, the mean decreases in BMI, from baseline, were more similar among the procedures: 8.8, 8.3, and 8.0, respectively.
Glucose Control
For the three procedures, a mean reduction of HbA1c of 1.0 % or more was maintained at all three time points. Mean HbA1c decreased by 2.0 % in the first year following RYGB, substantially and significantly more than following SG and GB (p < 0.001), and at 5 years was 1.4 % lower than the baseline mean (Fig. 3). The mean HbA1c decreased slightly more following SG than following GB (1.3 vs. 1.2 %) during the first year postoperatively; the difference in mean HbA1c reduction between SG and GB lessened during the subsequent 4 years. No statistically significant difference was observed among the procedures in HbA1c reduction after 5 years (p = 0.098).
Diabetes Remission
Considering all patients together, more than half were in diabetes remission at 1, 2, and 5 years follow-up (Table 2). At 1 year follow-up, remission rates were significantly higher for patients who underwent RYGB or SG, compared to GB. During the subsequent 4 years, rates of remission decreased for patients who underwent both RYGB and SG, and were equal for those who underwent GB, reaching similar rates for all the procedures.
Remission Prediction
In a multiple regression model (Table 3), SG and RYGB were associated with increased likelihood of diabetes remission at the three follow-up points, though the advantage over GB was not statistically significant at 5 years. Older age, higher baseline HbA1c, and treatment with insulin or with other diabetes medications at baseline were associated with decreased likelihood of diabetes remission at all follow-up points. Female gender was associated with lower likelihood of remission, which was only statistically significant in the first year. Higher baseline BMI was associated with diabetes remission.
Conclusions
The main findings of this large observational study of diabetic patients are the following: (1) the greatest reductions in BMI and HbA1c occurred during the first year following bariatric surgery; at 5 years post-operatively, improvements were attenuated, though still significantly below baseline. (2) Compared to SG and GB, RYGB showed a greater reduction in BMI during the first and second years, but this difference was diminished by 5 years follow-up. (3) Compared to SG and GB, RYGB showed a greater reduction in HbA1c, which lessened but persisted during the 5 years follow-up. (4) Diabetes remission was greater following RYGB and SG at the first year of follow-up but equal to that of GB at 5 years follow-up. (5) Older age, higher baseline HbA1c, and baseline insulin use predicted lower diabetes remission rates.
Over the long duration of this observational study, the distribution of operations changed greatly. Altogether, rates of RYGB, SG, and GB were 6, 47, and 47 %, respectively. During the same period, the distribution of operations among individuals without diabetes was 4, 32, and 64 %, respectively. The low rate of RYGB reflects the fact that it has been performed in Israel in considerable numbers only from 2009. Thus, the proportion of operations available for long-term analysis was even lower. Rates of GB remained constant throughout the study period and rates of SG increased dramatically since 2006. Similarly, an email questionnaire distributed in 2011 by the International Federation for the Surgery of Obesity and Metabolic Disorders revealed a substantial rise in the prevalence of SG during 2003–2013, making it the most frequently performed procedure in the USA, Canada, and Asia and second to RYGB in Europe and South America [13].
We showed that reduction in BMI was greater following RYGB than SG or GB during the first and second years postoperatively. A large meta-analysis [14], as well as more recent observational studies [6, 15], showed greater weight loss to be associated with more improved glucose control.
RYGB showed a greater mean reduction in HbA1c than did the other surgeries, which may be partially explained by the higher mean baseline HbA1c level of the RYGB group. This finding is in line with the prospective STAMPEDE study that showed RYGB to be more effective than SG in achieving HbA1c goals at 3 years postoperatively [16], and with small single-center observational studies that reported greater improvement in glucose control in obese patients with diabetes, following bypass and SG, compared to banding surgery, with up to 3 years follow-up [17, 18]. In contrast, a Spanish observational study showed similar rates of remission for the two procedures [15].
Nevertheless, the large magnitude of reduction in HbA1c levels following RYGB supports the notion that RYGB may have a role other than weight loss in improving glucose control. Examples of such effects include increases in peptide YY (PYY) and glucagon-like peptide-1 (GLP-1) [19–21], reduction in the hunger-stimulating hormone ghrelin [22], increased insulin sensitivity and enhanced β-cell function [23, 24], the enhancement of an alternative insulin-independent pathway for glucose transport [25], and increases in the regulation of glucose transporter-1, in basolateral glucose uptake, and in aerobic glycolysis, due to the exposure of the Roux limb to undigested nutrients [26]. In addition, the notion of microbiota alteration after RYGB has become an important explanation for these effects [27].
A multiple regression analysis that controlled for several demographic and clinical characteristics showed RYGB and SG to predict diabetes remission, compared to GB, though the advantage was not statistically significant at 5 years. Similarly, two large meta-analyses showed greater diabetes resolution following bypass than banding procedures [14, 28]. One of these analyses showed that diabetes resolution was also greater following bypass procedures than following sleeve gastrectomy [28]. The long-term positive results for GB in the current study, compared to other reports, may be due, at least in part, to the regular follow-up regime at some of our centers. The band was first adjusted 4–6 weeks after surgery and then five more times every 3 weeks, with the aim of reducing weight by 0.5–1 kg a week. Subsequent visits were scheduled at 6-month intervals.
Older age, higher baseline HbA1c, and insulin use were associated with lower rates of diabetes remission. Others have reported higher baseline HbA1c and insulin treatment at baseline to be associated with lower rates of diabetes remission [15, 29, 30]. We also found female gender to be negatively associated with remission during the first year postoperatively. Considering the poorer profile of our RYGB patients, characterized by a higher mean baseline HbA1c and a higher proportion of women and of insulin users at baseline, the achievement of a similar rate of remission suggests that RYGB may be more beneficial than other procedures for patients with diabetes. Hence, our study highlights the importance of considering patient characteristics in any study of bariatric surgery. The association of older age, higher baseline HbA1c, and the use of insulin and other diabetic medications with lower rates of diabetes remission stresses the importance of earlier bariatric surgery and suggests that a staging system and prediction models may contribute to decision-making about bariatric surgery procedures in diabetic patients.
Strengths of the current study are the large number of diabetes patients, the comparison of three rather than two procedures, and the 5 years follow-up including data for more than 70 % of the patients. Most studies that compared outcomes of types of bariatric surgery did not relate to the diabetes state of their patients. Differences that have been reported between those with and without diabetes support the separate analysis of outcomes on diabetes.
As an observational study, this research has a number of limitations. We did not assess and compare complications of the different bariatric procedures. We assessed BMI but not waist circumference, though the latter is considered a more relevant measure of adiposity for glucose control.
In conclusion, our study demonstrated weight loss and improvement in glucose control and diabetes remission following three types of bariatric surgeries, attenuated but still substantial after 5 years. A recent report that diabetes remission after RYGB and SG may be associated with distinct glycemic profiles suggests that different procedures may be more suited to different patients [31]. The present study showed greater weight reduction and improved glucose control following RYGB than SG or GB, and a higher likelihood of diabetes remission following RYGB or SG than GB. However, the attenuation of the advantage of RYGB during 5 years follow-up highlights the importance of long-term studies for comparing outcomes of bariatric procedures on diabetes disease and its complications.
References
Finucane MM, Stevens GA, Cowan MJ, et al. National, regional, and global trends in body-mass index since 1980, systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet. 2011;377(9765):557–67.
Danaei G, Finucane MM, Lu Y, et al. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980, systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2.7 million participants. Lancet. 2011;378(9785):31–40.
American Diabetes Association. Standards of medical care in diabetes-2015 abridged for primary care providers. Clin Diabetes. 2015;33(2):97–111.
Ribaric G, Buchwald JN, McGlennon TW. Diabetes and weight in comparative studies of bariatric surgery vs conventional medical therapy: a systematic review and meta-analysis. Obes Surg. 2014;24(3):437–55.
Yu J, Zhou X, Li L, et al. The long-term effects of bariatric surgery for type 2 diabetes: systematic review and meta-analysis of randomized and non-randomized evidence. Obes Surg. 2015;25(1):143–58.
Brethauer SA, Aminian A, Romero-Talamás H, et al. Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg. 2013;258(4):628–36.
Sjöström L, Peltonen M, Jacobson P, et al. Association of bariatric surgery with long-term remission of type 2 diabetes and with microvascular and macrovascular complications. JAMA. 2014;311(22):2297–304.
Kim MK, Kim W, Kwon HS, et al. Effects of bariatric surgery on metabolic and nutritional parameters in severely obese Korean patients with type 2 diabetes: a prospective 2-year follow up. J Diabetes Investig. 2014;5(2):221–7.
Lakdawala M, Shaikh S, Bandukwala S, et al. Roux-en-Y gastric bypass stands the test of time: 5-year results in low body mass index (30–35 kg/m2) Indian patients with type 2 diabetes mellitus. Surg Obes Relat Dis. 2013;9(3):370–8.
Ikramuddin S, Korner J, Lee WJ, et al. Roux-en-Y gastric bypass vs intensive medical management for the control of type 2 diabetes, hypertension, and hyperlipidemia: the Diabetes Surgery Study randomized clinical trial. JAMA. 2013;309(21):2240–9.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med. 2012;366(17):1577–85.
Prevention or delay of type 2 diabetes. Diabetes Care. 2015; 38(Suppl. 1):S31–2.
Angrisani L, Santonicola A, Iovino P, et al. Bariatric surgery worldwide 2013. Obes Surg 2015.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248–256.e5.
Jiménez A, Casamitjana R, Flores L, et al. Long-term effects of sleeve gastrectomy and Roux-en-Y gastric bypass surgery on type 2 diabetes mellitus in morbidly obese subjects. Ann Surg. 2012;256(6):1023–9.
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes—3-year outcomes. N Engl J Med. 2014;370(21):2002–13.
Abbatini F, Rizzello M, Casella G, et al. Long-term effects of laparoscopic sleeve gastrectomy, gastric bypass, and adjustable gastric banding on type 2 diabetes. Surg Endosc. 2010;24(5):1005–10.
Pham S, Gancel A, Scotte M, et al. Comparison of the effectiveness of four bariatric surgery procedures in obese patients with type 2 diabetes: a retrospective study. J Obes. 2014;2014:638203.
Karamanakos SN, Vagenas K, Kalfarentzos F, et al. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-YY levels after Roux-en-Y gastric bypass and sleeve gastrectomy: a prospective, double blind study. Ann Surg. 2008;247(3):401–7.
Ramón JM, Salvans S, Crous X, et al. Effect of Roux-en-Y gastric bypass vs sleeve gastrectomy on glucose and gut hormones: a prospective randomised trial. J Gastrointest Surg. 2012;16(6):1116–22.
Rhee NA, Vilsbøll T, Knop FK. Current evidence for a role of GLP-1 in Roux-en-Y gastric bypass-induced remission of type 2 diabetes. Diabetes Obes Metab. 2012;14(4):291–8.
Cummings DE, Weigle DS, Frayo RS, et al. Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med. 2002;346(21):1623–30.
Kashyap SR, Bhatt DL, Wolski K, et al. Metabolic effects of bariatric surgery in patients with moderate obesity and type 2 diabetes: analysis of a randomized control trial comparing surgery with intensive medical treatment. Diabetes Care. 2013;36(8):2175–82.
Jiao J, Bae EJ, Bandyopadhyay G, et al. Restoration of euglycemia after duodenal bypass surgery is reliant on central and peripheral inputs in Zucker fa/fa rats. Diabetes. 2013;62(4):1074–83.
Allen RE, Hughes TD, Ng JL, et al. Mechanisms behind the immediate effects of Roux-en-Y gastric bypass surgery on type 2 diabetes. Theor Biol Med Model. 2013;10:45.
Saeidi N, Meoli L, Nestoridi E, et al. Reprogramming of intestinal glucose metabolism and glycemic control in rats after gastric bypass. Science. 2013;341(6144):406–10.
Zhang H, DiBaise JK, Zuccolo A, et al. Human gut microbiota in obesity and after gastric bypass. Proc Natl Acad Sci U S A. 2009;106(7):2365–70.
Panunzi S, De Gaetano A, Carnicelli A, et al. Predictors of remission of diabetes mellitus in severely obese individuals undergoing bariatric surgery: do BMI or procedure choice matter? A meta-analysis. Ann Surg. 2015;261(3):459–67.
Chikunguwo SM, Wolfe LG, Dodson P, et al. Analysis of factors associated with durable remission of diabetes after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2010;6(3):254–9.
Schauer PR, Burguera B, Ikramuddin S, et al. Effect of laparoscopic Roux-en Y gastric bypass on type 2 diabetes mellitus. Ann Surg. 2003;238(4):467–84. discussion 84–5.
Jiménez A, Ceriello A, Casamitjana R, et al. Remission of type 2 diabetes after Roux-en-Y gastric bypass or sleeve gastrectomy is associated with a distinct glycemic profile. Ann Surg. 2015;261(2):316–22.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Since all data were obtained from medical records and no identifying information was included in any of the study documentations, informed consent from patients was not required.
All procedures performed were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
The work was performed in Clalit Health Services in Israel.
Rights and permissions
About this article
Cite this article
Dicker, D., Yahalom, R., Comaneshter, D.S. et al. Long-Term Outcomes of Three Types of Bariatric Surgery on Obesity and Type 2 Diabetes Control and Remission. OBES SURG 26, 1814–1820 (2016). https://doi.org/10.1007/s11695-015-2025-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-2025-8